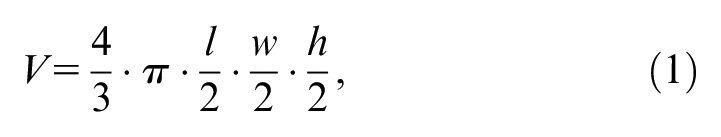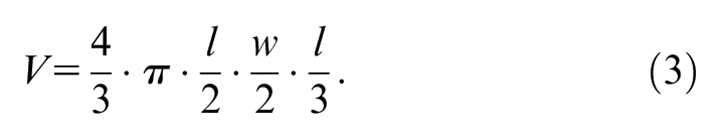Abstract
Objective
To perform a systematic review of the literature evaluating clinical characteristics and management of cervical ganglioneuromas (CGNs).
Data Sources
PubMed, Embase, and Cochrane Library databases were searched. Data such as patient demographics, imaging, and treatments were obtained.
Review Methods
Pertinent studies were downloaded, and the full text was reviewed by 4 authors (N.P., S.S., C.F., D.T.). Results were reported via the PRISMA guidelines (Preferred Reporting Items for Systematic Reviews and Meta-analyses).
Results
Fifty-two studies with 58 patients were identified in the literature. Of the 58 patients, 22 were adults and 36 were pediatric. The most common reported location of CGN was within the parapharyngeal space (76%), followed by the retropharyngeal (19%) and paravertebral/prevertebral (7%) spaces. The most common presenting symptoms included a nontender mass (29.3%), dysphagia (17.2%), and hoarseness (10.3%). Interestingly, the average tumor volume for patients with postoperative Horner’s syndrome was 183 mm3 (n = 21, 47.7%) vs 946 mm3 in patients without Horner’s syndrome (n = 23, 52.3%). This represents a statistically significant finding (P = .018). There exists no significant difference in tumor volumes between adult and pediatric patients with Horner’s syndrome (P = .645).
Conclusion
CGN is a rare tumor of the sympathetic nervous system. Management should involve complete surgical excision with biopsy. We found that patients with small-volume CGNs are significantly more likely to experience postoperative Horner’s syndrome. This finding is independent of age and should therefore be taken into consideration in any patient with suspected CGN.
Ganglioneuromas are rare benign neurogenic tumors of the sympathetic nervous system. Ganglioneuromas, neuroblastomas, and ganglioneuroblastomas constitute a trio of neurogenic tumors that differ by their potential for malignancy and differentiation. Typically found in the posterior mediastinum or retroperitoneum, ganglioneuromas represent the benign and well-differentiated form of a neurogenic tumor.1,2 Neuroblastomas are malignant, undifferentiated, and aggressive while ganglioneuroblastomas are more intermediate. Based on a literature review of 26 patients by Ma et al, ganglioneuromas in the cervical region are most frequently found in young adults and more commonly in females. The most frequent site of origin is the cervical sympathetic chain, with other possible sites including the larynx, pharynx, and ganglion nodosum of the vagus nerve. 3
The typical presentation is an isolated painless mass with a slow growth rate. Pathologic examination is critical for its diagnosis, and fine-needle aspiration (FNA) biopsy is considered limited in its confirmatory diagnostic capacity.
Accurately diagnosing ganglioneuromas prior to surgical excision is often a challenge. A review by Sinha et al demonstrated that preoperative FNA cytology had an identification failure rate of 60% and even led to misleading diagnoses. 4 Preoperative counseling of potential postoperative complications and sequelae, particularly regarding Horner’s syndrome (the classic triad of ptosis, miosis, and anhidrosis) and vocal cord injury, is imperative. The preferred management is complete surgical excision, as ganglioneuromas contain a ganglionic and thereby radioresistant component. 4
This systematic review presents baseline patient characteristics, imaging, complications, and an in-depth volumetric analysis. Data presented herein were gathered from a combination of case reports, case series, and 1 retrospective case study. There currently exist no prospective randomized controlled trials comparing management of cervical ganglioneuroma (CGN). To our knowledge, this is the only systematic review of CGN to date.
Methods
This systematic review was completed in accordance with the PRISMA guidelines (Preferred Reporting Items for Systematic Reviews and Meta-analyses). 5 A preliminary literature search of PubMed/MEDLINE (1950–February 30th, 2019), Embase (1950–February 30th, 2019), and the Cochrane Library was performed. The search included the following key terms alongside Medical Study Heading terminology related to ganglioneuromas: (parapharyngeal, retropharyngeal, cervical).
Study Selection Process and Inclusion Criteria
Titles and abstracts of all initial studies retrieved were screened for inclusion by 2 independent authors (N.P. and C.F.). The primary inclusion criterion for the studies was that they reported patient cases of CGN, the most common ganglioneuroma that would be treated by a head and neck surgeon.
Non-English literature, nonhuman studies, review articles, studies unrelated to CGN, studies with insufficient individual patient data, and patients with neurofibromatosis were excluded. Pertinent studies were downloaded, and the full text was reviewed by 4 authors (N.P., S.S., C.F., D.T.). A thorough bibliography review yielded several additional studies for inclusion. The publication dates of the studies that fulfilled the inclusion criterion of containing primary data related to CGN ranged between 1950 and March 30, 2019. A total of 52 studies met criteria for inclusion and were comprehensively reviewed. Figure 1 outlines the search strategy and inclusion process employed for this systematic review.
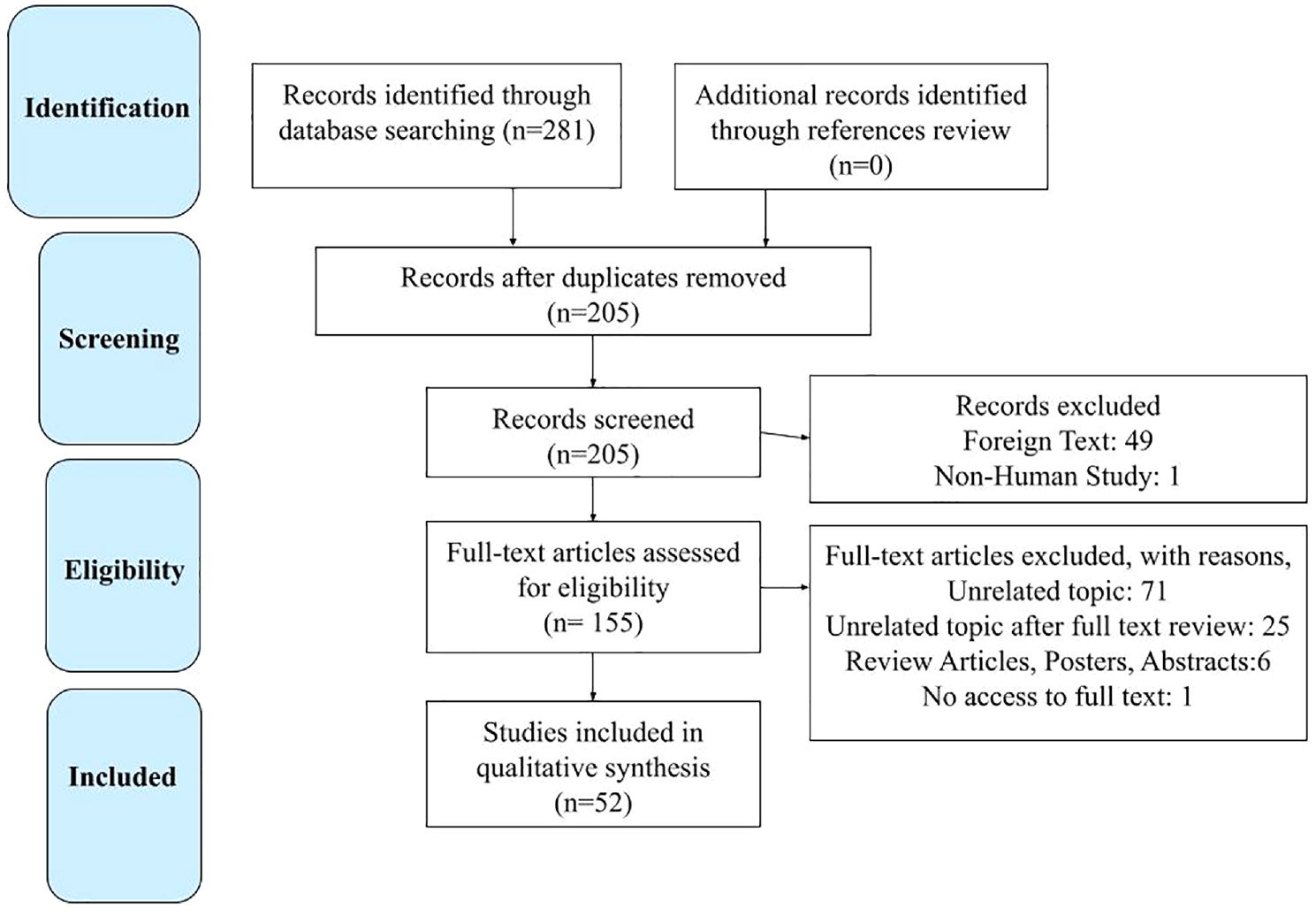
Article selection process based on the PRISMA guidelines (Preferred Reporting Items for Systematic Reviews and Meta-analyses) and search algorithm employed.
All studies were allocated a quality score for level of evidence and risk of bias via the GRADE criteria (Grading of Recommendations, Assessment, Development and Evaluation), MINORS criteria (Methodological Index for Non-randomized Studies), and the Cochrane Bias Tool.
Data Extraction
From the studies, patient demographics, clinical data, and outcomes were obtained and analyzed. Patient demographics included sex and age at the time of CGN diagnosis. Clinical data included presenting symptoms, primary indication for surgical intervention, surgical approach, and management. The reviewed surgical treatments were surgical excision and cervicotomy. Outcomes consisted of surgical complications, reconstruction, follow-up duration, and treatment success (defined in this study as complete resolution of presenting symptoms at time of last recorded follow-up).
Statistical Analysis
Relevant tumor and subject characteristics were compared as appropriate by independent samples t test, Mann-Whitney U test, chi-square test, or Fisher exact test. All statistical tests were 2-sided, and P values were evaluated at the alpha level of 0.05. Data analysis was performed with SPSS 85 version 24.0 (IBM). 6
Volumetric Analysis
Tumors are 3-dimensional objects composed of 3 diameters (length, width, and height). Before volume is estimated, tumor shape must be assumed. Magnetic resonance imaging (MRI) findings and photographs of excised ganglioneuroma tumors tend to show an elongated sphere-like shape known as an ellipsoid. In other clinical contexts, the assumption of ellipsoid shape has proven to be the most accurate approach for calculating tumor volume 7 :
where l is tumor length, w is tumor width, and h is tumor height. Although most articles reported all 3 measurements, 10 articles in this review mentioned only 2 dimensions. Calculations of tumor volume in cubic millimeters (mm3) requires a third parameter. 8 A possible solution utilized by other groups is a height approximation via the longest known dimension of the tumor, which by definition is the length:
Calculation of the ellipsoid volume can then be achieved by substituting equation 2 into equation 3:
In 3 articles, just a single measurement of diameter was reported. Coupled with the mention of an approximate sphere shape in the text, this knowledge was sufficient to calculate tumor volume by the following formula:
Results
The preliminary literature search yielded 281 abstracts, studies, and review articles. No prior systematic reviews or meta-analyses relating to cervical CGN were identified in the current literature. In total, 52 studies met inclusion criteria. Between 1950 and March 30, 2019, 58 cases of CGN were identified from 47 case reports, 4 case series, and 1 retrospective case study. No randomized controlled trials were identified. According to the Cochrane Bias Tool, 1 study was assessed at low risk of bias, 49 at unclear risk, and 2 at high risk. Per the GRADE and MINORS criteria, the quality of evidence was considered low to moderate; therefore, additional research is required to verify our conclusions. A complete overview of the key study findings is shown in Supplemental Table S1 (available online).
Patient Characteristics
Patient characteristics were evaluated from 52 studies involving 58 unique cases. Fifty-two studies with 58 patients were identified in the literature. Of the 58 patients, 22 were adults. Of these 22 patients, 11 (50%) were female and 11 (50%) were male. Of the remaining 36 pediatric patients, 24 (66.7%) were female and 12 (33.3%) were male. The age of patients at the time of CGN diagnosis was reported in 57 cases (mean, 20.4 years; range, 0.5-65). Regarding location of the tumor, 40 cases (69%) of CGN were in the parapharyngeal space, 7 (12.1%) in the retropharyngeal space, 4 (6.9%) in the parapharyngeal/retropharyngeal space, 4 (6.9%) in the paravertebral/prevertebral/spinal region, and 3 (5.2%) in regions such as the peripheral cutaneous region or as diffuse invasion from the upper thorax ( Table 1 ).
Clinical Characteristics of 58 Patients.
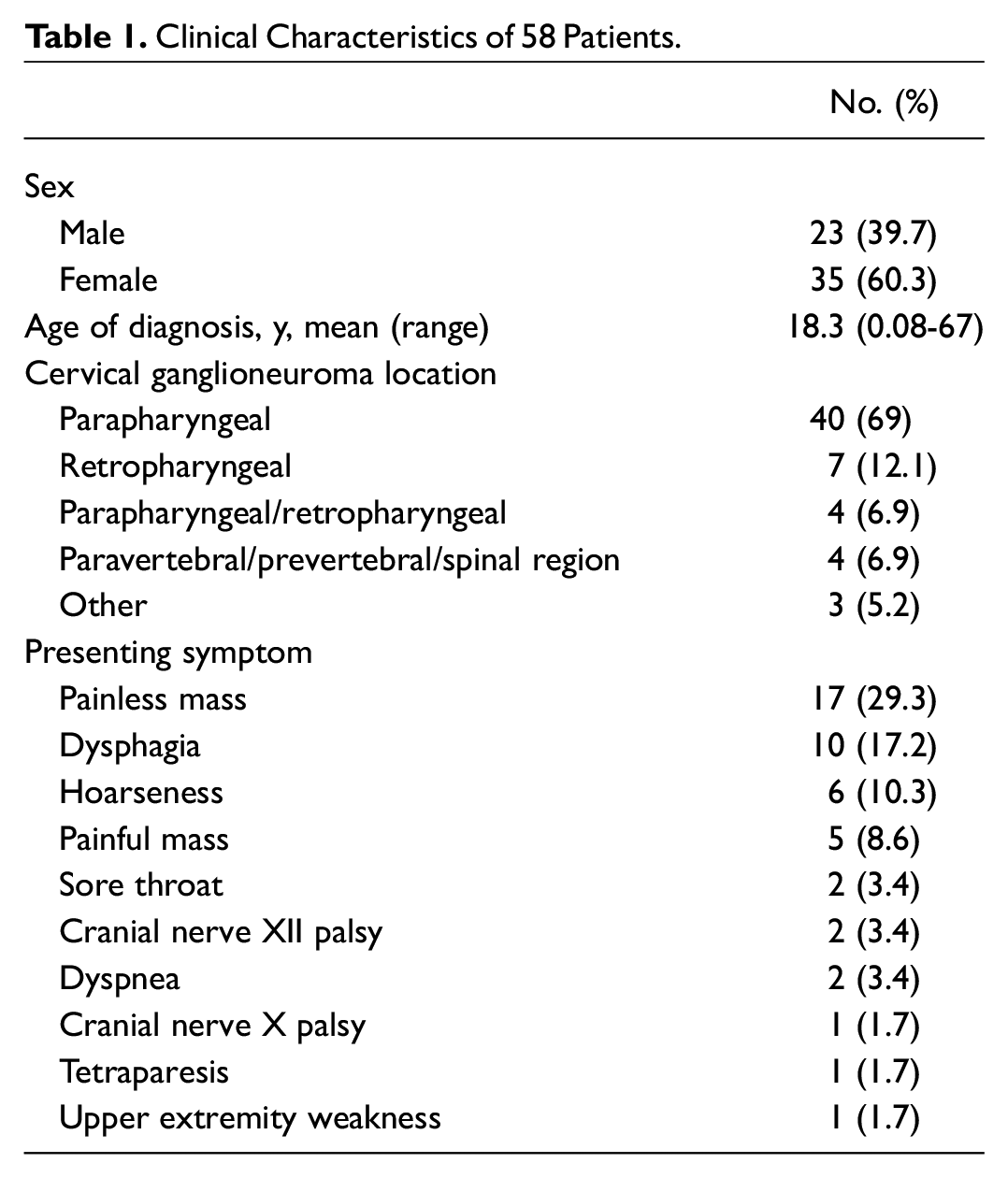
The most common presenting symptoms of CGN were a painless mass (29.3%), dysphagia (17.2%), hoarseness (10.3%), painful mass (8.9%), cranial nerve XII palsy (3.4%), sore throat (3.4%), dyspnea (3.4%), cranial nerve X palsy (1.7%), other respiratory complications (1.7%), gait disturbance (1.7%), tetraparesis (1.7%), and muscle weakness (1.7%; Table 1 ). Of the 22 parapharyngeal tumors, 21 (95.4%) presented with neck mass, 4 (18.2%) with hoarseness, 3 (13.6%) with sore throat, and 3 (13.6%) with dysphagia. Of the 8 retropharyngeal tumors, 6 (75%) presented with dysphagia, 3 (37.5%) with neck mass, and 1 (12.5%) with hoarseness. Of the 4 paravertebral tumors, 3 (75%) presented with neck mass and 1 (25%) with upper extremity weakness.
Imaging
In total, 26 (44.8%) patients had computed tomography (CT) imaging, 24 (41.4%) had MRI, and 8 (13.3%) had ultrasound. The most common finding on ultrasound scan was a solid, hypoechoic, and well-encapsulated mass. The CT findings were reported inconsistently. The most common finding on CT scan was an expansible lesion that displaced surrounding structures (n = 10, 38.5%). A well-circumscribed mass was noted in 10 cases (38.5%). Two studies indicated that the CGN swellings had resulted in an inward bulging of the oropharynx.9,10 MRI findings were variably reported. Of note, all studies with MRI findings cited enhancement with contrast. A “fusiform” enhancement pattern was indicated in 1 case. 11 Of those studies reporting T1 and T2 signal characteristics, 5 exhibited hypointensity on T1 and hyperintensity on T2, and 6 exhibited isointensity on T1 and hyperintensity on T2.
Histology
Of the 58 patients in this study, 19 (32.8%) had a history of preoperative FNA. Of the 36 pediatric patients, 11 (30.6%) underwent FNA. Of the 22 adult patients, 8 (36.4%) underwent FNA. Among the combined 19 FNA reports, 4 (21.1%) had ganglion cells, 6 (31.6%) noted spindle-shaped cells, and 6 (31.6%) were inconclusive. Of the inconclusive findings, 2 were in pediatric cases and 4 were in adult cases. Ganglion cells were observed only in pediatric patients. Of the 6 spindle-shaped cell findings, 5 were observed in pediatric patients and 1 in an adult.
Of the 58 cases, only 50 (86.2%) had histologic findings from a postexcisional biopsy. All these cases reported finding ganglion cells, with 29 (58.0%) specifying mature ganglion cells and 6 (12.0%) noting immature ganglion cells. Spindle-shaped cells on biopsy were seen in 34 (68.0%) cases, of which 20 (58.8%) were pediatric and 14 (41.2%) were adults. In 21 (42.0%) cases, these histologic findings were seen in a Schwannian stroma and 6 (12%) in a myxoid background.
Management and Postoperative Complications
Surgical resection was performed in all 58 patient cases, and 47 provided sufficient information for volumetric analysis of the tumors. The average tumor volume was 1100 mm3 with a standard deviation of 2378 mm3. A threshold of 2 standard deviations above and below the mean was used to exclude outliers. Three outliers with volumes of 6805, 7640, and 11,611 mm3 were excluded. There was no statistically significant difference between pediatric and adult tumor volumes (P = .860).
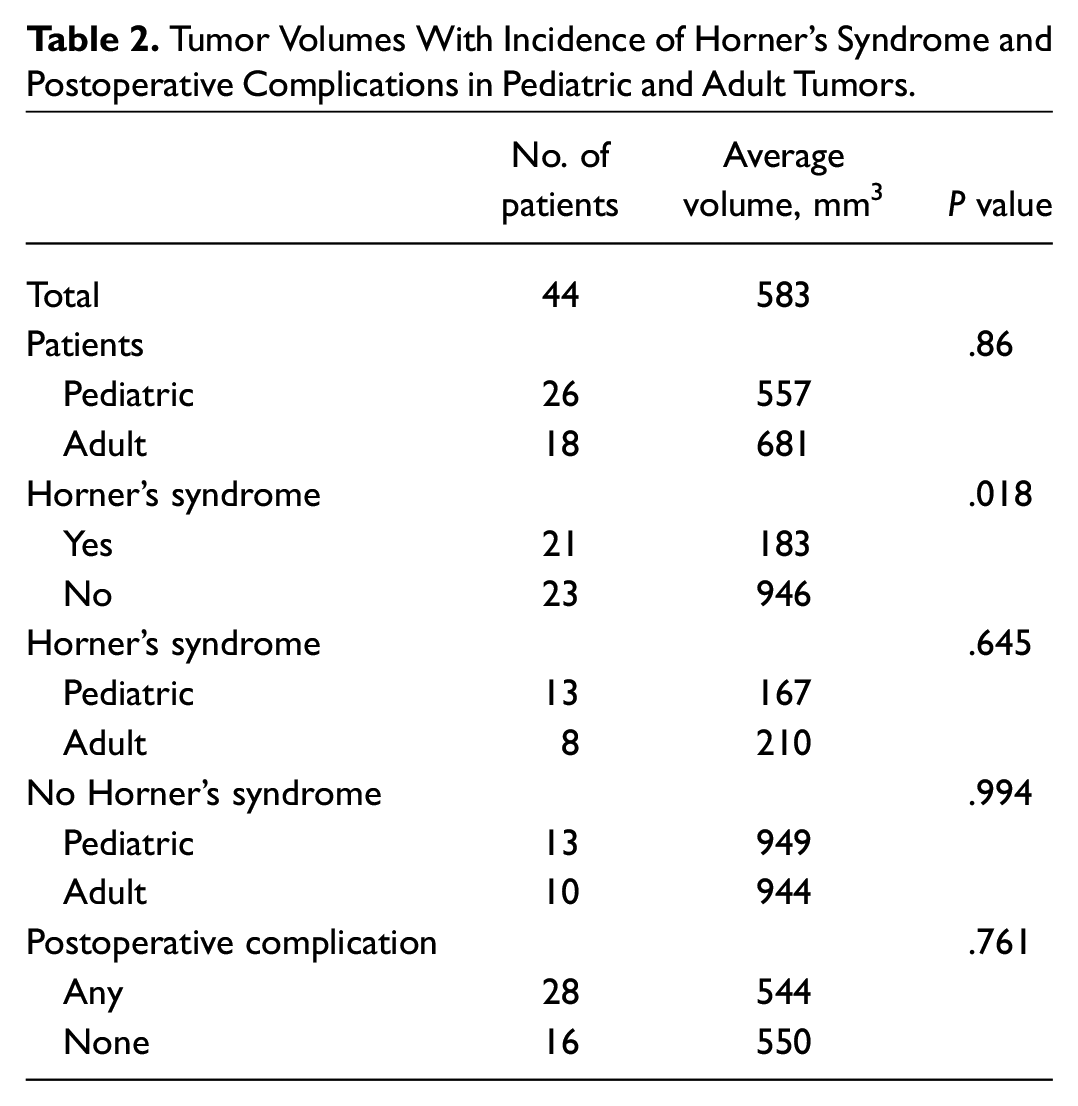
In the literature, there are 21 cases of postoperative Horner’s syndrome. The average tumor volume of these cases was 183 mm3. The average tumor volume of the 23 cases that did not report postoperative Horner’s syndrome was 946 mm3. This association between postoperative Horner’s syndrome following CGN resection and smaller tumor volume represents a statistically significant finding (P = .018). There was no significant difference in tumor volumes between adult and pediatric patients with Horner’s syndrome (P = .645) or without (P = .944). Furthermore, there was no statistically significant difference in tumor volumes for patients with any complication vs those without (P = .761). A detailed breakdown is presented in Table 2 .
Tumor Volumes With Incidence of Horner’s Syndrome and Postoperative Complications in Pediatric and Adult Tumors.
Discussion
Presenting Symptoms
CGN often presents as a solitary, painless, and slow-growing mass, and multiple occurrences in the cervical region are extremely rare. There have been case reports of hormonal activation of the mass via catecholamine secretion resulting in hypertension, diabetes, or virilization.12,13 According to our analysis, the most common presenting symptoms were a painless mass (29.3%), dysphagia (17.2%), and hoarseness (10.3%). These symptoms typically arise from tumor compression of structures surrounding the mass as opposed to hormonal activation, highlighting the significance of identifying physical traits of the tumor such as tumor volume, location, and orientation to anatomic structures, especially nerves.
Diagnosis
Algorithms for identification and treatment of CGN have yet to be defined. One possible course toward approaching and ultimately confirming a diagnosis of CGN is imaging, followed by FNA and finally histologic confirmation via surgical excision. Interpretations and diagnoses derived solely from imaging or FNA findings are frequently inconclusive or misleading.
Imaging tools such as ultrasound, CT, and MRI are for evaluating characteristics of the cervical mass but are unable to distinguish ganglioneuromas from other tumors. Ultrasound findings of a homogeneous, hypoechoic neck mass with well-defined borders should prompt CGN to be considered in the differential diagnosis. Comparatively, MRI and CT are more valuable imaging techniques in the diagnosis of ganglioneuroma. MRI is superior to CT in the diagnosis of intraspinal tumors. 14 Although ganglioneuroma tends to be a more homogeneous tumor than neuroblastoma or ganglioneuroblastoma, imaging evaluation is insufficient to discriminate among these 3 tumors. 15
Due to its cost-effectiveness and minimally invasive nature, FNA is often a first-line technique for investigating thyroid masses. The most common complication of FNA is pain and discomfort at the site of aspiration. 13 A systematic review of clinical complications following FNA biopsy of thyroid tumors reported hemorrhaging and hematoma as the next common complication. With more aggressive tumors and larger-caliber needle, there is an increased risk of tumor seeding along the needle track. 13 Due to ganglioneuroma’s benign nature, needle-track seeding from a previous FNA should not be a clinical concern. However, FNA is not reliable in diagnosing ganglioneuroma, and FNA cytology is often inconclusive.10,15,16 From these results, FNA is not recommended as a primary diagnostic tool for CGN.
The frequency of misleading and inconclusive findings from imaging and FNA results highlights the need to obtain a surgical biopsy for a definitive diagnosis. The most characteristic histologic feature of ganglioneuromas is the presence of mature ganglion cells. In this study, the 50 available excisional biopsy reports included 29 (58.0%) cases with mature ganglion cells and 6 (12.0%) with immature ganglion cells. While mature ganglion cells are most characteristic, Schwann and spindle cells are often found as well. Although FNA results can demonstrate the presence of ganglion cells and Schwann cells, the degree of observed differentiation from this limited sample could lead to misdiagnoses regarding tumor malignancy. 17
Management
Currently, the majority of cases of CGN were managed with complete surgical excision of the tumor. 18 The objectives of tumor excision are confirmation of the diagnosis and cessation of further growth and subsequent compression of anatomic structures. Ganglioneuromas do not exhibit aggressive behavior. None of the patients who underwent complete resection of their tumors showed evidence of recurrence on follow-up. Successful management depends on complete resection with sufficient exposure to avoid injury of surrounding vascular and neural structures that may cause significant morbidity, particularly Horner’s syndrome.19,20
We performed an objective post hoc calculation of tumor volumes. Comparing the average tumor volume for patients who did and did not experience Horner’s syndrome after CGN resection revealed a surprising finding. Patients who experienced Horner’s syndrome postoperatively had significantly smaller tumors. There was no statistically significant difference in tumor volumes between adult and pediatric patients who experienced Horner’s syndrome in the postoperative period. This finding is thus not age dependent and can be applied to the entire patient population.
The association between smaller tumor volume and Horner’s syndrome is likely due to multiple interacting factors. Smaller tumors may invade into the originating and surrounding nerves, which precipitate symptoms early in the disease course when the tumor is still small. This invasion may cause the tumor to be more physically adherent to nerves of the sympathetic pathway, thus predisposing patients to excisional complications and Horner’s syndrome postoperatively. In contrast, larger tumors may cause symptoms via mass effect rather than invasion.
Limitations
Although the present study summarizes the literature describing presenting symptoms, imaging, and histologic characteristics and management of CGN, several limitations exist. First, a significant portion of the CGN data was collected from the observation of case reports or case series. There are no randomized controlled trials in the current literature that compare outcomes of surgical treatment. The compiled data from each case are derived from single-surgeon or single-institutional studies, which may be subject to confounding factors and bias. In addition, it was challenging to analyze the data of treatment modalities due to the inherent variability and heterogeneity across the studies. To address these limitations, more extensive and standardized studies are required to corroborate these findings. Last, larger and more controlled studies comparing treatments are likely required to establish a proper standard of care. We defined treatment success as complete resolution of presenting symptoms at time of last recorded follow-up.
Conclusion
CGNs are rare benign tumors with a good prognosis. Patients present with an array of symptoms that arise from compression of surrounding structures. CGN is often misdiagnosed preoperatively, and excisional biopsy is essential to confirm the diagnosis. It is important to consider the tumor’s clinical, imaging, and pathologic features—such as immature ganglion cells—to conclude an appropriate preoperative differential diagnosis.
We recommend FNA to assist in the preoperative diagnosis alongside cautious awareness of the high rate of inconclusive findings from FNA results. Surgical management involves total tumor resection but carries the significant risk of postoperative Horner’s syndrome. We found an association between Horner’s syndrome following CGN resection and smaller tumors, representing a statistically significant finding (P = .018). Surgical measures may adequately control the disease process and symptomatology; however, randomized controlled studies comparing treatments would serve to corroborate these findings.
Supplemental Material
sj-docx-1-opn-10.1177_2473974X221106784 – Supplemental material for A Systematic Review of Cervical Ganglioneuromas
Supplemental material, sj-docx-1-opn-10.1177_2473974X221106784 for A Systematic Review of Cervical Ganglioneuromas by Saad Saadat, Christian Fritz, Deanna Tran, Nathan Parry, Brian T. Yuhan, Alyssa Bolduan and Eric Thorpe in OTO Open: The Official Open Access Journal of the American Academy of Otolaryngology-Head and Neck Surgery Foundation
Footnotes
Author Contributions
Disclosures
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.