Abstract
Objective
To assess the prevalence of laryngeal muscle tension patterns among patients with functional dysphagia.
Study Design
Retrospective study.
Setting
The study took place at a university medical center.
Material and Methods
The medical charts and laryngeal video recordings were reviewed for all patients who presented with dysphagia and who were referred for barium swallow between 2012 and 2017. A total of 170 cases were identified. Only those with normal findings on barium swallow and the absence of vocal fold pathology (exudative lesions, masses or tumors, paresis, and paralysis), referred to as functional dysphagia, were included in this study. Information retrieved included swallowing and phonatory symptoms in addition to patterns of laryngeal muscle tension.
Results
The mean ± SD age of the total group was 41.90 ± 15.10 years with a male:female ratio of 4:1. Seventy-five percent had evidence of at least 1 type of laryngeal muscle tension pattern. The most common pattern was type III, characterized by supraglottic anteroposterior compression (13 of 20), followed by type II, characterized by medial compression of the false vocal folds (5 of 20); only 1 patient had muscle tension pattern type IV, characterized as sphincter-like closure of supraglottic structures. The most common laryngopharyngeal symptom was throat discomfort when swallowing (35%), followed by throat clearing and choking/coughing when eating and drinking (25%).
Conclusion
The high prevalence of laryngeal muscle tension pattern among patients with functional dysphagia supports the notion that laryngeal tension may be one of the underlying causes of dysphagia.
Keywords
Dysphagia is a common symptom often reported by patients in the otolaryngology practice. It may present in isolation as a solitary complaint or in constellation with other symptoms related to gastroesophageal diseases or disorders of the laryngopharyngeal complex. It is defined as the subjective sensation of difficulty in swallowing solids or liquids and can be divided into 2 general categories: oropharyngeal dysphagia and esophageal dysphagia. Oropharyngeal dysphagia is described as the feeling of inability to initiate the swallowing process, whereas esophageal dysphagia is the sensation of difficulty in swallowing a short time after the swallowing is initiated and as the food bolus moves down the esophagus. 1 The etiology is multifactorial and includes intrinsic factors (eg, esophagitis, carcinoma, and strictures), extrinsic factors (eg, tumors and masses), or motility disorders secondary to neurogenic or neuromuscular diseases. 2
The etiology of dysphagia can hardly be diagnosed per the patient’s medical history alone. When persistent, the workup entails diagnostic tests, such as fiberoptic nasopharyngeal endoscopy, barium swallow, pharyngeal and esophageal manometry, and videofluoroscopy. Given that dysphagia may be the presenting symptom of alarming diseases, many professionals consider esophagogastroduodenoscopy or endoscopy to be the first line of investigation. Newer diagnostic technologies include high-resolution manometry, which makes use of closely spaced sensors to get a higher-resolution image of the movement of the esophageal muscles. 3 The decision on which diagnostic test to use is usually driven by the patient’s history, the range of differential diagnosis, and the physician’s preference.
Despite the advances in the diagnostic workup of dysphagia, many patients are left with no clear etiology. These patients are often referred to as having idiopathic functional dysphagia, described as symptomatic dysphagia with no evident anatomic or physiologic cause. 4 According to Rome IV criteria, functional dysphagia must include “a sense of solid and/or liquid foods sticking, lodging, or passing abnormally through the esophagus” with “no evidence of esophageal mucosal or structural abnormality” or “major esophageal motor disorder” or “evidence of gastroesophageal reflux disease or eosinophilic esophagitis.” 5
The pathogenic role of laryngeal disorders and, in particular, laryngeal muscle tension in patients with swallowing disorders has not been thoroughly investigated in the literature. The first study on the association between dysphagia and laryngeal muscle tension was reported by Kang et al, with a group of 67 patients with normal videofluoroscopic swallowing study results who were labeled by the authors as having functional dysphagia. The high prevalence of laryngeal muscle tension in this group of patients led to a new term: muscle tension dysphagia (MTD). 6 The purpose of this investigation is to cast further information on this entity by assessing the prevalence of laryngeal muscle tension patterns (MTPs) among patients with normal barium swallow. These patients are referenced in this study as having functional dysphagia. We hypothesize that laryngeal muscle tension may have a pathogenic role among patients with functional dysphagia.
Materials and Methods
After approval from the Institutional Review Board at the American University of Beirut Medical Center, the medical charts and laryngeal video recordings were reviewed of all patients who presented with dysphagia to the Voice Unit and had undergone barium swallow between 2012 and 2017. Dysphagia was reported by patients as difficulty in swallowing. A total of 170 cases were identified. Only those with absence of vocal fold pathology (exudative lesions, masses or tumors, paresis, and paralysis) and normal findings on barium swallow, referred to as functional dysphagia, were included. Barium swallow is a test suggested for the workup of difficulty in swallowing, where the patient is asked to swallow a liquid suspension of barium sulphate before a series of radiographic images are taken of the upper digestive tract—namely, the pharynx, esophagus, and stomach. The images produced are serial digital x-ray images, anteroposterior and lateral, and are viewed by a radiologist on a screen while observing the outflow of fluid through the pharynx to the stomach.7,8
Hence, inclusion criteria included patients with a primary symptom of dysphagia, with normal barium swallow study results, and with no laryngeal pathology on videostroboscopic evaluation. Patients with vocal fold pathology were excluded given the well-known laryngeal compensatory behavior among them. A total of 20 patients were included.
Material retrieved from the medical charts included demographic data (age, sex, smoking, and alcohol consumption) and laryngopharyngeal symptoms in addition to dysphagia, such as throat discomfort when swallowing, throat clearing, coughing/choking, and dysphonia. The material retrieved from the laryngeal videostroboscopic examination included the patterns of laryngeal muscle tension described by Koufman and Blalock. 9 The MTPs were classified as follows: MTP I, denoting the persistence of a posterior glottic gap during phonation; MTP II, denoting medial compression of the false vocal folds during phonation; MTP III, denoting anteroposterior shortening of the distance between the petiole and interarytenoid area; and MTP IV, denoting complete sphincter-like closure of the supraglottic structures.9,10 MTPs were analyzed by a well-trained and experienced otolaryngologist using frame-by-frame analysis (60 frames per second) of a 2- to 3-second window during sustained vowel /e/ at a comfortable pitch and loudness. The percentage muscle tension score was computed as follows 9 : number of frames showing MTP × 100 / total number of scored frames.
Statistical Method
Descriptive statistics at baseline were conducted to describe the demographic characteristics of the recruited group of subjects. Means with standard deviations or medians with interquartile ranges were reported for continuous variables, as appropriate. Frequencies and percentage were reported for categorical variables. The data collected were entered into a database with SPSS 22 (IBM, Chicago, Illinois).
Results
Demographic Data
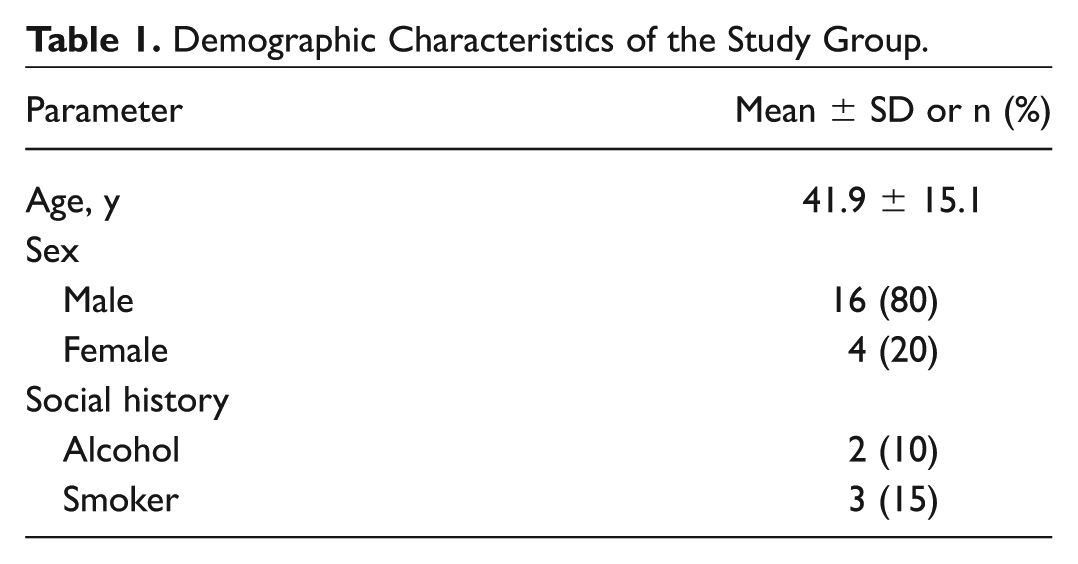
The mean age of the total group was 41.90 ± 15.10 years with a male:female ratio of 4:1. Fifteen percent were smokers ( Table 1 ).
Demographic Characteristics of the Study Group.
Laryngopharyngeal Symptoms
All 20 subjects included in this study had dysphagia. Other reported symptoms included throat discomfort when swallowing (35%) and throat clearing and choking/coughing when eating and drinking (25%). Only 5 patients had history of dysphonia, 4 of whom had evidence of at least 1 MTP and 1 had irritation (mucosal redness and edema; Table 2 ).
Prevalence of Laryngopharyngeal Symptoms in the Study Group.

Patterns of Laryngeal Muscle Tension
Seventy-five percent of patients had evidence of at least 1 type of laryngeal MTP. The most common pattern was type III (13 of 20), followed by type II (5 of 20), and only 1 patient had MTP IV (note that some patients had at least 1 type of MTP; Figure 1 ). The mean score of each MTP is displayed in Figure 2 . Of the 20 patients with dysphagia, 5 had evidence of nonspecific laryngeal irritation (edema and redness). Of 20 patients with functional dysphagia, 75% had evidence of at least 1 type of MTP, and 20% exhibited 2 types of MTPs.
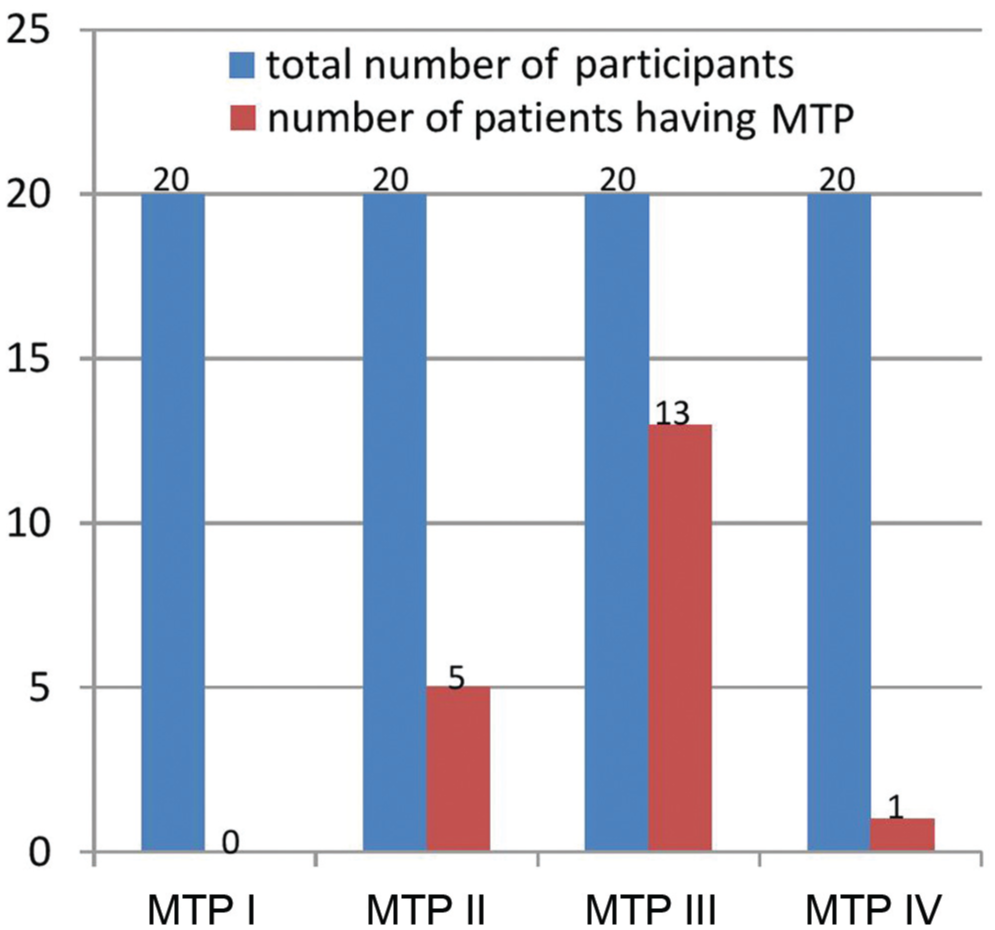
Prevalence of the different muscle tension patterns (MTPs) in the study group.
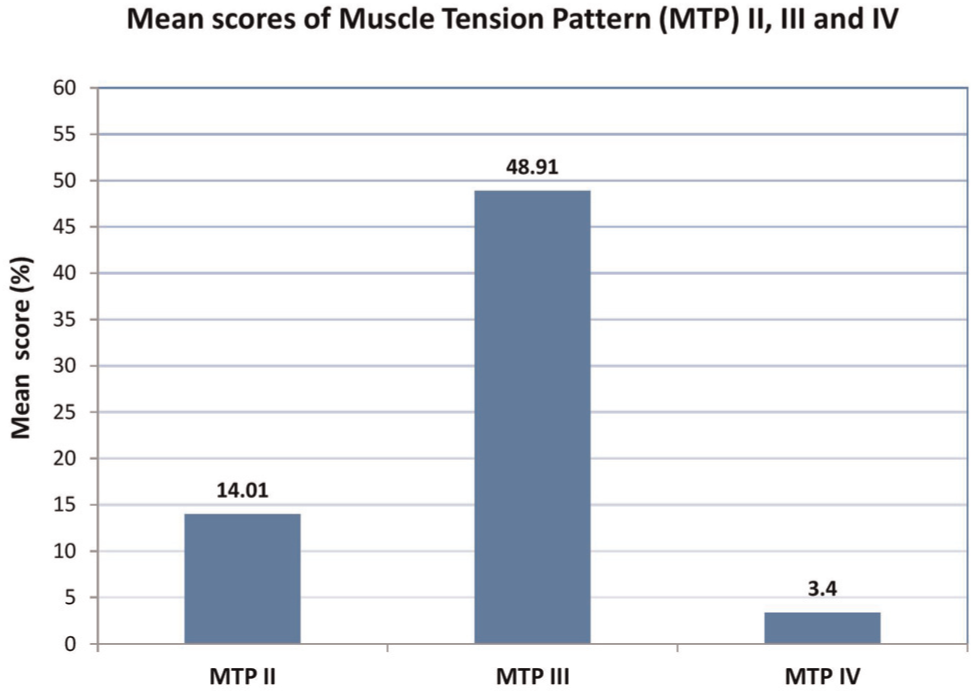
Mean scores of muscle tension patterns (MTPs) II, III, and IV (MTP I, n = 0).
Discussion
Given the proximity in the anatomic structures of the upper respiratory and digestive systems and the presence of inherent protective mechanisms for aspiration, such as the pharyngeal reflex swallow and the vocal fold closure reflex, it is not surprising to observe aberrant supraglottic laryngeal activity in patients presenting primarily with dysphagia. The results of this investigation support the hypothesis set forth in the introduction—namely, the correlation between laryngeal MTPs and dysphagia as a symptom. More so, 1 of 4 patients with dysphagia had dysphonia, 80% of whom had evidence of MTP. It is also worth noting that 25% of the subjects investigated had evidence of edema or redness on laryngeal examination. Our results are in accordance with the results of Kang et al, where 97% of 67 patients with functional dysphagia had MTP on laryngeal examination. More so, 55% had dysphonia, which accounted for 58% of those with signs of laryngeal inflammation. According to the authors’ classification, patients with dysphagia who exhibited characteristic patterns of MTD with no signs of nonspecific laryngeal inflammation were labeled as having primary MTD, and those without signs of laryngeal inflammation were labeled as having secondary MTD. 6
This crosscutting in the prevalence of laryngeal MTP and dysphagia is not shocking, given the intimate and intertwined sensorimotor innervation of the laryngopharyngeal complex. Numerous investigators examined the interplay between phonation and the kinematics of swallowing. In their investigation on changes in the upper and lower esophageal sphincters during phonation, Perera et al indicated a significant increase in the upper esophageal sphincter pressure in a group of 17 healthy subjects who were asked to perform high and low pitch vowels at different intensities. 11 These results were not in keeping with the findings of Van Houtte et al, who failed to detect any differences in the upper esophageal sphincter pressure during phonation between patients with and without MTD. 12 However, patients with dysphagia may also exhibit abnormal laryngeal MTPs as reported by Kang et al. Possible pathophysiologic factors include restricted movement of the larynx and hyoid bone, excessive tension in pharyngeal muscle constriction, or dysfunction in the upper esophageal sphincter. 6 The last of which is intimately linked to the laryngeal framework through the cricopharyngeal and thyropharyngeal muscles, the dysfunction of which may perpetuate abnormal pharyngeal and laryngeal MTP. These suggested pathogenic factors remain hypothetical given the lack of any laryngeal electromyographic or pharyngeal manometric studies.
Another possible mechanism for the high prevalence of muscle tension among patients with functional dysphagia is the strong association between reflux and MTD. Van Houtte et al reported that 70% of patients with MTD have evidence of reflux as documented by double-probe pH-metry. 12 Although not all subjects investigated in the present study had MTD (only 4 given that 25% had dysphonia, 80% of whom had MTP), MTD patterns may be observed among patients with no vocal complaints, as reported by Van Houtte et al. 13 Based on their recent review of the current literature on the pathophysiology of MTD, the authors described MTD as a spectrum where subjects on one end exhibit dysphonia due to decompensation of the intrinsic laryngeal muscles and those on the other end may have a normal voice due to a compensatory behavior. With that premise at hand, the aforementioned pathogenic role of reflux disease may be extrapolated to subjects with MTD patterns and normal voice (ie, to 70% of the studied population in this investigation). The results of this investigation cannot corroborate or refute this hypothesis, given the lack of diagnostic data on the true prevalence of laryngopharyngeal reflux disease among these patients. Nevertheless, the 25% prevalence of nonspecific laryngeal irritation in the form of redness in the laryngeal structures may allude to the pathogenic role of laryngopharyngeal reflux. A prospective investigation is warranted to examine the prevalence of laryngopharyngeal reflux disease among patients with functional dysphagia and laryngeal muscle tension.
The results of this investigation have important clinical implications. The high presence of laryngeal tension among patients with dysphagia and normal barium swallow results may indicate speech pathology therapy as a treatment modality. Vocal hygiene practice, such as adequate hydration and adoption of healthy phonatory habits (eg, avoidance of excessive usage of voice, especially in noisy environment), may prove to be beneficial for patients with dysphagia. Direct mode of therapy, such as circumlaryngeal manual therapy, traditionally applied to patients with MTD may also be applicable to those with functional dysphagia who exhibit characteristic features of MTD. The aim of such therapy is to reduce the tension within the extrinsic laryngeal and paralaryngeal muscles and subsequently within the pharyngeal muscles as well.14-16 Indeed, numerous studies demonstrated a substantial difference in tension in the laryngeal and paralaryngeal musculature among patients with MTD as compared with controls.17,18 These investigations were based on surface electromyographic analysis of supra- and infrahyoid muscles. As suggested by Kang et al, patients with dysphagia who exhibit characteristic features of MTD similar those of to the subjects analyzed in this study may also benefit from this therapeutic option. 6 This suggestion remains a hypothesis that warrants further investigation into the prevalence of muscle tension before and after therapy.
This study is the second to that of Kang et al in delineating the potential etiologic role of laryngeal muscle tension among patients with functional dysphagia. 6 Unlike the study by Kang et al—where the majority had secondary MTD in view of the high prevalence of laryngeal hyperresponsiveness (67%) and nonspecific laryngeal inflammation (52%)—the results of our investigation indicate that 75% had primary MTD, given that only 5 patients had evidence of laryngeal irritation as a possible contributing factor to the laryngeal muscle tension behavior observed on laryngeal endoscopy. This leads us to assume that primary MTD is more common than secondary MTD; hence, the lack of any organic cause (eg, nonspecific inflammatory changes) or functional etiology (eg, paradoxical vocal fold movement or intractable cough) should not make us suspect less the diagnosis of primary dysphagia. More so, this study provides information to the literature on the type of laryngeal MTP exhibited by these patients. The study by Kang et al does not describe the prevalence of each type of laryngeal MTP among affected patients. Our investigation revealed that patients invariably have 1 type of laryngeal muscle tension and that the sphincter-like closure is rarely observed. The diversity in the prevalence and severity of these laryngeal MTPs alludes to the polymorphic nature of the laryngeal behavior among patients with functional dysphagia. Further clinical implications on these findings, in relation to the pathogenesis and treatment of primary dysphagia, warrant further investigation.
This study has 2 main limitations: the first is the relatively small number of subjects investigated, and the second is the lack of information on the prevalence of laryngopharyngeal reflux disease among these patients, given the retrospective nature of this study. A future investigation is warranted into the characteristic patterns of MTD among patients with functional dysphagia based on Rome IV criteria.
Conclusion
This investigation highlights the strong interplay between patients with dysphagia and normal barium swallow results, referred to as functional dysphagia, and abnormal laryngeal muscle tension behavior. The high prevalence of MTP in this group supports the notion that laryngeal muscle tension may be one of the underlying causes of dysphagia among patients with no obvious structural or motility disorder. Further studies exploring the laryngeal behavior of patients with dysphagia who have been thoroughly investigated with >1 diagnostic method will cast more information on the interplay between phonation and swallowing.
Author Contributions
Disclosures
Footnotes
No sponsorships or competing interests have been disclosed for this article.
