Abstract
Keywords
Syphilis describes a constellation of symptoms caused by colonization with Treponema pallidum, most commonly transmitted through sexual contact. 1 Since reaching a historic low of 2.1 per 100,000 in 2000, incidence of primary and secondary syphilis has increased almost every year, reaching 11.9 per 100,000 in 2019. 2 Given current epidemiologic trends, it is imperative that clinicians remain aware of the various manifestations of syphilis.
The manifestations of syphilis are staged as primary, secondary, or tertiary. Primary syphilis manifests as a chancre at the inoculation site, associated with regional lymphadenopathy. 1 In the head and neck, the chancre of primary syphilis is seen on the lips, tongue, or tonsil, with rare presentation in the nose or larynx. 3 Secondary syphilis occurs 2 to 12 weeks following untreated primary syphilis, presenting in ~25% of patients. 4 Due to hematogenous dissemination, secondary syphilis has extremely variable presentation. Secondary syphilis is associated with symmetric generalized rash involving the entire trunk and extremities, plus palms and soles. 5 Oral lesions of secondary syphilis include elevated plaques with ulceration or coalescent mucous patches rising to serpiginous “snail-track” ulcers. Manifestations of tertiary syphilis include an asymptomatic latent phase, followed by cardiovascular syphilis, neurosyphilis, or gummatous lesions of the liver, bones, and spleen. 1 Otolaryngologic manifestations of tertiary syphilis include gummas of the hard and soft palate.
Despite a recent increase in syphilis, the incidence of head and neck manifestation is still relatively rare. We present a unique case of a male smoker with a persistent oral cavity lesion and cervical lymphadenopathy, which were found to be oral syphilis.
This study is exempt from Bon Secour Mercy Health Institutional Review Board evaluation.
Case Report
An otherwise healthy 27-year-old man with a 1–pack-year smoking history was referred to our clinic for evaluation of a left oral ulcer and neck mass. The patient reported a progressively enlarging left-sided neck mass with a painful ulcerated left lower lip lesion, which were associated with mild dysphagia, sore throat, intermittent tachycardia, and chest pain for the past 4 to 5 months. Clinical examination showed a ~3-cm hard fixed lymph node on the left side (level IIA), bilateral scattered cervical lymphadenopathy, and a 2.5-cm ulcerated lesion over the buccal aspect of the left lateral lower lip ( Figure 1 ). Computed tomography of soft tissue neck with contrast was performed and showed mild hypertrophy of Waldeyer’s ring and bilateral scattered jugulodiagastric chain lymphadenopathy, the largest node present at left level IIA (2.8 × 2.1 × 4.0 cm). In-office incisional biopsies were performed, and histopathologic review was consistent with the diagnosis of syphilis. Further spirochete immunostaining confirmed the diagnosis. The patient was not surprised by this diagnosis, admitted to similar ulcerative painful lesions near his rectum for several months, and had multiple sexual partners with unprotected intercourse. The patient was treated with 1 intramuscular dose of 2.5 million units of penicillin G benzathine. Follow-up at 1 week showed significant improvement of symptoms with resolution of the oral lesion ( Figure 2 ). The patient tolerated therapy without adverse effects and with swift resolution of symptoms.
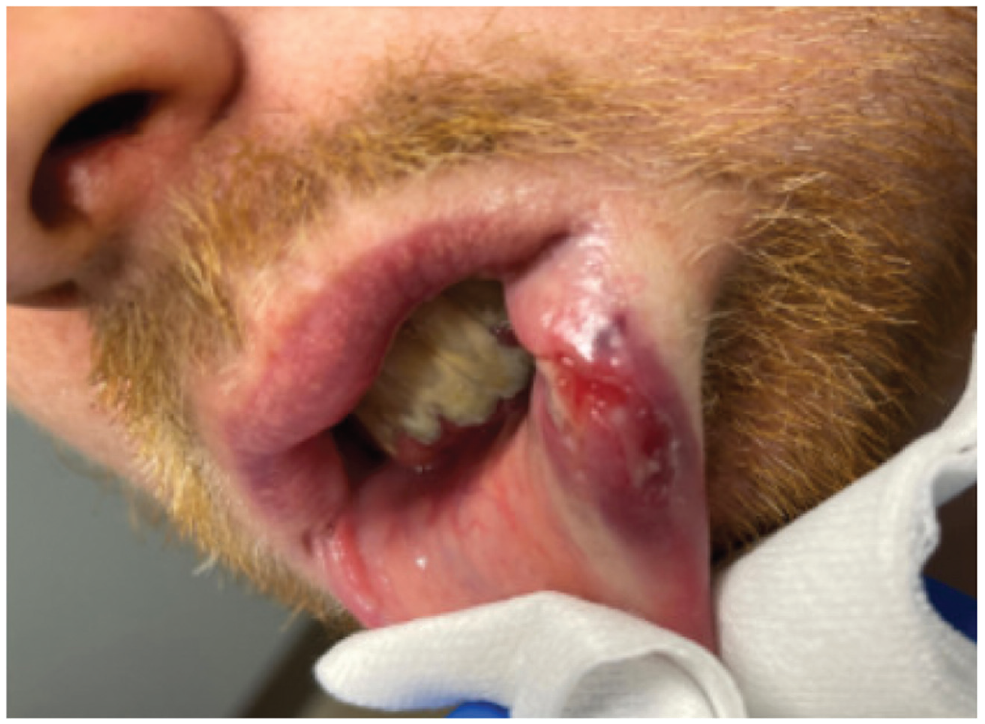
Pretreatment left lateral lip oral lesion. The oral lesion at initial presentation over the buccal aspect of the left lateral lower lip measures about 2.5 cm.
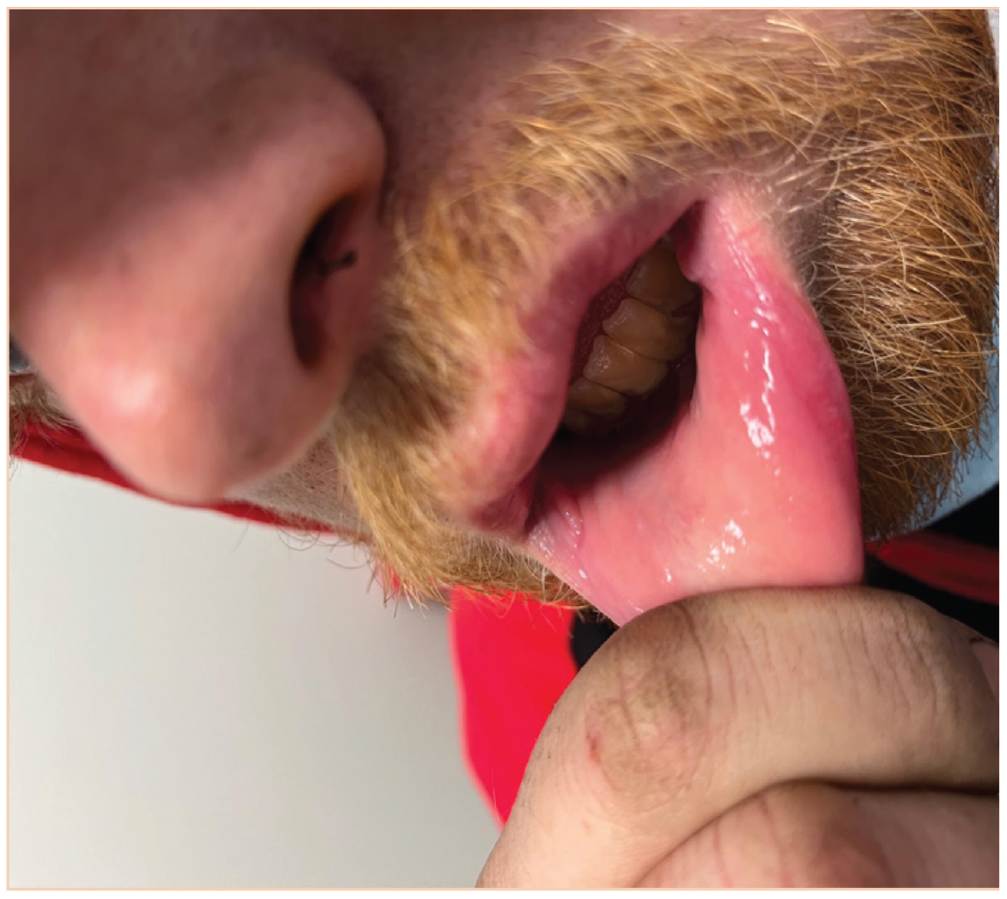
Posttreatment left lateral lip oral lesion. The site of the previous oral lesion has resolved after treatment with appropriate antibiotic therapy.
Discussion
Typically, when a patient presents with an oral lesion and with lymph node enlargement for several months, syphilis is not on the top of the differential. The differential diagnosis for lymph node enlargement with associated painful oral ulceration may include neoplastic, autoimmune, or infectious processes. In our case, concern for a neoplastic process was high due to the length and overall symptomatology.
Clinical suspicion for syphilis relies on history, with an emphasis on sexual history, and physical examination leading to laboratory testing. Laboratory testing for syphilis includes a nontreponemal serologic test (eg, venereal disease research laboratory or rapid plasma reagent), followed by a treponemal test (eg, T pallidum particle agglutination assay, fluorescent treponemal antibody absorption, or T pallidum hemagglutination assay). Treponemes may also be directly visualized from biopsies of primary and secondary lesions via Warthin-Starry or immunohistochemical staining. 4
Most cases of primary and secondary syphilis are managed with a single intramuscular injection of 2.5 million units of penicillin G benzathine. Tertiary syphilis requires a longer treatment. 4 In cases of penicillin allergy, oral doxycycline (100 mg, twice daily for 14 days) has been shown to have similar outcomes to penicillin. 4
With the presentation of oral syphilitic lesions, otolaryngologists play an important role in early identification of syphilis. Here we presented a case of secondary syphilis masquerading as suspected oral cavity cancer, highlighting the importance of maintaining a high index of suspicion for syphilis when presented with atypical oral lesions.
