Abstract

Keywords
First reported in 1918 by Schottmuller and further popularized by Andre Lemierre in 1936, Lemierre’s syndrome (LS) is characterized by a history of recent oropharyngeal infection, clinical or radiologic evidence of internal jugular vein (IJV) thrombosis, and isolation of an anaerobic pathogen, mainly Fusobacterium necrophorum. 1 It is also named postanginal sepsis or necrobacillosis and is seen mostly in healthy teenagers and young adults. 2 Anaerobic infection may result in septic thrombophlebitis of the ipsilateral IJV with subsequent septicemia and septic embolization, which cause metastatic abscesses in the lungs, bones, large joints, liver, kidneys, and peritoneum.
Since the discovery of penicillin in the 1940s, the incidence of LS has dramatically fallen. 3 According to one review, however, 121 LS articles were written between 2001 and 2008 versus 6 between 1980 and 1990. 2 This rapid increase can be attributed to increased cases due to antibiotic resistance, changes in the pattern of antibiotic prescriptions, and higher-resolution scanning for the easy diagnosis of IJV thrombosis. In the preantibiotic era, LS often followed a fulminant course with a mortality rate of 90%. 1 More recently, the mortality rate quoted in different studies averages 5%. 3 Institutional Review Board and ethics committee approval was obtained via the West Cancer Center for this study.
Case Report
A 45-year-old-man presented to the Veterans Administration Medical Center–Memphis. He had a history of polysubstance abuse and was admitted for agitation and mental status changes. Admission history and physical examination revealed a sore throat for 2 weeks prior to presentation. Admission drug screen was positive for opioids and alcohol. He developed fever, painful right neck swelling, and trismus on the fifth hospital day. No lesions of visible oral and pharyngeal mucosa were found, but prominent erythema, tenderness, and edema were noted in the submandibular area extending posteriorly to the angle of the mandible and inferiorly to the level of the clavicle. Blood culture was positive for Staphylococcus aureus, and white cell count was elevated. Contrast-enhanced computed tomography (CT) ruled out a deep neck abscess and detected complete absence of intravenous contrast at the level of the jugular foramen. Multilevel cervical subcentimeter lymph nodes were also present on axial view. Reconstructed sagittal images delineated a thrombus in the IJV from the jugular foramen to the angle of the mandible with diffuse soft tissue stranding, confirming LS. Culture-directed intravenous antibiotics were administered, and anticoagulation was instituted. Subsequently, fever and neck swelling resolved. Reconstruction of initial axial CT images confirmed the diagnosis of LS ( Figures 1 and 2 ).
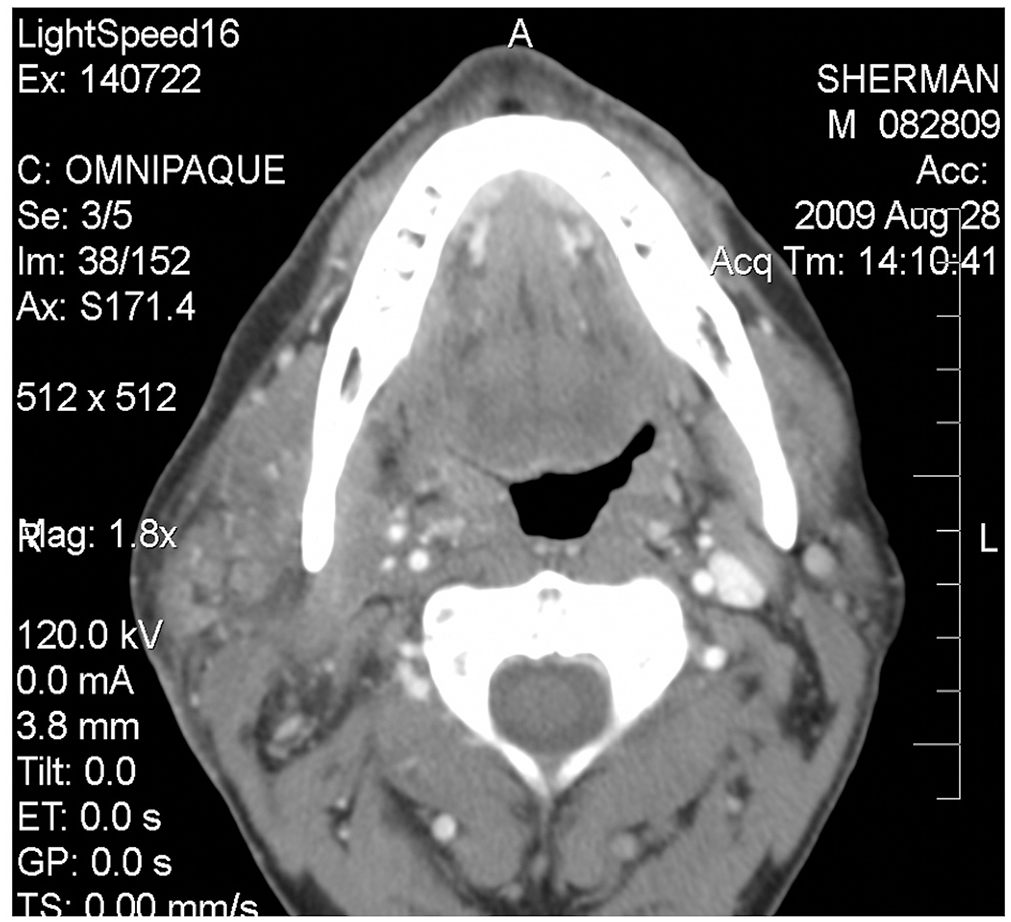
Axial view demonstrates the lack of contrast in the right internal jugular vein just above the angle of mandible.
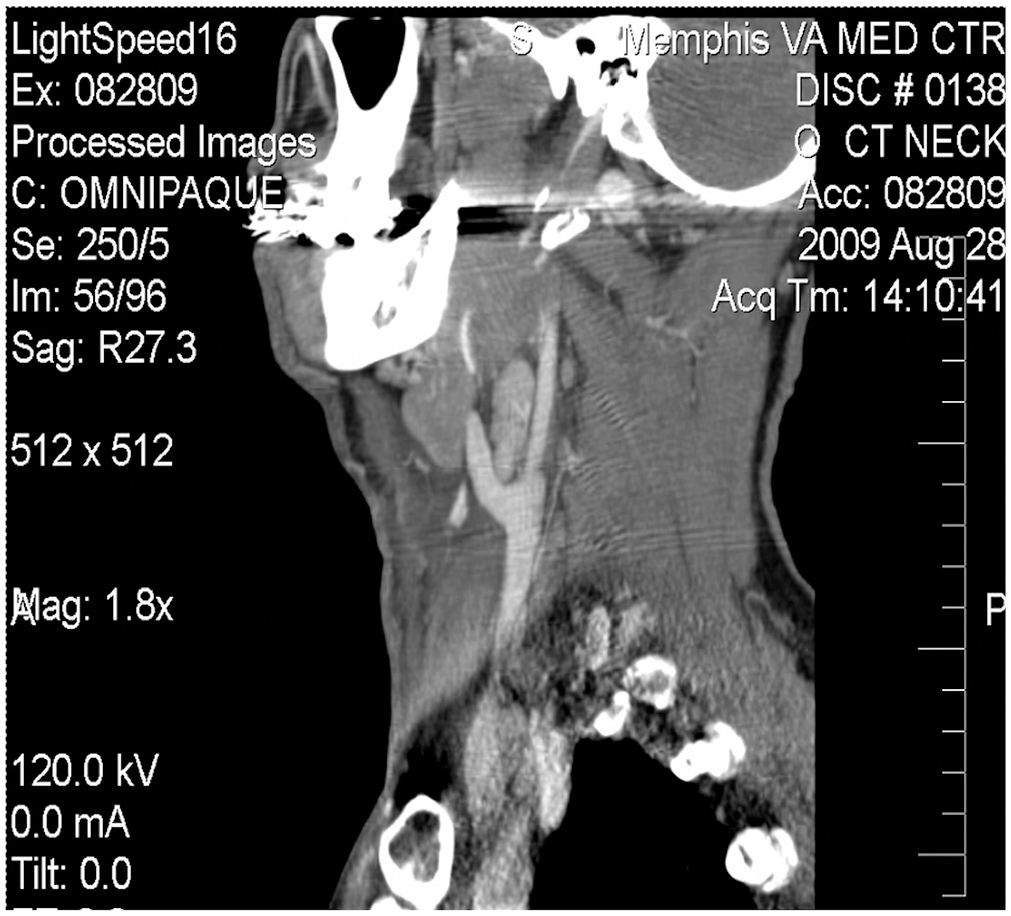
Sagittal view shows the right internal jugular vein and common facial vein with a lack of contrast in the vein above the angle of mandible.
Discussion
Although F necrophorum is involved in most cases (81%), 4 additional pathogens that can cause LS include other Fusobacterium species, Bacteroides, and group A, B, and C streptococci. Community-acquired methicillin-resistant S aureus bacteremia has been also reported. 5 F necrophorum is peculiar in its ability to invade as a primary pathogen without the presence of serious underlying disease. Infection of the parapharyngeal space occurs as a result of direct spread of infection from the tonsillar bed or by lymphatic or venous dissemination.
Contrast-enhanced CT is the imaging study of choice to assess for neck pathology, including thrombus in the IJV or an abscess in the deep neck spaces. However, to more definitively demonstrate IJV thrombosis, additional imaging studies can be done, such as ultrasound or contrast angiography. Ultrasound has the advantage of being an investigation without ionizing radiation. However, thrombi below the clavicle and above angle of the mandible can be missed. Early thrombi without an organized clot may be overlooked. It is also operator dependant. 2 Traditional angiography is invasive and requires high doses of contrast.
As in our report, multiplanar reconstruction of CT images, including a reconstruction in the sagittal plane, delineated a thrombus in the IJV from the jugular foramen to the angle of the mandible with diffuse soft tissue stranding. Reconstructed images in sagittal and/or coronal planes facilitate a 3-dimensional concept of thrombus extent and the relationship to adjacent structures, particularly major blood vessels.
Conclusion
LS is a rare but life-threatening condition with a high mortality rate (5%-18%). Diagnosis is made by radiologic finding of thrombosis of IJV with oropharyngeal infection. This case suggests that advanced imaging with contrast CT and reconstruction in alternate planes may avoid angiography for the diagnosis of LS.
Footnotes
Authors’ Note
All issues related to ethics were taken into consideration throughout the study design and proposal and implemented during the research study itself. Informed consent was obtained, beneficence was made a top priority, and respect for confidentiality and privacy was upheld during the study and its various analysis and information assertation components.
