Abstract
Reconstruction of the nipple–areolar complex usually marks the final stage of breast reconstruction in postmastectomy patients. There are many approaches to the nipple reconstruction using autologous, allogenic, and synthetic materials. However, different methods have their own pros and cons and there is no current consensus for the best technique. A review of the literature showed that there is a low level of evidence for synthetic material–based nipple reconstruction providing the best nipple projection, but it is also associated with more complication. We present a case where revision of nipple reconstruction with MEDPOR implant overlying an implant-based breast reconstruction preceded the loss of both the nipple and breast construction secondary to infection.
Introduction
Breast reconstruction post-mastectomy has been shown to improve patients’ body image and psychological well-being. 1 Reconstruction of the nipple–areolar complex (NAC) usually demarks the final stage of breast reconstruction. Addition of the NAC correlates with significantly greater breast reconstruction satisfaction. 2 There are many approaches to NAC reconstruction using autologous tissue, allogenic tissue, and synthetic material. Currently, there is no consensus on the best method and no clear record of complication rate associated with each technique. 3 This article presents a patient whose breast reconstruction was compromised by her NAC reconstruction.
Case Presentation
A 52-year-old woman presented with lobular carcinoma in situ (LCIS) and atypical lobular hyperplasia in the upper left breast in June 2013 (Figure 1), which was treated with wide excisional biopsy. Follow-up surveillance found nuclear grade 3 invasive lobular carcinoma, in situ lobular carcinoma of classic and focal pleomorphic type, and in situ ductal carcinoma of the left breast in October 2013. The cancer was found to be positive for estrogen receptors and progesterone receptors but negative for human epidermal growth factor receptor 2. She was otherwise healthy except for being on long-term azithromycin and hydroxychloroquine for recurrent Lyme disease. She did not smoke or drink alcohol. In January 2014, she underwent a skin-sparing left mastectomy with sentinel lymph node biopsy and immediate reconstruction with a direct-to-implant approach using an anatomical gel implant placed under the pectoralis muscle and acellular dermal matrix (ADM). Final pathology showed invasive lobular carcinoma with no evidence of invasive disease or lymph node involvement. She started raloxifene in March 2014 as a prophylactic chemotherapy for her right breast because of her LCIS status and she did not require radiation.
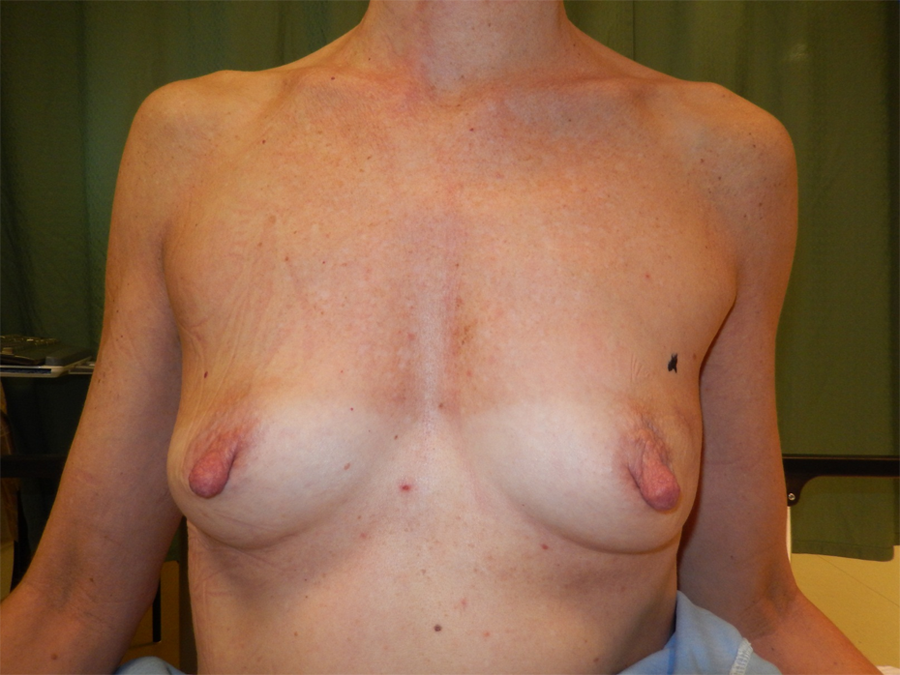
Preoperative photo before mastectomy.
In January 2015, a left breast mound revision with lipofilling and left nipple reconstruction with C-V flap and labial graft were performed (Figure 2). In July 2015, in order to improve the nipple projection to match her large contralateral nipple, a MEDPOR implant measuring 2.2 × 1.3 × 1.0 cm was carved to a size matching the opposite side and inserted into a pocket under the nipple. The implant healed without complication, but later shifted. A revision was then performed in March 2016 to correct the shifting and increase the nipple projection further. This was achieved by dissecting and freeing the MEDPOR from all its deep attachments and using a through-and-through 4-0 nylon suture to anchor the implant inferiorly and to spin onto its axis. The suture was planned to be left in place for 3 weeks. During follow-up for suture removal, swelling and redness were noted in the left breast; however, there was no drainage, no significant tenderness, and no other evidence of infection, fever, or chills. Cephalexin was prescribed for 1 week, and upon follow-up 1 week later, she was noted to be unwell and febrile with headache. Her breast examination revealed clean and dry incisions with no signs of infection. However, the left breast remained swollen and was now tender. A blind needle aspiration was performed in the area posterior to the implant and 300 mL of murky dark tinged fluid was aspirated. The fluid then reaccumulated and required ultrasound-guided aspiration 2 and 8 days after the initial aspiration, each time returning several hundred mLs of fluid. The fluid was cultured and grew coagulase-negative staphylococcus. She was eventually admitted with increasing pain and swelling of the left breast (Figure 3).
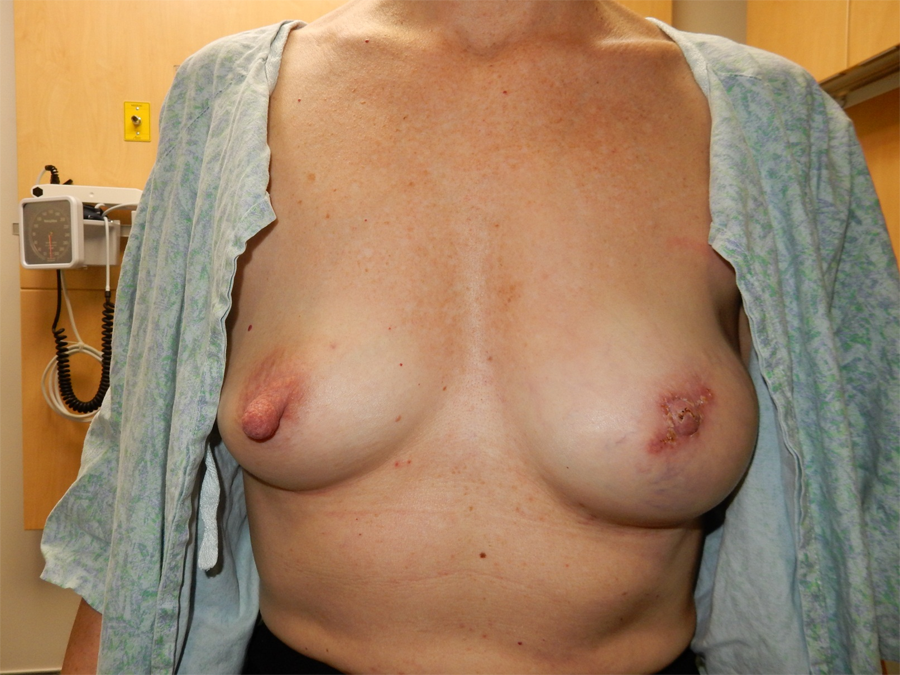
Postoperative photo after left breast mound revision with lipofilling and left nipple reconstruction with C-V flap and labial graft was performed. Note the lack of projection compared to the large contralateral nipple.
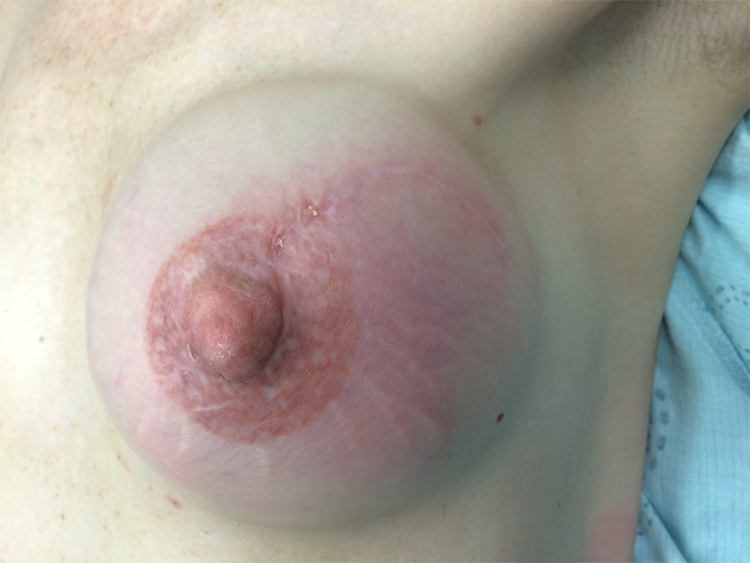
Periprosthetic infection of the left breast after MEDPOR implant revision.
In May 2016, she was booked for urgent exploration in the operating room to remove the infected breast and nipple implants. It was discovered there that the nipple implant eroded from the subcutaneous plane into the subpectoral plane in direct contact with the breast implant and damaged the implant surface with abrasions (Figure 4). However, the breast implant remained intact with no leakage. Pathology examination of the left breast capsule and implants supported clinical impression of periprosthetic infection and revealed no evidence of anaplastic large cell lymphoma within the capsule. The patient’s surgical site healed very well; however, she was left with significant pain in the area.
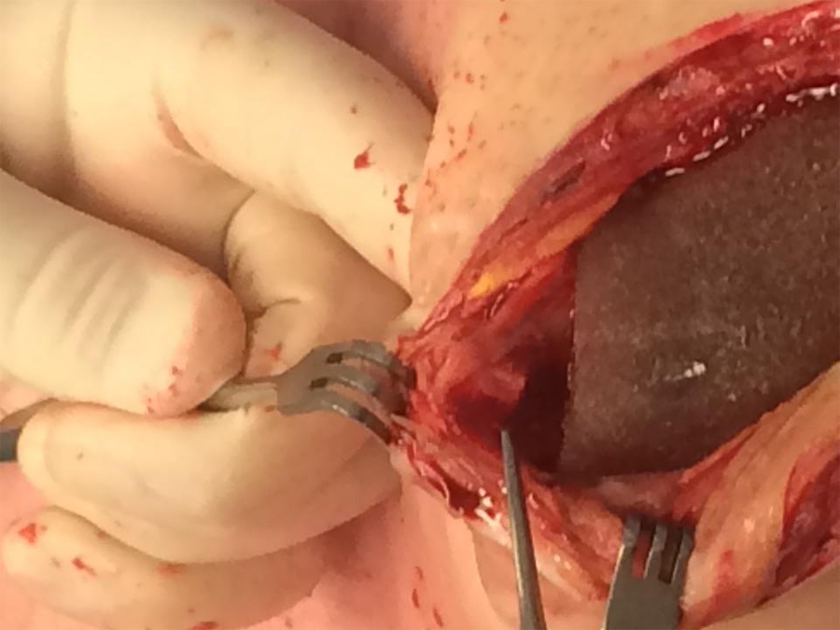
Intraoperative photo demonstrating the breast implant surface abrasions from being in direct contact with the eroded through nipple implant.
Discussion
In this patient, revision of the MEDPOR nipple implant preceded a complete loss of the implant-based reconstruction that had been stable for 2 years prior. The finding of erosion of nipple implant from the subdermal plane into the subpectoral plane in direct contact with the breast implant was unexpected. A search of the literature showed no similar report of MEDPOR used in nipple reconstruction resulting in loss of breast reconstruction. Interestingly, while the risk of infection is known to be increased with the use of a synthetic implants, 3 in this patient, incisions around the NAC remained clean and intact with no signs of infection. In addition, the location of fluid collection was at the posterior aspect of the patient’s breast implant. It should be noted that the patient’s status on long-term azithromycin and hydroxychloroquine may have created resistance and impacted the outcome.
Arguably, the greatest challenge in nipple reconstruction is the maintenance of nipple projection over time. 2 Various materials have been used in the past to increase and maintain the projection of the reconstructed nipple, but it remains unclear which one is the best method. They include the use of autologous tissue such as fat, cartilage, bone, toe pulp, nipple sharing, labia minora, and dermal grafts; the use of allogenic tissue with ADM, bone allograft, and extracellular matrix collagen; or the use of synthetic implants made of silicone, polyurethane, polytetrafluoroethylene, and calcium hydroxyapatite. A recent systematic review revealed great variation in the technique and material used in nipple reconstruction. 3 A low level of evidence was found for synthetic materials having the least loss of projection over time but also higher complication rate secondary to exposure due to their nonadherent property and contraction of overlying skin. 4,5 In comparison, allogeneic and autologous grafts had greater and comparable losses of nipple projection. Acellular dermal matrix has shown promising outcomes with good maintenance of projection, low complication rate, and no donor site morbidity; however, ADM is very expensive. This may be circumvented by banking excess ADM left over from breast reconstructions. 3 It should be noted that in the majority of studies, nipple reconstruction was performed over autologous breast reconstruction. Only 4 of the 31 studies had implant-based breast reconstructions, which may have introduced a level of bias in the review.
In our patient, it was originally felt that the use of composite nipple graft was the best method of nipple reconstruction as she had a rather large NAC on the contralateral breast. Reconstruction of the left nipple to match the patient’s natural right nipple’s projection was felt to be difficult. However, the patient declined the option of nipple sharing due to potential donor site morbidity such as numbness, pain, and scarring. 6 Due to patient preference and the degree of projection required, a MEDPOR implant inserted under the nipple was determined to be the most appropriate method of reconstruction.
MEDPOR is a high-density porous polyethylene (HDPP) soft tissue implant material primarily used for craniofacial, orbital, nasal, and auricular reconstruction. 7 Its advantages include that it can be easily shaped through carving, sutures can be passed through, 8 its pores allow for rapid tissue ingrowth which reduces the rate of infection and capsule formation while promoting its stabilization, 7 and there is no absorption. No literature was found on the use of HDPP for nipple reconstruction, in particular over breast implants. The overall complication rate of MEDPOR was found to be low, with the most common complications being pain, paresthesia, implant exposure, and infection. Implant placement in areas such as nose, maxilla, and ear and in grafts covered by thin and scarred tissues are more prone to extrusion and infection. 9 The overall rate of complication in craniofacial and orbital regions varied from 6.31% to 12.5%. 9 -12 The highest rate of complication occurred when used in lower eyelids for lid heightening and stabilization where the complication rate was 49%. 13 Another factor to consider for MEDPOR placement is the overlying tissue’s radiation status, where increased healing time was demonstrated in the radiated group in a canine study. 14 Due to the paucity of available data on the use of MEDPOR in nipple reconstruction, it is difficult to assess its complication rate when used in the area and how it impacts underlying implant-based breast reconstructions.
Conclusion
This was an unfortunate case where the revision of nipple reconstruction with MEDPOR implant to increase nipple project preceded the loss of both the nipple reconstruction and implant-based breast reconstruction for the patient. A search of the literature revealed a low level of evidence for synthetic material–based nipple reconstruction providing the best projection but also associated with more complications. Overall, MEDPOR has been more commonly used as an implant material for other parts of the body with relatively low complication rates. No similar case report has been reported, however, for nipple reconstruction leading to complication. While MEDPOR is an implant material with many advantages, this case illustrates the need to exercise caution when reconstructing a nipple overlying an implant-based reconstruction.
Footnotes
Statement of Human and Animal Rights
This article does not contain any experimental studies with human or animal subjects.
Statement of Informed Consent
Not applicable, no identifying information is included in this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
