Abstract

Airway foreign bodies in the pediatric population have a variable presentation, from acute aspiration to a chronically ill patient. Most foreign body aspirations occur in preschool-aged children, and management is typically achieved by rigid bronchoscopy.1,2 Expeditious removal of the foreign body is of primary importance to prevent long-term sequelae, 1 but it may be difficult to confirm the diagnosis based on history and basic physical exam alone, especially if the aspiration is not a witnessed event. At our institution, the decision to take a potential foreign body aspiration to the operating room is dependent on having at least 2 of 3 factors: convincing history or witnessed event; clinical findings such as wheezing, stridor, or diminished lung sounds; and positive radiographic findings. We present a case of an aspiration of a peculiar foreign body, creating an ambiguous clinical presentation with dire consequences for the patient. The University of Arkansas for Medical Sciences (UAMS) Institutional Review Board approved this study (IRB No. 262546).
Case Presentation
A 3-year-old boy was initially evaluated by his primary care provider for symptoms of gastroenteritis. Abdominal series x-rays were obtained and incidentally found opacification in the region of the left lung. The patient was sent to the emergency department at a satellite-affiliated hospital for concern for pneumonia, where chest x-ray revealed significant atelectatic collapse of the left lung, confirmed by computed tomography (CT) of the chest. Otolaryngology was consulted for assistance with management of the suspected foreign body, and the patient was taken to the operating room for a diagnostic bronchoscopy. The left mainstem bronchus ended in a blind fibrotic pouch concerning for a chronic foreign body reaction ( Figure 1 ). Further aggressive management was deferred to our tertiary care children’s hospital with pediatric general surgeons available for further assistance dependent on intraoperative findings.
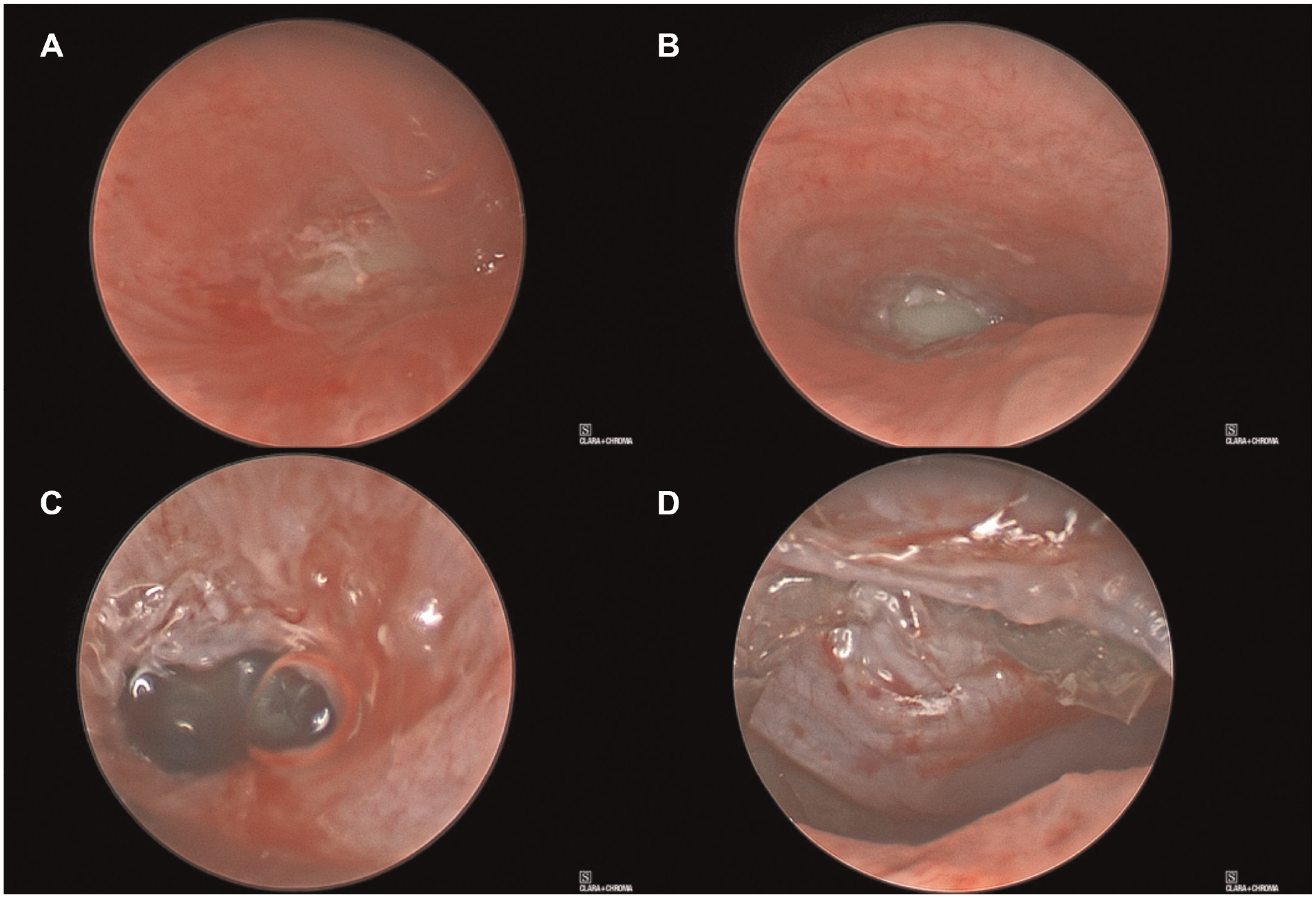
(A, B) Left mainstem bronchus ending in blind pouch after fibrotic tissue removal with suction catheter. (C) Gel-like material expressed immediately upon further dissection. (D) Gel-like material visible in mediastinum from eroded bronchus.
Definitive management was achieved by rigid ventilating bronchoscopy. The fibrous tissue was incised with blunt and sharp instrumentation revealing green inorganic gel material. Further examination revealed evidence of erosion of most of the bronchus with exposed mediastinum and pericardium ( Figure 2 ). The foreign body was removed in fragments from the bronchus and mediastinum, via the defect in the bronchus, with optical forceps (see Supplemental File 1 in the online version of the article). The patient was safely extubated postoperatively and had an uncomplicated hospital course. Upon follow-up, the left lung has been noted to have stable atelectatic collapse via x-ray, although the patient is stable from a clinical perspective. The foreign body was shown to the patient’s mother, and after further discussion, it was identified as an “Orbeez” gel bead that the child had been playing with over a year in the past.
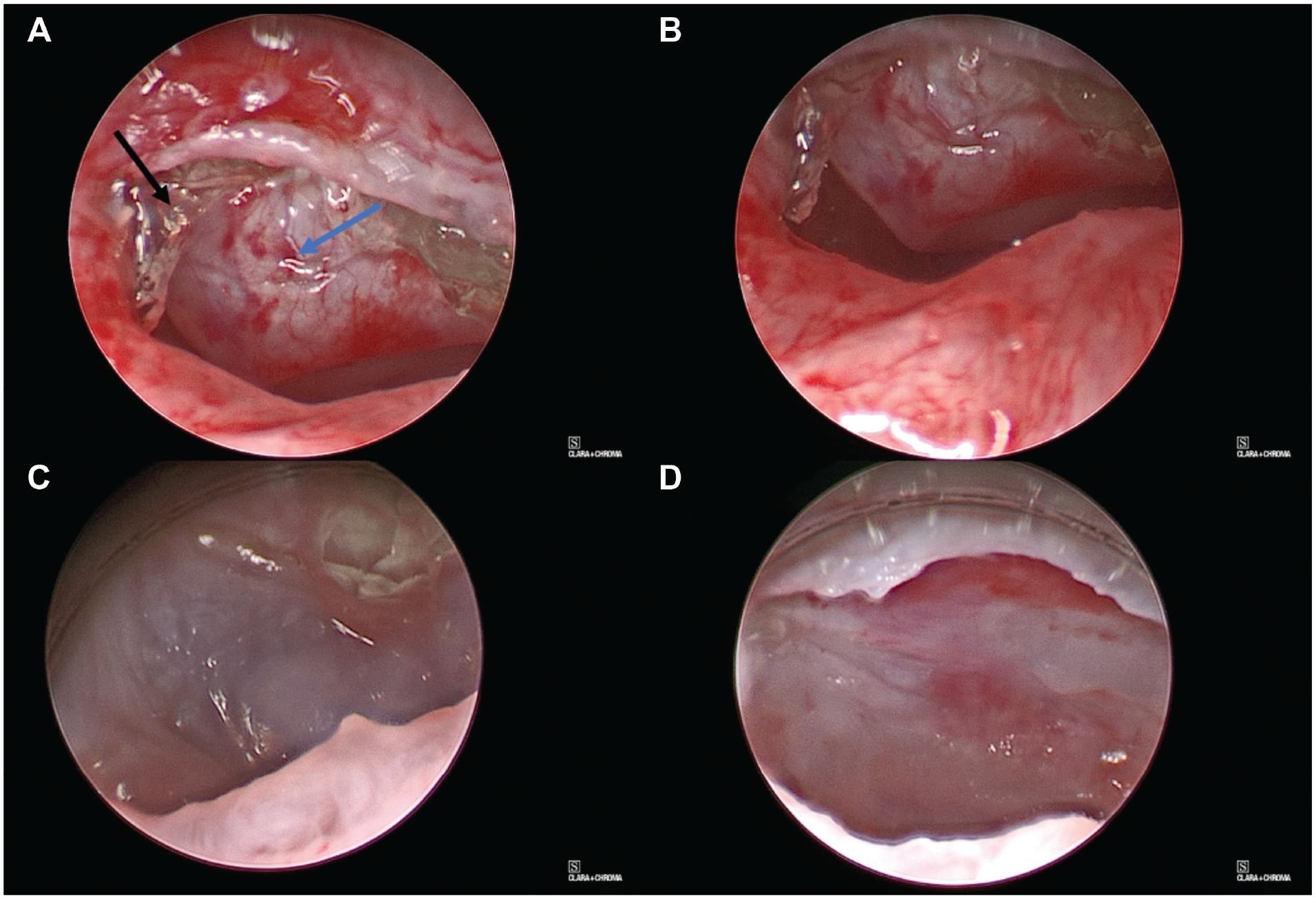
(A) Gel-like material (black arrow). Pericardium (blue arrow) pulsating within the mediastinal cavity. (B-D) Additional views of eroded bronchus and mediastinal cavity with material removed.
Discussion
This case highlights an atypical presentation of a foreign body aspiration resulting in chronic pulmonary consequences. The patient did not initially present for pulmonary concerns, indicating an indolent course with gradual compensation. The superabsorbent polymer aspirated in this case has been documented as a serious potential risk to children who ingest or aspirate it. 3 After exposure to mucous or other bodily fluids, the bead will expand to a much larger diameter over time, and aspiration of this inorganic substance can cause chronic obstruction due to a lack of airway inflammation and radiolucency of the bead.3,4 In this case, the gel bead may have gradually expanded, causing both fibrotic tissue formation as well as bronchial erosion over time. The continued airspace collapse in this patient caused by the chronic nature of aspiration will necessitate further monitoring. However, there is hope that return of normal airspace or compensatory lung growth may occur, as seen in the course of disease of some congenital lung malformations following pneumonectomy. 5
Author Contributions
Disclosures
Footnotes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
