Abstract

Myositis ossificans (MO) is nonneoplastic heterotopic bone formation within muscle or soft tissues. MO typically presents in the upper arm or thigh following trauma, and occurrence in the head and neck is rare. 1 Nonsurgical treatment with rest and ice is often successful 2 with some literature supporting bisphosphonate therapy. 3 Surgical indications include intractable pain, lesions that compress vital neurovascular structures, and severe functional impairment after failure of conservative management. Surgical debridement is typically curative, and recurrence is not common. 2 However, surgery is not indicated in fibrodysplasia ossificans progressiva (FOP), a rare genetic disease characterized by heterotopic ossification progression within soft tissue. We report a case of a patient with a neck mass that initially revealed nodular fasciitis (NF), which then, after excisional biopsy, was diagnosed as MO. However, after disease progression and treatment failure, FOP was suspected. This article was exempt from approval by the University of Miami investigational review board.
Report of a Case
A 22-year-old African American woman with no pertinent medical history presented to the emergency department with dyspnea and a rapidly enlarging neck mass for one week. Associated symptoms included tenderness, orthopnea, and odynophagia. She denied trauma but endorsed recent chiropractor adjustment to alleviate new-onset neck myalgia. The patient was in no acute distress, breathing comfortably on room air with normal vital signs. Physical examination revealed a tender, firm, nonmobile right neck mass without overlying erythema. Imaging ( Figure 1 ) demonstrated an extensive soft tissue process in the right sternocleidomastoid extending to the visceral space of the neck, carotid space, and posterior triangle, suggestive of intramuscular hematoma causing leftward deviation of the upper trachea and esophagus.
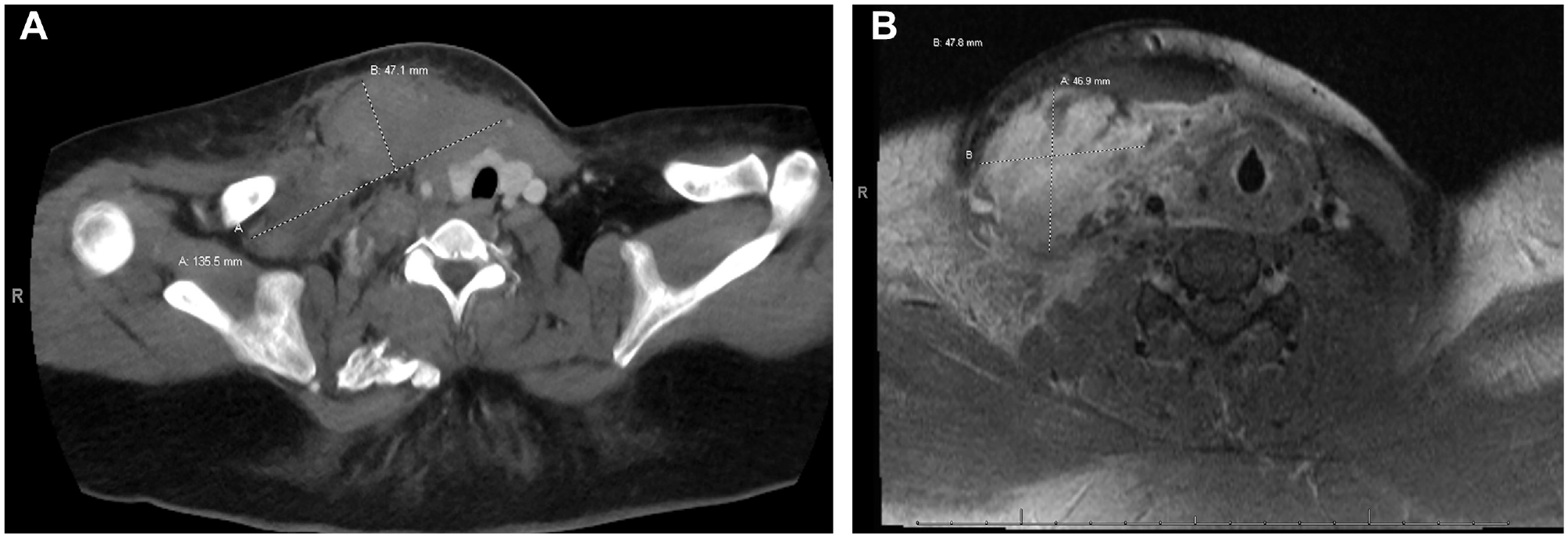
Initial imaging. (a) Computed tomography demonstrated asymmetric density of right sternocleidomastoid muscle concerning for hematoma extending into carotid space, with leftward deviation of trachea. (b) Magnetic resonance imaging demonstrated T2/short tau inversion recovery hyperintense and enhancing mass measuring 9.2 × 4.7 × 4.8 cm with extensive edema.
The patient started steroid therapy and underwent right neck exploration with excisional biopsy. Review of the pathology slides at multidisciplinary head and neck tumor board revealed NF ( Figure 2a ), and the consensus was to offer surgical resection and obtain deeper tissue biopsies. She underwent right neck re-exploration for conservative debulking of the mass given its proximity to the carotid sheath, with injection of intralesional steroids in the remaining mass. Pathologic review of the specimens from the second operation revealed MO ( Figure 2b ).
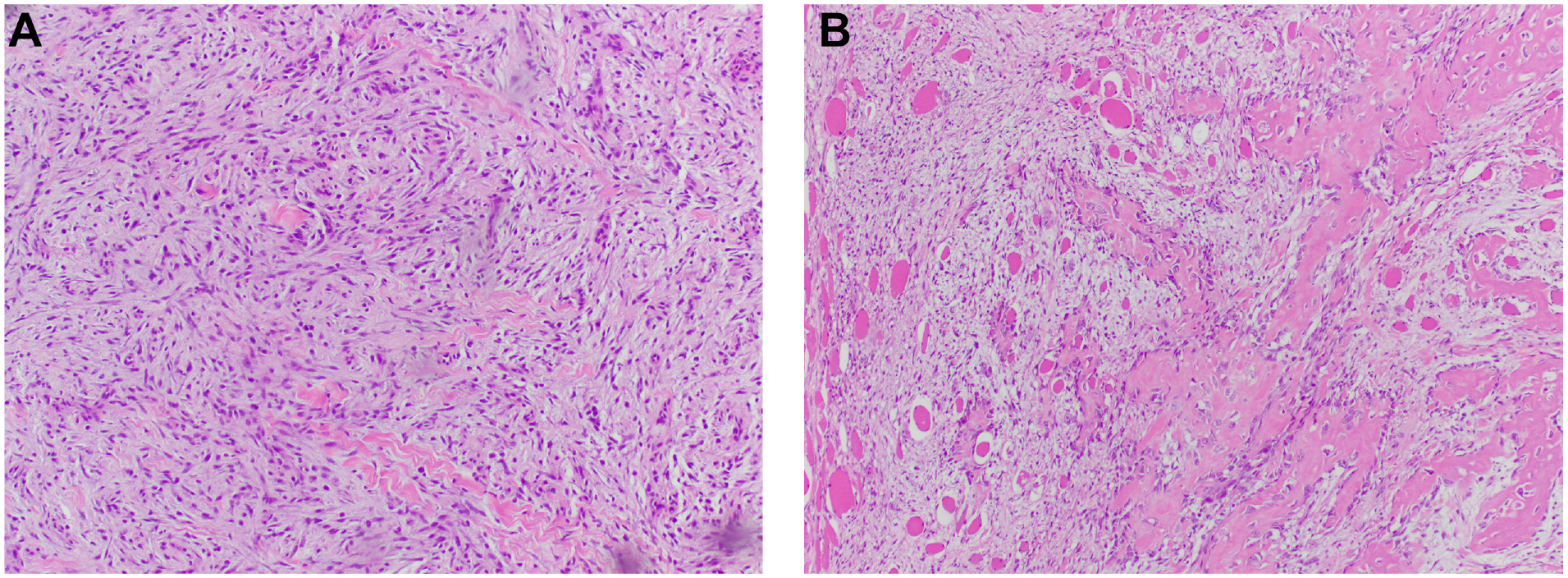
Histopathology (hematoxylin and eosin stain). (a) Initial right neck biopsy. Spindled fibroblasts and myofibroblasts with no high-grade features, consistent with nodular fasciitis. (b) Right neck dissection biopsy. Woven bone with fibroblasts and myofibroblasts with no high-grade features, consistent with myositis ossificans.
Further workup by medical services revealed no associated rheumatologic, infectious, or malignant conditions. The disease progressed over the ensuing months with the development of a similar mass within the left neck soft tissues. An interval computed tomography scan of the neck revealed a lesion of similar soft tissue density in the left sternocleidomastoid muscle, with significant interval increase in heterotopic ossification throughout the previously explored right neck mass. At 6-month follow-up, her symptoms progressed to include near-complete neck immobility, significant trismus, and a diet restricted to softs and liquids. The condition was deemed nonsurgical from the otolaryngology standpoint, and her respiratory status has remained stable without need for tracheostomy. Genetic referral was recommended to evaluate for FOP due to her disease progression and negative medicine workup, which her insurance unfortunately denied.
Discussion
MO is a nonneoplastic, heterotopic ossification within muscle or soft tissues, while NF is a rapidly growing benign self-limited fibroblastic tumor. The spindle component in MO is morphologically identical to NF, which explains the diagnosis made on the initial biopsy. No bone was present in the initial biopsy specimen, nor did the imaging demonstrate bony features in the lesion.
Given the progression and unresponsive nature of this patient’s MO, we referred the patient to genetics for further assessment as her presentation began demonstrating findings suggestive of FOP, a disabling genetic disorder of connective tissue. FOP is characterized by the progression of heterotopic bone within soft tissue and commonly affects the shoulders, neck, and spine, leading to compression of vital structures and restriction of movement resulting in difficulty swallowing, speaking, and breathing. 4 Molecular genetic testing is used to confirm the diagnosis, and congenital skeletal anomalies are common but not necessary for diagnosis. 5 Given the incidence of approximately 1 patient per 2 million people, 4 clinical awareness of FOP is low. Delayed diagnosis increases the risk of unnecessary interventions, such as biopsies, surgical procedures, and intramuscular injections, as these bring about worsening or inevitable recurrence of ossification, as seen in our patient.
