Abstract
Background:
Compartment syndrome of the hand is a well-described phenomenon with potentially devastating consequences. Although numerous mechanisms have been proposed, the extravasation of peripheral intravenous (IV) fluids remains a relatively rare etiology.
Objective:
Surgical dogma mandates emergent decompressive fasciotomies in the presence of hand dysfunction and impending tissue loss from supraphysiologic compartment pressures. The role of the subcutaneous space in acute compartment syndrome remains unclear.
Methods:
In this report, we present a case of a dorsal hand IV extravasation leading to an acute compartment syndrome of the subcutaneous space.
Results:
An emergent skin-only incision was used for decompression, with immediate improvement in symptoms and no long-term adverse sequelae.
Discussion:
The subcutaneous space appears capable of sustaining supraphysiologic pressures that impair cutaneous perfusion. This closed anatomic space can be readily decompressed, resulting in rapid improvement in soft tissue perfusion. However, its role in contributing to acute compartment syndrome of the hand requires further research.
Conclusion:
We propose consideration of the subcutaneous space as a distinct hand compartment and advocate selective compartment release when prudent.
Introduction
Acute compartment syndrome of the hand is caused by elevated interstitial pressure within a confined anatomic space. 1 Experimental and clinical reports demonstrate that sustained supraphysiologic pressures result in ischemia, cellular death, and irreversible tissue necrosis. Diagnostic criteria are imperfect and include assessment of swelling, tension, pain, and variable pressure thresholds measured using imprecise tools. Surgical dogma advocates emergent dorsal and volar fasciotomies to release 10 intrinsic hand compartments (thenar, hypothenar, adductor, 4 dorsal interosseous, and 3 volar interosseous) and the carpal tunnel (Figure 1). 1,2 The subcutaneous space of the hand is bounded by the overlying skin and deep myofascial layers but is rarely considered in the pathophysiology of acute compartment syndrome.
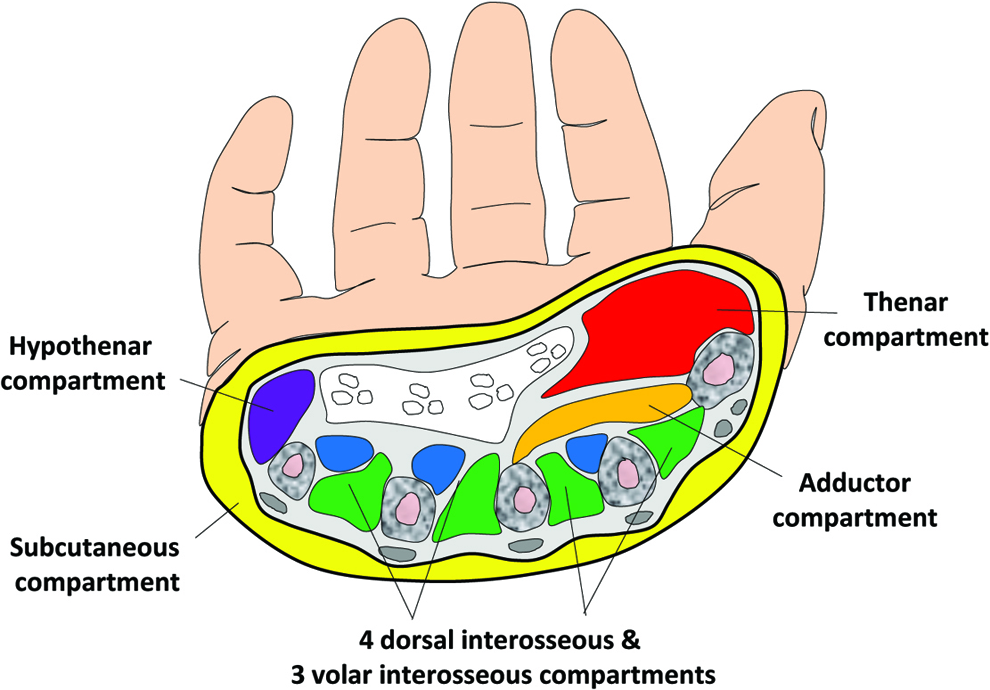
Schematic of 10 traditional myofascial compartments (thenar, hypothenar, adductor, 4 dorsal interosseous, and 3 volar interosseous) of the hand. Note the subcutaneous compartment that is bounded by the overlying skin and deep fascia.
Case Report
A 5-month-old boy in the pediatric intensive care unit developed a swollen, blistered hand after infiltration of a dorsal hand peripheral intravenous (IV) catheter. A solution of 5% dextrose in 0.45% sodium chloride was infused at a rate of 24 mL/h for approximately 2 hours prior to detection. Examination revealed a tense, blanched dorsal hand with absent capillary refill and limited spontaneous finger movement (Figure 2A). Epidermolysis was present at the digits, dorsal hand, and forearm. The blood pressure was 92/52 and hand compartment pressures were not measured. A 1-cm dorsal skin incision (Figure 2B) was performed emergently at bedside to decompress the hand. Capillary refill returned after several minutes and was complete within 2 hours (Figure 2C). Hand elevation and topical petroleum dressings were initiated. Follow-up at 10 days demonstrated a functional hand with no major skin necrosis (Figure 2D).
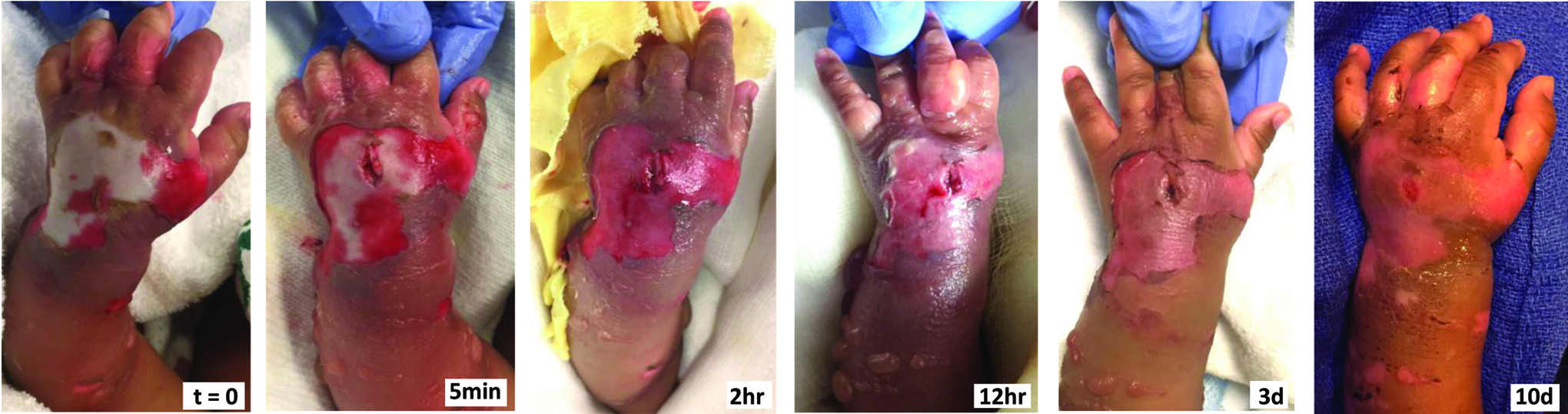
Clinical photographs demonstrating the appearance on initial examination (t = 0). A 1-cm incision is made through the skin only, decompressing the subcutaneous space. Note the improved skin perfusion at the wound margins by 5 minutes. At 2 hours, dorsal hand perfusion has been restored. At 12 hours, the blisters continue to evolve and epidermolysis has resolved by 3 days with continued hand elevation and topical petrolatum therapy. Outpatient follow-up at 10 days demonstrates skin healing with no major tissue loss.
Discussion
Nearly 200 million peripheral IV catheters are placed annually in the United States. 3 The extravasation of IV fluid into the perivascular tissues is a well-established complication, though generally minor in consequence. Conservative management including elevation, cool compression, hyaluronidase, and/or topical wound care is sufficient in a majority of cases, with less than 20% requiring surgical intervention. 4 Age is a significant risk factor for infiltration, occurring in 11% of hospitalized children and up to 28% of the pediatric intensive care population. 5 This is due in part to the smaller, more fragile vessels found in children. Accordingly, smaller gauge peripheral catheters are typically used, which paradoxically exposes the delicate vessels to higher infusion velocities as described by Bernoulli’s inverse relationship between velocity and cross-sectional diameter. 5 Not only are infiltrations more common in children but, when identified, tend to be more severe. This is due to delays in detecting infiltrations as children are limited in their ability to communicate symptoms, are frequently swaddled in blankets and bulky dressings that cover catheter sites, and may be uncooperative with examinations. 6
Once infiltrated, an increase in compartmental pressure develops from both the direct volume expansion and the secondary inflammatory effects of the infiltrated agent on the soft tissues. 1 The osseous–fascial boundaries enclosing deep hand compartments exhibit low compliance, resulting in dramatic increases in pressure for a given increase in volume. When compartmental pressure overcomes venous capillary perfusion pressure, circulation is impaired, leading to ischemia, cellular death, and, ultimately, irreversible necrosis of the structures contained within that space. 2 Early diagnosis remains challenging, particularly in the hand where the traditional signs and symptoms of compartment syndrome are frequently absent. 2,5 Instead, clinicians must rely on subjective findings, such as the extent of swelling, pain with motion, and intrinsic minus positioning. 1,2 Compartment pressure measurements can be used as a diagnostic aid; however, available devices are imprecise, invasive, and lack consensus on thresholds for intervention. 2
A recent systematic review of infiltration-related compartment syndromes reviewed 51 cases, of which 20 occurred in the hand. 6 Age was found to be a significant risk factor, with 40% of cases occurring in the pediatric population. Other risk factors included pressurized infusion systems and barriers to communication, such as altered mental status or mechanical ventilation. Physiologic IV fluid solutions or radiographic contrast were the causative agent in over 70% of cases. In each of the reviewed cases, emergent surgical intervention was performed to relieve compartment pressures. However, the specific decompressive techniques (skin only vs selective compartment vs total compartment release) were not delineated. Although a majority of cases reported no long-term deficits, 1 case required amputation and 5 reported significant functional deficits. 6 Another report described 3 cases of compartment syndrome in children caused by peripheral IV infiltrations, 2 of which were in the dorsal hand. 5 In each case, IV fluids were delivered via a pressure sensing infusion pump. All patients in the series underwent emergent fasciotomies to release the dorsal, volar, and carpal tunnel compartments.
Fasciotomy remains the definitive management for suspected compartment syndromes regardless of location. In the hand, classic teaching advocates the release of all 10 intrinsic hand compartments in addition to the carpal tunnel. DiFelice et al were among the first to characterize these compartments using cadaveric injection studies. 7 Despite noting significant variation in fascial distribution and frequent sub-compartmentalization, the authors strongly encouraged 10 compartment release when compartment syndrome is suspected. However, the validity of these findings has been questioned, as injection studies are frequently unreliable and highly user dependent. A recent cadaver study investigating hand compartments also noted substantial variability in fascial distribution and concluded that dense fascia did not reliably encase any of the intrinsic hand muscles. 8 Notably, the authors observed that the overlying skin and subcutaneous fat were tightly adherent to the underlying musculature, hypothesizing that this relatively unyielding layer could withstand high pressures and contribute to the development of compartment syndrome.
Experimental evidence demonstrates that pressures in the adult forearm and fingers as low as 33 and 23 mm Hg, respectively, can impair vascular flow through the subcutaneous space. 9 Even lower subcutaneous pressures would theoretically restrict flow in children given their lower systemic mean arterial pressures. In fact, a “subcutaneous compartment syndrome” has previously been described in burn patients. 10 Burn injury can produce acute volume expansion of the subcutaneous compartment which is restrained by the tight overlying skin/eschar, resulting in compression of the deeper compartments.
Here, we describe a case in which extravasation of physiologic IV fluid into the subcutaneous space resulted in acute compartment syndrome-like phenomena within the hand. Due to early detection and the known mechanism of injury, we were able to perform a limited skin incision to decompress the pressurized compartment and restore limb perfusion. Clinicians must maintain a high suspicion for the development of compartment syndrome and act promptly to relieve supraphysiologic pressures. Future research is needed to examine the potential of elevated subcutaneous pressures to impair vascular flow and cause ischemic damage to the skin, nerves, and muscle. We propose consideration of the subcutaneous space as a distinct hand compartment capable of producing acute compartment syndrome and advocate for selective compartment release when clinically indicated.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
