Abstract
Objective
Anterior cervical discectomy and fusion have become a common intervention for cervical spine stabilization. However, complications can cause life-threatening morbidity. Among them, esophageal perforation is associated with severe morbidity, including dysphagia, malnutrition, and infection with the potential development of mediastinitis. Presentation is variable but often results in chronic morbidity. Herein we examine our experiences in the management of esophageal perforation with microvascular free tissue transfer.
Study Design
Retrospective review from January 2013 to September 2020.
Setting
Single academic tertiary care center.
Methods
This study comprised all patients (age, 41-73 years) undergoing free tissue transfer for the repair of chronic esophageal perforation secondary to anterior cervical discectomy and fusion at an academic tertiary care center. Four patients underwent repair via vastus lateralis myofascial onlay grafting for defects ≤2 cm in greatest dimension, while 1 patient underwent a fasciocutaneous radial forearm free flap repair of an 11 × 5–cm defect.
Results
Defect location ranged from hypopharynx to cervical esophagus. Mean operative time was 6.2 hours; the average length of stay for all patients was 6.6 days. Of 5 patients, 1 required additional hardware placement for spine stabilization. All patients underwent gastrostomy tube placement to bypass the surgical site during healing, and all eventually resumed an oral diet postoperatively. Recurrent fistula occurred in 1 of 5 patients. No flap failures were encountered in the study population.
Conclusion
Vastus lateralis myofascial onlay grafting and fasciocutaneous radial forearm free flap are robust, relatively low-morbidity interventions with a high success rate for definitive repair of chronic esophageal perforation. Repair should be undertaken in concert with a spine surgeon for management of the cervical spine.
Keywords
The anterior approach to the cervical spine for decompression of neural elements and arthrodesis has become a staple of spine surgery over the last several decades. However, complications can occur and cause life-threatening morbidity. Adverse events may include damage to neural structures, durotomy, vertebral or carotid artery injury, stroke, vocal cord paralysis, neck hematoma, hoarseness, paralysis, postoperative airway compromise, graft dislodgement, implant migration or failure, and esophageal injury.1-6
Esophageal perforation is a rare complication of anterior cervical spine surgery and may occur in the acute period from intraoperative injury or, more commonly, as a delayed occurrence from cervical instrumentation eroding into the esophageal lumen.1,7 Incidence of esophageal perforation ranges from 0.02% to 1.52% in the literature.7-13 Associated morbidity is secondary to dysphagia, malnourishment/failure to thrive, aspiration pneumonia, and retropharyngeal abscess with potential progression to mediastinitis, together producing a reported mortality rate of 6%. 14
Management of esophageal perforation after anterior cervical instrumentation requires a multidisciplinary approach for diagnosis, management of the cervical spine, esophageal repair, and appropriate postoperative management. While several small studies have described the repair of esophageal perforation with locoregional flaps and free tissue transfer,15-17 there is no standard approach to repair or means of determining the best approach to repair at this time. As such, we seek to present our institutional experience for the repair of these defects.
Patients and Methods
Patient Selection
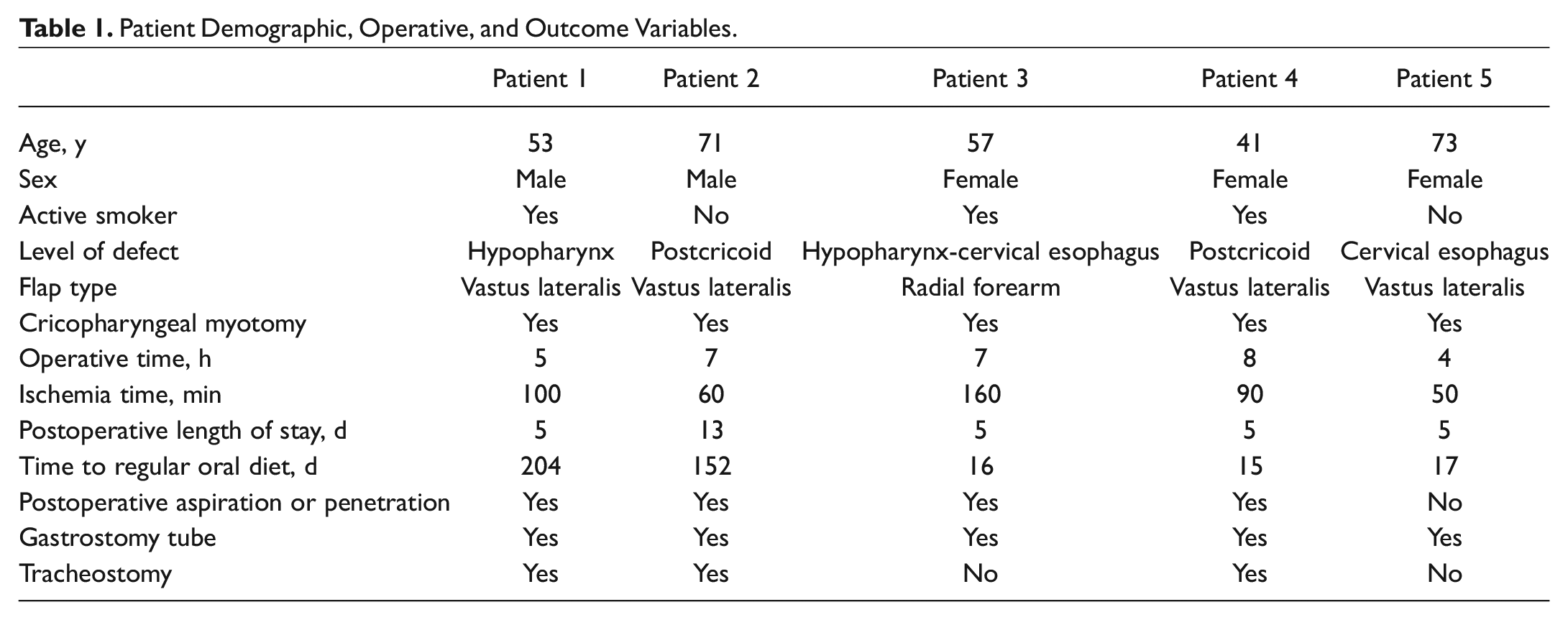
This was a retrospective chart review of all patients with chronic esophageal perforation, defined as >6 months after anterior cervical instrumentation, who were treated at a single academic tertiary care center from January 2013 to September 2020. Patients presenting with acute esophageal perforation or those managed conservatively were excluded. The study population thus consisted of 5 patients (2 men and 3 women) ranging in age from 41 to 73 years who were treated with surgical therapy 22 to 96 months from the initial anterior cervical discectomy and fusion. Three of 5 patients endorsed current tobacco use, while 1 cited former use and the last was without a history ( Table 1 ). The University of Arkansas for Medical Sciences Institutional Review Board determined that this study was exempt from oversight.
Patient Demographic, Operative, and Outcome Variables.
Surgical Technique
Vastus lateralis onlay graft (VLOG) was performed in 4 patients and fasciocutaneous radial forearm free flap (FC-RFFF) in a single patient ( Table 1 ). In all instances, preoperative computed tomography soft tissue neck with contrast was reviewed for visualization of level and laterality of hardware and the suspected site of esophageal perforation. Computed tomography neck was also reviewed for suitable vessels for microvascular anastomosis. In 4 patients, the defect was relatively small (≤2 cm), and repair was performed with primary mucosal closure and VLOG ( Figure 1 ). One patient had a large mucosal defect, approximately 11 × 5 cm, repaired with FC-RFFF ( Figure 2 ). Prior to free flap harvest, the neck was explored for suitable vessels for microvascular anastomosis, which most commonly consisted of the facial or superior thyroid artery and the common facial vein. Finally, cricopharyngeal myotomy was performed in all patients for the prevention of postoperative stenosis/dysphagia.
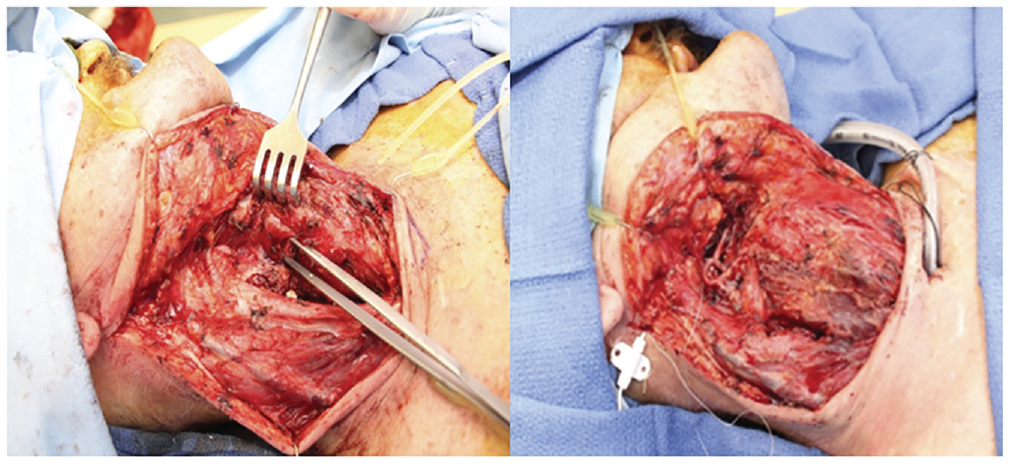
The 1 × 1–cm defect in the posterior esophagus, superior to cricopharyngeus, is indicated by the pick-ups. The vastus lateralis flap encircles the esophagus in an onlay fashion.
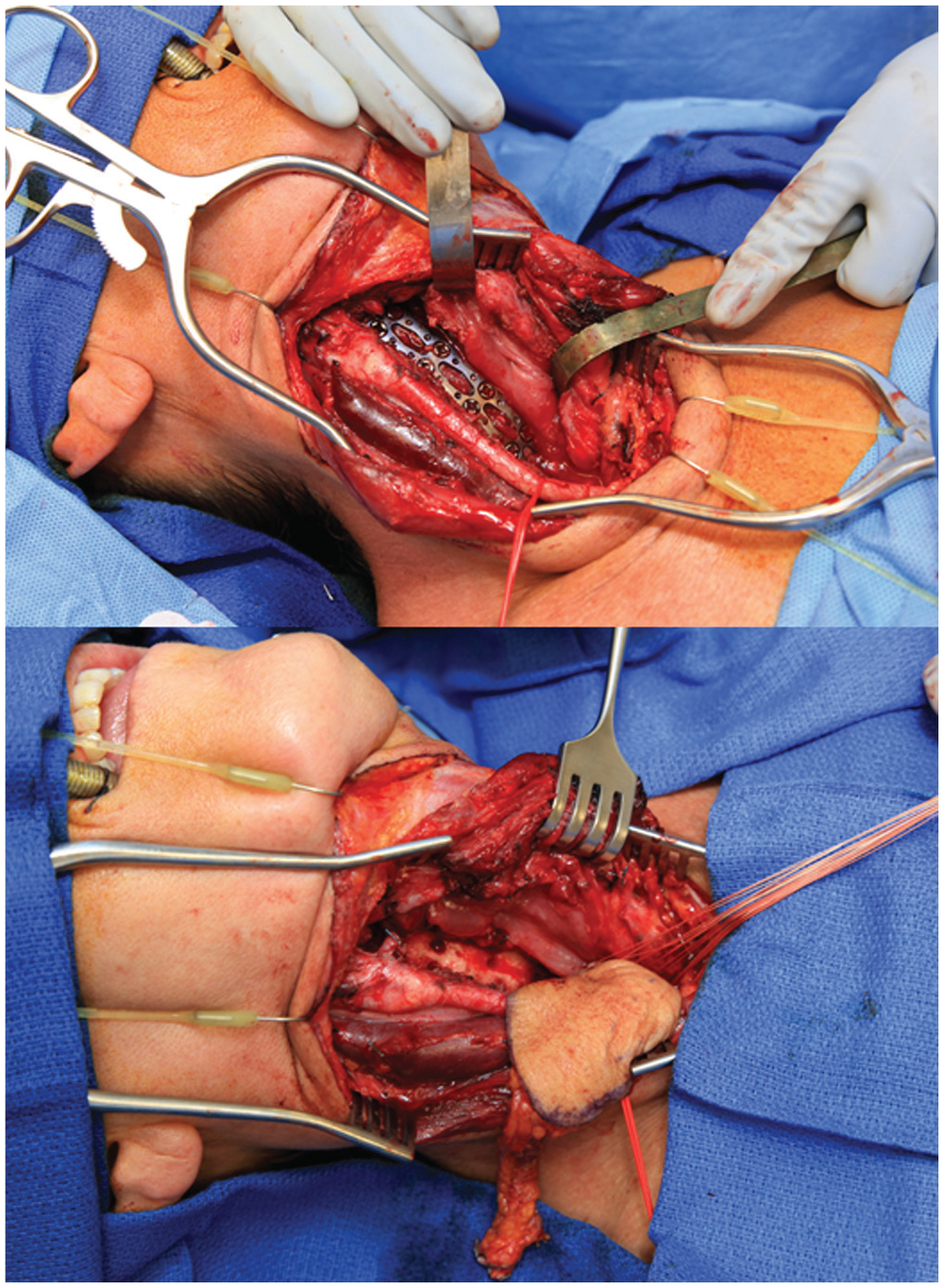
Esophageal defect measures 11 × 5–cm with visible anterior cervical spine hardware. An interpositional radial forearm free flap is inset beginning at the inferior aspect of the defect and proceeding superiorly.
For harvesting the VLOG (n = 4), the flap is based on the descending branch of the lateral femoral circumflex. Cutaneous perforating vessels are ligated as no cutaneous portion is included in the VLOG, as previously described. 18 In the reconstruction of small esophageal perforations (≤2 cm) where the mucosa can be closed primarily, the VLOG acts as a vascularized interposition between the esophageal perforation and the cervical spine. The muscle is secured with tacking sutures to the paraspinal musculature of the neck as well as anteriorly around the esophageal perforation ( Figure 1 ).
For the performance of FC-RFFF (n = 1), the flap is harvested through a standard technique incorporating the anterior perforating vein via the median cubital and cephalic veins into the pedicle, thereby including superficial and deep venous systems in a single venous anastomosis. 19 The flap is oriented such that the proximal pedicle is directed superolaterally in the direction of the prepared cervical recipient vessels ( Figure 2 ).
In all cases, a spine surgeon was available and assisted in pre- and intraoperative decision making for the management of the cervical spine and the associated hardware to ensure maintained stability.
Results
The site of the perforation defect ranged from the hypopharynx to the cervical esophagus ( Table 1 ). VLOG (n = 4) was utilized in small perforations (≤2 cm), while FC-RFFF (n = 1) was utilized for a large hypopharyngeal mucosal defect (11 × 5 cm) not amenable to primary mucosal closure. In all cases, removal of the offending cervical hardware and pharyngoesophageal reconstruction was performed in the same setting. One patient required additional hardware for spine stabilization, which was performed in a separate staged procedure. This patient required C4-C7 anterior fixation and extension of posterior fixation from C5-C6 to C3-C7 due to pseudoarthrosis, likely secondary to chronic infection from the esophageal perforation. The remaining patients had mature fusion at the time of hardware removal and required no additional hardware placement.
The mean operative time was 6.2 hours and the mean ischemia time was 92 minutes. Postoperatively, the mean length of stay was 6.6 days ( Table 1 ). All patients had a percutaneous endoscopic gastrostomy tube placed pre-, intra-, or postoperatively to facilitate administration of enteral nutrition while bypassing the site of perforation during healing, and all were placed on dual proton pump inhibitor and antihistamine blocker for reflux prophylaxis. Additionally, all patients received a cricopharyngeal myotomy at the time of repair to prevent esophageal stenosis/dysphagia and aid in the resumption of an oral diet.
While severity and duration of postoperative dysphagia varied, all patients experienced aspiration (n = 3) or penetration (n = 2) on initial postoperative videofluoroscopic swallow study (VFSS), and all eventually progressed to a normal oral diet. Diet advancement was based on rehabilitative progress as assessed via VFSS by speech-language pathologists. Of 5 patients, 4 showed no evidence of a leak on the initial postoperative VFSS. The time to resumption of an oral diet ranged from 15 to 204 days, with a median 17 days and a mean 80.8 days, exhibiting a bimodal distribution. The patient with the longest time to resumption of an oral diet had a postoperative course that was complicated by a persistent fistula that closed at 6 months postoperatively following conservative treatment. No instances of new-onset vocal cord paralysis were encountered in this patient population. Of 5 patients, 3 underwent tracheostomy at the onset of the surgical case for definitive perforation repair as part of management for airway protection due to intractable aspiration. All eventually underwent decannulation following demonstration of functional swallowing without aspiration (mean, 81.3 days). No significant donor site morbidity or flap failure was encountered in the study.
Representative Cases
A 73-year-old woman with a paraesophageal abscess adjacent to her anterior cervical hardware ( Figure 3 ) was taken to the operating room for management of her cervical spine and repair of suspected esophageal perforation. She had experienced prolonged dysphagia since her initial spinal surgery 2 years prior. In the operating room, a perforation was identified in conjunction with frank purulence and mobile spinal hardware. After hardware removal and irrigation, primary closure of the defect was followed by reinforcement with VLOG as indicated in Figure 1 . A gastrostomy tube was placed to facilitate the restricted oral feeding in the postoperative setting. The patient’s postoperative course was uncomplicated, with return to oral diet at 17 days postoperatively in concordance with the recommendation of a speech pathologist, following VFSS that demonstrated no evidence of leak ( Figure 4 ).
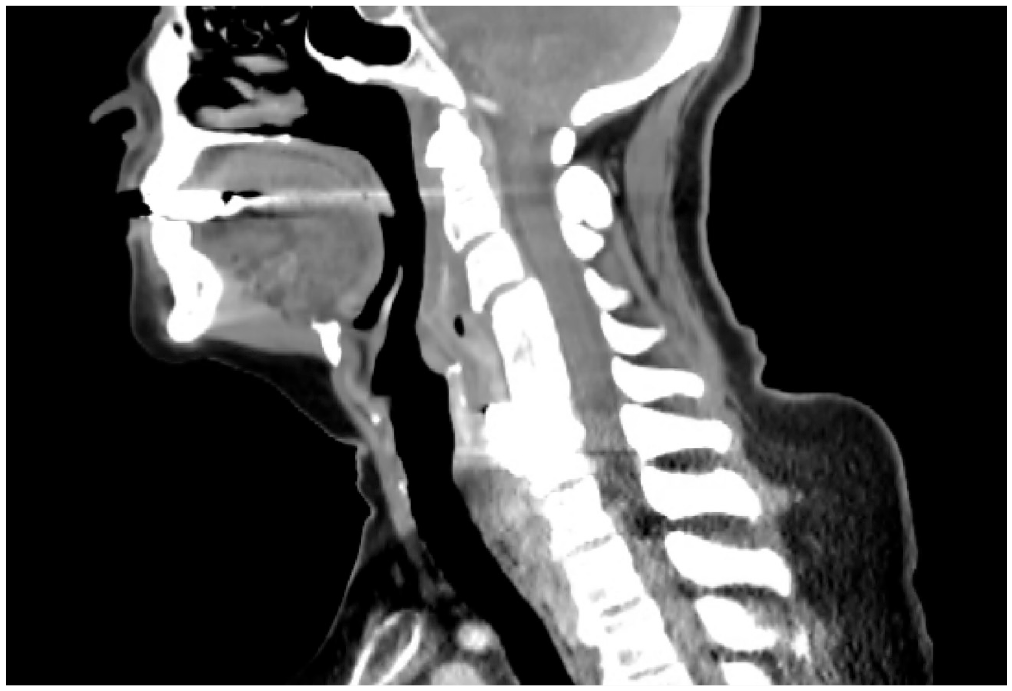
Preoperative computed tomography imaging displays prevertebral free air, indicating paraesophageal abscess.

Postoperative videofluoroscopic swallow study indicates durable repair with no extravasation of contrast medium.
A 57-year-old woman was referred for suspected esophageal perforation discovered with computed tomography imaging of the neck following a 7-year history of dysphagia that began after her initial neurosurgical intervention ( Figure 5 ). The patient was taken to the operating room, where a large esophageal mucosal defect was appreciated. Following hardware removal and fistulous tract excision, an FC-RFFF was harvested and inset in an interpositional fashion ( Figure 2 ). The patient received a gastrostomy tube for enteral feeding in the postoperative period, until sufficient healing could occur. The patient’s postoperative course was uncomplicated and led to the resumption of an oral diet on postoperative day 16, following demonstration of an absence of esophageal leak on VFSS ( Figure 6 ).
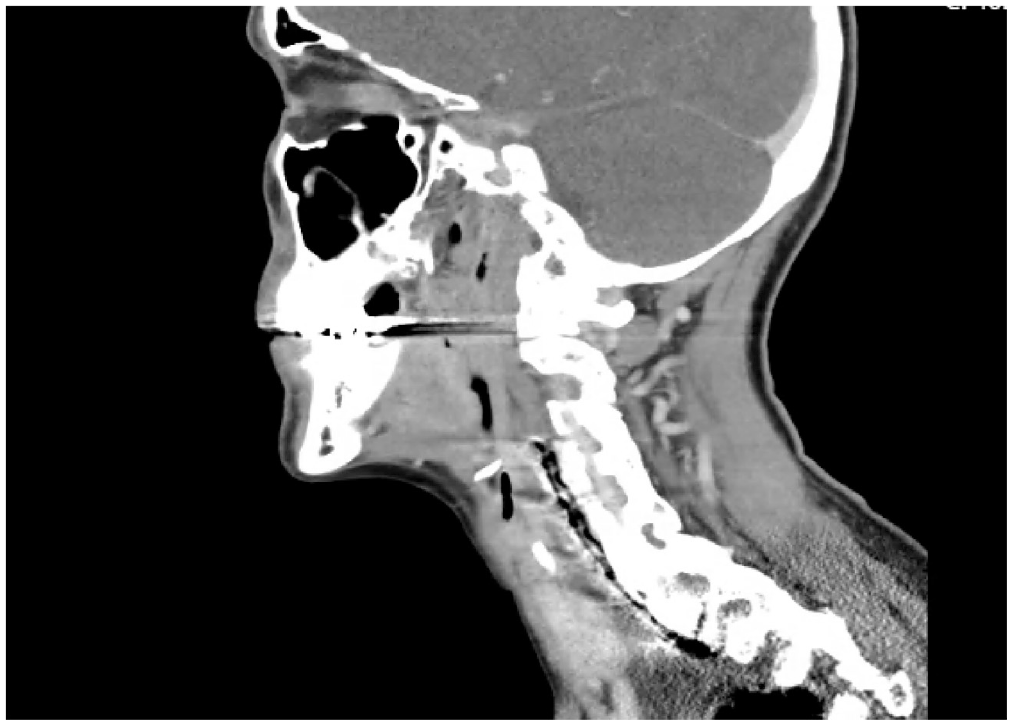
Preoperative computed tomography imaging shows a large volume of prevertebral air and large tract extending inferiorly in the neck.
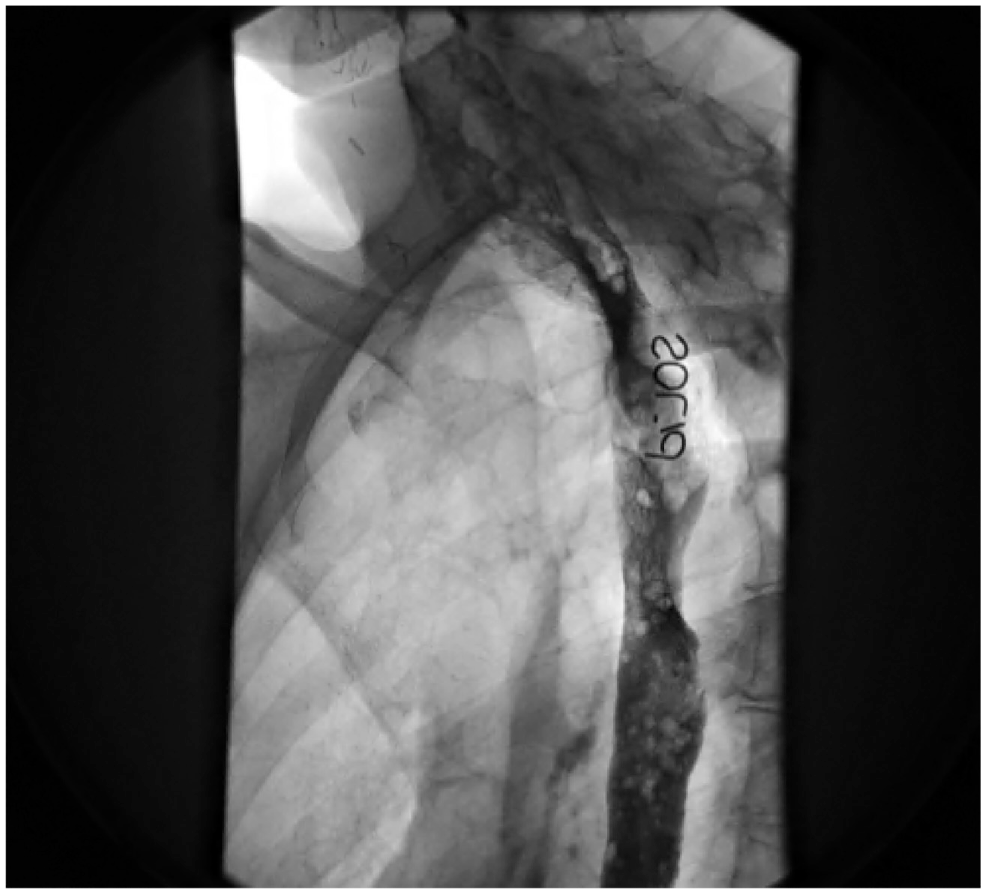
Postoperative videofluoroscopic swallow study displays no extravasation of contrast medium, indicating no leak following fasciocutaneous radial forearm free flap.
Discussion
The optimal surgical management for the repair of esophageal perforation is debatable in the literature. Due to the rarity of its occurrence, most studies contain small sample sizes, thus preventing the development of an evidence-based treatment algorithm for this challenging complication. Several studies have advocated for the utilization of locoregional flaps, predominantly the sternocleidomastoid muscle rotation flap (SCMRF) and pectoralis major myofascial flap, with demonstrated success in small cohorts.15,20 However, SCMRFs are known to have a tenuous and somewhat unpredictable segmental blood supply with a Mathes and Nahai class IV pattern. 21 Furthermore, the middle segment of the muscle is usually supplied by the superior thyroid artery, which is commonly ligated as part of a standard anterior cervical discectomy and fusion approach. 22 The flap also has limited reach and volume of available muscle for defect coverage, all of which are theoretical limitations. In combination, these factors diminish the utility of the SCMRF as a stand-alone reconstructive option. Pectoralis major myofascial flaps were the workhorse of head and neck reconstruction, but excessive bulk, limited reach, and significant donor site morbidity resulted in selective utilization of this option following the successful development and implementation of free tissue transfer. 15 The supraclavicular artery island flap (SCAIF) has recently been described as a possible reconstructive option for these defects. 23 However, Gibson et al noted that the vascular pedicle cannot necessarily be relied on, as previous neck surgery may have compromised these structures. In addition, Kokot et al found the SCAIF to be best suited to cutaneous defects due to a significantly higher rate of complications observed in the utilization of SCAIF for mucosal defect repair in comparison with other reconstructive options. 24 The fasciocutaneous omental free flap is a robust reconstructive option that circumvents the potential complications of locoregional flaps. However, omental free flaps require a complex multiteam harvest with significant donor site morbidity associated with entering the abdomen. Anterior lateral thigh free flaps have been scarcely reported in the literature for this indication. Because of associated flap bulk, they often require modification from the traditional fasciocutaneous harvest (predominantly in the form of adipofascial harvest), which can be technically challenging and, depending on patient habitus, still result in significant flap bulk for a posterior esophageal repair.16,25
For smaller esophageal defects (<2 cm), we believe that the best available reconstructive option consists of the VLOG. VLOG harvest is technically straightforward as it requires only pedicle dissection of the descending branch of the lateral femoral circumflex. As no skin paddle is harvested, no perforator dissection is necessary, and the leg can easily be closed primarily. The muscle volume harvested can be safely modified as necessary for adequate coverage of the defect without unnecessary bulk, and pedicle length is abundant. Donor site morbidity is significantly decreased in comparison with previously mentioned reconstructive options, and the patient is encouraged to begin ambulating the following day.
For large mucosal defects where the esophageal mucosa cannot be primarily closed, we believe that utilization of thin and pliable flap, such as the FC-RFFF, is an excellent reconstructive option. The thin pliable nature of the FC-RFFF is desirable for posterior esophageal reconstruction as it contours to the defect nicely without associated flap bulk, which may place the patient at risk for postoperative dysphagia. Flap harvest is also well known to be technically straightforward with consistent anatomy. The morbidity of the radial forearm donor site is well tolerated and relatively small in comparison with the aforementioned reconstructive options.
Although the small size of our study population certainly limits statistical power and thus prohibits arrival at a definitive conclusion, all 5 repairs within our population were functionally successful. The decision to begin an oral diet was made in consultation with the speech-language pathologists, who provide continued dietary rehabilitation to these patients. Not surprising, the first 2 patients treated within our population had the longest time to resumption of oral diet (204 and 152 days), with the other 3 patients averaging 16 days until resumption following our increased familiarity with the management of this complication. Time to resumption of oral diet was likely affected by the wound-healing capabilities of each patient, patient compliance with nothing-by-mouth status, and disordered pharyngeal motility, as evidenced by aspiration in 3 patients with available preoperative studies. These 3 patients include the one with the largest mucosal defect, who underwent FC-RFFF for repair and resumed a regular oral diet on postoperative day 16. Additional consideration should be given to patient-related factors, as 3 of 5 were current smokers and 1 was a previous smoker, which is a known wound-healing risk factor.26,27 Despite this, all patients achieved perforation repair with the restoration of functional swallowing at time of last follow-up visit.
We recognize that our sample size is small and that other viable reconstructive options exist, preventing the development of an evidence-based treatment algorithm. While beyond this scope of this study, more conservative measures of repair warrant consideration in populations that are not amenable to locoregional flaps or free tissue transfer. Such measures, including T-tube cervical esophagostomy with esophageal exclusion, have been reported to result in reasonable outcomes. 28 Despite these limitations, our experience with these 5 cases supports that VLOG and FC-RFFF warrant legitimate consideration in the management of hardware-related esophageal perforations, provided that a microvascular surgeon is available. We believe that locoregional flaps may be reserved as a backup reconstructive option for patients who are not candidates for free tissue transfer or are presenting in limited-resource settings, similar to the flaps’ current role in oncologic head and neck reconstruction. 29 Furthermore, large-volume studies are needed to more clearly delineate the optimal reconstructive algorithm for treatment chronic esophageal perforations.
Conclusion
VLOG and FC-RFFF are robust, relatively low-morbidity interventions that merit consideration for definitive repair of chronic esophageal perforation for this serious and challenging complication. Repair should always be undertaken in concert with a spine surgeon for management of the cervical spine and associated hardware.
Author Contributions
Disclosures
Footnotes
This article was presented at the Southern Neurosurgical Society Annual Meeting; February 20-23, 2019; Key Largo, Florida.
