Abstract
Background:
Foot type significantly impacts the development and progression of foot and ankle pathologies by influencing biomechanics and force distribution. However, it is typically assessed qualitatively and with a 2D radiographic measurement called Meary’s angle. This study seeks to determine the minimum number of bones required in a statistical shape model (SSM) to accurately represent the full cavus through planus spectrum, enabling future machine learning applications in clinical practice.
Methods:
Our study included weightbearing computed tomography (WBCT) data from 151 patients grouped based on clinical diagnosis or Meary’s angle: 33 Charcot-Marie-Tooth (CMT), 29 cavus, 28 rectus, 27 planus, and 34 progressive collapsing foot deformity (PCFD). Ten multi-bone SSMs, with varying numbers of bones, were created from bony segmentations. Principal component analysis (PCA) assessed the modes of variation for all SSMs.
Results:
PCA mode 1 demonstrated significant results (α = 0.05) for all SSMs, with the 2-bone subtalar joint (STJ) model capturing the most variance at 70.9% and the largest effect size of 0.75. The mean shape of all SSMs exhibited neutral STJ and midfoot alignment, whereas severe cavus and planus deformities were observed at 2 SDs from the mean shape. Models that included the STJ had statistical differences between all group PCA score comparisons. In contrast, models without the STJ had significant differences between all groups, except between the planus and rectus groups.
Conclusion:
STJ orientation and morphology appear fundamental for determining foot type. Our study revealed that the STJ alone offers sufficient information for computational differentiation because of its high variance and effect sizes when included in SSMs, highlighting the possible clinical utility as a simplified model. Although full foot models provide additional insights, the STJ model’s effectiveness makes it ideal for streamlined assessment and treatment planning.
Clinical Relevance:
Modeling the STJ captures the full cavus-planus foot type spectrum, suggesting its morphology may drive foot type and related pathologies. This underscores the potential of using simplified models in combination with machine learning as a rapid morphologic classifier; clinical impact remains to be determined.

Keywords
Introduction
Foot type plays a critical role in the development and progression of many foot and ankle pathologies because of its influence on biomechanics and force distribution.9,26,28,51 Foot type is a clinical concept designed to streamline the anatomical intricacies of the human foot (Figure 1). Three general foot types exist: pes planus (low medial longitudinal arch), rectus (neutral alignment), and pes cavus (high medial longitudinal arch).37,49 Pes planus individuals demonstrate overpronation, impingement, and reduced range of motion during gait, which may lead to conditions such as plantar fasciitis, arthritis, and tendon dysfunction.9,31 Progressive collapsing foot deformity (PCFD) is a clinical diagnosis characterized by collapse of the medial longitudinal arch, often presenting with severe pes planus that reflects an advanced stage of arch collapse.3,42 Conversely, the pes cavus foot presents with varus hindfoot, high calcaneal pitch, and increased lateral column ground reaction forces.2,26,31 These characteristics often result in poor shock absorption and eccentric loading, which increases the risk of stress fractures and metatarsalgia. Charcot-Marie-Tooth disease (CMT) is an inherited neuromuscular disorder presenting a range of foot deformities, including pes cavus, often accompanied by muscle weakness and sensory loss, with severity varying among patients.1,2,35 Most infants appear flatfooted at birth, with the arch typically developing during early childhood as the foot matures.22,52 However, the biological and mechanical factors influencing the formation of low or high arches remain unclear. In individuals who later present with PCFD or pes planus, the arch may either fail to develop entirely or may form initially and collapse over time. Understanding foot type development supports accurate classification, may lead to improvements in orthotic and footwear design, and lays the groundwork for future research into its role in foot and ankle pathologies with clinical relevance.

Charcot-Marie-Tooth (CMT) through progressive collapsing foot deformity (PCFD) foot deformity spectrum. The foot types in the middle of the spectrum include cavus (raised arch), rectus (neutral arch), and planus (low arch). Pink and blue lines represent the talus and first metatarsal longitudinal axes, respectively.
Foot type is typically determined qualitatively or by radiographic measure called Meary’s angle (MA), which is the angle formed between the longitudinal axes of the talus (midtalar axis) and the first metatarsal on lateral weightbearing foot imaging.30,46,57 Cavus foot type is defined as MA >4 degrees, planus as MA <−4 degrees, and the rectus range as −4 degrees ≤ MA ≤ 4 degrees.16,39,47 CMT and PCFD often exhibit greater deviation of normative MA values, but patients are ultimately diagnosed with these pathologies through comprehensive testing and evaluation.3,43 Efforts have been made to classify subcategories of foot type, but no quantitative or computational system exists.19,37,42
Morphologic analysis can be performed on weightbearing computed tomography (WBCT) data using statistical shape models (SSMs) to quantify and compare foot and ankle shapes between patient groups.10,33 WBCT offers a unique advantage by capturing the foot and ankle bones under physiological load, enabling detailed 3D assessment of joint alignment and morphology that surpasses conventional radiographs or nonweightbearing CT. Multidomain, or multibone, SSM can evaluate not just morphologic differences, but also alignment variations. 45 Although previous studies have used SSM to compare patient data within a specific deformity, it has yet to be used to describe or classify the cavus through planus foot type spectrum.4,32,33
With the bony complexity of the foot and ankle, it is difficult to determine the influence each segment or combination of segments may have. We hypothesize that the subtalar joint (STJ) will be a key determinant in distinguishing foot types because of its central anatomical location and pivotal influence on arch posture. Its complex 3D orientation directly affects load distribution and foot alignment, and including it in an SSM would enhance the ability to differentiate between deformities (CMT, cavus, rectus, planus, PCFD) while enabling shape analysis with reduced processing and computational demands. To evaluate this hypothesis, we created 10 multibone SSMs using WBCT data from patients with a broad range of foot types. Each model included the same patient data but varied in the number of bones, allowing for a systematic comparison of patient shape distributions based on the different foot segments. Our objective was to identify the minimum number of bones in an SSM that retained diagnostic utility while minimizing computational complexity. We employed principal component analysis, parallel analysis, and effect size calculations to assess the SSMs. Additionally, we assessed the spectrum of deformities by statistically evaluating Meary’s angles of each patient in the SSM.
Methods
Patient Data
WBCT data (0.37-mm3 voxels) from 151 patients (33 CMT, 29 cavus, 28 rectus, 27 planus, 34 PCFD) were acquired retrospectively with IRB approval or material transfer agreement from the University of Utah, the University of Iowa, and Nara Medical Center (Japan) (Table 1). Data with active fractures, severe osteoarthritis, metal hardware, or bony fusions were excluded. Unilateral data were used for all patients (n = 151), except for 15 cases in which bilateral data were included (9 CMT, 2 cavus, 3 planus, 1 PCFD). The 3 general foot type groups were initially classified by radiologic technologist MSK assessment based on weightbearing radiographs and subsequently confirmed using MA values determined computationally. MAs were calculated with an in-house 3D radiographic measurement toolkit that uses 3D bony segmentations to measure MA. Rectus MA range was −4.5 degrees ≤ MA ≤ 4.5 degrees, planus was MA < −4.5 degrees, and cavus was MA > 4.5 degrees.16,39,46,47 The cutoff value of 4.5 degrees accounted for rounding to 4 degrees. Patients were grouped as PCFD by a foot and ankle fellowship-trained orthopaedic surgeon. Individuals assessed as CMT had confirmed genetic or clinical diagnosis.
Patient Demographics and Meary’s Angle Results of Foot Type Data.

Data Processing
WBCT data were semiautomatically segmented using a commercial software (Disior Bonelogic 2.0; Paragon28, Helsinki, Finland) to generate segmentations of the calcaneus, cuboid, cuneiforms (intermediate, lateral, medial), fibula, metatarsals (1-5), navicular, talus, and tibia. Mimics 24.0 and 3-Matic 16.0 (Materialise, Leuven, Belgium) were used to manually audit, smooth, and decimate the initial segmentations to ensure all bone reconstructions were meshed comparably. All left feet were reflected to right-sided anatomy, and iterative closest point alignment methods were implemented in MATLAB 2024a (Mathworks Inc, Natick, MA) to align all 14 bones of each patient to one another. 56 Aligned and smoothed 3D meshes of each patient’s bony anatomy served as inputs for SSM, following similar methods from previous studies,5,23,28 and were also used in our in-house radiographic measurement toolbox in MATLAB to calculate MA automatically (Figure 2). This toolbox leverages coordinate systems derived from AAFACT 44 to calculate MA mathematically.

Methods pipeline. The top panel shows preprocessing steps from WBCT to smoothed and decimated bony segmentations. Following this, the segmented bones are used to build a statistical shape model and perform statistical analyses from shape model data (bottom left), as well as calculate Meary’s angle in MATLAB using the Automatic Anatomic Foot and Ankle Coordinate Toolbox (AAFACT) (bottom right). WBCT, weightbearing computed tomography.
Statistical Shape Modeling
SSMs were created in ShapeWorks 6.6.0 (SCI Institute, Salt Lake City, UT), an open-source SSM software. 10 The foot was divided into multiple segments: tibia/fibula (TF), subtalar joint (STJ), midfoot (MF), and forefoot (FF). 7 The 10 models were of each segment independently (TF, STJ, MF, FF) and different combinations of these segments (Table 2). All models used the same patient data and optimization parameters and had the same number of particles on each bone. The only difference between the models was the number of bones included. A generalized Procrustes analysis was applied in ShapeWorks to scale each patient’s bony anatomy and ensure inherent foot size differences did not interfere with variation analysis. ShapeWorks optimization uses a particle-based modeling approach to represent correspondence points as interacting sets of particles. Under an energy optimization scheme, these particles redistribute themselves to maintain correspondence between subjects and accurately describe the bone’s surface geometry. 10 The number of correspondence particles varied for each bone to ensure similar surface coverage across each bony surface, allowing a more accurate representation of each bone’s geometry. Once optimization and good particle correspondence were achieved, statistical analyses were performed.
SSM Model Segments and Combinations.

Abbreviations: FF, forefoot; MF, midfoot; SSM, statistical shape model; STJ, subtalar joint; TF, tibia/fibula.
Statistical Analyses
Principal component analysis (PCA) assessed the modes of variation determined by the correspondence particle locations in each SSM. Parallel analysis was performed to determine which modes of variation were significant to retain. 17 The Kolmogorov-Smirnov test (α = .05) assessed the normality of the PCA score distributions for each mode.38,41 With all the PCA score data normally distributed, one-way analysis of variance (ANOVA) was performed on the retained component scores to identify statistically significant patient group distributions with Tukey’s post hoc analysis (α = .05). 54 Effect size (η²) was computed for each retained mode from ANOVA results. 11 Cohen’s conventional effect benchmarks were used to assess η², where 0.01 is small, 0.06 is medium, and 0.14 is large.12,29 Analyses were performed separately for each SSM. Welch’s ANOVA with Games-Howell post hoc (α = .05) and Hedge’s g effect size were implemented to assess differences in MA values between foot type groups, accounting for unequal variances across groups.15,18,48,55 A standard Hedge’s g effect size range was used for assessment, where a small effect size is g >0.20, medium is g >0.5, and large is g >0.8.
Results
Patient Demographics
The data set had a median age of 53 years, a male-female ratio (%) of 48:52, and a left/right ratio (%) of 47:53 (Table 1). The median MA of the full spectrum was 0.5 degrees with a range from −37 to 52 degrees.
Meary’s Angle Group Comparison
All group comparisons were significantly different (P < .05) (Figure 3). Effect sizes were all considered large, except the comparison between PCFD and planus groups (g = −0.68), which identified a medium effect (0.5 < g < 0.8). The CMT group had the highest median MA at 25 degrees, followed by the cavus group at 16 degrees. The rectus group median MA was near neutral at 0.4 degrees, whereas the planus and PCFD groups had values at −11 and −15 degrees, respectively.

Meary’s angle distributions for each foot type group. Mean angles for each group include: 27 degrees for CMT (95% CI: 22.62-31.65 degrees), 17.42 degrees for cavus (95% CI: 14.16-20.68 degrees), 0.29 degrees for rectus (95% CI: −0.69 to 1.26 degrees), −10.65 degrees for planus (95% CI: −8.90 to −12.40 degrees), and −15.77 degrees for PCFD (95% CI: −12.59 to −18.94 degrees). Bars are annotated with P values and Hedge’s g effect size with 95% CIs, indicating significant differences between groups, which Welch’s analysis of variance determined with Games-Howell post hoc analysis (α = .05). All group comparisons were significantly different. Large effect size is g >0.80, medium is g >0.5, and small is g >0.2.
Statistical Shape Modeling and Principal Component Analysis
For all SSMs, mode 1 ranged from extreme cavus deformity with posterior subluxation of the talus at the STJ (at −2 SDs [σ] below the mean shape) to extreme flatfoot deformity with sinus tarsi impingement (at +2σ above the mean shape). The mean shape for all models exhibited neutral subtalar joint and midfoot alignment. In models with the midfoot, cuneiform alignment changes were present, where the cuneiforms are stacked nearly vertically at +2σ and horizontally at −2σ. All models maintained the same patient distribution trends, where CMT aligned closest with −2σ below the mean shape, followed by the cavus group. The rectus group was around the mean shape, whereas the planus and PCFD groups aligned best with the shape at +2σ above the mean. In single-segment SSMs (Figure 4), we see that the STJ and TF have significant differences in PCA score distributions between all groups. The MF and FF models have significant differences for all groups except between the planus and rectus groups. The distance maps of the shape ±2σ about the mean shape show that the STJ model has the largest distance values, ranging from −24 mm to 24 mm. We see a similar trend of the 2-segment SSMs (Figure 5), where models that include the STJ have significant differences between all foot type group PCA scores, whereas those without do not have significant differences between the planus and rectus groups. Of the multisegment SSMs (Figure 6), the STJ+MF+FF model explained the most variance in mode 1, followed by the TF+STJ+MF and full foot model.

Single-segment mode 1 principal component analysis results in top-down order of highest to lowest overall variance. Surface distances are displayed within the 2 SDs (σ), indicating the variation from the mean shape (center; gray), measured in millimeters. Red indicates shape differences away from the bone, representing an increase in feature size, whereas blue indicates shape differences toward the bone, representing a decrease. The legend explains the group markers that represent each patient in each foot type group, with their corresponding distribution along the 2-SD shape range. Significant differences between groups were determined by one-way analysis of variance and Tukey’s post hoc analysis (α = .05) and are indicated by asterisks. FF, forefoot; MF, midfoot; STJ, subtalar joint; TF, tibia/fibula.

Two-segment mode 1 principal component analysis results in top-down order of highest to lowest overall variance. Surface distances are displayed within the 2 SDs (σ), indicating the variation from the mean shape (center; gray), measured in millimeters. Red indicates shape differences away from the bone, representing an increase in feature size, whereas blue indicates shape differences toward the bone, representing a decrease. The legend explains the group markers that represent each patient in each foot type group, with their corresponding distribution along the 2-SD shape range. Significant differences between groups were determined by one-way analysis of variance and Tukey’s post hoc analysis (α = .05) and are indicated by asterisks. FF, forefoot; MF, midfoot; STJ, subtalar joint; TF, tibia/fibula.

Multi-segment mode 1 principal component analysis results in top-down order of highest to lowest overall variance. Surface distances are displayed within the 2 SDs (σ), indicating the variation from the mean shape (center; gray), measured in millimeters. Red indicates shape differences away from the bone, representing an increase in feature size, whereas blue indicates shape differences toward the bone, representing a decrease. The legend explains the group markers that represent each patient in each foot type group, with their corresponding distribution along the 2-SD shape range. Significant differences between groups were determined by one-way analysis of variance and Tukey’s post hoc analysis (α = .05) and are indicated by asterisks. FF, forefoot; MF, midfoot; STJ, subtalar joint; TF, tibia/fibula.
The STJ model had the largest variance in PCA mode 1, at 70.9%, and an η² of 0.75 (95% CI: 0.26-0.89), indicating a large effect size. Of the SSMs that are combinations of segments, only those that included the STJ had significant differences between all foot type group comparisons; those without the STJ showed nonsignificant differences between the planus and rectus groups (Table 3).
PCA Mode 1 Variance and η² Effect Size for Each SSM. a
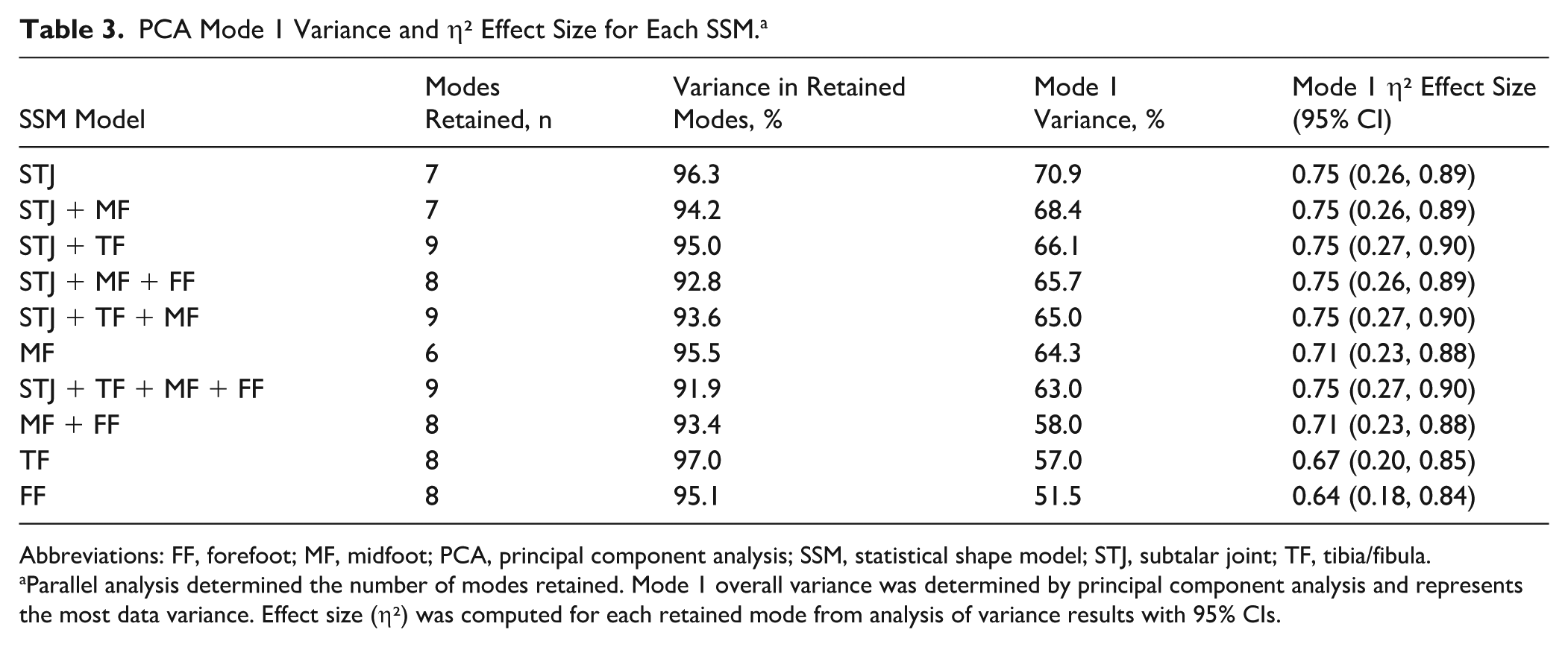
Abbreviations: FF, forefoot; MF, midfoot; PCA, principal component analysis; SSM, statistical shape model; STJ, subtalar joint; TF, tibia/fibula.
Parallel analysis determined the number of modes retained. Mode 1 overall variance was determined by principal component analysis and represents the most data variance. Effect size (η²) was computed for each retained mode from analysis of variance results with 95% CIs.
Discussion
This study established the minimum number of bones required in an SSM to classify the cavus-planus spectrum using WBCT data by systematically evaluating foot morphology and alignment variations between foot type groups. The STJ has long been regarded as one of the most complex and misunderstood joints in the human body, a reputation supported by early and recent studies.6,27,53 Notably, this study found that the 2-bone STJ SSM outperformed the other models statistically, with the largest amount of explained variance in PCA mode 1 (70.9%) and the largest effect size (η² = 0.75). Across all models tested, only those that included the STJ could successfully differentiate between foot type groups, underscoring the joint’s critical role in foot biomechanics and classification. However, although the model captures morphologic features and weightbearing alignment, it does not establish causal or functional relationships. Full-foot models may offer potential added insights, such as “compensation” patterns involving metatarsal alignment and cuneiform stacking, but the STJ model distinguishes itself through its simplicity and effectiveness in detecting the unique morphologic differences along the cavus-planus spectrum.
Although MA is a straightforward measure for evaluating sagittal plane alignment, there is limited research on the expected range of MA in pathologic groups such as PCFD or CMT disease. Our study identified that some individuals diagnosed with PCFD exhibit MA values that fell within the range typically associated with a rectus aligned foot (−4 degrees ≤ MA ≤ +4 degrees) and demonstrated only a medium effect size between the PCFD and planus groups (g = −0.68). This discrepancy is likely due to the collapse primarily occurring in the midfoot region, which MA does not fully capture, as it only considers alignment of the talus and first metatarsal. As observed in clinical practice, PCFD can present in different forms—some cases appear driven primarily by subtalar joint collapse, whereas others involve a midfoot break with relatively preserved STJ orientation. SSM can capture these distinctions when the midfoot is included, as it enhances the ability to differentiate between PCFD subtypes. Although the simplified STJ model offers greater clinical practicality because of its efficiency and focus, incorporating the midfoot provides added detail that is especially helpful for distinguishing complex deformities. This ability to capture subtle structural differences goes beyond what simpler measures like MA can offer. Overall, SSM enables more comprehensive and precise evaluation of foot types, supporting improved clinical assessment and surgical planning.
Shape modeling from WBCT data combined with MA for group classifications extends the 2-dimensional (2D) radiographic measurement to 3-dimensional (3D) space that considers the shape and alignment of the entire foot and ankle in weightbearing position. The weightbearing component of this analysis is critical, as nonweightbearing assessments may fail to detect structural abnormalities when the foot is functionally loaded, particularly in individuals with flexible flatfoot.13,24 Using WBCT leads to consistent positioning compared to the uncontrolled unloaded supine position during conventional CT scans.8,20,34 Shape modeling from WBCT data allows for the analysis of the entire bony structure of the foot and ankle in 3D, capturing not just alignment changes but subtle variations in bony morphology and joint relationships that are often occluded in 2D views. This approach is especially valuable in pathologic conditions like PCFD or CMT, where structural changes may be more extreme in the midfoot or hindfoot planes that are not visible on traditional lateral or anteroposterior radiographs. By quantifying and comparing anatomical variations across populations, SSM offers an objective and reproducible method for classifying foot types, assessing deformity severity, and evaluating the foot and ankle.
Contributions from multiple regions of the foot and ankle influence the structural characteristics of different foot types. The proximal segments, like the tibia and fibula, can affect the global alignment, particularly in the sagittal and frontal planes, whereas the midfoot and forefoot often exhibit compensatory adaptations such as arch collapse, cuneiform stacking, or metatarsal splaying in response to deformities elsewhere.14,36 However, the STJ consistently emerges as the most influential segment of the foot, driving foot-type classification. Its 3D motion in all planes, combined with the unique anatomic feature of the talus having no direct muscular or tendon attachments, allows it to move more freely within the ankle mortise. 25 This biomechanical independence may be a key factor in the STJ’s ability to mediate complex motion and alignment changes throughout the foot and ankle. Our findings reinforce this, showing that only the models that included the STJ could statistically differentiate the full foot type spectrum. This underscores the STJ’s dominant influence on foot morphology and highlights its critical role in understanding and classifying complex deformities.
Building on this, our findings further emphasize how STJ orientation and its articular relationships contribute to hindfoot alignment. Restoring the calcaneal plumb line is crucial for reestablishing correct subtalar positioning and articulations, which many clinicians recognize as essential for effective deformity correction and perform procedures such as osteotomies for realignment.21,40,50 This research provides objective evidence that supports these clinical principles, reinforcing the need for precise anatomical realignment of the hindfoot to optimize functional outcomes throughout the foot and ankle. The positioning of the STJ is fundamental to achieving successful surgical outcomes in foot and ankle deformity correction.
This study uses SSM and WBCT data to effectively differentiate the different foot type groups, but several limitations remain. WBCT provides static images that may not capture functional compensation. Bilateral scans introduce unmodeled nonindependence, and external or patient-reported validation is lacking. Additionally, the study groups the 3 intermediate foot types (cavus, planus, and rectus) on radiographic interpretation from a musculoskeletal radiologist and MA values. More measurements, such as calcaneal pitch or calcaneus–first metatarsal angle, would provide further quantitative insights into these multiplanar deformities and may reinforce these initial groupings or provide a refined set of foot-type groups. Another limitation is that the individuals grouped as cavus ranged from minimal to severe deformations (minimum MA = 5.2 degrees, maximum MA = 33 degrees). Two-thirds of adults with symptomatic cavus foot type have an underlying neurologic condition, most commonly CMT. 2 Although the cavus group was composed of asymptomatic individuals with low suspicion of motor/sensory neuropathy to warrant neuroelectrophysiologic study, it is possible that available genetic testing could reveal an underlying inherited cause in some patients of this cohort.
The STJ SSM provides an efficient alternative to full foot models, particularly when time or computational resources are limited. Although not yet ready for clinical implementation, its integration with machine learning demonstrates potential for future development of rapid, accurate foot type classification tools, supporting objective assessment, personalized treatment planning, and STJ-focused interventions.
Conclusion
By leveraging 3D SSM, we demonstrate that the STJ plays a pivotal role in defining foot types. Increased emphasis on the STJ during assessment using advanced imaging modalities like WBCT may enhance classification accuracy and inform targeted treatment strategies. As foot and ankle care continues to evolve toward precision-based approaches, the STJ should be recognized as a central structure. Further studies linking these morphologic clusters to symptoms, functions, and outcomes are needed before the method can inform treatment.
Supplemental Material
sj-pdf-1-fao-10.1177_24730114251390497 – Supplemental material for Subtalar Joint Statistical Shape Modeling Differentiates Cavus-to-Planus Foot Types From Weightbearing CT
Supplemental material, sj-pdf-1-fao-10.1177_24730114251390497 for Subtalar Joint Statistical Shape Modeling Differentiates Cavus-to-Planus Foot Types From Weightbearing CT by E. Renae Lapins, Andrew C. Peterson, Charles L. Saltzman, Shireen Y. Elhabian, Bopha Chrea, Takuma Miyamoto and Amy L. Lenz in Foot & Ankle Orthopaedics
Footnotes
Acknowledgements
We would like to acknowledge Melissa Requist, Kas Knutson, Andrew Peterson, Takuma Miyamoto, Meghan Carter, Eliana Moreno, and Brian Keller for their invaluable contributions in segmenting and preprocessing image data used in this study.
ORCID iDs
Ethical Considerations
This use of data for this study was approved by the institutional review board of both institutions (IRB00154634). An opt-out statement regarding the application of medical data was published on our institute’s website. This study was performed under the principles of the World Medical Association Declarations of Helsinki.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: funding provided by the National Institutes of Health (NIAMS K01AR080221). Additionally, the National Institutes of Health provided ShapeWorks development grants (NIH U24EB029011 and NIH R01AR076120).
Declaration of Conflicting Interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Charles L. Saltzman, MD, reports being the Editor-in-Chief of Foot & Ankle International. Bopha Chrea, MD, reports general disclosures of Paragon 28: consultant. Amy L. Lenz, PhD, reports general disclosures of Foot & Ankle International / Foot & Ankle Orthopaedics: specialty content editor. Disclosure forms for all authors are available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
