Abstract
Objective
To evaluate the efficacy of preoperative 18F-fluorodeoxyglucose positron emission tomography/computed tomography (PET/CT) for detecting cervical lymph node (LN) metastasis in papillary thyroid carcinoma (PTC).
Study Design
Case series with chart review.
Setting
University tertiary care facility.
Subjects and Methods
We retrospectively compared the pathologic results for 409 cervical LN levels in 140 patients who underwent thyroidectomy and central neck dissection with/without lateral neck dissection with the findings of preoperative PET/CT, ultrasonography (US), and CT. We judged LN metastasis in PET/CT using the maximum standardized uptake value (SUVmax) at the optimal cutoff value in receiver operating characteristic curves and compared the sensitivity, specificity, and diagnostic accuracy of the 3 imaging tools.
Results
At all neck levels (central and lateral compartments), PET/CT had a sensitivity of 57.5%, specificity of 68.6%, and diagnostic accuracy of 63.6% when the cutoff value of SUVmax was 1.125. The corresponding values were 59.1%, 90.6%, and 76.3%, respectively, for US and 53.8%, 91.9%, and 74.6% for CT. In the central compartment (level VI), sensitivity, specificity, and diagnostic accuracy were 48.9%, 67.4%, and 59.9% for PET/CT (cutoff SUVmax 1.125); 47.8%, 96.3%, and 76.7% for US; and 41.3%, 97.0%, and 74.4% for CT, respectively. In the lateral compartment (levels II-V), the corresponding values of sensitivity, specificity, and diagnostic accuracy were 70.2%, 69.3%, and 69.8% for PET/CT (cutoff SUVmax 1.055); 70.2%, 81.8%, and 75.8% for US; and 65.9%, 84.1%, and 74.7% for CT.
Conclusion
PET/CT is less effective as a preoperative diagnostic tool for detecting cervical lymph node metastasis in PTC than US or CT.
Keywords
Cervical lymph node (LN) metastasis of papillary thyroid carcinomas (PTCs) occurs in about 30% to 80% of patients1,2 and is an important prognostic factor for local or regional recurrence of PTC.3,4 It also has an adverse prognostic effect on survival, especially in older patients. 5 American Thyroid Association guidelines recommend that therapeutic central neck dissection (CND) for patients with clinically involved central LNs should accompany total thyroidectomy. Prophylactic CND should be considered for advanced primary tumors (T3 or T4) or clinically involved lateral neck nodes (cN1b), or if the information obtained will be used to plan further steps in therapy, although this is still controversial. 6 For lateral compartment LNs, most surgeons recommend therapeutic lateral compartmental LN dissection for clinically proven metastases. However, prophylactic lateral neck dissection for PTC is usually not recommended.7,8 Therefore, strict evaluation of cervical LN metastases is important for accurate staging and for planning the appropriate treatment before surgery and to minimize unnecessary neck dissection.
Cervical LN metastasis of PTC can be evaluated by physical examination and imaging tests such as ultrasonography (US), computed tomography (CT), magnetic resonance imaging (MRI), and 18F-fluorodeoxyglucose (18F-FDG) positron emission tomography/computed tomography (PET/CT). Ultrasonography and CT are currently the most popular diagnostic imaging methods for preoperative evaluation of cervical LN metastasis of PTC.9,10
In recent years, 18F-FDG PET/CT has become widely used to detect primary tumors, occult LN metastasis, and distant metastasis in a variety of malignancies, including thyroid cancer. It is especially useful in establishing recurrence in patients with elevated serum thyroglobulin and negative radioiodine whole-body scans after total thyroidectomy.11,12 There have been a few studies analyzing the features and diagnostic value of 18F-FDG PET/CT in evaluating cervical LN metastasis in PTC, but most of these studies were based on low numbers of patients or contained bias because they were multicenter studies. Also, they set an arbitrary maximum standardized uptake value (SUVmax) of 2.0, which is the general cancer uptake criterion for thyroid nodules themselves. Also, FDG uptake was graded on a subjective visual scale. Therefore, the exact effectiveness of 18F-FDG PET/CT in evaluating cervical LN metastasis has not been fully established.
The purpose of this study was to evaluate the diagnostic value of preoperative 18F-FDG PET/CT for detecting cervical LN metastasis in PTC by comparing it with US and CT. We also aimed to establish the optimal value of SUVmax of LNs for use in the differential diagnosis of metastatic and benign LNs.
Materials and Methods
Patients and Operation
We retrospectively analyzed the medical records and preoperative 18F-FDG PET/CT, US, and contrast-enhanced CT imaging findings for 140 patients with PTC who underwent thyroidectomy and CND with/without lateral neck dissection (LND) and who underwent preoperative 18F-FDG PET/CT in a tertiary hospital from March 2007 to December 2012. Preoperative 18F-FDG PET/CT was not performed routinely in all patients with PTC in our hospital: some patients underwent 18F-FDG PET/CT preoperatively to evaluate distant and regional metastasis after diagnosis with PTC by fine-needle aspiration cytology; others underwent 18F-FDG PET/CT during a routine health examination and PTC was found incidentally. Exclusion criteria were other types of thyroid cancer, distant metastases, recurrent cases, cancer of other organs, and histories of head and neck irradiation and surgery. This study was approved by the Institutional Review Board of Hanyang University Guri Hospital (GURI 2017-08-002-001).
Ultrasonography and Contrast-Enhanced CT
Preoperative US and CT with contrast enhancement were carried out routinely in all patients with PTC. All US and CT examinations and their interpretation were performed by 1 expert radiologist. The criteria for identifying metastases in US images were as follows: round shape (ratio of long/short diameter, <2), extracapsular spread, cystic change, calcification (microcalcification), hyperechogenicity, and heterogeneous inner structure. 13 The criteria in the case of CT images were round shape, enhancement, heterogeneity, and cystic and necrotic change. The size criteria for both US and CT were nodal diameter >1.5 cm for the long axes of the jugulodigastric and submandibular nodes and >1.0 cm for all other cervical lymph nodes except for level VI. 14
18F-FDG PET/CT
A dedicated whole-body 18F-FDG PET/CT system (Biograph 6; Siemens Medical Systems, Knoxville, Tennessee) was used. Before the injection of 18F-FDG, all patients fasted for at least 6 hours to maintain serum glucose concentrations below 200 mg/dL. Sugar-free liquids were permitted. After the intravenous injection of 18F-FDG (0.21 mCi/kg), a CT scan was used to adjust attenuation before the PET scan. PET scans were acquired from the proximal thigh to the base of the skull. 18F-FDG uptake by cervical lymph nodes was evaluated by the naked eye and by quantitative measurement using SUVmax. If any focally increased uptake lesion was detected by eye in the neck on maximum-intensity projection images, uptake by lymph nodes was assessed by careful examination of the axial 18F-FDG PET/CT images by 2 expert nuclear medicine physicians. Then SUVmax was calculated from the following formula: SUV = [FDG activity concentration (Bq/mL)] × [total lean body mass (kg)] / [injected FDG activity (Bq)]. If the uptake was not distinct from the blood or muscle tissue, it was excluded.
Data Analysis
We analyzed both cervical LNs on a per level basis, using the cervical LN levels in the American Joint Committee on Cancer staging manual. 15 A total of 409 cervical LN levels in 140 patients with findings of preoperative 18F-FDG PET/CT, US, and CT were evaluated. The neck levels were divided into 3 groups: total (central and lateral compartments), central (level VI), and lateral (levels II-V) compartments. We used receiver operating characteristic (ROC) curve analysis to determine the optimal SUVmax for differential diagnosis between benign and malignant LNs. We analyzed and compared the sensitivity, specificity, and diagnostic accuracy of the 3 imaging tools as applied to the total, central, and lateral neck compartments. The McNemar test was used to determine whether the sensitivities, specificities, and diagnostic accuracies of US, CT, and 18F-FDG PET/CT differed significantly. All analyses were performed using SPSS Statistics for Windows, Version 18.0 (SPSS, Inc, an IBM Company, Chicago, Illinois).
Results
Patient demographics and tumor characteristics are summarized in Table 1 . Of the total of 140 patients, 131 underwent total thyroidectomy and 9 unilateral lobectomy. All patients underwent ipsilateral (39 cases, 27.9%) or bilateral (101 cases, 72.1%) CND with thyroidectomy. Of total 241 central LN levels, 227 levels were analyzed. Fourteen central LN levels were excluded because of no distinct SUV uptake compared to the blood vessels or muscle tissue. Therapeutic lateral neck dissection was performed in 51 patients with LN metastasis suspected on the imaging findings. Ipsilateral lateral neck dissection was performed in 44 patients (31.4%) and bilateral lateral neck dissection in 7 patients (5%). Of 58 lateral necks, the extent of lateral neck dissection was levels II, III, IV, and V in 30 necks; levels II, III, and IV in 5 necks; levels III, IV, and V in 5 necks; and others in 18 necks. No patients underwent level I dissection with suspected metastatic LNs at level I. Therefore, total 182 lateral LN levels were analyzed in this study.
Demographic and Clinicopathologic Characteristics of the Patients. a
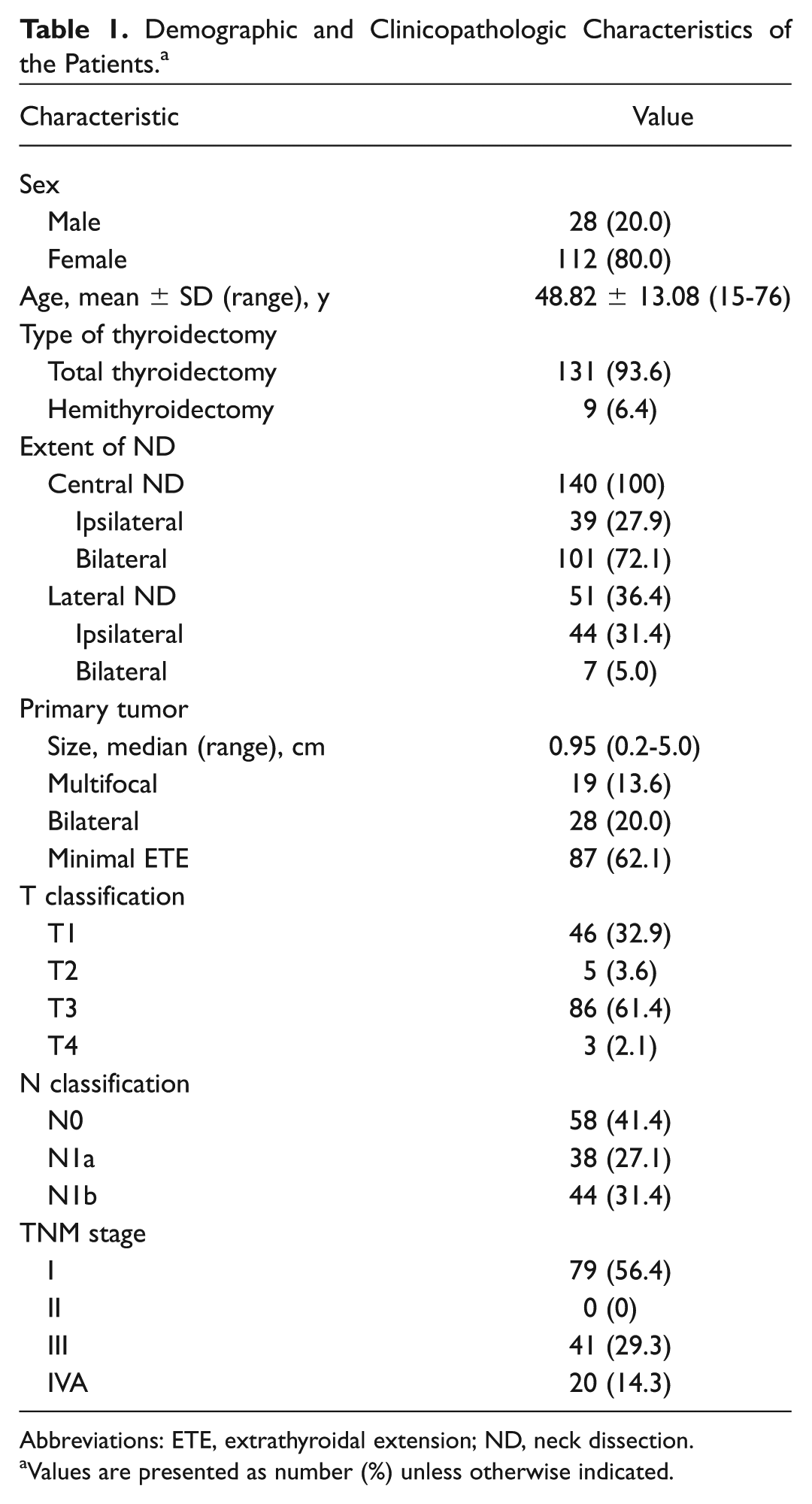
Abbreviations: ETE, extrathyroidal extension; ND, neck dissection.
Values are presented as number (%) unless otherwise indicated.
Cervical LN Metastasis Rate
Pathologic examination showed that of the total of 409 neck LN levels, 186 (45.5%) contained metastatic LNs. In the central compartment (level VI), 92 of 227 LN levels were positive for metastatic LNs; in the lateral compartment, 94 of 182 LN levels were positive ( Table 2 ).
Pathologic Results for Cervical Lymph Node Metastasis According to Lymph Node (LN) Level.
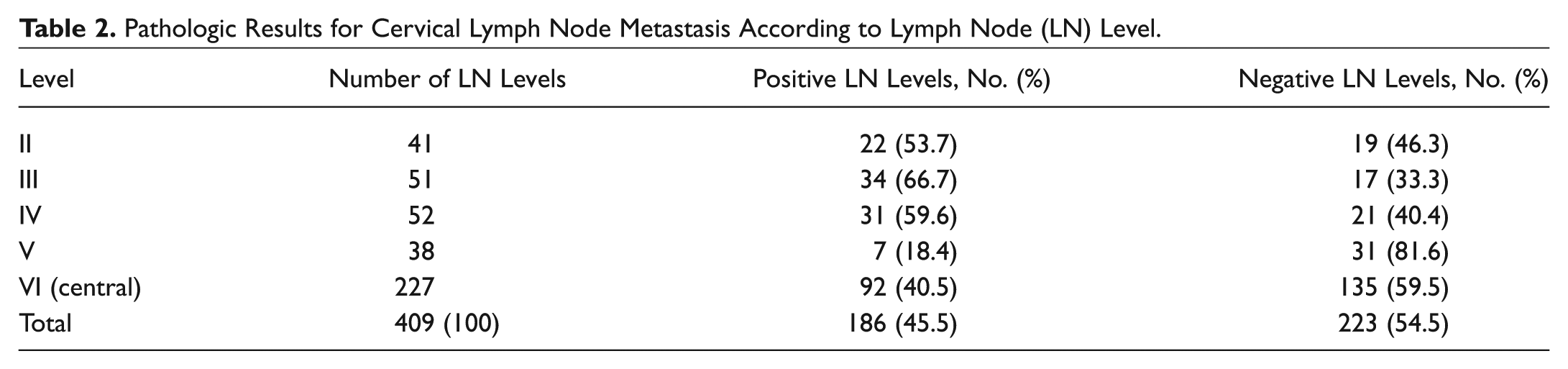

Diagnostic Efficacies of 18F-FDG PET/CT, US, and CT
The diagnostic power of 18F-FDG PET/CT was highest at SUVmax 1.125 in the total and central compartments and 1.055 in the lateral compartments, based on the ROC curve analysis ( Table 3 ). We compared the results of US, CT, and 18F-FDG PET/CT using these cutoff values of SUVmax. Figure 1 shows the diagnostic values for each imaging modality in the total, central, and lateral compartments. In the total and central compartments, the specificity of 18F-FDG PET/CT was significantly lower than those of US and CT (P < .001, P < .001), as was the diagnostic accuracy of 18F-FDG PET/CT (P < .001, P < .001). In the lateral compartment, the specificity of 18F-FDG PET/CT was significantly lower than that of CT (P < .001).
Cutoff Values of SUVmax for Metastatic Lymph Nodes Based on Receiver Operating Characteristic Curves and the Sensitivity, Specificity, and Diagnostic Accuracy of 18F-fluorodeoxyglucose Positron Emission Tomography/Computed Tomography.
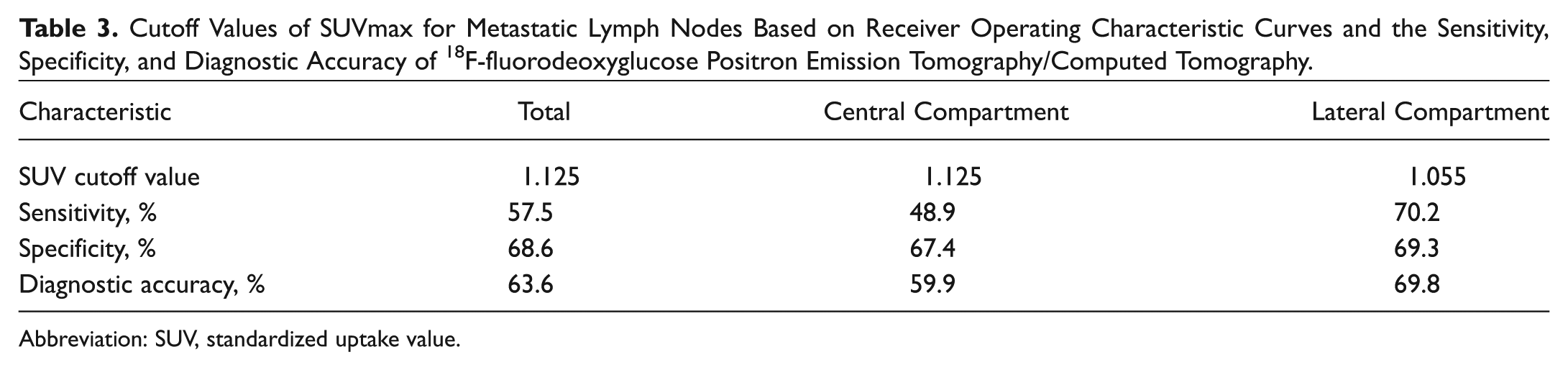
Abbreviation: SUV, standardized uptake value.
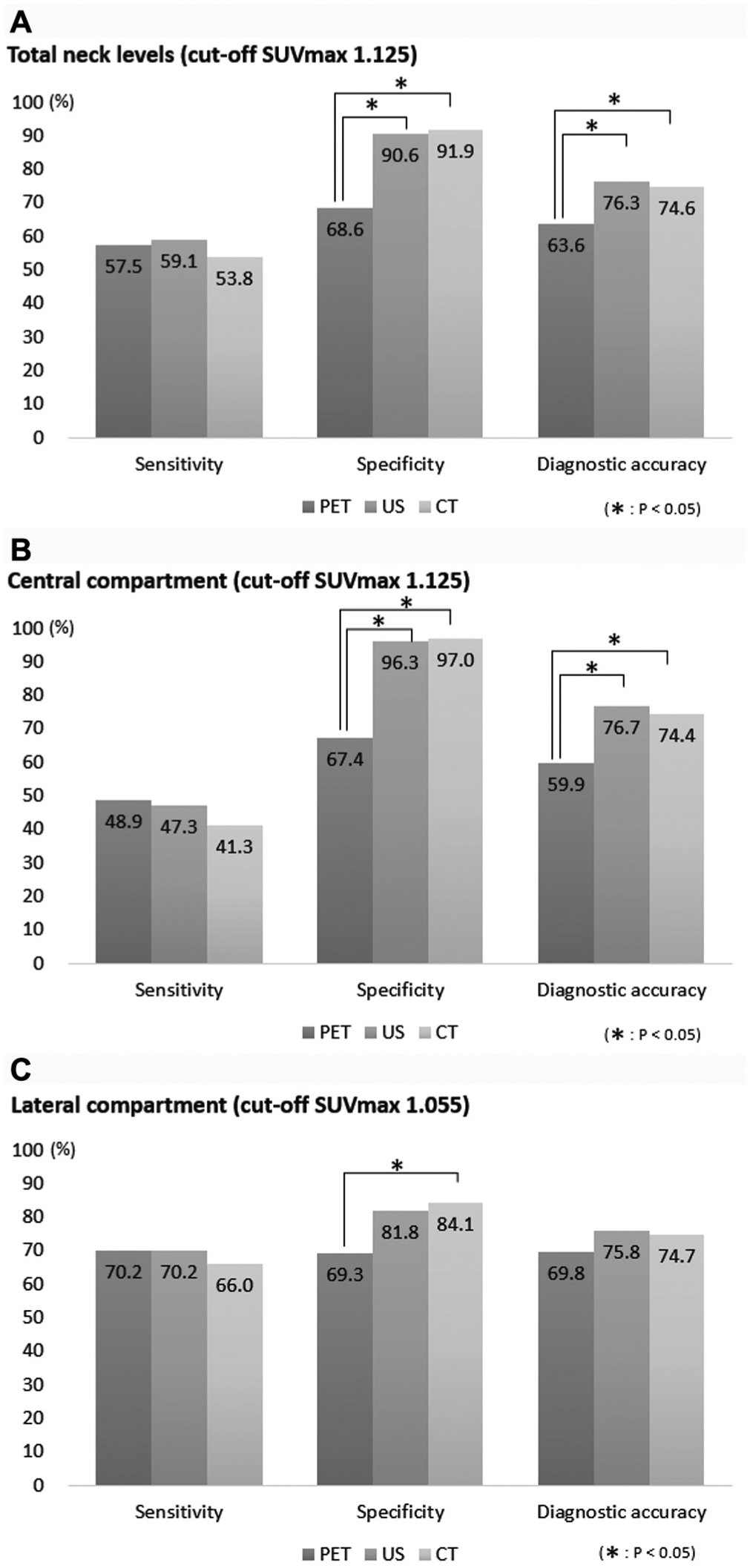
Diagnostic accuracies of ultrasonography (US), computed tomography (CT), and 18F-fluorodeoxyglucose positron emission tomography/computed tomography (PET/CT) in the total compartment (A), the central compartment (B), and the lateral compartment (C). SUVmax, maximum standardized uptake value.
The SUVmax value that reduced false positives to zero (specificity 100%) was 2.585 in the total compartment, 2.27 in the central compartment, and 2.585 in the lateral compartment. Sensitivities were 14%, 8%, and 22.3%, respectively.
Comparison of the Mean Sizes and SUVmax Values of the Central and Lateral LN Compartments
The sizes and SUVmax values of the malignant metastatic LNs of the lateral compartments were significantly larger than those of the central compartment ( Table 4 ). However, the sizes and SUVmax values of benign LNs in the central and lateral compartments were not significantly different ( Table 4 ).
Comparison of the Sizes and SUVmax Values of Malignant and Benign Lymph Nodes in the Central and Lateral Compartments.
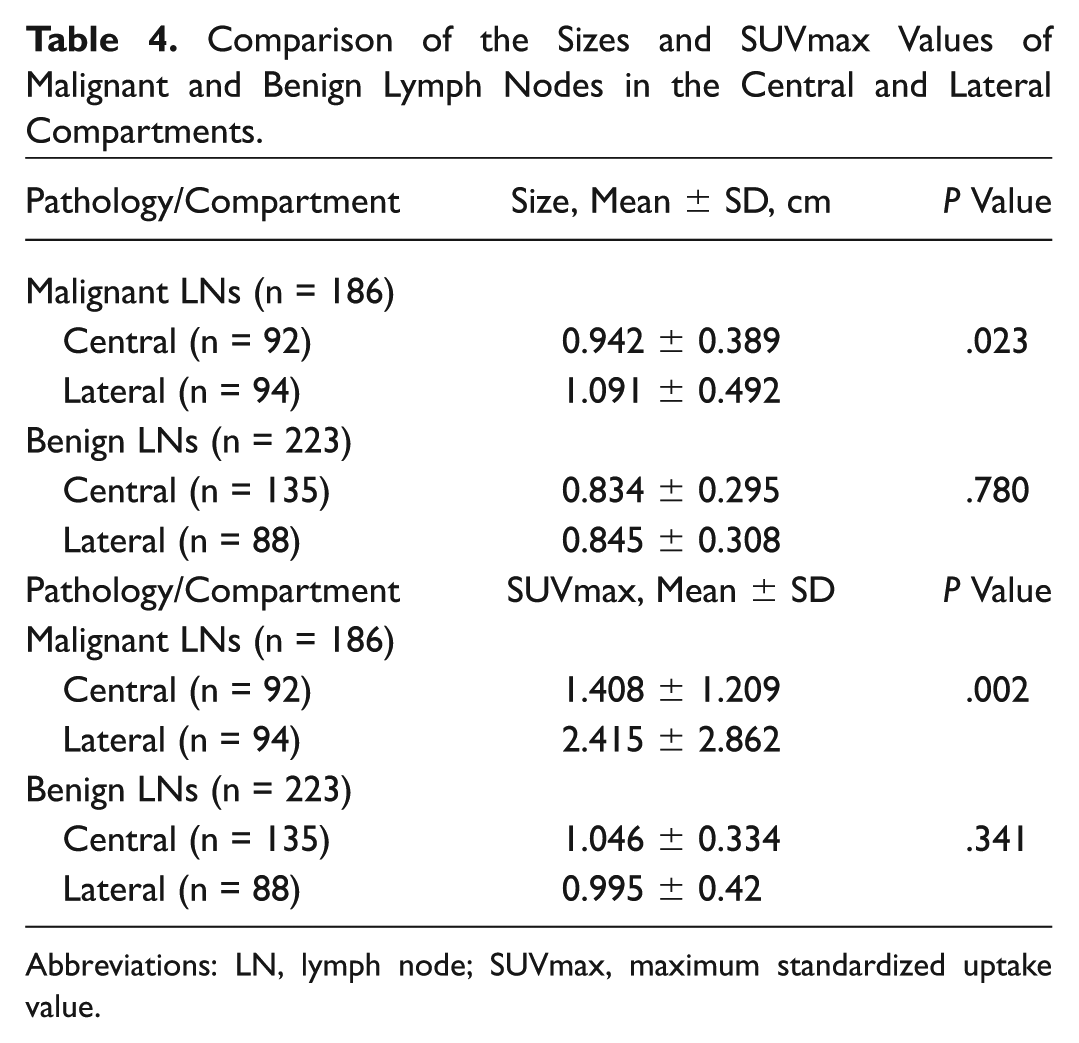
Abbreviations: LN, lymph node; SUVmax, maximum standardized uptake value.
Discussion
Conventional US, CT, and MRI are useful methods for visualizing morphological and anatomical structures in cancer. On the other hand, 18F-FDG PET is able to identify cancers by visualizing changes in the metabolism of cells, so-called functional changes, which can be detected prior to anatomical changes. In addition to 18F-FDG PET, 18F-FDG PET/CT can provide anatomical information based on synthetic images from CT. 16
A few studies have evaluated the ability of 18F-FDG PET/CT to detect cervical LN metastases in patients with PTC. Chong et al 17 compared preoperative LN staging using contrast-enhanced 18F-FDG PET/CT and neck CT at 4 institutions and found that contrast-enhanced 18F-FDG PET/CT was more sensitive and reliable than CT for preoperative LN staging, using a cutoff value of SUVmax of 2.0. Some authors used the SUVmax of the primary tumor (pSUVmax) to predict LN metastasis in patients with PTC. Jung et al 18 reported that pSUVmax >4.6 was associated with central LN metastasis. Byun et al 19 similarly reported that pSUVmax >2.8 was associated with central LN metastasis and that the pSUVmax values of both 18F-FDG PET/CT and US were effective in preoperative prediction of central LN metastasis from papillary thyroid microcarcinomas.
However, other studies have reported that preoperative 18F-FDG PET/CT in patients with PTC is not effective in preoperative regional LN staging. Morita et al 20 reported that US was better for preoperative LN evaluation than 18F-FDG PET/CT and CT, using a subjective visual scale of FDG uptake in 18F-FDG PET/CT. Jeong et al 21 showed that the diagnostic results of US, CT, and 18F-FDG PET/CT did not differ significantly: 18F-FDG PET/CT did not provide any additional benefit for the initial evaluation of LN in patients with PTC. Choi et al 22 also reported that 18F-FDG PET/CT afforded no additional information to US. Both Jeong et al and Choi et al used SUVmax 2.0 as the cutoff value of LN metastasis in 18F-FDG PET/CT.
The previous studies that evaluated the effectiveness of 18F-FDG PET/CT for detecting cervical LN metastasis in PTC have major limitations. Some of the studies used the SUVmax of the primary thyroid tumor instead of the SUVmax of LNs, and most of the studies used arbitrary values of SUVmax, such as 2.0, or a subjective visual scale for LNs instead of the optimal cutoff value of SUVmax. As far as we are aware, there are no studies using the optimal SUVmax cutoff value of LN itself as an indicator of LN metastasis. In the present study, we used the optimal cutoff value of SUVmax of LNs derived from an ROC curve to evaluate cervical LN metastasis. That is an important advantage of the present study. Actually, the optimal cutoff value of SUVmax may vary from machine to machine in different institutions. Therefore, the appropriate cutoff value of SUVmax in a given institution should be determined.
In the current study, sensitivity did not differ significantly between US, CT, and 18F-FDG PET/CT, and the specificity and diagnostic accuracy of 18F-FDG PET/CT were lower than those of US and CT in the central and lateral compartments, even though we applied the optimal SUVmax of LNs. This implies that 18F-FDG PET/CT does not provide any additional benefit over conventional US or CT. Therefore, 18F-FDG PET/CT should not be considered the primary test for cervical LN metastasis in PTC; moreover, 18F-FDG PET/CT is costly. However, the high cutoff values of SUVmax that gave 100% specificity (such as 2.585 in the total compartment, 2.27 in the central compartment, and 2.585 in the lateral compartment) might be helpful to identify PTC if some patients had higher SUVmax values than these.
The overall sensitivity of all 3 methodologies tended to be lower for the central LN compartment than for the lateral LN compartments in this study. This is similar to the results of previous studies.20,23,24 This could be due to the anatomical complexity of the thoracic inlet, which makes it more difficult to evaluate LN metastasis in the central compartment than in the lateral compartments.20,23
Actually identifying metastatic LNs with 18F-FDG PET/CT is difficult because many nonspecific, enlarged LNs show increased uptake. Also, a cutoff SUVmax value of LNs of <1.5 is actually similar to that of the blood, so it is not easy to evaluate the uptake signals in 18F-FDG PET/CT images. Well-differentiated thyroid carcinomas are also associated with reduced glucose metabolism, which results in reduced SUV uptake. On the other hand, dedifferentiated thyroid carcinomas that do not accumulate 131I show elevated glucose utilization, and metastatic tumors in the LNs tend to grow slowly and have a lower glucose metabolism than primary tumors.25,26 Also, the partial volume effect can influence the results of 18F-FDG PET/CT. This effect is defined as the loss in apparent activity due to the limited spatial resolution of PET scanners (typically 5-7 mm full-width at half-maximum). 27 The smaller the tumor, the greater the underestimate of SUVmax. 28 Correction for the partial volume effect may improve the accuracy of SUVmax for LN metastasis. 27 To test this idea, we also analyzed and compared the sensitivity, specificity, and diagnostic accuracy of 18F-FDG PET/CT with those of US and CT in LNs that exceeded 6 mm to avoid the partial volume effect, but the results were similar to the results for the total cases. In the total and central compartments, the specificity and diagnostic accuracy of 18F-FDG PET/CT were significantly lower than those of US (P < .001 in both) and CT (P < .001 and P = .003, respectively). In the lateral compartment, there were no significant differences between the 3 methodologies, except the specificity between 18F-FDG PET/CT and CT.
This study has several limitations. First, there was inevitable selection bias because it was a retrospective nonrandomized study. Second, we analyzed cervical LN metastasis on a per level basis rather than in individual LNs. Therefore, we do not know whether the metastatic LNs at each level of the pathologic results exactly matched the positive LNs in the imaging studies. Third, the optimal cutoff value of SUVmax used for differential diagnosis between malignant and benign LNs was too low. Therefore, it was difficult to interpret the signals.
Conclusion
18F-FDG PET/CT is less effective as the primary preoperative diagnostic tool for detecting cervical LN metastasis in PTC than US and CT.
Author Contributions
Disclosures
Footnotes
No sponsorships or competing interests have been disclosed for this article.
