Abstract
Brodie abscess is an uncommon form of osteomyelitis. Diagnosis can be difficult due to the insidious onset of symptoms and radiographic features that closely resemble more common pathology. The present report describes a patient with a Brodie abscess of the metacarpal head. The presentation, workup, management, and patient outcome are described.
Keywords
Introduction
Brodie abscess or “cystic osteomyelitis” is a form of subacute osteomyelitis characterized by an intramedullary abscess. 1 -3 First described in 1832 by Sir Benjamin Collins Brodie, a Brodie abscess is an uncommon infection that is typically found in children. 4-6 In adults, Brodie abscess occurs predominantly in young males with a history of trauma. 5 The abscess is classically located in the metaphysis of long bones in the lower extremity. 3 The bone is seeded with bacteria hematogenously or spontaneously. 1-3,6
Diagnosis can be clinically and radiographically challenging. Symptoms may not arise for weeks to years after abscess formation and are nonspecific—pain, swelling, and erythema are commonly reported. 1,3,4 Systemic symptoms such as fever, chills, and malaise can be absent. 3 Radiographically, Brodie abscess mimics common bone pathology such as chondroblastoma, Ewing sarcoma, and nonossifying fibroma. 3 Staphylococcus aureus is the causative organism in most but not all cases. 1,3
The present report describes the first reported case of a Brodie abscess in a metacarpal caused by Aggregatibacter actinomycetemcomitans. The patient presented several years after a “fight bite” injury (note 1) that is believed to be the inciting event.
Case Report
A 52-year-old right-hand-dominant male presented to the emergency department with pain and swelling over the right fourth metacarpal phalangeal (MCP) joint and hypothenar eminence. Symptoms began 3 days prior after he had a blunt injury to his right hand while using a jackhammer at work. His medical history was significant for several right hand injuries associated with physical altercations. He could not recall the specific details, but thought he fractured his right fifth metacarpal at least once. He also remembers having surgery for a laceration over his fourth MCP joint. The patient described undergoing irrigation, debridement, and antibiotic therapy for a “fight bite” injury. He denied requiring immobilizing for an associated fracture. This injury was more than 8 years prior and managed at a distant facility; thus, the medical records were not available.
On physical examination, the patient was systemically well. He had significant edema but no erythema or lymphangitis. The swelling was localized to the dorsal hand over the third, fourth, and fifth MCP joints. The was a well-healed scar over the dorsal surface of the fourth MCP joint in keeping with the history of a previous irrigation and debridement. The patient was tender to palpation of the dorsal surface of the third, fourth, and fifth MCP joints as well as the hypothenar eminence. No fluctuance was noted. At rest, his digits were held in flexion at the MCP joints. Active range of motion (ROM) was reduced in the third, fourth, and fifth MCP and interphalangeal joints due to pain. Passive flexion and extension of his fourth MCP joint elicited pain. Passive movement of the other digits was not painful.
Investigations in the emergency department revealed an elevated white blood cells (12.6 × 109 cells/L), platelets (433 × 109 cells/L), and C-reactive protein ; 15.9 mg/L). An X-ray revealed remote healed fractures of the right fourth and fifth metacarpal. A radiolucent lesion involving the distal metaphysis and head of the right fourth metacarpal was identified (Figure 1). The patient was initially diagnosed with hand trauma and resulting a pathologic fracture secondary to a presumed enchondroma.
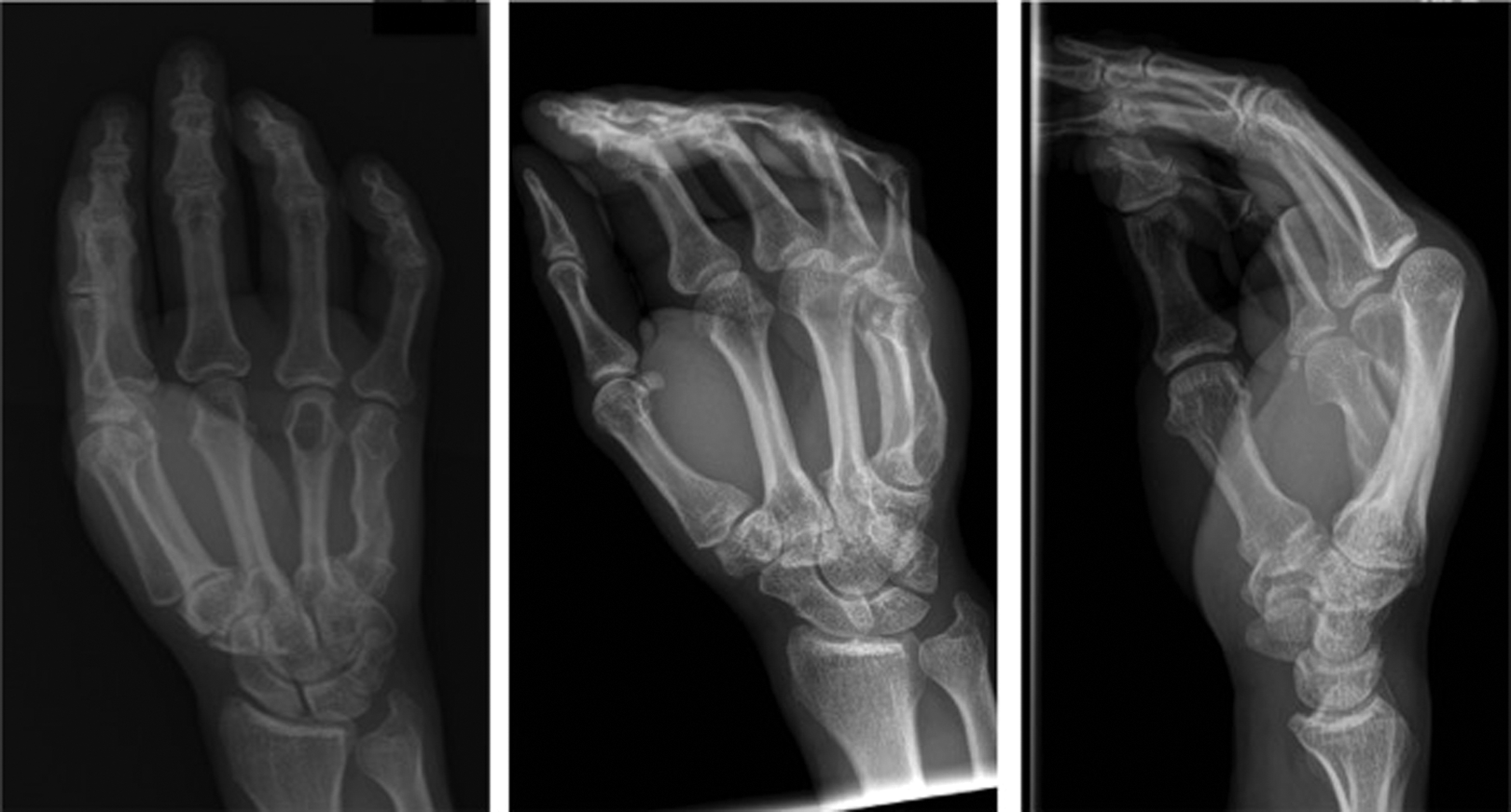
Right-hand X-ray (posterior–anterior [PA], oblique, lateral) demonstrating radiolucent lesion of the fourth metacarpal and remote healed fractures of the fourth and fifth metacarpals.
The patient presented for follow-up 2 days later with increased swelling, pain, and new erythema on the dorsal surface of the right hand. An infective process was suspected. Computed tomography (CT) was ordered to better characterize the lesion in the fourth metacarpal. Computed tomography demonstrated an ill-defined lytic lesion replacing most of the fourth metacarpal head with associated periostitis (Figure 2). Cortical destruction was present on the volar and dorsal surfaces of the metacarpal. These findings were consistent with fourth metacarpal head Brodie abscess (osteomyelitis) and surrounding soft tissue infection.
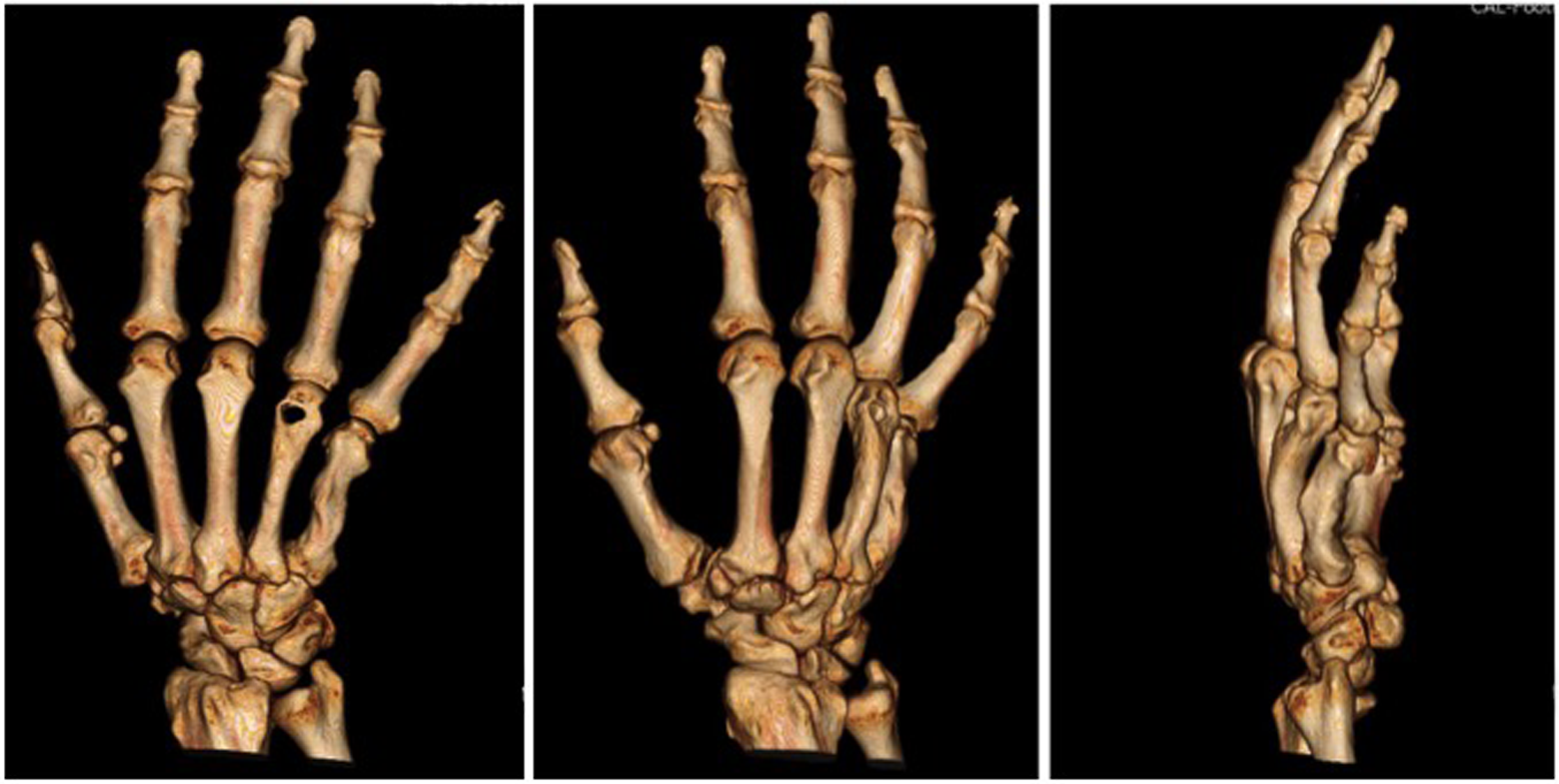
Right-hand computed tomography (CT) scan with 3-dimensional reconstruction (anterior–posterior, oblique, lateral).
The patient underwent surgical irrigation and debridement (Figure 3). Purulent fluid was found in the intramedullary canal and dorsal and palmar spaces. Following 2 debridements, the fourth metacarpal head and distal shaft were deemed unsalvageable and removed. A temporary spacer was created by moulding gentamicin-impregnated methyl methacrylate (Figure 4). Wound and bone cultures were positive for A actinomycetemcomitans, an organism normally found in the oral cavity. 7 Post-operatively, the patient was treated with 6 weeks of intravenous antibiotics.
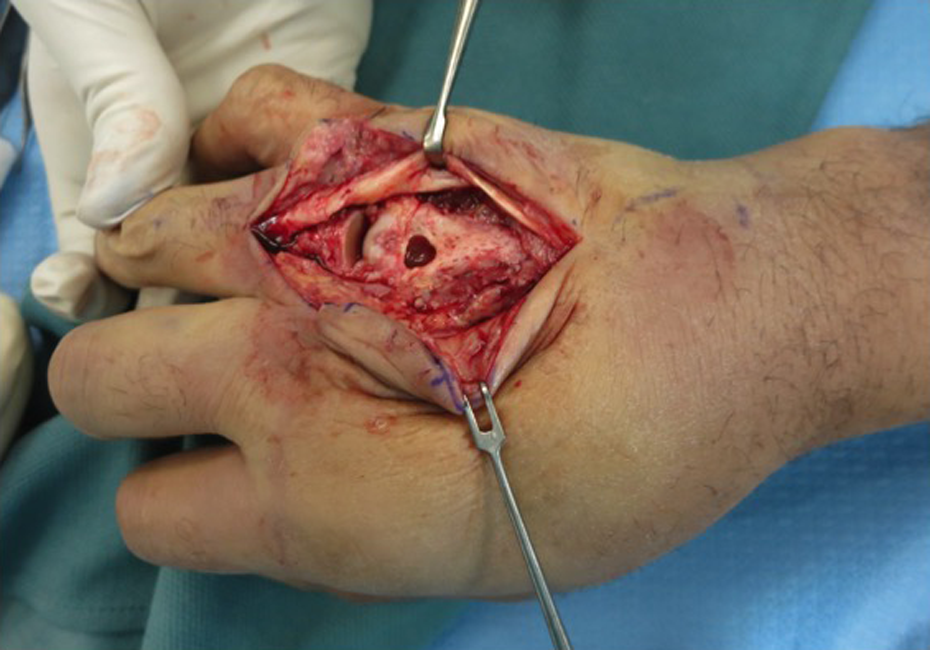
Intraoperative photo at initial irrigation and debridement. A hole in the dorsal cortex of the fourth metacarpal opens into a medullary canal containing purulent fluid. Loss of joint capsule with surrounding soft tissue infection.
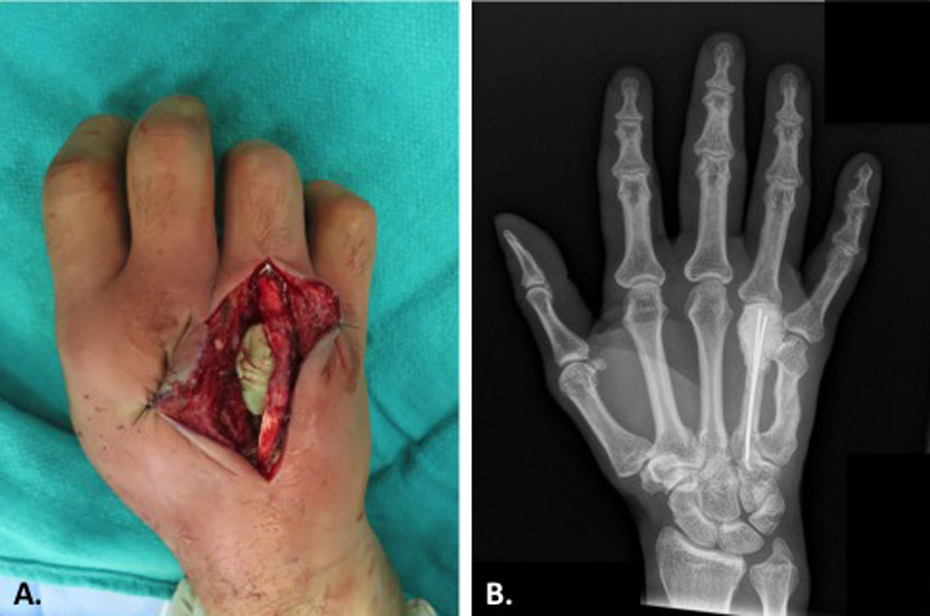
Placement of a gentamicin-impregnated methyl methacrylate spacer following debridement of distal metacarpal. A, Intraoperative photo. B, Right-hand posterior–anterior (PA) X-ray.
Reconstruction of the fourth metacarpal and MCP joint was performed 6 weeks after completion of antibiotics using an iliac crest bone graft. A sleeve of periosteum was harvested with the bone graft and wrapped around the distal end in hopes of creating an articular surface with the proximal phalanx. Stability of the reconstructed fourth MCP joint was achieved using the capsule from cement spacer and a temporary K-wire (Figure 5).
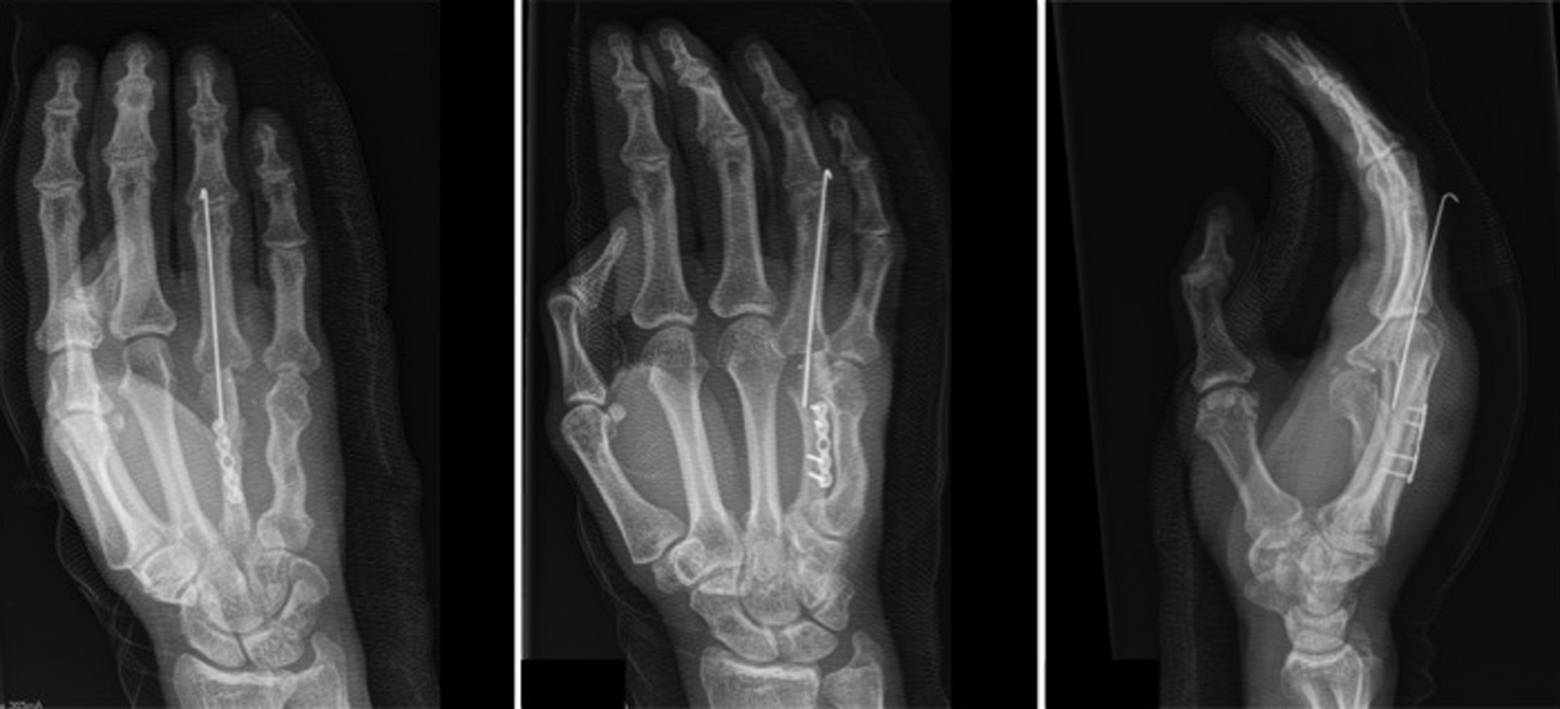
Right-hand X-ray (posterior–anterior [PA], oblique, lateral) following placement of iliac crest bone graft.
Six months following reconstruction, the patient is pain-free and has returned to his premorbid employment as a labourer. There is bony union at the site of the bone graft. Reconstruction of the fourth MCP joint was not successful in creating a joint with active or passive ROM. Despite this, the patient’s dominant hand functions well holding and using tools including those requiring significant grip strength (ie, hammer). His active ROM (flexion/extension) is as follows: MCP joint: 10°/+10°, proximal interphalangeal joint (PIPJ): 90°/0°, distal interphalangeal joint (DIPJ): 50°/0°. His strength at last follow-up was 15 kg·F for his right hand and 30 kg·F for the left.
Discussion
To our knowledge, this is the first reported case of a Brodie abscess in the hand. The time between presumed bacterial inoculation by a “fight bite” and presentation was at least 8 years. We hypothesize that the Brodie abscess formed in medullary canal of the metacarpal shortly after the “fight bite.” Years later, relatively minor hand trauma caused a cortical break and an acute infectious presentation. The presence of a gram-negative microbe (A actinomycetemcomitans) commonly associated with periodontal disease in the medullary canal of the metacarpal supports this theory. 7,8
A Brodie abscess may present in a variety of ways, making diagnosis challenging. On X-ray, Brodie abscess may resemble other benign and malignant bone lesions. 3 Common features include a radiolucent lytic lesion with well-defined sclerotic borders ranging in diameter from 4 mm to 5 cm. 1-3,6 Additional imaging including scintigraphy, CT, and magnetic resonance imaging can help narrow the diagnosis. Definitive diagnosis is achieved through biopsy. 3
Treatment of Brodie abscess can be surgical or nonsurgical depending largely on the patient’s signs and symptoms. In patients who are systemically well and do not have an associated soft tissue infection, surgical debridement can be delayed until treatment with antibiotics alone has failed. 5,6 The prognosis is generally very good with high rates of infection clearance. 1
The nature and location of the infection in this patient created some challenges. The acute, aggressive nature of this patient’s infection necessitated surgical excision of the fourth metacarpal head and neck in his dominant hand. The potential for long-term disability was relatively great in this case. Fortunately, the digit was salvaged and the patient was able to return to work despite a permanent change in the fourth MCP joint on his dominant hand.
Summary
We have described the first instance of a Brodie abscess of the metacarpal caused by A actinomycetemcomitans. This case highlights the importance of a thorough history and physical examination in the setting of human bite injuries in the past or present. Treatment of aggressive hand infections often requires a combination of medical and surgical intervention. Although the potential for long-term disability is high in aggressive hand infections, rapid treatment, early physiotherapy, and common reconstructive techniques can produce a good functional outcome.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
