Abstract
Objective
The power output from carbon dioxide (CO2) laser fibers has the potential to be diminished if there are any bends along its course, which may alter the effect the laser has on the target tissue. In this study, we assess how bending of CO2 laser flexible fiber assemblies affects the energy output measured at the end of the fiber.
Study Design
Laboratory study.
Setting
Laboratory.
Methods
Eight separate flexible fibers were tested—4 were of a type commonly used in endoscopic airway procedures, and the other 4 were a type used in otologic surgery. Fibers were bent in various configurations, and the power output of a CO2 laser fired through the bent fiber was measured. The output through the bent fiber was normalized to the output with a straight fiber. Correlations between bend parameters and power outputs was tested using Spearman’s correlation coefficient.
Results
For the airway fibers, there was a weak trend toward increasing energy outputs with greater radius of curvature (P = .714) and a negative correlation between the energy output and arc of rotation (P = .043). For the otologic fibers, there was a trend toward increasing energy outputs with greater radius (P = .084) and a strong negative correlation between the energy output and the arc of rotation (P = .006).
Conclusion
CO2 laser energy output is reduced by bending of the laser fiber assembly. When using the CO2 laser fiber, surgeons should be aware of any bends in the fiber and are encouraged to take measures to minimize bending.
The carbon dioxide (CO2) laser is a tool frequently used in a wide variety of otolaryngologic procedures.1-8 The radiation emitted by the CO2 laser is readily absorbed by water present in biologic tissues. This gives the surgeon precise control while manipulating the target tissues and minimizes thermal damage to surrounding tissues. 9 As such, its use has been described in a wide range of applications, including stapes surgery, endoscopic airway surgery, transoral robotic surgery, and endoscopic sinus surgery.1-8
Early CO2 laser use in the operating room was limited as there was no means of directing the laser using a handheld instrument.10,11 Rather, the laser energy was transmitted as a free beam to the surgical site and directed with a micromanipulator mounted on the surgical microscope. More recently, flexible fiber assemblies with the capability of transmitting CO2 laser energy have been developed, allowing the surgeon to precisely direct the CO2 laser’s energy as required to dissect tissues.9,11,12 The flexible fiber assembly uses a hollow tube to guide the laser’s electromagnetic energy along the axis of the fiber to the end held by the surgeon.10,11
It is possible that bending of the CO2 laser fiber will affect the amount of energy that is transmitted all the way through the laser fiber to the end held by the surgeon as some of the energy may be absorbed by the fiber itself instead of being transmitted to the end. 11 Even if bending along the course of the flexible fiber does not permanently damage it, bending may dissipate the energy that is introduced into the assembly. Because of this, the effect of the laser energy on the target tissues might not be as robust as intended by the surgeon. Surgeons typically test fire a laser before direct patient use, to confirm appropriate tissue effect. If the power output is altered during any subsequent bending or unbending of the fiber, the tissue effect may be altered. Unexpected power-level changes could reduce the safety and effectiveness of the CO2 laser tool.
While the effect of bending other types of laser fibers has been studied, this effect in a CO2 laser fiber has not been published in the literature.13,14 In this study, we assess how bending of CO2 laser flexible fiber assemblies frequently used in otolaryngologic surgeries affects the energy output measured at the end of the fiber. We hypothesize that bending the flexible fiber will reduce power output, with the output being directly correlated with the bend radius and inversely correlated with arc of rotation.
Methods
This study does not involve human subjects and was thus exempted from review by the Rush University Medical Center Institutional Review Board.
Eight separate CO2 laser flexible fiber assemblies manufactured were studied. Four of these were a type commonly used in endoscopic airway surgery (Elevate Elite fiber; OmniGuide Surgical), and the other 4 were a type that is intended for use in otologic surgery such as stapedectomy (BeamPath OTO-S fiber; OmniGuide Surgical).
For each trial, the CO2 laser was fired through the flexible fiber at a power level in accordance with the manufacturer’s recommendation. The Elevate Elite fibers were tested with the laser firing at a setting of 10 W with 50 psi helium flow. The OTO-S fibers were tested with the laser set to 5 W with 10 psi helium flow. The power output at the end of the fiber was measured using an optical power meter (Ophir Photonics).
The output was first measured with the fiber in a straight configuration as a baseline or control. Next, the power output was measured with the fiber sequentially at a radius of 15 cm, followed by 10 cm, and finally 5 cm, each with a 360° arc of rotation. The output was then once again measured with the fiber in a straight configuration to ensure there was no mechanical damage to the fiber, defined as a greater than 10% drop in the power output from baseline. Damaged fibers were to be excluded from further study. Finally, outputs were measured with the fiber bent at a fixed radius of 5 cm with a 180° arc followed by a 720° arc. This same procedure was repeated with all 8 flexible laser fibers.
The output of every fiber in each bending condition was expressed as a percentage of the baseline. These percentages were plotted to determine the effects of the radius and arc of rotation on power output. A Spearman correlation test was performed to identify trends, with P < .05 considered statistically significant. Statistical testing was performed using SPSS 27 (SPSS, Inc).
Results
Plots summarizing the results of the experiment for the airway fibers are shown in Figure 1 . There was a weak trend toward increasing energy outputs with greater radius of curvature, but this was not statistically significant (Spearman ρ = 0.118, P = .714). The mean power output as a percentage of the baseline was 75% for a 5-cm radius of curvature, 79% for 10 cm, and 82% for 15 cm. There was also a negative correlation between the energy output and arc of rotation, which was weakly significant on statistical testing (Spearman ρ = −0.591, P = .043). The mean power output as a percentage of the baseline was 92% for a 180° bend, 75% for 360°, and 62% for 720°. None of the airway fibers were determined to have mechanical damage after bending according to our criteria as outlined above.
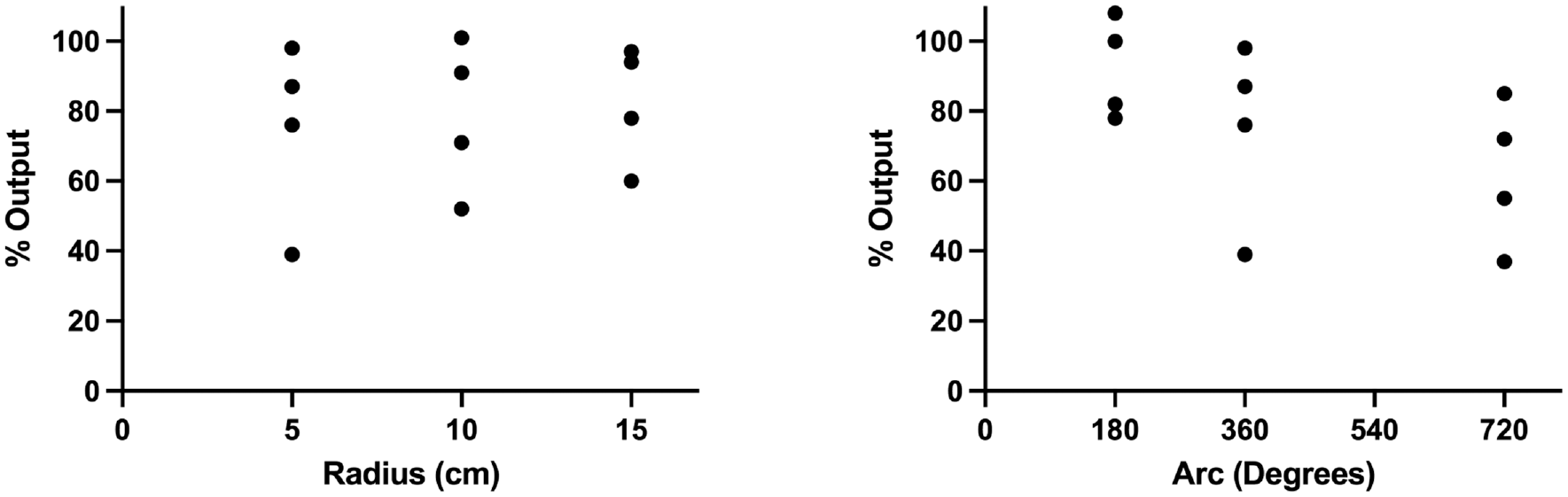
OTO Elite fiber for use in airway surgery. Left: percent output as a function of radius of curvature in cm (Spearman ρ = 0.118, P = .714). Right: percent output as a function of arc of rotation in degrees (Spearman ρ = −0.591, P = .043).
Plots summarizing the results of the experiment for the otologic fibers are shown in Figure 2 . There was once again a trend toward increasing energy outputs with greater radius of curvature, which was approaching statistical significance (Spearman ρ = 0.518, P = .084). The mean power output as a percentage of the baseline was 67% for a 5-cm radius of curvature, 79% for 10 cm, and 86% for 15 cm. There was a strong negative correlation between the energy output and the arc of rotation (Spearman ρ = −0.739, P = .006). The mean power output as a percentage of the baseline was 84% for a 180° bend, 67% for 360°, and 43% for 720°. None of the otologic fibers were determined to have mechanical damage after bending according to our criteria as outlined above.
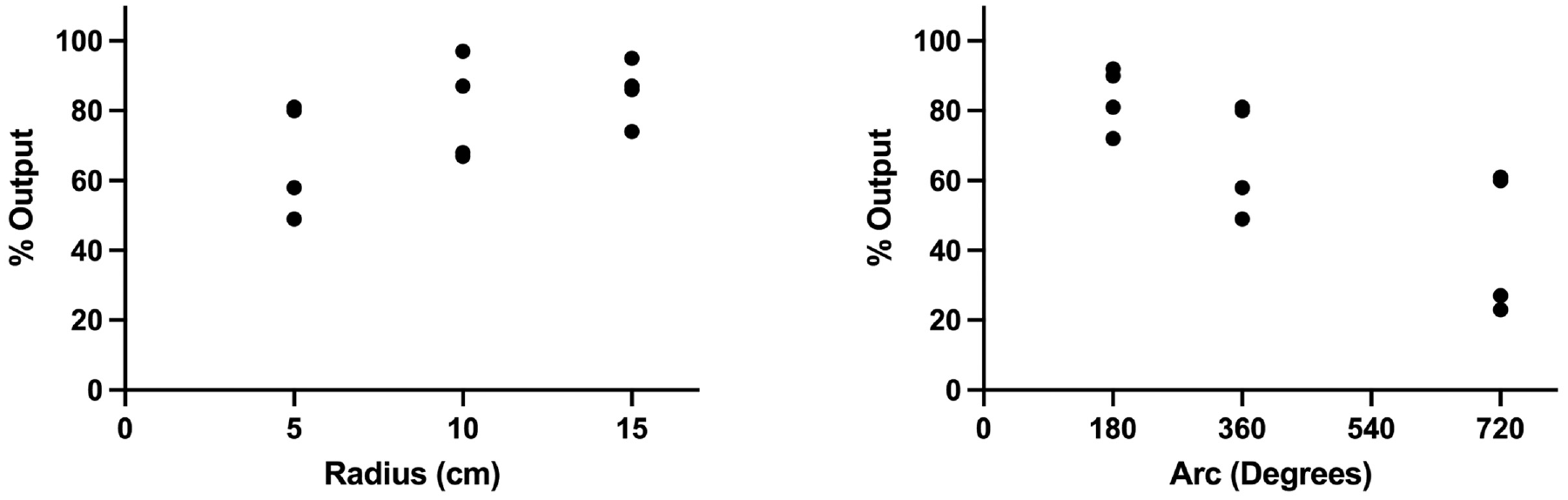
OTO-S fiber for use in otologic surgery. Left: percent output as a function of radius of curvature in cm (Spearman ρ = 0.518, P = .084). Right: percent output as a function of arc of rotation in degrees (Spearman ρ = −0.739, P = .006).
Discussion
This study assessed the effect of bending CO2 laser flexible fiber assemblies on their power output. The results show that there is overall a weak positive correlation of power output with increasing radius of curvature and a more significant negative correlation with the arc of rotation. The otologic fiber was more sensitive to bending than the airway fiber.
The design of the OmniGuide CO2 laser fiber assembly has been described in a prior publication by Shurgalin and Anastassiou. 11 The design is considerably different from the silica glass optical fibers used with other types of medical lasers because the long wavelength emitted by the CO2 laser is incompatible with silica fibers. The CO2 laser fiber consists of a hollow core surrounded by a casing that serves as an omnidirectional dielectric mirror capable of reflecting light at all angles of incidence. The mirror confines the laser’s beam within the hollow core and guides it along the axis of the fiber. Helium flow through the core of the fiber cools the walls and clears smoke and debris from the surgical site. When the fiber is bent, more energy is absorbed by the fiber wall, diminishing the energy output at the end of the fiber directed at the surgical site.
The otology fiber was more sensitive to bending due to its smaller diameter resulting from a smaller core. With a smaller core, there is greater interaction between the laser beam and the walls of the fiber, resulting in greater energy dissipation. The smaller-diameter fiber allows for more precise application of the CO2 laser’s energy during surgical procedures requiring manipulation of very delicate structures, such as stapedectomy.6,10 While the smaller-diameter fiber is required for otologic surgery, surgeons should be aware that these fibers may be more prone to bending, which in turn may reduce the energy output.
The results of the study should encourage surgeons to be mindful of the curvature applied to the CO2 laser fiber during surgery. Dramatic changes to the energy output of the CO2 laser only happened under bending conditions that are unlikely to spontaneously occur in the operating room. Nonetheless, surgeons with prior experience using the CO2 laser may be able to notice even small changes in the laser’s ability to manipulate tissues. If it appears during CO2 laser use intraoperatively that the energy is not interacting with tissues in the expected manner, the surgical team should reassess and minimize any bending in the laser fiber assembly. Even if a single severe bend is not present in the fiber, the effect of multiple small bends may be additive, resulting in a more substantial change in power output. As shown with these results, the minor amount of bending that is more likely to occur spontaneously in the operating room does not cause a significant decrease in energy output. In cases where a significant alteration in tissue interactions is seen with only mild fiber bending, the surgical team should quickly turn to other methods of troubleshooting the laser assembly beyond simply straightening the fiber.
Operating room preparation is another important consideration to minimize bending of the laser fiber. The distance between the laser and the surgeon, the handedness of the surgeon, and the laterality of the surgical site in otologic surgeries are all important considerations when preparing the operating room for a laser procedure. Ideally, the laser is located behind the surgeon, at a diagonal toward the hand in which the surgeon will be using the laser. The laser should be at a distance that allows comfortable maneuverability of the handpiece without resistance but not so close to the surgeon that the fiber begins to coil.
Conclusion
CO2 laser energy output is reduced by bending of the laser fiber assembly. Both the radius and arc of the bend can affect the energy output. The smaller-diameter otologic fiber is more sensitive to the effects of bending than the larger-diameter airway fiber. When using the CO2 laser fiber, surgeons should be aware of any bends in the fiber and are encouraged to take measures to minimize bending.
