Abstract
Objective
Juvenile recurrent parotitis (JRP) is a rare disease that may adversely affect normal development and quality of life. The objective of this study was to report on the demographics, characteristics, and treatment outcomes of JRP and to offer evidence-based management recommendations.
Study Design
Retrospective review.
Setting
A single tertiary care pediatric teaching hospital.
Methods
Medical records, imaging studies, and laboratory findings over a 10-year period were retrospectively collected and reviewed, resulting in 41 patients with JRP between the ages of 8 months and 16 years.
Results
Black males aged 2 to 8 years were most commonly affected by JRP. Overall, 18 (44%) patients received ≥3 antibiotics, and 17 (42%) underwent sialendoscopy for treatment. Over 75% of patients had no JRP recurrences after 3 sialendoscopies. The most common imaging approach was computed tomography (42%), and the most frequent laboratory results were elevated amylase (83%) and C-reactive protein (82%). Atopy (61%) and excess weight (42%) were routinely associated with JRP, especially in severe cases.
Conclusion
JRP workup and treatment plans should begin with the least burdening modalities, including over-the-counter analgesics, minimal laboratory studies in the acute phase, and ultrasonography over computed tomography. Clindamycin is an effective initial antibiotic of choice, and severe recurrences may be controlled with sialendoscopy. Optimizing the health of patients with JRP includes managing comorbidities, especially of atopic and overweight origins, which are associated with more severe cases.
Juvenile recurrent parotitis (JRP) is an inflammatory condition of unknown etiology characterized by recurrent episodes of unilateral, or less commonly bilateral, parotid swelling. 1 Since no specific etiology has been widely established, JRP is often a diagnosis of exclusion, based on the clinical history and physical examination, complemented with imaging and laboratory studies. JRP typically begins in children aged 3 to 6 years, affects males more often than females, and is reported to spontaneously resolve around puberty. 2 Therefore, treatment of the condition is primarily focused on symptomatic relief and prevention of recurrent episodes in an effort to preserve long-term salivary gland functions. As universal vaccination progresses, JRP may become the leading cause of salivary disease in children, overtaking mumps infection. 2
While nonfatal, JRP has potential to be a major disruptor of normal childhood development with adverse impact on quality of life. There is a scarcity of information on optimal prevention and management strategies for JRP. Additionally, little is understood regarding the correlation between JRP and concurrent comorbidities, limiting the development of impactful treatment algorithms. In this study, we aim to examine the demographic, medical, and surgical characteristics of JRP to offer evidence-based recommendations to safely and effectively control JRP symptoms, decrease health care expenditure, and reduce unwarranted treatment morbidity.
Methods
Study Population
A retrospective review of pediatric patients from a single tertiary care center was conducted. All patients <18 years of age at LeBonheur Children’s Hospital, Memphis, Tennessee, diagnosed with sialoadenitis between January 1, 2011, and December 31, 2020, were eligible for inclusion in this study. Patients were excluded if any of the following applied: only 1 event of parotitis; subjective reports of recurrence but no documentation in the electronic medical record; complaints regarding the submandibular glands only; sialolithiasis; and history of juvenile Sjögren syndrome, lymphoma, or human immunodeficiency virus and/or mumps infection. Institutional Review Board approval was obtained for this study from the University of Tennessee Health Science Center (18-05816-XP).
Data Collection and Analysis
Charts of pediatric patients with repeated sialoadenitis were reviewed for demographics, imaging and laboratory studies, concurrent disease states, and treatment methods and outcomes. Demographics include sex, race, and age (during every JRP episode). Concurrent disease states were categorized as follows: atopy, overweight/obese, otolaryngologic, endocrinologic, gastrointestinal, psychiatric, hematologic, neurologic, cardiovascular, and developmental. Treatment methods consisted of antibiotics, pain medications, and surgical interventions. Accurate diagnoses were identified via ICD-9/10 codes (International Classification of Diseases, Ninth Revision or Tenth Revision), such as unspecified sialoadenitis (527.2/K11.20), acute sialoadenitis (527.2/K11.21), acute recurrent sialoadenitis (527.2/K11.22), sialolithiasis (527.5/K11.5), and unspecified disease of the salivary glands (527.9/K11.9). The ICD-9/10 codes for sialolithiasis were included for an exhaustive chart search to capture cases of miscoding, but patients with true sialolithiasis were eliminated upon detection. Excel 2016 (Microsoft) was utilized for data organization and representation. Chi-square contingency tables were performed with Prism (version 8.4.3, GraphPad).
Results
Among 752 charts reviewed, 41 met the inclusion and exclusion criteria for this study. The demographic information of the patients with JRP is summarized in Table 1 . Most patients were male (54%) and Black (46%) with an age range of 241 days to 16.9 years. The highest incidence for JRP lies between 2 and 8 years of age (63%), as shown in Figure 1 . Eighteen (44%) patients received ≥3 antibiotics and 17 (42%) underwent surgery. Eight (20%) patients, included in the 2 previous groups, required both therapies to manage their salivary complaints. Patients with severe JRP symptoms requiring surgery and ≥3 antibiotics for treatment had the lowest age at onset (mean ± SD, 4.4 ± 1.5 years) and first recurrence (5.7 ± 2.2 years).
Demographics of Patients With Juvenile Recurrent Parotitis From a Tertiary Care Teaching Hospital Over a 10-Year Period. a
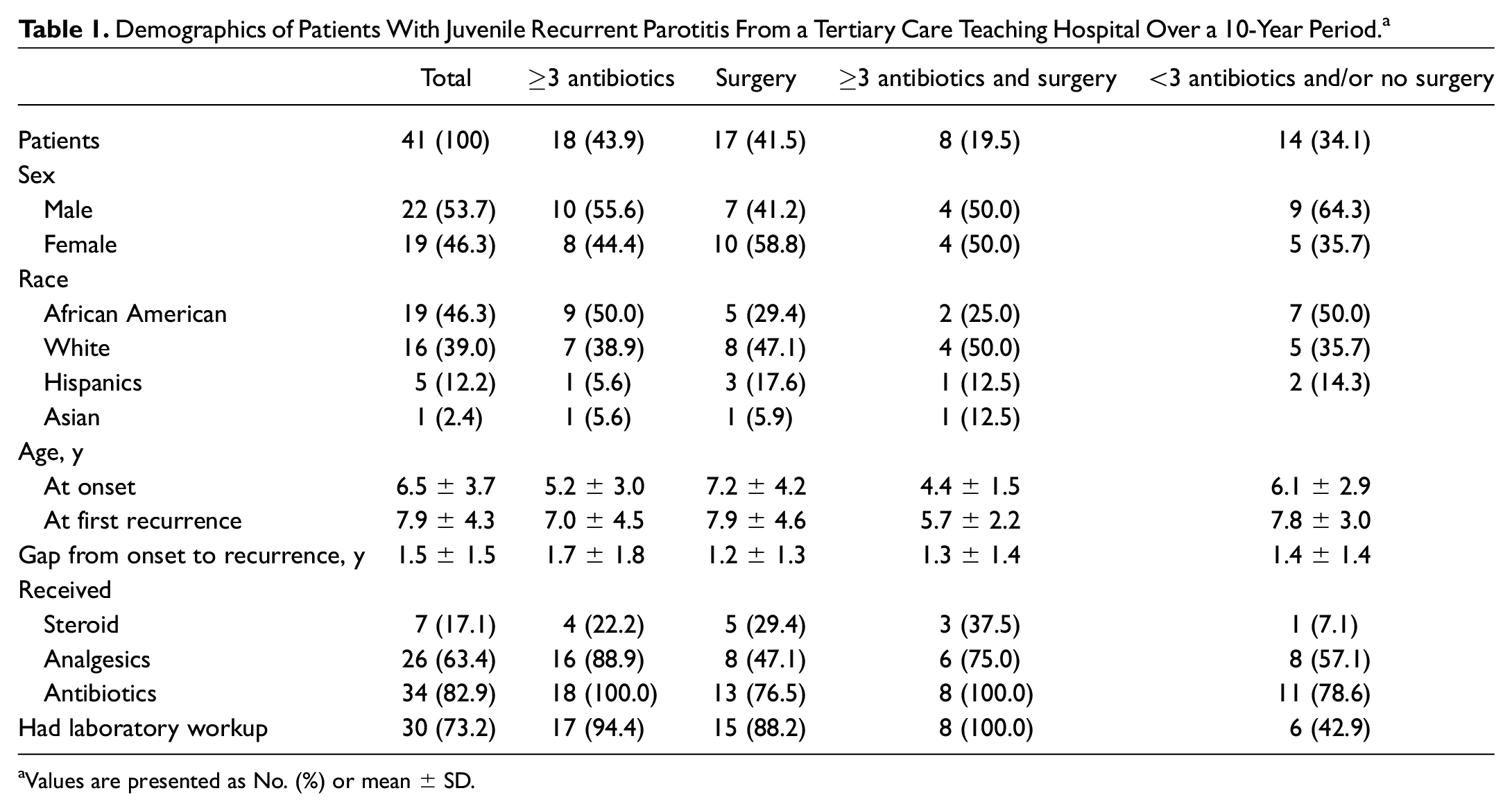
Values are presented as No. (%) or mean ± SD.
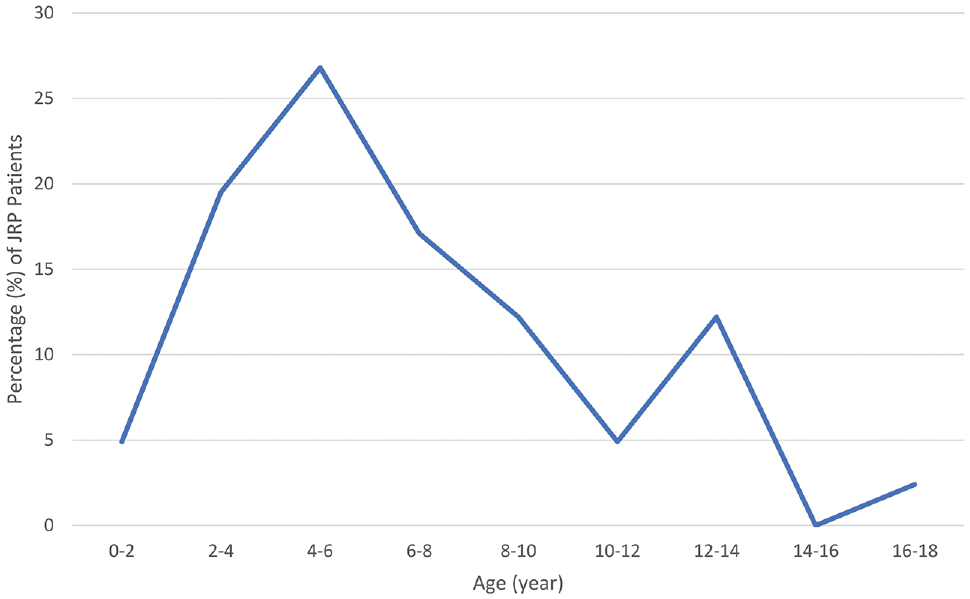
Distribution of onset age for patients with JRP (juvenile recurrent parotitis).
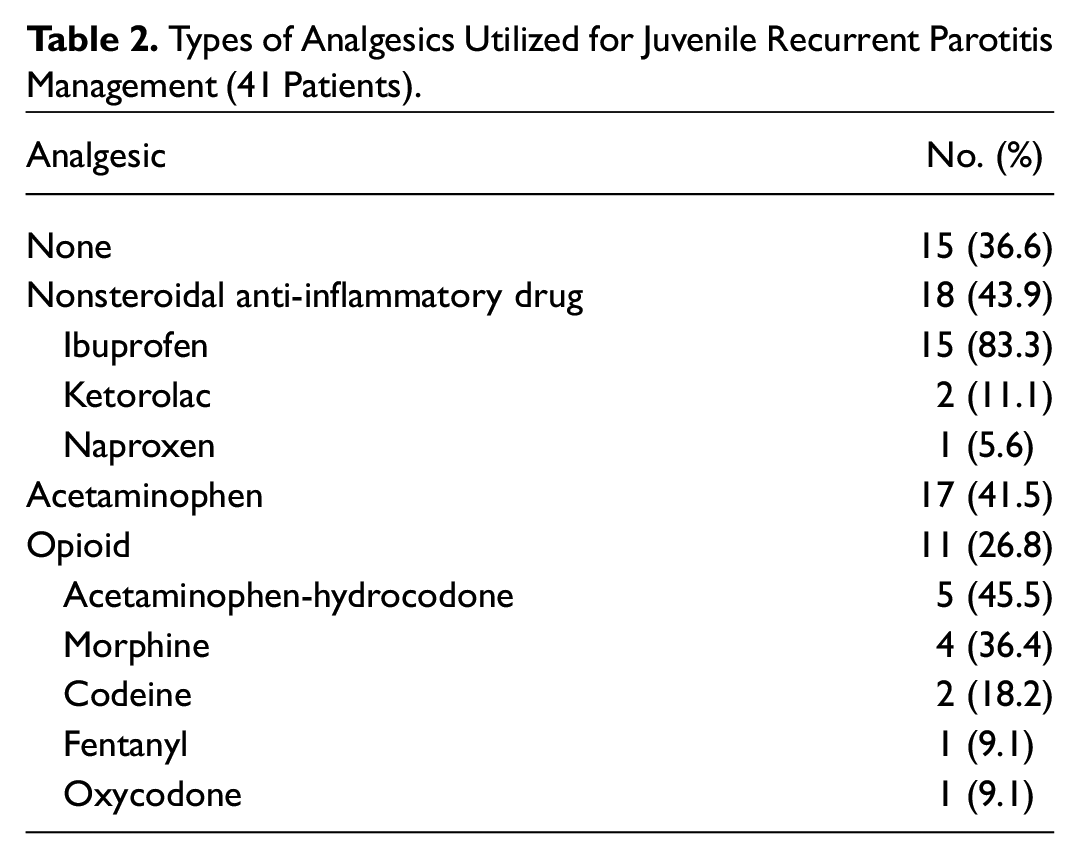
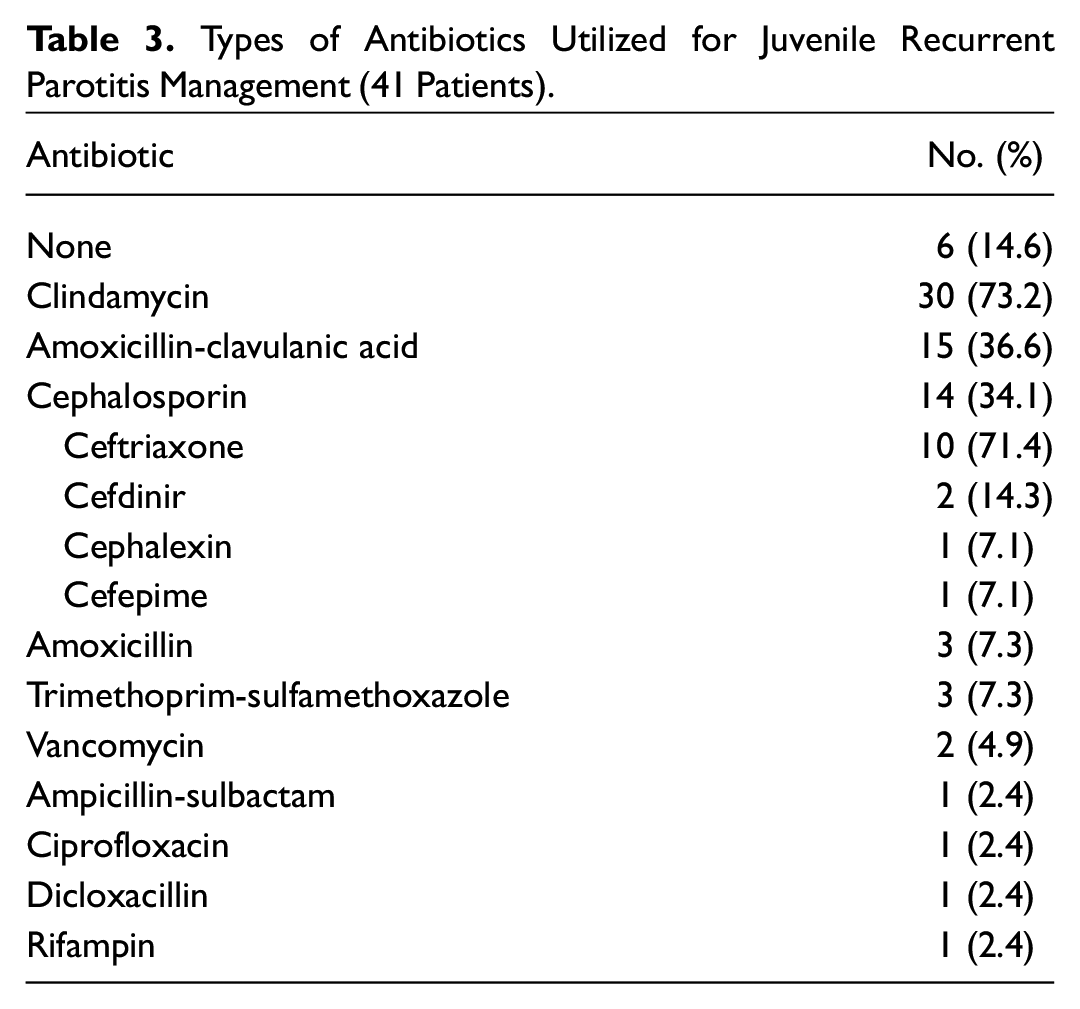
Overall, 17% of patients received steroids, 63% analgesics, and 83% antibiotics for symptomatic management. Details regarding analgesics and antibiotics are listed in Table 2 and Table 3 , respectively. The most common analgesics taken involved some variation of nonsteroidal anti-inflammatory drugs (44%), with ibuprofen being the most common subtype. Additionally, 27% of patients received some form of opioid, of which acetaminophen-hydrocodone was the most regular choice (5/11, 46%). All opioids were provided in the emergency department or during admission in the hospital. Females were more likely to receive pain medication. No differences were noted in race, age, or number of JRP events. Clindamycin (73%) was the most popular antibiotic used, followed by amoxicillin-clavulanic acid (37%) and some form of cephalosporin (34%). Ceftriaxone was the most frequent cephalosporin subtype (10/14, 71.4%). Patients who received ≥3 antibiotics were more likely to be <6 years old (P < .001) and have ≥3 cases of JRP (P < .01). No significant differences were noted in race or sex.
Types of Analgesics Utilized for Juvenile Recurrent Parotitis Management (41 Patients).
Types of Antibiotics Utilized for Juvenile Recurrent Parotitis Management (41 Patients).
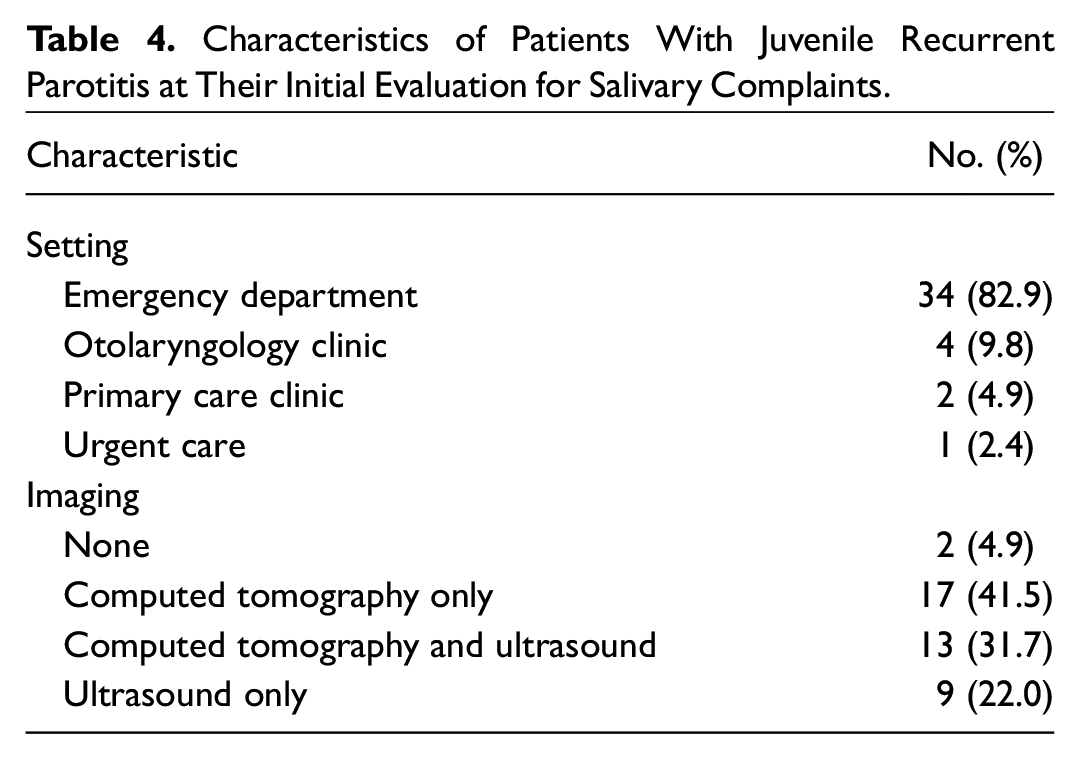
At the initial encounter, 83% of patients with JRP presented to the emergency department. Imaging (95%) and laboratory (73%) studies were regular components of the preliminary workup, as correspondingly summarized in Table 4 and Table 5 . Computed tomography (CT) alone (42%) was the most common imaging approach, while the most frequent laboratory findings were elevated amylase (83%) and C-reactive protein (82%). Sialendoscopy was employed for controlling severe JRP symptoms, with a success rate of 77% after 3 repeats (ie, no further episodes of parotitis). For patients who received sialendoscopy, 3 had CT scans beforehand, 5 received ultrasound, and 6 had both. Table 6 highlights details regarding sialendoscopy for patients with JRP. Patients with at least 3 episodes of JRP were more likely to receive sialendoscopy. No significant differences were noted in race or sex.
Characteristics of Patients With Juvenile Recurrent Parotitis at Their Initial Evaluation for Salivary Complaints.
Laboratory Findings for Patients With Juvenile Recurrent Parotitis (41 Episodes).
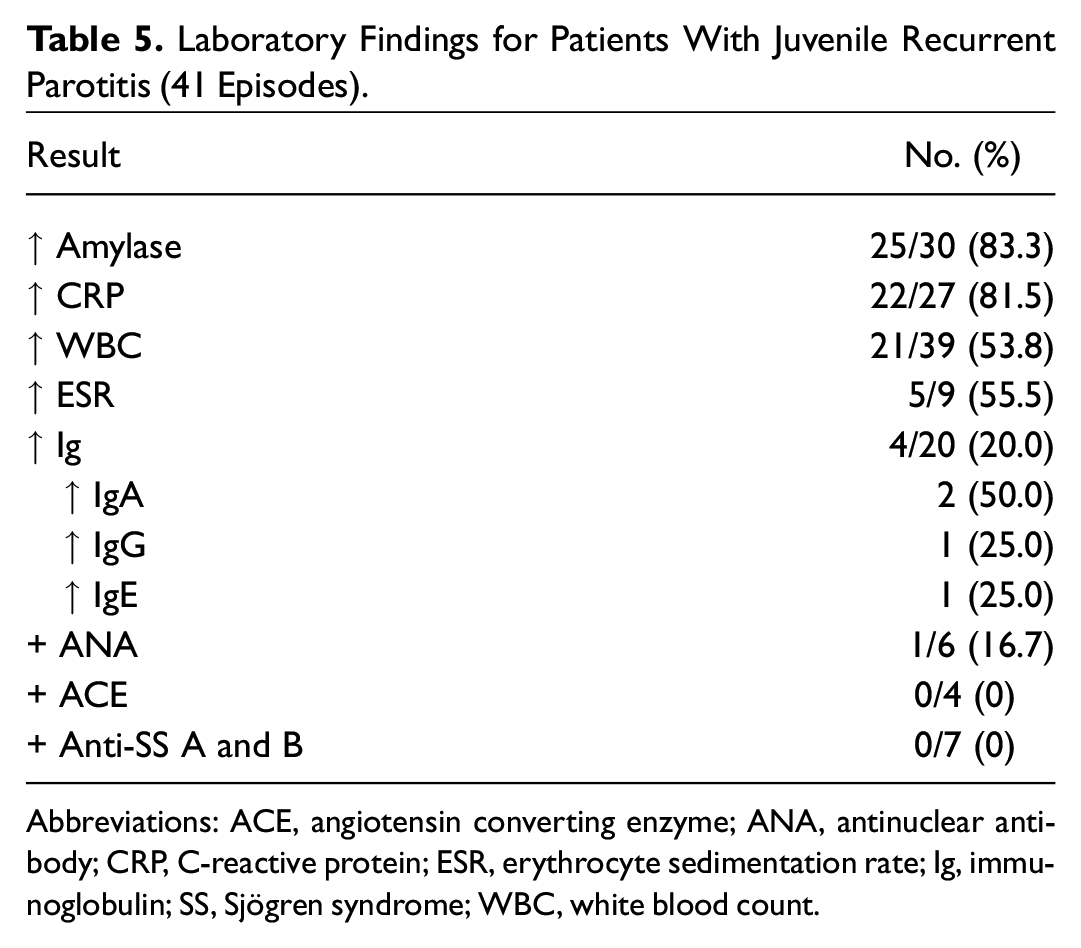
Abbreviations: ACE, angiotensin converting enzyme; ANA, antinuclear antibody; CRP, C-reactive protein; ESR, erythrocyte sedimentation rate; Ig, immunoglobulin; SS, Sjögren syndrome; WBC, white blood count.
Characteristics of Sialendoscopy Performed for JRP (17 Patients).
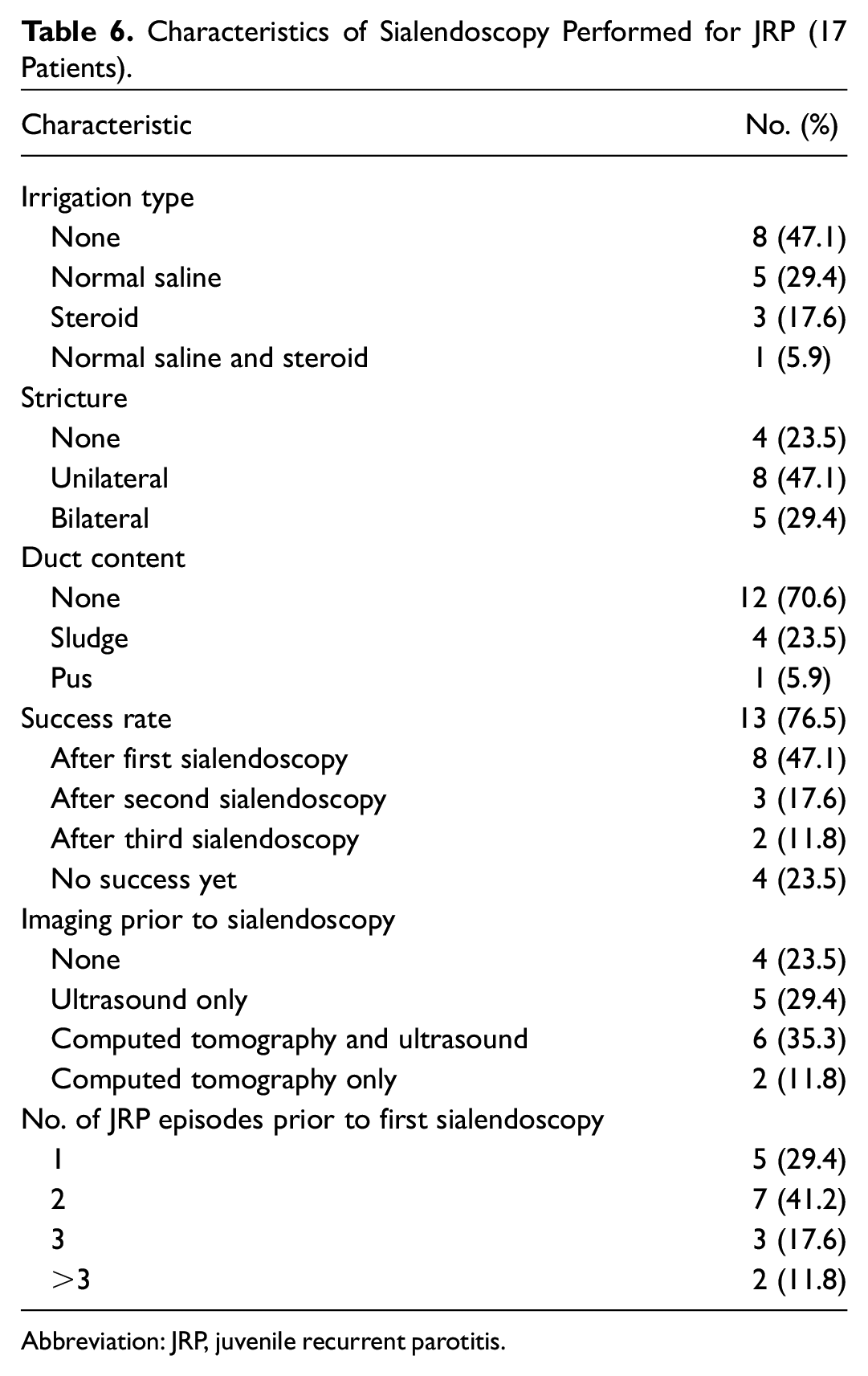
Abbreviation: JRP, juvenile recurrent parotitis.
A wide range of concurrent diseases exist for patients with JRP, as demonstrated by Table 7 . The top 3 most common comorbidities were of atopic (61%), excess weight (42%), and otolaryngologic (29%) etiologies. Among the cohort receiving ≥3 antibiotics, however, otolaryngologic comorbidities were overtaken by psychiatric conditions (33%), which were mostly attention-deficit/hyperactivity disorder (ADHD; 6/7, 86%). Three patients with ADHD were treated with medications (1 on lisdexamfetamine and 2 on methylphenidate). A higher percentage of patients with JRP who required ≥3 antibiotics or surgery exhibited concurrent atopy and obesity/overweight conditions as compared with patients who did not require extensive treatment. To note, no statistically significant differences were found (P = .15 for obesity/overweight and P = .26 for atopy).
Concurrent Comorbidities of Patients With Juvenile Recurrent Parotitis. a
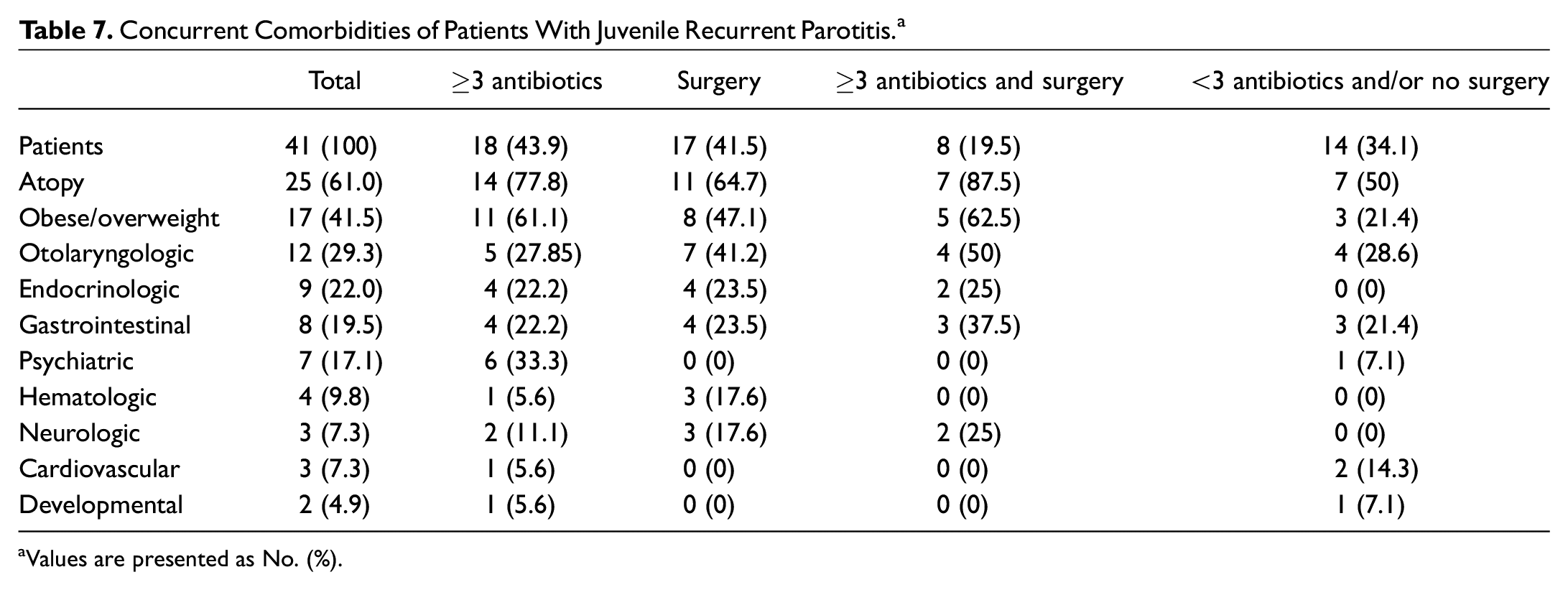
Values are presented as No. (%).
Discussion
JRP is a rare pediatric entity with recurrent episodes of inflammation of the major salivary glands, and it is a clinical diagnosis of exclusion. Patients present with recurrent swelling of 1 or both parotid glands (100%) accompanied by pain (92%) and fever (42%). 1 Thick, cloudy saliva can often be expressed with glandular massage. Symptoms usually last a few days and resolve spontaneously, followed by an asymptomatic period that varies widely in length. The true incidence rate of JRP may be greater due to subclinical symptoms and/or rapid resolution of symptoms after flare-ups. 3 Garavello et al proposed a set of inclusion criteria for JRP that encompass age <16 years, recurrent unilateral or bilateral swelling, and ≥2 episodes during the last 6 months. 4 The episodic nature of the diagnosis adds a significant burden to affected patients and caretakers via interrupted school and workdays, increased visits to health care facilities, and heightened likelihood of surgical intervention. 5
Our demographic findings were consistent with previous reports of patients with JRP. 6 Male children were more commonly affected by JRP, except for the cohort requiring surgical interventions. Black American was the most frequently affected racial group, which is congruent with the local population. 7 The JRP onset ages were bimodally distributed with a primary peak at 4 to 6 years, followed by a smaller peak at 12 to 14 years. Patients with the most severe symptoms, requiring ≥3 antibiotics and sialendoscopy for management, were typically younger.
Originally, JRP was attributed to congenital dilation and malformations and/or recurrent infections,8,9 but a multifactorial approach to etiology is more widely accepted today. Genetically, JRP exhibits an autosomal dominant pattern with incomplete penetrance and variable expressions. 10 An infectious etiology is supported by higher concentrations of Streptococcus pneumoniae and Haemophilus influenzae isolated in the saliva of patients with JRP. 11 Alternatively, JRP has been connected with hypogammaglobulinemia 12 and immunoglobulin G3 (IgG3) and IgA deficiency.13-15 In patients with older ages of onset, JRP may be associated with Sjögren syndrome.16-20 In addition, JRP is associated with human leukocyte antigen B27 seropositivity, 21 and matrix metalloproteinases 2 and 9 have direct correlations with the severity of parotid gland damage due to JRP. 22
As a diagnosis of exclusion, JRP requires extensive investigation to rule out autoimmune, immunodeficient, infectious, and obstructive causes for final confirmation. Among the many laboratory tests used, however, only a few may be correlative. Amylase and C-reactive protein were often elevated during acute parotitis events and may be supportive of a JRP diagnosis for equivocal cases. In contrast, white blood count and erythrocyte sedimentation rate were elevated in just half of the cohort, diminishing their clinical significance. In our cohort, 2 patients had elevated IgA, and none had IgA deficiency. One patient had positive antinuclear antibody, and none had positive angiotensin-converting enzyme and anti–Sjögren syndrome antibody A and B, demonstrating that the aforementioned tests may be low yield.
Ultrasonography and CT are often utilized for general parotitis workup and may be used to evaluate obstructive causes, such as sialolithiasis, mucoceles, and neoplasms. The noninvasive nature of ultrasonography makes it an ideal imaging modality for children. Expected ultrasound findings for JRP include scattered hypoechoic foci (referred to as “Swiss cheese” or “moth eaten”) within an enlarged salivary gland,2,23 which was observed in 15 of our patients. In contrast, CT scans have radiation exposure and are more costly, and usage in pediatric patients should be conservative. 24 CT scans were beneficial only when ultrasound results were inconclusive or further evaluation for a detected mass was warranted at our institution. In all other cases, CT was equal to ultrasonography in parotid evaluation. No noticeable differences in rates of patients undergoing sialendoscopy following CT or ultrasound existed (9 vs 11 patients, respectively), indicating that ultrasound may be the better clinical choice for pediatric patients. Thus, we recommend employing a bilateral ultrasound of the parotid and submandibular glands for first-line JRP assessment, while reserving CT for atypical cases and/or ruling out other possible etiologies.
Conservative therapy for acute JRP episodes consists of sialagogues, warm compress, massage, and analgesics. 25 Alternating acetaminophen and ibuprofen was the most common analgesic regimen used in our patients, and excellent outcomes were observed. Opioid usage should be reserved for severe pain, after failure of other analgesic trials, to prevent unnecessary pediatric exposure and risk of misuse. For persistent or severe episodes, antibiotics may be given, but the exact practice is controversial and unstandardized. 25 In this study, clindamycin was the most routinely prescribed antibiotic, followed by amoxicillin-clavulanic acid for persistent episodes or cases with secondary bacterial infections. No complications due to infections or antibiotic usage were noted for our patients. Given the findings, we recommend maximizing acetaminophen and ibuprofen for pain control and prescribing clindamycin or amoxicillin-clavulanic acid as first-line antibiotics for acute JRP flare-up management.
Sialendoscopy has emerged as a new treatment modality for recurrent JRP cases to simultaneously confirm the diagnosis with direct visualization and provide treatment via steroid infusion. Patients with JRP often have diminished vascularization of the Stensen duct upon sialendoscopy. 26 In a study of 36 participants, Schneider et al found that patients with JRP who undergo at least 1 sialendoscopy have noninferior treatment outcomes vs conservative treatment. 2 After the first sialendoscopy, 47% of our patients had no JRP recurrences, and the success rate increased to 76% after 3 sialendoscopies. Our patient outcomes lie in the middle of reported success rates for sialendoscopy (24%-73%), and the variability can be attributed to differing definitions of JRP and follow-up periods.4,6 Currently at our institute, patients with ≥2 recurrences, without evidence of sialolithiasis, were treated with sialendoscopy with steroid irrigation. There are no limits on the total number, and sialendoscopies were performed as many times as necessary for sialoadenitis cessation. As a result, we recommend repeating sialendoscopy with steroid irrigation for JRP management after 2 episodes to shorten the pathologic course and prevent future recurrences.
In this study, obesity/overweight and atopic comorbidities (asthma, seasonal allergies, and allergic rhinitis) were commonly associated with patients with JRP who had severe symptoms requiring ≥3 antibiotics and/or sialendoscopy. While no allergic components have been linked to JRP through histologic and cytologic evaluations, 27 possible overlap may exist between JRP and eosinophilic sialodochitis, characterized by salivary duct mucus plugs containing numerous eosinophils causing reactive inflammation and focal narrowing. 28 Although the relationship between obesity and JRP is unclear, obesity promotes proinflammatory changes in the salivary glands, which may increase risks for dental decay and reduction in salivary flow rate. 29 This is congruent with a hypothesis that JRP is caused by inadequate salivary secretion and excretion. 30 In addition, obesity has been associated with fatty infiltration of the salivary glands in adults, which may contribute to sialadenosis. 31 Consequently, optimization of atopy and/or weight management may be instrumental in controlling JRP symptoms and preventing recurrences. Of note, lisdexamfetamine and methylphenidate, common medications prescribed for ADHD, may cause xerostomia, which could have exacerbated JRP symptoms for our patients, necessitating ≥3 antibiotics for management.32,33 Furthermore, patients with atopic disease may be taking antihistamines, which have varying effects on decreasing salivary flow. 34
Several limitations exist in our study. JRP presents episodically, which makes it difficult to measure the true efficacy of treatment methods without performing a randomized controlled trial. The retrospective nature of data collection and small sample size limit accurate assessment of the true characteristics of JRP. The small sample size may be preventing the finding of a statistical association between JRP and concurrent conditions. Additionally, all patient data originated from a single institution, which may be influenced by local patient demographics and regional practice preferences. As the study is based in a tertiary center, other JRP cases treated by primary care and/or outside urgent care centers may be missed. No uniform JRP diagnosis and ICD-9/10 codes are established, which restrict the consistency of evidence reporting and may lead to inaccurate low incidence rates. Future studies focused on establishing a standardized JRP definition and treatment algorithms are necessary.
Conclusion
At our institution, JRP was most commonly observed in Black males aged 2 to 8 years. Our limited data support the following clinical management recommendations for JRP:
In equivocal cases of acute flare-up, only draw amylase and C-reactive protein routinely.
Prioritize ultrasonography for acute assessment, and reserve CT for cases with poor imaging quality or detected mass.
Utilize acetaminophen and ibuprofen for first-line pain control, with avoidance of opioid.
Prescribe clindamycin for complicated cases with signs of infections, such as fever, purulent discharge, and/or failure to resolve within 48 hours of conservative treatment.
Patients with JRP with ≥2 recurrences may benefit from sialendoscopy with steroid flush treatments. Further translational and clinical research into concurrent diseases, such as atopy and excess weight, is necessary, as managing these diseases could be a crucial part in treatment strategy.
Author Contributions
Disclosures
Footnotes
This article was presented at the 2021 AAO-HNSF Annual Meeting & OTO Experience; October 3-6, 2021; Los Angeles, California.
