Abstract
Objective
To report the efficacy and safety of electromyography-guided percutaneous botulinum toxin injection into the cricopharyngeus muscle in an office setting for treatment of the inability to belch and associated symptoms caused by retrograde cricopharyngeus dysfunction (R-CPD).
Study Design
Retrospective case series of treated patients.
Setting
Tertiary care laryngology clinic.
Methods
A retrospective review was performed on 18 consecutive patients who were diagnosed syndromically with R-CPD. The combined diagnostic test and treatment—specifically, botulinum toxin injection into the cricopharyngeus muscle—was accomplished in an office setting by a single surgeon using electromyography guidance. Items assessed are efficacy, safety, complications, and duration of benefit.
Results
All 18 patients (100%) treated in the in-office setting gained the ability to burp with improvement in the associated symptoms of R-CPD at initial follow-up. Of those who had the in-office procedure performed initially, 80% maintained the ability to burp at 6 months with relief of all the associated symptoms of R-CPD. No patients experienced permanent complications from the injection, but 7 patients experienced varying degrees of noisy breathing within 1 week after the procedure, which was managed with breathing techniques and resolved.
Conclusion
In a case series of 18 patients with R-CPD, all patients gained the ability to burp with improvement in the majority of their symptoms of R-CPD at the time of their initial follow-up at 1 week. None experienced severe complications, and 7 experienced transient noisy breathing, which resolved.
In March 2019, Bastian and Smithson first described the syndrome now known as retrograde cricopharyngeus dysfunction (R-CPD), with the details of the first 51 patients whom they diagnosed and subsequently treated with botulinum toxin injection. 1 As described by these authors, R-CPD can be diagnosed syndromically by match to a constellation of almost universal symptoms that are severe and a daily occurrence. The primary ones are the inability to belch, socially awkward gurgling sounds, abdominal/chest pressure and bloating, and excessive flatulence. These symptoms significantly affect patients’ quality of life and often lead to social inhibition and anxiety. Clinical diagnosis is made by a patient’s match to this syndrome, and the diagnosis is validated by relief of symptoms after botulinum toxin (BT) injection into the cricopharyngeus muscle (CPM). The injection is, at the same time, a diagnostic test and treatment that seems to resolve the syndrome permanently in approximately 80% of patients.
The standard method of treatment for the patients reported by Bastian and Smithson was via endoscopic esophagoscopy with injection into the CPM under brief outpatient general anesthesia. 1 Part of the reason for choosing this method was the great distance that many patients traveled for treatment and the desire for certainty in targeting, because the upper esophageal sphincter can be seen and palpated easily with this method. In a follow-up publication by Hoesli et al, the few and minor complications of this treatment approach were mainly related to esophagoscopy or anesthesia, not BT side effects. 2 Thus, it would be preferable to identify a technique of injection that could avoid esophagoscopy and general anesthesia.
Percutaneous access to the CPM has been described for monitoring and for swallowing difficulties caused by antegrade cricopharyngeus dysfunction.3-7 Ertekin et al described a percutaneous approach for recording CPM activity by inserting a concentric electromyography (EMG) needle through the skin “about 1.5 cm lateral to the palpable lateral border of the cricoid cartilage.” 4 With this technique, Verhulst et al performed a retrospective study of 64 patients who had a total of 91 BT injections into their upper esophageal sphincter for major swallowing disorders, the majority of whom were treated with a percutaneous approach. 5 In 49 of the 91 BT injection cases, swallowing ability improved significantly. In 2 other studies, Suzukia et al and Restivo et al used percutaneous BT injection into the CPM for antegrade cricopharyngeus dysfunction and showed that it was an “effective and less invasive treatment for dysphagia” 6 and could “be performed in outpatient clinics, needing neither hospitalization nor general anesthesia.” 7 Additionally, Restivo et al showed that BT injection can be repeated for antegrade cricopharyngeus dysfunction when symptoms reappear, while retaining its efficacy. 7
Adapting this technique for treatment of R-CPD would have the benefit of avoiding general anesthetic and decreased cost. Additionally, for the 20% of patients who do not experience long-lasting relief of their symptoms, in-office injection could provide a more convenient method for those who choose repeated injections over cricopharyngeus myotomy. Our objective was therefore to evaluate the efficacy and safety of in-office BT injections into the CPM for R-CPD.
Materials and Methods
This is a retrospective case series of all patients with R-CPD treated in an office setting with percutaneous BT injection. Institutional Review Board approval was obtained from AspireIRB. Patients were identified via a prospective database of R-CPD cases at Bastian Voice Institute, maintained for clinical purposes. All patients fill out an extensive questionnaire at their initial appointment, as detailed in the article by Hoesli et al. 2 Diagnosis is then based on the history and match of the symptoms. Finally, normal neurologic function of the palate, pharynx, and larynx and swallowing ability is evaluated with a videoendoscopic swallow study. The risks and benefits of in-office treatment versus the operating room are discussed extensively, as well as expected postoperative course. The initial 13 patients who chose to proceed with in-office treatment underwent injection of 50 U of BT and then 75 U for the remainder. The dose was increased for all patients in the larger series as well in an attempt to reduce the number of patients who might need reinjection in the future.
The technique is similar to the already described method of injection for abductory spasmodic dysphonia. 8 For this procedure, the skin overlying the cricothyroid membrane was infiltrated with 2% xylocaine with epinephrine 1:100,000. Then, 1 mL was introduced into the subglottis for topical anesthesia. A Teflon-coated EMG needle was used to pierce the cricothyroid membrane. From there, the needle traversed the lumen, posterior cricoid plate, and posterior cricoarytenoid muscles to reach the CPM. After confirmation of location per EMG, 50 or 75 U of BT was infiltrated, half per side ( Figure 1 ). The posterior cricoarytenoid muscles were protected from injection by having the patients “sniff.” Specifically, sniffing activates the posterior cricoarytenoid muscles, resulting in a burst of EMG signal and injection is avoided.
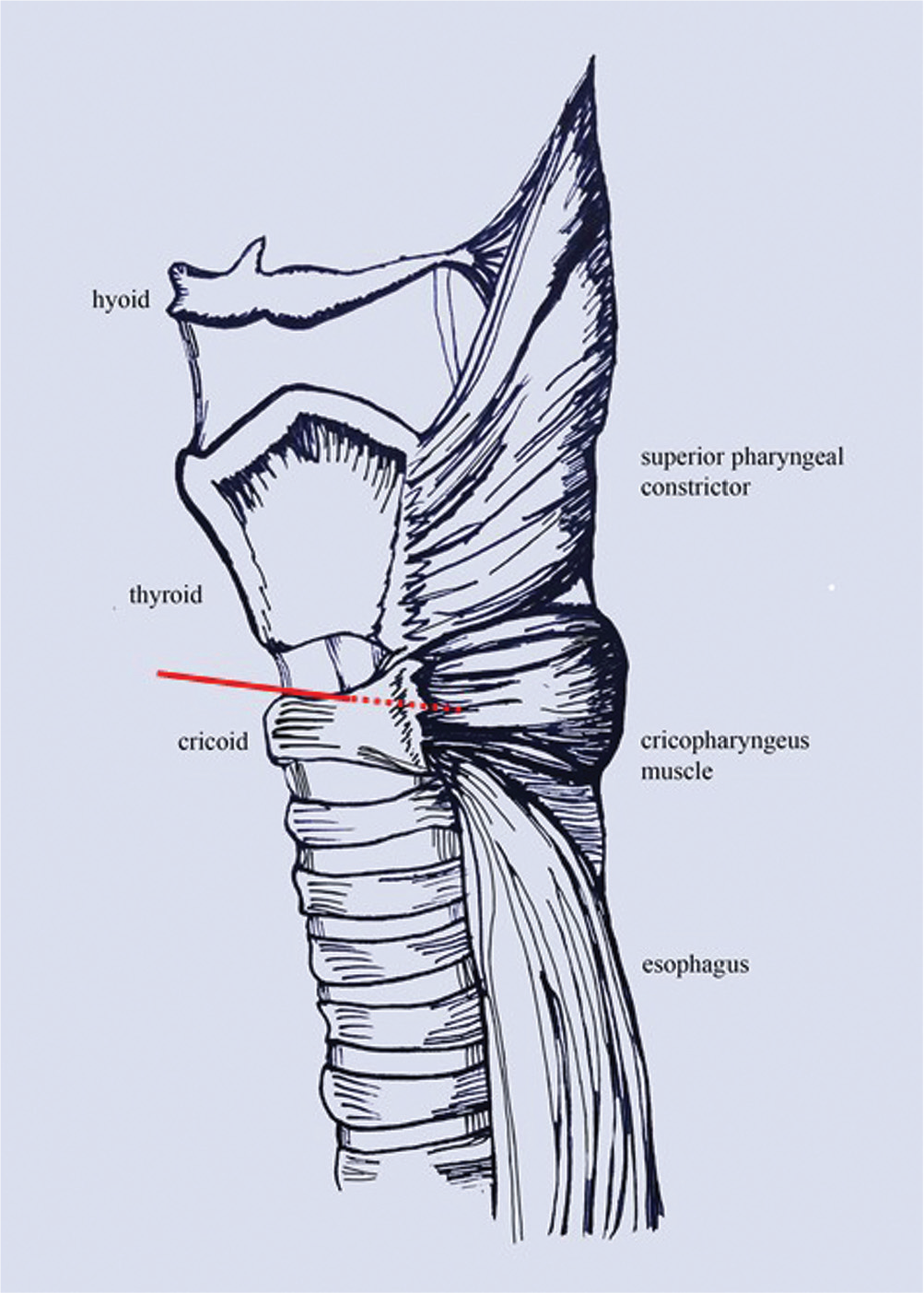
Approximate injection trajectory.
Patients were counseled on the expected postoperative effects of the injection, including the nature and timing of burp onset, alteration in swallowing as described by Bastian and Smithson, and possible noisy inspiration (especially upon exertion). 1 Patients received extensive teaching on “straw breathing,” a technique that would assist in management of symptoms in case there was diffusion into the posterior cricoarytenoid muscles, as previously detailed by the senior author. 9 Patients were then followed up at 1 week, 6 weeks, 3 months, 6 months, and then yearly and asked to report on the presence or absence of symptoms of R-CPD and any other concerns or complications.
Data were collected from this initial questionnaire and the patients’ charts on sex, age at diagnosis, previous studies performed, rating of severity/motivation for treatment (scale, 1-7), status of symptoms at follow-up, response to treatment, and reported complications or issues. Simple statistics were performed with Microsoft Excel.
Results
Eighteen consecutive patients with R-CPD underwent in-office BT injection by the senior author between August 2017 and December 2019. Patient characteristics are included in Table 1 . These patients came from 12 states and 1 foreign country. Ages ranged from 19 to 59 years, with a mean of 32.5 years. Patient follow-up after initial injection ranged from 1 to 35 months, with a mean of 13.0 months and a median of 12.0 months. The majority of patients (94.4%) described lifelong symptoms, with only 1 patient noting the onset of symptoms later, at age 25 years. When patients were asked about severity of their symptoms on a scale of 1 to 7, with 7 being most severe, the mean of all 18 ratings was 6.2. When they were asked about their motivation to solve their issue, the mean was 6.7.
Demographics for Cohort With R-CPD Who Underwent In-office BT Injection.

Abbreviations: BT, botulinum toxin; R-CPD, retrograde cricopharyngeus dysfunction.
The initial 13 patients received 50 U of BT, and the most recent 4 received 75 U. One of the 18 patients underwent injection 4 times, each time with relief of symptoms for approximately 4 months, receiving 50 U for the first, second, and third injections and 75 U for the fourth.
All 18 patients (100%) treated in the in-office setting reported gaining the ability to burp, with significant improvement in associated symptoms of R-CPD at 1 week after injection. Of the 18 patients who underwent the in-office injection, 6 had previously undergone injection into the CPM via upper esophagoscopy. In this subgroup, the prior procedure had validated the diagnosis and relieved other symptoms markedly for some months; however, these benefits were lost when the BT effects wore off, so patients elected for reinjection in office. Of the 6 patients, all gained the ability to burp. All patients additionally had significant improvement in the associated symptoms of R-CPD, with the exception of 2 who had improvement in all other associated symptoms except for flatulence.
At 6 months, out of these 6 patients, 1 patient reported continued relief. Two of the 6 patients lost the effect again after 3 to 6 months and have not yet proceeded with further treatment. One patient proceeded with a total of 4 injections, with a good effect every time, which would then fade at 3 to 6 months. After the most recent injection, he was doing well but then was lost to follow-up. Finally, 2 patients proceeded with myotomy after multiple injections, 1 patient after 2 injections, and 1 patient after 4 injections ( Figure 2 ).
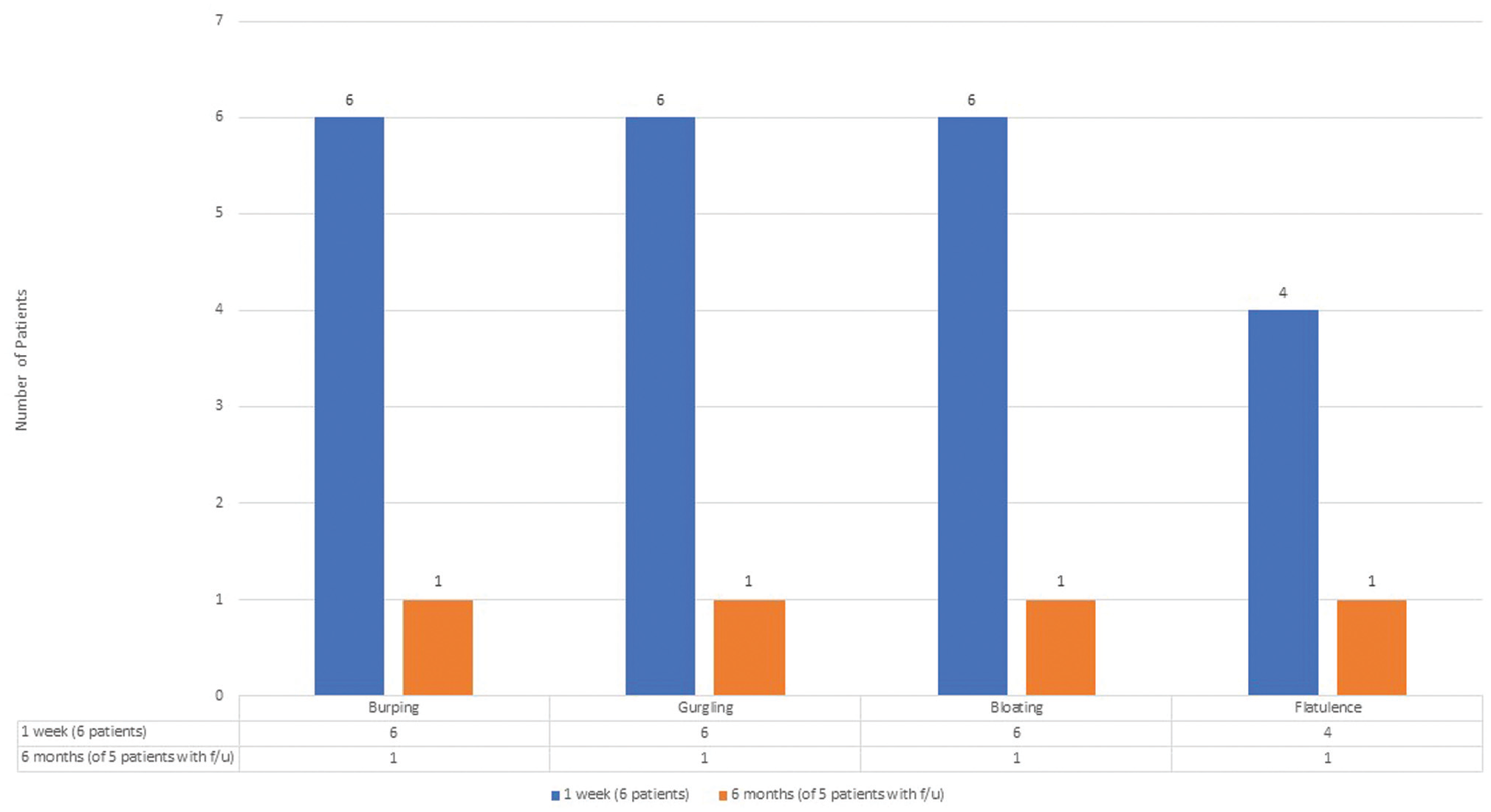
Resolution of symptoms for 1-week and 6-month follow-up periods for patients undergoing in-office injection for recurrence of symptoms after their initial injection in the operating room.
The remaining 12 patients proceeded with in-office injection as their initial treatment. All patients gained the ability to burp at the 1-week follow up. All patients noted significant improvement in all associated symptoms of R-CPD at 1 week, with the exception of 1 patient who noted no improvement in gurgling and 1 patient who had no improvement in flatulence. Otherwise, these 2 patients had improvement in all other symptoms.
At 6 months, 2 of the 12 patients were lost to follow-up. Of the 10 patients with follow-up data at 6 months, 8 (80%) maintained the ability to burp with continued resolution of all of the cardinal symptoms of R-CPD. The other 2 patients maintained the ability to burp, although less easily than at peak benefit, and they also noted the return of a lesser degree of the associated symptoms of R-CPD ( Figure 3 ).
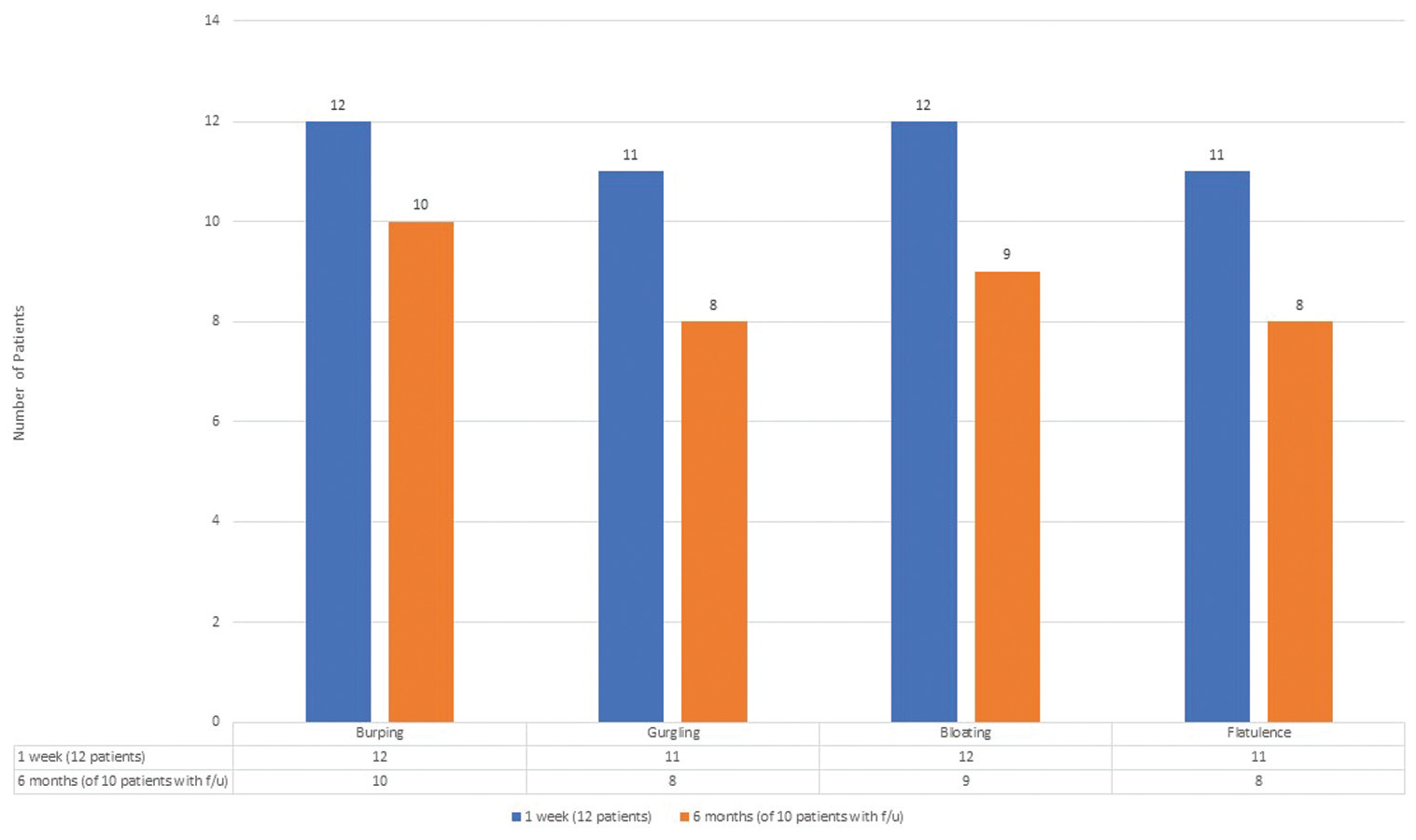
Resolution of symptoms for 1-week and 6-month follow-up periods for patients undergoing in-office injection for initial treatment of retrograde cricopharyngeus dysfunction.
No patient experienced major complications from the procedure of the injection of the BT itself or at the BT injection site. One week after the procedure, 10 patients (55.6%) reported the swallowing difficulties routinely expected after treatment of R-CPD, whether endoscopic or EMG guided, and 7 patients reported breathing changes (38.9%), which resolved. Of these 7 patients, 2 noted slight shortness of breath with exertion; 2 cited some noisy breathing with exertion; 1 had slight shortness of breath that lasted a day; and 1 reported some noisy breathing at night. This side effect was not viewed as “urgent” but rather an annoyance or limitation on activity level. These 6 patients managed their symptoms with the breathing technique mentioned earlier with minimal reported difficulty. Only 1 patient noted noisiness and sense of restriction that required avoidance of exertion. This peaked on day 4 or 5 and then gradually resolved. This patient also managed her symptoms with the breathing technique but reported more limitation of activity when symptoms were at their worst. One patient experienced transient weakness of the voice, and 1 patient had a vasovagal reaction during the procedure ( Figure 4 ).
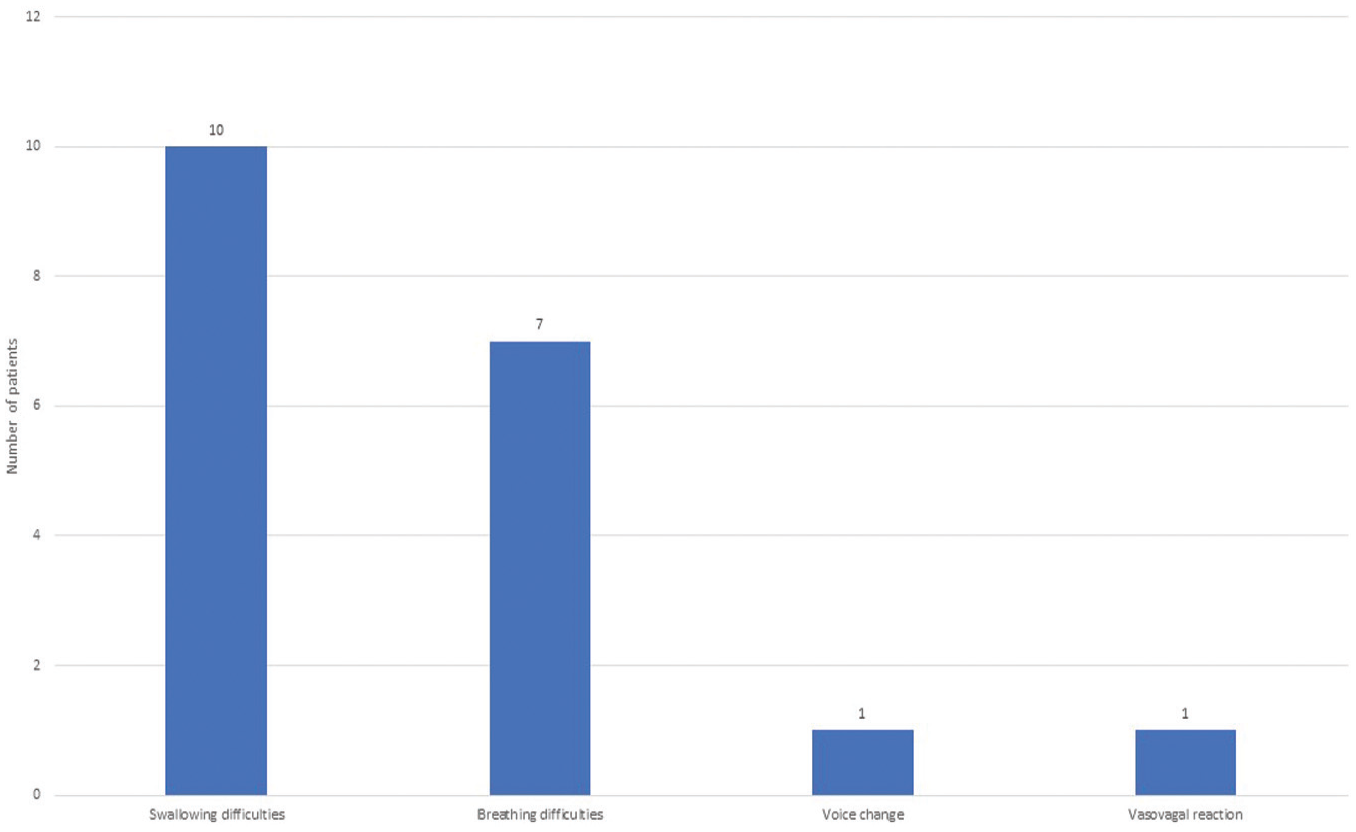
Number of patients with complications at 1-week follow-up period.
Discussion
As previously described, R-CPD has been successfully managed via endoscopic esophagoscopy with injection into the CPM under brief outpatient general anesthesia.1,2 Although 80% of patients achieve long-lasting relief with just 1 injection, 20% develop recurrence of symptoms when the BT wears off. More convenient methods of injection would allow for repeated injections if needed and reduce the minor risks and costs of treatment that involves esophagoscopy and general anesthesia.
Our study shows that the EMG-guided percutaneous approach to BT injection into the CPM for treatment of R-CPD can be very accurate, since 100% of patients were relieved of the symptoms. This technique can be performed in an in-office setting, and it avoids the minor complications previously reported for injection via esophagoscopy under general anesthesia. 2 It also provides an alternate treatment for patients who cannot tolerate general anesthesia. Additionally, in-office injections are more cost-effective for patients. Based on procedure costs from the Bastian Voice Institute, in-office injection costs approximately $1190 less than the endoscopic injection under general anesthesia.
It is notable that 80% of patients who underwent in-office injection as their initial treatment for R-CPD maintained their ability to burp at 6 months, consistent with previous reports for the esophagoscopy approach.1,2 Interestingly, of those who underwent this procedure after having lost the ability after a previous injection in the operating room, only 1 maintained the ability to burp at 6 months, while the others lost the ability as BT began to wear off. For these patients, this technique provided a more convenient way to obtain relief of their symptoms, but it suggests that those who lose the ability might have continued difficulty maintaining it.
Due to its location near the posterior cricoarytenoid muscles and possibly due to the chosen trajectory of the needle, one expected risk of this technique is transient noisy breathing and, with exertion, shortness of breath due to risk of injection or diffusion of BT into the posterior cricoarytenoid muscle. This potential side effect is a significant drawback of this technique, and in our patient population, this occurred in 38.9%. However, patients were able to manage this via a breathing technique previously used by patients receiving posterior cricoarytenoid muscle injection to treat their abductory spasmodic dysphonia and by patients with laryngospasm. 9
A primary limitation of this study is its retrospective nature. Further study of a larger population of randomized patients could compare the efficacy between the techniques. This clinician group has recently added a second method of injection (laterally), and it remains to be seen if effectiveness can remain as high and with fewer instances of transient noisy breathing. Finally, all injections reported here were performed by single surgeon, and it must be shown that these results are reproducible by others.
Conclusion
In a case series of 18 patients with R-CPD, all gained the ability to burp with marked reduction of the majority of their symptoms of R-CPD after in-office BT injection of the CPM. At 6-month follow-up, 80% of patients who underwent the procedure primarily maintained the ability to burp with resolution of all cardinal symptoms of R-CPD. No significant complications were noted; however, 38.9% of patients reported mild transient noisy breathing, which was managed behaviorally when needed via straw breathing.
Author Contributions
Disclosures
Footnotes
Acknowledgements
We acknowledge the contribution of Zachary Bastian, MD, who provided the artistic rendering of Figure 1.
