Abstract
Bizarre parosteal osteochondromatous proliferation, also known as Nora lesion, is a rare benign surface lesion of the bone commonly affecting the hands and feet. It has an aggressive local growth pattern and high rate of recurrence post-excision. The authors report a case of recurred Nora lesion involving thumb metacarpal neck. En bloc resection with immediate reconstruction using distal radius bone graft was provided as a treatment with no clinical or radiological recurrence at 2-year follow-up.
Keywords
Introduction
Bizarre parosteal osteochondromatous proliferation, also known as Nora lesion, is a rare benign exophytic lesion of osteochondromatous origin. 1 It most commonly presents in the hands and feet; despite being benign, it has an aggressive local growth pattern. 2,3 It has only been reported in case reports or series due to its rarity. There is no official treatment guideline and it has a high recurrence rate post-excision. 3,4 Due to its rare presentation, Nora lesion can easily go unrecognized and therefore inappropriately managed. A delayed presentation can result in aggressive surgical management such as a ray amputation that significantly affect hand function. 5 We report a recurred Nora lesion involving thumb metacarpal (MC) neck and our management to preserve function and prevent recurrence.
Case Report
A 20-year-old right-hand-dominant nurse with no significant medical history presented with a right thumb mass that was first noticed in 2011. The mass was initially regarded as a ganglion cyst but became progressively firmer, leading to her plastic surgery consultation in July 2014. The mass slowly increased in size over the years and caused discomfort with repetitive thumb motion but was non-painful at rest. There was no history of trauma or fracture of the right hand. On examination, there was no overlying skin change. The fixed firm mass was 1 × 1 cm in size and located at the radial side of MC neck distal to the insertion of abductor pollicis brevis. Range of motion (ROM) of the thumb was full. Neurovascular exam was normal. X-ray imaging showed a well-calcified bony growth continuous with the first MC and circumscribed with internal trabeculation and overlying solid cortex. The first metacarpal phalangeal (MCP) joint space was maintained (Figure 1).
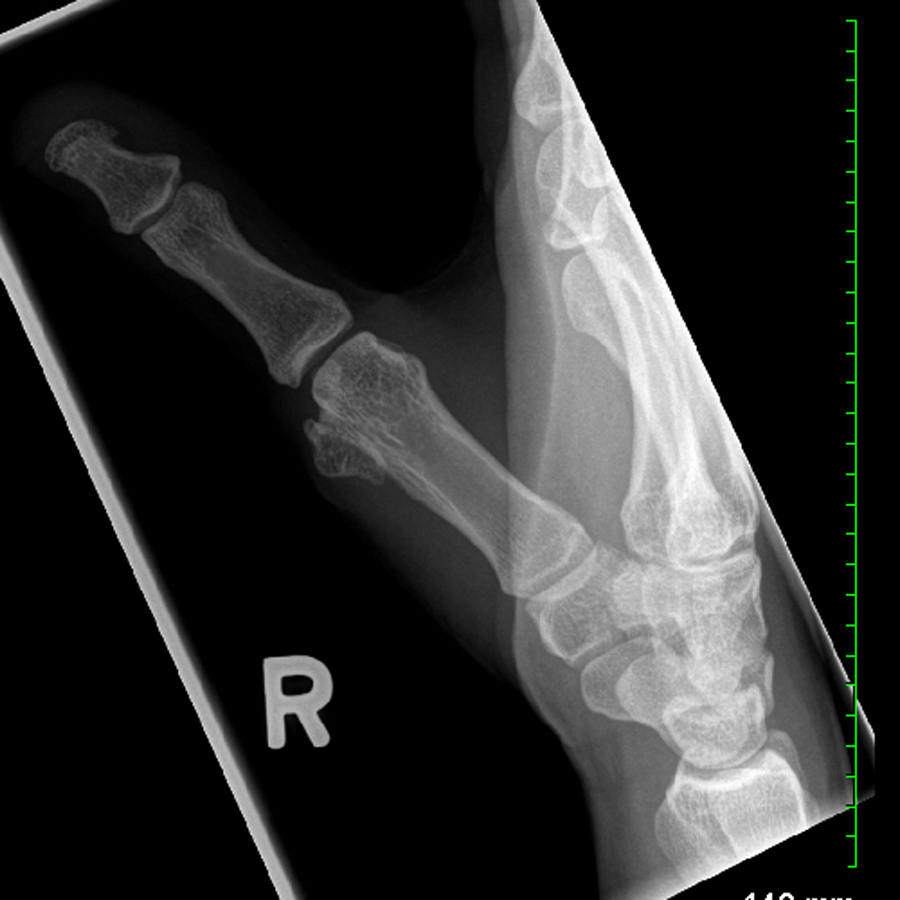
Radiograph of the right hand at the initial presentation showing broad-based exostosis at the radial side of first metacarpal neck with normal trabecular and cortical margins and no continuity of lesion with the medulla.
Benign exostosis was regarded as the most likely diagnosis by both the plastic surgeon and the radiologist. Simple resection of the nodule was offered to the patient. The bony lesion, which was found to be 5 to 6 mm in diameter, was shaved from the MC head to achieve a smooth contour. Histology and pathology revealed benign appearing bone, cartilage, and fibrous tissue arranged in a bizarre pattern with the characteristic “blue bone,” typical of Nora lesion 4 (Figure 2).
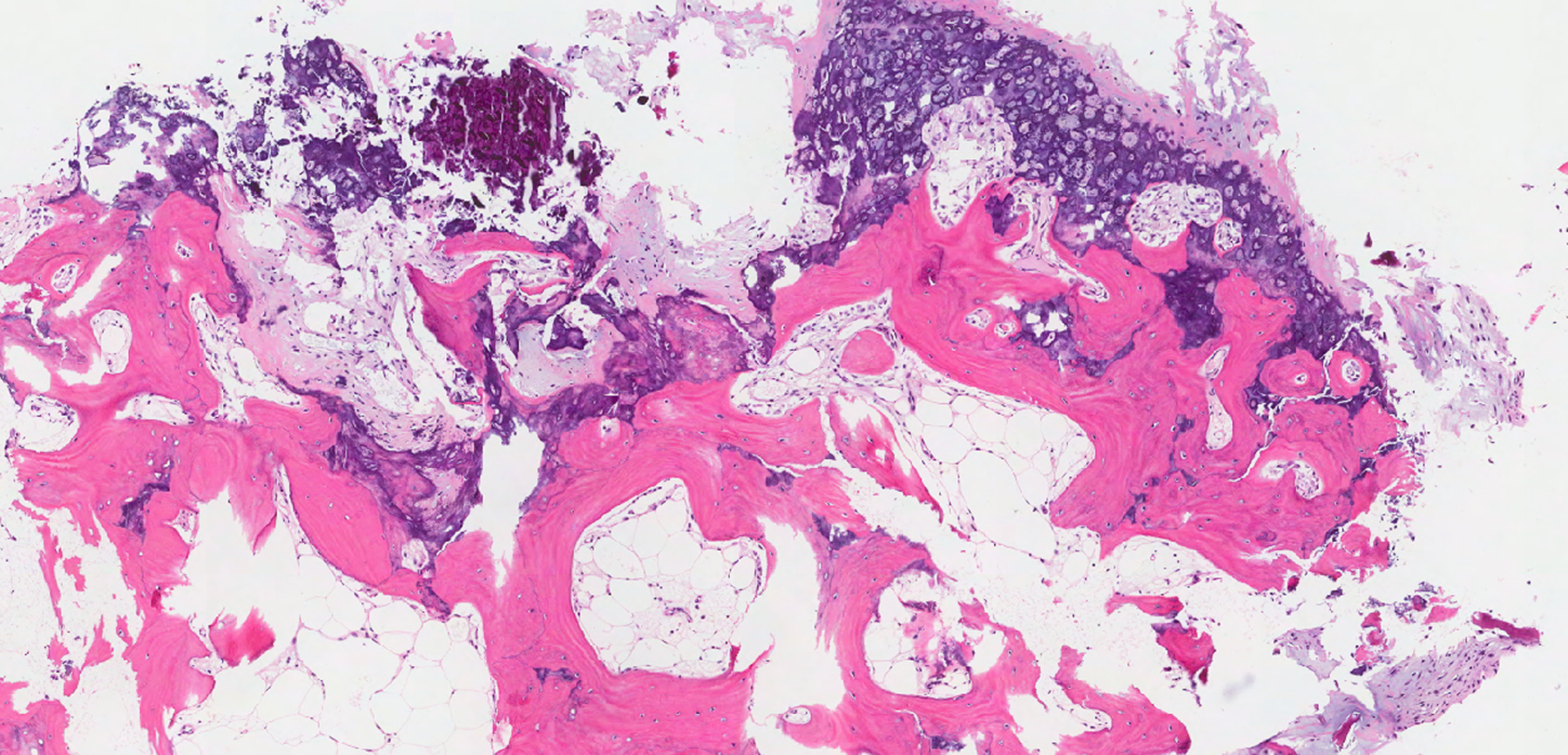
Initial resection specimen demonstrating irregular maturation of hypercellular cartilage into bone, producing bone with the characteristic blue quality (“blue bone”). At this low-power magnification, a zonal pattern can be appreciated (40× magnification, hematoxylin and eosin stain).
One year later, the patient returned to the clinic with increased pain and swelling at the same radial aspect of the first MC neck. X-ray imaging revealed recurrence of the bony lesion with increased size (Figure 3). The patient consented to en bloc resection of the lesion. Intraoperative finding revealed a 1.5 cm well-circumscribed firm mass with a white cartilage cap that occupied two-third of the MC neck and head and abutted the articular surface (Figure 4). An oscillating saw was used to excise the tumor en bloc with 2 to 3 mm margin. A baby rongeur was used to curette the cancellous part of the MC head with preservation of the articular cartilage. The pseudocapsule over the lesion and any abnormal periosteal tissue was excised. A clear margin was felt to be achieved clinically on gross examination. This left a sizable defect of the MC head/neck region with only ulnar side of the cortex intact. A 2 × 1.2 × 0.8 cm cortico-cancellous bone graft harvested from the distal radius was wedged into the MC defect and fixed to the remaining ulnar side MC cortex using 2 lag screws. The patient was then splinted with a plaster thumb spica for 6 weeks. The pathology confirmed the diagnosis of recurrence of Nora lesion (Figure 5).
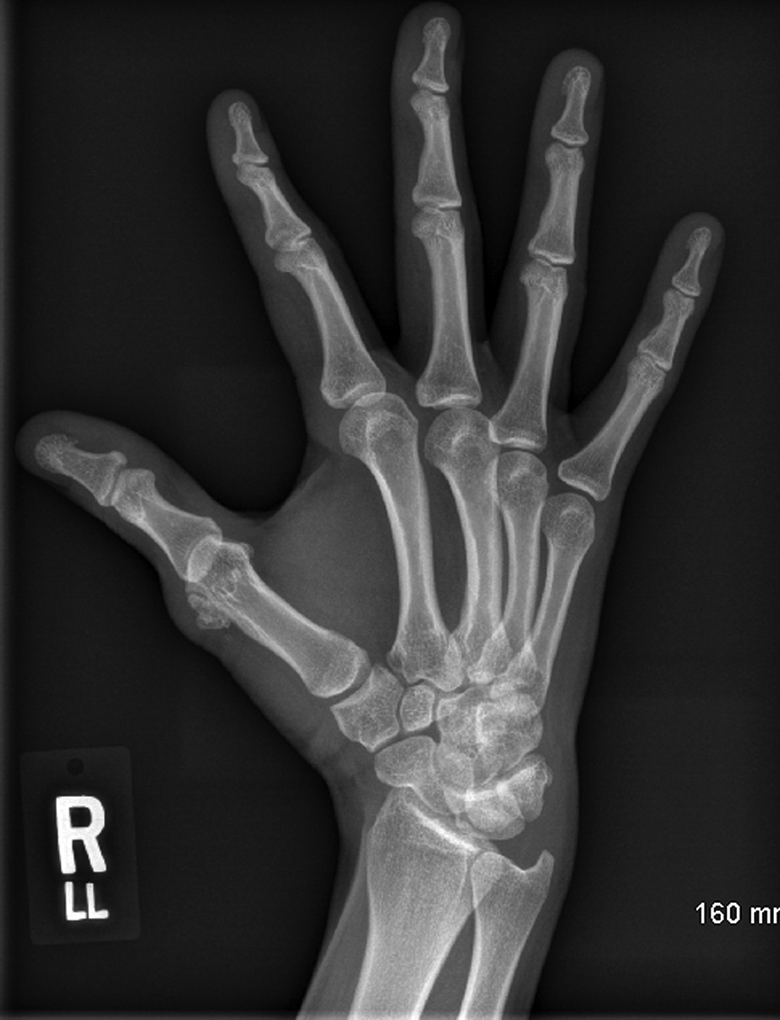
Radiograph of the right hand 1 year post-first excision showing recurrence of the broad-based exostosis.
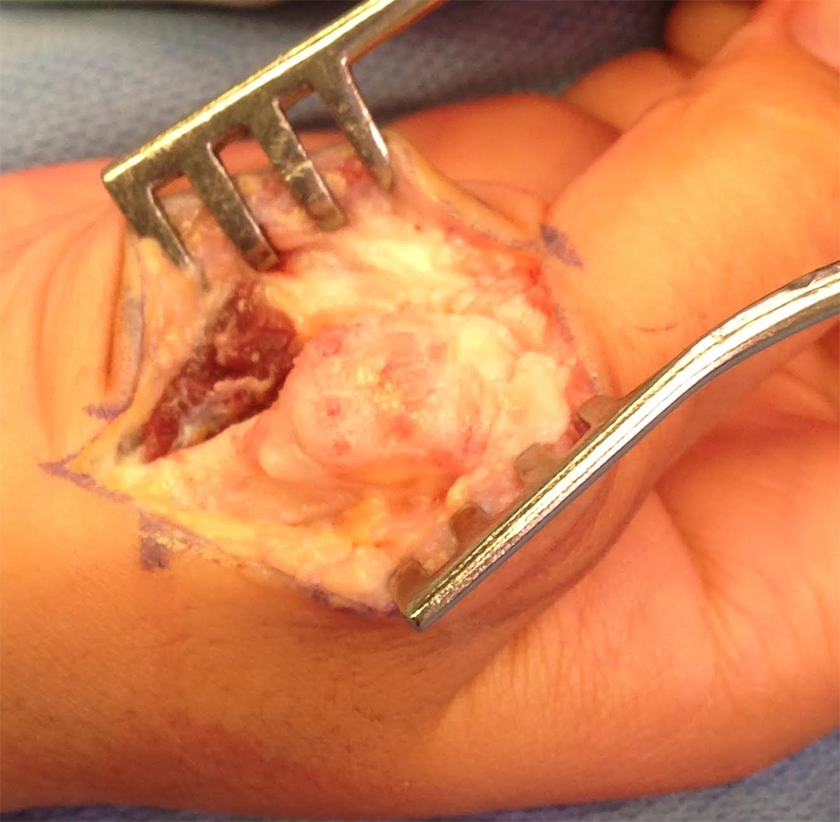
Intraoperative exposure of the recurrent Nora lesion at the first metacarpal of her right thumb.
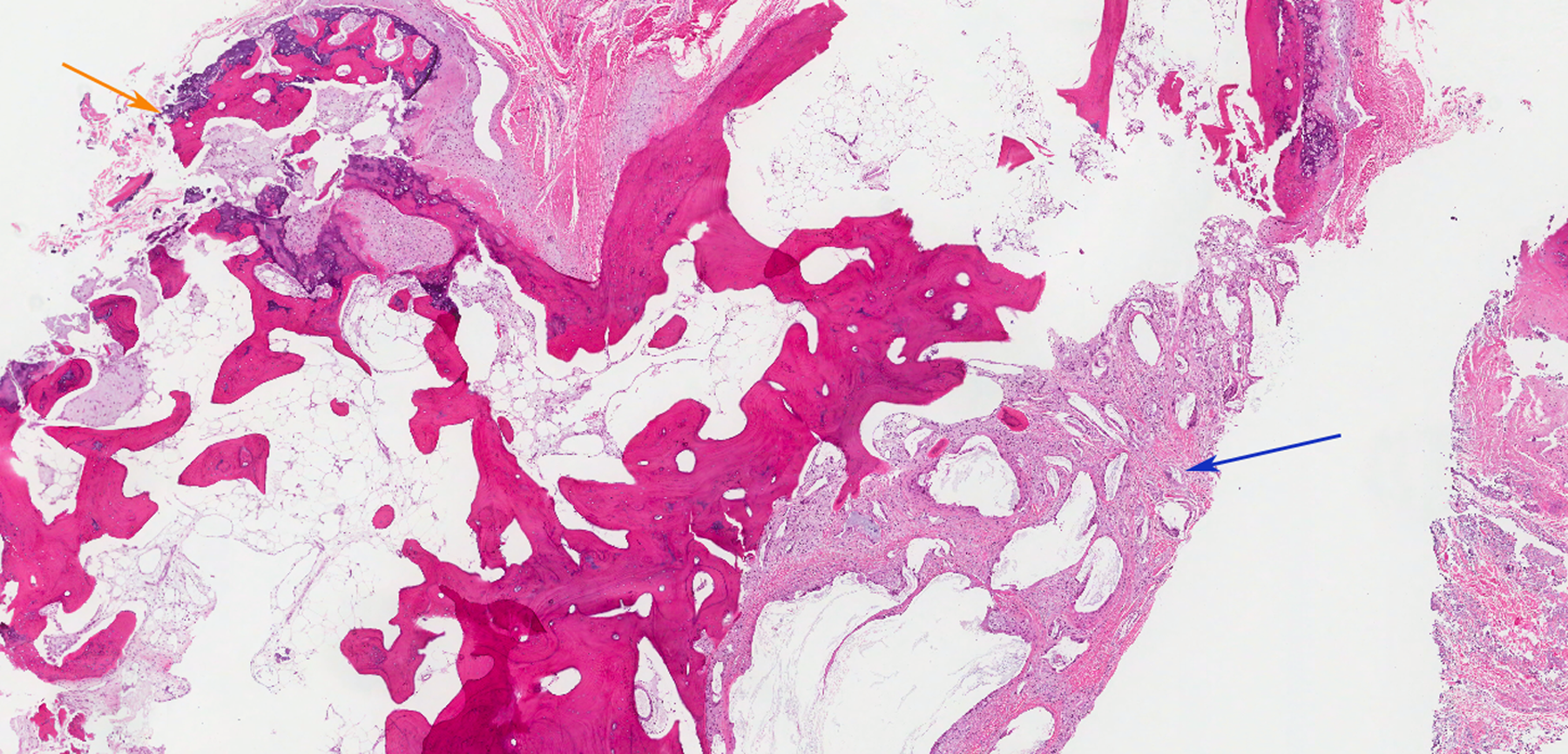
Recurrent lesion with prior surgical related changes (blue arrow) including foreign body giant cell reaction, chronic inflammation and reactive fibrosis, and recurrent Nora lesion (orange arrow) (40× magnification, H&E stain).
The patient recovered well from the en bloc resection without complication. At the 1-year follow-up in September 2016, she has normal ROM of right thumb with normal pinch and grip strength and no pain at the thumb MCP. X-ray imaging at the 22-month follow-up showed a congruent thumb MCP joint with normal joint space and no recurrence of the bony lesion. The bone graft showed no sign of non-union or mal-union and the 2 lag screws remained intact without signs of loosening (Figure 6).
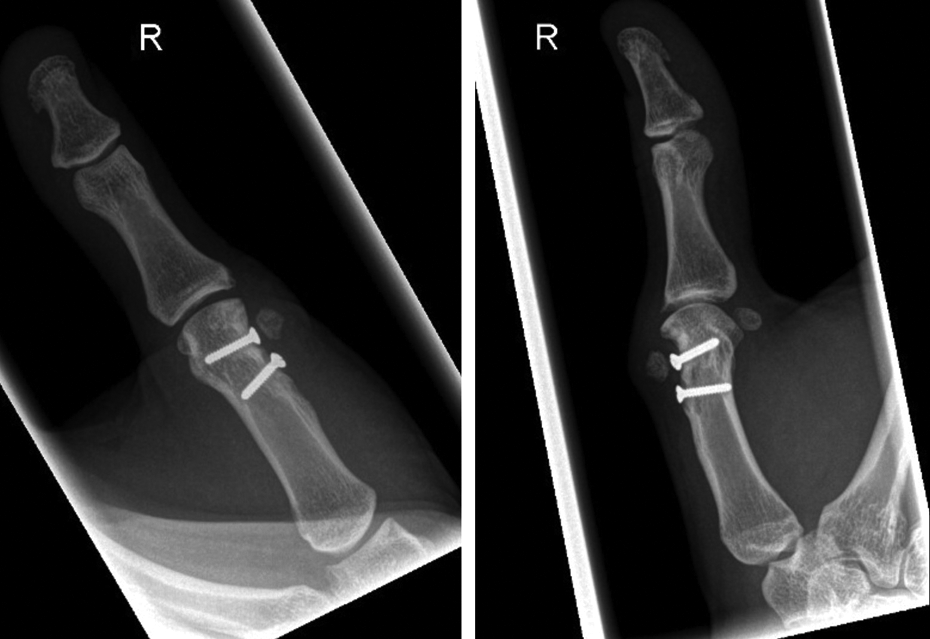
Radiograph of right thumb metacarpal at 22-month follow-up post-en bloc resection of Nora lesion and bone graft reconstruction. Both anteriorposterior (left panel) and lateral (right panel) views demonstrate preserved joint space and no evidence of recurrence.
Discussion
Bizarre parosteal osteochondromatous proliferation, also known as Nora lesion, is a rare benign exophytic lesion of osteochondromatous origin. 1 It most often affects the bones of distal extremities of young (20- to 30-year-olds) adults, equally in both sexes. 2 Hands are affected 4 times as common as the feet, with the most common sites being the proximal and middle phalanges and the MC or metatarsal bones. 2 To date there are over 200 reported cases 3 ; however, as most lesions are reported as case studies, it is difficult to elucidate its prevalence or etiology. 2 There are arguments both for 4,6,7 and against 8-10 trauma as a cause, while others label it as a neoplastic process 11 with possible associated genetic translocation. 12,13
Clinically, Nora lesion typically presents as a minimally painful swelling in the hands or feet that slowly grows over months to years. 1 The lesion is considered to be benign with no known case of metastasis; however, its local growth pattern is aggressive. 3 On plain radiography, Nora lesion typically shows a well-marginated exophytic lesion. It can be differentiated from osteochondroma from its lack of communication with the underlying medulla and lack of cortical flaring. 1,4 Microscopically, Nora lesion demonstrates irregular maturation of hypercellular cartilage into bone, producing bone with the characteristic blue quality (“blue bone”). 4 The lobules of cartilage contain atypical binucleate chondrocytes, and between the bony trabeculae, there is a benign spindle cell proliferation. 14 A zonal pattern can be appreciated with a transition from the fibroblastic proliferation at the periphery of the lesion to the cellular cartilage and “blue bone” adjacent to the cortex (Figure 2). Because of its disorganized architecture and cytologic atypia, Nora lesion may be mistaken for chondrosarcoma or osteosarcoma. However, at low power, a characteristic zonal pattern can be appreciated.
Since Nora lesion is benign, no treatment is needed if there are no symptoms. 15 However, given its typical aggressive local growth pattern, treatment of choice is local excision. Recurrence rate after local excision is high, ranging between 20% and 55%. 3,4,6,16 The degree of resection required to prevent recurrence remains controversial. 3 Intra-lesional excision using curettage is generally not recommended due to association with higher recurrence rate. 17 Some surgeons recommend formal excision of the pseudocapsule, underlying periosteum, and any suspicious-looking cortex to ensure a clear margin. 14,18 However, some advocate against wide excision as the first-line treatment due to the risk of surgical morbidity such as segmental bone loss that results in amputation of fingers or toes. 2,19 Several factors should be considered prior to excision. First is the location of the lesion and the impact of en bloc resection on function. Second is the appearance of the lesion being pedunculated versus sessile. Marginal resection is recommended for fingers and/or pedunculated lesions. En bloc resection is recommended for toes and/or sessile lesions. 18 In addition, Ly et al. has also suggested delaying surgery until the lesion is no longer active as recurrence is more common in the active growth phase which showed increased bone scan uptake. 20 Currently, there is no consensus on how to reconstruct the bony defect post-resection of the Nora lesion. Unlike enchondroma, which has evidence for comparable healing, ROM, and recurrence rate regardless of graft material used, 21 there is no evidence on how graft choice impacts the disease outcome regarding Nora lesion. Most reports on Nora lesion did not discuss the reconstructive method used—that is, autograft, allograft, or no graft. 1,2,3,7,8,9,14,17,18
Given the rare nature, high local recurrence rate, and lack of adjuvant therapy, Nora lesion should have long-term follow-up. Timeline between excision and recurrence has been reported to be between 2 months and 2 years. 4,22,23 It is recommended that follow-up should be every 6 months for the first year and annually for the next 2 years. In addition, patients should be clearly informed of the high risk of recurrence. 24
In this case, the initial intra-lesional excision led to local recurrence. On the second surgery, the mass was excised as an en bloc to achieve clinically adequate margin and preserve the joint surface. Immediate reconstruction with bone graft and robust fixation was provided to restore anatomical alignment. The en bloc resection with reconstruction proved to be effective in preserving function and preventing local recurrence.
Conclusion
Nora lesion is a rare locally aggressive bony tumor with high rate of recurrence post-excision. For patients with recurrence, adequate margin en bloc resection offers the best chance of cure. Immediate reconstruction should be offered when possible to preserve function and minimize surgical morbidity.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
