Abstract
Zenker’s diverticulum is a rare cause of progressive dysphagia that is treated surgically. Potassium titanyl phosphate (KTP) laser–based diverticulotomy is one effective treatment. Developing a simulation model is helpful for rare conditions. Pigs have a natural hypopharyngeal pouch similar to a diverticulum. We present a model for performing rigid endoscopic KTP laser diverticulotomy in a porcine model with a laryngeal dissection station. Eleven pigs were examined to confirm presence of the hypopharyngeal pouch. A specimen was mounted on the modified laryngeal dissection station, and a KTP laser–based diverticulotomy was performed. Novel aspects include use of the laryngeal dissection station and application of the model for simulating rigid endoscopic KTP laser diverticulotomy. This model allows trainees to practice equipment setup, positioning of the laryngoscope to isolate the cricopharyngeal bar, tissue handling, laser safety techniques, and use of the KTP laser through the laryngoscope under microscopic visualization.
Zenker’s diverticulum is a pulsion diverticulum in Killian’s triangle,1-4 characterized by progressive symptoms including dysphagia with obstruction, regurgitation, cough, globus, and halitosis. 3 This can lead to aspiration and pneumonia. 5 Disease prevalence is 2 per 100,000, 6 and treatment is surgical.
As patients are typically older, 7 endoscopic approaches can be desirable, offering shorter operative time, reduced hospital stay, and earlier oral intake.8-11 Recent reviews demonstrated a mortality of 0.2% to 0.4% with endoscopic approaches, compared with 0.6% to 0.9% with open procedures.12,13 Notably, endoscopic procedures are not feasible for patients with unfavorable anatomy, recurrent diverticulum, or small or large diverticulum.14-17 Furthermore, open procedures have a lower rate of symptom recurrence and need for revision procedures. 18 When an endoscopic approach is feasible, options include stapler, 19 carbon dioxide laser, 20 and potassium titanyl phosphate (KTP) laser. 2 The KTP laser has advantages, such as coagulation around the incision, which seals the wound edges, and a lower probability of postoperative leakage. 1
Given the rare prevalence, simulation training is desirable. There has been an emphasis on simulation from the American Residency Review Committee for Surgery, 21 and surgeons with prior simulation training demonstrate greater skill and make fewer errors than do those without. 22
There are 2 models of endoscopic treatment for Zenker’s diverticulum. The first uses a latex glove on a wooden frame to simulate stapler diverticulostomy. 23 Trainees can become familiar with the Weerda laryngoscope and stapler; however, this model does not allow for tissue handling and cannot be used with lasers. A second model simulates flexible endoscopic approaches on a porcine model. 24 The domestic pig has a natural hypopharyngeal pouch,24-26 making it an ideal animal model for Zenker’s diverticulum. We used the porcine model to simulate rigid endoscopic treatment of Zenker’s diverticulum using an adapted laryngeal dissection station 27 and KTP laser. Novel aspects include use of the laryngeal dissection station and application of the model for simulating rigid endoscopic KTP laser diverticulotomy.
Methods
This study was exempt from animal protocol review. The larynx, pharynx, and cervical esophagus were excised from 11 pigs obtained from slaughterhouses. All had a hypopharyngeal pouch ( Figure 1 ). The trachea was trimmed. The station is portable, easy to clean, and applicable for open and endoscopic laryngeal procedures, and it costs about $800. 27
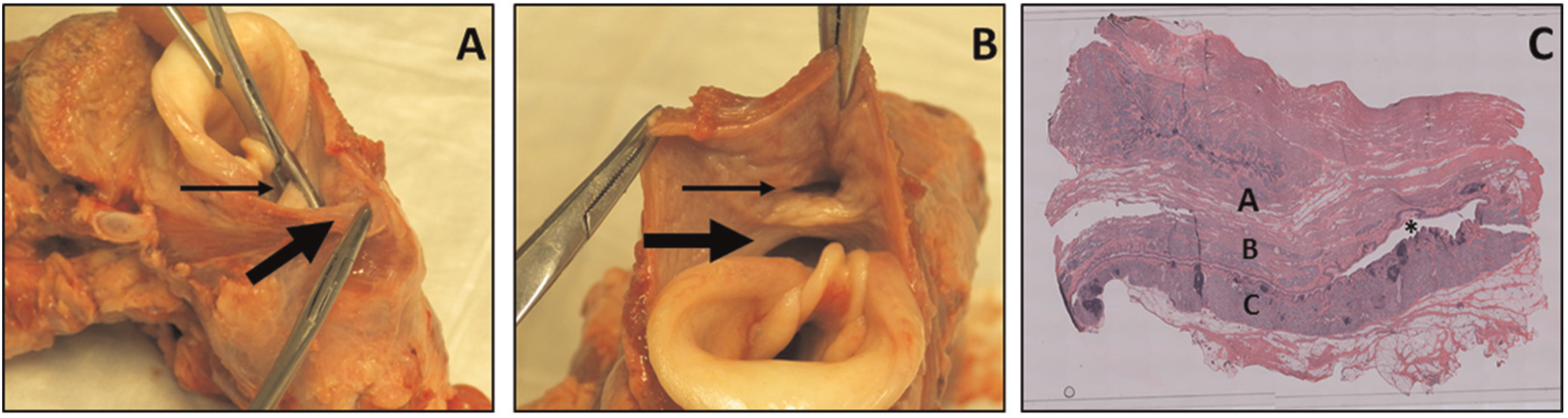
(A) Hemostat with tine in esophagus (left) and diverticulum (right); small arrow identifies bar. Second hemostat holds posterior pouch border (large arrow). (B) Esophagus (large arrow) and diverticulum (small arrow). (C) 4X hematoxylin and eosin–stained axial section of hypopharyngeal pouch (asterisk): A, anterior esophageal wall; B, common wall; C, posterior hypopharyngeal wall.
The laryngoscope has 2 ends: an end simulating the Zeitels glottiscope and a dual-lipped end used for balancing instruments. This is similar to the Hollinger-Benjamin laryngoscope used to expose a cricopharyngeal bar. For this simulation, the laryngoscope is turned 180° such that this end exposes the segment between the hypopharyngeal pouch and esophageal lumen. Hemostats next to the epiglottis provide anterolateral tension, and additional hemostats grasping the interarytenoid space and posterior pouch are suspended along the laryngoscope to provide superior tension ( Figure 2 ). Hemostats are secured with rubber bands. Setup takes approximately 3 minutes once the specimen is prepared. Laser safety precautions are instituted, including goggles, towels, statement on oxygen level, placement of pledgets in the esophagus, and orders for “laser on”/“laser off.”
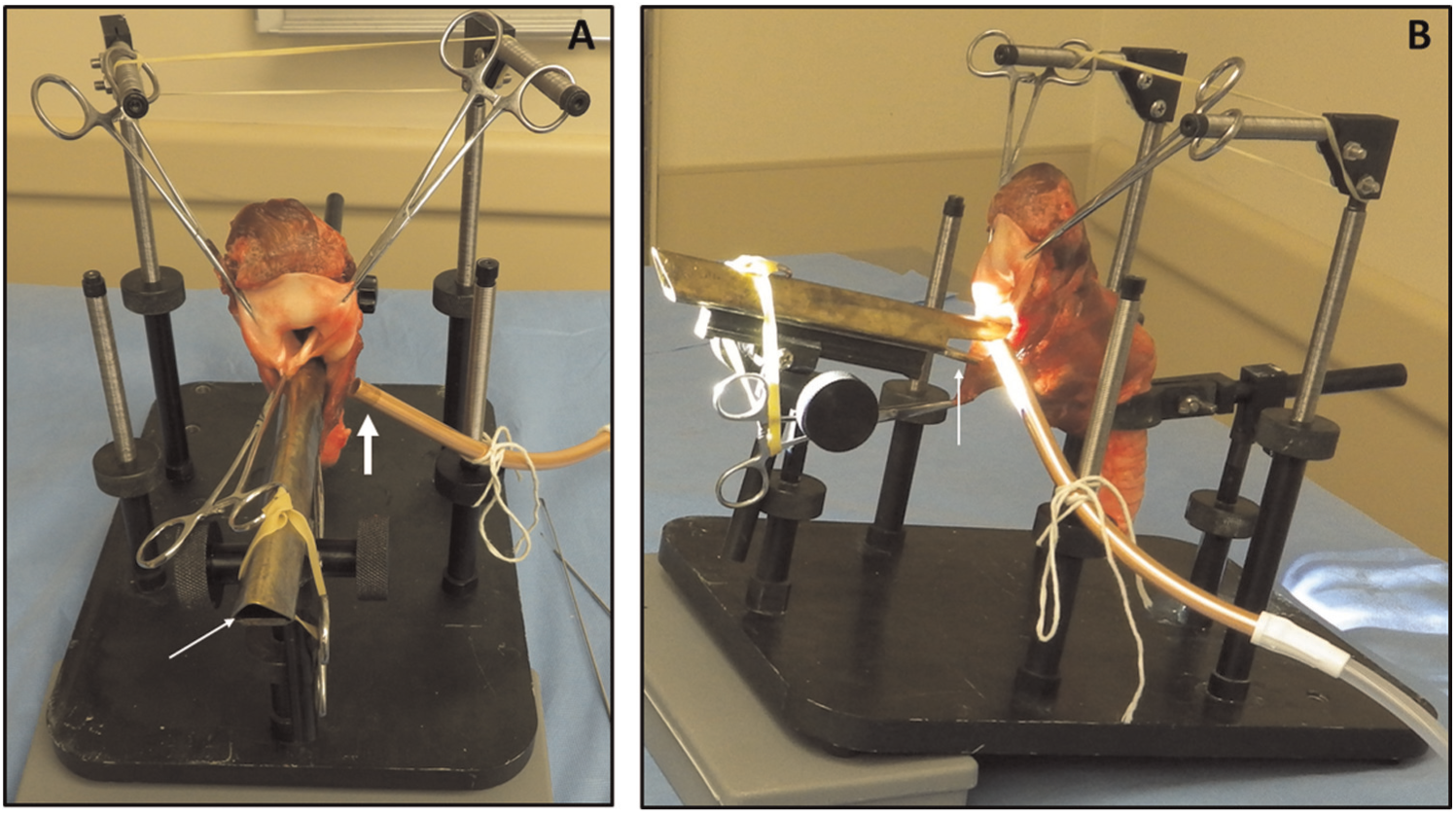
(A) Hemostats grasp epiglottis, interarytenoid notch, and posterior diverticulum. Laryngoscope opening (small arrow). Suction (large arrow) eliminates smoke. (B) Two lips of laryngoscope (arrow) expose cricopharyngeal bar: upper lip in esophagus, lower lip in pouch.
An operating microscope is used. Continuous suction is provided next to the laryngoscope ( Figure 2A ). The KTP laser at 5 W continuously incises the cricopharyngeal bar in anterior-to-posterior fashion while a Bouchayer forceps provides countertraction ( Figure 3 ). Outcomes for trainee performance include isolation of the cricopharyngeal bar, appropriate laser safety precautions, proper instrument handling, and division of the cricopharyngeal bar.
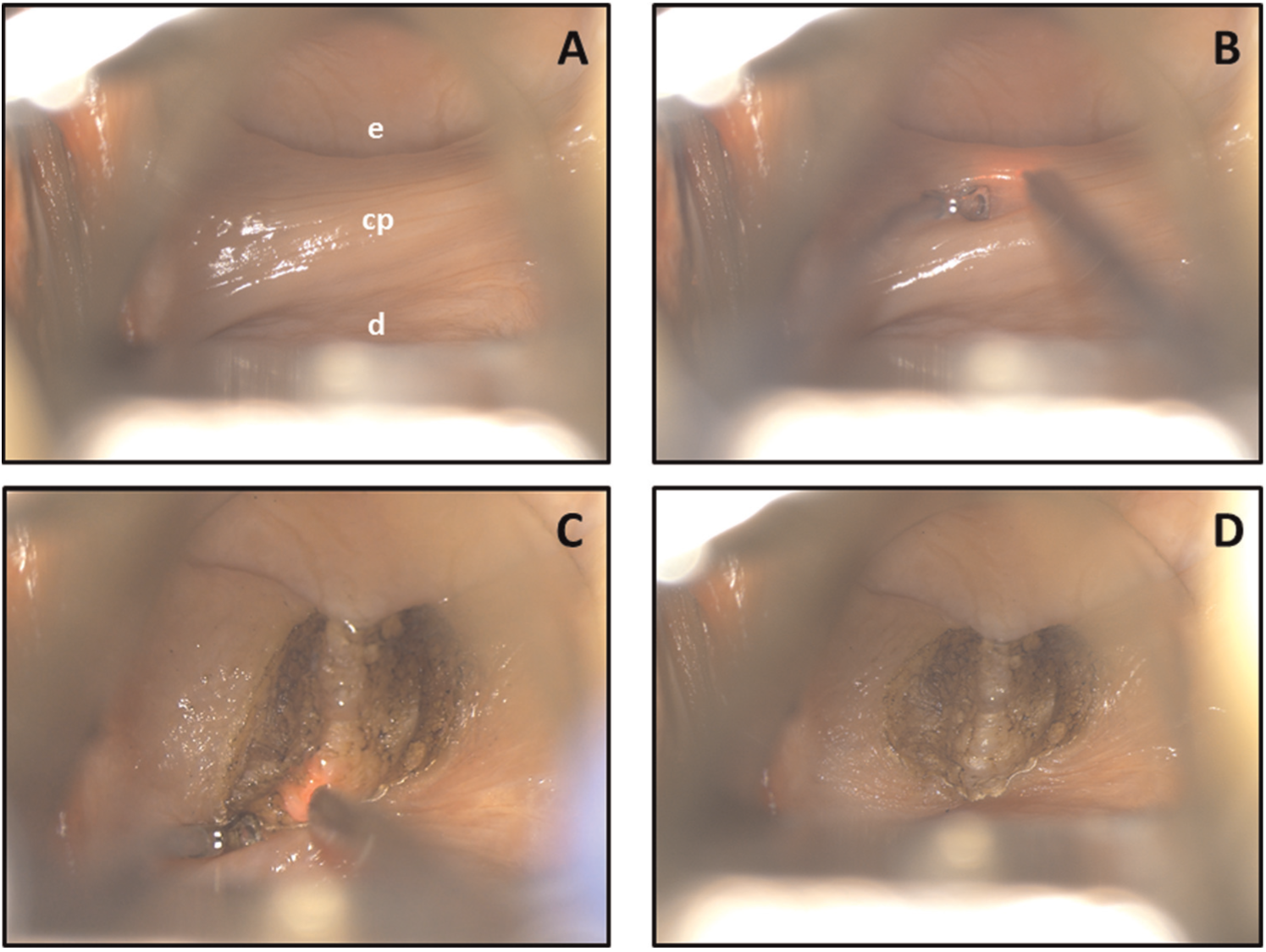
KTP laser diverticulotomy. (A) Exposing cricopharyngeal bar (cp), esophagus (e) anteriorly, and diverticulum (d) posteriorly. (B) Bouchayer forceps provides traction while laser handpiece is positioned. (C) Posterior bar is divided. (D) Partially divided cricopharyngeal bar.
For hematoxylin and eosin staining, the hypopharyngeal pouch and cervical esophagus were embedded in optimum cutting compound, snap-frozen in 2-methylbutane cooled by liquid nitrogen, and stored at −80°C. The optimum cutting compound–embedded tissue was cut into 25-µm axial sections with a −12°C cryostat (Leica CM1850; Leica Biosystems, Wetzlar, Germany); sections were mounted and stained with standard hematoxylin-eosin protocol. Photographs were taken with 4× magnification and combined to generate 1 image with Olympus cellSens Imaging Software ( Figure 1C ).
Results
The hypopharyngeal pouch simulated Zenker’s diverticulum ( Figure 1 ); the laryngoscope exposed the cricopharyngeal bar ( Figure 2 ); and the cricopharyngeal bar could be ablated with the KTP laser ( Figure 3 ).
Discussion
Surgical simulation gives trainees exposure to uncommon procedures and is linked to improved patient outcomes.21,22 Zenker’s diverticulum represents an ideal disorder for simulation: it is rare 6 ; resident and attending cannot participate in the procedure simultaneously; and the porcine hypopharyngeal pouch closely approximates the pathology, providing an ex vivo model without need for animal sacrifice specific to the simulation.
This model is useful to help trainees with equipment setup, endoscope positioning around the cricopharyngeal bar, laser safety, tissue handling, simultaneous retraction and laser treatment, and use of the KTP laser, including application of laser energy, suctioning of laser plume, and tissue ablation. Furthermore, pig specimens are inexpensive, available from slaughterhouses, and similar size to human specimens. The laryngeal dissection station is easily adapted to simulating rigid endoscopic interventions. A key limitation of the model is its lack of an oral cavity and oropharynx to practice laryngoscope placement without incurring dental injury. Study limitations include the lack of a formal performance evaluation and confirmation that the trainee’s comfort level increased following the simulation; future studies will address these issues.
Recent literature on the KTP laser approach following the initial 10-patient series 2 in 1992 is limited, with an 18-patient series in 1998 and a case report in 2005.1,28 Potential benefits include decreased bleeding intraoperatively and decreased leak risk postoperatively. Furthermore, one can see the cricopharyngeal fibers as they are being divided to increase precision. With an available model, providers may become comfortable with the procedure and perform it more frequently. This model description is an initial step in that direction.
Author Contributions
Disclosures
Footnotes
Sponsorships or competing interests that may be relevant to content are disclosed at the end of this article.
