Abstract
Objective
An aging population requires increased focus on geriatric otolaryngology. Patients aged ≥65 years are not a homogenous population, and important physiologic differences have been documented among the young-old (65-74 years), middle-old (75-84), and old-old (≥85). We aim to analyze differences in dysphagia diagnoses and swallowing-related quality-of-life among these age subgroups.
Study Design
Retrospective chart review.
Setting
Tertiary care laryngology clinic.
Subjects and Methods
We identified chief complaint, diagnosis, and self-reported swallowing handicap (Eating Assessment Tool [EAT-10] score) of all new patients aged ≥65 years presenting to the Johns Hopkins Voice Center between April 2015 and March 2017. Dysphagia diagnoses were classified by physiologic etiology and anatomic source. Diagnostic categories and EAT-10 score were evaluated as functions of patient age and sex.
Results
Of 839 new patients aged ≥65 years, 109 (13.0%) reported a chief complaint of dysphagia and were included in this study. The most common dysphagia etiologies were neurologic and esophageal. Most common diagnoses were diverticula (15.6%), reflux (13.8%), and radiation induced (8.3%). Diverticula, cricopharyngeal hypertonicity, and radiation-induced changes were associated with higher EAT-10 score (
Conclusion
Important differences among dysphagia diagnosis and EAT-10 score exist among patients aged ≥65 years. Knowledge of these differences may inform diagnostic workup, management, and further investigations in geriatric otolaryngology.
Keywords
Dysphagia is a symptom of significant concern and impact, with an estimated prevalence of 3% to 4% in the United States.1,2 A total of $547 million is spent annually on dysphagia-related care in the United States. 3 Patients with dysphagia have markedly reduced swallowing-specific and overall health-related quality of life as a result of dietary alterations and impaired social functioning.4-6
Dysphagia can result from multiple medical disorders, and management is dependent on the localization and physiologic etiology of the underlying disease. Dysphagia can be categorized by anatomic location, including oropharyngeal and esophageal sources, in addition to extrinsic compression of the upper gastrointestinal tract from adjacent masses, musculoskeletal abnormalities, or cardiovascular processes. 7 Similarly, dysphagia can be characterized by etiology, including neuromuscular and structural causes. 7 Given this wide characterization, the presentation of dysphagia is variable, ranging from mild discomfort with swallowing to complete inability to tolerate oral intake.6-8
In particular, dysphagia may be of greater burden on older adults, with an estimated prevalence of 13.8% to 33% in those aged ≥65 years.9-11 Coupled by the heightened risk of severe consequences in the elderly, including aspiration, dehydration, and malnutrition, it is imperative to understand the etiologies, quality-of-life handicap, and diagnostic evaluation across various age categories of older patients. 12
With an aging baby boomer population, the country’s health care infrastructure faces a unique challenge in adapting to the needs of a greater volume of older patients. By 2030, the population of older adults will nearly double current totals, with persons aged ≥65 years soon accounting for 20% of the population. 13 However, it is important to recognize that older adults are not a uniform population. Gerontology literature has highlighted the heterogeneity of older adults, and important physiologic differences have been documented in the young-old (65-74 years), middle old (75-84), and old-old (≥85).14-16 There has been little work in otolaryngology, however, exploring diagnostic differences and quality-of-life handicap across the geriatric age subgroups and particularly little work concerning dysphagia in this population.
In this study, we aimed to evaluate and describe the clinical features of patients presenting to a tertiary laryngology clinic with a chief complaint of dysphagia. In doing so, we hope to inform more nuanced, patient-based approaches to this increasingly important topic.
Methods
Study Population
A retrospective chart review was conducted for all patients who presented to the Johns Hopkins Department of Otolaryngology–Head and Neck Surgery Voice Center over a 2-year period between April 1, 2015, and March 30, 2017. New patients with a chief complaint of dysphagia and age ≥65 years qualified for inclusion. This study received approval from the Johns Hopkins Institutional Review Board.
Variables and Outcomes
Demographic information, underlying diagnosis, imaging and diagnostic study findings, and Eating Assessment Tool (EAT-10) scores were abstracted from all eligible charts. Exact patient age at the date of visit was calculated from the date of birth and date of visit and used for assignment to the appropriate age subgroup. Age categorization was in accordance with an existing schema from the emerging literature highlighting the physiologic differences that occur with aging: young-old encompassed those aged 65 to 74 years, middle-old comprised those aged 75 to 84 years, and old-old included individuals aged ≥85 years.14-16
Underlying diagnosis was retrieved from chart review, and dysphagia assessment was performed as clinically indicated, including some combination of history, physical examination, speech-language pathology assessment, flexible laryngoscopy, and follow-up diagnostic tests, such as videofluoroscopic swallow study (modified barium swallow), esophagram (barium swallow), esophagogastroduodenoscopy (EGD), esophageal manometry, and 24-hour esophageal pH monitoring. For assignment of isolated cervical spine abnormalities as the primary diagnosis, patients must have demonstrated significant arthritic or postsurgical spine changes on imaging in the absence of any other identifiable cause of dysphagia. Understanding that fluoroscopic studies may not always demonstrate reflux, reflux was assigned as the primary diagnosis if the patient had compatible symptoms with either abnormal pH monitoring or symptom resolution with antacid therapy in the absence of any other identifiable cause of dysphagia. 17
Based on a previously described classification schema, dysphagia diagnosis was classified by anatomic location and physiologic etiology. 7 Classification by anatomic location was defined as disorders of the oropharynx or esophagus or as extrinsic (ie, processes of nongastrointestinal origin) or unknown. Extrinsic pathologies include, but are not limited to, diseases of the spine, thyroid, and cardiovascular structures that may affect swallowing. Classification by etiology was defined as motor, obstructive, or unknown. Motor sources are those of neuromuscular origin and encompass esophageal spasm and dysmotility, cricopharyngeal hypertonicity, radiation-induced fibrosis, reflux, and primary neurologic diseases such as stroke, Parkinson’s disease, or amyotrophic lateral sclerosis. Obstructive sources are structural lesions and include esophageal diverticulum, stricture, neoplasm, and cervical spine disease.
EAT-10 is a self-administered instrument for documenting dysphagia severity and is routinely completed by patients at the time of the initial clinic visit. EAT-10 is an internally consistent, validated 10-question survey scored from 0 to 40, wherein a score ≥3 is considered abnormal. 18
Statistical Analysis
Primary univariate measures were initially used to describe the overall population, including mean age, sex distribution, etiologies of dysphagia, and mean EAT-10 scores. The population was subdivided by sex and age to assess differences in the proportion of dysphagia etiology. Secondarily, bivariate analysis explored differences in dysphagia etiology or EAT-10 scores between sex and age categories with Pearson’s chi-square or analysis of variance tests. All statistical analyses were conducted with R (R Foundation for Statistical Computing, RStudio version 1.2.5033).
Results
Of 839 new patients aged ≥65 years presenting to the laryngology clinic during the study period, 109 (13.0%) had a chief complaint of dysphagia and are included in this analysis. The remaining 730 had chief complaints of dysphonia (n = 464), cough (n = 89), airway narrowing (n = 50), or other (n = 127) and are not included in further analysis. Of the 109 patients, 61 (56.0%) were male and 48 (44.0%) were female. The study population had a mean (SD) age of 75.4 (7.2) years: 61 (56.0%) were categorized as young-old, 33 (30.3%) as middle-old, and 15 (13.8%) as old-old. Patient characteristics are presented in Table 1 .
Etiology and Anatomic Source of Dysphagia by Age and Sex. a
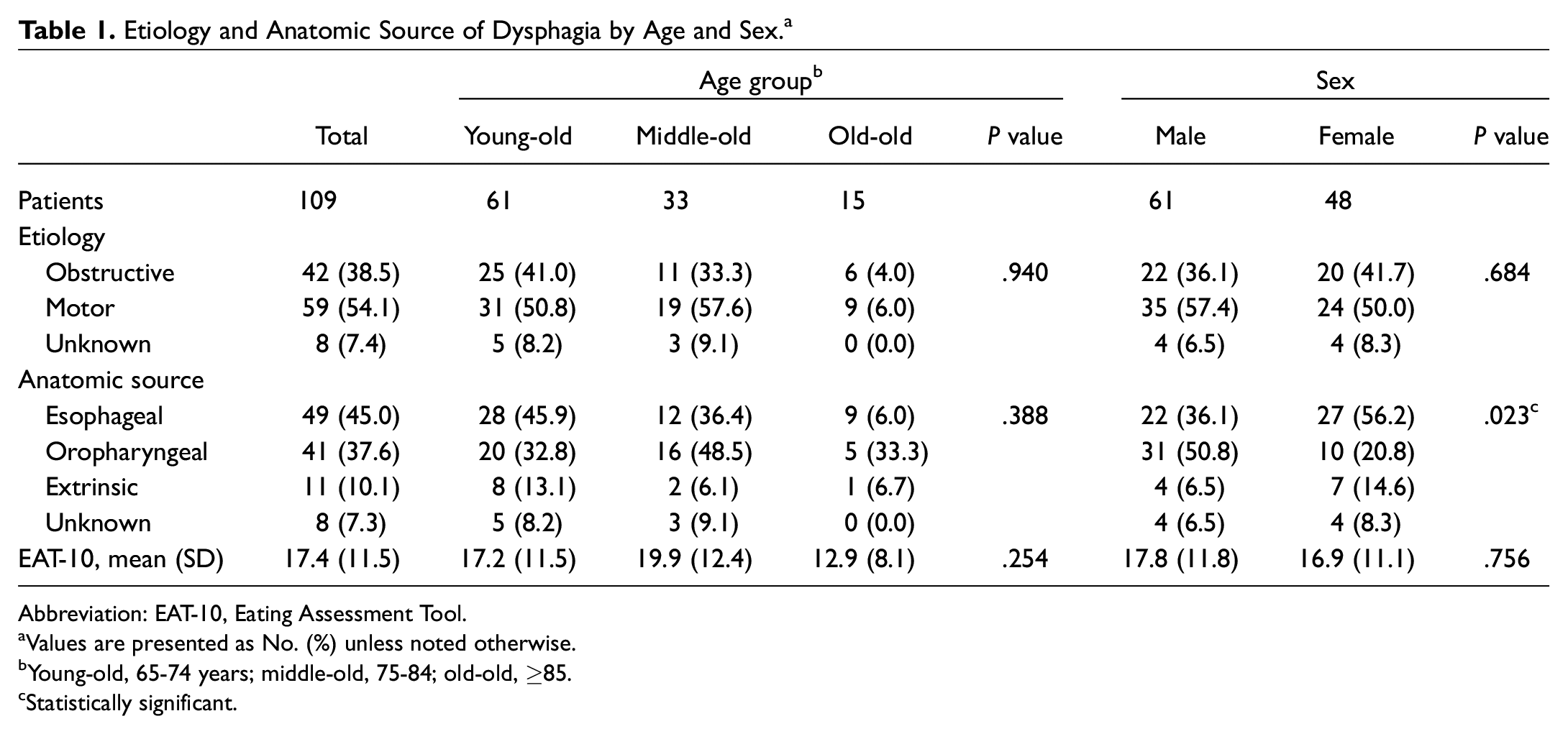
Abbreviation: EAT-10, Eating Assessment Tool.
Values are presented as No. (%) unless noted otherwise.
Young-old, 65-74 years; middle-old, 75-84; old-old, ≥85.
Statistically significant.
Seventy patients (64.2%) underwent a modified barium or barium swallow as part of the diagnostic workup. Fourteen (12.8%) had an EGD, 6 (5.5%) had manometry, and 3 (2.8%) had esophageal pH sensing. All patients received in-office fiberoptic laryngoscopy. There was no statistically significant difference noted in patients who received videofluoroscopic swallow study, EGD, manometry, or pH sensing by age subgroup (
In the overall cohort, the most common etiology of dysphagia was motor causes (54.1%). Obstructive causes accounted for 38.5% of cases. The most common anatomic source of dysphagia was esophageal (45.0%), followed by oropharyngeal (37.6%) and extrinsic (10.1%) causes. There was no statistically significant difference noted between age subgroup and dysphagia etiology (
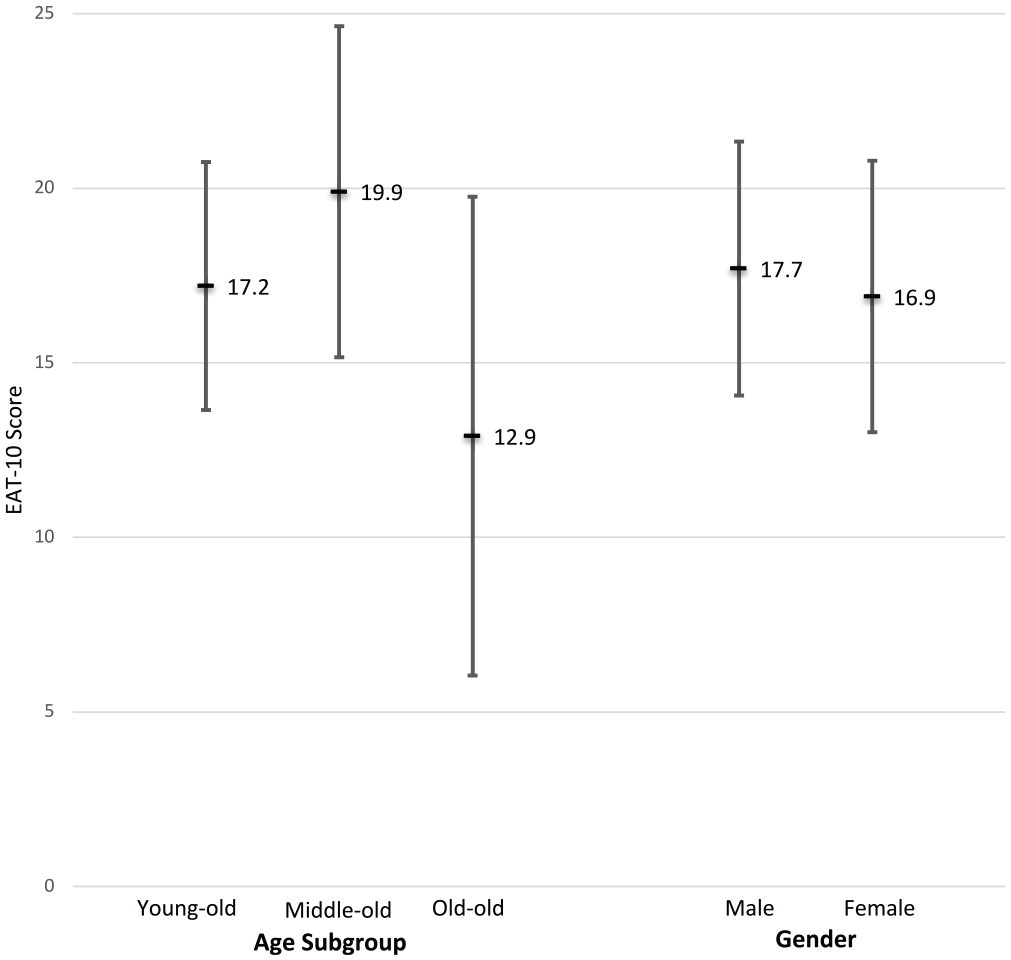
Mean Eating Assessment Tool (EAT-10) score by age and sex. Error bars represent 95% CIs.
The most common causes of oropharyngeal and esophageal dysphagia were of neurologic origin, representing 82.9% and 51.0% of diagnoses, respectively. The most common dysphagia diagnosis in the overall cohort was diverticular disease (15.6%); all but 1 of these were Zenker’s diverticula. This was followed by gastroesophageal and laryngopharyngeal reflux disease (13.8%) and radiation-induced changes (7.3%). The most common diagnoses in this cohort, with their mean EAT-10 scores, are presented in
Table 2
. There was a statistically significant difference (
EAT-10 Score by Most Common Diagnoses. a
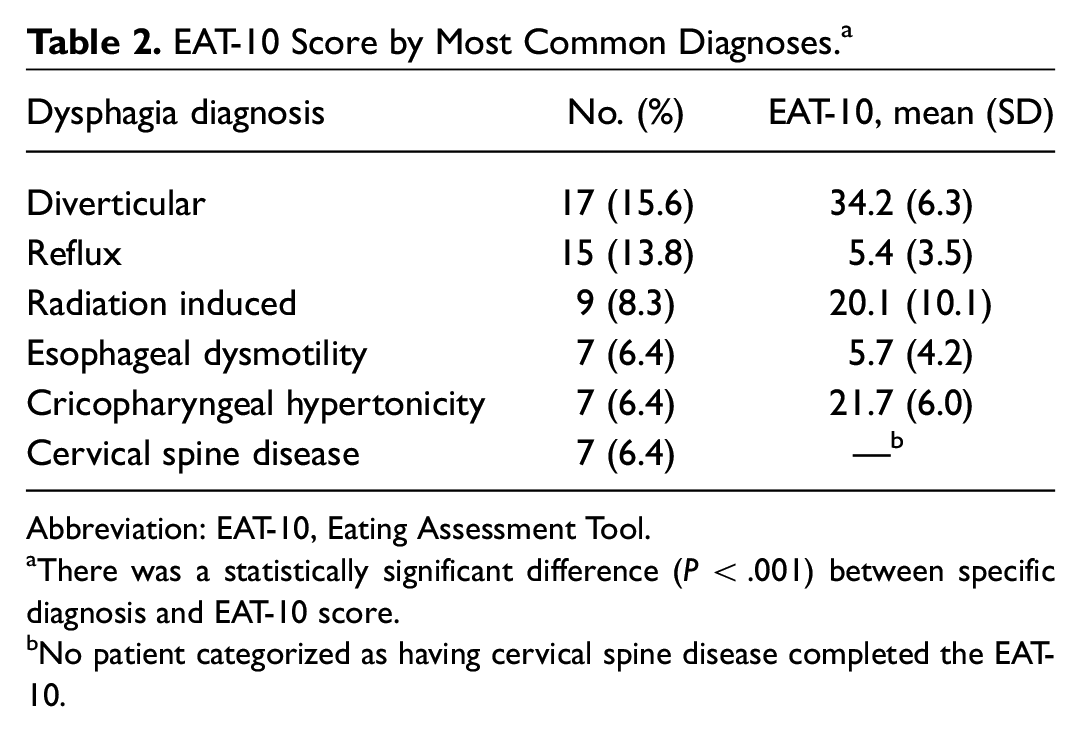
Abbreviation: EAT-10, Eating Assessment Tool.
There was a statistically significant difference (
No patient categorized as having cervical spine disease completed the EAT-10.
Discussion
As the elderly represent the fastest-growing segment of our nation’s population, understanding the causes of dysphagia across the age spectrum is important for older adults. 19 This is of particular importance given the increased mortality, morbidity, and adverse social and meal-related functioning in older adults with dysphagia.12,20,21 In this retrospective review of older adults presenting with dysphagia, we found the most common etiologies were neuromuscular and esophageal in origin. The most common diagnoses were diverticula, reflux-related disease, and radiation-induced fibrosis. Men were more likely to present with oropharyngeal disease and women with esophageal disease. The greatest quality-of-life impact occurred with diverticular disease, cricopharyngeal hypertonicity, and radiation-induced changes.
In our population, 15.6% had dysphagia attributed to diverticular disease; 13.8% to reflux-related disease; 8.3% to postirradiation fibrosis; and 7.3% to cervical spine disease, cricopharyngeal hypertonicity, and esophageal dysmotility disorders. Our patients had a mean EAT-10 score of 17.4. In a similar study of patients presenting to a tertiary swallowing center, 27% had dysphagia due to gastroesophageal reflux disease, and 14% to radiation changes, and 11% to cricopharyngeal dysfunction. 22 A similar quality-of-life handicap was demonstrated, with a mean EAT-10 score of 17.7. This reaffirms the most common etiologies of dysphagia among the elderly and the significant social and physiologic handicap on patients.
Our study also demonstrates a significant difference in EAT-10 score by specific dysphagia diagnosis, with diverticulum, postirradiation changes, and cricopharyngeal hypertonicity bearing the greatest impact of swallowing dysfunction. As a widely used, rapidly administered instrument, EAT-10 provides benefit in assessing initial disease severity and treatment response for a variety of dysphagia disorders.18,23 We found the highest quality-of-life burden to be among patients with diverticula, with a mean (SD) EAT-10 of 34.2 (6.3). Prior studies have demonstrated EAT-10 scores of 17.9 to 22.1 with diverticular disease, which significantly decrease with surgical repair.24-28 The larger impact of diverticula in this study may be biased, as our institution is a large referral center for endoscopic repair.29,30 Cricopharyngeal hypertonicity and radiation-induced changes also caused swallowing severity, with mean (SD) EAT-10 scores of 21.7 (6.0) and 20.1 (10.1), respectively. Prior studies have also demonstrated similar swallowing dysfunction with cricopharyngeal dysfunction, which reduce following myotomy or botulinum toxin injection.31-33 Although intensity-modulated radiotherapy has reduced radiation damage to oropharyngeal structures essential for swallowing, elevated EAT-10 scores remain among these patients, and the long-term prevalence of dysphagia is still 10% to 16%.34-39 We also noted a statistically significant difference in the anatomic site of dysphagia between men and women. In particular, men were more likely to present with oropharyngeal disease, and women were more likely to have esophageal disease. The oropharyngeal predominance in men likely represents known sex differences in smoking rates and head and neck cancer prevalence.40-42 The esophageal predominance in women is likely due to the high prevalence of reflux disease in our study (13.8%), which may be influenced by increased gastric secretions, delayed gastric emptying, and increased adiposity accompanying menopause.41,43,44 Our study did not identify a difference in etiology of dysphagia or EAT-10 scores among the 3 subgroups analyzed (young-old, 65-74 years; middle old, 75-84; and old-old, ≥85), consistent with a prior study analyzing self-perceived dysphagia in these age groups. 45
Swallowing is a complex process that relies on the successful formation and propulsion of a food bolus; the coordination of the epiglottis, vocal cords, and laryngopharyngeal muscles; and controlled esophageal movement. 46 Several physiologic changes to swallowing occur in the elderly, including weakened jaw strength and salivary production, pharyngeal and laryngeal muscle atrophy, and loss of esophageal sphincter compliance. 46 There is evidence, however, to suggest that these physiologic changes seen on fluoroscopy do not alone account for perceived dysphagia or increased risk of aspiration.47-50 Rather, perceived and diagnosed swallowing dysfunction may be the result of underlying disease. A complaint of dysphagia in older adults should therefore be regarded as pathologic, especially given the wide spectrum of neuromuscular and structural disorders that increase in prevalence with age.20,45,46,51
This study is not without limitations. This study consists of chart review, and data were limited to what was documented in the electronical medical record. Similarly, dysphagia etiology was determined by clinical judgment, as supported by imaging studies and diagnostic studies, which may introduce selection bias. Our cohort also represents a treatment-seeking population; therefore, results may not be generalizable to all older adults with dysphagia. Likewise, dysphagia cases that present to an otolaryngology clinic may not represent all treatment-seeking patients with dysphagia, particularly those whose workup may be initiated by neurologists, gastroenterologists, or other specialists. Last, while our clinic is a busy referral center for laryngological conditions, our patients with a chief complaint of dysphagia still comprised only 13.0% of all new patients over a 2-year period, and only 15 patients were in the old-old subgroup. A larger data set, by either a longer study period or multi-institution data collection, may have yielded more robust analysis.
This article is a descriptive analysis of dysphagia among the elderly, also subdivided by young-old, middle-old, and old-old age categories. This study adds to the growing literature highlighting the causes and quality-of-life impact of dysphagia in older adults, which may have future implication for how these individuals are evaluated and treated.
Conclusion
As the proportion of elderly people in the United States rises, so will the number of patients with swallowing complaints. The most common causes of dysphagia among an elderly population presenting to a tertiary care swallowing center were neurologic and esophageal in nature, with the top causes comprising diverticula, reflux, and postirradiative changes. These etiologies also result in significant quality-of-life burden, thereby pointing to the need for further research in the evaluation and treatment of dysphagia in older age.
