Abstract
Acquired internal nasal stenosis as a result of radiotherapy to the sinonasal region can be highly distressing for patients and difficult to correct surgically. We describe our experience using a controlled radial expansion balloon to dilate the area of stenosis, followed by stenting to the region. We achieved excellent results in 3 patients using this technique, with improvement in subjective nasal airflow across 100% of stenoses and complete resolution in 83%. This technique offers a simple and low-morbidity option for the management of acquired anterior nasal stenosis and is of particular value in cases of irradiation, which has the potential for poor tissue healing.
Acquired anterior nasal stenosis is a challenging problem. It may occur as a result of direct trauma to the nasal valve region during nasal packing and instrumentation 1 or from indirect trauma, including thermal and radiation burns. Nasopharyngeal stenosis has been reported following radiation to the nasopharynx, 2 but stenosis affecting the nasal passages is previously unreported. With the increasing use of proton radiotherapy to the sinonasal region and anterior skull base, it is likely that there will be a corresponding increase in internal nasal stenoses.
Surgical management is the mainstay of treatment for nasal stenosis. Various techniques have been described, including excision and skin grafting, laser resection, local flap rotation, and composite graft reconstruction.3,4 Repair can be difficult due to the tendency of the area to cicatrize and restenose. Balloon dilatation of congenital pyriform aperture stenosis and acquired nasopharyngeal stenosis has been described, but its utility in the setting of internal nasal stenosis has never been reported. 5
We describe a novel technique for correction of PAINS—proton-associated internal nasal valve stenosis—using a controlled radial expansion balloon dilatation, and we report our outcomes for 3 patients treated this technique.
Method
The study population was derived from the multidisciplinary skull base clinic. The intervention was offered as part of routine care and therefore exempt from approval by the Memorial Sloan Kettering Institutional Review Board.
Patients who had undergone proton radiotherapy to the sinonasal region were assessed in the office as part of their routine surveillance. Examination of the nasal passages was performed with a 0° nasal endoscope. Patients with stenoses involving the nasal passage were identified. We designed a numeric scale to describe the degree of nasal stenosis ( Table 1 ). Two surgeons graded stenoses independently, and the calculated intraclass correlation coefficient was 1.0. The dilatation procedure was offered to all patients with grade II or III nasal stenosis with symptomatic nasal obstruction.
Classification of the Degree of Anterior Nasal Stenosis.

The procedure is performed in the operating room under general anesthesia with a 0° endoscope for visualization ( Figure 1 ). The stenotic region is infiltrated with a mixture of 1% lidocaine and 1:10,000 epinephrine. The stenosis is then sharply divided with a sickle knife. An endoscopic controlled radial expansion balloon (Boston Scientific) is selected: for female patients, 10-11-12 mm; for male patients, 12-13.5-15 mm. The balloon is passed through the stenosed region and dilated to a pressure according to manufacturer instructions for 120 seconds each side. The region is reassessed, and dilatation can be repeated if required. The margins are infiltrated with 1 mL of a steroid solution (triamcinolone, 40 mg/mL). A silastic splint is inserted and remains in place for 2 weeks postoperatively. No antibiotics are administered.
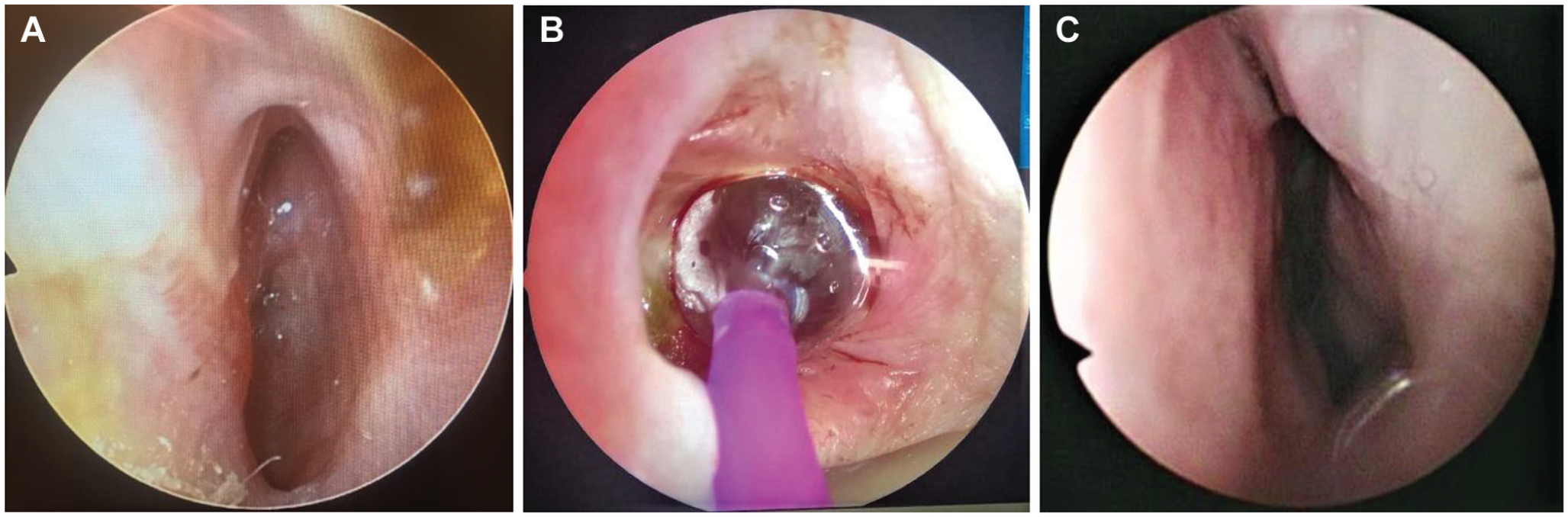
Left-sided PAINS (proton-associated internal nasal valve stenosis): (A) preoperatively, (B) dilation with Boston Scientific controlled radial expansion endoscopic balloon, and (C) 3 months postoperatively.
Results
Three patients were treated with the described technique. Each had bilateral stenosis, resulting in a total of 6 stenoses treated. The stenoses were each noted between 2 and 4 months following the completion of proton radiotherapy.
Each of the 6 stenoses was dilated with the technique described in the Methods section. All patients were followed for at least 2 months postprocedure with serial endoscopic examinations in the office, with a mean follow-up of 4 months.
All patients had improvement in their degree of nasal stenosis at last follow-up. Five of 6 stenoses remained widely patent. One patient developed local recurrence of her sinonasal undifferentiated carcinoma, requiring reirradiation; following this, she began to restenose, resulting in a more limited degree of improvement on the affected side ( Table 2 ). This could be redilated in the future if desired. There were no complications from the procedure.
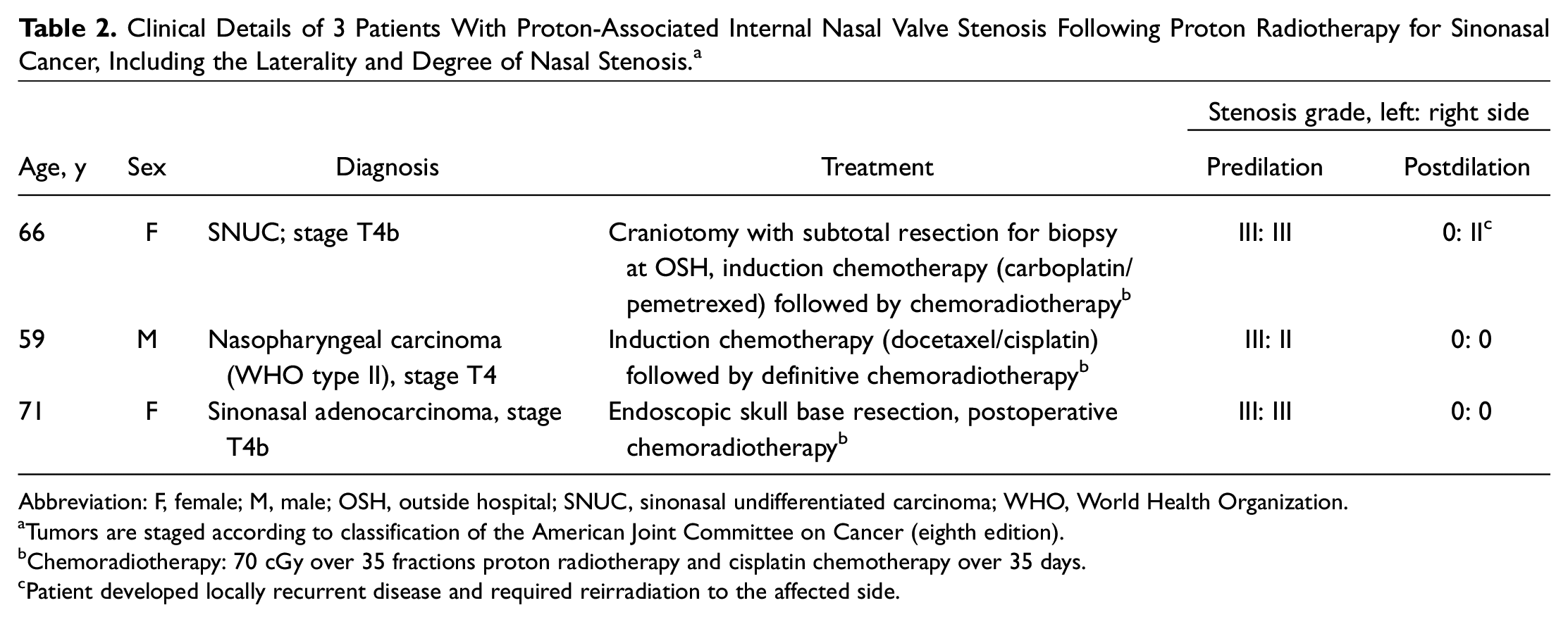
Clinical Details of 3 Patients With Proton-Associated Internal Nasal Valve Stenosis Following Proton Radiotherapy for Sinonasal Cancer, Including the Laterality and Degree of Nasal Stenosis. a
Abbreviation: F, female; M, male; OSH, outside hospital; SNUC, sinonasal undifferentiated carcinoma; WHO, World Health Organization.
Tumors are staged according to classification of the American Joint Committee on Cancer (eighth edition).
Chemoradiotherapy: 70 cGy over 35 fractions proton radiotherapy and cisplatin chemotherapy over 35 days.
Patient developed locally recurrent disease and required reirradiation to the affected side.
Discussion
Acquired nasal stenosis can be highly distressing for patients. Lack of nasal airflow results in impaired olfaction, xerostomia, and, in some, a subjective sensation of dyspnea. There is a clear indication to reestablish nasal airflow. However, achieving this goal can be particularly challenging in the postradiotherapy setting. The irradiated tissues are prone to further scarring or breakdown, so minimal instrumentation is preferable.
This is the first reported use of balloon dilatation for acquired nasal stenosis. Our results show good short-term outcomes with this technique, with no reported complications. Our results are somewhat limited by the small patient numbers and short duration of follow-up. Ongoing surveillance is required to ascertain the long-term patency of the dilatation.
The benefit of this technique as compared with more aggressive procedures lies in minimizing epithelial disruption, thereby reducing the risk of restenosis. Some have advocated for division and stenting alone without adjunctive dilatation, which reduces the procedural cost; however, we believe that dilatation results in a larger aperture. The necessity of postprocedure stenting remains to be determined. We chose to use a stent for our patients to reduce the risk of contracture and synechiae, although it is possible that this is not required due to the superior epithelial preservation. It is likely that the technique will evolve over time, and it is our hope that stenting may be reserved for those patients who have more extensive epithelial disruption—for example, those with long segment stenosis. We anticipate that this procedure could be performed in the office with local anesthesia in select patients.
Conclusion
The balloon dilatation procedure offers a low-morbidity alternative to the management of acquired anterior nasal stenosis. It is of particular value in cases of irradiation, where poor tissue healing may be considered a relative contraindication to more involved reconstructive techniques.
Author Contributions
Disclosures
Footnotes
This article was presented as a poster at the North American Skull Base Society Annual Meeting; February 7, 2020; San Antonio, Texas.
