Abstract
Background:
Generalized pustular psoriasis (GPP) is a rare, severe neutrophilic skin disease with significant unmet clinical need. Historically, GPP has not been well characterized; however, the advent of the International Classification of Diseases, 10th revision, has made it possible to more accurately characterize patients with GPP.
Objective:
To describe the characteristics and estimate the burden of disease in patients with GPP compared with those with plaque psoriasis.
Methods:
A retrospective study was conducted using a US administrative claims database, Optum® Clinformatics® Data Mart, between October 1, 2015, and March 31, 2019. Patients with at least 1 inpatient or 2 outpatient diagnosis codes for GPP (L40.1) or psoriasis vulgaris (L40.0) were included. The main outcome measures included the percentage of individuals with comorbidities, medication use, and healthcare resource utilization (HCRU), which were compared between patients with GPP and those with plaque psoriasis and a general population comparator control cohort.
Results:
Overall, 1,669 patients with GPP were identified at baseline; most patients were female (67.6%). Patients with GPP had more comorbidities than those with plaque psoriasis, specifically metabolic disorders: hyperlipidemia and type 2 diabetes. Medication use for patients with GPP differed from those with plaque psoriasis—patients with GPP required more frequent use of antihypertensives and antibiotics than those with plaque psoriasis. Patients with GPP also had higher HCRU than those with plaque psoriasis.
Conclusion:
Although this study has limitations, it shows that patients with GPP have a high burden of illness that differs from patients with plaque psoriasis.
Keywords
Introduction
Generalized pustular psoriasis (GPP) is a rare, potentially life-threatening disease characterized by relapsing or remittent flares of generalized erythematous skin with multiple sterile pustules. 1,2 Although GPP is clinically distinct from plaque psoriasis, the diagnosis of patients with GPP includes an evaluation of the presence or absence of plaque psoriasis. 3 Mutations in the IL36RN, CARD14, and AP1S3 genes are associated with an increased risk of GPP; variants of these genes are present in almost 50% of patients with GPP and may contribute to an earlier age of onset and more severe disease. 4 -6 Serious complications associated with GPP include sepsis, acute renal failure, congestive heart failure, and acute respiratory distress syndrome, 2 and comorbidities include metabolic, cardiac, and neurologic disorders. 7 Reported mortality rates range from 2% to 16%. 7 -10
There are currently no approved treatments for GPP in the USA or Europe and management guidelines (developed based on limited evidence) recommend a wide variety of treatments. These include immunosuppressants, such as cyclosporine and methotrexate; immunomodulators; systemic corticosteroids; and retinoids (such as etretinate). Other treatments include tumor necrosis factor (TNF) inhibitors (adalimumab, infliximab, and etanercept), other biologics, and psoralen plus ultraviolet A. 11 -13 The lack of well-controlled clinical trial efficacy data to guide treatment choices, and the need for effective long-term maintenance to prevent flares of GPP, highlight an unmet need in this patient population. 14 Some therapies are associated with toxicities that may limit their use for long-term disease control. 11 -14
There are few published data on the clinical characteristics of patients with GPP and there are currently no validated algorithms to identify cases of GPP or plaque psoriasis in claims databases, however, the advent of the International Classification of Diseases, 10th revision (ICD-10), in 2015, recognizing GPP as a distinct disorder with its own diagnosis code, has made it possible to characterize patients with GPP more accurately. Two independent studies were conducted using the Optum® Clinformatics® Data Mart and the IBM® MarketScan® Database, 15 characterizing the clinical profile and healthcare resource utilization (HCRU) of patients with GPP compared with those with plaque psoriasis and a US general population matched cohort, in a real-world setting. Here, we report the findings of the Optum® study, the results of which will help to better describe the burden of illness in patients with GPP.
Methods
This study utilized the administrative health insurance claims database Optum® Clinformatics® Data Mart between October 1, 2015 and March 31, 2019. Using ICD-10 diagnosis codes (Table S1), Current Procedural Terminology (CPT) (v4) and Healthcare Common Procedure Coding System (HCPCS) codes, diagnosis codes for comorbidities and diagnostic claims during inpatient, outpatient, and emergency department (ED) visits were identified. For inpatient hospitalizations, only patients with CPT and HCPCS J (respiratory) codes were identified for inclusion. Pharmacy and medical claims were used to identify medication use for the treatment of GPP and comorbidities. Site of service and provider specialty codes were used to identify clinical care visits and estimate HCRU.
Both new and existing patients with GPP or plaque psoriasis were identified based on at least 1 inpatient claim or 2 outpatient claims with an ICD-10 code of L40.1 or L40.0 (Table S2), respectively, separated by 30 days but within 365 days of one another, in line with standard criteria for identifying patients in claims databases. The date of the first qualifying diagnostic claim was used as the index date (first inpatient or second outpatient) to provide greater sensitivity (Figure S1). Three cohorts were evaluated in this study: patients with GPP, patients with plaque psoriasis, and a general population cohort matched to the GPP cohort. Patients with concurrent GPP and palmoplantar pustulosis (PPP) diagnosis codes were excluded from the cohort of patients with plaque psoriasis; however, patients with GPP and concurrent plaque psoriasis and/or PPP were not excluded from the GPP cohort. A comparator, general population, control cohort, without a diagnosis of psoriasis (according to ICD-10 codes: L40.0, L40.2, L40.4, L40.8, or L40.9), GPP (L40.1), or PPP (L40.3) (those with psoriatic arthritis [L40.5] were permitted) was also analyzed and matched 4:1 according to age category (<18 years, 18–64 years, and ≥65 years) and sex to those with GPP. For all ICD-10 codes and medications, see Supplementary Tables S1 and S2. Lower and upper age limits were not applied.
Patients must have had at least 12 months (365 days) of continuous enrollment to be included in the 12-month follow-up analyses. All analyses were conducted using the Aetion Evidence Platform®, v3.11, a scientifically validated analytic platform. 16 Data were analyzed using descriptive statistics, including the mean and standard deviation for normally distributed continuous variables, median and quartiles for skewed continuous variables, and frequencies and percentages for categorical variables. For HCRU analyses, all-cause visits were included.
Results
Patient Population and Demographics at Baseline
A total of 1,669 patients with GPP, 60,419 with plaque psoriasis, and 6,676 in the matched cohort were identified at baseline;1,014 patients with GPP, 32,665 with plaque psoriasis (Figure S2), and 4,130 in the matched cohort were included in the 12-month follow-up analysis. The majority of patients with GPP were female (67.6%) with a mean age of 63.9 years compared with patients with plaque psoriasis, where 50.7% were female and the mean age was 56.4 years (Table 1). More patients with GPP were ≥65 years of age (54.7%) compared with those with plaque psoriasis (35.8%) (Table 1).
Baseline Patient Characteristics.
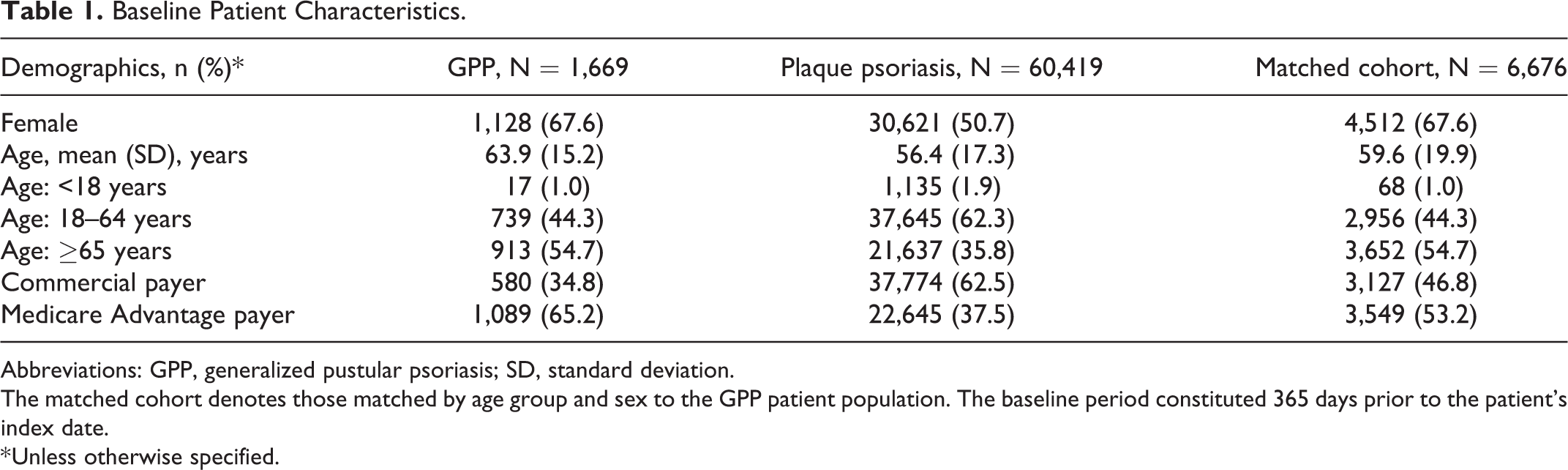
Abbreviations: GPP, generalized pustular psoriasis; SD, standard deviation.
The matched cohort denotes those matched by age group and sex to the GPP patient population. The baseline period constituted 365 days prior to the patient’s index date.
* Unless otherwise specified.
Comorbidities at Baseline
At baseline, patients with GPP were diagnosed with more comorbidities than those with plaque psoriasis and the matched cohort, specifically hyperlipidemia (39.6% vs 25.0% and 24.2%, respectively) and type 2 diabetes (36.1% vs 15.4% and 13.9%) (Figure 1). Other comorbidities included obesity, chronic obstructive pulmonary disease (COPD), and asthma (Figure 1). More patients with GPP had anxiety (11.6%) and depression (10.7%) compared with the plaque psoriasis and matched cohorts (6.7% and 5.8%; 5.5% and 5.0%, respectively) (Figure 1). The prevalence of certain cardiovascular conditions was also measured and were similar between the GPP and plaque psoriasis and matched cohorts; these included myocardial infarction (0.7%, 0.2%, and 0.3%, respectively) and stroke (1.2%, 0.5% and 0.8%, respectively).
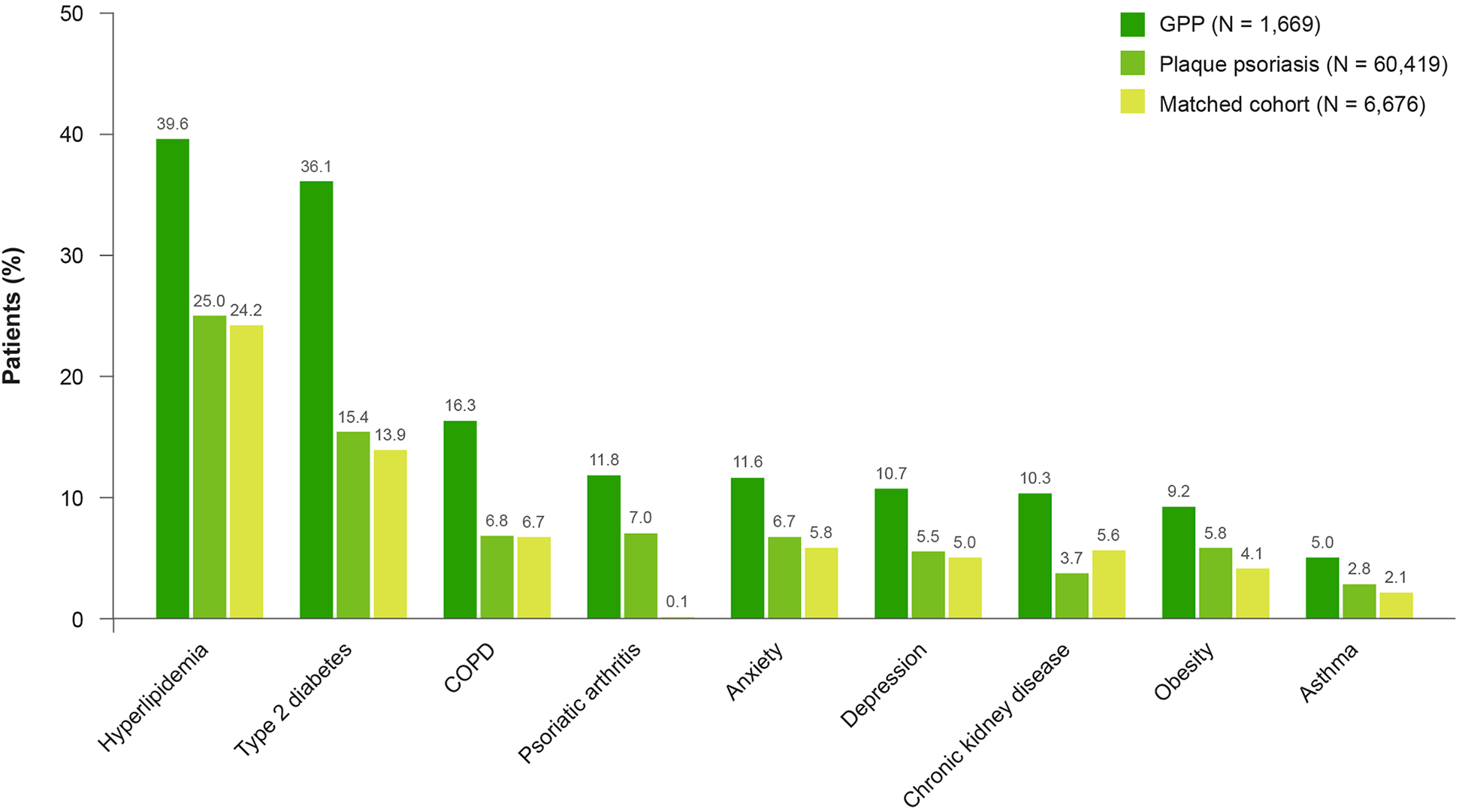
Proportion of patients with comorbidities at baseline. Patients could have multiple comorbidities. Data are not mutually exclusive. COPD, chronic obstructive pulmonary disease; GPP, generalized pustular psoriasis.
Concomitant Medication Use During the 12 Month Follow-Up
On average, patients with GPP received more treatments during the 12-month follow-up period than those with plaque psoriasis. These included treatments for hypertension; metabolic conditions, such as type 2 diabetes and hyperlipidemia; and respiratory conditions, such as COPD and asthma. Antihypertensives were the most frequently dispensed medication among patients with GPP (Table 2). The percent of patients receiving prescriptions for antibiotics was similar between the GPP and plaque psoriasis cohorts, but lower in the matched cohort (Table 2).
Most Common Concomitant Treatments During the 12-Month Follow-Up.
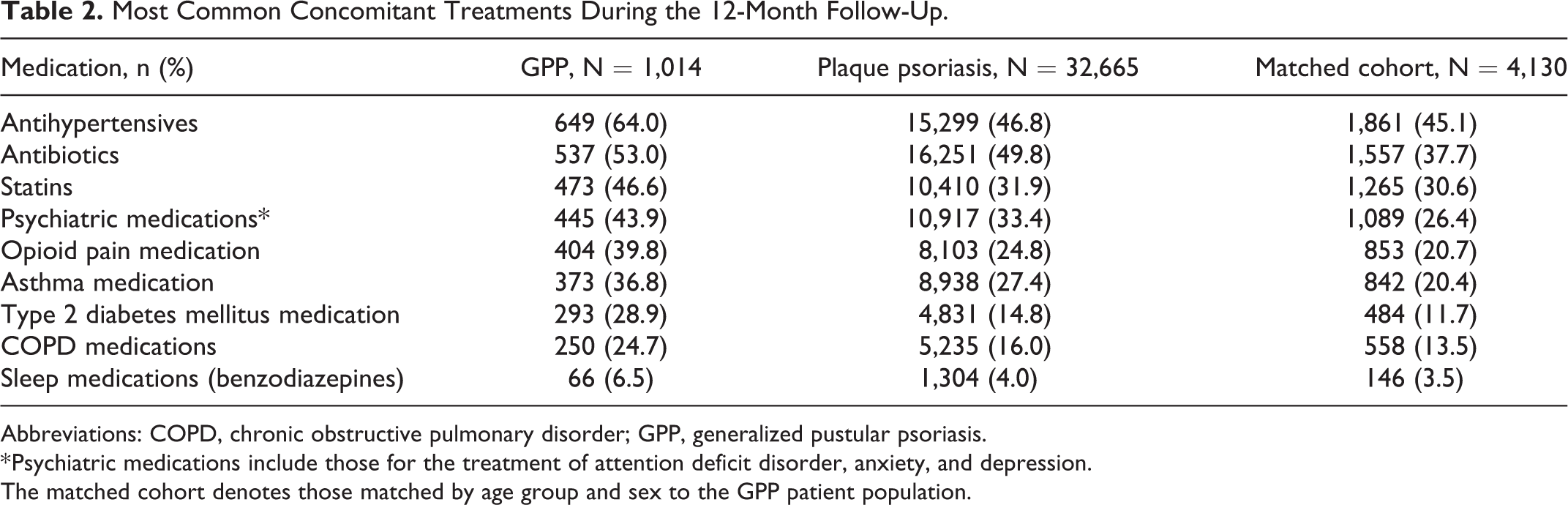
Abbreviations: COPD, chronic obstructive pulmonary disorder; GPP, generalized pustular psoriasis.
* Psychiatric medications include those for the treatment of attention deficit disorder, anxiety, and depression.
The matched cohort denotes those matched by age group and sex to the GPP patient population.
A higher proportion of patients with GPP (39.8%) were prescribed opioid pain medication than patients with plaque psoriasis or those in the matched cohort (24.8% and 20.7%, respectively) (Tables 2 and S3).
Dermatologic Medication Usage in GPP and Plaque Psoriasis During the 12-Month Follow-Up
During the 12-month follow-up, a lower proportion of patients with GPP were treated with biologic monotherapy than those with plaque psoriasis (5.0% vs 9.6%, respectively); however, a higher proportion of patients with GPP received non-biologic systemic monotherapy than those with plaque psoriasis (15.0% vs 7.2%) (Table S4). Fewer patients with GPP were also treated with a prescription topical medication alone than patients with plaque psoriasis (14.4% vs 24.5%) (Table S4).
Fewer patients with GPP were treated with TNF inhibitors and interleukin inhibitors compared with patients with plaque psoriasis (Figure 2). In both cohorts, adalimumab was the most prescribed TNF inhibitor (6.7% and 11.2%, respectively), and ustekinumab was the most prescribed interleukin inhibitor (4.8% and 9.6%). Abatacept (a T-cell inhibitor) was prescribed for few patients in both cohorts (≤0.1%). Of the non-biologic systemic therapies, methotrexate was the most used therapy in both patients with GPP and those with plaque psoriasis (Figure 2).
Of the 449 patients with GPP who received systemic therapies, a lower percentage of patients with GPP (54.6%) received combination therapies compared with patients with plaque psoriasis (67.4%) (Table S4). Compared with plaque psoriasis, fewer patients with GPP received combination therapies comprising a topical medication with a biologic systemic treatment (3.5% [n = 35] vs 7.9% [n = 2,586]), and a topical medication with a non-biologic systemic treatment (12.4% [n = 126] vs 17.4% [n = 5,689]) (Table S4). A similar proportion of patients received combination treatment with a biologic and non-biologic therapy for GPP (3.0% [n = 30]) and plaque psoriasis (3.5% [n = 1,157]). The percent of patients with GPP or plaque psoriasis who received a combination of topical treatment, non-biologic treatment, and biologic treatment was also similar (5.3% [n = 54] vs 5.9% [n = 1,933], respectively) (Table S4; see Table S5 for included therapies).
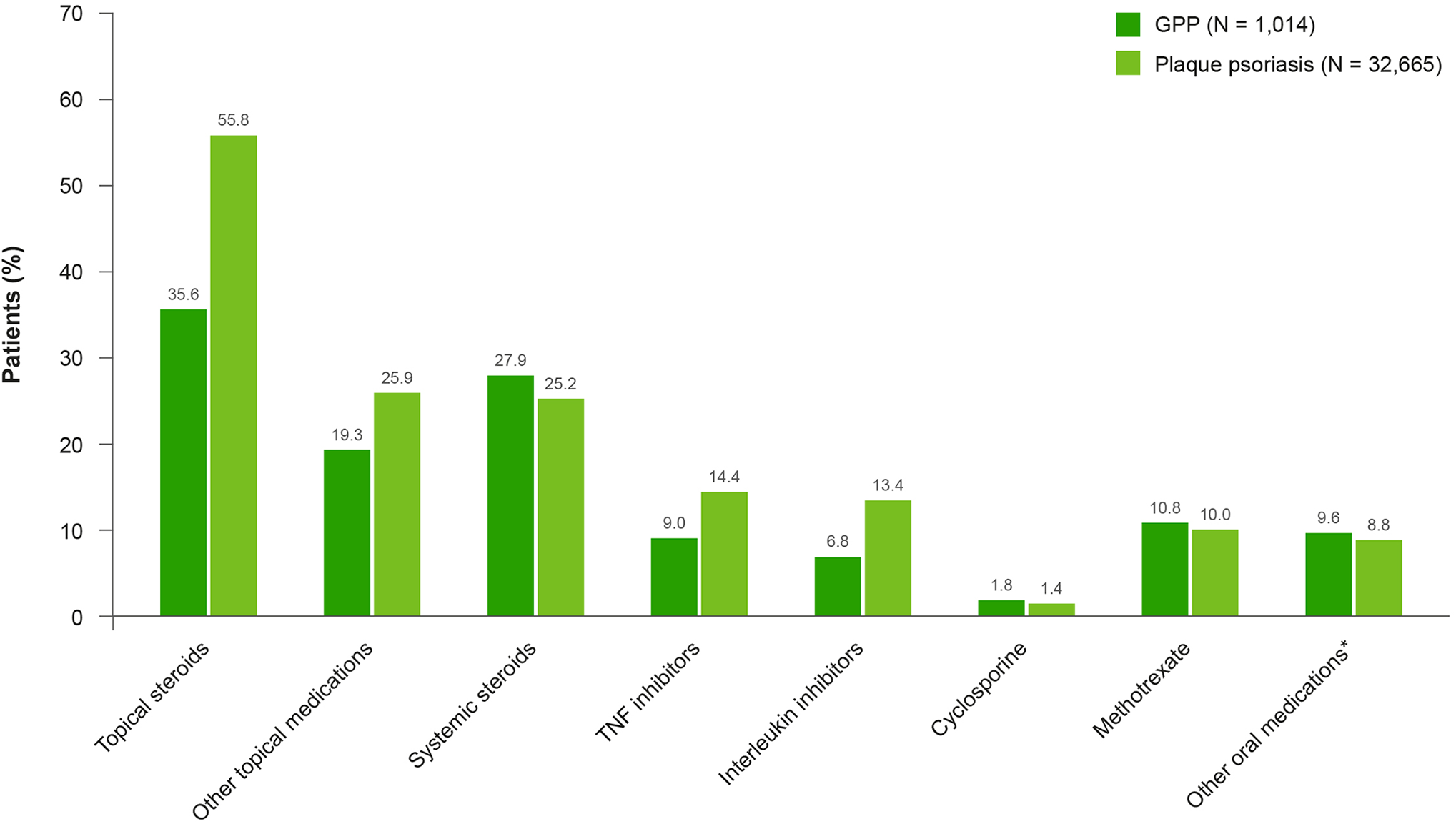
Medication use by class during the 12-month follow-up. Data are not mutually exclusive. “Systemic steroids” represents a class of medication rather than one specific systemic steroid. *Other oral medication includes 6-thioguanine, apremilast, hydroxyurea, mycophenolate mofetil, sulfasalazine, and tacrolimus. GPP, generalized pustular psoriasis; TNF, tumor necrosis factor.
Medication Usage by Age
Of the patients with GPP aged ≥65 years, 54.1% received no treatment compared with 33.4% of those aged ≥65 years with plaque psoriasis. The percentage of patients with GPP or plaque psoriasis who received biologic monotherapy was low (1.7% vs 3.1%, respectively), of which adalimumab was the most frequently prescribed biologic (2.6% vs 4.0%, respectively). More patients with GPP received non-biologic systemic treatment (16.2%) compared with those with plaque psoriasis (6.8%) (Table S4).
In contrast, among patients <65 years, 24.1% of patients with GPP received no treatment, compared with 17.3% of patients with plaque psoriasis. Patients with GPP or plaque psoriasis <65 years were more likely to receive biologic treatment compared with those ≥65 years, and adalimumab was the most commonly prescribed biologic in both those with GPP and those with plaque psoriasis. Patients with GPP were more likely to receive non-biologic monotherapy (13.7%) than those with plaque psoriasis (7.5%).
All-Cause HCRU During the 12-Month Follow-Up
Patients with GPP had more all-cause outpatient visits compared with the plaque psoriasis cohort and the matched cohort (Table 3). Patients with GPP had the same median number of all-cause inpatient visits as the plaque psoriasis and matched cohorts (Table 3). Despite this, a higher proportion of patients with GPP had an in patient visit (all-cause) than both the plaque psoriasis and matched cohorts. The median duration of the inpatient stays was also longer for patients with GPP than for those in the plaque psoriasis and matched cohorts (Table 3). The most common reasons for inpatient hospitalizations were complications from sepsis (ICD-10 code: A41; “other sepsis”) (12.3%) and COPD (ICD-10 code: J44; “other COPD”) (7.9%) (Table S6). The sepsis code A41 was also the most common reason for inpatient stays for patients with plaque psoriasis, although the proportion of patients who had an inpatient stay was lower (8.4%) than in the GPP cohort.
A higher proportion of patients with GPP had ED visits, and visited the ED more frequently, than those in the plaque psoriasis and matched cohorts (Table 3).
Overall All-Cause HCRU During the 12-Month Follow-Up.
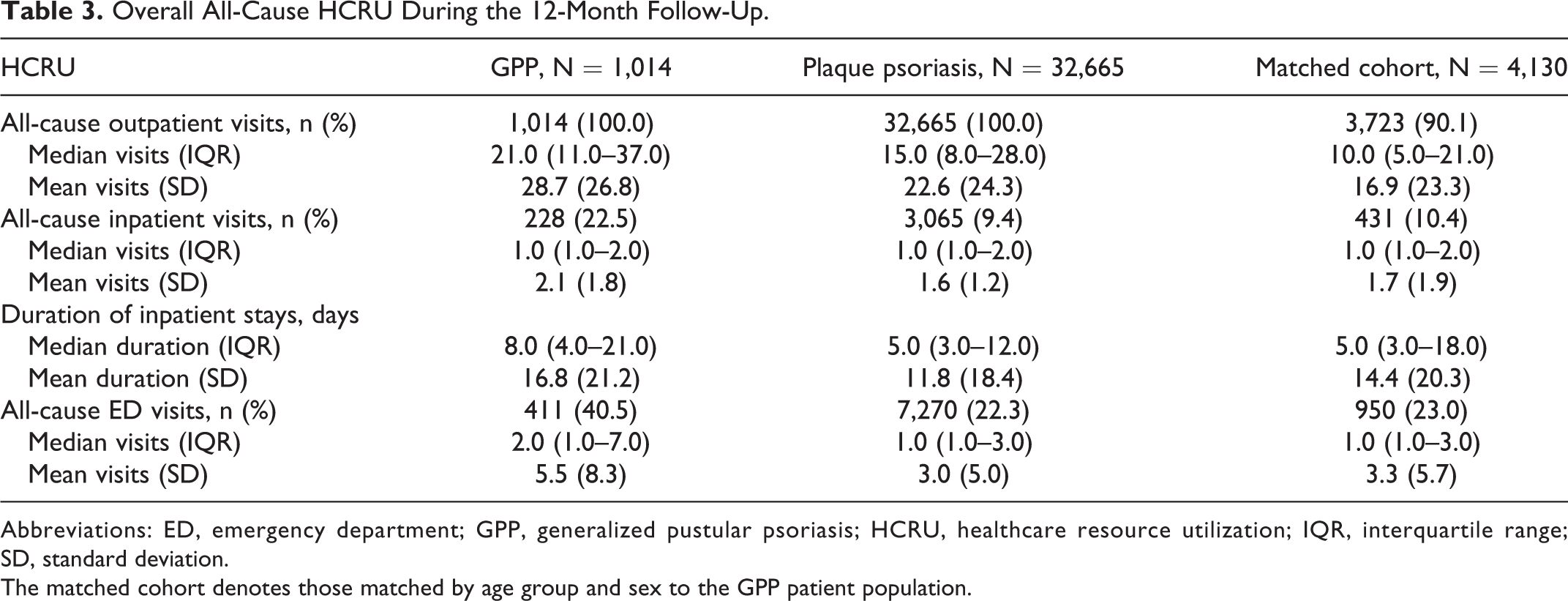

Abbreviations: ED, emergency department; GPP, generalized pustular psoriasis; HCRU, healthcare resource utilization; IQR, interquartile range; SD, standard deviation.
The matched cohort denotes those matched by age group and sex to the GPP patient population.
The specialties of physicians who treated those with GPP and those with plaque psoriasis, respectively, are shown in Table S7.
Discussion
This study describes the clinical characteristics of over 1,000 patients with GPP using real-world data obtained from one of the largest US claims databases, Optum® Clinformatics® Data Mart, which includes approximately 100 million people. The increased prevalence of GPP in women compared with men identified in this study is consistent with a similar study conducted using data from the IBM® MarketScan® claims database. 15 In this Optum® study patients with GPP experienced a higher prevalence of all measured comorbidities compared with the plaque psoriasis and matched control cohorts; the most prevalent of these comorbidities in both GPP and plaque psoriasis cohorts were hyperlipidemia and type 2 diabetes. The prevalence of both hyperlipidemia and type 2 diabetes, as well as other comorbidities, in the plaque psoriasis cohort is in line with previous database studies of patients with plaque psoriasis. 17 -19 Systemic inflammation, as seen with plaque psoriasis and GPP, is associated with the development of insulin resistance in some patients, which can result in comorbid type 2 diabetes. 20 Both type 2 diabetes and hyperlipidemia can also be risk factors for the development of cardiovascular disease (CVD). In contrast to previous reports, this study did not find that patients with GPP or plaque psoriasis had a higher prevalence of CVD compared with the matched cohort 18,19 ; this could be because CVD would typically take a longer period of time to manifest after the initial diagnosis of type 2 diabetes or hyperlipidemia than the duration of the study. In addition, increased risk of CVD has been associated with obesity, a known comorbidity of GPP that is also associated with hypertension and type 2 diabetes. 3,21 Although a diagnosis of obesity was reported in a higher proportion of patients with GPP compared with those with plaque psoriasis, the Optum® database does not allow for overall body mass index analysis. The use of antihypertensives in patients with GPP in this study suggests that hypertension is more prevalent in those with GPP compared with those with plaque psoriasis, which may increase the risk of cardiovascular and renal complications developing in these patients. Another plausible explanation for higher prevalence of comorbid hypertension in patients with GPP would be their older average age compared with those with plaque psoriasis, and therefore it may not be directly attributable to GPP.
The greater prevalence of anxiety and depression in the GPP cohort suggests that these patients experienced a greater emotional burden compared with the plaque psoriasis and matched cohorts; this indicates that the management of patients with GPP may require a multidisciplinary approach to address both the psychological and physical manifestations of the disease.
Given the higher occurrence of comorbidities in patients with GPP, it is not surprising that these patients had an increased medication burden compared with those with plaque psoriasis. However, it is not possible to determine the reason for prescribing medications in this study. The increased use of opioid pain medication in the GPP cohort (almost twice that of the plaque psoriasis cohort) suggests that patients with GPP are more likely to experience severe pain than those with plaque psoriasis. One explanation for the increased use of opioids in patients with GPP could be the presence of systemic symptoms, which can cause significant pain-and/or inflammation-induced joint pain.
GPP skin pustules may explain the high use of antibiotics in patients with GPP, who may require treatment for pustule infection, which can lead to sepsis if left untreated (a common complication of GPP). 2 Lung infections related to COPD and/or asthma, which had a greater prevalence in the GPP cohort compared with the plaque psoriasis cohort, may also explain the increased antibiotic use in the GPP cohort. However, these data do not identify the proportion of patients experiencing stable or residual disease, nor do they include measures of disease severity, and diagnosis codes were not linked to prescriptions, therefore, the exact reasons for high opioid and antibiotic medication use in this heterogeneous population of patients with GPP remains unknown.
There are reports that some medications (e.g. systemic steroids) can either exacerbate the symptoms or trigger flares of GPP. 7, 22, 23 Despite being associated with disease worsening, systemic steroids as a class of medication were among the highest prescribed medications for both the GPP and plaque psoriasis cohorts in this study. However, it was not possible to ascertain whether the use of systemic steroids lead to worsening of GPP.
A smaller proportion of patients with GPP were treated with topical medications than patients with plaque psoriasis; however, a greater proportion of patients with GPP required combination therapies of both systemic and topical medications, suggesting that the severity of disease in patients with GPP often cannot be managed by topical medications alone. Overall, the proportion of patients with GPP or plaque psoriasis receiving systemic therapies were similar (70% versus 60% in patients with plaque psoriasis), suggesting that both cohorts had similar levels of disease severity. Generally, patients ≥65 years of age received systemic therapies less frequently than those <65 years; this may be because physicians are reluctant to treat older patients with immunosuppressive biologic medications because they are more likely to be immunocompromised than younger patients, increasing their risk of infection. The risk of complications from systemic treatments may, therefore, impact the treatment options for disease and associated comorbid conditions in both plaque psoriasis and GPP; this could explain why some older patients were treated with topical therapies only, even though they are less effective than other treatment options. Older patients may also receive different therapies to younger patients due to differences in access to treatment.
Notably, a smaller proportion of patients with GPP in the Optum® database received TNF inhibitors and interleukin inhibitors compared with those with GPP in the IBM® MarketScan® database 15 ; this may be influenced by the nature of prescription drug coverage in the Optum® database, which includes a larger proportion of Medicare Advantage patients than the MarketScan® database. 15 Medicare patients also have limited access to biologics due to the high copayments required in Medicare Part D. Overall, the proportion of patients with a filled prescription fora biologic was lower in the Optum® database than those with plaque psoriasis compared with those enrolled in the MarketScan® database, in which patients with GPP were equally likely to receive biologics as those with plaque psoriasis. 15 The overall incidence of all-cause hospitalization in patients with GPP highlights that the complications experienced by this patient population could be more extensive and/or severe than in those with plaque psoriasis.
The limitations of this study include that the Optum® database only includes individuals from a single insurance provider and also includes Medicare Advantage patients, who have limited coverage for certain medications, for example, biologics; as such, the overall use of biologics in this study may not be representative of the commercially insured population in the USA. As these data are from an administrative claims database, there may be incomplete records for individuals. Further, patients added to the database prior to the implementation of the GPP-specific ICD-10 code may not have been included in this analysis due to the lack of an appropriate diagnosis code in the ICD-9 system. Additionally, patients with GPP seen in private practices may not have been captured by the newer ICD-10 codes, as ICD-10 coding may not have been utilized consistently. These results may not fully reflect the US population with GPP as a whole since many US individuals are uninsured and therefore would not be captured in this, or any other claims-based, database. The lack of a validation algorithm with positive predictive value to accurately identify patients with GPP, as well as a lack of consensus on the diagnostic criteria for a diagnosis of GPP specifically, also presents a limitation in studies of this kind; however, the stratification used in this study was based on standard procedures for retrospective claims database studies.
As these data are from an administrative claims database, there may be incomplete records for individuals, additionally, these data were collected for reimbursement purposes rather than scientific research; thus, there may be miscoding and over-/under-reporting of some comorbid conditions. In addition, medications being used by patients self-managing their symptoms such as over-the-counter medications (e.g. analgesics for pain relief) are not reflected in this database. Consequently, medications for symptom management may by under-represented, reflecting another potential bias. This is confounded by the lack of information about medications received by patients in hospital settings. Data on disease severity were not evaluated in this study because the Optum® database does not include information relating to specific measures of psoriasis such as the Psoriasis Area and Severity Index or the body surface area affected by GPP. With regard to disease severity, it is difficult to determine whether patients with milder disease may have diluted the prevalence of comorbidities, particularly in the plaque psoriasis cohort. Despite this, the proportion of patients receiving systemic therapies was more than 50% in both the GPP (approximately 70%) and plaque psoriasis (approximately 60%) cohorts, indicating that the majority of patients in both cohorts may have been experiencing moderate-to-severe disease, suggesting that the two cohorts are comparable. Indeed, the use of systemic therapy was used as a marker for severe disease in patients with plaque psoriasis in a previous study. 24
Despite these limitations, the data on treatments are generally considered to be robust and reflect what the patient received at the pharmacy. The results of this study provide detailed clinical characterization of patients with GPP, and the introduction of separate ICD-10 codes for GPP and plaque psoriasis has allowed a better understanding of the similarities and differences in the burden of illness and HCRU between these 2 populations.
In conclusion, the data presented here demonstrate that patients with GPP experience a higher burden of disease and HCRU than patients with plaque psoriasis and a matched cohort. A strength of the Optum® database is the inclusion of Medicare Advantage patients, which has shown that treatments received by patients ≥65 years differ to those received by patients <65 years, potentially reflecting the different provision of healthcare and the complexity of managing a highly comorbid elderly patient population. Together, the findings from this study are consistent with those from a similar study, and demonstrate an overview of the current clinical profile of patients with GPP, of all ages, in the USA. 15 Further understanding of the differences between patients with GPP and those with plaque psoriasis should encourage the development of specific treatments and management practices for patients with GPP to help alleviate their burden of illness.
Supplemental Material
Supplemental Material, sj-pdf-1-jps-10.1177_24755303211021786 - Clinical Characteristics and HealthCare Resource Utilization in Patients With Generalized Pustular Psoriasis: Real-World Evidence From a Large Claims-Based Dataset
Supplemental Material, sj-pdf-1-jps-10.1177_24755303211021786 for Clinical Characteristics and HealthCare Resource Utilization in Patients With Generalized Pustular Psoriasis: Real-World Evidence From a Large Claims-Based Dataset by Jeffrey Crowley, Amanda K. Golembesky, Nirali Kotowsky, Ran Gao, Rhonda L. Bohn, Elizabeth M. Garry, Julia A. Pisc, Wendell C. Valdecantos, Steven R. Feldman and Alan Menter in Journal of Psoriasis and Psoriatic Arthritis
Supplemental Material
Supplemental Material, sj-pdf-2-jps-10.1177_24755303211021786 - Clinical Characteristics and HealthCare Resource Utilization in Patients With Generalized Pustular Psoriasis: Real-World Evidence From a Large Claims-Based Dataset
Supplemental Material, sj-pdf-2-jps-10.1177_24755303211021786 for Clinical Characteristics and HealthCare Resource Utilization in Patients With Generalized Pustular Psoriasis: Real-World Evidence From a Large Claims-Based Dataset by Jeffrey Crowley, Amanda K. Golembesky, Nirali Kotowsky, Ran Gao, Rhonda L. Bohn, Elizabeth M. Garry, Julia A. Pisc, Wendell C. Valdecantos, Steven R. Feldman and Alan Menter in Journal of Psoriasis and Psoriatic Arthritis
Supplemental Material
Supplemental Material, sj-pdf-3-jps-10.1177_24755303211021786 - Clinical Characteristics and HealthCare Resource Utilization in Patients With Generalized Pustular Psoriasis: Real-World Evidence From a Large Claims-Based Dataset
Supplemental Material, sj-pdf-3-jps-10.1177_24755303211021786 for Clinical Characteristics and HealthCare Resource Utilization in Patients With Generalized Pustular Psoriasis: Real-World Evidence From a Large Claims-Based Dataset by Jeffrey Crowley, Amanda K. Golembesky, Nirali Kotowsky, Ran Gao, Rhonda L. Bohn, Elizabeth M. Garry, Julia A. Pisc, Wendell C. Valdecantos, Steven R. Feldman and Alan Menter in Journal of Psoriasis and Psoriatic Arthritis
Footnotes
Authors’ Note
To ensure independent interpretation of clinical study results, Boehringer Ingelheim grants all external authors access to summarized results and other relevant material as needed by them to fulfill their role and obligations as authors under the International Committee of Medical Journal Editors (ICMJE) criteria. Furthermore, clinical study documents (e.g. the study report, study protocol and statistical analysis plan) and participant clinical study data are available to be shared after publication of the primary manuscript in a peer-reviewed journal and if regulatory activities are complete and other criteria met as per the Boehringer Ingelheim policy on transparency and publication of clinical study data (see ![]() ). Prior to providing access, documents will be examined, and, if necessary, redacted and the data will be de-identified, to protect the personal data of study participants and personnel, and to respect the boundaries of the informed consent of the study participants. Clinical study reports and related clinical documents can also be requested via the link https://trials.boehringer-ingelheim.com/. All requests will be governed by a document sharing agreement. Bona fide, qualified scientific and medical researchers may request access to de-identified, analyzable participant clinical study data with corresponding documentation describing the structure and content of the datasets. Upon approval, and governed by a data sharing agreement, data are shared in a secured data-access system for a limited period of 1 year, which may be extended upon request. Researchers should use the https://trials.boehringer-ingelheim.com/ link to request access to study data.
). Prior to providing access, documents will be examined, and, if necessary, redacted and the data will be de-identified, to protect the personal data of study participants and personnel, and to respect the boundaries of the informed consent of the study participants. Clinical study reports and related clinical documents can also be requested via the link https://trials.boehringer-ingelheim.com/. All requests will be governed by a document sharing agreement. Bona fide, qualified scientific and medical researchers may request access to de-identified, analyzable participant clinical study data with corresponding documentation describing the structure and content of the datasets. Upon approval, and governed by a data sharing agreement, data are shared in a secured data-access system for a limited period of 1 year, which may be extended upon request. Researchers should use the https://trials.boehringer-ingelheim.com/ link to request access to study data.
Acknowledgments
This study was funded by Boehringer Ingelheim. Editorial and writing assistance in the preparation of this manuscript was provided by Amy Pashler, PhD and Leigh Church, PhD of OPEN Health Communications (London, UK) and funded by Boehringer Ingelheim. The listed authors have authorized the submission of their manuscript via third party and approved any statements or declarations. In addition, we wish to acknowledge Emma Payne and Jocelyn R. Wang for implementation support using the Aetion Evidence Platform.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: J Crowley is a Consultant, Speaker, Investigator for: AbbVie, Amgen, Boehringer Ingelheim, Bristol Myers Squibb, Novartis, Lilly, MC-2, Merck, Pfizer, Regeneron, Sanofi-Aventis, Sun Pharma, UCB, and Verrica. AK Golembesky was an employee of Boehringer Ingelheim during the implementation of this study and is now employed by GlaxoSmithKline. RL Bohn is the Owner and Principal of Bohn Epidemiology, LLC. EM Garry is a full-time employee of Aetion, Inc., of which she has stock options. JA Pisc was a full-time employee of Aetion, Inc., during the implementation of this study and has equity. SR Feldman received research, speaking, and/or consulting support from Galderma, Almirall, Alvotech, Leo Pharma, BMS, Boehringer Ingelheim, Mylan, Celgene, Pfizer, Ortho Dermatologics, AbbVie, Samsung, Janssen, Lilly, Menlo Therapeutics, Merck, Novartis, Amgen, Helsinn, Arena, Regeneron, Sanofi, Novan, Qurient, National Biological Corporation, Caremark, Advance Medical, Sun Pharma, Suncare Research, Informa, UpToDate, and National Psoriasis Foundation. SR Feldman is founder and majority owner of ![]() and founder and part owner of Causa Research. A Menter reports being on the advisory board and a consultant, investigator, and speaker for, and receiving grants and honoraria from Abbot Labs, Amgen, Janssen Biotech, Inc., and LEO Pharma; being on the advisory board and an investigator for, and receiving grants and honoraria from Boehringer Ingelheim; being a consultant, investigator, and speaker for, and receiving grants and/or honoraria from Sun Pharma and UCB; being a consultant and investigator for, and receiving honoraria from Novartis and Eli Lilly; and being an investigator for and receiving grants from Celgene and Merck. R Gao, N Kotowsky, and WC Valdecantos are employees of Boehringer Ingelheim.
and founder and part owner of Causa Research. A Menter reports being on the advisory board and a consultant, investigator, and speaker for, and receiving grants and honoraria from Abbot Labs, Amgen, Janssen Biotech, Inc., and LEO Pharma; being on the advisory board and an investigator for, and receiving grants and honoraria from Boehringer Ingelheim; being a consultant, investigator, and speaker for, and receiving grants and/or honoraria from Sun Pharma and UCB; being a consultant and investigator for, and receiving honoraria from Novartis and Eli Lilly; and being an investigator for and receiving grants from Celgene and Merck. R Gao, N Kotowsky, and WC Valdecantos are employees of Boehringer Ingelheim.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Boehringer Ingelheim sponsored this study and provided funding for the conduct, data analysis, and medical writing assistance for the study’s publication.
Supplemental Material
Supplemental material for this article is available online.
Abbreviations
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
