Abstract
Objective
To assess olfactory and clinical morbidity in primary (idiopathic)–type atrophic rhinitis and its course following treatment.
Study Design
Prospective nonrandomized controlled cohort study with follow-up.
Setting
Department of Otorhinolaryngology and Head and Neck Surgery of a university hospital (tertiary heath care center).
Methods
Sixty-one patients with atrophic rhinitis underwent assessment of clinical severity with baseline olfaction with the Brief Smell Identification test, while the improvement of their status following surgical versus nonsurgical treatment was further assessed.
Results
Olfaction was universally deranged with bimodal age presentation and female predominance (61%). Clinical improvement was significantly associated with surgical treatment but did not reveal any relation with up-front severity of disease. A near-significant association of age with severity did not reveal significance when stratified by age group. Baseline olfaction or its change following treatment did not reveal any significance with severity of disease or clinical improvement. Radiologic atrophy also did not reveal any significant relation with severity criteria.
Conclusions
Olfactory functions as compared with clinical parameters provided better reflection of underlying (systemic) pathology with environmental interaction, while later it mainly signified localized condition. Accordingly, olfaction was affected early and recovered slowly (or not at all), independent of clinical morbidity, which in turn is affected rather late but recovers early. Olfactory dysfunction at the initial stage may be a surrogate marker of potential worsening clinical condition, since bacteria often superinfect underlying susceptible nasal environment. While surgery mainly improved clinical parameters without affecting olfaction directly, a true improvement would include recovery of both.
Keywords
Primary atrophic rhinitis (ATR) is characterized by chronic progressive atrophy of the mucosa and greenish crusts responsible for foul odor (ozaena). A wide roomy nasal cavity resulting from bony (turbinates) resorption is a characteristic feature with abnormal patency.
1
ATR is predominantly seen in women (6:1.5).
2
It is common in tropical countries3,4 and more prevalent with lower socioeconomic status and poor hygiene.
5
The etiology is debatable. Polygenic inheritance is appreciated in 15% to 30%, in addition to autosomal dominant (67%) or recessive (33%)
6
penetrance. Chronic bacterial infection is implicated,4,7 particularly
Method
This prospective study is based on 61 patients with ATR attending a university hospital of North India. Proper ethical clearance was obtained by the institutional review board of the King George’s Medical University India (reference code 72nd ECM II A/P2; May 2015), and informed consent was undertaken. The inclusion criteria included wide nasal cavity, mucosal atrophy, and thick crust with or without epistaxis or ozaena. Those with secondary ATR, mental retardation, and pregnancy were not included. Apart from routine anamnesis, classical nasal endoscopy focused on mucosal atrophy, bony resorption, thick crust, fetid odor, and free mucous. Nasal swab and mucosal sample were obtained for microbiological and histopathologic examinations, respectively. The disease was defined arbitrarily as
Arbitrary Criteria Used for Defining Categories.

While most patients with predominantly mild-moderate disease refused to undergo surgery, the surgical arm focused mainly on the severe disease category. Despite surgical counseling, the preference of nonsurgical treatment by a majority of patients is not uncommon in India. Surgical candidates underwent modified Young’s operation with continued multivitamin support and subsequent recannulation after 8 months. The modified Young’s procedure permits a 1- to 2-mm residual aperture, as opposed to complete closure as in classical Young’s surgery. The rationale of selecting the former was to allow some odorant stimuli into the nasal cavity to not hamper sensitivity of olfactory nerves by depriving them of any stimulus. The nonsurgical candidates were prescribed nasal lubricants with continued alkaline douche and multivitamins for 8 months. A fresh alkaline solution douche (NaCl [36.7 g] + Na2CO3 [28.4 g] + sodium diborate [28.4 g] in 280 mL of water) has been specially mentioned 18 for ATR. Within 2 weeks following completion of 8 months of either treatment, repeat nasal endoscopy (for reappearance of free mucous), nasal swab examination, and olfactory assessment (BSIT) were undertaken. Hence the first BSIT assessment was carried out just before the start of the treatment, while the second was undertaken within 2 weeks following completion (mean, 8 days). Therefore, pretreatment BSIT score and difference of scores (pre- vs posttreatment) were 2 olfactory parameters used for analysis. Arbitrary subjective and objective criteria were considered to label the clinical improvement as either satisfactory or unsatisfactory ( Table 1 ).
The following comparisons (analyses) were performed to better understand the disease process:
Mean BSIT score of severe versus mild-moderate category with a
Mean BSIT score of satisfactory versus unsatisfactory improvement with a
Mean difference in BSIT scores between satisfactory and unsatisfactory improvement with the
Mean radiologic atrophy (radiolucent area) of severe versus mild-moderate category with the
Mean difference in BSIT scores between severe and mild-moderate category with the
Mean age between severe and mild-moderate category with the
Two categories of disease severity were compared with 2 categories of clinical improvements via the 2 × 2 table and chi-square analysis with 1 degree of freedom.
Two categories of treatments were compared with 2 categories of clinical improvements via the 2 × 2 table and chi-square analysis with 1 degree of freedom.
The distribution of age groups was compared between severe and mild-moderate disease via the chi-square test with 5 degrees of freedom.
SPSS (v 21; IBM) was undertaken for analysis. The discrete/categorical variables were analyzed by chi-square test and the continuous variables by
Results
A clear predominance of younger age and female (61%) sex was noted. The age varied between 18 to 72 years, and its distribution with sex is depicted in Figure 1 . About a third of patients (31%) were <30 years old (female, 52.63%) while another peak (31%) was between 45 and 55 years old (female, 73.68%). However, there was a clear dip in incidence in the fourth decade. With a single case in the eighth decade, any definite conclusion cannot be made. Importantly, extreme degrees of bony resorption with saddle nose and palatal perforation are still seen in India ( Figure 2 ).
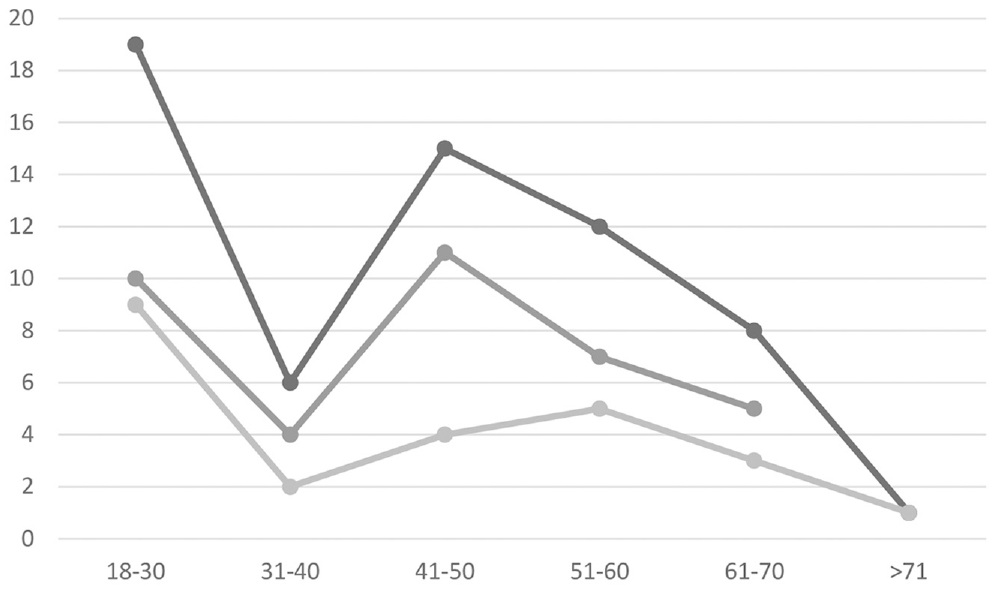
Age distribution with sex variability. Frequency is charted on the
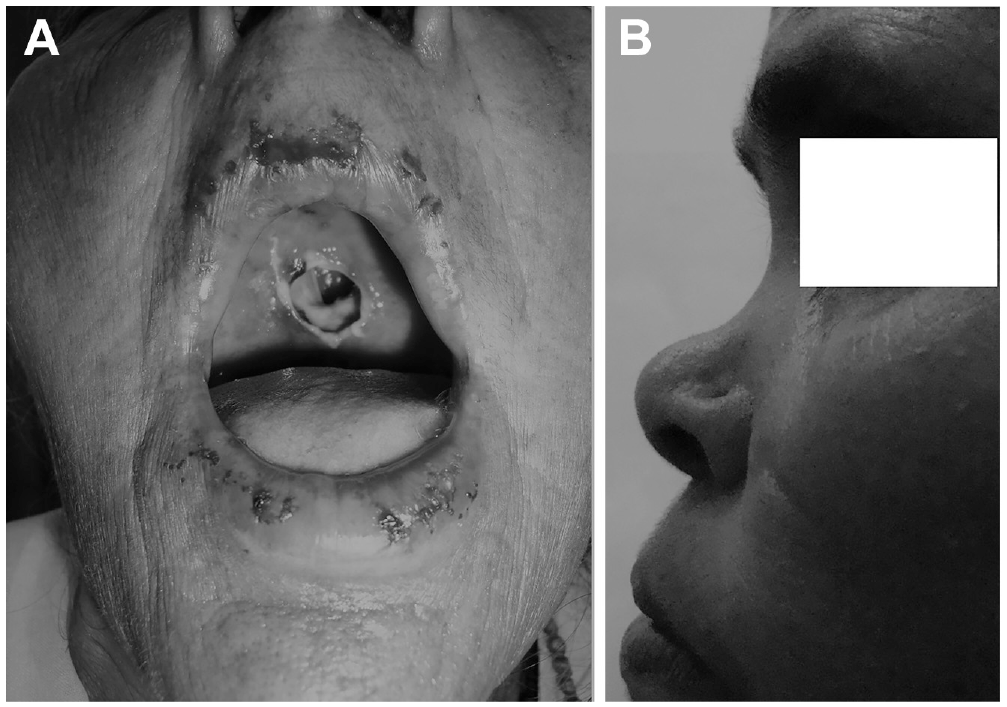
Bony resorption in advanced atrophic rhinitis resulting in (A) palatal perforation and (B) saddle nose.
A comprehensive summary of all observations and parameters used in the analysis is presented in
Table 2
. Olfactory dysfunction was universally present. Anosmia and hyposmia were appreciated in 13 (22%) and 46 (78%) cases, respectively. The distribution of females and males with anosmia was 38.46% (n = 5) and 61.53% (n = 8) and with hyposmia 65.21% (n = 30) and 34.78% (n = 16). Only 5 hyposmic cases (8.47%) belonged to the near-normal category. Mild-moderate disease was seen in 16 (27.11%) and severe in 43 (72.88%). Male incidence was marginally more in the severe category (41.86%) than in the mild-moderate group (37.5%). Of the 55% of cases that showed
Comprehensive Summary of Clinical, Radiologic, and Olfactory Parameters Before and After Treatment. a
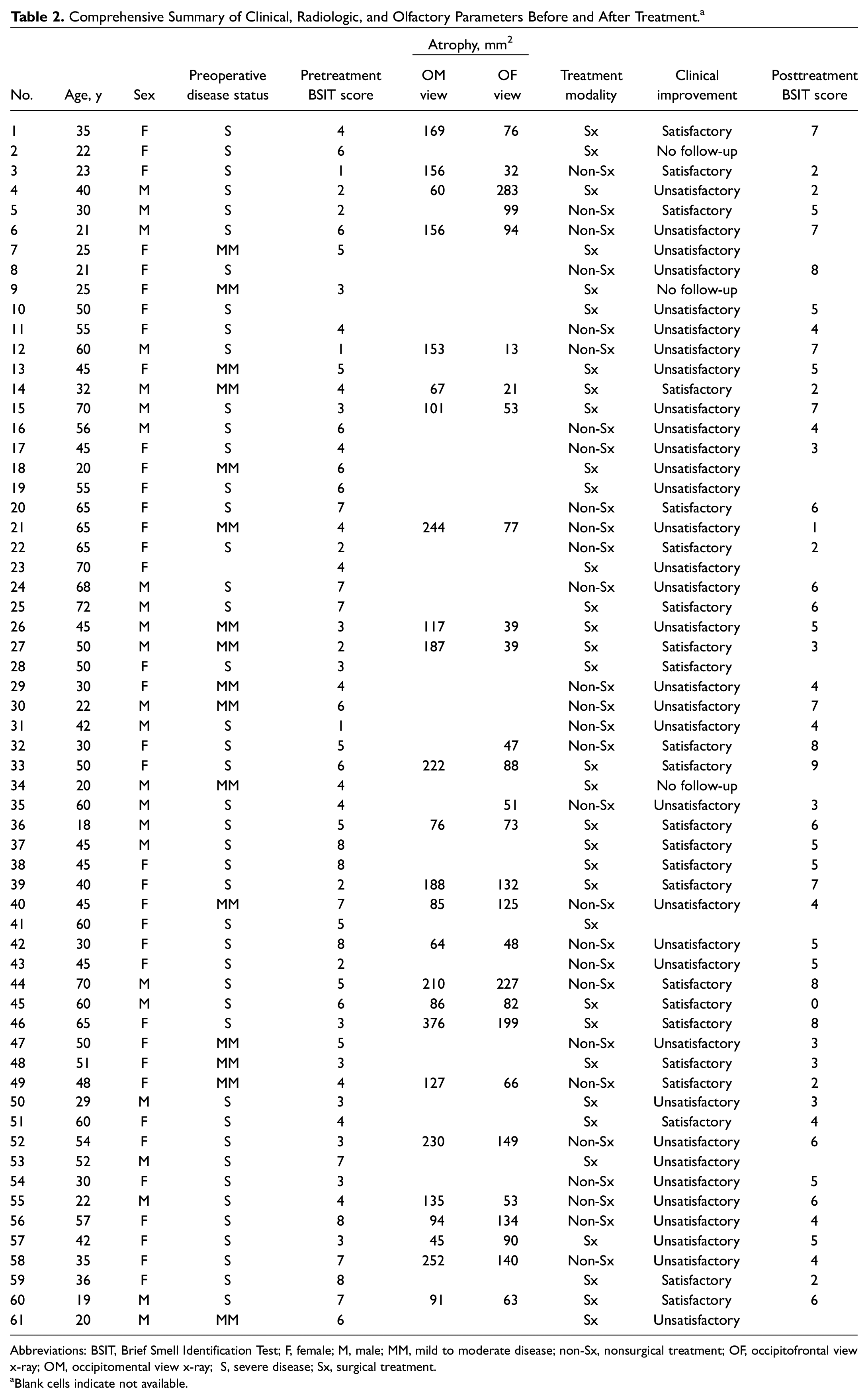
Abbreviations: BSIT, Brief Smell Identification Test; F, female; M, male; MM, mild to moderate disease; non-Sx, nonsurgical treatment; OF, occipitofrontal view x-ray; OM, occipitomental view x-ray; S, severe disease; Sx, surgical treatment.
Blank cells indicate not available.
Statistical Analysis.
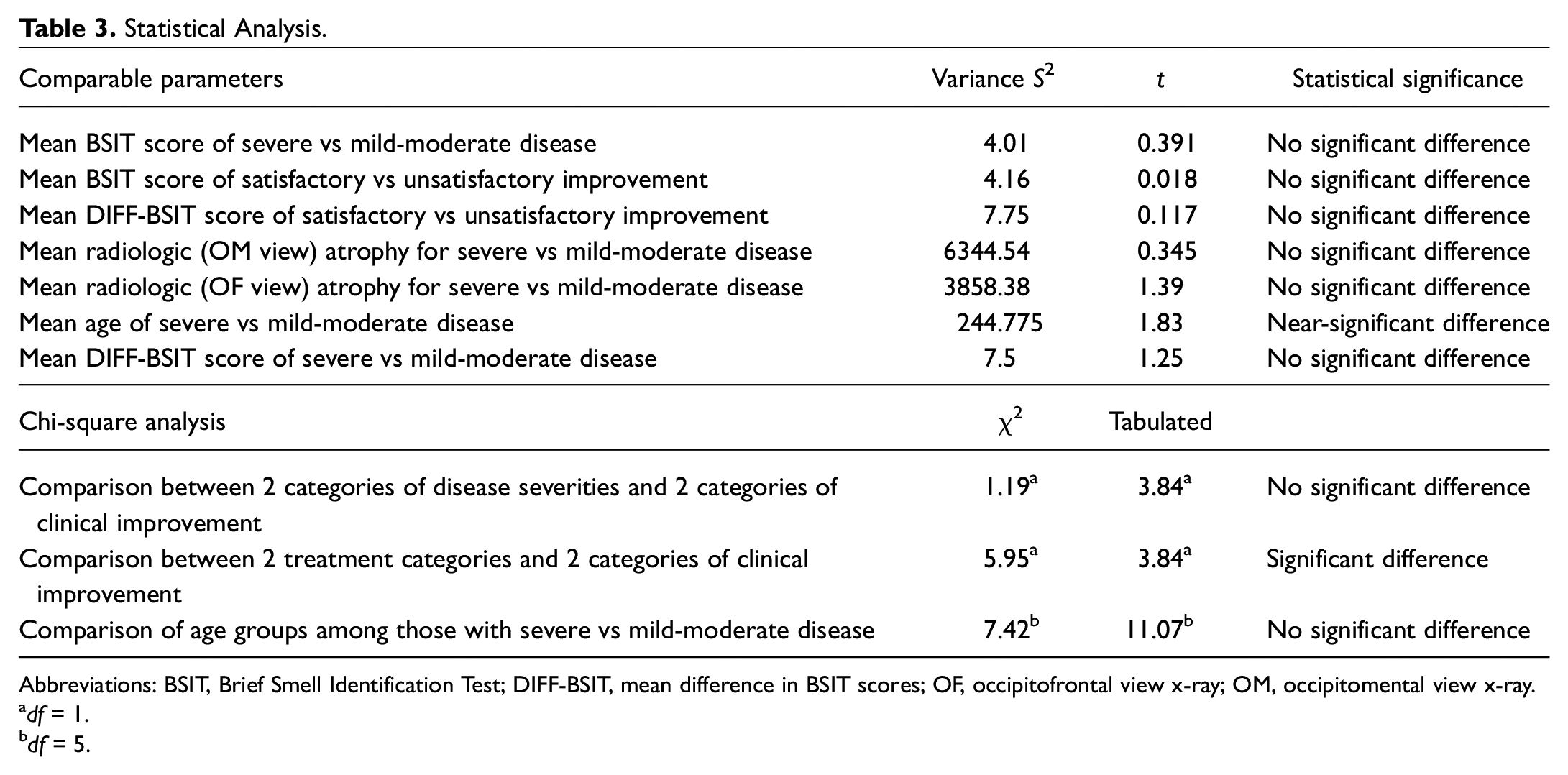
Abbreviations: BSIT, Brief Smell Identification Test; DIFF-BSIT, mean difference in BSIT scores; OF, occipitofrontal view x-ray; OM, occipitomental view x-ray.
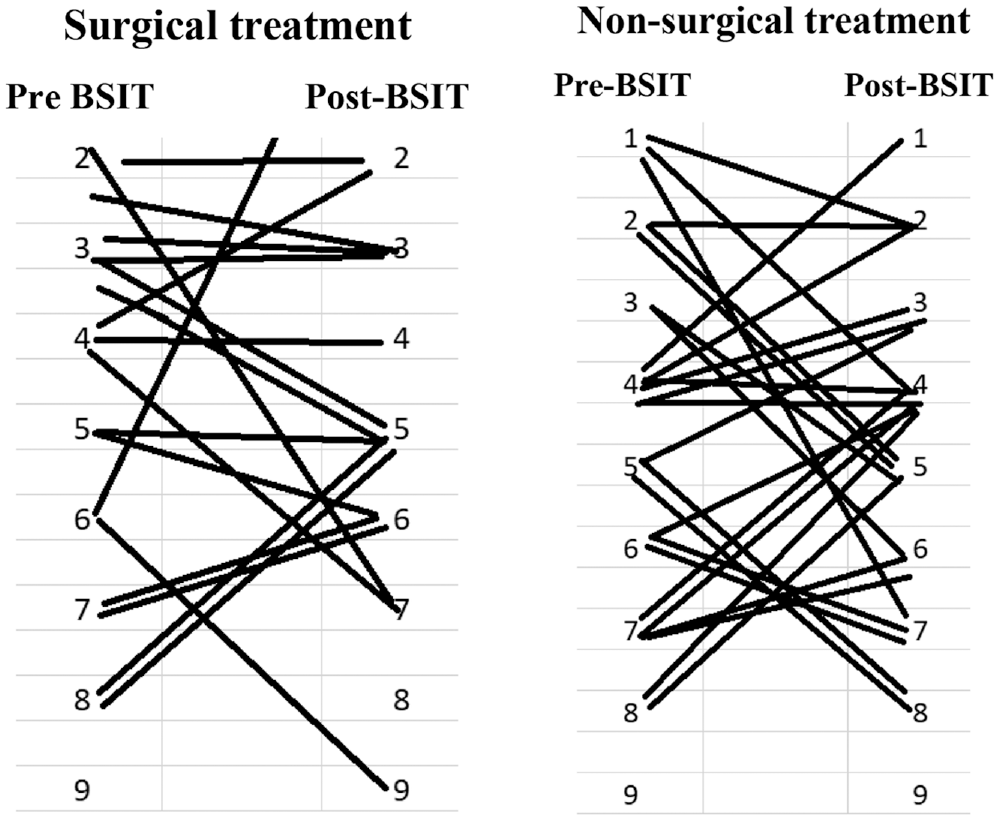
Changes in Brief Smell Identification Test (BSIT) scores with surgical and nonsurgical treatments.
Discussion
Olfaction was universally deranged in ATR. Bimodal age presentation and female predominance were noted. Better clinical improvement was significantly associated with surgical treatment, suggesting the latter as better modality over nonsurgical treatment. However, the degree of clinical improvement did not show any relation with up-front severity of disease. A near-significant association of age with severity of disease did not, however, reveal significance when analyzed for different age groups. Baseline olfactory status or change in olfaction following treatment did not show any relationship with severity of up-front disease or clinical improvement criteria. Finally, radiologic atrophy showed no significance with severity criteria.
The main strength of this study is the first-time use of a validated psychophysical scale (BSIT) in assessment of olfactory dysfunction of ATR and olfaction with disease severity and the effect of nonsurgical and surgical management on olfaction. Despite limited cases, our sample is still the largest. Better results may theoretically be obtained by comparing different etiologic subsets independently, but this again may be difficult for this rare disease. Moreover, there is potential bias for allocating the severe category to the surgical arm; hence, it is possible to better appreciate large subjective improvement as compared with smaller change in the mild-moderate category. A proper randomized controlled trial may resolve this issue. In the absence of high-resolution imaging due to financial constraints, plain radiography seems very crude to conclude a nonsignificant association. In addition, histologic assessment of ultrastructural mucosal changes was not possible in all cases. Furthermore, this study did not include any validated quality-of-life assessment mainly due to the fact that none to date has been developed for ATR exclusively and using the existing ones may not truly reflect this particular disease per se. Hence, subjective and objective parameters, though arbitrary but specific to ATR, were selected to score improvement. Here it is important to mention that the arbitrary definitions cited in
Table 1
were based on our institutional experience for >6 decades (with S.C.M. being faculty since 1966). Selected criteria are most essential (per the literature) and seem quite practical to be adapted in countries with limited resources where ATR is more prevalent. With only basic objectivity criteria, the current scoring algorithm (satisfactory/unsatisfactory) is easy to reproduce and likely to help in validation. Assessment following antibiotic course (before starting definitive treatment) was purposely not undertaken, since the aim was to assess comprehensive improvement at the end of treatment. Ignoring the presence of bacteria other than
Anosmia in ATR is well appreciated in the literature1,13,19 and reported to occur between 40% and 91%.
20
Anosmia may be due to nerve inflammation, atrophy of olfactory mucosa, derangement in the central olfactory pathway, or reduced air entry due to crusts. The loss of sensory nerves of the nasal cavity reduces local sensations, and the cumulative effect makes the patient unaware of foul nasal discharge. In addition, flies (
The age distribution in our population revealed 2 peaks at comparatively younger age groups, while the elderly population was relatively less affected. These peaks roughly correspond to puberty and menopause. The therapeutic effect of estrogen on 1 subset of ATR has already been mentioned, 17 suggesting some possible endocrinal influence. The genetic factors may also play some role in preferential age presentation. Although radiologic assessment of atrophy was undertaken by 2 persons independently, the nonsignificant association with severity of disease is not unexpected, given the small sample, nonuniform quality, and difficulty in deciding areas of atrophy. Hence, radiography can best help in documenting maxillary sinusitis or bony erosion (myasis).
The lack of significant objective recovery of olfaction may be due to the predominance of patients with severe disease (73%) that may have significantly affected olfactory functions; moreover, the follow-up period may have been too short to assess any neurologic recovery. Since baseline olfactory status did not always reflect up-front clinical severity, it may be possible that olfactory functions are sensitive enough to be affected much earlier. This, however, does not support the fact that all those with near-normal olfaction (BSIT score = 8) had severe disease on presentation, and the olfactory scores, despite surgical management, eventually worsened. Also since the recovery of olfaction was no different between mild-moderate and severe disease, it is possible that other influences (eg, genetic, metabolic, endocrinal, autoimmune, degenerative, inflammatory) may be more important than simply mucosal atrophy, osteocartilaginous resorption, or anatomic obstruction induced by dried crusts in so-called advanced disease. Again, since recovery of olfaction did not show any relation with clinical improvement, it is assumed that clinical improvement occurs early independent of olfactory recovery and that the olfactory functions are either quite slow to recover or do not recover fully after being irreversibly damaged. Hence, it seems evident that the pattern of olfactory dysfunction in ATR is quite different from the usual clinical parameters, and while the latter may add to the dysfunction of former, both progress and regress independently. Good clinical improvement may be a prerequisite for improvement in olfaction, but that in turn does not guarantee satisfactory olfactory recovery. Since surgical treatment was significantly associated with better clinical improvement, it is likely more effective in resolving local conditions with associated recurrent infections (and not necessarily olfaction) as seen with empty nose syndrome. Near-total surgical closure (modified Young’s) is likely to prevent mucosal desiccation and secondary bacterial invasion, as opposed to medical management with an open nasal aperture. The various shades of olfactory losses do suggest some ongoing neuropathy, and surgical closure to facilitate clinical improvement will provide a favorable environment for olfactory recovery and even prevent further insult induced by recurrent infections, dryness, or crusting. Otherwise, surgery per se may not have any direct effect on improvement of olfaction, with dysfunction being a combined systemic and environmental effect. Long-term studies need to be undertaken to establish the same.
As a nonuniform outcome of antibiotics on ATR is reported in immigrants with different backgrounds, 23 resistant infection may account for nonsatisfactory clinical improvement, as seen in 59.64%. Its incurable yet nonfatal status was well addressed by Fraenkel in 1876. 24 The ongoing postinflammatory fibrosis and existing endarteritis or periarteritis 25 may resist recovery of olfactory functions. Since bacteria superinfects the underlying immunocompromised (susceptible) nasal environment, olfactory dysfunction detected at an initial stage may be considered a surrogate marker of clinical worsening. Studies involving early ATR are required to establish the same, and unfortunately, our study could recruit only full blown established cases as the patients in India usually present late in the course of illness..
The conclusion regarding relevant clinical care based on this study is straightforward. Since the onset and recovery of olfactory and clinical parameters in ATR occur independently (except for being indirectly related) it is likely that even after complete clinical recovery of ATR, the residual olfactory deficit may reflect a fragile residual state with a potential for repeat worsening of the clinical condition and a possibility of bacterial superinfection. Hence, it is important to continue proper lubrication, local care, and conservative management with repeated follow-up olfactory assessments to determine either a true improvement or further deterioration in fragile residual state depending on the underlying immunologic state. It is the latter subset that needs particular attention. Larger studies are needed to better understand the relationship of olfaction with multiple etiologic factors to enhance the quality of life of patients of low socioeconomic status in resource-poor countries .
Author Contributions
Disclosures
Supplemental Material
appendix – Supplemental material for Olfaction in Primary Atrophic Rhinitis and Effect of Treatment
Supplemental material, appendix for Olfaction in Primary Atrophic Rhinitis and Effect of Treatment by Anupam Mishra, Nimisha Mishra Shukla, Veerendra Verma and Subhash Chandra Mishra in OTO Open: The Official Open Access Journal of the American Academy of Otolaryngology-Head and Neck Surgery Foundation
Footnotes
Acknowledgements
We acknowledge Professor Richard L. Doty, director of Smell and Taste Center, Department of Otorhinolaryngology and Head and Neck Surgery, Hospital of University of Pennsylvania, for his time, guidance, as well as moral support. In addition, Dr Girja Kant Shukla, professor of statistics, Indian Institute of Technology Kanpur and Indian Institute of Management Lucknow, needs due acknowledgment for his statistical guidance and support.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
