Abstract
The use of polyacrylamide hydrogel (PAAG) as an injectable filler for breast augmentation has fallen out of popularity since its first use in the 1980s but has produced an increasing patient population presenting with complications related to PAAG injections. Polyacrylamide hydrogel use was popularized most notably in China, Russia, and Iran. However, given immigration trends and medical tourism, PAAG-related complications have become increasingly more common in North America. These complications can be difficult to treat, often necessitating complex surgery that includes gel removal, debridement procedures, and often breast reconstruction. Approaches to surgical treatment and subsequent breast reconstruction are not universally defined primarily because of the limited knowledge about this group of patients. This article presents the option of autologous free flap reconstruction for a patient with extensive muscular involvement and aims to summarize complications and risks associated with PAAG through case report and a review of the literature.
Introduction
Polyacrylamide hydrogel (PAAG) injectable filler is 2.5% cross-linked polyacrylamide combined with non-pyrogenic water. No clinical trials were ever conducted for the safety and use of PAAG for tissue augmentation, but it was used for over 2 decades in the treatment of breast tissue atrophy, reconstruction following malignant tumor mastectomy, and breast augmentation due to mammary dysplasia. 1,2 This form of augmentation was popularized in the former Soviet Union and was most notably practiced in Russia, China, and Iran. 3 Polyacrylamide hydrogel injections were further portrayed by the media and advertised as a relatively cheap procedure requiring no anesthesia or surgical skill that could be performed in an office setting. 4 As many as 300 000 women have been treated for PAAG injections. 5 Polyacrylamide hydrogel injections have been used in both legal and illegal institutions, such as beauty parlors by non-medical professionals. 2
Aquamid is a representative of PAAG. The monomer of Aquamid in low enough concentrations has been regarded as atoxic to humans and other animals. However, the acrylamide monomer possesses neurotoxicity and teratogenicity. These monomers can often be residually present during the synthesis of PAAG, which has the potential to cause toxicity to nerve and muscle function. 1,5 With these findings, in 2006, the Chinese State Food and Drug Administration announced that PAAG would be prohibited from production and clinical application in plastic surgery. 6
Currently, we are now progressing into the era where we can expect to see patients presenting for treatments of PAAG complications and adverse reactions. 6 Documented complications following PAAG injections include induration, lumps, hematoma, infection, inflammation, persistent mastodynia, poor cosmetic result, glandular atrophy, gel migration, and potentially a delayed diagnosis of breast cancer. 2,7 These complications can be difficult to treat and often necessitate complex surgery that includes gel removal, debridement procedures, and most often breast reconstruction. Approaches to surgical treatment and subsequent breast reconstruction are not defined primarily because of the limited knowledge about this group of patients. 5 This article aims to summarize complications and the risks associated with PAAG through a case report and review of the literature.
Case Report
A 45-year-old female Asian patient presented initially with complaints of painful breast masses. She had immigrated to Canada from China in 2010 and had previously received PAAG for breast augmentation in 1996 at a local city hospital. She was an otherwise healthy female who had become recently pregnant with her first child. She was referred to our plastic surgery service by Obstetrics/Gynecology and Genetics as they were following her for her new pregnancy and were worried about the teratogenicity surrounding her PAAG injections and wondered about removal of the implants and termination of her current pregnancy. Given this history of PAAG injections, magnetic resonance imaging of the breasts was obtained (Figure 1).
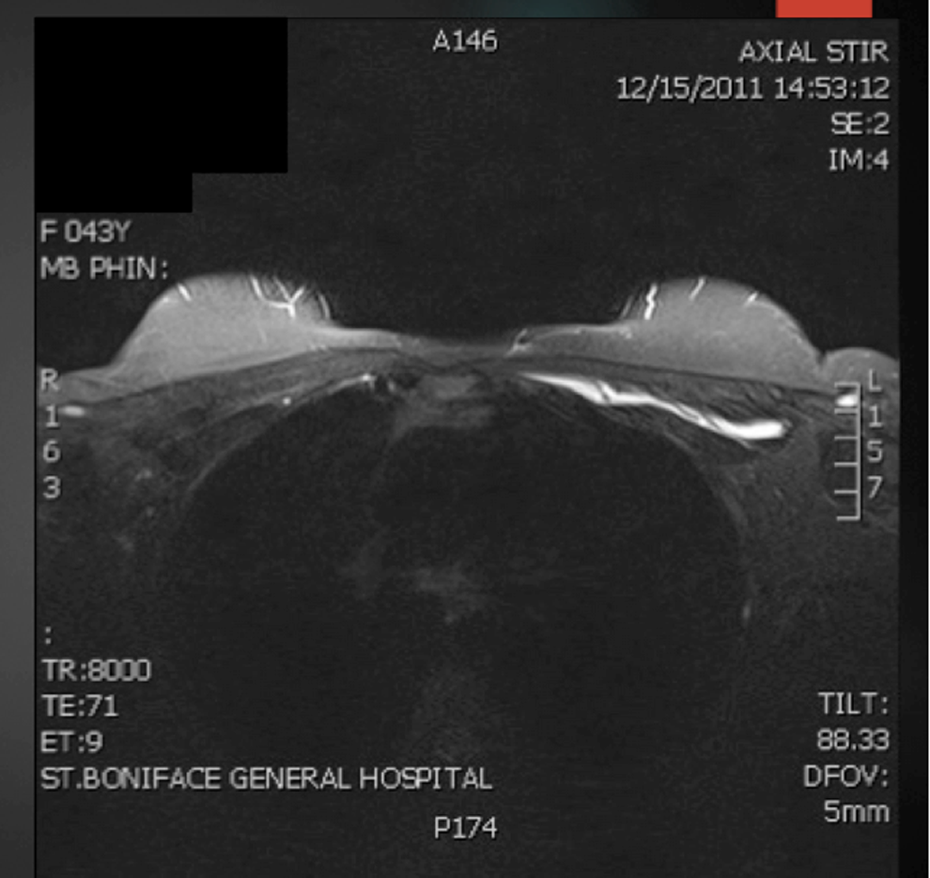
Magnetic resonance imaging (MRI) showing retroglandular, intraglandular, intrapectoral, and retropectoral extension of polyacrylamide gel.
Magnetic resonance imaging revealed multiple masses in both breasts. The right-sided injectable was more subglandular and the left injectable was more intramuscular and submuscular. At the initial assessment by our service, painful hard mass was observed in both right and left breasts. The patient stated this had been unchanged soon after her initial augmentation. There had been enlargement of breasts with pregnancy but no signs of infection, nipple drainage, or inflammation (Figure 2).
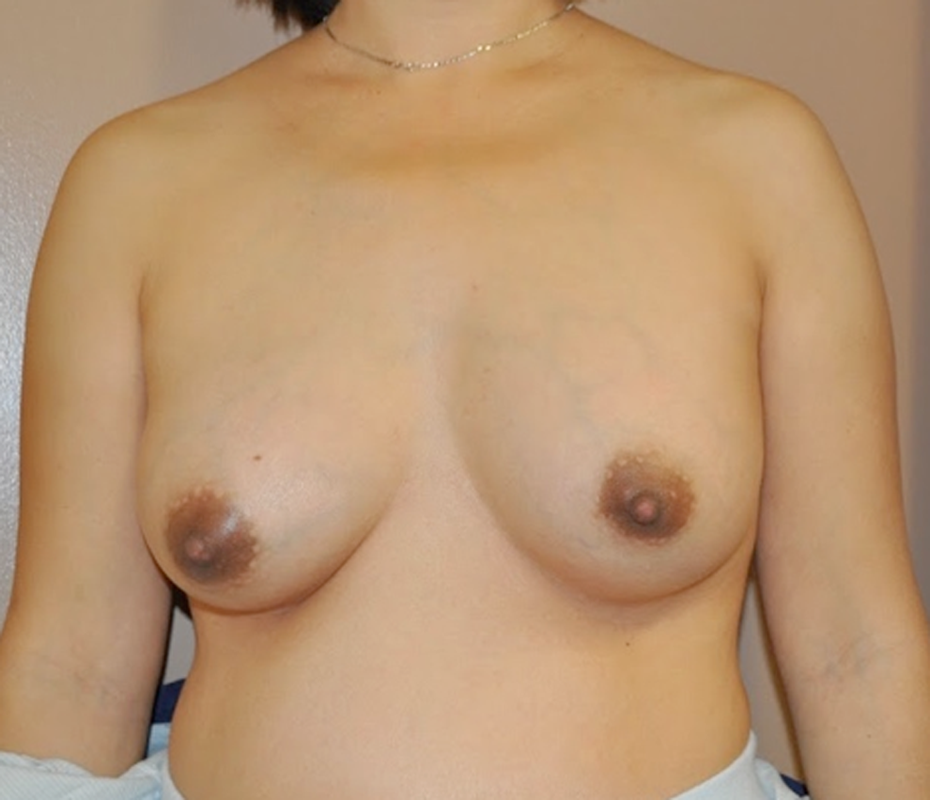
Pre-operative appearance.
A decision to continue with the pregnancy was made by the patient and the genetics service, given the lack of specific known teratogenic effects. The patient went on to deliver her child in May 2012; she did not attempt to breast-feed postpartum. Shortly after the birth of her son, during a second consultation with plastic surgery, she was given the option of PAAG removal and subsequent prosthetic or autologous reconstruction. The patient had wished for the PAAG to be removed as much as possible in order to minimize future complications. Therefore, given the amount of pectoralis major muscle resection required, concerns about placement of breast implants were raised. Ultimately, the patient elected to undergo bilateral mastectomy with immediate bilateral Deep Inferior Epigastric Artery Free Flap (DIEP) flaps (Figure 3).
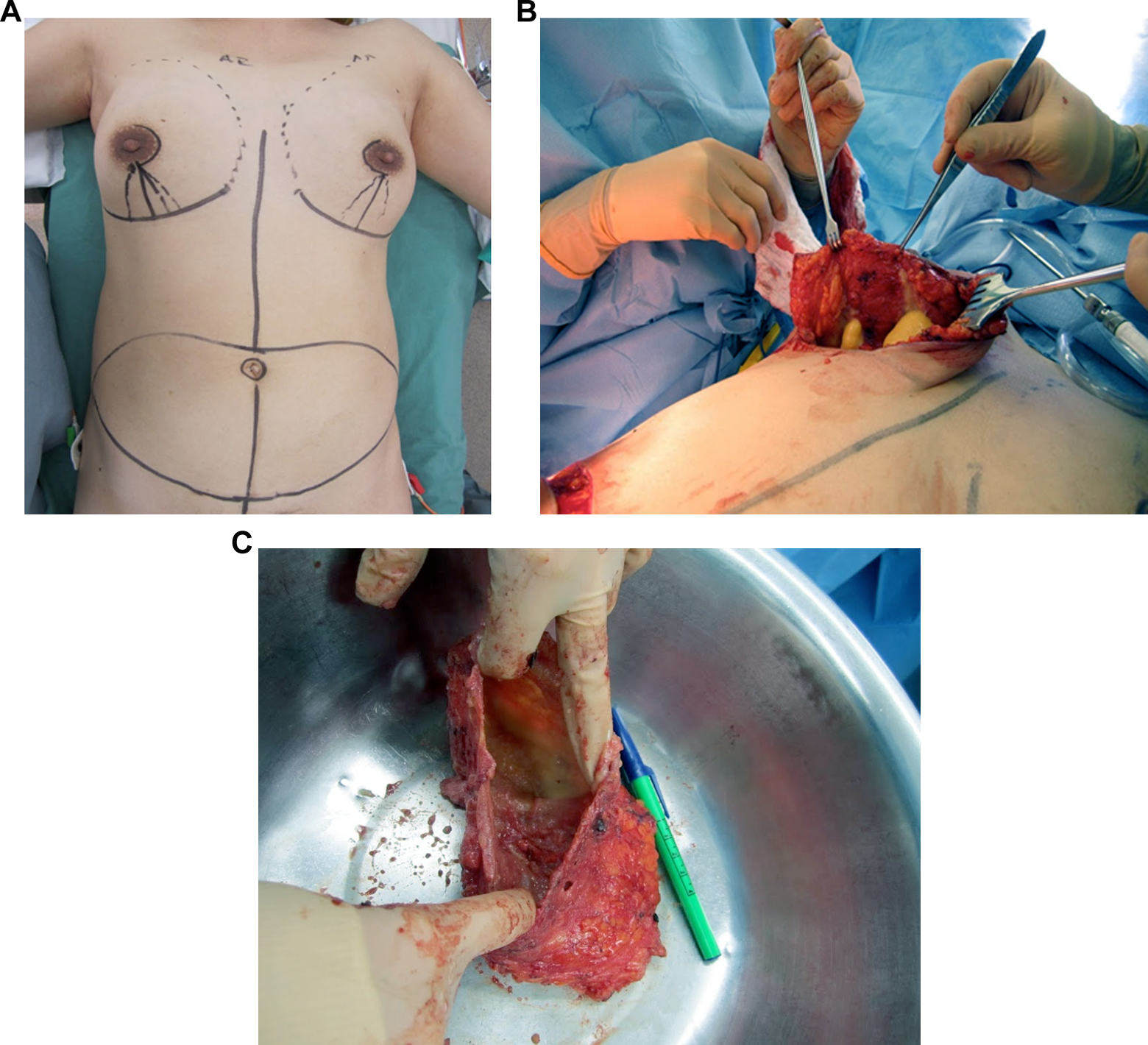
A, Pre-operative markings. B, Inframammary fold incision dissection revealing PAAG (yellow) material. C, Disected capsule that encased PAAG. PAAG indicates polyacrylamide hydrogel.
Surgery was carried out at the end of December 2012. Intraoperative findings included large amounts of PAAG with a porridge-like consistency deeply infiltrated in multiple planes of gland and muscle. Partial capsule formation was identified around some pockets of filler. There was diffuse infiltration throughout pectoralis major, especially on the left side, which necessitated significant amounts of muscle to be removed for maximal PAAG eradication. An uncomplicated immediate reconstruction with bilateral DIEP flaps was performed (Figure 4).
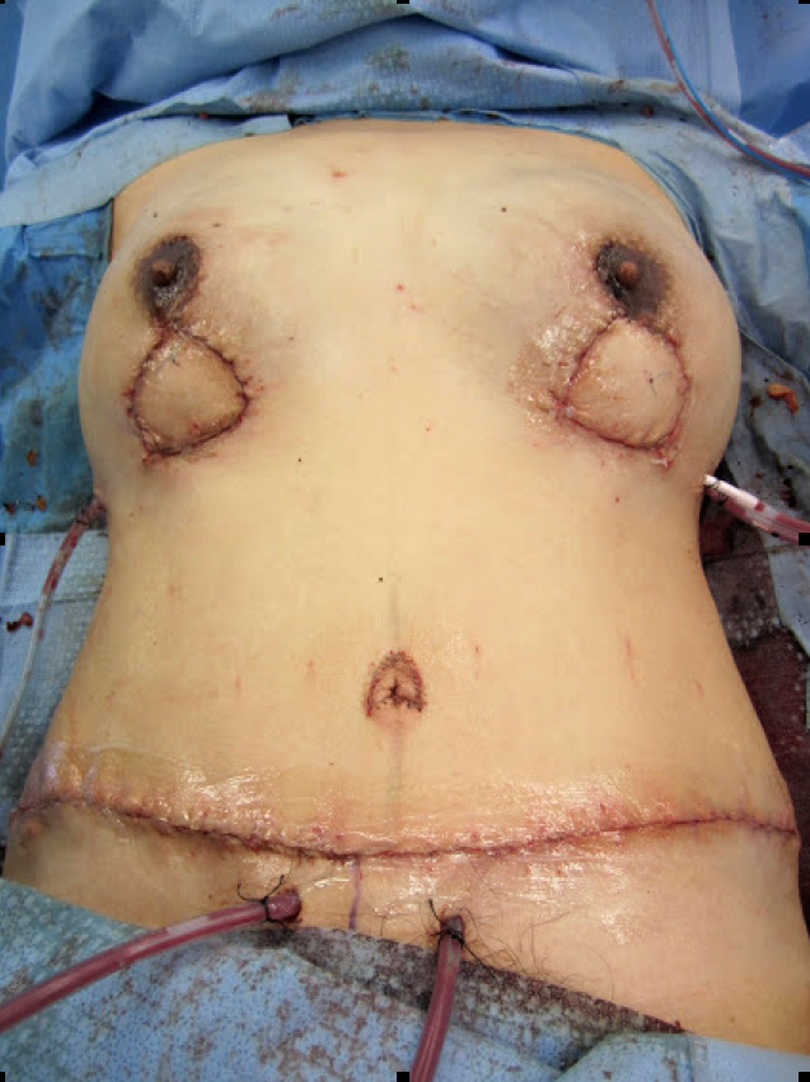
Post-operative appearance.
The patient had an uneventful recovery in hospital with complete flap survival bilaterally. On follow-up, good healing was noted of all surgical sites with no wound dehiscence and the painful masses had a complete resolution. Patient was pleased with the result with future plans to excise the flap skin paddle, which was used for monitoring and perform bilateral mastopexy discussed (Figure 5).
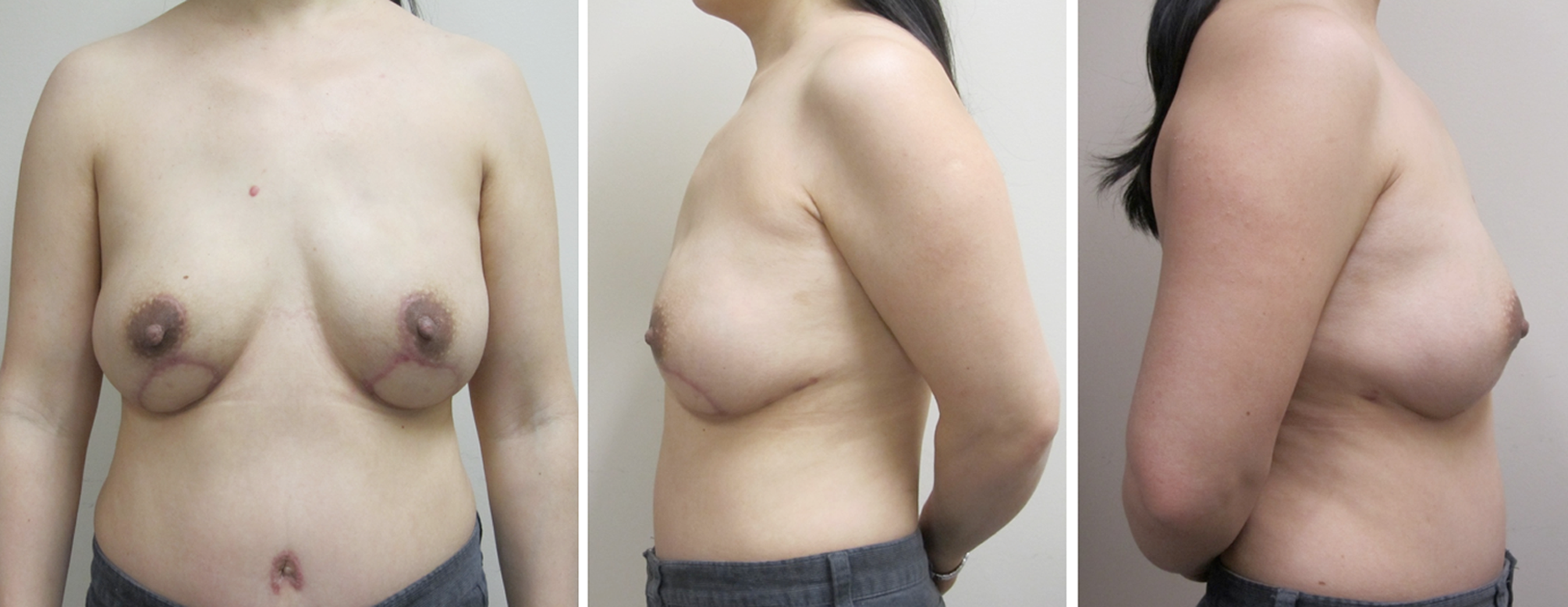
Final result at 3 months post operation.
Discussion
Global public awareness of PAAG injections has been increasing as of late. Surgeons without any experience with these injections are now beginning to see patients with PAAG-related complications. 5 Knowledge of this implant is important as Canada has a high Asian population, as well as increasing immigration from the Ukraine and the recent popularity of the medical tourism industry.
Complications
The largest case series of PAAG breast augmentation-related complications was described by Luo et al in their experience with 235 patients. 6 The population ranged in age from 20 to 38 years, and the time from injection to complication presentation ranged from 6 months to 10 years (39 months). They found the most common complication to be induration and masses (single or multiple) after PAAG breast augmentation, accounting for 78.9% of patients. The second most common being pain (67.2%). 6 Other more infrequent complications include asymmetry (20%), psychological problems or worry (12.3%), mastalgia with movement (8.5%), distant gel migration (8.9%), and nipple retraction and infection (2.5%). Approximately 72.8% of patients had multiple complications simultaneously, accounting for a total of 171 patients. 4,6
Patlazhan et al shared their 10-year experience in treating patients for PAAG breast augmentation complications in Ukraine and Sweden as fitting into 2 broad categories: those with (21%) and without (79%) signs of acute inflammation at presentation (mastalgia, hyperaemia, fever, swelling, fistula, or discharge). All complained of breast asymmetry and/or deformity, with 54% showing significant gel migration. 4
The most concerning complication by far is the increased risk of breast cancer. Cheng et al described 2 cases of breast cancer following PAAG augmentation. There is evidence to suggest that injectable biomaterial such as PAAG does put patients at a greater risk of breast cancer for several reasons. Polyacrylamide hydrogel will inhibit the growth of human fibroblasts and may cause the apoptosis of human fibroblasts, which leaves the potential for carcinogenicity. 7 Polyacrylamide hydrogel also can alter physical parameters such as the size and the granularity of human fibroblasts and induce an increase in messenger RNA expression of c-myc, a regulatory gene that codes for transcription factor and growth control. 7 Also given the most common clinical manifestations are in fact induration or lump and inflammatory reaction caused by PAAG, this might mask the presentation of breast cancer, delaying correct early diagnosis of malignant changes. Other reasons for a delay in recognition can be accounted for by confounding effects on interpretation of radiologic studies, as mammography cannot accurately assess the post-operative state of a PAAG-injected breast. 7
Wang et al have described special considerations for complications related to pregnancy, claiming that PAAG injections cause acute inflammation and galactocele formation during breast-feeding. 2 A large number of PAAGs have the potential to cause mastodynia, the mechanism being secondary to fibrosis and blockage of ducts due to osmotic self-expansion of PAAG. This gel-like substance mixes with breast milk and cannot be excreted. The deposits of PAAG can become a culture medium for infection and inflammation in breast tissue. Additionally, the pressure that is a result of injection may oppress lactiferous ducts, resulting in narrowing. Breast milk outflow becomes obstructed leading to fermentation in a short time and rapid breeding of bacteria contributing to infection. 2
Treatment
Eliciting the appropriate history and early recognition is key to diagnosis and treatment of PAAG-related complications. Magnetic resonance imaging is recommended as the most reliable screening method for the detection of masses following augmentation; the same is true for a PAAG-injected breast. Sentinel lymph node biopsy is also suggested for a PAAG augmented when a palpable mass is indistinguishable from a gel collection. 4,5,7
A treatment protocol developed by Patlazhan et al uses the presence of acute inflammation and infection as a major factor as to whether or not a patient will receive single-stage or 2-stage treatment. Those with signs of infection received 2-stage treatment, removal and delayed reconstruction, whereas those with no signs of infection had PAAG masses excised and immediately reconstructed. 4 Similarly, Wang et al suggest treating local and systemic infections first, allowing for the breast to retain its normal shape before performing surgery. This process ranged from about 2 to 8 weeks. 5 The literature describes either inframammary or periareolar incision for evacuation of the injectable PAAG. 8
Successful treatment of the PAAG augmentation complication requires removal of as much of the material as possible. Conservative management such as aspiration is ineffective. Discussion with the patient should explain complete removable is impossible and that residual PAAG will be left behind. The location, size, and extent of infection and the interrelation between infected tissues and surrounding tissues will influence surgical planning and technique. Commonly, incisions at inframammary fold and drainage at low sites are applied. 8 In addition, the injected PAAG that is scattered, foci usually have a capsule and fibrous septum is common between lesions. The key to surgical procedures is to completely separate the infected tissues and cysts and thoroughly remove the materials and necrotic tissues, granulation tissues, and fistula. Given the hydrophilicity of PAAG, the wound should be repeatedly irrigated with antibiotics in normal saline until the fluid in the drainage is clear, and PAAG granules and pus are not observed. 5
Reconstruction
There is no literature documenting immediate autologous tissue reconstruction. Reports have only been made on prosthetic reconstruction. Luo et al performed periareolar evacuation of hydrogel in 235 patients, 136 desired volume reconstruction, which was performed via implantation post surgical resection of PAAG. Dual plane silicone implants placed immediately in 108 patients or after 6 months in 28 patients. Of 136 who underwent reconstruction, 3 developed a Baker 2-3 capsular contracture and 1 inflammatory reaction was documented. Nearly all patients reported a complete resolution of pain, lumps, and infection. 6
Deep inferior epigastric perforator autologous free flap was chosen in our patient because of the extensive amount of PAAG deposits involving the left pectoralis major muscle necessitating the removal of majority of the muscle, thus an implant could not be placed. Furthermore, the patient also did not desire the look of implants. That being said, in other patients choosing an implant-based reconstruction and the recent popularity of acellular dermal matrix, a total subglandular positioning of an implant could be carried out.
Conclusion
Although PAAG breast augmentation has been confined to Europe and Asia, North American surgeons may increasingly encounter foreign patients with PAAG-related problems given globalization and the recent popularity of medical tourism in today’s society. Complications from PAAG injections present from months to years following injection and include lumps, pain, asymmetry, and inflammation. Other concerns include breast cancer detection, long-term toxicity of the material, and breast-feeding issues. Although PAAG is difficult to eradicate, surgical drainage and debridement are successful in relieving most symptoms. Post-debridement reconstruction is primarily reported with prostheses. We present a case using autologous free flap reconstruction to be a potentially successful form of reconstruction.
Footnotes
Authors’ Note
This material has not been published previously and will not be submitted for publication elsewhere.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
