Abstract
Removal of foreign bodies from the infratemporal fossa is surgically challenging and fraught with risks. This report describes our experience with a minimally invasive transoral technique, utilizing endoscopic and image guidance technology, for retrieval of infratemporal fossa foreign bodies in 6 patients. The technique was successfully applied in all cases with identification and retrieval of the foreign bodies, which included 4 hypodermic needles broken off during dental injections, a cottonoid surgical sponge lost during a facial fracture repair, and a maxillary molar displaced during attempted extraction. Complications were limited to transient postoperative lingual and inferior alveolar nerve sensory deficits in 1 patient.
Although foreign bodies of the infratemporal fossa (ITF) are rare, when they do occur, retrieval can be challenging because of the close proximity to neurovascular structures. Dislodgment of the third molar into the ITF has been reported as a complication of extraction, 1 as have broken-off needles used for local anesthesia. 2 If a foreign body (FB) is not retrieved from the ITF, persistent inflammation and infection may occur, resulting in temporomandibular joint impairment with chronic pain and trismus, as well as pseudoaneurysm or arteriovenous fistula formation. 3 Several techniques have been described for surgical retrieval of such a FB, ranging in invasiveness from the hemicoronal 4 to the transoral approach.1,5 Herein we describe our experience with a novel image-guided, endoscopically assisted transoral technique for FB retrieval from the ITF.
Methods
A retrospective review was performed of patients who underwent removal of a FB by the senior author (R.M.) between 2005 and 2018. Approval was granted by the Institutional Review Board of Partners HealthCare (protocol 2019P000571).
Each patient underwent preoperative computed tomography (CT) scan to localize the FB ( Figure 1 ) and enable image guidance use (KARL STORZ optical navigation system) during retrieval ( Figure 2 ). The preoperative CT scans performed at our institution were completed with each patient’s mouth in an open position to simulate anatomic positioning in the operating room. All surgical procedures were performed under general anesthesia with use of a Molt mouth gag, paddle retractors for the tongue and buccal tissue, mosquito dissector, needle-tip monopolar electrocautery, and image guidance probe.
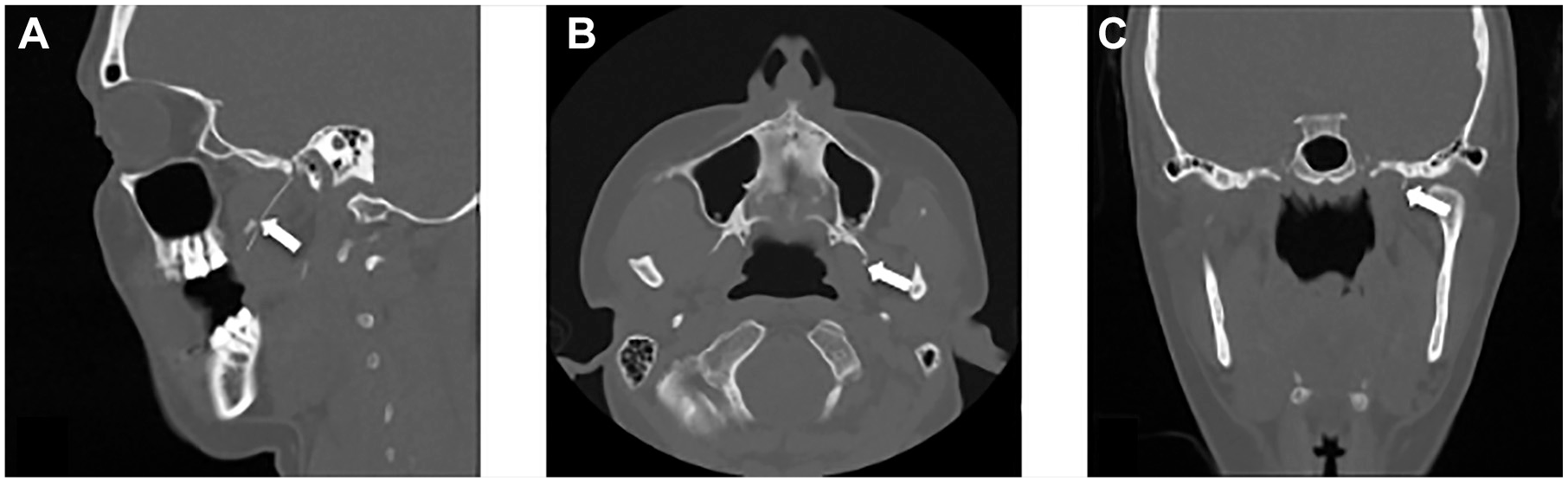
Preoperative computed tomography imaging of a needle foreign body in the infratemporal fossa (case 6). (A) Sagittal view shows the needle in the infratemporal fossa. (B) Axial view. (C) Coronal view.
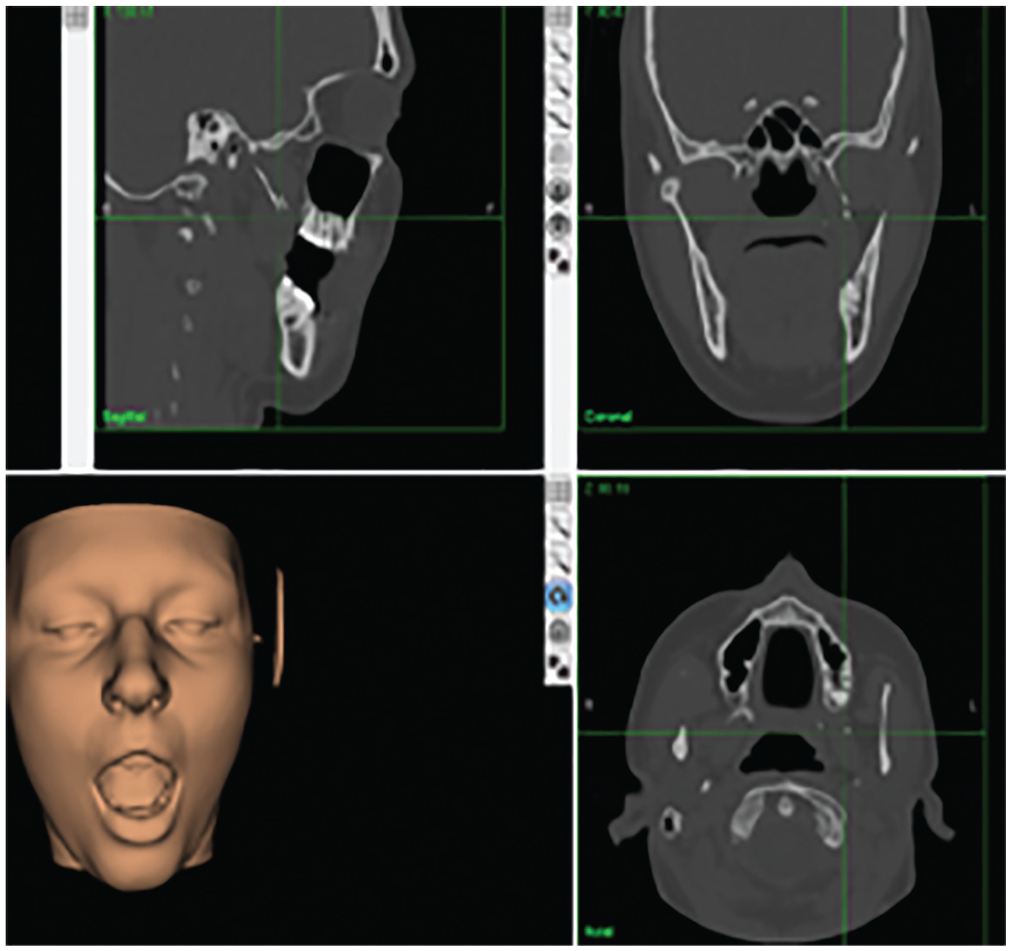
Intraoperative image guidance monitor view shows localization of a foreign body within the infratemporal fossa (case 6). Crosshairs depict the image guidance probe tip. The preoperative computed tomography with the patient’s mouth open anticipates intraoperative foreign body movement.
Surgical Technique
An approximately 2-cm intraoral incision was made just medial to the mandibular ramus in the gingivobuccal sulcus on the side of the FB ( Figure 3 ). An image guidance probe and endoscope were then passed through the incision. The probe was slowly advanced until its tip was in contact with the FB in the axial, coronal, and sagittal planes as verified on the image guidance monitor. A needle-tip electrocautery was then used to hemostatically dissect along the nonconductive probe shaft in short bursts. Continuous placement of the probe tip at the FB allowed for ongoing verification of the trajectory of dissection with frequent pauses to confirm this on the image guidance monitor. In this fashion, dissection was undertaken through the surrounding pterygoid musculature until the FB was visualized through the endoscope in the vicinity of the probe tip. A mosquito dissector was then used to stabilize and withdraw the FB. (See Supplemental Video for an example of the surgical technique.)
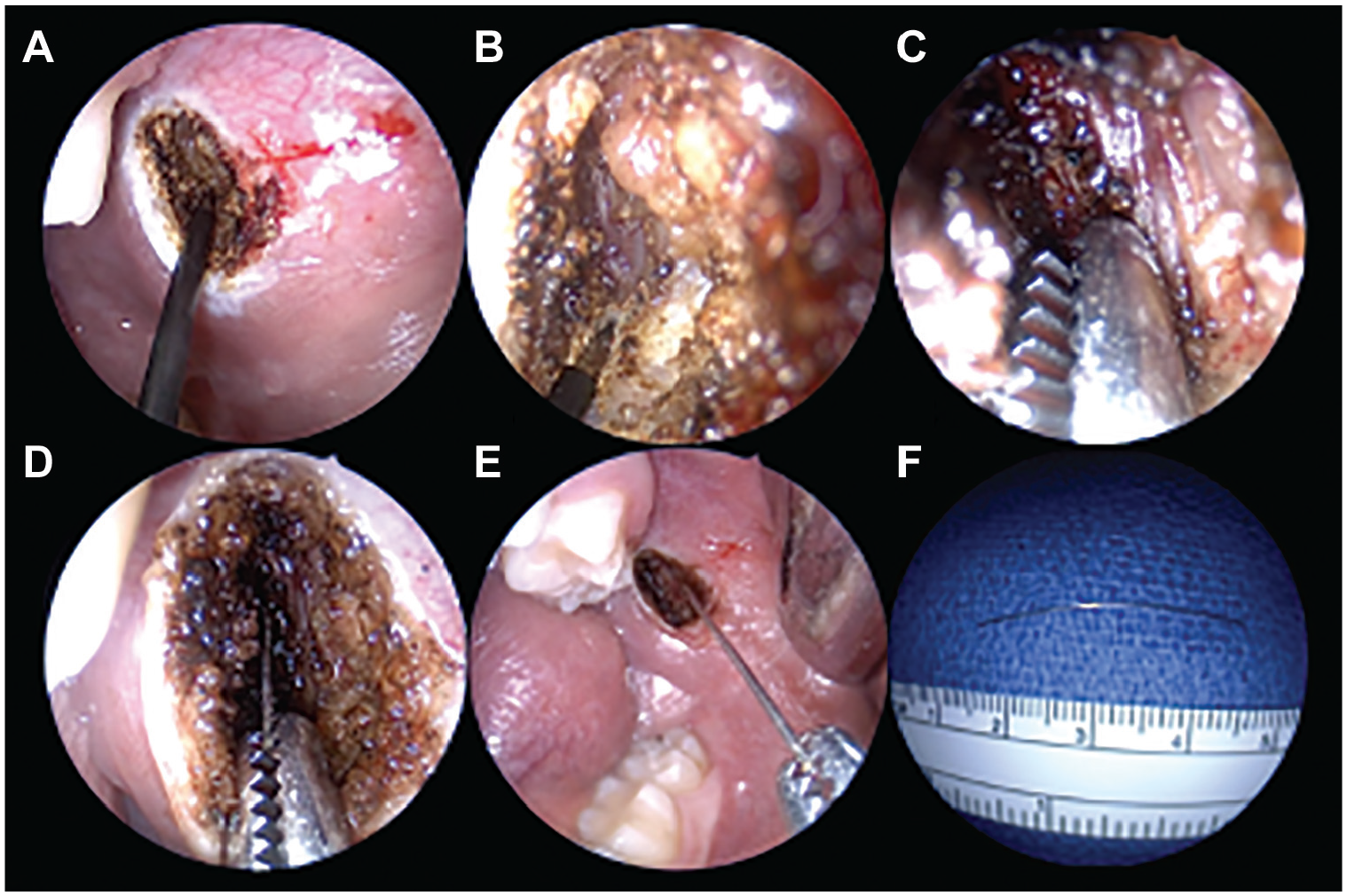
Endoscopic transoral retrieval of an infratemporal fossa foreign body. Through (A) an intraoral incision, (B) electrocautery dissection revealed (C) the needle tip, which was (D) grasped, (E) removed, and (F) measured (case 6).
Results
The described technique of ITF FB retrieval was performed in 6 patients, 3 of whom were male, with a mean ± SD age of 28.6 ± 19.0 years. Retrieved foreign bodies included 4 hypodermic needles (length, 19-33 mm), a cottonoid surgical sponge, and a maxillary molar. The duration of FB retention from the time of loss until removal ranged from 6 to 146 days (median, 17 days). Complications were limited to postoperative lingual and inferior alveolar nerve sensory deficits in 1 patient (case 5), which resolved after 2 months. Patient demographics and case details are listed in Table 1 .
Patient Demographics, Foreign Body Characteristics, and Pertinent Case Notes.
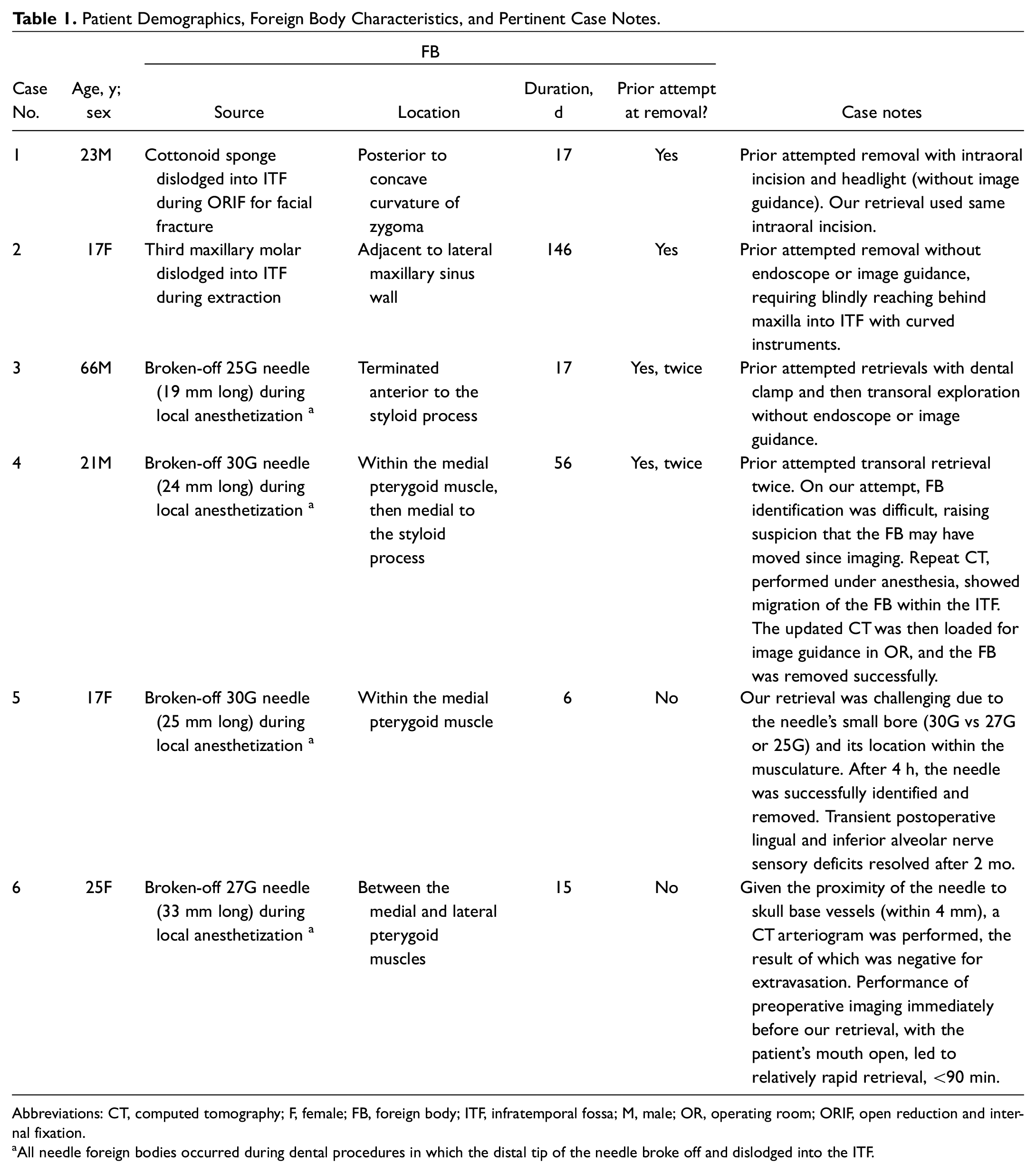
Abbreviations: CT, computed tomography; F, female; FB, foreign body; ITF, infratemporal fossa; M, male; OR, operating room; ORIF, open reduction and internal fixation.
All needle foreign bodies occurred during dental procedures in which the distal tip of the needle broke off and dislodged into the ITF.
Discussion
Removal of foreign bodies from the ITF is surgically challenging and fraught with risks. Injury to the internal maxillary artery and pterygoid venous plexus may result in untoward bleeding. 1 The chorda tympani, otic ganglion, and trigeminal nerve branches present risks of neural injury. 1 Indeed, in case 5, a small-bore broken-off needle FB required extensive dissection around the pterygoid musculature within which it was lodged, likely resulting in the observed transient neuropraxia of the lingual and inferior alveolar nerves, 2 branches of the trigeminal nerve’s mandibular division that are near the pterygoid musculature in the ITF. Furthermore, migration of a FB during attempted removal in the ITF may endanger additional critical structures, such as those within the infraorbital fissure, which could result in visual loss. 2
Whereas retrieval of ITF foreign bodies has been described with either image guidance (transnasally) 2 or endoscopy (transorally),1,5 the technique described in this report leverages the advantages of endoscopy, image guidance, and the transoral approach in combination. The endoscope allows for optimal visualization throughout the procedure, while image guidance confirms the appropriate dissection trajectory, as well as the proximity of critical structures. The transoral approach minimizes patient morbidity by providing direct access to the ITF without the need for external incisions or resection of intervening structures, as is often necessary when approaching from alternative vectors.
The following technical pearls may help overcome pitfalls in the treatment of patients with ITF foreign bodies. Preoperative imaging should occur (1) immediately prior to the operating room to ensure accurate FB localization and (2) with the patient’s mouth open to mimic the anatomic position during surgery. Adequate exposure is achieved with ample retractor use. Once the FB is localized with the image guidance probe, electrocautery is used in short bursts along the probe, while the image guidance monitor is used to confirm the accuracy of the dissection trajectory and the absence of intervening critical structures before each short burst of electrocautery. Bleeding can often be controlled by needle-tip electrocautery. Suction electrocautery may be used judiciously if higher-volume bleeding is encountered. Avoiding manual palpation within the ITF reduces inadvertent FB migration. If not found within a reasonable time, a FB may be relocated with intraoperative CT.
Conclusion
Our experience demonstrates the safety and efficacy of a minimally invasive transoral approach, utilizing endoscopic instrumentation and image guidance, for the treatment of patients who present with foreign bodies of the ITF.
Author Contributions
Disclosures
Footnotes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
