Abstract
Continuous fasciculation that occurs without weakness is referred to as benign fasciculation. Although generally considered non-threatening, cases that persist can significantly impact an individual's quality of life. This study presents a case of a male patient in his 30s experiencing unyielding twitching localized to the sole of his left foot for 2 years. His medical history was devoid of any notable neuromuscular diseases. Results from electromyography testing were also normal for all parameters. Attempts with pharmacological intervention did not yield any improvement of his condition. Although a nerve block targeting the left tibial nerve managed to reduce the severity of the twitching, it failed to decrease its frequency or provide a lasting solution. In search of a more effective treatment, botulinum toxin was administered via ultrasound guidance into the flexor hallucis and digitorum longus muscles. This approach resulted in a marked reduction in both the frequency and severity of the twitching, enabling the patient to resume his daily activities and achieve restful sleep without experiencing any adverse effects. Through this case, the efficacy of botulinum toxin injections as a treatment for intractable twitching is underscored, offering valuable insights into potential therapeutic strategies for similar clinical presentations.
Introduction
Twitching or fasciculation involves spontaneous, involuntary muscle fibre contractions in skeletal muscles. This can stem from diverse aetiologies, encompassing neurological conditions (such as amyotrophic lateral sclerosis, radiculopathy and peripheral neuropathy), metabolic disorders (such as thyrotoxicosis), pharmaceutical agents (such as steroids or caffeine), infectious diseases (such as HIV), psychological disorders (including stress and anxiety), electrolyte imbalances, and intense and lengthy daily exercise, among other potential causative factors.1–3 Hence, to ascertain the underlying cause of fasciculation, comprehensive neurological examinations, pertinent blood tests, imaging studies and additional diagnostic evaluations may be imperative.
This phenomenon can manifest even in otherwise healthy individuals without any abnormal findings, with occurrences lasting from weeks to years and varying from person to person.4,5 Continuous fasciculation in the absence of muscular weakness is referred to as benign fasciculation. Although such fasciculations are frequently observed, cases that prove to be intractable can significantly detract from an individual's quality of life. 2 Fasciculations in the lower legs are particularly problematic as they can disrupt walking, running, and even periods of rest, leading to a state where the individual is unable to achieve true restfulness. 6 This disruption can extend to nocturnal hours and prevent the patient from obtaining necessary sleep, further compounding the impact on overall quality of life and well-being. 7 Treatment guidelines for fasciculation lack robust evidence. Nonetheless, medication options such as vitamin B complex, naftidrofuryl and calcium channel blockers such as diltiazem may be contemplated. Non-pharmacological modalities such as stretching exercises might also be suggested to patients, although evidence supporting these interventions (regarded as adjunctive) is limited.1,8 The absence of well-established, evidence-based treatment protocols makes the management of patients who are experiencing persistent twitching exceedingly complex. This current case report demonstrates a marked improvement in fasciculations of the left sole muscle through administration of botulinum toxin in a healthy individual.
Case report
In March 2022, a male patient in his 30s (height: 174 cm, weight: 78 kg) presented to the Department of Anaesthesiology and Pain Medicine, The Catholic University of Korea, St Vincent’s Hospital, Suwon, Korea with a 2-year history of persistent, involuntary twitching localized to the left sole. Initially, these symptoms occurred intermittently, approximately 1–2 times per week. However, the frequency increased over time, eventually leading to continuous twitching 24 hours a day, which was first noted approximately 2 months before seeking medical care. The intensity of the twitching also increased progressively. The patient reported no pain associated with the twitching, but he noted that the persistent twitching caused discomfort during daily activities and disrupted his sleep patterns. He denied experiencing any associated weakness, sensory abnormalities or other neurological symptoms.
The patient's medical history included an injury to the left medial malleolus 10 years previously. It was treated conservatively without surgery. Additionally, 7 years prior to presentation, the patient suffered a lumbar vertebra disc injury resulting from a traffic accident, for which he underwent multiple lumbar injection therapies, achieving symptom resolution by the time of presentation. The patient denied any other significant medical or family history.
The patient initially sought consultation with a neurologist undergoing a battery of tests and initiating medication therapy. However, despite these efforts, his symptoms persisted without improvement. Subsequently, seeking further evaluation, the patient consulted an orthopaedic specialist, who eventually referred him to the Department of Anaesthesiology and Pain Medicine, The Catholic University of Korea, St Vincent’s Hospital, Suwon, Korea.
Physical examination revealed isolated twitching of the left sole, particularly noted in the anterior portion of the middle arch. It was distinct from arterial pulsation. It occurred at a rate of 1–2 twitches per second. No evidence of muscle atrophy or weakness was observed. Additionally, the twitching was accompanied by mild flexion of the left great toe. Inducing extension or flexion of the left toe ceased the twitching (Figure 1). There were no tenderness points. The tarsal tunnel Tinel sign was negative. Laboratory investigations, including a complete blood count, comprehensive metabolic panel and creatine kinase levels, were all within normal limits. Ultrasound examination identified spasm-like motion within the flexor hallucis longus muscle and flexor digitorum longus muscle (Figure 2). Nerve conduction studies showed increased nerve conduction velocity in the lateral portion of the left peroneal nerve and left tibial nerve. The electromyography (EMG) results showed no abnormalities.
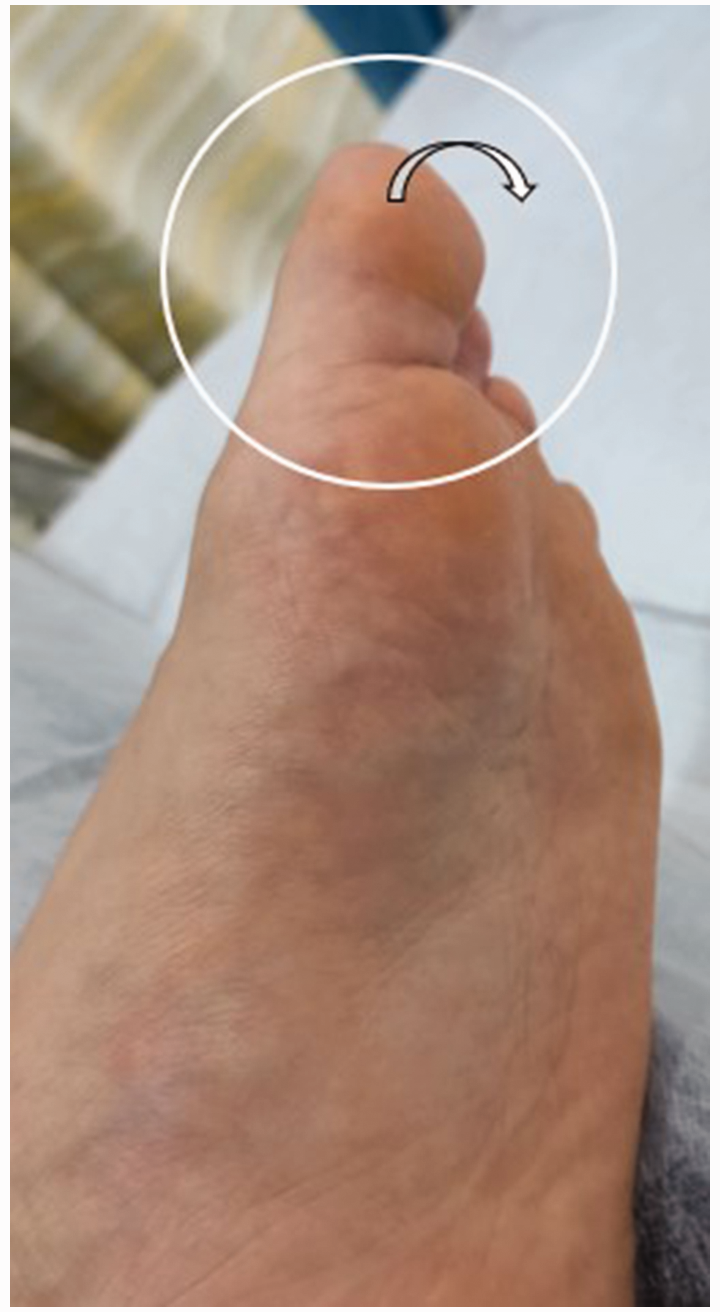
Involuntary flexion of the left large toe and continuous twitching of the muscles in the sole of the foot are observed visually in a male patient in his 30s who presented with a 2-year history of persistent, involuntary twitching localized to the left sole. The colour version of this figure is available at: http://imr.sagepub.com.

Ultrasound examination of the medial side of the thigh in a male patient in his 30s who presented with a 2-year history of persistent, involuntary twitching localized to the left sole. A, soleus muscle; B, posterior tibial artery; C, flexor digitorum longus muscle.
The patient began treatment with 200 mg carbamazepine oral twice a day, 10 mg baclofen oral twice a day and 0.25 mg clonazepam oral twice a day, which did not produce effective results over a 2-week period. Consequently, the medication regimen was adjusted to increase carbamazepine to 400 mg twice a day with the clonazepam dosage maintained. Further diagnostic tests including magnetic resonance imaging scans of the lumbar spine and ankle were performed. These tests revealed central disc protrusion at the L4–L5 and L5–S1 levels and signs of minimal chronic sprain, synovitis and retrocalcaneal bursitis in the ankle, although these findings were not conclusively linked to the patient's symptoms (Figure 3).

Lumbar spine magnetic resonance images showing disc protrusion at the L4–L5 and L5–S1 levels in a male patient in his 30s who presented with a 2-year history of persistent, involuntary twitching localized to the left sole.
Due to the ineffectiveness of the medication therapy, trials with nerve blocks were initiated. The first trial, a left tibial nerve block using lidocaine (0.4% lidocaine 5 ml), led to only a modest improvement in the severity of the twitching without decreasing the frequency or showing a lasting effectiveness. The patient reported that injections into muscles were comparatively more effective than receiving nerve blocks during previous treatments. However, the duration of relief provided by lidocaine injected into the muscles was limited to approximately 6 h. Following discussions with the patient, it was mutually agreed to pursue botulinum toxin injections as the preferred treatment approach. A subsequent trial involving injections of botulinum toxin (BOTOX®; Allergan, Dublin, Ireland; 100 IU) into the left flexor hallucis longus and digitorum longus muscles significantly reduced both the frequency and intensity of the twitching a week after injection (Figure 4). This improvement significantly enhanced the patient's daily functioning and sleep quality. A second follow-up was conducted 6 weeks after the injection and as the symptoms were not severe, the patient was advised to return as and when needed. However, the patient did not return for further treatment.

Ultrasound guided botulinum toxin injection to the flexor digitorum longus muscle in a male patient in his 30s who presented with a 2-year history of persistent, involuntary twitching localized to the left sole. A, soleus muscle; B, posterior tibial artery; C, flexor digitorum longus muscle; arrow, needle in the flexor digitorum longus muscle.
The patient provided verbal informed consent for publication of this case report. This case report was approved by the Institutional Ethics Committee of St. Vincent’s Hospital, Suwon, Korea (approval no. VC21ZISI0247). All patient details have been de-identified to ensure anonymity. The reporting of this study conforms to CARE guidelines. 9
Discussion
Botulinum toxin exerts its therapeutic effect by specifically targeting and inhibiting the release of acetylcholine, a neurotransmitter, at the neuromuscular junction.10,11 This action can significantly decrease muscle hyperactivity and twitching. By preventing normal communication between nerve cells and muscles, botulinum toxin can effectively diminish excessive muscular contractions that are characteristic of conditions presenting with involuntary twitching. 11 This mechanism of action underscores the toxin's utility in providing relief from symptoms and enhancing the quality of life for patients experiencing neuromuscular disorders. Botulinum toxin has been established as a safe and effective treatment for blepharospasm and hemifacial spasm.12,13 Its ability to temporarily paralyze affected muscles can reduce the severity and frequency of spasms, thus significantly improving the patient’s quality of life.12,13 Botulinum toxin is utilized for a multitude of purposes beyond the management of fasciculations. It is employed for the prevention and treatment of headaches such as migraines and it also serves as a non-surgical intervention for conditions such as hyperhidrosis.14–16 In addition, it is effective in treating chronic joint pain, myofascial pain syndrome and related conditions.17,18 While botulinum toxin finds broad applications with diverse purposes, especially through muscle injections, its utilization in patients with intractable fasciculation is indeed uncommon. Only one case report has documented the successful use of botulinum toxin in achieving complete resolution of fasciculations in the teres major muscle accompanied by abnormal EMG findings. 19
This particular case was noteworthy because it dealt with the challenge of managing fasciculations in a smaller muscle group that exhibited normal EMG results, a situation where traditional treatments such as peripheral nerve blocks were ineffective. The use of botulinum toxin injections in this context not only achieved complete resolution of the persistent twitching, but also highlighted the toxin's versatility and efficacy beyond its conventional applications. This successful management opens up new avenues for the therapeutic use of botulinum toxin in treating similar focal neuromuscular disorders when other treatment modalities fail to provide relief. It underscores the importance of considering botulinum toxin injections as a viable treatment option in complex cases of neuromuscular dysfunction, thereby expanding the scope of its clinical utility.
While additional research is needed to determine the optimal dosing regimen and assess the long-term efficacy of botulinum toxin injections for similar cases, our experience indicates that it could serve as a valuable treatment option for patients experiencing refractory twitching. This suggests the potential for botulinum toxin to fill a therapeutic niche for individuals who have not found relief through conventional treatments. It offers hope for improved management of challenging neuromuscular conditions.
In conclusion, botulinum toxin injection has emerged as a beacon of hope, presenting a promising therapeutic avenue for alleviating intractable twitching among patients grappling with focal neuromuscular disorders. The call for further scholarly inquiry is imperative to meticulously chart the course for optimal treatment protocols and to determine the long-term outcomes encapsulated within this intervention. This pursuit not only beckons a deeper understanding, but also heralds the dawn of refined, sophisticated approaches in the realm of neuromuscular therapeutics, embodying the confluence of elegance, intellect and clinical prowess.
Footnotes
Acknowledgements
We thank all those who contributed to this work.
Author contributions
So Young Kwon contributed to study conception, design and data acquisition. Jaesuk Kim contributed to writing the original draft. Seongjin Park and So Young Kwon provided editorial support. All authors contributed to the interpretation and analysis of the published literature as well as carefully and critically revising and approving the final manuscript.
Data availability statement
The authors confirm that the data supporting the findings of this study are available within the article.
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
