Abstract
Difficulties are associated with reconstruction of middle ear bony structures in surgery for destructive lesions, including cholesteatoma. Although autologous cartilage appears to be the optimal choice because of its resistance to infection, the harvesting of sufficient volumes may be challenging. Therefore, regenerative medicine techniques to obtain sufficient material for reconstruction are awaited. We herein present a case of middle ear surgery for cholesteatoma with a sufficient volume of stick-shaped tissue-engineered cartilage produced from a piece of autologous auricular cartilage and autologous serum, with sufficient firmness to reconstruct bony structures. During surgery, sections of tissue-engineered cartilage were placed side by side to reconstruct the posterior canal wall. The postoperative course was uneventful. This is the first-in-human report of reconstructing middle ear bony structures with tissue-engineered cartilage. The results suggest a promising future for the satisfactory reconstruction of middle ear structures with minimal morbidity at the donor site.
Keywords
Difficulties are associated with reconstruction of middle ear bony structures in surgery for destructive lesions, including cholesteatoma. Surgical procedures for cholesteatoma have been reviewed in detail in the literature. 1 They have been principally classified into open mastoidectomy (the “canal wall down” method), closed mastoidectomy (the “canal wall up” method), and open mastoidectomy with reconstruction of the posterior canal wall. Open mastoidectomy permits better eradication of the lesion but may result in so-called cavity problems, such as intractable infection of the augmented external ear canal. Closed mastoidectomy preserves the physiology of the external canal but is associated with an increased risk of recurrence because of residual lesions. The complete removal of lesions with open mastoidectomy, followed by posterior canal wall reconstruction, to restore a normal-sized ear canal is regarded as a good option. However, the materials used for reconstruction may have adverse effects: the risk of postoperative infection is increased with artificial materials, and bone dust may be absorbed. Although autologous cartilage appears to be the optimal choice because of its resistance to infection, 2 the harvesting of sufficient volumes may be challenging. Therefore, regenerative medicine techniques to obtain sufficient material for reconstruction are awaited in this field.
We herein present a case of middle ear surgery for cholesteatoma with a sufficient volume of tissue-engineered cartilage. Tissue-engineered cartilage was originally invented to reconstruct the nasal bridge in patients with cleft lip-nose, 3 and manufacturing authorization has since been applied for (Fujisoft Incorporated, Tokyo, Japan). This is part of an off-label use study for this product. Since the stable formation of cartilage tissue with a perichondrium was observed within 3 to 6 months in animal studies, the principal result was assessed 6 months after surgery.
Technology and Case Presentation
The patient was a 31-year-old man with left-sided pars flaccida–type cholesteatoma. Apart from middle ear surgery for right-sided cholesteatoma 2 years before, his previous medical history was unremarkable.
The procedure was approved by the Institutional Review Board of the university (15-245) and by the Japanese Ministry of Heath, Labor and Welfare (PB3170008). Written informed consent was obtained from the patient. Detailed procedures to produce tissue-engineered cartilage have been described in the literature. 3 Figure 1 summarizes the principal processes. Autologous serum for cell cultures was prepared from approximately 600 mL of venous blood. A small full-thickness cartilage plate (a square of approximately 10 mm) was harvested from the concha of the auricle and sent to a licensed facility that manufactures specific processed cells (Fujisoft Tissue Engineering Co, Ltd, FSTEC CPC; Tokyo, Japan) to produce tissue-engineered cartilage. Chondrocytes were isolated and expanded by cultures and subcultures. Cultured cells were recovered and placed in the porous body of a poly-L-lactic acid scaffold with atelocollagen hydrogel and then kept in a shaking culture. The final product was stick-shaped tissue-engineered cartilage (length, 50 mm; width, 6 mm; thickness, 3 mm) with a half moon–shaped cross section ( Figure 2a ) and of sufficient firmness (compressive strength, ≥0.1 MPa) to reconstruct bony structures.
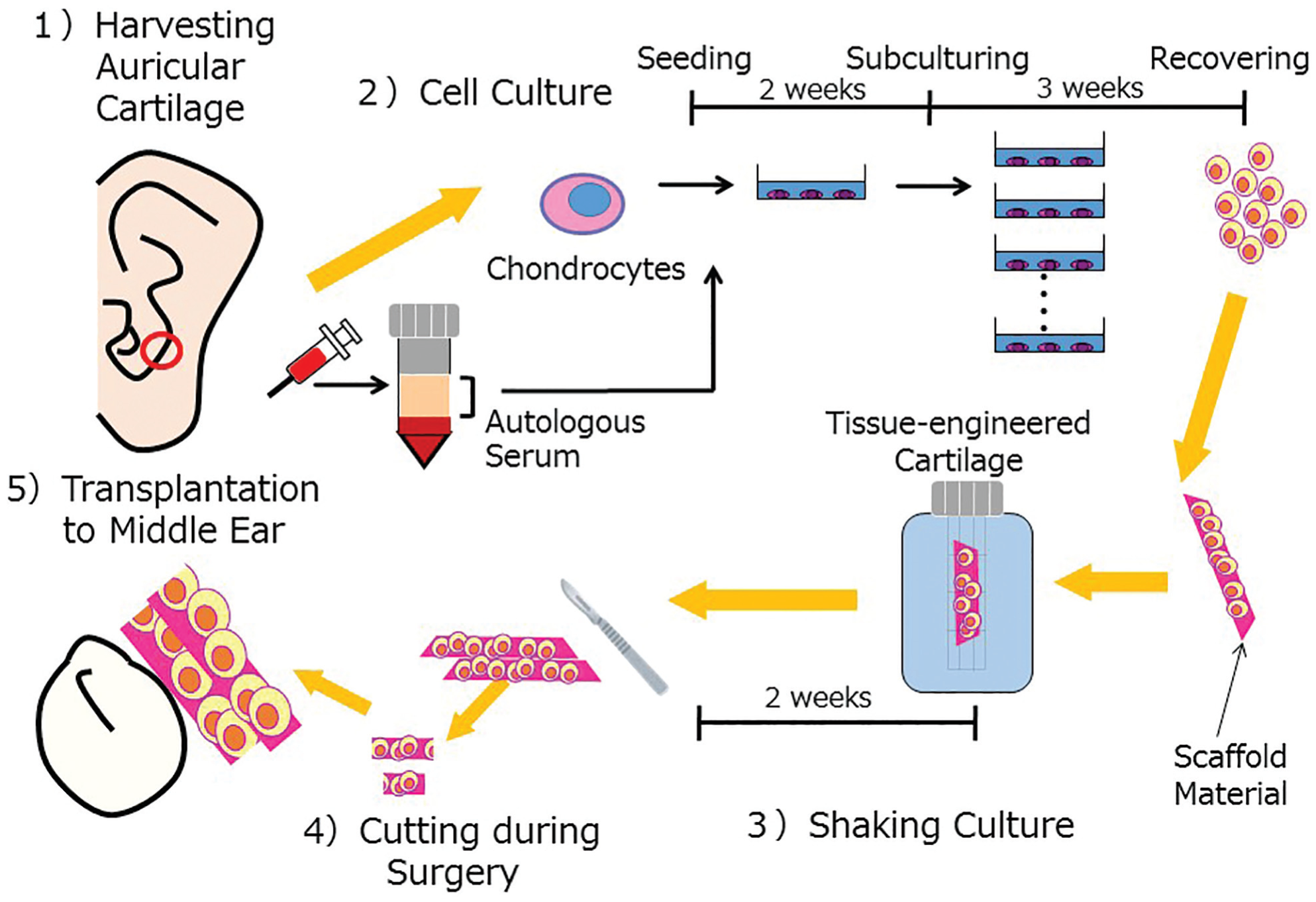
Schemata showing procedures to manufacture and transplant tissue-engineered cartilage.
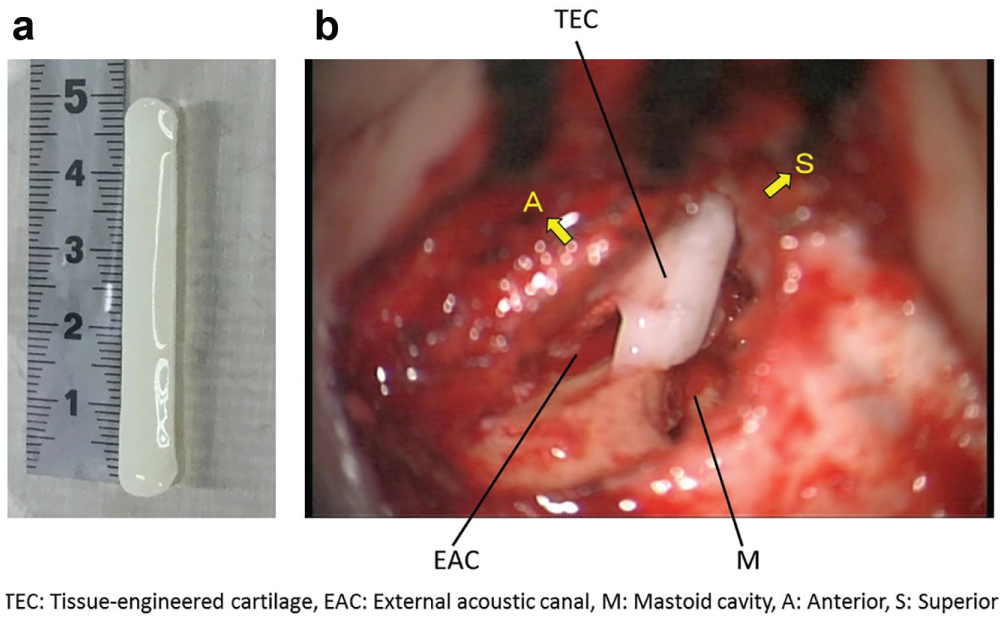
(a) Stick-shaped tissue-engineered cartilage. (b) Intraoperative image with sections of tissue-engineered cartilage placed to reconstruct the posterior canal wall, corresponding to the schema shown in Figure 3b .
Surgery (open mastoidectomy with posterior canal wall reconstruction and tympanoplasty) was performed with a postauricular incision. Open mastoidectomy was performed by drilling. The skin of the external acoustic canal (EAC) was preserved with the tympanic membrane (no incision in EAC). After removal of the cholesteatoma matrices, the ossicular chain was reconstructed by placing the reformed incus body between the head of the stapes and tympanic membrane. The size of the posterior canal wall defect was then measured with a piece of cardboard, and tissue-engineered cartilage was carved accordingly. Three sections of cartilage were placed side by side to form the reconstructed posterior canal wall ( Figure 2b ). These sections of tissue-engineered cartilage were completely wrapped by free fascia grafts to avoid exposure and contact with other materials. A defect in the tympanic membrane was also repaired with temporalis fascia grafts. EAC was finally packed with small pieces of sterilized gauze soaked in saline. Schemata for the procedure are shown in Figure 3 .
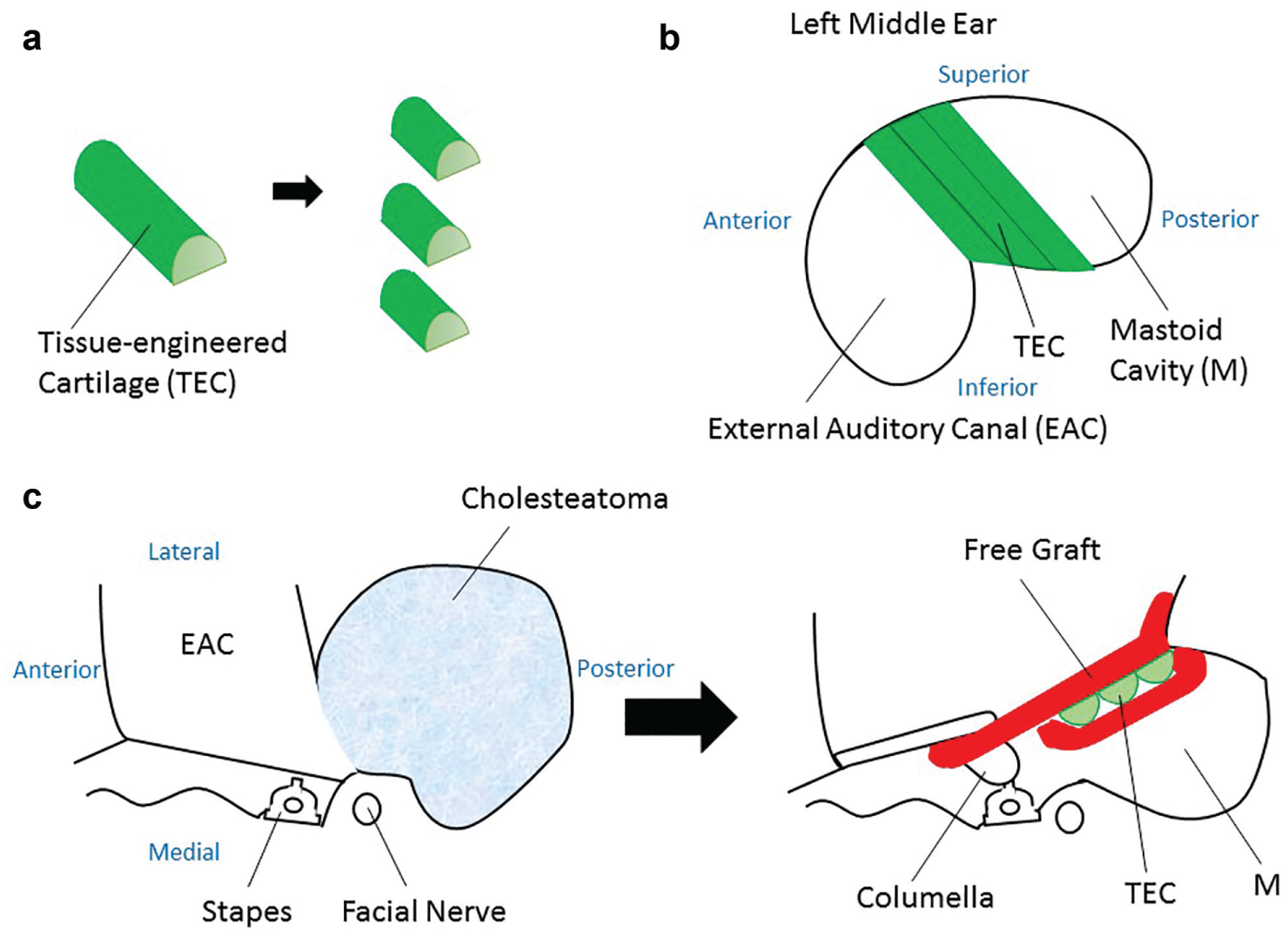
(a) Cutting tissue-engineered cartilage just before transplantation. (b) Placement of pieces of tissue-engineered cartilage to reconstruct the posterior canal wall after open mastoidectomy. (c) Transverse sections representing pre- and postoperative configurations.
The postoperative course was uneventful. Epithelialization of the tympanic membrane and external ear canal showed progress within 1 month and was complete by 3 months after surgery. The reconstructed posterior canal wall showed no retraction until 6 months after surgery. Local and computed tomography findings are shown in Figure 4 . The pure tone average was unchanged (23 dB HL before surgery and 20 dB HL 6 months after surgery). Severe adverse effects were not observed. Therefore, the procedure for this patient was considered “successful” according to the study criteria.
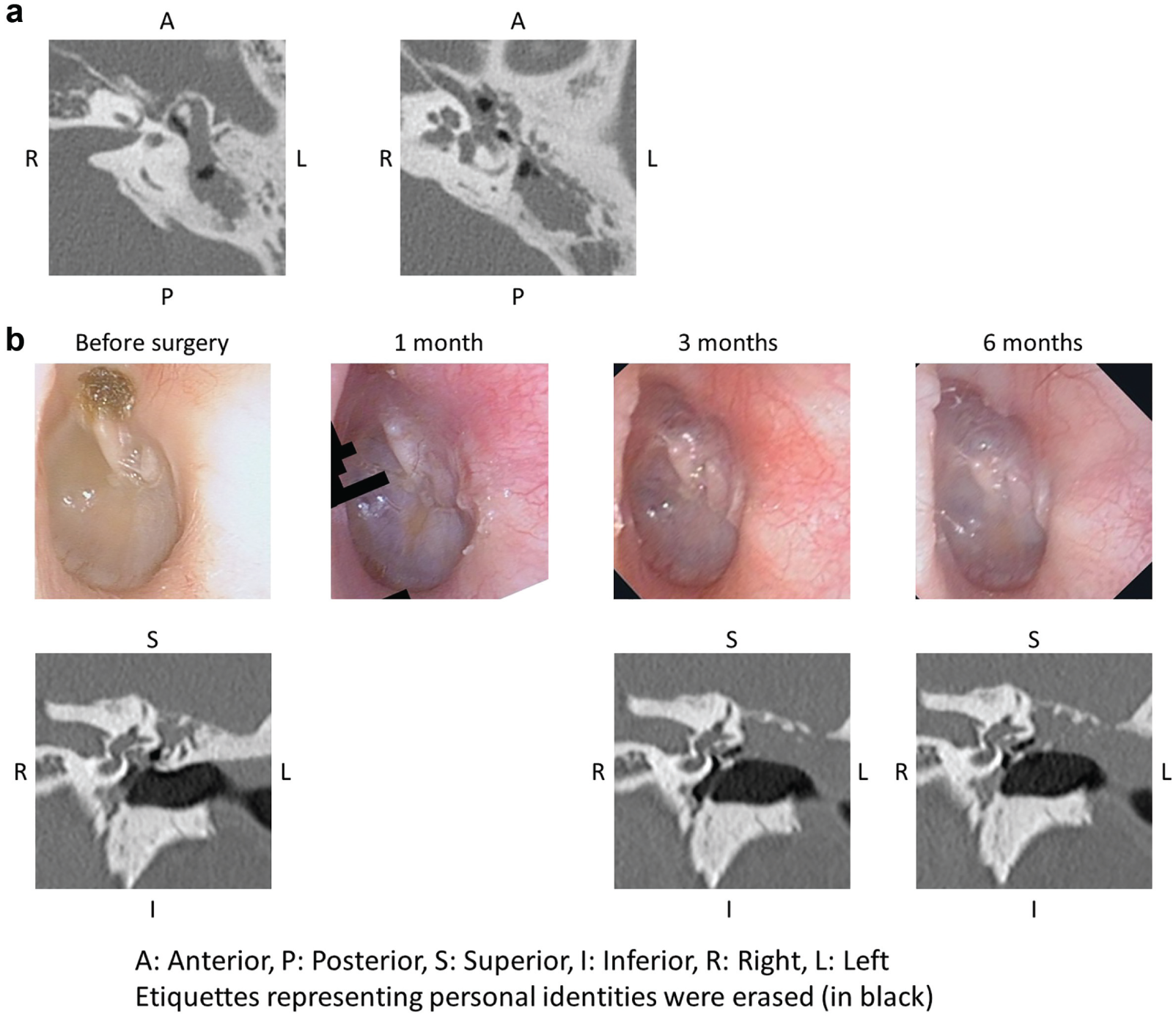
(a) Preoperative axial computed tomography scans showing the attic, antrum, and mastoid cavity. (b) Local findings and coronal computed tomography scans before and 1 month (photo only), 3 months, and 6 months after surgery.
Discussion
To the best of our knowledge, this is the first-in-human case of reconstructing middle ear bony structures with tissue-engineered cartilage, suggesting a promising future for satisfactory reconstruction with minimal morbidity at the donor site. The product was initially invented to reconstruct the nasal bridge (ie, a 1-dimensional structure). The present case is also important because it shows that the application of this product may be expanded to reconstruct a plane (ie, a 2-dimensional structure).
Although a large amount of artificial material is acceptable (eg, artificial hip/knee joints) in other body parts protected by thick subcutaneous tissues and muscles, solid tissue reconstruction in our field of otolaryngology is frequently associated with difficulties. In reconstructive approaches with tissue-engineered cartilage, pediatric laryngotracheal reconstruction was successful in animal models, 4 and a clinical application for auricular reconstruction with patient-specific ear-shaped cartilage was recently reported. 5 Tissue-engineering approaches for solid tissue reconstruction in otolaryngology are no longer a fantasy, but they are steadily becoming a reality.
Author Contributions
Disclosures
Footnotes
No sponsorships or competing interests have been disclosed for this article.
