Abstract

Granulomatosis with polyangiitis (GPA) or Wegener’s granulomatosis is a multisystemic disease with a complex genetic background. The clinical presentations are characterized by necrotizing granulomatous inflammation of the upper and lower respiratory tract, glomerulonephritis, and small-vessel vasculitis. 1 Systemic symptoms of GPA are nonspecific and include fatigue, fever, arthralgia, and weight loss. Head and neck manifestations occur in 90% of patients. The nose and paranasal sinuses are most commonly affected in up to 80%. 2 Nasal symptoms include serosanguinous discharge and headache and pain over the dorsum. Nasal findings include crusts covering friable mucosa, ulceration, septal perforation, and saddle-nose deformity. Involvement of salivary glands occurs in less than 1%. 3 A high level of clinical suspicion and appropriate diagnostic and laboratory investigations are crucial for early diagnosis. We report a case of bilateral parotid gland swelling and pus-draining parotid sinus secondary to GPA and discuss its presentations and management. The study was approved by the ethics committee of Alexandria Faculty of Medicine.
Case Report
A 25-year-old woman presented to the Alexandria University Hospital ENT clinic complaining of bilateral parotid swelling and right parotid sinus. The condition started 4 months prior by right parotid abscess, which was treated elsewhere by incision and drainage. The patient received medical treatment with partial improvement. Although partial improvement was noted, there was right parotid sinus formation with persistent pus drainage and no response to medical treatment. On admission, complete physical examination was done. The patient was conscious and alert with toxic look and fever. Standard ear, nose, and throat examination revealed bilateral parotid and submandibular gland swellings. The right parotid was tender with pus-draining sinus ( Figure 1 ). There was grade IV facial palsy on the right side. Examination of the external nose demonstrated supratip nasal depression (saddling) ( Figure 1 ). Nasal endoscopy revealed nasal crustations, inflamed mucosa, and 2 posterior septal perforations. Rheumatoid factor and cytoplasmic antineutrophil cytoplasmic antibodies (C-ANCA) were negative with elevated erythrocyte sedimentation rate (ESR) and C-reactive protein. Both chest X-ray and abdominal ultrasound were normal. Histopathological assessment of parotid open biopsy revealed heavy chronic suppurative granulomatous inflammation with fistula formation. Histopathological assessment of nasal biopsy revealed heavy chronic lymphoplasmacytic granulation tissue with granulomatoid lesions, vasculitis, and superadded heavy suppurative necrosis, featuring GPA ( Figures 2 and 3 ). The patient was referred to the rheumatology department to start the definite treatment of GPA: corticosteroids and immunosuppressant.
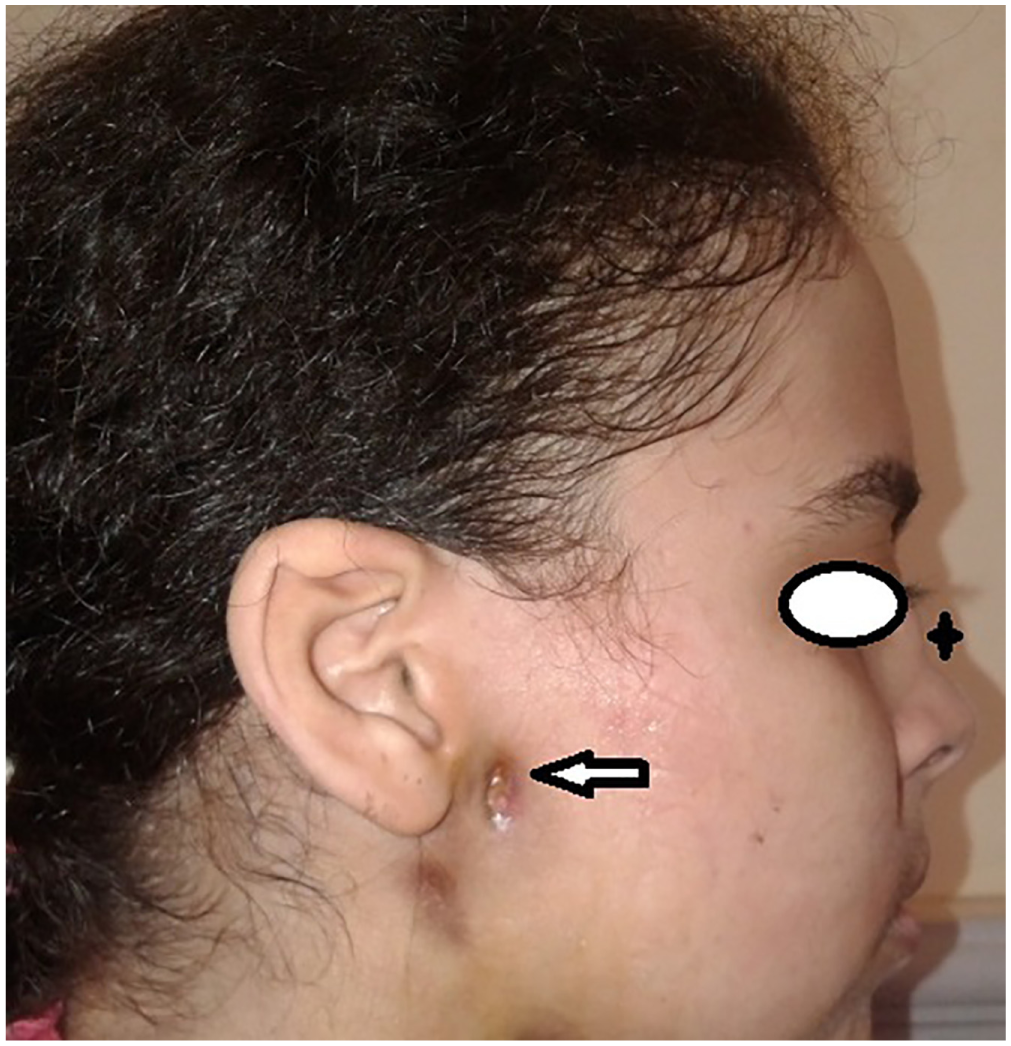
Right parotid fistula and nasal saddling.
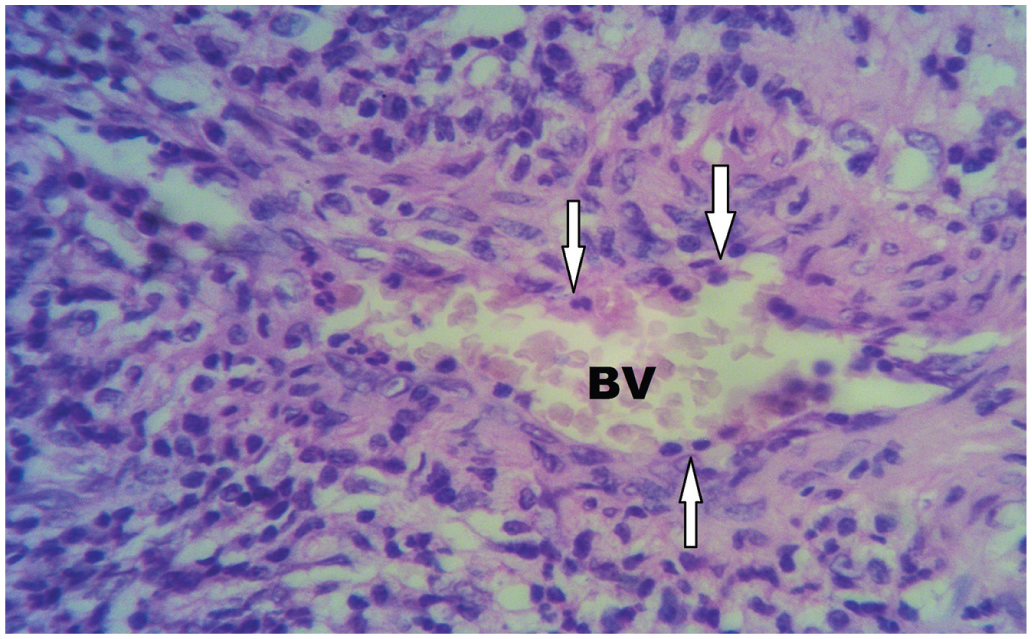
An area of heavy inflammatory infiltrate including a larger blood vessel (BV) with acute inflammatory cells in the wall (arrows) (hematoxylin and eosin, ×200).
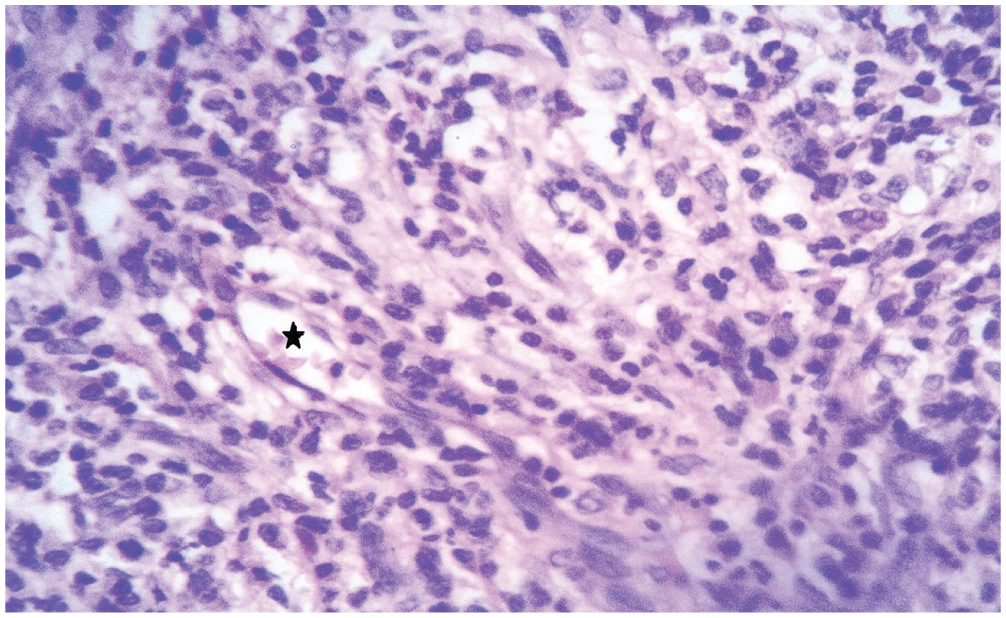
Chronic inflammatory cells, mainly lymphocytes and plasma cells, among compressed blood vessels (asterisk) (hematoxylin and eosin, ×200).
Discussion
In this case report, the clinical presentation of persistent pus-draining parotid sinus and diffuse affection of major salivary glands pointed to a systemic disease. The nasal findings of crustations, spontaneous septal perforation, and nasal saddling are among the clinical features of GPA. The confirmation of GPA was done based on the histopathological findings of necrotizing granulomatous inflammation with vasculitis.
Geyer et al 4 reported a case of GPA in a 69-year-old white woman presenting initially with a left parotid abscess that failed to respond to empiric therapy. The diagnosis of GPA was validated based on the clinical features (nasal and pulmonary), positive C-ANCA, and biopsy-proven necrotizing granulomatous inflammation with vasculitis. Other authors described patients with progressive parotid enlargement 5 or pus-producing sinus 6 refractory to medical treatment secondary to GPA.
Accurate diagnosis of GPA is based on clinical, histopathological, and laboratory investigations. The American College of Rheumatology (ACR) criteria permit the diagnosis with high sensitivity and specificity. 7 However, in the localized form of GPA, the ACR criteria are not fulfilled. Elevated C-ANCA titer is essential to confirm the diagnosis of GPA. The sensitivity of the test in systemic and localized GPA is 96% and 67%, respectively. 8
GPA can be treated effectively with immunosuppressive agents (cyclophosphamide or azathioprine) combined with steroids. The therapeutic response is good, with remission rates of up to 90%. If treatment is initiated early, serious systemic complications may be avoided. Long-term follow-up is essential to detect possible relapse, suggested by rising C-ANCA levels. 4
Author Contributions
Disclosures
Footnotes
