Abstract
Fazio-Londe syndrome is a rare neurodegenerative disorder caused by riboflavin transporter deficiency. Clinical presentation includes variable hypotonia or muscle weakness, sensory gait ataxia, optic atrophy, sensorineural hearing loss, and bulbar palsies. We described the case of a 37-year-old patient with a suspected Fazio-Londe syndrome who was referred to us for oral incompetence with dysarthria and drooling and impaired facial expression. First, we provided static sling suspension of the lower lip with Silhouette sutures (Silhouette Lift). Due to recurrent sutures exposure, we had to remove the sutures and insert a bilateral fascia lata graft to resuspend the lower lip. Two months postoperatively, the patient had good oral competence and there were no complications. In our opinion, this is a simple and minimally invasive procedure that can restore the right lower lip position in challenging patients.
Introduction
Fazio-Londe syndrome is a rare neurodegenerative disorder caused by pathogenic mutations in SLC52A2 and SLC52A3 genes, which encode the riboflavin transporter. Clinical presentation includes variable hypotonia or muscle weakness, sensory gait ataxia, optic atrophy, sensorineural hearing loss, and bulbar palsies. Untreated cases have a low survival rate. Treatment is based on the administration of riboflavin (10 mg/kg). 1 Here, we describe the surgical treatment we offered to a patient with suspected Fazio-Londe syndrome with facial weakness and oral incompetence.
Case Report
A 37-year-old female presented with facial and limb weakness. Particularly she had bilateral facial weakness, her extraocular movements were full, but she presented with eyelid ptosis and difficulty in swallowing. She also had respiratory distress (she needed continuous positive airway pressure) and a hoarse voice. Further, she had oral incompetence with dysarthria and drooling, and impaired facial expression, causing a major functional and social impediment, and was therefore referred to us (Figure 1).
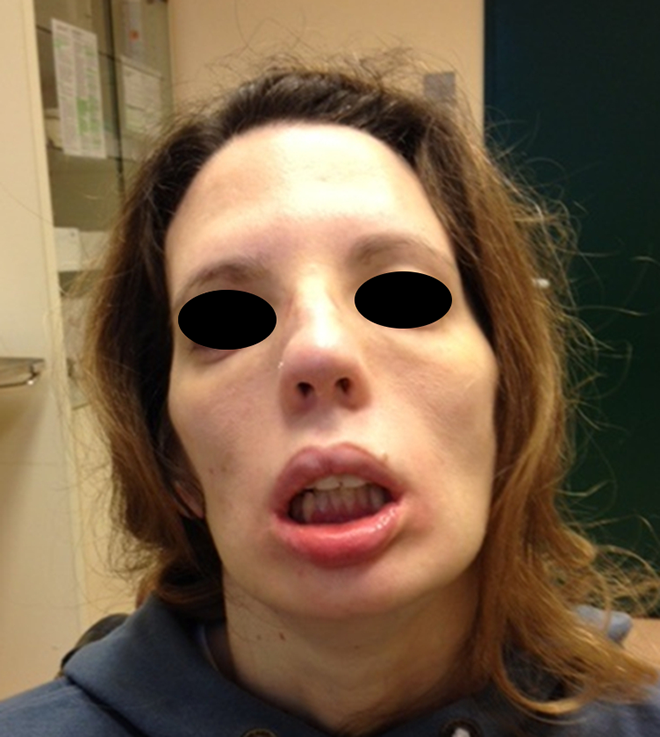
Preoperative figure.
Although molecular genetic testing could not identify either SLC52A2 or SLC52A3 mutations, clinical presentation and good response to riboflavin treatment led us to suspect Fazio-Londe syndrome caused by an unknown mutation with a slower clinical presentation.
Respiratory muscle weakness, dysphagia, and difficulty in clearing oropharyngeal secretions represented risk factors for ventilatory dysfunction with general anesthesia, which led us to provide first, under local anesthesia, static sling suspension of the lower lip with 3/0 polypropylene sutures with polylactic acid bioabsorbable cones (Silhouette Lift; Kolster Methods Inc, Corona, California). We passed the sutures from the preauricular region to the white roll of the lower lip through a subcutaneous tunnel and, after placing appropriate tension, we anchored the sutures to the deep temporal fascia bilaterally.
After surgery, the patient had no immediate complications and we were able to restore the static function of the lower lip. Restoration of an oral competence allowed improvement in deglutition, speech, and salivary continence.
Unfortunately, the patient experienced recurrent suture extrusion in the vestibular mucosa 5 and 23 months postoperatively and we had to replace the sutures. After 2 months from the last surgical procedure, the patient had one more episode of extrusion of the suture even if tensile strength was still present.
We decided to remove the sutures and substitute them with a bilateral fascia lata graft, eliminating synthetic materials and possible future extrusions. In order to reduce the operative time and to avoid possible complications in the donor area, we used a cadaveric fascia lata graft provided by Tissue Bank of our hospital (Treviso Tissue Bank Foundation, FBTV). Under general anesthesia, through a bilateral preauricular incision, we created a subcutaneous tunnel to reach an incision in the white roll of the lower lip. Then we tunneled the fascia sling from the preauricular region to the lower lip, creating a hammock-like support for the lower lip. Lastly, we sutured the fascia graft to the deep temporal fascia with a nonabsorbable suture (3/0 nylon suture), tightening it to restore the correct position of the lower lip (Figure 2).
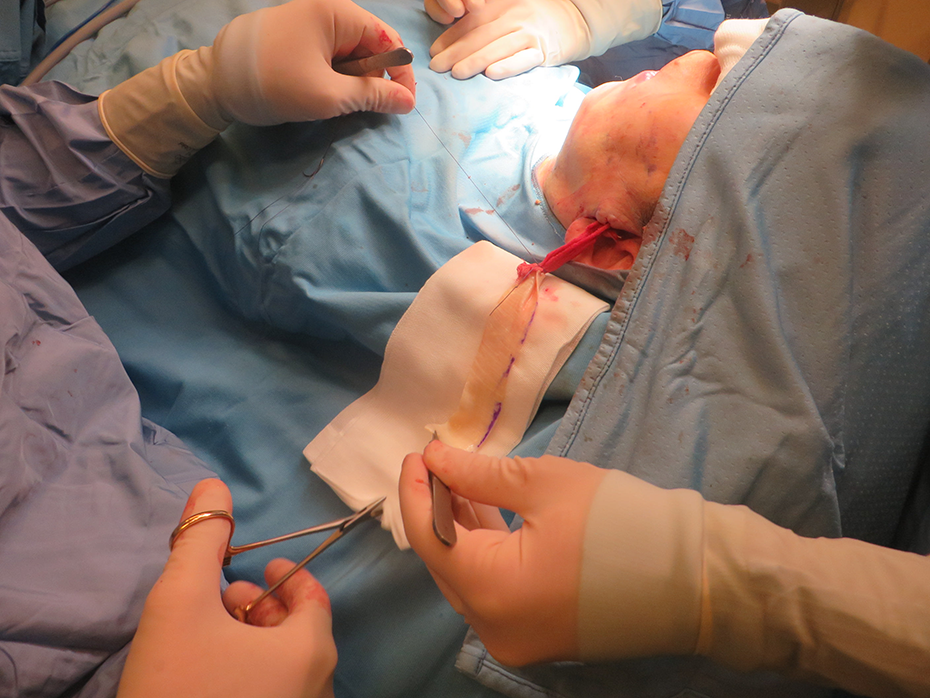
Intraoperative figure.
No respiratory complications were noted during or after general anesthesia. Four months postoperatively, the patient had good oral competence and there were no complications. She was very pleased with the obtained result (Figure 3). The disadvantages of this technique are related to the cost of the cadaveric fascia lata graft and some visibility and stiffness of the graft in patients with very thin subcutaneous tissues.
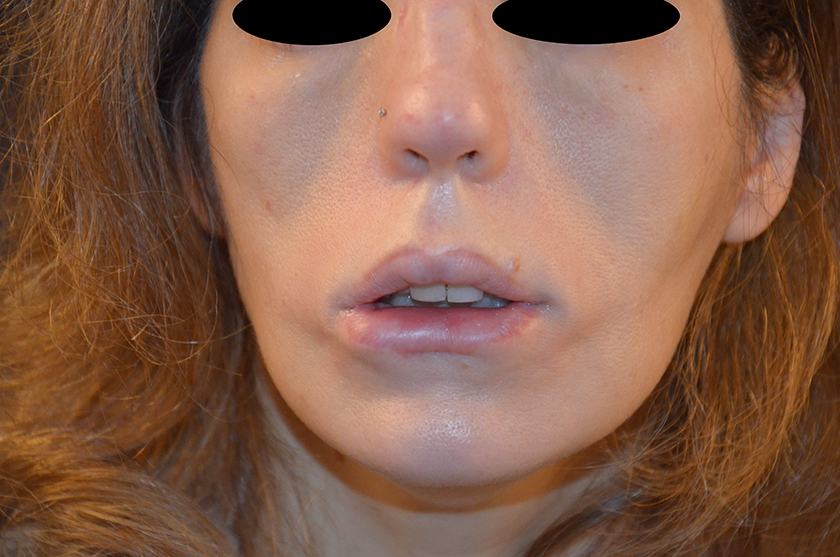
Postopertive figure.
Discussion
Static treatment modalities of patients with facial palsy are various and well described. Face lift, brow lift, facial musculature plication or shortening, fascial sling procedures, eyelid weight surgeries, and canthopexy are some of the static techniques used to improve the appearance and disfunction related to facial palsy. 2 Static procedures can also be employed in a multimodal approach including physical therapy, chemodenervation with botulinum toxin, and standard muscle transfers. 3
Suture suspension technique is currently employed for face and neck rejuvenation. 4 Its use in facial palsy correction is an easy and minimally invasive procedure and it can be performed under local anesthesia in an outpatient setting. 5 Navarrete Álvaro et al used Silhouette sutures to correct a left facial palsy in a 79-year-old patient. They achieved good aesthetic and functional results and the patient was satisfied. 6 As we described, we also obtained a remarkable result, but unfortunately due to recurrent sutures exposure we had to remove the sutures.
Static slings represent a common solution to restore oral competence and symmetry in the lower third of the face. The support can be provided by autologous tissue grafts, allografts, or synthetic materials (usually Gore-Tex). 7 High rates of complications are reported using Gore-Tex: In fact, stretching over time and wound infection can lead to a failure of the surgical correction. 8 Autologous tissue grafts reduce the risk of extrusion or infection. Fascia lata and palmaris longus tendon are 2 common options. Main disadvantages are increased surgical time and donor site morbidity. 7 Laina and Orlando reported a similar case to the one we described above: They treated a patient with bilateral facial palsy and oral incompetence with a palmaris longus tendon graft. The graft was sutured to the orbicularis oris muscle of the lower lip and to the deep temporal fascia bilaterally. The authors preferred to harvest a palmaris longus tendon graft instead of a fascia lata sling in order to reduce donor site morbidity. 9 We preferred to use a cadaveric fascia lata graft, thus eliminating any donor site morbidity and reducing operative time and the respiratory complications rate connected to general anesthesia. This solution, of course, has higher costs.
Conclusion
Bilateral cadaveric fascia lata graft represented a simple solution to restore the correct lower lip position in a challenging patient affected by Fazio-Londe syndrome with recurrent extrusion of previously inserted suspension sutures. We achieved a good result with a minimally invasive procedure. Main disadvantages are visibility of the fascia sling and costs associated with an allograft.
Footnotes
Ethical Statement
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Statement of Informed Consent
Written informed consent was obtained from the patient for publication of this case report and any accompanying images. Informed consent was obtained from all individual participants included in the study. Additional informed consent was obtained from all individual participants for whom identifying information is included in this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
