Abstract
An increased incidence of breast cancer has been observed in women, including in those with silicone breast implants. We describe here the use of a flap made of fibrous capsule to complete the coverage of breast implants in patients undergoing nipple-sparing mastectomy with immediate breast reconstruction, who previously had undergone breast augmentation with silicone implants. All patients underwent ipsilateral therapeutic mastectomy and contralateral prophylactic mastectomy for breast cancer risk reduction and breast symmetrization. The capsular flap was successfully used in 16 patients. No postoperative complications occurred. This is a simple and safe technique and an additional option for this procedure.
Introduction
Breast augmentation is one of the most commonly performed cosmetic surgeries in Brazil and in the United States. 1,2 The incidence of breast cancer in women is increasing throughout the world; it is the second most common cancer worldwide and the most common among women, accounting for 22% of new cancer cases. 3,4 Thus, an increased incidence of breast cancer has also been observed in women with silicone breast implants.
In cases of skin-sparing mastectomy with or without conservation of the nipple-areolar complex, breast reconstruction is commonly performed using silicone implants. 5 Breast implants are usually placed in the retropectoral plane with or without the detachment of the serratus anterior muscle. The use of acellular dermal matrices or synthetic meshes has been recommended for implant coverage. 5 –9 We describe here the use of a flap made of fibrous capsule to complete the coverage of breast implants in patients undergoing nipple-sparing mastectomy with immediate breast reconstruction, who previously had undergone breast augmentation with silicone implants placed in subglandular plane. The aim of this study was to describe a capsular flap for covering breast implants after nipple-sparing mastectomy.
Idea
Sixteen consecutive adult women with breast implants referred for nipple-sparing mastectomy with immediate breast reconstruction were selected to participate in the study. Written informed consent was obtained from all patients prior to their inclusion in the study and anonymity was assured.
All patients underwent bilateral nipple-sparing mastectomy (ie, in 12 patients ipsilateral therapeutic mastectomy [in situ carcinoma] and contralateral prophylactic mastectomy for breast cancer risk reduction and breast symmetrization, and in 4 patients bilateral prophylactic mastectomy) with immediate breast reconstruction using a capsular flap. All the patients had previous subglandular breast augmentation.
Surgical Technique
Nipple-sparing mastectomy was performed with conservation of the breast implant capsule. A flap was then constructed including the anterolateral portion of the fibrous capsule of a size sufficient to cover the new breast implant, which was, at this time, placed in the retropectoral plane. In 10 patients we used round implant and in 6 anatomic implants (all of them textured).
The flap was opened like a book page (the open-book technique) and attached to the lateral aspect of the inframammary fold and to the side of the new breast mound, completely covering the implant (Figures 1 and 2).
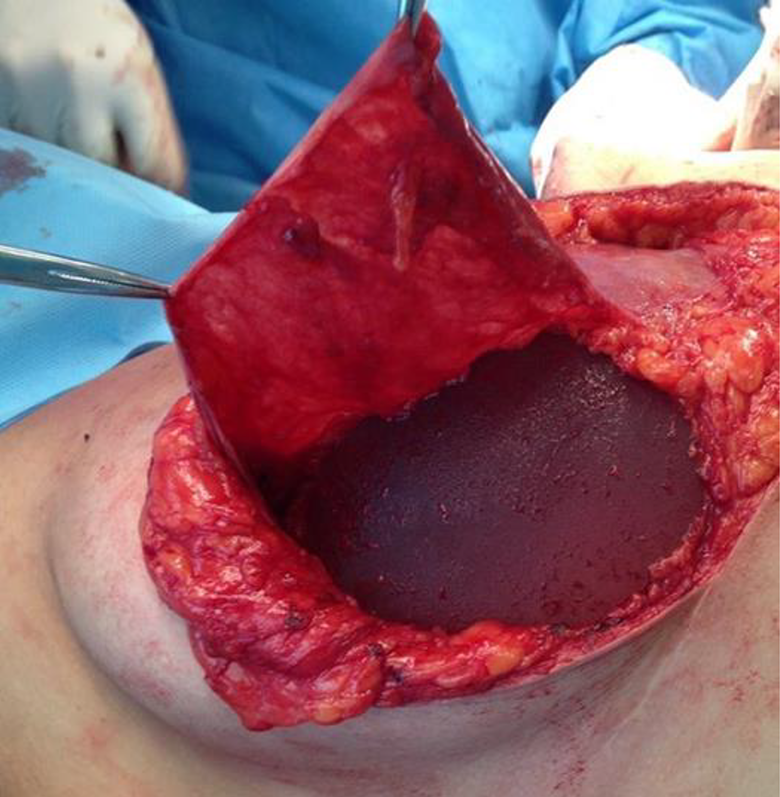
Capsular flap raised and breast implant placed.
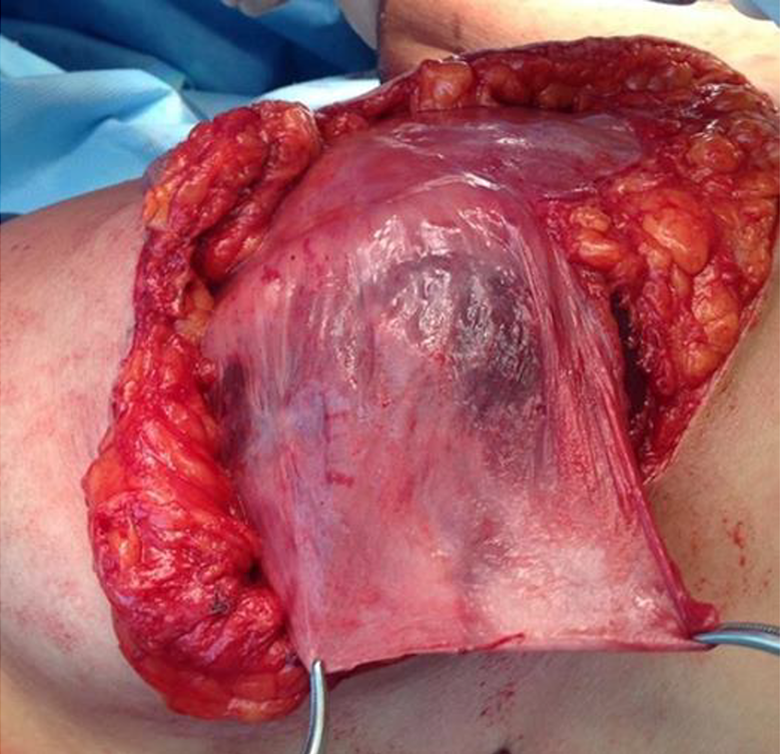
Capsular flap covering the silicone implant.
The capsular flap was successfully used in the 16 patients. In all cases, the capsule was thick enough to cover the implant. No postoperative complications occurred. In 2 patients, the capsule was removed from one of the breasts because it was close to the tumor; thus, part of the capsule from the contralateral breast was used as a graft.
Discussion
The technique showed to be rapid, easily performed, and to provide a safe coverage for the silicone implant in breast reconstruction. Because the fibrous capsule is an autologous tissue, there is no additional cost in contrast to the use of acellular dermal matrices or synthetic meshes.
The limitations of this technique include the possible presence of calcification in the fibrous capsule and need to remove the fibrous capsule as tumor margin. In cases where the capsule has to be removed as tumor margin, the implant can be covered using part of the fibrous capsule from the contralateral breast as a graft (Figure 3). The capsular graft may be secured in the same way as an acellular dermal matrix or a synthetic mesh (Figure 4).
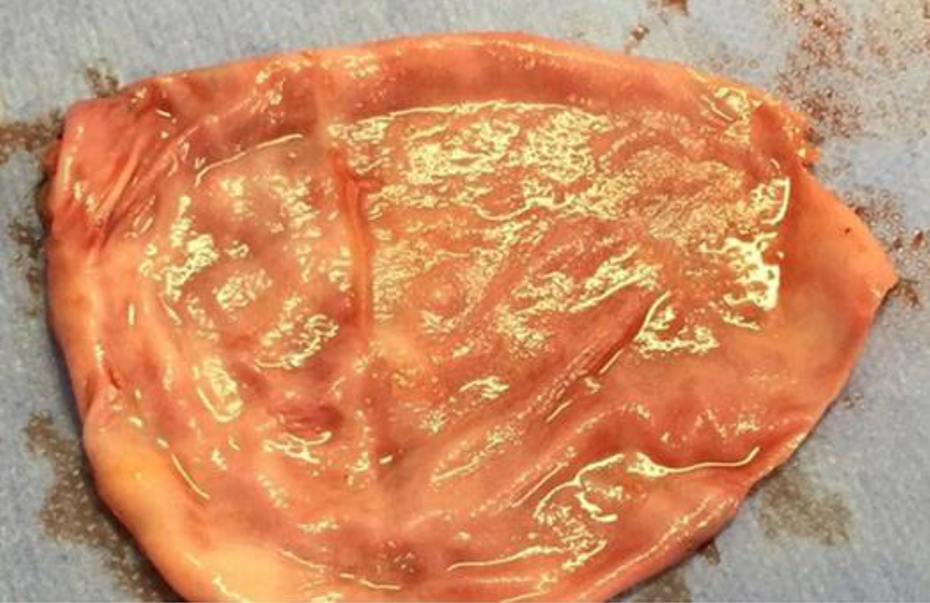
Capsular graft harvested from the contralateral breast.
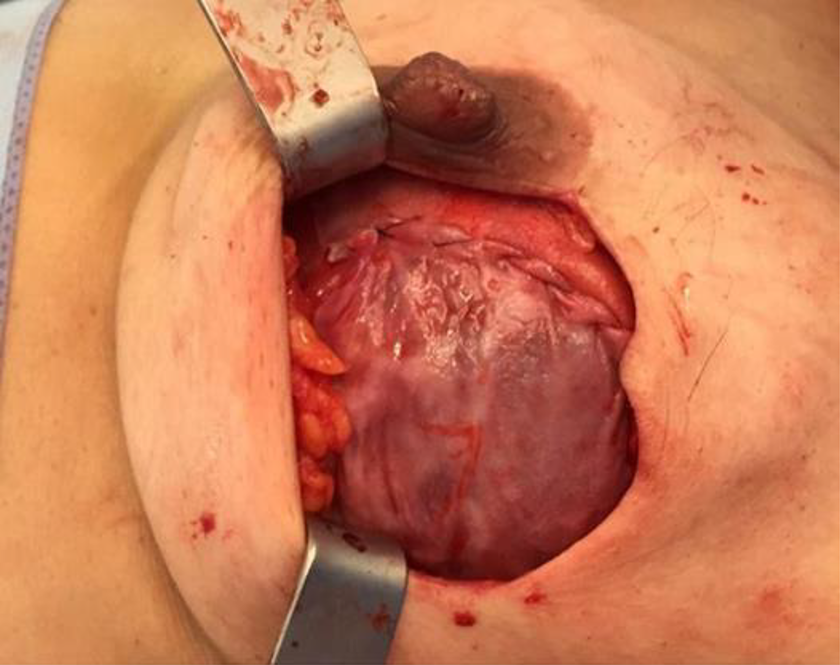
Capsular graft covering the silicone implant.
In conclusion, the use of a capsular flap for implant coverage in nipple-sparing mastectomy with immediate breast reconstruction is a simple and safe (in prophylatic and initial breast cancer) technique and an additional option for this procedure.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
The study was approved by the Research Ethics Committee of the Universidade Federal de São Paulo (UNIFESP), Brazil, and performed in accordance with the ethical standards of the World Medical Association Declaration of Helsinki.
