Abstract
Background:
The optimal osteotomy technique for severe hallux valgus deformity using minimally invasive surgery remains unknown. This study aimed to explore the clinical and radiographic outcomes between chevron and transverse osteotomies in patients with severe hallux valgus deformity
Methods:
A retrospective cohort study was conducted including 131 feet (109 patients) with complete radiographic follow-up who underwent hallux valgus correction using either percutaneous chevron and Akin osteotomy (PECA) (n = 43 patients, 50 feet) or metaphyseal extra-articular transverse and Akin osteotomy (META) (n = 66 patients, 81 feet) techniques. Radiographic parameters including hallux valgus angle (HVA) and intermetatarsal angle (IMA) were measured at baseline, 6 weeks, and final follow-up. Patient-reported outcome measures were assessed using the Manchester-Oxford Foot Questionnaire (MOXFQ), visual analog scale (VAS) for pain, and EuroQol 5 dimension–5 level questionnaire. Recurrence was defined as a final HVA exceeding 20°. Complication rates and passive correctability were also analyzed.
Results:
Baseline characteristics were similar between groups, except for significantly higher initial IMA in the PECA group (17.8° vs 15.8°, P = .001). Both techniques achieved significant deformity correction. At final follow-up, the PECA group demonstrated a significantly lower HVA compared to the META group (11.7° vs 14.5°, P = .045), whereas final IMA measurements were similar (5.2° vs 4.9°, P = .642). Recurrence rates were significantly lower in the PECA group (10.0% [95% CI: 4.3%–21.4%] vs 27.2% [95% CI: 18.7%–37.7%], P = .025). Pre-operative passive correctability was significantly higher in the PECA group (68.0% vs 46.9%, P = .020), particularly amongst recurrent cases (80.0% vs 27.3%, P = .047). No significant differences were observed in MOXFQ scores between groups, although VAS pain favored the META group (6.2 [SD 12.3] vs 11.9 [SD 17.5], P = .046). Complication rates were comparable (PECA: 13.2% vs META: 8.6%, P = .40). Complication rates were comparable (PECA: 13.2% vs META: 8.6%, P = .40), with different complication profiles noted between techniques.
Conclusion:
Both PECA and META techniques provide effective correction of hallux valgus deformity. The higher recurrence rate observed in the META group was associated with a significantly lower rate of pre-operative passive correctability in that cohort.
Level of Evidence:
Level III, retrospective comparative study.
Keywords
Introduction
Background/rationale
Minimally invasive surgery (MIS) for hallux valgus has gained widespread acceptance across the spectrum of deformity severity, from mild to severe cases.1 -7 The evolution from first-generation techniques without fixation to third and fourth-generation approaches with rigid screw fixation and multi-planar deformity correction has demonstrated equivalent clinical and radiographic outcomes to traditional open procedures whilst offering potential advantages of reduced soft tissue disruption, faster recovery times, reduced recurrence rates and smaller incisions.7 -14
Third-generation percutaneous chevron and Akin osteotomies (PECA) have been extensively studied and show excellent outcomes for mild to moderate deformity, with growing evidence supporting their use in severe cases.3 -5,15 Fourth-generation techniques using a metaphyseal extra-articular transverse and Akin osteotomy (META) may theoretically offer enhanced 3-dimensional correction capabilities and reduced risk of lateral wall fractures associated with chevron osteotomies (Figures 1 and 2).7,9,16
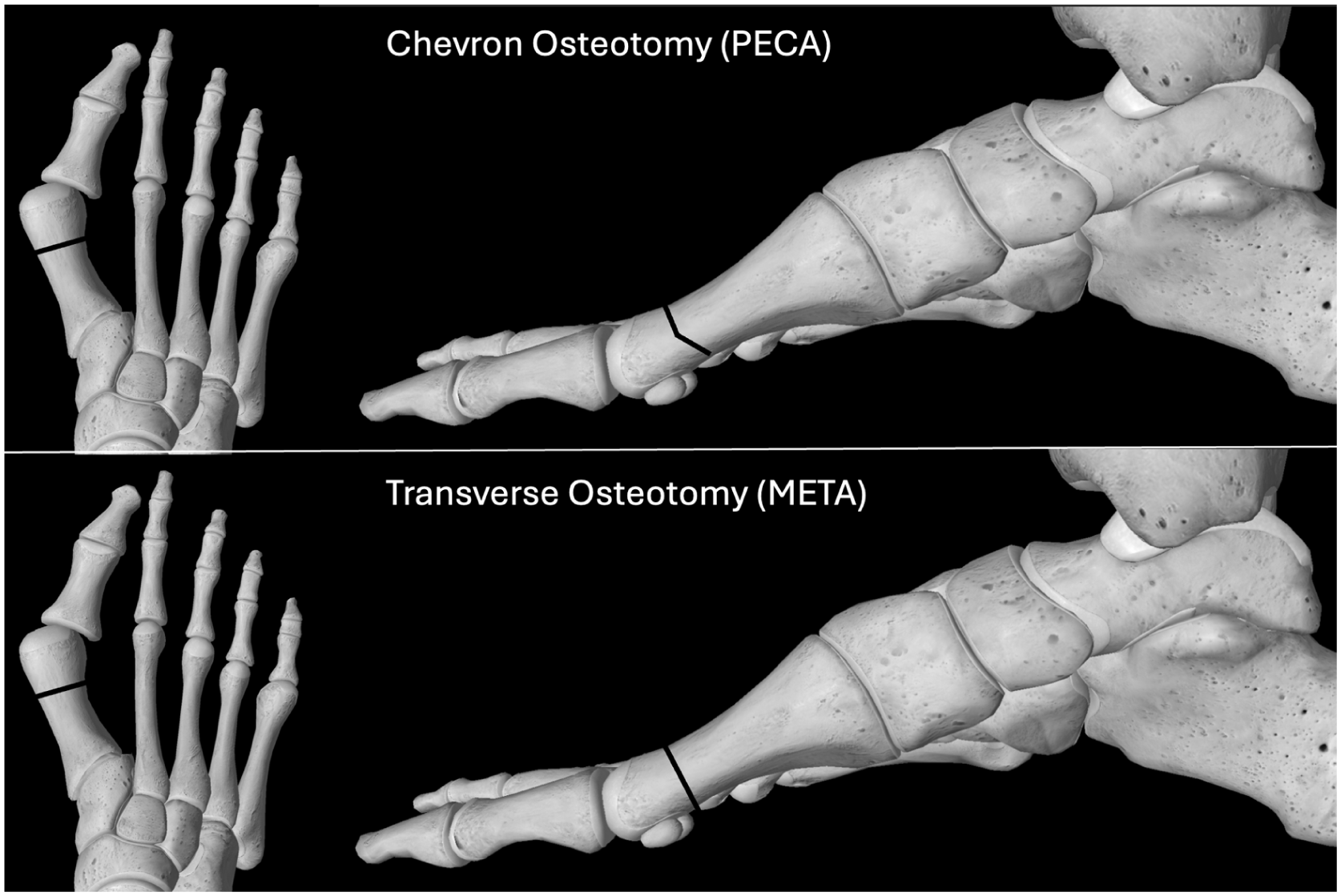
Schematic illustrations demonstrating chevron (left) and transverse (right) metatarsal osteotomy techniques.

Preoperative and postoperative weightbearing radiographs comparing chevron (PECA) (top) and transverse (META) (bottom) techniques in severe hallux valgus deformity. META, metaphyseal extra-articular transverse and Akin osteotomy; PECA, percutaneous chevron and Akin osteotomy.
Despite advances in understanding screw configuration and fixation techniques, comparative evidence between transverse and chevron osteotomies remains extremely limited.17 -19 The theoretical advantages of transverse osteotomies include improved biomechanical stability through the ability to achieve complete metatarsal head displacement and potentially reduced fracture risk at the lateral cortex. 20 However, only 1 study by Loder et al 17 has directly compared these techniques in a clinical setting, finding no significant difference in radiographic deformity correction between third-generation chevron and fourth-generation transverse osteotomies.
Severe hallux valgus deformity presents particular challenges, with historically higher rates of recurrence, incomplete correction, and patient dissatisfaction compared to mild and moderate cases.21,22 Recurrence of hallux valgus is a significant concern as it often necessitates revision surgery, leads to poor patient satisfaction, and may result in ongoing pain and functional limitation. 23 Understanding factors that influence recurrence risk is crucial for optimising patient selection, surgical technique, and postoperative management.23 -25 One under-explored factor that may play a role is the degree of coronal plane stiffness and passive deformity correction.
Objectives
The primary aim was to compare clinical and radiologic outcomes and recurrence rates between third-generation chevron and fourth-generation transverse osteotomy techniques in severe hallux valgus. Our secondary aim was to investigate whether pre-operative passive deformity correctability influences recurrence risk. We hypothesised that both techniques would achieve comparable deformity correction and patient-reported outcomes, with recurrence rates primarily influenced by pre-operative deformity characteristics rather than osteotomy type.
Methods
Study Design and Setting
This study is a retrospective cohort study with 2 discrete cohorts who underwent primary percutaneous chevron-Akin osteotomy (PECA) for severe deformity or metaphyseal extra-articular transverse and Akin osteotomy (META). An experienced MIS surgeon (P.L.) in Sydney, Australia, completed the surgeries from 2012 to 2019 for the PECA group and from 2017 to 2023 for the META group with previously described techniques for third- and fourth-generation MIS hallux valgus surgery.4,9,26 Percutaneous lateral soft tissue release was performed when residual MTPJ incongruity persisted after completion of M1 and Akin osteotomies, assessed intraoperatively by fluoroscopy. There was a minimum of 2-year follow-up for the cohorts. This study was reported in line with STROBE guidelines for observational studies. 27
Participants
Patients were included in this study if they were aged 18 years and older with severe hallux valgus angles (HVAs > 40° and/or intermetatarsal angle [IMA] > 20°). 3 If patients underwent concomitant forefoot procedures such as lesser toe corrections, they were also included. We excluded revision surgery or patients with advanced symptomatic first MTPJ osteoarthritic changes. We only included patients who had a complete set of radiographs.
Variables
The primary outcome measure was the Manchester Oxford Foot Questionnaire (MOXFQ), which is validated for hallux valgus surgery. Secondary outcome measures included radiographic angle measurements including hallux valgus angle and intermetatarsal angle, 28 recurrence (defined as HVA >20°), 23 scores on the pain visual analogue scale (VAS-Pain) and the EuroQol 5 dimension–5 level questionnaire, passive deformity correctability, and complications.
Data Sources and Measurement
A dedicated research nurse recorded patient-reported outcome measures stored on an electronic database (REDCap). The primary outcome measure was the MOXFQ, a validated outcome measure. 29 Pre-operative PROMS for the PECA cohort were not available as they were not routinely collected at this point in time. The secondary measures were other validated PROMs including the EQ-5D-5L and VAS Pain. Radiographic measurements were in accordance with AOFAS guidelines including HVA and IMA preoperatively, at 6 weeks, and final follow-up. 28 Radiographs were assessed by a Foot and Ankle Fellow. Passive deformity correctability was performed by the senior author and data extracted from pre-operative outpatient assessment records. Complications were recorded and classified according to a modified Clavien-Dindo classification. 30
Passive Deformity Correctability
Passive deformity correctability was defined as “the ability to passively correct the medial deviation of the first metatarsal to neutral and correct the hallux valgus angle to zero degrees in an awake patient” as shown in Figure 3. This was performed in a standardized fashion for each patient. The knees are placed at 90° with the foot flat on the floor. One hand is used to stabilise the first MTPJ and 1 index finger is used to then passively correct the deformity purely in the coronal plane. The outcome is binary: either fully correctible whereby clinical assessment of the HVA was 0° or not passively correctible whereby clinical assessment of the HVA demonstrated residual deformity of any amount (even if partially correctible to “normal” limits; eg, a deformity corrected to 7° may be considered “normal” but for the purposes of this test would be considered not passively correctible).

Clinical demonstration of passive incomplete deformity correction manoeuvre assessed preoperatively, showing the hallux in natural position (A) and with gentle passive manipulation corrected to neutral (B). Images C and D show a similar manoeuvre in a severe deformity case that is not passively correctable to neutral.
Bias
A prospectively maintained database reduced the risk of selection bias and recall bias by the patients. The primary operating surgeon was not involved in the data analysis and was blinded to the clinical outcomes recorded.
Statistical Analysis
Statistical analyses were performed using Python. Continuous variables were reported as mean ± SD with 95% CIs, whereas categorical variables were presented as frequencies and percentages. The Shapiro-Wilk test was used to assess the normality of continuous data distribution. For normally distributed variables, between-group comparisons were conducted using independent samples t tests. For non-normally distributed variables, the Mann-Whitney U test was used. Effect sizes for continuous variables were calculated using Cohen d, with values of 0.2, 0.5, and 0.8 interpreted as small, medium, and large effects, respectively. Categorical variables were compared using χ2 tests, or Fisher exact test substituted when expected sample sizes were small. A P value of .05 was considered significant.
Ethical Approval and Funding
This study was approved by the local ethical review board (2025/ETH/0052). There was no funding to report for this study. Disclosure forms for all authors are available online.
Results
Study Population
After excluding ineligible patients, a total of 109 patients (43 in the PECA group and 66 in the META group) comprising 131 feet (50 PECA feet and 81 META feet) were included in this study (Table 1, Figure 4). The cohort was predominantly female patients in both groups (90.7% in PECA and 95.5% in META). Bilateral procedures were performed in 8 PECA patients (18.6%) and 15 META patients (22.7%). Both groups demonstrated similar age distributions (62.2 ± 10.9 years in PECA vs 62.5 ± 10.3 years in META, P = .860). All feet included in the analysis had complete radiographic follow-up (pre-operative, 6-week, and final follow-up) at all 3 time points. Radiographic follow-up time was significantly longer in the PECA group compared with the META group (3.2 ± 1.1 years vs 2.3 ± 1.1 years, P = .011).
Patient Demographics.

Abbreviations: META, metaphyseal extra-articular transverse and Akin osteotomy; PECA, percutaneous chevron and Akin osteotomy.

Flowchart demonstrating patient selection and final cohort allocation.
Radiographic Outcomes
Radiographic assessment found significant differences between the 2 surgical techniques at both baseline and final follow-up (P < .05) (Table 2, Figure 5). At baseline, the PECA group demonstrated similar HVA (44.1° ± 4.3° vs 45.1° ± 4.1°; P = .076) but significantly higher IMA (17.8° ± 3.5° vs 15.8° ± 3.3°; P = .001) compared to the META group. At the 6-week follow-up, both groups showed significant improvements in alignment. Final radiographic assessment demonstrated the mean HVA was corrected to within normal parameters in both groups; however, there was a statistically significant difference in HVA between groups, with the PECA group having a decreased HVA (11.7° ± 6.8°) compared with the META group (14.5° ± 8.6°; P = .045). Final IMA measurements were similar between groups (5.2° ± 3.3° in PECA vs 4.9° ± 2.9° in META; P = .642). The overall correction achieved for HVA (32.4° ± 7.6° in PECA vs 30.6° ± 8.8° in META, P = .229) demonstrated substantial deformity correction with both techniques, whereas IMA correction was significantly greater in the PECA group (12.6° ± 3.7° vs 10.8° ± 3.6°, P = .009).
Radiographic Parameters Following Percutaneous Hallux Valgus Surgery for Severe Deformity.

Abbreviations: HVA, hallux valgus angle; IMA, intermetatarsal angle; META, metaphyseal extra-articular transverse and Akin osteotomy; PECA, percutaneous chevron and Akin osteotomy.

Comparison of radiographic parameters (HVA, IMA) and patient-reported outcome measures (MOXFQ, VAS) between PECA and META groups at preoperative, and final follow-up. Error bars represent 95% CIs. HVA, hallux valgus angle; IMA, intermetatarsal angle; META, metaphyseal extra-articular transverse and Akin osteotomy; MOXFQ, Manchester-Oxford Foot Questionnaire; PECA, percutaneous chevron and Akin osteotomy; VAS, visual analogue scale.
Recurrence vs Incomplete Deformity Correction
At 6 weeks postoperatively, the HVA >20° was present in 4.0% of PECA feet (n = 2/50) and 11.1% of META feet (n = 9/81), suggesting incomplete deformity correction. By final follow-up, this increased to 10.0% (n = 5/50) and 27.2% (n = 22/81), respectively, which was significantly different between the 2 groups (P = .025). Both groups demonstrated statistically but not clinically significant deterioration in HVA between 6 weeks and final follow-up (PECA: mean increase 2.2°, P = .004; META: mean increase 2.1°, P < .001). In recurrent cases, baseline radiographic parameters were comparable between groups, with initial HVA of 45.9° ± 6.8° in PECA and 47.0° ± 4.0° in META (P = .74), and initial IMA of 13.8° ± 3.6° in PECA vs 16.0° ± 2.9° in META (P = .26). The final radiographic deformity was also similar in both groups, with final HVA measurements of 24.5° ± 3.7° in PECA and 25.2° ± 3.8° in META (P = .78), and final IMA of 7.0° ± 3.7° and 7.6° ± 2.8°, respectively (P = .98). Despite radiographic recurrence, patient-reported outcomes remained generally favourable (mean MOXFQ Index: PECA: 10.6 ± 10.1, META: 15.0 ± 17.7), with no significant differences between groups in any of the MOXFQ domains or VAS pain scores (P > .05).
There were significantly higher rates of pre-operative passive deformity correctability in the PECA group compared to the META group (68.0% vs 46.9%, P = .020). This difference was even more pronounced when examining only the subset of patients with recurrent deformity (final HVA > 20°), where 80.0% of PECA cases were passively correctable pre-operatively compared to 27.3% of META cases (P = .047). The rate of lateral release performed during the procedure was similar between groups (PECA: 94.3% vs META: 97.5%, P = .384), indicating that differences in outcomes were not attributable to variations in this aspect of the surgical technique. Pre-operative failure to passively correct the deformity did not affect decision making for a lateral release, which was only performed when there was residual joint incongruity of MTPJ1 after M1 osteotomy and Akin osteotomy.
Patient-Reported Outcomes
Post-operative clinical outcomes were evaluated using validated PROMs including MOXFQ, VAS for pain, and EuroQol 5 dimension–5 level questionnaire (Table 3, Figure 6). The MOXFQ domains showed no significant differences between groups. VAS pain scores were significantly lower in the META group (6.2 ± 12.3) compared with the PECA group (11.9 ± 17.5, P = .046). Quality of life measures demonstrated no significant differences between groups.
Clinical Parameters Following Percutaneous Hallux Valgus Surgery for Severe Deformity.

Abbreviations: META, metaphyseal extra-articular transverse and Akin osteotomy; MOXFQ, Manchester-Oxford Foot Questionnaire; PECA, percutaneous chevron and Akin osteotomy; PROM, patient-reported outcome measure; VAS, visual analogue scale.
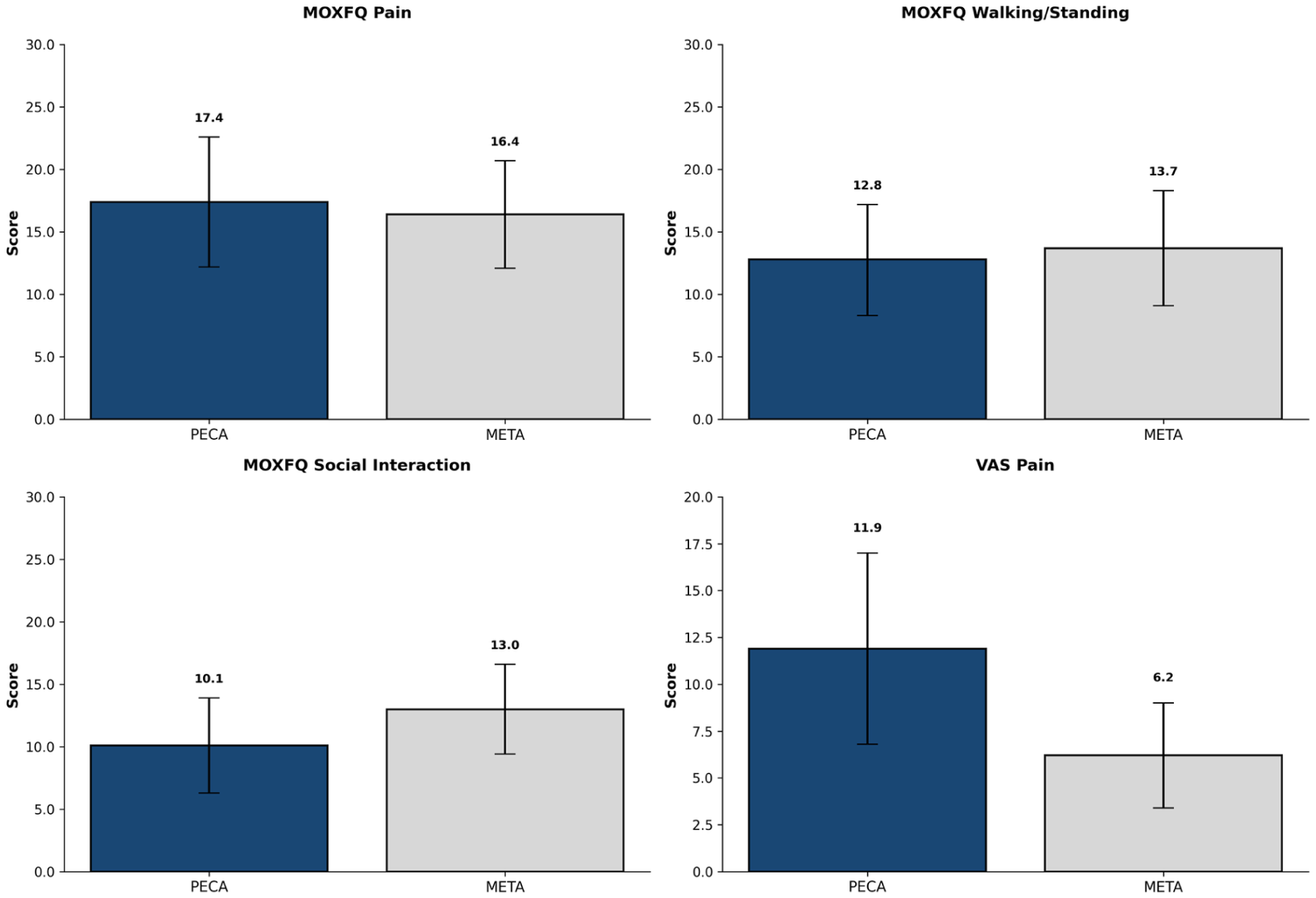
Comparison of patient-reported outcome measures between PECA and META groups at final follow-up. Pre-operative PROM data were only available for the META group. Error bars represent 95% CIs. META, metaphyseal extra-articular transverse and Akin osteotomy; PECA, percutaneous chevron and Akin osteotomy; PROM, patient-reported outcome measure
Pre-operative passive correctability
When patients were stratified by pre-operative passive correctability (Table 4), several differences emerged in clinical and radiographic outcomes. The passively correctable group (n = 72) demonstrated a significantly lower baseline hallux valgus angle compared with the non-correctable group (n = 59) (43.7° vs 46.0°, P = .006). At 6 weeks post-operatively, the passively correctable group achieved superior correction of the intermetatarsal angle (5.0° vs 6.6°, P < .001) and hallux valgus angle (10.1° vs 12.8°, P = .038). At final follow-up, the passively correctable group maintained significantly better hallux valgus angle correction (11.9° vs 15.4°, P = .013). Notably, the recurrence rate, defined as final hallux valgus angle greater than 20°, was significantly lower in the passively correctable group (13.9% vs 28.8%, P = .050). Despite these radiographic differences, patient-reported outcome measures, including all MOXFQ domains and VAS pain scores, showed no statistically significant differences between the 2 groups at final follow-up (all P > .05).
Clinical and Radiographic Parameters Following Percutaneous Hallux Valgus Surgery for Severe Deformity Stratified by Pre-operative Passive Correctability Status. a
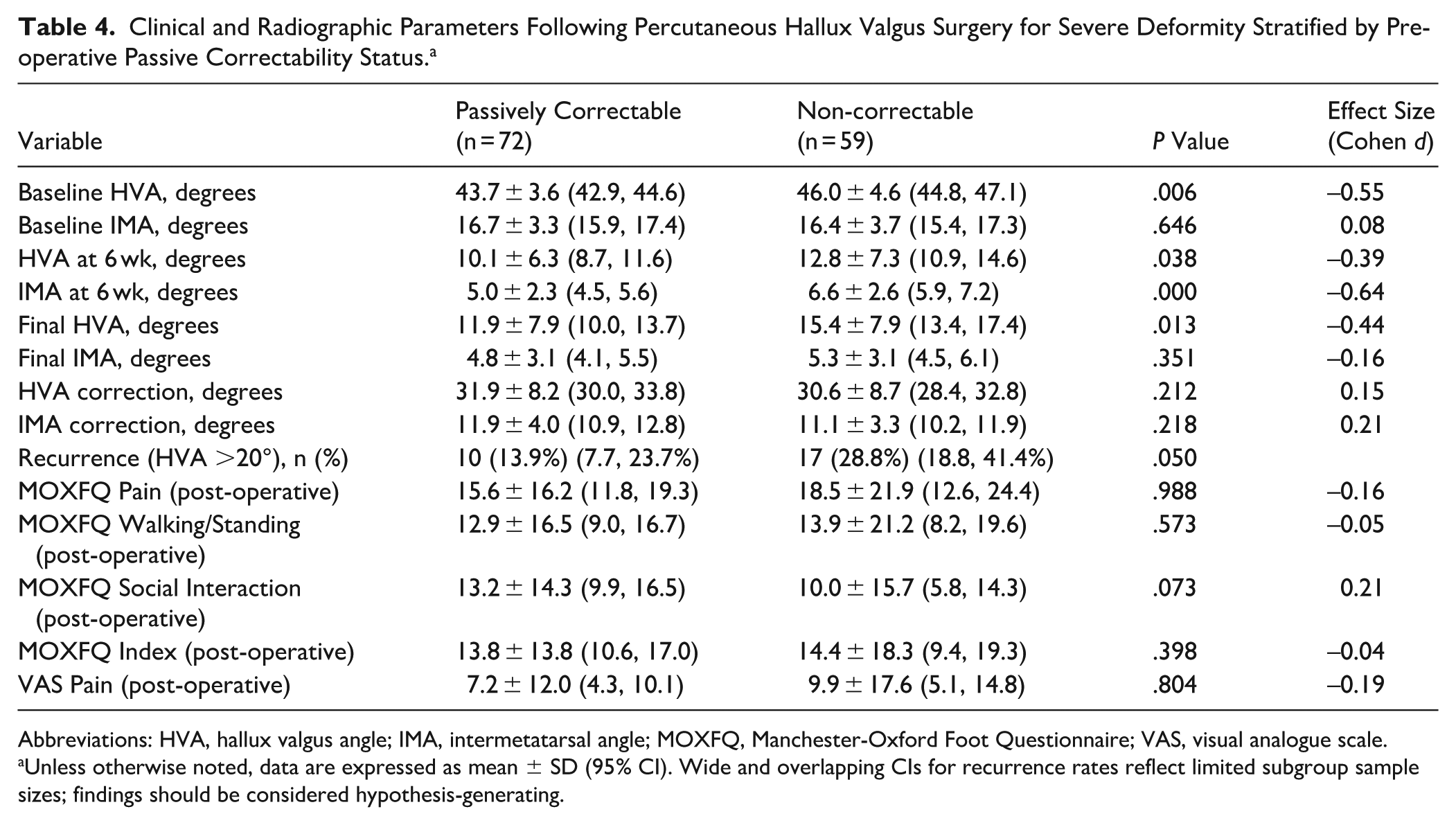
Abbreviations: HVA, hallux valgus angle; IMA, intermetatarsal angle; MOXFQ, Manchester-Oxford Foot Questionnaire; VAS, visual analogue scale.
Unless otherwise noted, data are expressed as mean ± SD (95% CI). Wide and overlapping CIs for recurrence rates reflect limited subgroup sample sizes; findings should be considered hypothesis-generating.
Complications
There was no significant difference in complication rate between osteotomy technique (META: n = 9/81, 11.1%; PECA: n = 7/50, 14.0%), Fisher exact test, P = .784; odds ratio 0.77, 95% CI 0.27 to 2.21. However, the severity profile differed markedly between cohorts. In the META data set, most complications were minor wound infections (grade 1A: n = 6) and prominent residual bone (grade 2A: n = 1), with only 2 requiring surgical intervention (grade 3A: hallux varus correction and P1/P2 osteotomy with screw removal). Conversely, all PECA complications were severe, classified as grade 3A (screw removals and corrective osteotomies, n = 4) or grade 3B (open medial capsulorrhaphy for symptomatic recurrence, n = 3). Although overall complication rates were similar, the PECA cohort demonstrated exclusively surgical complications (100% grade 3) compared with predominantly minor complications in the META cohort (67% grade 1).
Discussion
This study compared clinical and radiographic outcomes between third-generation PECA and fourth-generation META techniques for severe hallux valgus deformity. The results demonstrate that both techniques achieve substantial deformity correction in this technically challenging patient population, with comparable patient-reported outcomes but notable differences in recurrence rates that appear to be related to pre-operative passive correctability rather than osteotomy type.
Both surgical techniques achieved substantial angular correction in severe hallux valgus deformity, with mean HVA corrections of 32.4° in the PECA group and 30.6° in the META group, and IMA corrections of 12.6° and 10.8°, respectively. These findings corroborate with existing studies that minimally invasive techniques can reliably address severe deformities, which historically presented considerable challenges with higher rates of incomplete correction and patient dissatisfaction.21,22 The magnitude of correction achieved in both groups compares favourably with published outcomes for severe hallux valgus surgery, supporting the expanding role of minimally invasive approaches across the deformity spectrum. 5
Validated patient-reported outcome measures (MOXFQ, EQ-5D-5L, and VAS pain), showed no significant differences between the 2 techniques with both groups demonstrating favourable outcomes, suggesting that the choice between chevron and transverse osteotomies does not impact clinical foot function. We also noted that the chevron osteotomy group did not show a higher rate of subsidence/loss of correction due to potential screw cut out at the cortical purchase zone. 31
However, the most important finding was the significant difference in radiographic recurrence rates between the 2 groups, with 10.0% in the PECA cohort compared with 27.2% in the META cohort. This difference requires careful interpretation, as several factors beyond osteotomy technique likely contributed to this outcome including the technical complexity of this type of surgery, passive deformity correction, patient demographics and pre-existing osteoarthritis. 22 The META group included patients with more severe deformities at baseline, as evidenced by the higher proportion of cases with initially uncorrectable deformities. Although the mean baseline HVA was similar between groups, the META group demonstrated significantly lower rates of pre-operative passive deformity correction (46.9% vs 68.0%, P = .020), and this difference was particularly pronounced amongst cases that subsequently recurred (27.3% vs 80.0%, P = .047). This finding suggests that passive correctability may be associated with recurrence risk and highlights the importance of pre-operative patient counselling regarding realistic expectations when treating rigid, uncorrectable deformities when identified in clinic prior to surgery. Although there were very high rates of lateral soft tissue release, we did not automatically perform a lateral soft tissue release if uncorrectable deformities were encountered, and future studies should explore if this reduces the risk of recurrence in these severe cases. The high lateral soft tissue release rate (94.3% PECA, 97.5% META) reflects severity of deformities treated and operating surgeon's threshold for ensuring complete MTPJ alignment. In severe hallux valgus, contracted lateral structures frequently prevent optimal joint reduction even after achieving satisfactory angular correction with osteotomies alone. Similar rates between groups (P = .384) indicate this was not responsible for observed recurrence difference. Rather, recurrence may be related to inherent deformity rigidity as assessed pre-operatively, independent of intraoperative soft tissue releases. It is important to contextualise our high lateral soft tissue release rates (94.3% PECA, 97.5% META) against the severity of deformity treated. Our cohort had a mean preoperative HVA of approximately 45°, considerably greater than the moderate deformity series (mean HVA ~30°) against which these figures are often compared. In severe deformity of this magnitude, isolated bony correction with osteotomy is frequently insufficient to restore congruent metatarsophalangeal joint alignment, and these procedures should more accurately be considered as composite bony and soft tissue corrections. The similar release rates between groups (P = .384) confirm this reflects cohort-level deformity severity rather than a systematic difference in surgical approach.
Although this is a comparative study, we do not believe the difference in recurrence rates is directly attributable to the osteotomy technique itself. Both chevron and transverse osteotomies in severe deformity cases require near-complete metatarsal head displacement (100% shift) to achieve adequate correction of 1-2 IMA as shown in Figure 7. Although baseline intermetatarsal angle differed significantly between groups (17.8° in PECA vs 15.8° in META, P = .001), both cohorts met our inclusion criteria for severe hallux valgus deformity (HVA > 40° and/or IMA > 20°), and baseline hallux valgus angle was similar (44.1° vs 45.1°, P = .076). Importantly, the higher baseline IMA in the PECA cohort would theoretically predict greater technical challenge and higher recurrence risk in this group, yet the opposite was observed. Our stratified analysis by passive correctability (Table 4) suggests that this clinical factor, rather than baseline angular measurements alone, may be associated recurrence. Patients with passively correctable deformities demonstrated significantly lower recurrence rates (13.9% vs 28.8%, P = .050) regardless of their baseline angular measurements. This suggests that the observed recurrence difference between techniques is better explained by differences in pre-operative deformity rigidity, which likely reflects the temporal evolution in surgical indications towards progressively more complex cases as experience increased, rather than inherent superiority of one osteotomy configuration over another.

Pre-operative, 6-week, and final radiographs illustrating the principle of 100% metatarsal head displacement required for optimal correction in both chevron (top) and transverse (bottom) osteotomy techniques.
The temporal evolution in practice between the PECA (2012-2019) and META (2017-2023) cohorts likely reflects an expansion of surgical indications with increasing surgeon experience and confidence in treating progressively more challenging cases. Improved technical proficiency likely contributed to different complication profiles, with META showing predominantly minor complications (67% grade 1) vs exclusively surgical complications in PECA (100% grade 3). Paradoxically, increased experience also enabled treatment of progressively more challenging deformities, evidenced by significantly lower passive correctability rates in META group (46.9% vs 68.0%, P = .020). The META group may therefore represent a cohort with more complex pathoanatomy beyond what is captured by angular measurements alone, including greater soft tissue contracture and potentially more advanced articular degenerative changes not meeting exclusion criteria. This selection effect, combined with the significantly lower rates of passive correctability, provides a more plausible explanation for the observed recurrence differences than osteotomy geometry. In this retrospective study, passive correctability assessment did not influence surgical decision making. However, our findings suggest patients with rigid deformities may benefit from enhanced counselling regarding recurrence risk or consideration of alternative procedures such as arthrodesis. Future prospective studies should investigate whether incorporating passive correctability into treatment algorithms improves outcomes
Importantly, despite the higher radiographic recurrence rate in the META group, patient-reported outcomes remained favourable and statistically similar between groups. This dissociation between radiographic appearance and patient-reported outcomes has been previously reported in hallux valgus surgery and underscores the importance of considering patient satisfaction alongside objective measures when evaluating surgical success.3,5,11
Limitations
This study has several limitations that should be acknowledged. The retrospective design inherently limits the strength of causal inferences that can be drawn. Pre-operative patient-reported outcome measures were not collected for the PECA group although the similarity in demographic characteristics and surgical indications between cohorts suggests that baseline symptoms and functional limitations may well be comparable. The modest sample sizes, particularly when examining subgroups such as recurrent cases, limit statistical power for detecting smaller between-group differences. Although we employed a standardized definition of passive correctability, the assessment was binary and operator-dependent. In clinical practice, deformity stiffness exists on a spectrum. Future studies should employ a validated graded assessment system to better characterize this relationship.
The non-concurrent nature of the two cohorts introduces potential confounding from temporal changes in surgical technique, patient selection, and surgeon experience. The META cohort represents a later period in the evolution of minimally invasive hallux valgus surgery, during which time there was both increased technical refinement and a tendency towards treating more challenging deformities. This temporal confounding makes it difficult to completely isolate the effect of osteotomy type from other evolving factors in surgical practice. Additionally, the significantly longer radiographic follow-up in the PECA group (3.3 years vs 2.3 years) may influence recurrence detection, although the majority of recurrences typically manifest within the first 18-24 months post-operatively. 21 A further limitation relates to the assessment of passive correctability. Although a standardised binary definition was employed, the assessment was performed by a single surgeon across cohorts separated by several years. Without a validated quantitative instrument, the possibility of intra-observer inconsistency over time cannot be excluded. The observed reduction in passive correctability rates between the PECA (68.0%) and META (46.9%) cohorts may therefore partly reflect measurement drift rather than a true change in patient pathology, and this should be considered when interpreting these findings
This study found that pre-operative passive deformity correctability appears to be a more important determinant of recurrence risk than minimally invasive osteotomy technique in severe hallux valgus. Patients presenting with rigid, non-correctable deformities represent a distinct subset with inherently higher recurrence risk, regardless of the specific osteotomy employed. This observation has important implications for patient counselling and surgical decision making. Surgeons should carefully assess passive correctability during pre-operative examination and discuss the elevated recurrence risk with patients who demonstrate fixed deformities, particularly when considering alternative treatment strategies such as arthrodesis. The study is limited by its retrospective design and fixed sample size, which may have been underpowered to detect smaller differences in patient-reported outcomes. We believe the differences observed between groups reflect expanding surgical indications and the treatment of progressively more challenging deformities rather than inherent superiority of one osteotomy type over another.
Conclusion
Minimally invasive chevron and transverse osteotomies both achieve substantial correction in severe hallux valgus deformity with favourable patient-reported outcomes. Lack of pre-operative passive correctability was associated with increased recurrence risk and surgeons should assess passive correctability during pre-operative evaluation and explicitly counsel patients with rigid, non-correctable deformities. Future prospective comparative studies with standardised patient selection criteria and longer-term follow-up are needed to refine understanding of factors that predict successful correction in severe deformity.
Supplemental Material
sj-pdf-1-fao-10.1177_24730114261434234 – Supplemental material for Increased Risk of Recurrence in Severe Hallux Valgus Associated With Inability to Passively Correct Deformity Prior to Surgery: A Comparative Study of Transverse vs Chevron Osteotomy Minimally Invasive Surgery Techniques
Supplemental material, sj-pdf-1-fao-10.1177_24730114261434234 for Increased Risk of Recurrence in Severe Hallux Valgus Associated With Inability to Passively Correct Deformity Prior to Surgery: A Comparative Study of Transverse vs Chevron Osteotomy Minimally Invasive Surgery Techniques by Thomas L. Lewis, Clare Watt, Lily Fletcher, Evelyn Murphy, Gabriel Ferraz Ferreira, Andreas Toepfer, Choon Chiet Hong and Peter Lam in Foot & Ankle Orthopaedics
Footnotes
ORCID iDs
Ethical Considerations
Ethical approval for this study was obtained from Ramsey Health Care HREC, Sydney, Australia (HREC Reference Number: 2025/ETH/0052).
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Thomas L. Lewis, MBChB, BSc, FRCS(Tr&Orth), MFSTEd, PhD, reports general disclosures of PhD tuition fees supported by MIFAS, and consulting fees from Vilex. Gabriel Ferraz Ferreira, MD, MSc, PhD, reports disclosures relevant to manuscript of consulting fees from Arthrex and Techimport. Andreas Toepfer, MD, PhD, reports disclosures relevant to manuscript of support from Arthrex. Choon Chiet Hong, MBBS, MMed(Ortho), MPH, FRCSEd(Orth), reports general disclosures of honorarium from Arthrex and DKSH-Stryker for educational talks unrelated to this research study. Peter Lam, MBBS, FRACS, reports general disclosures of consulting fees from Enovis/Novastep, Paragon 28; AOFAS Ken Johnson Lecture 2024. Disclosure forms for all authors are available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
