Abstract
Synovial chondromatosis (SC) is a benign proliferative metaplasia of joint synovium into cartilaginous tissue. The relative scarcity of presentation in the wrist or hands contributes to the difficulties in accurately diagnosing and obtaining the necessary treatment for SC. We present a 43-year-old man with a 10-month history of stiffness and decreased range of motion of his right first metacarpophalangeal (MCP) joint. On examination, a firm mass was palpated surrounding his MCP joint. X-rays showed only a joint effusion. Subsequent magnetic resonance imaging (MRI) showed an effusion, high signal intensity joint distension, and small erosions. Surgical exploration and complete synovectomy with excision of loose bodies was performed. The pathological diagnosis, based on the clinical examination as well as MRI, was consistent with that of tenosynovial chondromatosis. This case illustrates surgical exploration and pathological investigations may be necessary for SC diagnosis. The literature was reviewed for greater understanding of SC’s presentation, diagnosis, and treatment.
Keywords
Introduction
Synovial chondromatosis (SC) is a benign proliferative metaplasia of joint synovium into cartilaginous tissue. 1-5 It arises within the synovium of tendon sheaths, bursa, or joints. 6,7 The typical clinical presentation is pain and decreased ROM with joint swelling or effusion. 8-12 The cartilaginous tissue present within the joint may also detach and form loose bodies that can undergo calcification and ossification. 1 The origin may be extra-articular or intra-articular. Intra-articular or synovial is most common in the knee, shoulder, or hip joints; extra-articular or tenosynovial most commonly affects the finger flexor tendons. 1,2,5,13-15 The relative scarcity of presentation in the wrist or hands contributes to the difficulties in accurately diagnosing and obtaining the necessary treatment for SC. 16
Synovial chondromatosis has a bimodal presentation, seen more commonly in males aged 30 to 50 years and becoming female dominant in later years. 1,8,10,12,13,17 This condition can be subdivided into primary and secondary, with secondary being due to another process affecting the joint such as degeneration or trauma. Milgram described a type of classification of SC in which early, intermediate, or late stages were described, depending on the presence of synovial disease and loose bodies. Early stage was described as only active disease within the synovium, intermediate also had the presence of loose bodies, and late stage had only loose bodies present with an inactive synovium. 18 However, as Milgram’s classification is based on pathology, arthroscopic examination is often necessary prior to staging of SC. 19
The treatment of SC is controversial. Surgical excision, involving removal of loose bodies and synovectomy, is the treatment modality of choice. 10,15 There is a high rate of recurrence, and a complete synovectomy mediates this risk. There may be a malignant transformation to synovial chondrosarcoma in 1% to 7% of cases. 10,14,20 This case illustrates the complexity of making an SC diagnosis and how the radiological may differ from the clinical assessment and ultimately requires pathological evidence to be diagnostic.
Literature Search
A literature search was conducted for publications discussing SC of the hand or wrist through PubMed using the following search strategy: ((((“Chondromatosis, Synovial/pathology”[Mesh] OR “Chondromatosis, Synovial/physiopathology”[Mesh]) OR “Chondromatosis, Synovial/surgery”[Mesh]) OR “Chondromatosis, Synovial/diagnosis”[Mesh]) OR “Chondromatosis, Synovial/complications”[Mesh]) AND (hasabstract[text] AND “humans”[MeSH Terms] AND English[lang]). Abstracts and articles in English were included. References of relevant papers were reviewed. A separate search was also conducted for general articles on the disease. The literature search yielded 391 publications, and after review, 79 papers were chosen which discussed SC of the wrist or hand (1962-2017).
Case Report
A 43-year-old healthy male engineer presented to his family doctor for stiffness and decreased ROM of his right first metacarpal (MCP) joint. He reported a sensation “like there was something inside” his MCP joint as well as pain with activity. He also noticed that his MCP joint appeared swollen. There was no history of trauma. His family physician ordered thumb radiographs which did not show a bony abnormality. At that time, the patient tried topical anti-inflammatory cream without relief.
Ten months later, he was still symptomatic and revisited his family doctor who ordered repeat radiographs (Figures 1 and 2). These were reported as normal with no bony abnormality identified. However, soft tissue swelling surrounding his MCP joint was noted.
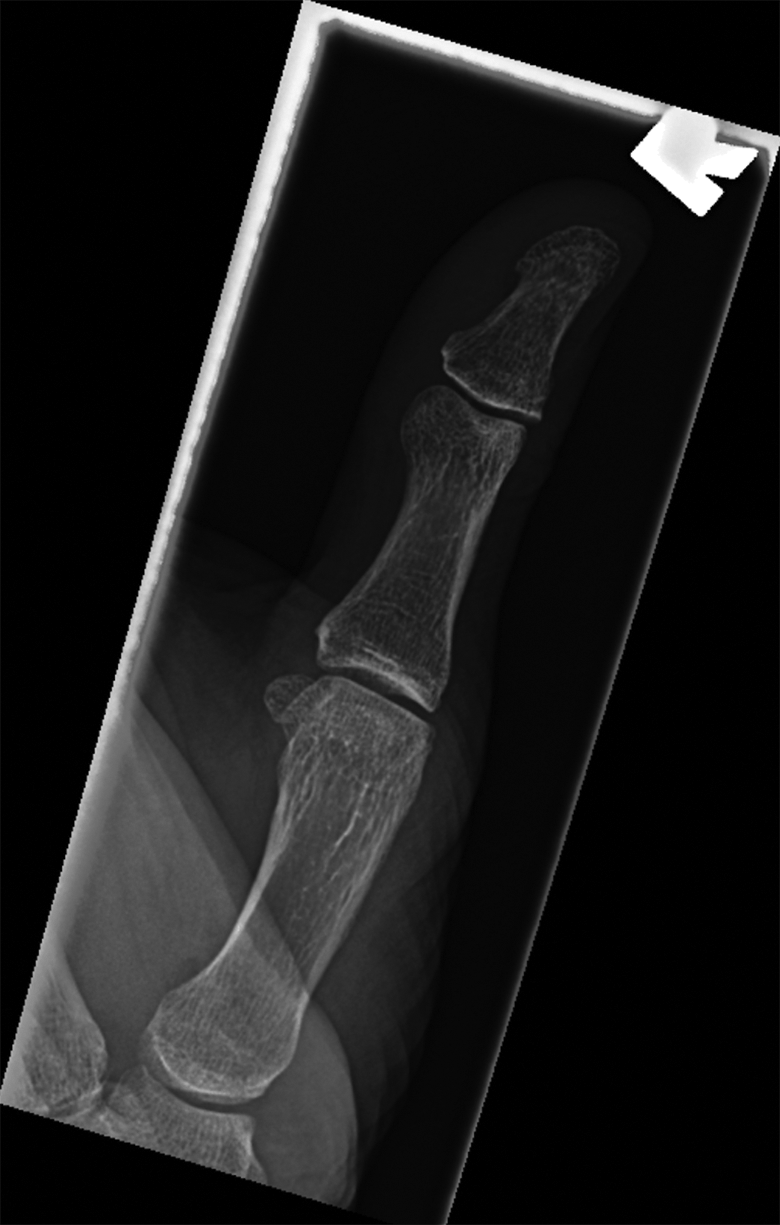
Preoperative X-ray of the right thumb (anteroposterior).
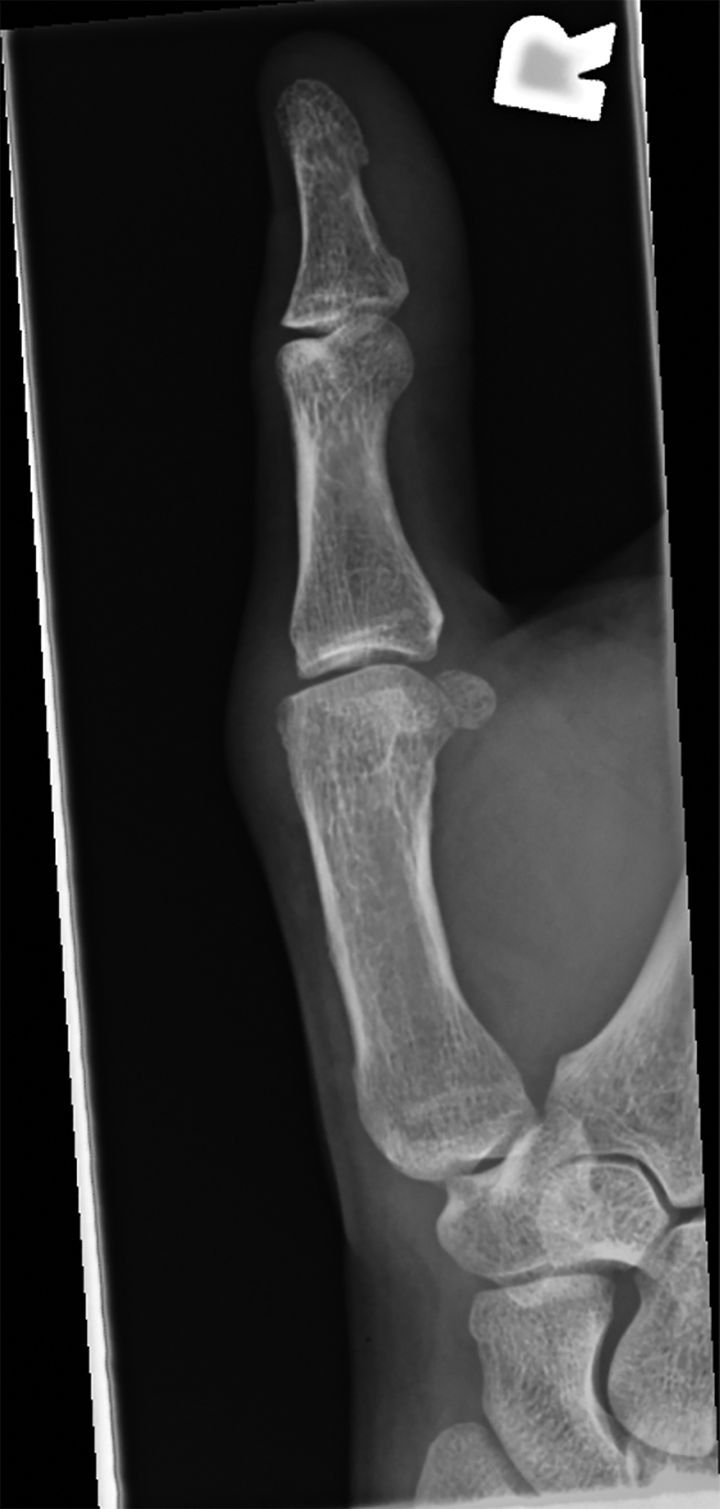
Preoperative X-ray of the right thumb (lateral).
Six months later, he was consulted to plastic surgery. His symptoms were continuing to worsen and he was now experiencing decreased strength in the joint, severely decreased ROM, and pain with movement. He was unable to open a jar due to pain. On physical examination, there was a palpable fullness to the MCP joint, with an asymmetrical hard palpable mass. The preliminary diagnosis was a giant cell tumor of the tendon sheath. There was decreased ROM in flexion, extension, adduction, and abduction of the MCP joint. Neurovascular status was normal. After assessment, a magnetic resonance imaging (MRI) was ordered to better characterize his ongoing MCP joint swelling. He received a multiplane multisequence MRI of the right first MCP joint without and with intravenous gadolinium (Figures 1 –10).
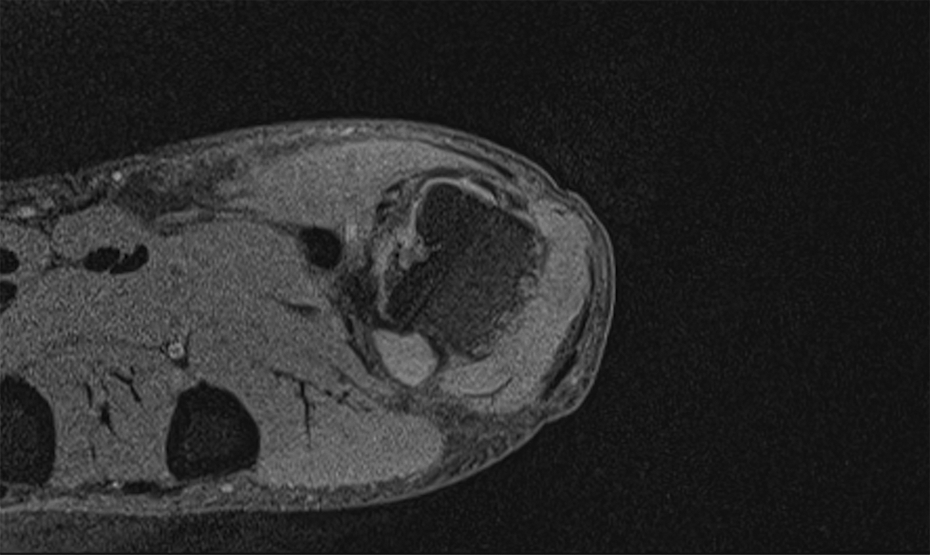
Axial T1-weighted fat-saturated pregadolinium.
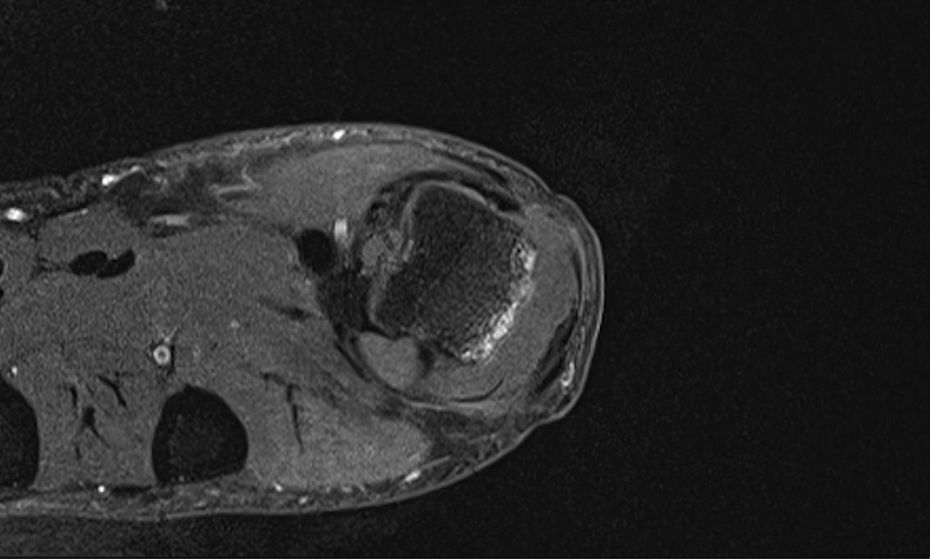
Axial T1-weighted fat-saturated postgadolinium.
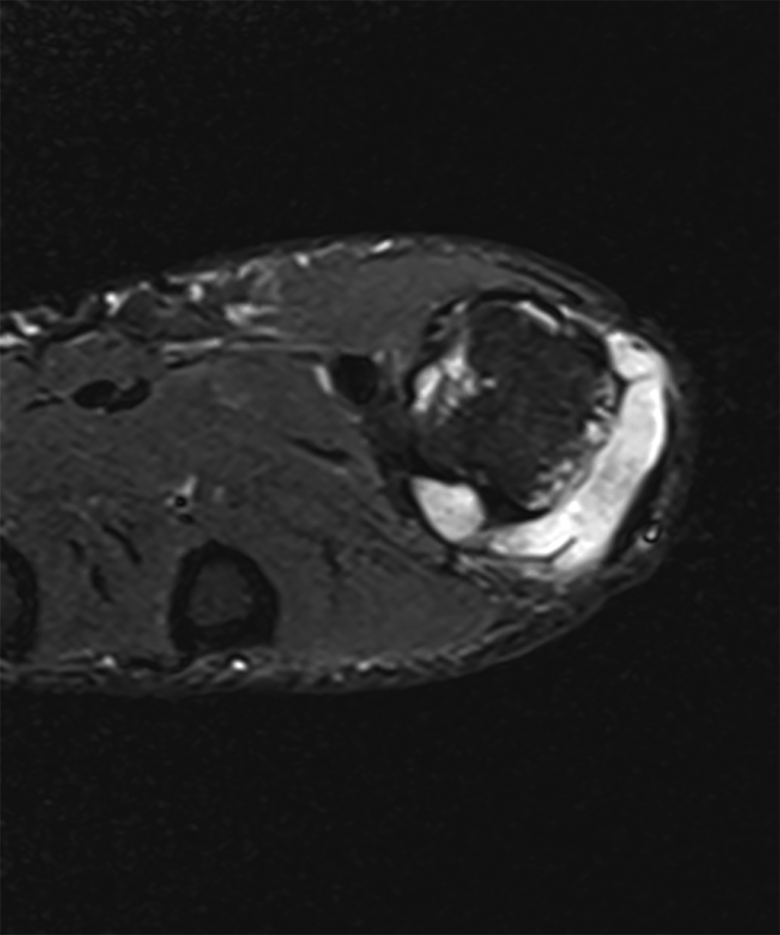
Axial short TI inversion recovery (STIR).
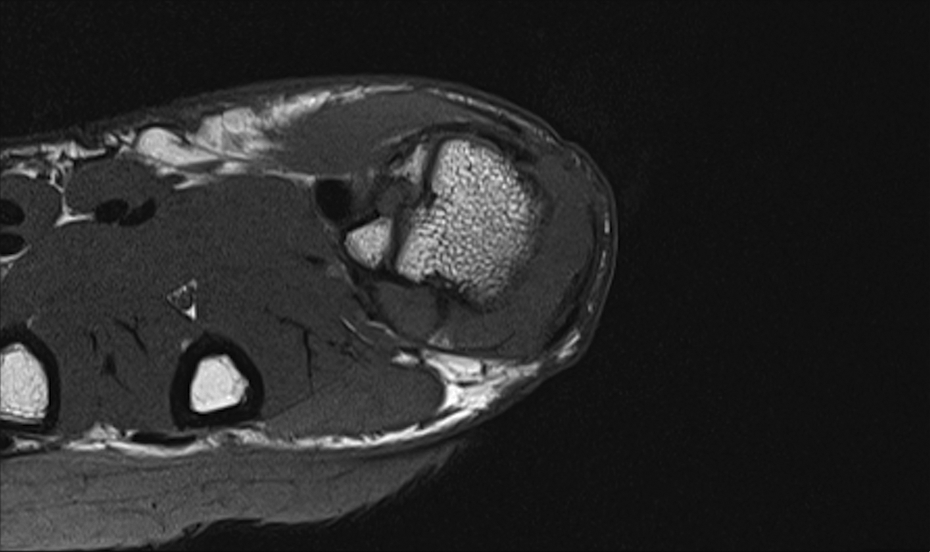
Axial T1-weighted.
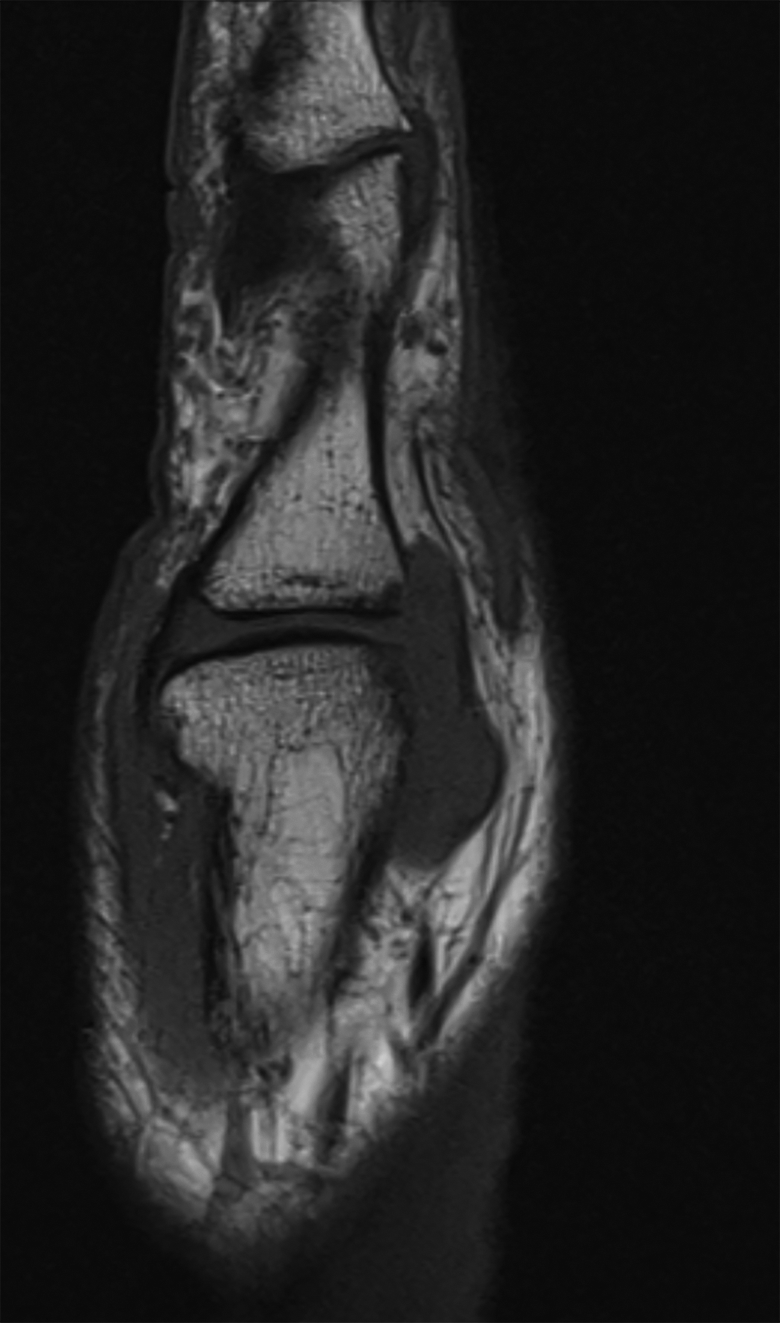
Sagittal T1-weighted.
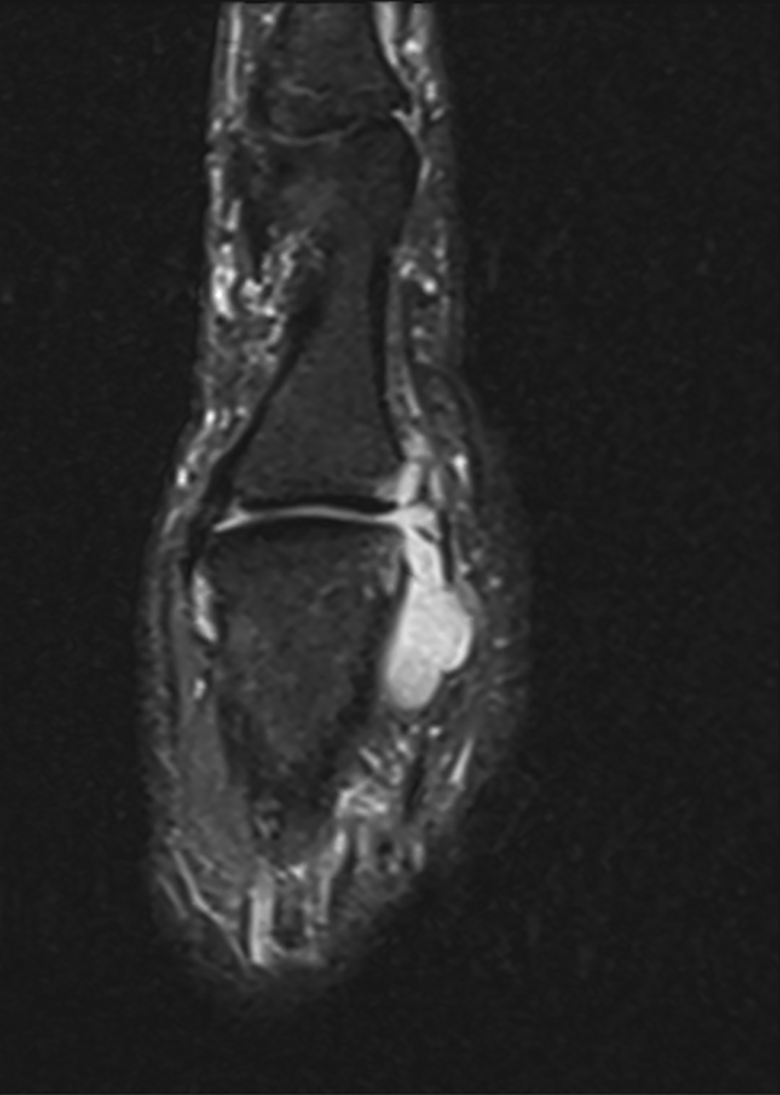
Coronal short TI inversion recovery (STIR).
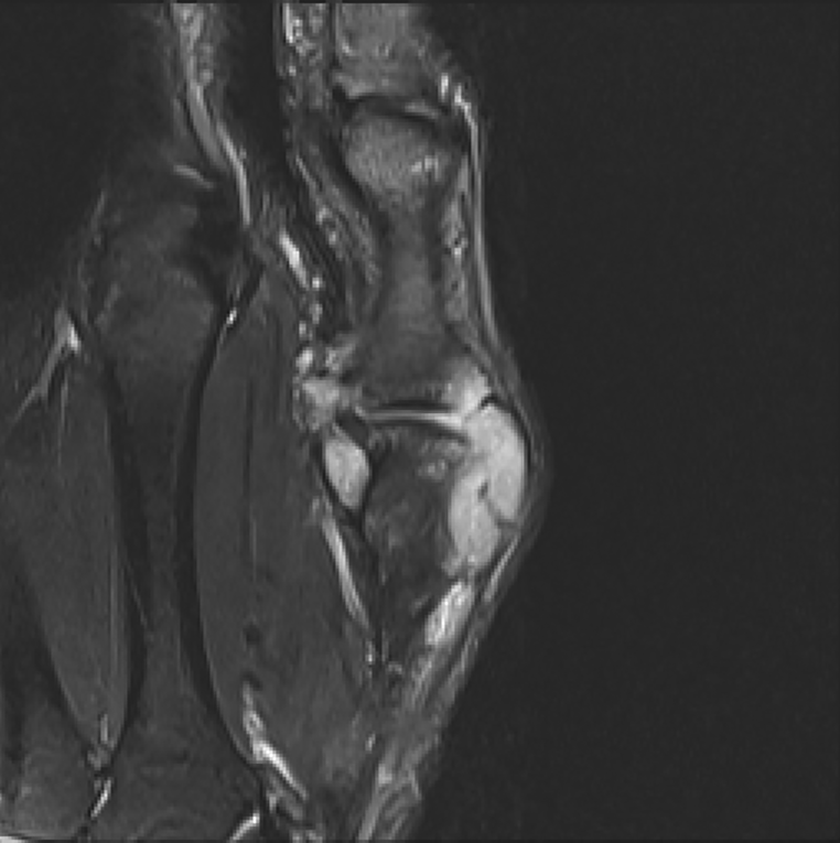
Sagittal T2-weighted fat saturated.
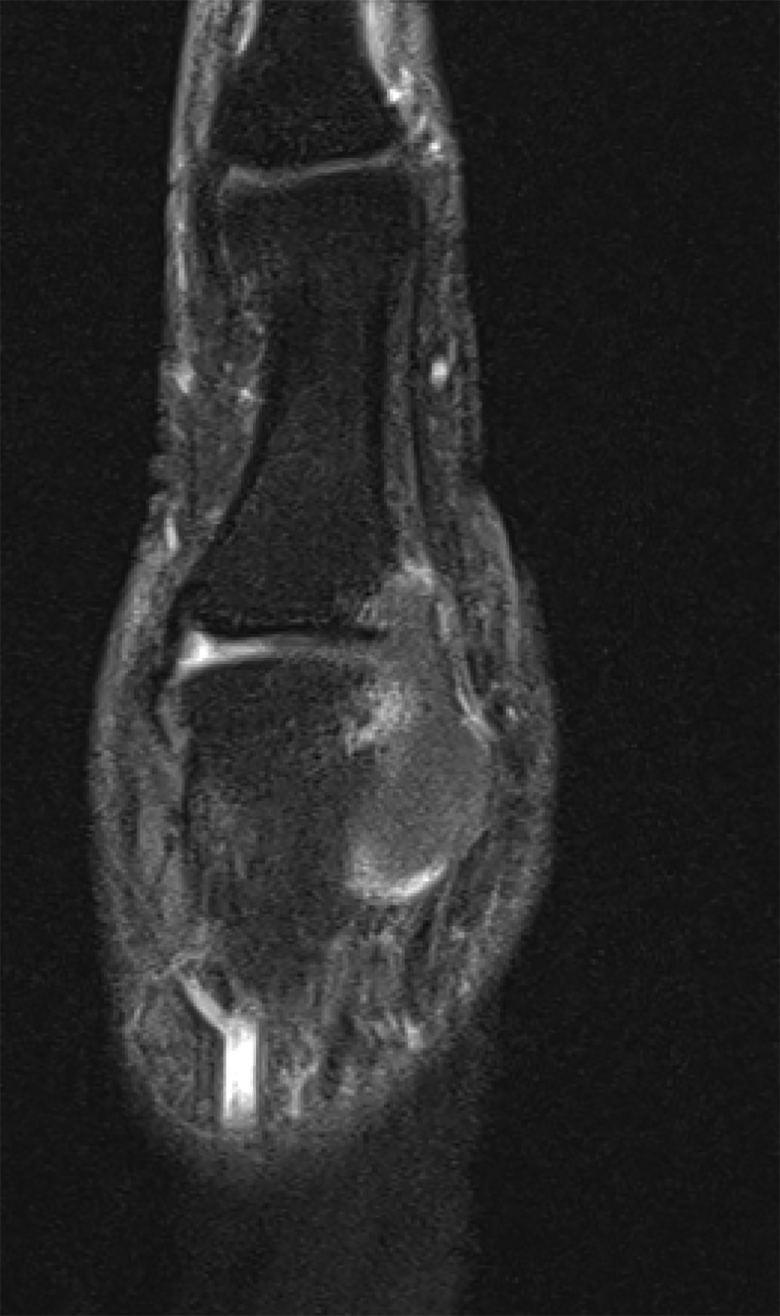
Coronal T1-weighted fat-saturated postgadolinium.
The MRI report described an effusion present in the MCP joint, associated with a lobulated high signal intensity joint distension. It also depicted small erosions at the dorsal aspect of the MCP joint involving the MCP head and phalangeal base. There was no reported abnormality of the ligaments or tendons. Based on MRI imaging, the overall impression was that the patient’s symptoms were due to synovial proliferation or joint distension with fluid/atypical ganglion cyst. It was not believed to be inflammatory in origin due to lack of enhancement with gadolinium.
The preoperative diagnosis was predicted to be a synovial-based process or a complex ganglion cyst. Given the discrepancy of the clinical findings of a hard palpable mass and the MRI suggestion of fluid distension of the joint, the proposed etiology was that of an unusual synovial process, atypical ganglion, or neoplasm. The clinical suggestion of a giant cell tumor of the tendon sheath was considered highly unlikely due to the high T2 signal on MRI. It was decided to proceed to surgical exploration.
An arthrotomy was performed and the joint was explored and found to be affected by the lesion. The lesion was excised and a synovectomy was completed (Figures 11 and 12).
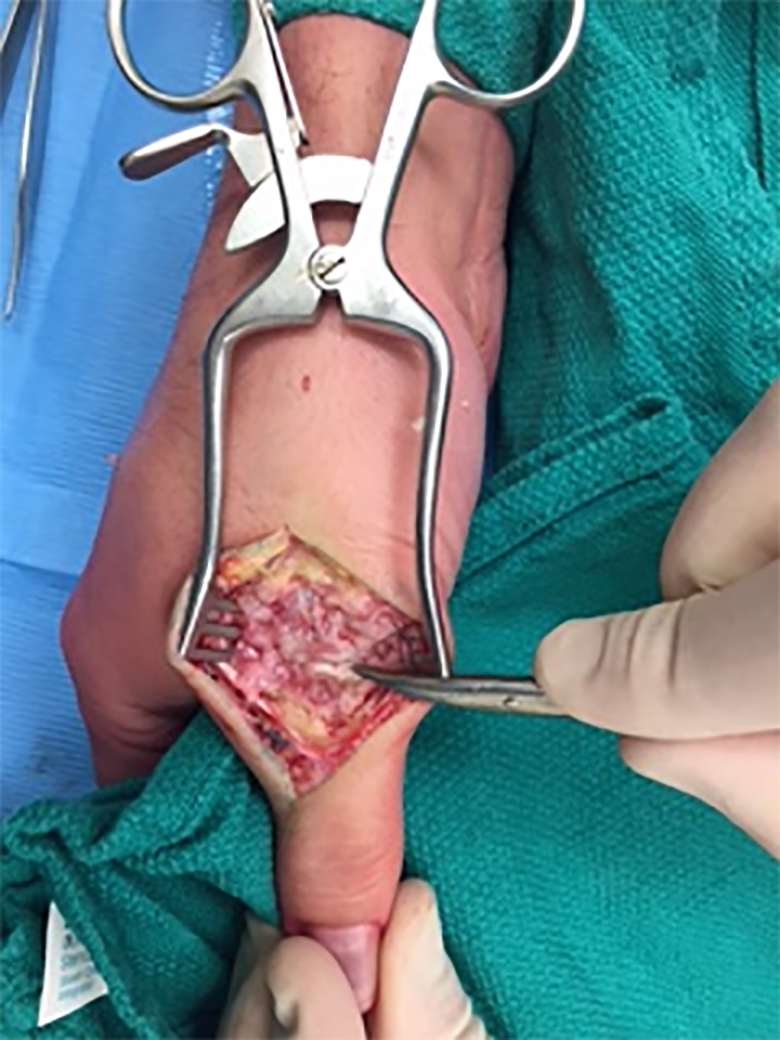
Intraoperative assessment of the right metacarpal (MCP) joint.
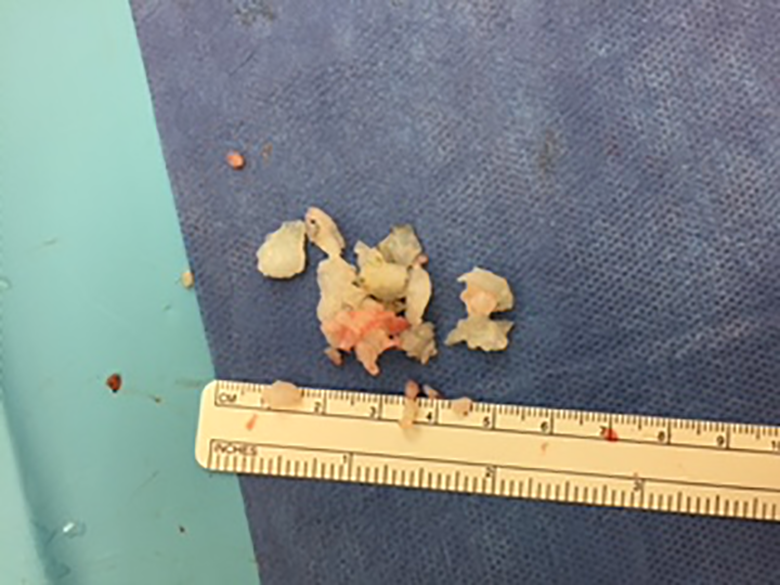
Loose bodies extracted from synovium right thumb.
Gross histological examination described the excised bodies as gray white firm tissue measuring 4.0 × 1.5 × 1.5 in size in aggregation (Figure 8). Microscopically examined, the tissue was described as multilobulated hyaline cartilage with clusters of mildly atypical chondrocytes. There was also binucleation described as well as open chromatin (Figures 9 and 10). Initially, the possibility of an enchondroma was evaluated and the pathology was reviewed with the Pathology Department at Brigham and Women’s Hospital in Boston, Massachusetts. Their diagnosis, based on the clinical presentation as well as MRI and pathological report, would be consistent with that of tenosynovial chondromatosis. It was described as multiple nodules of well-differentiated cartilaginous tissue showing mild hypercellularity as well as mild cytologic atypia. The sample did not have any evidence of bony involvement (Figures 13).
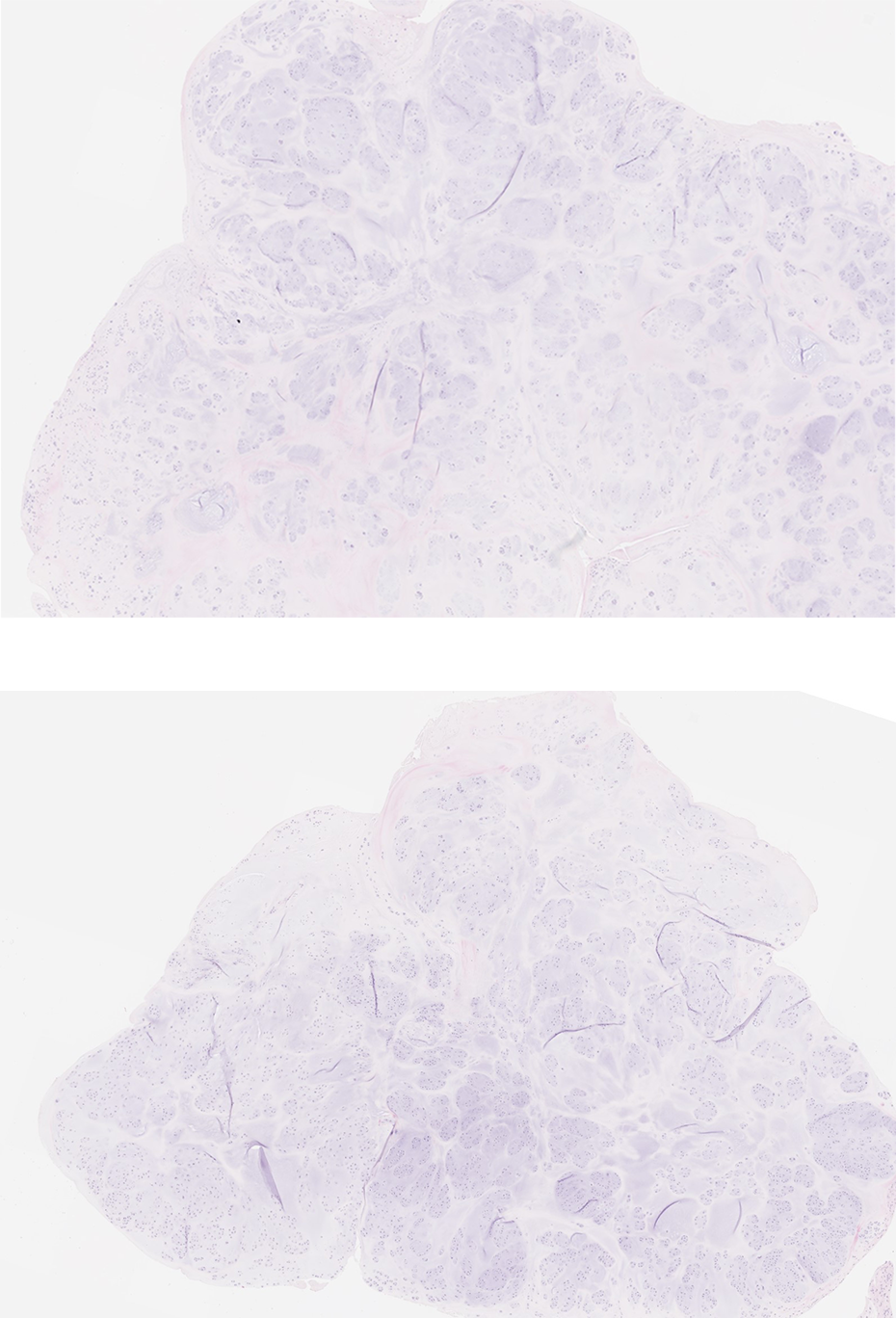
Pathological examination demonstrating multiple nodules of well-differentiated cartilaginous tissue.
Discussion
Synovial chondromatosis is rarely seen in the joints of the wrist and hands. Our literature review retrieved approximately 65 case reports. The etiology of this condition in its primary form is largely unknown. 12,21 When it is seen in the hand, it appears to be most commonly involving the flexor surfaces of the digits and usually on the dominant hand. 16
Synovial chondromatosis is often misdiagnosed as osteoarthritis, neuropathic arthritis, tenosynovitis, soft tissue chondroma, gout, osteochondritis dissecans, synovial hemangioma, rheumatoid arthritis, chondrosarcoma, ganglion cyst, or giant cell tumor of the tendon sheath. 1,7,12,13,22
Investigations
Imaging investigations in isolation may not definitively diagnose SC. In our case, X-ray imaging revealed no bony abnormality, and as time passed, soft tissue swelling became apparent. X-ray imaging may reveal a mass of soft tissue and calcifications. 1,16,23 If the disease has progressed, secondary degenerative features may be present such as subchondral sclerosis, joint space narrowing, and osteophytic changes. 24 The Milgram staging is associated with the progression of nodules as well as the clarity present on X-ray. Nodules tend to become more visible on imaging as the disease progresses. 12 It may be difficult to differentiate a chondrosarcoma from SC on imaging; however, if a lesion is attached to bone, it may favor a possible chondrosarcoma. 24
Other imaging modalities for SC are MRI imaging and, to a lesser extent, computed tomography or ultrasound. 1,11,13,25 In our case, MRI detected the presence of a cystic mass, but not the presence of any loose bodies or osteophytes. Hettiaratchy and Nanchahal 11 stated that MRI is likely the most accurate imaging modality for the diagnosis of SC, but the burden of disease is primarily determined operatively. Findings on MRI may differ depending on the amount of calcification that has occurred in the loose bodies. 12 If there is significant calcification, there may be low signal on both T1- and T2-weighted images. 24 If the disease is earlier in its progression, there may only be low signal in T1-weighted images and high on T2-weighted images. As in our case, the loose bodies may be partially or completely obscured by an effusion of the joint. 1 Also, as cartilage has a high water content, it may often be confused with a cyst as in our case report. 23 With regard to ultrasound imaging, nodules can be identifiable as hyperechoic areas. 24 Ultrasound was not used in our case. Computed tomography is reported in the literature as useful if calcifications are present. However, MRI remains the imaging modality of choice for these lesions.
Pathology
The pathogenesis of SC is largely unknown, but the formation of cartilage is often attributed to the metaplastic transformation of synovial tissue to cartilaginous tissue. Some literature supports a neoplastic process due to its rare progression to chondrosarcoma and appearance on cytology. 12,23,26,27
On gross pathological examination, loose cartilaginous bodies are observed. They are described as firm in consistency, oval to round, and are white or cream colored as seen in Figure 8. These nodules are generally concentrated near the synovium. Microscopically, the tissue resembles cartilage, may be well circumscribed, and have hypercellular and binucleate features as seen in our specimen. 8,12,13,23,28
Treatment
In the literature, the treatment performed was surgical in nature. 1,2,17,29 The exact procedures differed slightly, but the majority involved excision, removal of loose bodies, and synovectomy as seen in Table 1. 3,10,40 As reported by Spiers et al, 49 surgical procedures differed from a simple synovectomy to arthrodesis of patients with greater burden of disease. Recurrence was reported as 35% in the literature, as there were 23 of 65 cases in the hand and wrist which presented with recurrence (Table 1). The time line for recurrence in the literature was variable. It is often associated with incomplete resection operatively. 21 Documented management included close monitoring due to the risk of recurrence as well as the potential for malignant transformation.
Documented Cases of Synovial Chondromatosis Affecting the Joints of the Hand or Wrist.a
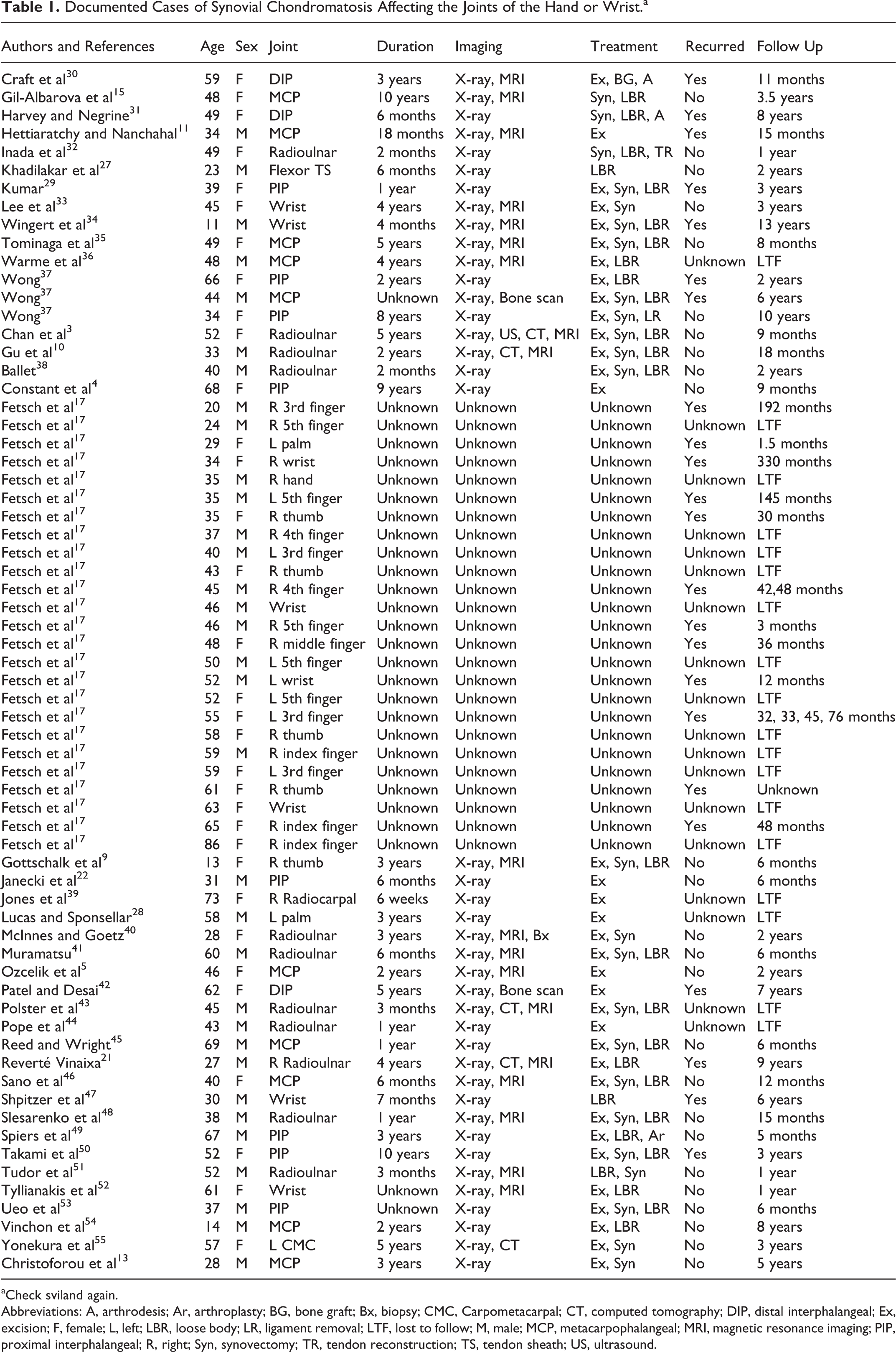
aCheck sviland again.
Abbreviations: A, arthrodesis; Ar, arthroplasty; BG, bone graft; Bx, biopsy; CMC, Carpometacarpal; CT, computed tomography; DIP, distal interphalangeal; Ex, excision; F, female; L, left; LBR, loose body; LR, ligament removal; LTF, lost to follow; M, male; MCP, metacarpophalangeal; MRI, magnetic resonance imaging; PIP, proximal interphalangeal; R, right; Syn, synovectomy; TR, tendon reconstruction; TS, tendon sheath; US, ultrasound.
Complications
In certain reports, osteoarthritis may present postoperatively, as well as mechanical issues such as joint locking or reduced ROM. 1 In our case, the only complication was subclinical reduction in ROM of the MCP joint opposition at 7 months postoperatively.
Another potential complication may be nerve compression by the mass or iatrogenic nerve damage. 16,41 Recurrence is a common complication, with rates ranging from 3% to 60% in the literature, and our review of cases in the hand and wrist had a recurrence prevalence of 35%. 12
Chondrosarcoma is a remote complication of SC and was reported in 2.5% of cases in a recent 155 case reviews. 20 It was reported in the hip joint and was present in 11% of cases. The likelihood of a transformation to a chondrosarcoma in the hand is unknown, and our research found that it had been reported once in the literature presenting in the wrist joint. 6
Conclusion
Synovial chondromatosis is a rare condition when presenting in the joints of the hand or wrist. Our case reported its occurrence in the metacarpophalangeal joint of the thumb. This case illustrated the importance of clinical correlation with radiographic findings. Magnetic resonance imaging imaging suggested a cystic etiology which clinically was solid to palpation. Ultimately, the diagnosis was elucidated as SC with surgical excision and histopathological examination. Excision, removal of loose bodies, or synovectomy is the treatment modality of choice. Further research and evidence is required to determine more accurate modalities of diagnosis and prevention of recurrence.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflict of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Statement of Human and Animal Rights
This case report does not contain any studies with human participants or animals performed by any of the authors.
Statement of Informed Consent
Informed consent was obtained from the individual included in this case report.
