Abstract
We report our experience using the ultrasonic bone aspirator (UBA) for transcanal endoscopic “inside out” mastoidectomy. The UBA has irrigation, suction, and nonrotatory ultrasonic bone-removing technology in 1 handpiece, which makes it appropriate for bone removal during this procedure. The results of our study show that this technique is safe and effective for patients with cholesteatoma in a small sclerotic mastoid. We also discuss the nuances associated with using the UBA during endoscopic ear surgery.
Drilling with simultaneous suction and irrigation during transcanal endoscopic “inside out” mastoidectomy (TEM) can be challenging. The rotating drill can tear the tympanomeatal flap, injure ossicles, or damage the facial nerve in the small working space of the external auditory canal (EAC). During TEM, instead of a standard drill, the ultrasonic bone aspirator (UBA) can be advantageous as it contains suction and irrigation in a single handpiece. This leaves the other hand free to navigate the endoscope. The UBA has a nonrotational head with a nonactive side, which protects the tympanomeatal flap and the surrounding tissue.
The primary aim of this article is to describe the use of the UBA in TEM for treatment of cholesteatoma in patients with a small sclerotic mastoid.
Methods and Results
A retrospective study of patients who underwent TEM with the UBA (Sonopet; Stryker Corporation, Kalamazoo, Michigan) was performed. Approval from the Louisiana State University Health Sciences Institutional Review Board (9738) was obtained for the study. Five patients with at least 12 months of follow-up were studied. Their ages ranged from 24 to 58 years. Mean follow-up was 1.7 years (range, 370-1105 days). All patients had an attic or posterior-superior retraction pocket with cholesteatoma extending to the antrum and contracted mastoids on computed tomography scan.
Rigid endoscopes (0° and 30°, 3 mm, 14 cm; Storz, Tuttlingen, Germany) were used. Procedures were performed under general anesthesia after local infiltration of 1% lidocaine with 1:100,000 epinephrine in the EAC. Facial nerve monitoring was performed in all cases. The extended tympanomeatal flap from 2 to 6 o’clock was elevated. If incudostapedial joint was intact, the incudostapedial joint was disarticulated and, if eroded, the incus remnant and malleus head were removed. The UBA with a 25-kHz angled handpiece was used at 80% power, 100% suction, and 10-mL/min irrigation. The Spetzler claw head was used to remove the bone from the outer attic wall and posterior-superior EAC wall to expose the cholesteatoma sac. The depth and extent of bone removal were assessed continuously to prevent injury to important structures. A stepwise atticotomy and atticoantrostomy were performed. The cholesteatoma was followed and removed from the attic to the antrum in a retrograde fashion.
With the endoscope, the sinus tympani and the anterior epitympanum were assessed for cholesteatoma. Ossicular reconstruction with partial prosthesis was done in 3 patients and deferred in 2 patients. The outer attic wall defect and tympanic membrane were repaired with tragal cartilage and perichondrium graft, and the tympanomeatal flap was reposited (
Figures 1
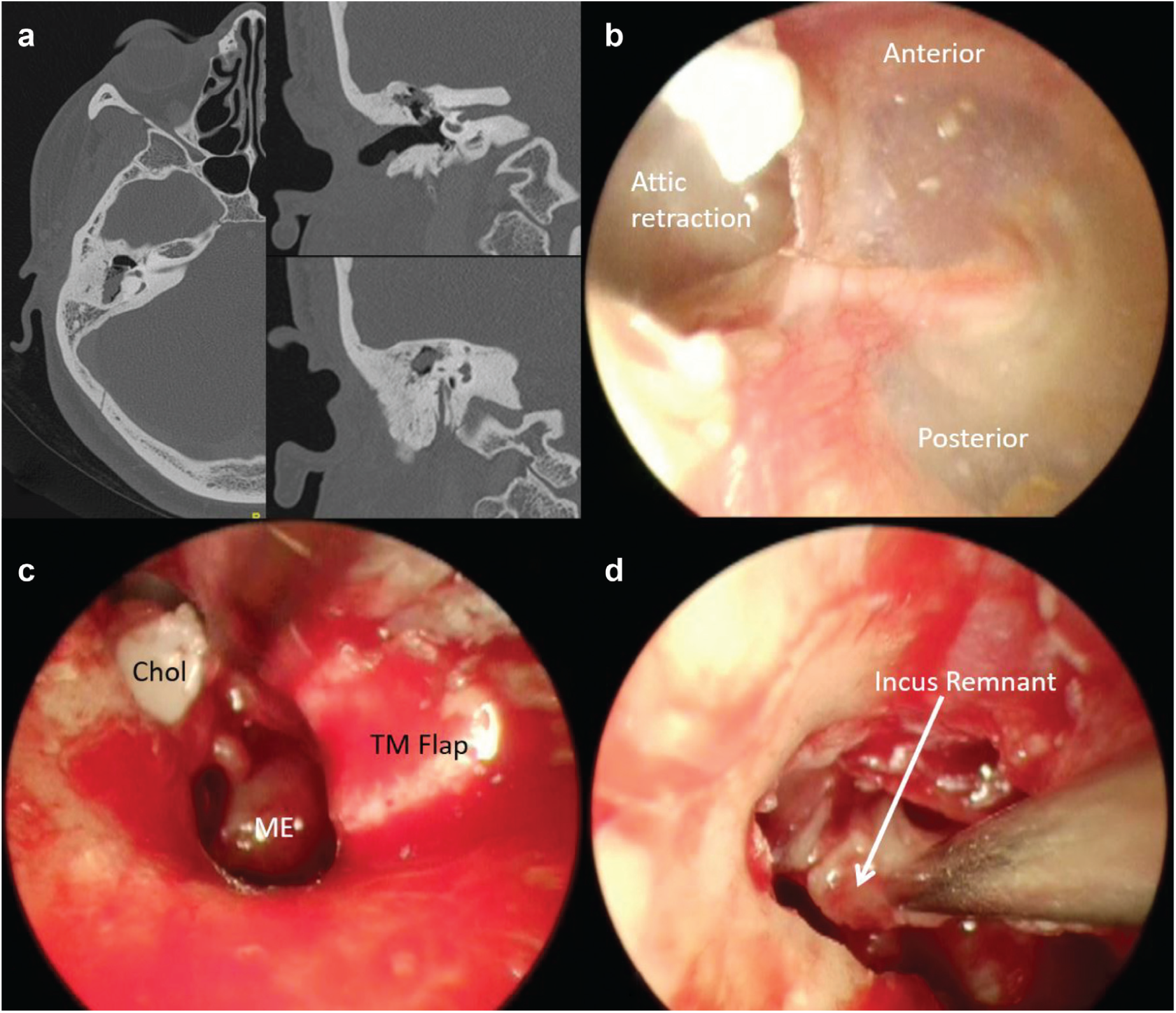
(a) Computed tomography temporal bone showing opacification of attic in sclerotic mastoid. Endoscopic view: (b) tympanomeatal (TM) flap with attic erosion, (c) after elevation of TM flap, and (d) incus removal. Chol, cholesteatoma; ME, middle ear.
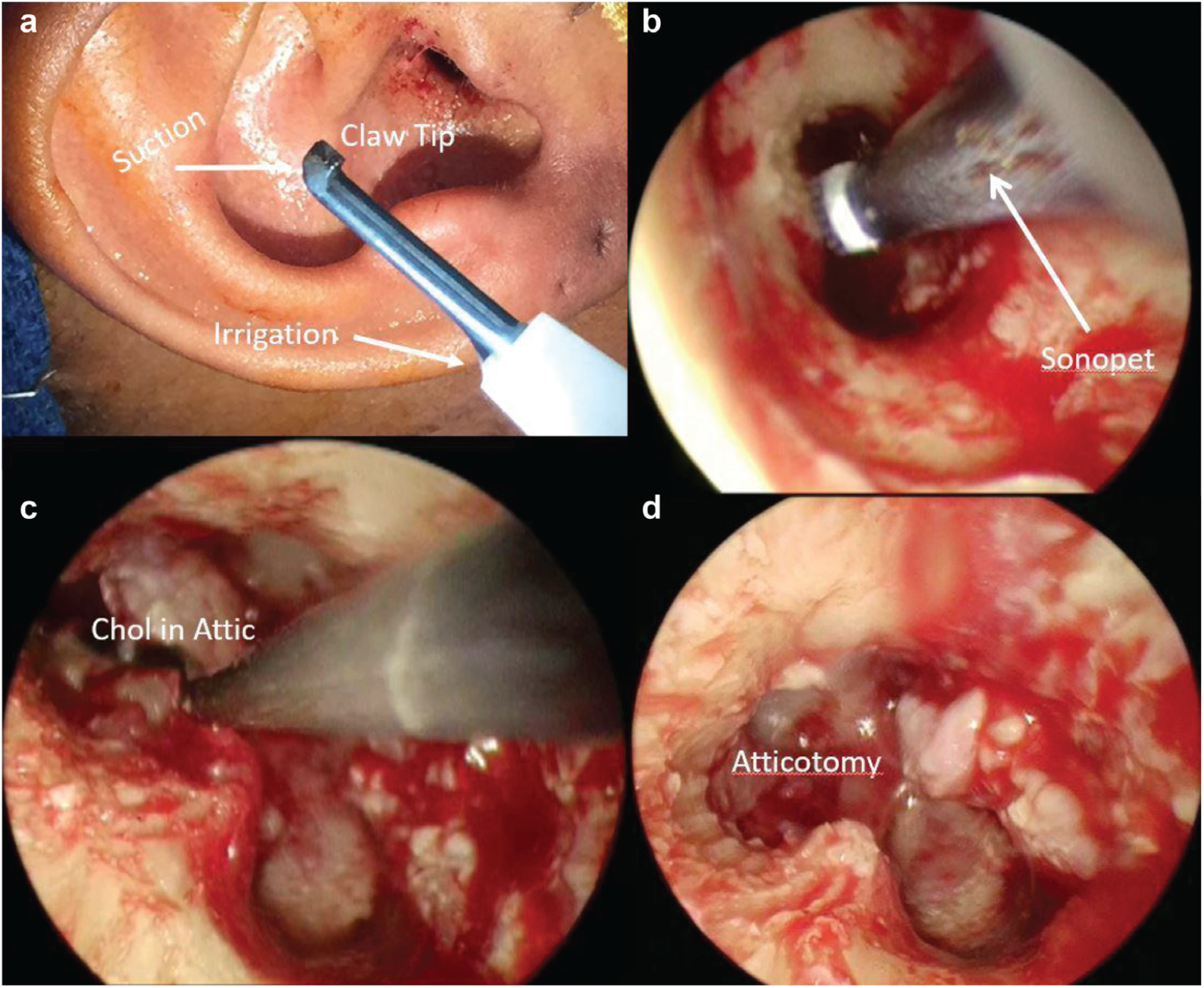
(a) Claw tip of the ultrasonic bone aspirator. (b) The ultrasonic bone aspirator removing posterior external auditory canal bone. (c) Endoscopic view of cholesteatoma (chol) in attic. (d) Endoscopic view of atticotomy.
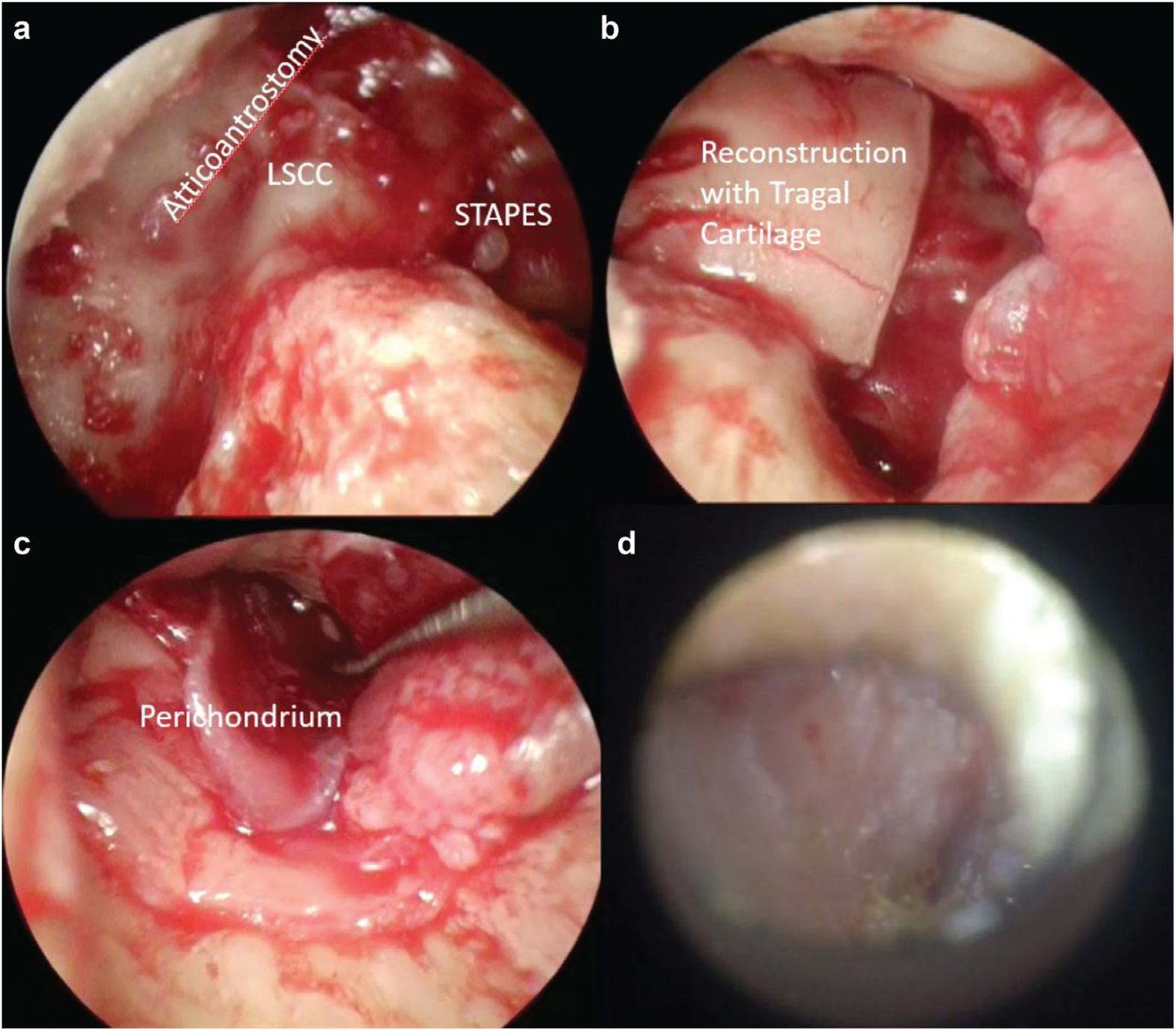
(a) After atticotomy and cholesteatoma removal. (b) Outer attic reconstruction with tragal cartilage. (c) View after reconstruction with cartilage, perichondrium, and tympanomeatal flap. (d) Postoperative 6 weeks. LSCC, lateral semicircular canal.
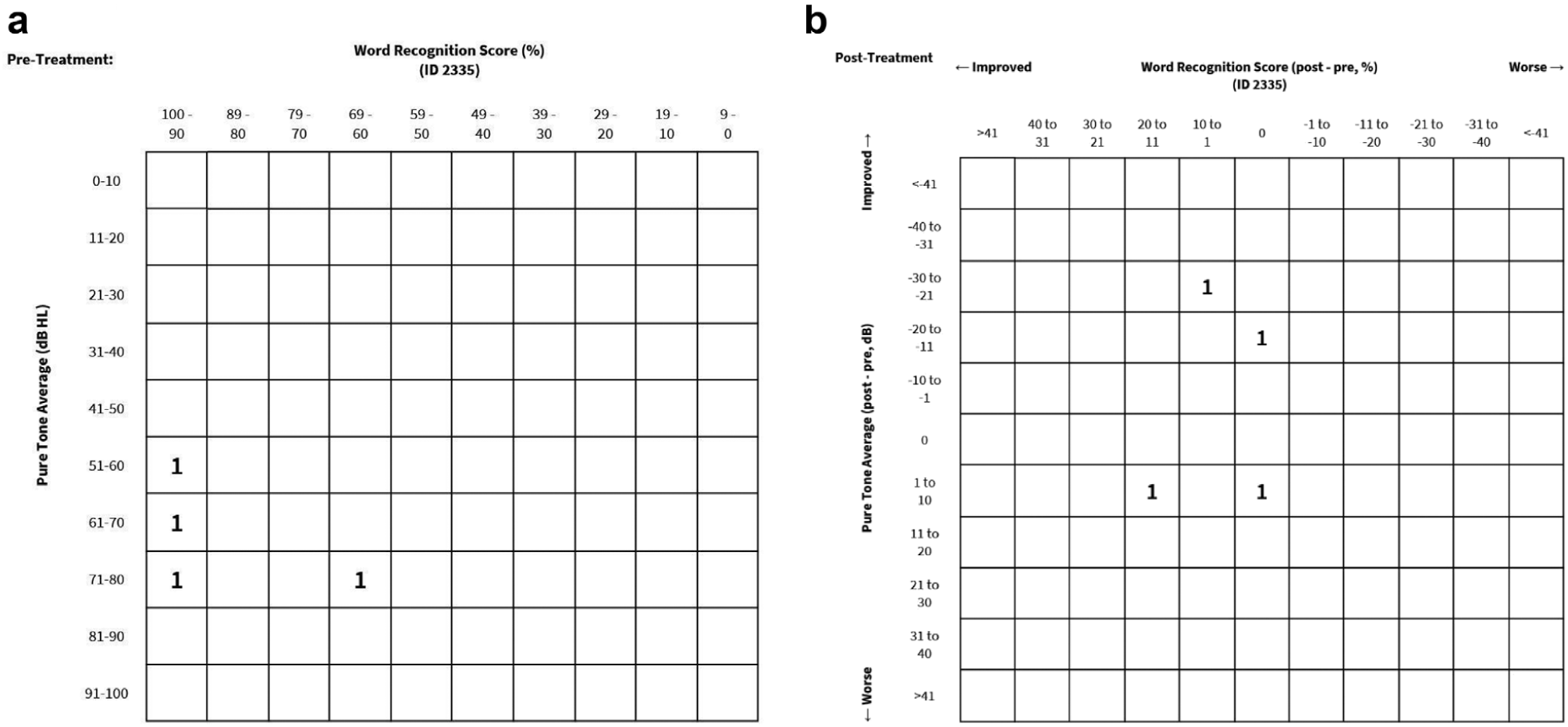
Scattergrams: (a) pretreatment and (b) posttreatment. For 4 patients, as 1 patient did not have a word recognition score because of a language barrier.
Discussion
Contracted mastoids can pose a challenge for traditional transcortical mastoidectomy with the microscope. There is a higher risk for tegmen, sigmoid sinus, or lateral semicircular canal damage. The “inside out” mastoidectomy approach may be safer than the “outside in” mastoidectomy for these patients. 1 As compared with the microscope, endoscopes greatly improve visualization of the middle ear and mastoid. A systematic review by Presutti et al 2 confirmed the importance of using endoscopes during cholesteatoma surgery. We perform TEM in a select group of patients with small sclerotic mastoids.
In this study, we used the UBA instead of a standard drill for TEM because it combines irrigation and suction in the handpiece itself, enabling the surgeon to perform 2-handed surgery using the endoscope. The UBA tip integrates longitudinal vibration with torsional oscillation to cut bone without absorbing ultrasonic vibrations. Meanwhile, the soft tissues oscillate and move away from the tip. The vibration amplitude ranges from 120 to 365 µm with a frequency of 25 kHz. The angled handpiece with its claw tip does not rotate 360°, thus preventing injury to the tympanomeatal flap. Irrigation emerges from a sheath near the tip of the handpiece and can be adjusted.
Kakehata et al 3 used the UBA to perform the atticotomy and then remove the thin bony attic shelf with hammer, chisels, and curettes. Finally, they polished the area with a high-speed curved burr. In contrast, we used the UBA with the Spetzler claw to perform the entire mastoidectomy.
Ito et al 4 measured the skull base vibrations created by the UBA and found identical levels as compared with those from a conventional drill. Brooks et al 5 showed minimal increase in the UBA temperature without excessive heat generation. These studies confirm that the UBA is safe for use in the ear. Our study corroborates their findings.
The main drawbacks of the UBA are its cost and the size of the handpiece. Cost is a legitimate concern in the current era of funding shortages. Sharing 1 machine across multiple specialties may be the way to keep the costs under control. Although the tip of the device is relatively small, the handpieces are not designed for otologic surgery. Therefore, for patients with an extremely narrow EAC, the size of the handpiece can make endoscopic ear surgery challenging.
The limitation of our study is the small number of patients and a relatively short follow-up. Further studies with a larger cohort of patients and a longer follow-up are required.
Conclusion
Endoscopic inside-out mastoidectomy with the UBA is a safe and effective technique for patients with cholesteatoma and a small sclerotic mastoid. Future goals include tailoring the ergonomics of the UBA handpiece for transcanal endoscopic ear surgery and studying outcomes in a larger series of patients with longer follow-up.
Author Contributions
Disclosures
Footnotes
No sponsorships or competing interests have been disclosed for this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
