Abstract
Objective
Oral human papillomavirus (HPV) infection is the precursor for a growing subset of oropharyngeal squamous cell carcinomas (OPSCCs) in the developed world. This study was designed to characterize oral HPV infection and OPSCC in a region with high rates of HPV-driven cervical cancer.
Study Design
Cross-sectional cohort study, retrospective case series.
Setting
Northwest Cameroon referral hospital.
Subjects and Methods
Individuals infected with human immunodeficiency virus attending an outpatient clinic were evaluated for oral HPV infection with oral swabs or rinses that were tested for 51 HPV types. HNSCCs diagnosed and/or treated at the same hospital from 2011 to 2017 were retrospectively reviewed to ascertain demographic and tumor characteristics, and available OPSCCs were tested for HPV.
Results
The oral HPV infection study population comprised 101 participants. Most (69%) were female and never-smokers (84%). Participants had median 4 lifetime sexual partners (interquartile range, 3-7; range, 1-100). Five participants (5%) had oral HPV infection; one had 2 HPV types. HPV types detected were HPV68 (n = 2), HPV82 (n = 2), HPV32 (n = 1), and unknown (n = 1). No significant demographic or behavioral differences were detected among individuals with vs without oral HPV infection. OPSCCs comprised just 8% (n = 11) of 131 HNSCCs in the retrospective study population. Two of 7 OPSCCs were HPV positive.
Conclusion
The low prevalence of OPSCC observed in northwest Cameroon together with the rarity of oral HPV infection suggests low rates of HPV-driven oropharyngeal carcinogenesis in the region. Future research should examine how geographic differences in oral HPV infection are influenced by cultural norms and affect HPV-OPSCC epidemiology.
Keywords
High-risk human papillomavirus (HPV) causes nearly all cervical cancers and a growing subset of oropharyngeal squamous cell carcinomas (OPSCCs); however, these diseases are epidemiologically dissimilar on a global stage. 1 The highest incidence of cervical cancer is observed in sub-Saharan Africa, with age-standardized incidence rates of greater than 30 per 100,000 in most countries compared with less than 10 per 100,000 in North America. 1 In contrast, OPSCC is dramatically increasing in incidence among primarily men in the United States and other developed countries, a trend that is attributable to the increasing proportion caused by HPV2-6 but has scarcely been observed in sub-Saharan Africa outside of South Africa.1,7,8 Although cancer registries are limited in most of Africa, studies of head and neck cancer from Central, East, and West Africa include very few OPSCCs overall, comprising just 2% to 15% of head and neck squamous cell carcinomas (HNSCCs) in most cohorts 7 compared with >30% of HNSCCs in the United States, 3 with almost no evidence implicating HPV as a causative agent in African studies.1,9-11 Three studies from Mozambique, Ghana, and Senegal have examined HPV tumor status among oropharyngeal tumors, with just 2 reported “pharyngeal” tumors containing HPV DNA 9 out of 38 total tumors tested.9-11
Reasons for the low incidence of HPV-related OPCC (HPV-OPSCC) despite a high incidence of cervical cancer in sub-Saharan Africa are not well understood, especially considering the high prevalence of human immunodeficiency virus (HIV) infection in this region, which confers an increased risk of HPV-related cancers.12-14 OPSCC incidence is likely also strongly influenced by patterns of other important risk factors for HPV-OPSCC, including sexual behaviors and tobacco smoking.15,16
The putative precursor to HPV-OPSCC is oral HPV infection, most of which are cleared while a small subset go on to cause cancer.17,18 Both HPV-OPSCC and oral HPV infection are strongly associated with sexual behaviors, tobacco use, and male sex, and both have a higher prevalence among HIV-infected individuals.16,19,20 Although the natural history of the transition from oral HPV infection to OPSCC is not well defined, understanding oral HPV infection can provide valuable insight into the epidemiology of HPV-OPSCC. 21
The purpose of this study was to characterize the unique epidemiology of HPV-OPSCC and its precursor, oral HPV infection, in rural northwest Cameroon. Our approach was 2-fold: we tested a cohort of HIV-infected individuals for oral HPV infection to ascertain the prevalence of oral HPV infection in a population expected to have a high infection rate. We then retrospectively examined the prevalence of OPSCCs among all HNSCCs diagnosed in the same geographic region and analyzed archival OPSCC tumor samples for HPV status.
Methods
Oral HPV Infection Cohort Study
This was a cross-sectional cohort study. Eligible participants were HIV-infected adults over age 21 years attending the HIV clinic at Mbingo Baptist Hospital (MBH), a large referral hospital in northwest Cameroon, during October 2014 and April to May 2015. Written informed consent was obtained, and demographic and behavioral data were collected using a written survey administered verbally with the assistance of a native Cameroonian study team member. Oral swabs of the oropharynx and oral cavity were collected in October 2014 (due to concern for shipping infectious material during the contemporaneous Ebola virus outbreak), and oral rinse and gargle samples were collected in April to May 2015. Samples were evaluated for DNA from 51 HPV types using a commercially available polymerase chain reaction (PCR)–based test (OraRisk; Access Genetics, Eden Prairie, Minnesota). Participants also underwent an oral and neck exam by a head and neck surgeon and were referred to an appropriate specialist for further evaluation of any abnormalities. In exchange for study participation, participants received a CD4 cell count blood test as part of their routine clinical care free of charge (US$11 value). Medical record abstraction was performed to obtain CD4 cell count, date of HIV diagnosis, and antiretroviral therapy status.
Retrospective Study of OPSCC Prevalence
Pathology records at MBH were queried for squamous cell carcinomas of the head and neck diagnosed and/or treated from August 2011 to August 2017. Cases eligible for inclusion were biopsy-proven squamous cell carcinomas of the larynx, oral cavity, oropharynx, nasopharynx, and nasal cavity/paranasal sinuses. Duplicate cases were excluded (eg, biopsy for a subsequent resection specimen). Age, sex, and primary site were recorded.
OPSCC HPV Tumor Testing
OPSCCs with available archival paraffin-embedded tumor specimens were tested for HPV tumor status. Hematoxylin and eosin sections from all cases were reviewed by a head and neck pathologist to confirm a diagnosis of squamous cell carcinoma. Whole-slide sections of formalin-fixed, paraffin-embedded primary tumors were cut at a 5-micron thickness and deparaffinized. Immunohistochemistry (IHC) was performed for p16 (clone INK4a; Ventana Medical Systems, Tucson, Arizona; prediluted) using the UltraView polymer detection kit (Ventana) on a BenchMark XT autostainer (Ventana). RNA in situ hybridization (ISH) for high-risk HPV E6/E7 messenger RNA (mRNA) was performed using the RNAscope HPV-HR18 Probe (Advanced Cell Diagnostics, Hayward, California), a single cocktail probe recognizing 18 high-risk HPV genotypes (16, 18, 26, 31, 33, 35, 39, 45, 51, 52, 53, 56, 58, 59, 66, 68, 73, and 82), also on a BenchMark XT autostainer (Ventana). All staining was done according to manufacturers’ instructions in the presence of appropriate controls. p16 was considered positive in the presence of >70% diffuse nuclear and cytoplasmic positivity. HPV RNA ISH was scored as positive if multiple punctate brown signals could be identified in the cytoplasm or nucleus of >50% of tumor cells. OPSCCs were considered HPV related if they were both p16 positive and HPV RNA ISH positive.
Data Analysis
Descriptive statistics were reported as number (%), median with interquartile range (IQR), and range or prevalence with 95% confidence interval (CI). Characteristics were compared by the presence of oral HPV infection using Fisher’s exact tests. This study was approved by the institutional review boards of both Johns Hopkins Medicine and Mbingo Baptist Hospital.
Results
Oral HPV Infection Cohort Study
There were 101 participants in this cohort study. Characteristics of the study population are described in Table 1 . Most (70 of 101, 69%) were female, and median age was 42 years (IQR, 37-48; range, 24-69). All but 2 participants were taking antiretroviral therapy, and median CD4 count was 474 cells/mm3 (IQR, 319-650; range, 14-2021). Few participants reported a history of tobacco smoking (16, 16%), and significantly more men than women had ever smoked (14 of 31 [45%] men compared with 2 of 70 [3%] women, P < .001). Just 2 men and no women reported current smoking. Most participants had a primary school education or less (59%), and most were either currently (50%) or previously (28%) married. Participants had a median of 4 lifetime sexual partners (IQR, 3-7; range, 1-100), and the median age of first sexual intercourse was 18 years (IQR, 17-20; range, 12-30).
Characteristics of Oral HPV Infection Study Population Recruited from HIV Clinic at Mbingo Baptist Hospital in Northwest Cameroon. a
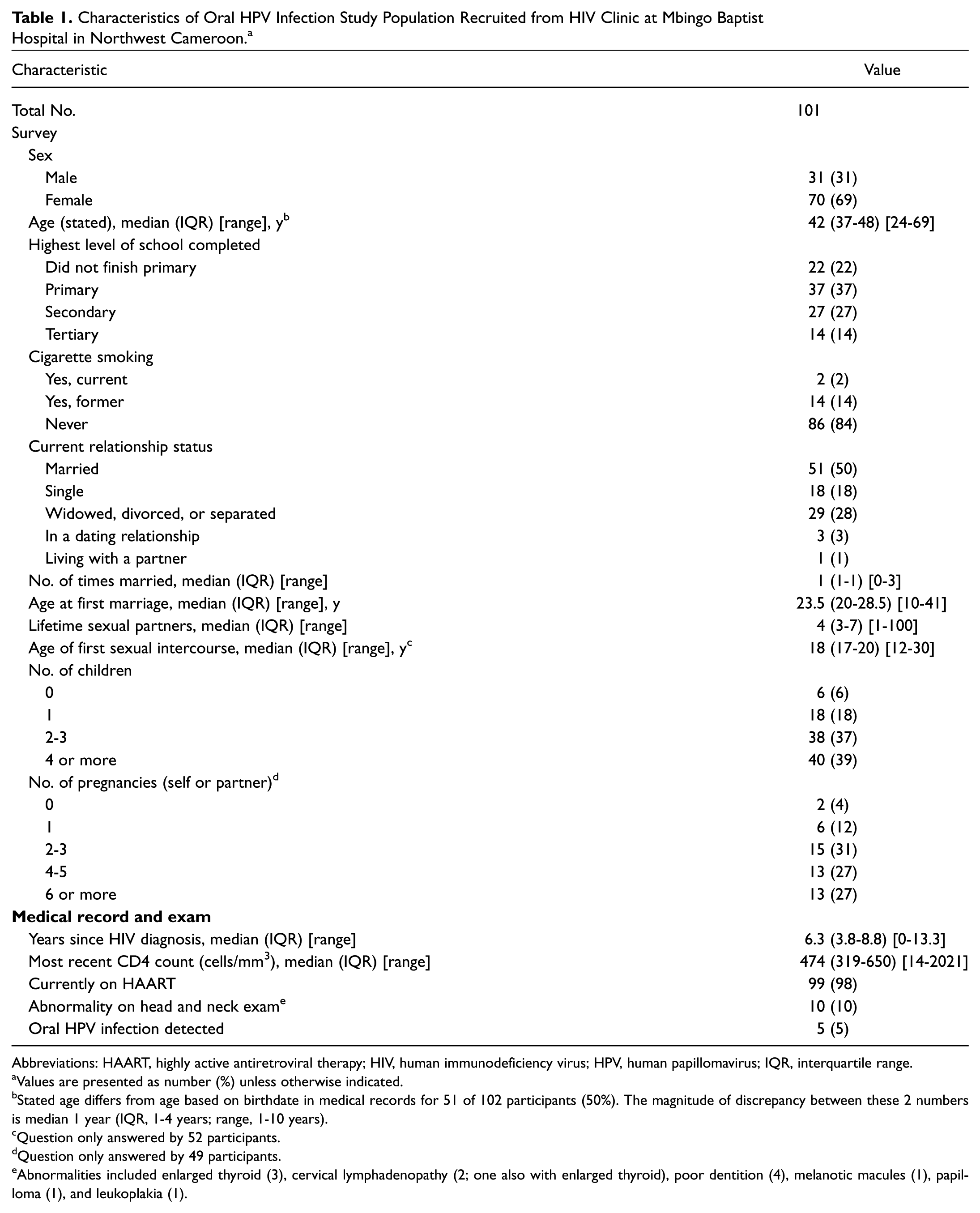

Abbreviations: HAART, highly active antiretroviral therapy; HIV, human immunodeficiency virus; HPV, human papillomavirus; IQR, interquartile range.
Values are presented as number (%) unless otherwise indicated.
Stated age differs from age based on birthdate in medical records for 51 of 102 participants (50%). The magnitude of discrepancy between these 2 numbers is median 1 year (IQR, 1-4 years; range, 1-10 years).
Question only answered by 52 participants.
Question only answered by 49 participants.
Abnormalities included enlarged thyroid (3), cervical lymphadenopathy (2; one also with enlarged thyroid), poor dentition (4), melanotic macules (1), papilloma (1), and leukoplakia (1).
Five participants (5%; 95% CI, 2%-11%) had any HPV detected in oral swab or rinse samples, and 4 (4%) had oncogenic HPV infections ( Table 2 ). HPV types detected included HPV68 (2 participants), HPV82 (2 participants), HPV32 (1 participants), and an unknown HPV type (1 participant). One participant, a married man with 8 lifetime sexual partners, had 2 types of HPV detected (HPV68 and HPV32). All 4 other participants were women and reported between 4 and 10 lifetime sexual partners. None of these 5 participants reported a history of smoking. Although a higher proportion of participants with oral HPV infection had some secondary education compared to those without oral HPV infection (80% vs 39%, P = .16), there were no significant differences in the demographics, behavioral profile, or CD4 count among individuals with compared to those without oral HPV infection.
Characteristics of Individual Study Participants with Oral HPV Infection (n = 5).
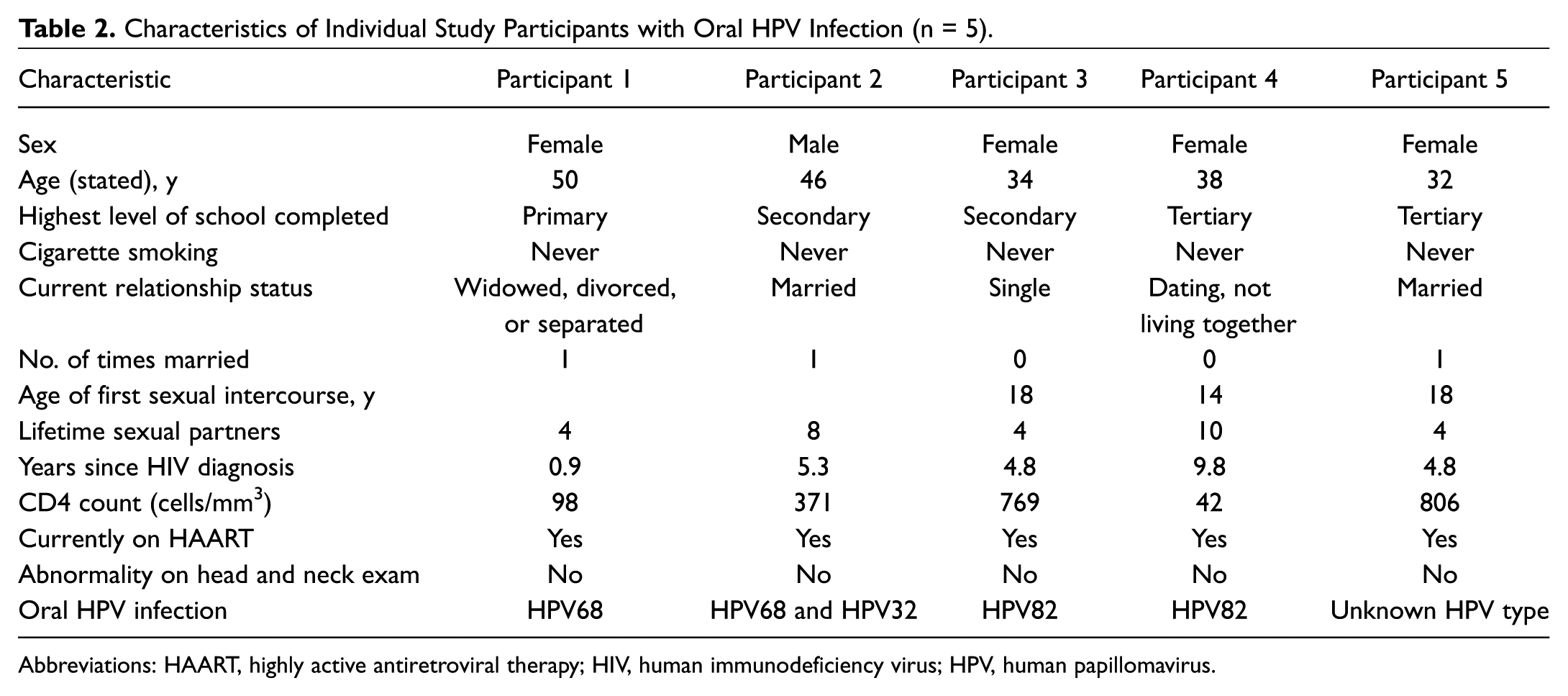

Abbreviations: HAART, highly active antiretroviral therapy; HIV, human immunodeficiency virus; HPV, human papillomavirus.
OPSCC Epidemiology and HPV Status
There were 131 HNSCCs identified in the pathology database at Mbingo Hospital between August 2011 and August 2017 ( Table 3 ). Most patients with HNSCC were men (97, 74%), and median age was 59 years (IQR, 50-68). The most common primary tumor sites were larynx (55, 42%) and oral cavity (41, 31%). There were only 11 (8%; 95% CI, 5%-14%) oropharyngeal squamous cell carcinomas, with the majority (8, 73%) diagnosed in men. Seven of these tumors were available for HPV testing, of which 2 (29%) were positive for both p16 IHC and HPV RNA ISH. Both of these HPV-related squamous cell carcinomas were from men.
Characteristics of Patients Diagnosed with Head and Neck Squamous Cell Carcinoma at Mbingo Baptist Hospital in Northwest Cameroon from 2011 to 2017.
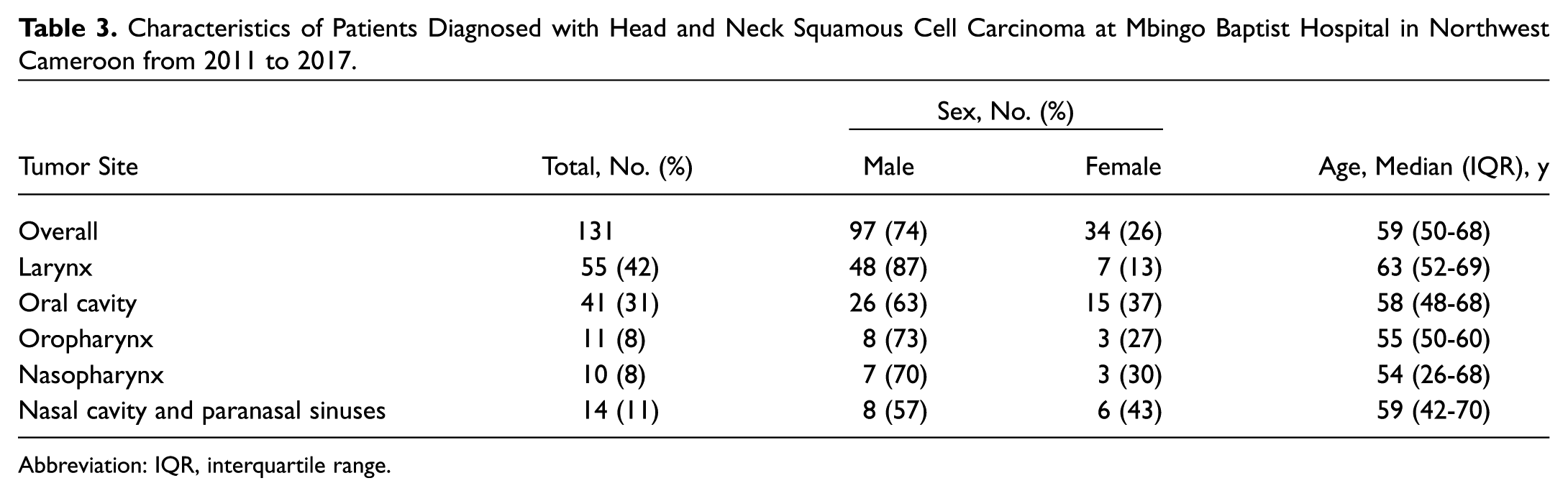
Abbreviation: IQR, interquartile range.
Discussion
Oral HPV infection was rare among HIV-infected individuals attending a referral hospital clinic in Mbingo, northwest Cameroon. The 5% prevalence of oral HPV infection that we observed is much lower than reported prevalence rates among cohorts of HIV-infected individuals in the United States (14%-45%),19,22 South Africa (20%-33%),23-25 and Europe (15%-20%).26,27 The oral HPV infection prevalence was lower even than the US general population prevalence of 7%. 20 HPV16, the most common oncogenic HPV type detected in oral rinses in other regions and the cause of over 90% of HPV-OPSCCs, 28 was not detected in our study, compared with a prevalence of up to 6% in other HIV-infected populations. 19 These findings are in agreement with the low rates of OPSCC observed in the region in ours and other studies1,7,9-11 and with the small percentage of OPSCCs that were HPV related.
Reasons for the low oral HPV infection rate in our study likely relate to patterns of non-HIV risk factors for oral HPV infection. Tobacco smoking is an independent risk factor for oral HPV infection, with higher risk of infection with increasing number of cigarettes smoked per day. 20 Few of our study participants reported ever smoking, and just 2 men reported current smoking, which is consistent with low reported Cameroonian smoking rates (6% overall; 0.5% for women and 12% for men). 29 HPV is a sexually transmitted infection that is strongly associated with oral sexual behaviors.21,30 Although we did not collect data regarding oral sexual behaviors in our study for reasons of cultural sensitivity, the limited information available from Cameroon and neighboring Nigeria suggests relatively low rates of oral sexual behaviors. A study of 2260 female sex workers in Cameroon found that only 22% reported ever having oral sex. 31 Another study of Nigerian male and female adolescents ages 15 to 24 years reported that although 97% reported having had vaginal sex, only 9% had ever participated in oral sex. 32 In contrast, 84% of a representative sample of the US population (2116 men and 2140 women) reported ever having had oral sex. 21 Finally, oral HPV infection is higher among men than women in other populations studied. 20 Our study included more women than men, so it is conceivable that a study population with more men may have yielded different results; however, only 1 of the 31 men in our study had oral HPV infection.
The low prevalence of 8% OPSCCs among the HNSCCs diagnosed and/or treated at Mbingo Baptist Hospital is consistent with other studies of HNSCC in sub-Saharan Africa 7 but differs markedly from the epidemiology observed in the United States and other developed countries. Nearly a third (31%) of HNSCCs diagnosed in the United States from 1992 to 2014 arose from the oropharynx, a percentage that is expected to increase as the incidence of OPSCC rises while that of nonoropharynx HNSCC falls. 3 In contrast, larynx and oral cavity tumors comprised 73% of HNSCCs at Mbingo Baptist Hospital in our study but accounted for just 57% of tumors in the United States. 3
The trends in OPSCC incidence in the United States and other developed countries are largely attributable to an increasing percentage of OPSCCs caused by HPV: whereas HPV was responsible for just 16% of OPSCCs in the 1980s, it now causes over 70% of tumors.4,5 Although there were only 7 tumors available for HPV testing in our study, just 2 were HPV related. Taken together with the rarity of oral HPV infection in the same geographic region, this suggests that the observed low prevalence of OPSCC in northwest Cameroon relative to other countries is related to limited oropharyngeal exposure to HPV, which in turn limits rates of HPV-driven carcinogenesis in the lymphoid tissues of the palatine and lingual tonsils.
Conclusion
In summary, the prevalence of oral HPV infection is low among HIV-infected individuals attending the Mbingo Hospital HIV Clinic in northwestern Cameroon, which may be a function of low rates of tobacco smoking and oral sex in the region. Correspondingly, the prevalence of OPSCCs and the percentage of OPSCCs caused by HPV are both markedly lower than have been observed in geographical regions with higher rates of oral HPV infection. Future research should examine how geographic differences in oral HPV infection are influenced by cultural norms and affect HPV-OPSCC epidemiology.
Author Contributions
Disclosures
Footnotes
Acknowledgements
We thank Debbie Bardin, Zita Acha, Aluv Victorine Ngwe, and the staff of the Care and Treatment Outpatient Clinic at Mbingo Baptist Hospital for their assistance, without which this study would not have been possible. We also thank our study participants for their courage and generosity. Finally, we thank the American Academy of Otolaryngology–Head and Neck Surgery Foundation for the Humanitarian Travel Grant that facilitated resident travel to Cameroon, during which this work was performed.
Sponsorships or competing interests that may be relevant to content are disclosed at the end of this article.
These data were presented in part at the American Head and Neck Society 9th International Conference on Head and Neck Cancer; July 16-20, 2016; Seattle, Washington.
