Abstract
Objective
To better understand the impact of the otolaryngology-specific workforce on the burden of related diseases.
Study Design
Retrospective analysis of existing workforce density data as compared with the incidence, mortality, and morbidity data for 4 otolaryngologic diseases.
Setting
An overall 138 countries with known otolaryngology–head and neck surgery workforce and epidemiologic data.
Methods
We obtained raw data on workforce estimates of ear, nose, and throat surgical specialists from the World Health Organization. Disease burdens for 4 conditions were estimated via 2 ratios, the mortality:incidence ratio (MIR) and YLD:incidence ratio (years lost to disability), as specified in the Global Burden of Disease database. These were correlated to country-specific otolaryngologist density data in univariate and multivariate analyses.
Results
Increased density of the ear, nose, and throat workforce correlated with better outcomes for otolaryngologic-treated surgical diseases. A 10% increase in otolaryngology workforce density was associated with a 0.27% reduction in YLD:incidence ratio for chronic otitis media, a 0.94% reduction in MIR for lip and oral cavity cancer, a 1.46% reduction in MIR for laryngeal cancer, and a 1.34% reduction in MIR for pharyngeal cancer (all P < .001)—an effect that remained after adjustment for health systems factors for all conditions but chronic otitis media.
Conclusion
The density of the surgical workforce is assumed to affect disease outcomes, but ours is the first analysis to show that increased workforce density for a specific surgical specialty correlates with improved disease outcomes. While there is a consensus to increase access to health care providers, quantifying the effect on disease outcomes is an important metric for those performing health economics modeling, particularly where resources are limited.
Keywords
Globally an estimated 4.8 billion people lack access to essential surgical care,1-3 and as of 2010, an estimated 16.9 million lives worldwide (a third of all deaths) were lost from conditions needing surgical care. 4 Key constituents of a functioning system for surgical care have been identified as timely access, financial risk protection, safe anesthesia, and an adequate surgical workforce.1,2 Arguably the most critical of these is the last: even if all other constituents are optimal, care cannot be delivered without an adequately trained workforce.
The availability and density of the surgical workforce are assumed to affect outcomes of surgical diseases, but at present there is little evidence to quantify this effect. Previous studies reported that a composite measure of the density of a surgical, anesthesia, and obstetric workforce correlated with lower maternal mortality5,6 and with improved outcomes for head and neck cancer, 7 but the data were from only a few countries where such data were available and without information on the specific skills or expertise of that workforce.
Members of the World Health Organization’s Program for the Prevention of Deafness and Hearing Loss recently published a detailed and extensive global estimate of the number and density of ear, nose, and throat (ENT) surgeons (also known as otolaryngology and head and neck surgeons). 8 We utilized that data set to investigate whether the density of the otolaryngology workforce correlates to outcomes of otolaryngological disorders amenable to surgical treatment, specifically those recorded by the Global Burden of Disease (GBD) 9 : chronic otitis media, lip and oral cavity cancer, laryngeal cancer, and pharyngeal cancer.
Methods
Country-Level Data on the ENT Workforce
This study was deemed to be Institutional Review Board exempt by the University of California San Francisco, given its use of open access country-level epidemiologic data. We obtained country-specific raw data on workforce estimates of ENT surgical specialists from the authors of the recent World Health Organization publication on this topic. 8 Those authors derived their data from a review of published literature, supplemented with data from several regional, national, and international surveys that they designed and distributed. Workforce density was expressed as number of specialists per 100,000 population, and we adapted this same metric. 8
Country-Level Data on the Frequency and Outcomes of Relevant Disease
We selected 4 ENT disorders commonly treated with surgery as described in the 2017 GBD database 7 : chronic otitis media, lip and oral cavity cancer, laryngeal cancer, and pharyngeal cancer (excluding nasopharyngeal cancer). We extracted estimates of the incidence, prevalence, mortality, and years lost to disability (YLD) for each of the 4 disorders. We used morbidity or mortality as an indicator of disease outcome, adjusted for disease incidence. This frequency measure was chosen rather than the overall prevalence of the disease in question to better capture incident cases as they arose and potentially required surgical intervention. This has been shown to better identify the surgical workforce’s impact on disease outcome. 7 Specifically, the morbidity outcome from chronic otitis media was defined as the YLD:incidence ratio (YLD-IR). Mortality outcomes from laryngeal, oral cavity, or pharyngeal cancer were defined as the mortality:incidence ratio (MIR), a measure previously used for international comparison of cancer survival.7,10-12
Comparison of Workforce Data With Frequency and Outcomes of Disease
We log-transformed country-level ENT workforce density to improve the linearity of the relationship between workforce density and disease indicator. We then plotted these log-transformed data against each indicator of disease outcome for the 4 ENT disorders of interest. Plots included representation of disease frequency and country income level as point size and color, respectively. We used World Bank 2019 definitions to define and label countries in our plots as high, middle, or low income. 13 For each analysis we plotted a line of best fit and calculated a correlation coefficient. The disease outcome measures were then compared by income level with analysis of variance. Each income level was compared and significance determined after a Bonferroni correction for multiple comparisons. Results were normalized to the value for high-income countries.
In multivariate analysis of the relationship between workforce and disease outcomes, we report unadjusted and adjusted estimates with covariates of surgical system capacity. As potential risk factors for each disease would affect disease incidence and as this was already incorporated into the morbidity outcome measure, we did not include risk factor covariates in the model (ie, alcohol or tobacco use for the malignant disease processes). Rather, we corrected for health systems covariates that could affect disease outcome after incident cases occurred—namely, country-specific measures of gross domestic product (GDP), health expenditure by country, and hospital beds per capita, as reported in 2017 GBD data. 9 Results were summarized as the percentage change in disease outcome with a 10% increase in density of ENT workforce. An a priori alpha of 0.05 was chosen for the significance level. All statistical analyses were performed with Stata/IC 16.1 (StataCorp LLC).
Results
Disease burden was analyzed for the 138 countries for which ENT workforce data were available. There was a notable difference in disease burden by country-level income. This difference was significant on univariate analysis for all 4 diseases studied (P < .001), as seen in Table 1 . The significance remained after Bonferroni correction for all income-level comparisons except chronic otitis media, for which there was no difference in outcome between middle- and low-income countries (P = .079). For each condition, the incidence-adjusted disease outcome measure was highest in low-income countries and lowest in high-income countries. This trend was most exemplified by the malignant conditions. The MIR was considerably higher in low-income countries, ranging from 62% higher on average for lip and oral cavity cancer to more than double (108% higher) for laryngeal cancer.
Burden of Disease by World Bank Income Level vs High-Income Countries. a
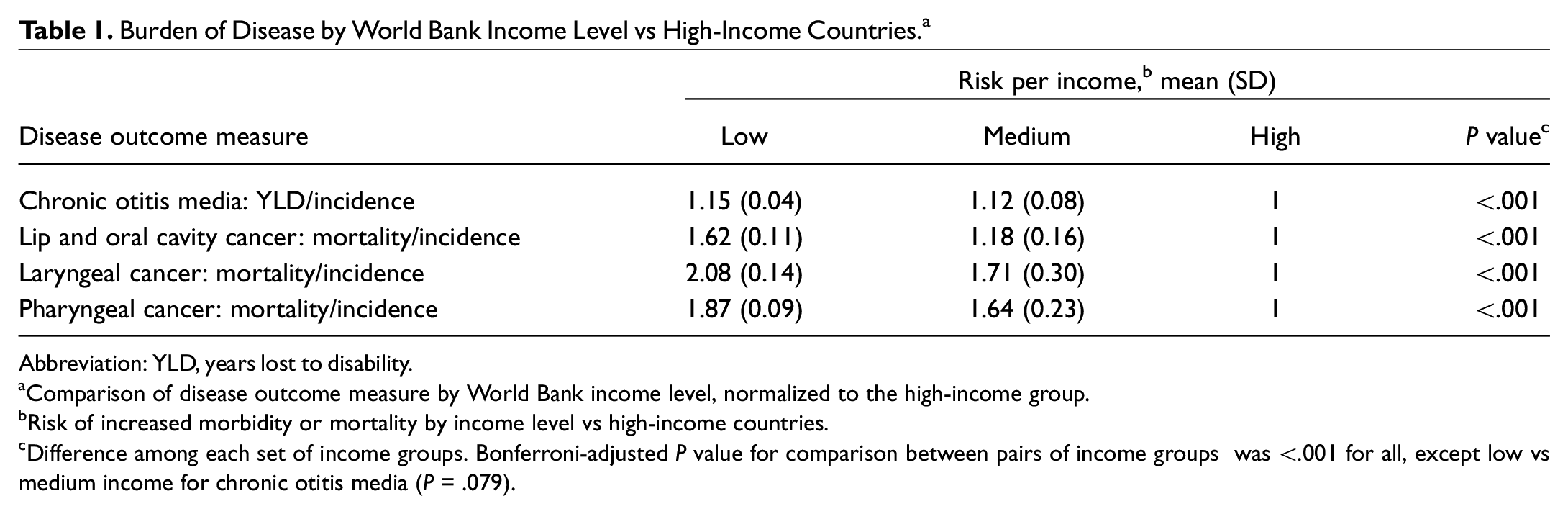
Abbreviation: YLD, years lost to disability.
Comparison of disease outcome measure by World Bank income level, normalized to the high-income group.
Risk of increased morbidity or mortality by income level vs high-income countries.
Difference among each set of income groups. Bonferroni-adjusted P value for comparison between pairs of income groups was <.001 for all, except low vs medium income for chronic otitis media (P = .079).
Figure 1 shows the disease burden measures plotted against the log-transformed ear nose and throat density data for the 4 selected diseases. Improved outcomes for chronic otitis media, lip and oral cavity cancer, laryngeal cancer, and pharyngeal cancer all correlated with an increasing density of ENT workforce (R 2 = –0.54, –0.68, –0.76, –0.72, respectively). Correlations clustered by income status, with lower-income countries having higher burden of disease, worse disease outcomes (MIR or YLD-IR), as well as lower workforce density.
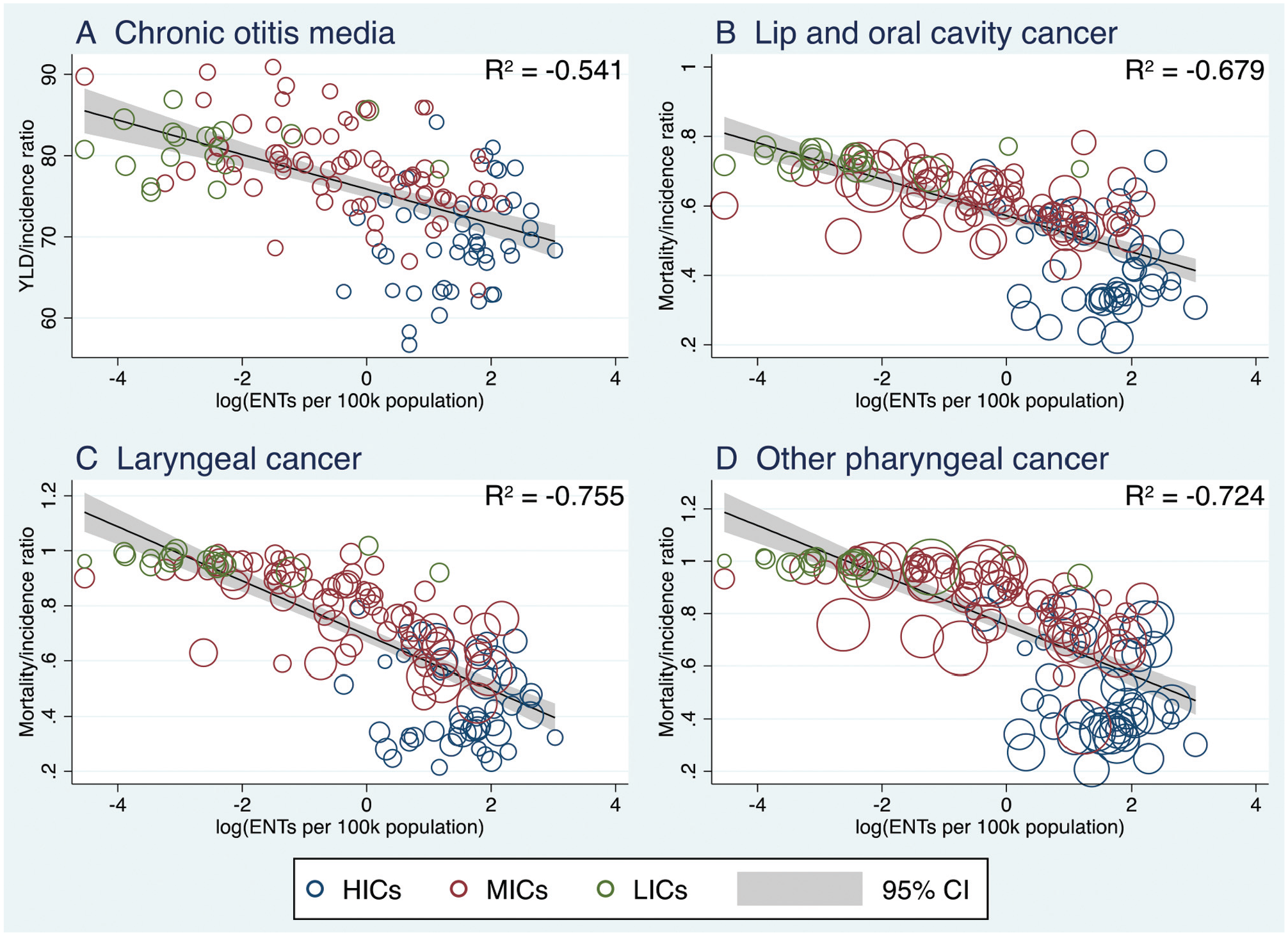
Improved outcomes for ENT-specific pathologies correlated to density of the ENT surgical workforce. Bubble size corresponds to disease incidence, and bubble color represents World Bank classification of high, middle, or low income (HIC, MIC, or LIC). ENT, ear, nose, and throat.
Table 2 presents measures of correlation between ENT workforce density and disease outcomes, before and after adjustment for covariates (GDP, health expenditure, and hospital beds per capita). In summary, a 10% increase in otolaryngology workforce density was associated with an unadjusted 0.27% reduction in YLD-IR for chronic otitis media, 0.94% reduction in MIR for lip and oral cavity cancer, 1.46% reduction in MIR for laryngeal cancer, and 1.34% reduction in MIR for pharyngeal cancer (all P < .001). In all instances, the size of that effect was mitigated by adjustment for covariates but remained statistically significant (all P < .005), except in the case of chronic otitis media (P = .089). For all regressions, there was no evidence of nonlinearity, nonlinearity of residuals, or collinearity of covariates, suggesting that P values were valid and that coefficient estimates were unbiased. This indicates that ENT workforce density is potentially an independent predictor of the outcomes of interest.
Correlation of Otolaryngology Workforce Density With Disease Outcomes, Adjusted for Health System Modifiers.
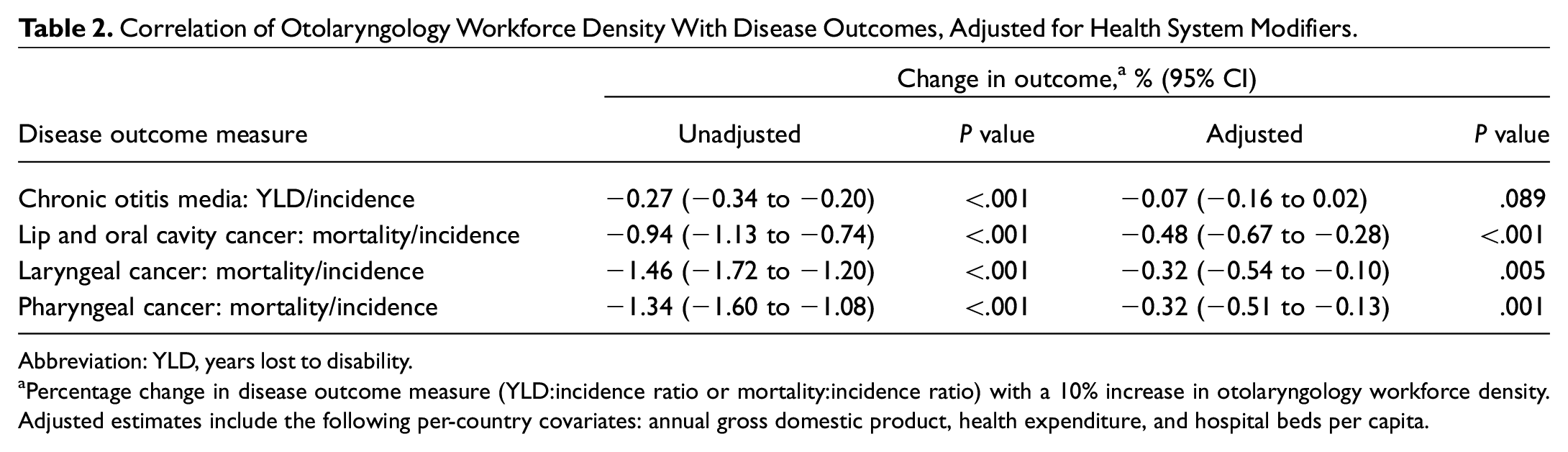
Abbreviation: YLD, years lost to disability.
Percentage change in disease outcome measure (YLD:incidence ratio or mortality:incidence ratio) with a 10% increase in otolaryngology workforce density. Adjusted estimates include the following per-country covariates: annual gross domestic product, health expenditure, and hospital beds per capita.
Discussion
Ours is one of the first studies to correlate outcomes of disease with density of the related health workforce. Our 4 index ENT surgical procedures were chronic otitis media (where the operation of tympanoplasty will usually stop infective ear discharge and may improve hearing) 14 and lip, oral cavity, laryngeal, and pharyngeal cancer (where treatment is often based on surgical excision and, in advanced cases, adjuvant chemo/radiotherapy). 15 This is also why we excluded nasopharyngeal cancer from our analysis, as this disease is commonly treated with radiation and other nonsurgical means. ENT workforce density was clearly and significantly clustered by country income level, with the MIR more than doubling between high- and low-income countries for laryngeal cancer. No malignancy had less than a 62% increase in MIR in low- vs high-income countries. This disparity indicates that the lack of ENT specialty surgical care is most noticeably felt in countries and by citizens that have fewer resources with which to make up for this shortage. In our unadjusted regression analysis, improved outcomes for each condition correlated with an increased density of the ENT workforce. Adjustment for other markers of health system capacity—including health care expenditure (a marker of state funding of care), GDP (a marker of potential self-financing of care), and hospital beds (a marker of physical infrastructure to provide care)—moderated the size of the effect of the ENT workforce on outcomes, but for all head and neck cancers the effect remained statistically significant. This demonstrates that even after attempted correction for other health systems variables, the ENT workforce is a significant predictor of improved outcomes for various surgically treated ENT conditions. This corroborates prior studies that indicated that the surgical workforce is crucial: although this requires support from the health care system, it may represent an argument to increasing the density of providers.16,17
The main strength of our study is that it is the first to use data on a subspecialist workforce and correlate those to subspecialist disease outcomes. Whereas measuring and analyzing the total number of surgeons in a country has value, outcomes of surgical disease are related to experience and expertise in managing specific diseases—for example, it would be less appropriate to correlate the total number of surgeons to outcomes for tympanoplasty, an operation that requires specialized training and equipment. 18 No other data sets have enabled such analysis. A 2020 study also reported that a lower MIR for head and neck cancer correlated with a greater density of providers, but it used data on a general rather than specific workforce. 7 A previous study estimated the number of neurosurgeons across the globe, 19 but it is difficult to correlate that to outcomes because we have only indirect estimates of the global incidence of neurosurgical diseases such as traumatic brain injury. 20
We acknowledge limitations to our study. The epidemiologic data underlying our analysis will have inaccuracies or in some places be incomplete, but this is more likely to lead to failure to find an association where one exists (type 1 error) rather than a false discovery. Our model cannot account for components of availability or access to care for which we have sparse or no data—for example, specialist equipment such as microscopes for tympanoplasty 21 or radiotherapy 22 or specialist perioperative care for head and neck cancer; likewise, we cannot account for patient-side barriers, such as physical access or fear of the hospital. 23 Again, our inability to incorporate these components is more likely to moderate any correlation rather than lead to false discovery and underestimate size of the effect of workforce density on outcomes for the diseases examined. ENT workforce density is just one of the many factors that may affect patient outcomes. While cancer care especially is multidisciplinary—including medical oncologists, radiation oncologists, pathologists, and radiologists, among others—this study analyzes only the effect of ENT surgical providers on disease outcome. However, we proposed to account for this by choosing conditions that are primarily treated with surgery, though we realize that no surgical treatment exists in a vacuum without other providers. Although we included hospital beds as a proxy of infrastructure, this does not necessarily correlate well with operative capacity or ability of otolaryngologic services to provide surgical or inpatient care. As each of these factors is likely to decrease the ability of our model to detect an association between ENT density and disease outcome, our significant findings (despite the lack of ability to correct for these factors) provides compelling evidence that availability of ENT care is an essential factor to reducing disease burden.
As we obtain more and improved data on global human resources for health, it will be important for the academic community to correlate those to outcomes with their related diseases. Whereas it may be self-evident that we need to invest in a workforce for delivering health, 24 quantifying the effect of such investment on outcomes is an important metric for those performing health economics modeling or those deciding on health policy or financing, particularly where resources are limited. Other mechanisms of increasing or redistributing workforce, such as an expansion of telemedicine services or more robust educational partnerships between low/middle- and high-income surgeons, may help to address some of this burden and could be a future area of research.
Conclusion
ENT specialty workforce density has a significant impact on disease outcomes for chronic otitis media, lip and oral cavity cancer, laryngeal cancer, and pharyngeal cancer. This association is maintained for the studied malignant conditions even when markers of health system capacity are taken into account.
Footnotes
Acknowledgements
This article is submitted on behalf of the research group Global Otolaryngology/Head and Neck Surgery Initiative.
This article was presented at the AAO-HNSF 2021 Annual Meeting & OTO Experience; October 3-6, 2021; Los Angeles, California.
Author Contributions
Disclosures
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
