Abstract
Background:
Medial malleolar stress fractures (MMSFs) are difficult to detect early because of subtle or absent findings on plain radiographs, which often delays diagnosis and return to play. Identifying measurable radiographic alignment patterns may assist in raising early clinical suspicion, particularly in settings where advanced imaging such as computed tomography (CT) or magnetic resonance imaging (MRI) is not readily available.
This study aimed to investigate the radiographic features of MMSFs in athletes by comparing specific ankle alignment angles on plain radiographs.
Methods:
A retrospective observational study was conducted. Athletes diagnosed with MMSFs were matched 1:1 with control athletes based on age, sex, and the laterality of the affected ankle. Radiographic measurements included the tibial anterior surface (TAS), tibial medial malleolus (TMM), tibial bimalleolar (TBM), and tibial lateral surface (TLS) angles.
Results:
The MMSFs group included 23 athletes (19 men, 4 women), and the control group included 23 athletes (20 men, 3 women). The TAS angle was significantly smaller in the MMSF group compared with controls (86.3 ± 2.1 degrees vs 89.3 ± 1.6 degrees, P < .01). Receiver operating characteristic curve analysis yielded an area under the curve of 0.86 (95% CI 0.75-0.96), with an optimal TAS angle cutoff value of 87.8 degrees showing 73.9% sensitivity and 91.7% specificity. No significant differences were observed for the TMM (P = .09), TBM (P = .14), or TLS angle (P = .84).
Conclusion:
These findings suggest that smaller TAS angles may be a radiographic feature associated with increased susceptibility to MMSFs in athletes and could support clinical suspicion during early evaluation.
Level of Evidence:
Level III, case-control study.

Keywords
Introduction
Medial malleolar stress fractures
Early diagnosis is essential to prevent progression and enable a timely return to play. However, diagnosis in the early stages is challenging because symptoms may be mild, and characteristic vertical fracture lines at the junction between the medial malleolus and tibial plafond may not be apparent on plain radiographs. Computed tomography (CT) and magnetic resonance imaging (MRI) are beneficial for diagnosing MMSFs early. However, these modalities are often not readily accessible in clinical practice, making plain radiography the first-choice imaging modality.
Given this challenge, it may be clinically helpful to identify subtle but measurable radiographic features that, although not definitive for diagnosis, could support early clinical suspicion and prompt further evaluation when CT or MRI is not readily available. This study aimed to identify characteristic radiographic findings of MMSFs in athletes, particularly focusing on measurable tibial alignment angles on standard ankle radiographs, to aid early diagnosis.
Methods
This retrospective observational study was approved by the institutional review board, and informed consent was obtained from all participants.
The study was conducted at our affiliated institutions and included patients who underwent ankle radiographic evaluation between January 2006 and April 2025. Athletes who underwent both standard ankle radiographs and CT were included in the MMSFs group (Figure 1). Although all patients had radiographs, the diagnosis of MMSFs was made based on CT findings to ensure consistency, as fracture lines were not always apparent on plain radiographs. The control group consisted of athletes who underwent standard ankle radiography between May 2024 and March 2025 for minor trauma and demonstrated no evidence of ankle fractures or ligament injuries on both plain radiographs and ultrasound examination (Table 1). Cases with small avulsion fractures of the tarsal bones were included, as these findings were considered unlikely to influence the occurrence of medial malleolar stress fractures or tibial alignment angle. Follow-up confirmed resolution of the initial symptoms and absence of recurrence for at least 3 months. Controls were matched to cases in a 1:1 ratio based on age, sex, and the laterality of the affected ankle. Patients with a history of ankle fractures, ligament injuries, osteochondral lesions (OCL), or previous ankle surgeries were excluded from both groups.

Representative plain radiograph of a medial malleolar stress fracture. Representative anteroposterior radiograph of the ankle showing an oblique fracture line at the medial malleolus (arrow).
Demographic and Athletic Characteristics of the Participants.

Abbreviation: MMSF, medial malleolar stress fracture.
Patient age, sex, height, body weight, body mass index, affected ankle side, type of sport, competitive level, and radiographic measurements were compared between the 2 groups. Standard anteroposterior and lateral ankle radiographs were used to evaluate the tibial anterior surface (TAS) angle, tibial medial malleolus (TMM) angle, tibial bimalleolar (TBM) angle, and tibial lateral surface (TLS) angle, as shown in Figure 2. Radiographic acquisition and measurement methods were performed in accordance with the procedures described by Sugimoto et al 14 : TAS, angle between the tibial axis and plafond; TMM, angle formed between the tibial axis and the inclination of the medial malleolus; TBM, angle formed between the tibial axis and the line connecting the medial and lateral malleoli; and TLS, angle formed between the tibial axis and the line connecting the anterior and posterior edges of the plafond. The tibial axis was defined as a line connecting the midpoints of 2 lines drawn perpendicular to the tibial shaft in the diaphyseal region, as illustrated in Figure 1. Radiographic measurements were performed by 2 independent observers in 2025. One observer, a board-certified orthopaedic surgeon with more than 10 years of clinical experience, was masked to group allocation (MMSFs or control) to reduce measurement bias. The second observer, who had more than 15 years of experience and had assessed more than 1000 ankle radiographs, was not masked and served as a reference standard to ensure consistency in landmark identification and measurement protocols. Interobserver reliability was assessed to confirm the robustness of the measurement process.

Measurement of radiographic alignment angles: (A) tibial anterior surface angle (TAS), (B) tibial medial malleolus angle (TMM), (C) tibial bimalleolar angle (TBM), and (D) tibial lateral surface angle (TLS).
Quantitative variables such as the TAS, TMM, TBM, and TLS angles were assessed for normality using the Shapiro-Wilk test. Normally distributed variables were summarized as mean ± SD and compared between groups using the unpaired t test. Non-normally distributed variables were expressed as median (IQR) and analyzed using the Mann-Whitney U test. For categorical variables such as sex and laterality, Fisher exact test was used. Statistical significance was defined as P <.05. Receiver operating characteristic (ROC) curve analysis was performed to assess the ability of the TAS angle to discriminate between the MMSF and control groups, and the optimal cutoff value was determined using the Youden index. The area under the curve and 95% CIs were reported.
Intra- and interrater reliabilities were assessed using intraclass correlation coefficients (ICCs). Intrarater reliability employed ICC(1,1), whereas interrater reliability used ICC(2,2). All statistical analyses were performed using the psych package in R (v4.3.1). 12 To further assess the agreement between observers, Bland-Altman analyses were performed for each radiographic parameter to assess the level of concordance between the 2 raters.
A priori power analysis using G*Power version 3.1.9.7 software (Franz Faul, Universitat Kiel, Germany) determined the required sample sizes. Effect sizes (Cohen d) for all radiographic parameters were calculated using the difference in mean values between the MMSF and control groups divided by the pooled SD. The calculated effect size was large (Cohen d = 0.95), with a significance level of .05, power of 0.80, and 2-tailed testing, yielding a sufficient sample size of 8 per group. In contrast, required sample sizes for TMM (d = 0.48), TBM (d = 0.37), and TLS angles (d = 0.14) were substantially larger because of the small effect sizes.
Results
The MMSF group included 23 athletes (19 men, 4 women), and the control group included 23 athletes (20 men, 3 women). The detailed characteristics of the participants are shown in Table 1. Of the 23 MMSF cases, 13 underwent surgical fixation, and the other 10 were successfully treated with conservative management. Among the MMSFs, 9 were complete fractures and 14 were incomplete fractures; 17 were classified as vertical type and 6 as oblique type. All patients returned to sport within 4 months (Table 1).
No significant differences in characteristics of participants (age, sex ratio, height, body weight, body mass index, or affected ankle side) were observed between the 2 groups (Table 2). The median TAS angle in the fracture group was 86.3 degrees ± 2.1, whereas the control group had a median of 89.4 ± 1.6 degrees, showing a statistically significant difference (P < .01). The ROC curve for the TAS angle is shown in Figure 3, demonstrating an area under the curve of 0.86 (95% CI 0.75-0.96), and the optimal TAS angle cutoff value of 87.8 degrees demonstrated 73.9% sensitivity and 91.7% specificity. No significant differences were observed for the mean TMM (25.2 ± 4.2 degrees vs 23.1 ± 3.8 degrees, P = .09), TBM (75.7 ± 3.6 degrees vs 77.1 ± 2.5 degrees, P = .14), or TLS angle (84.5 degrees ± 2.5 degrees vs 84.7 degrees ± 2.8 degrees; P = .84) (Table 3). Among the evaluated parameters, only the TAS angle demonstrated a significant difference between groups and was subjected to ROC analysis. Other parameters showed no significant discriminatory ability and were not further analyzed.
Baseline Characteristics of the MMSF and Control Groups. a

Abbreviations: BMI, body mass index; MMSFs, medial malleolar stress fractures.
Values are presented as mean ± SD for height and as median (IQR) for age, body weight, and BMI.
Fisher exact test.
Mann-Whitney U test.
Unpaired t test.
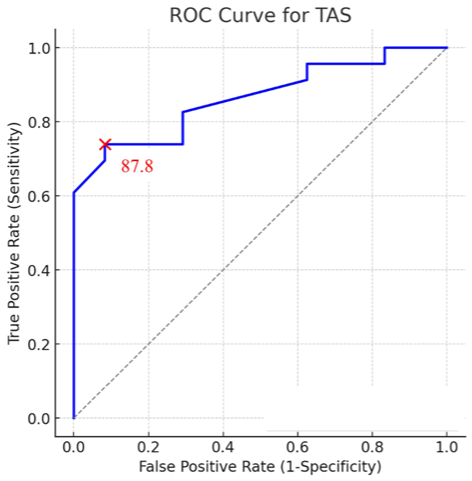
ROC Curve for TAS. AUC of 0.86(95% CI: 0.75-0.96), and the optimal TAS cut-off value of 87.8 degrees demonstrated 73.9% sensitivity and 91.7% specificity.
Comparison of Radiographic Measurements Between MMSF and Control Groups. a

Abbreviations: MMSF, medial malleolar stress fracture; TAS, tibial anterior surface; TBM, tibial bimalleolar; TLS, tibial lateral surface; TMM, tibial medial malleolus.
Values are presented as mean ± SD.
Intrarater ICC(1,1) values were as follows: TAS angle (0.727, 0.690), TMM angle (0.886, 0.617), TBM angle (0.699, 0.905), and TLS angle (0.910, 0.763). Interrater ICC(2,2) values were as follows: TAS angle (0.863), TMM angle (0.815), TBM angle (0.897), and TLS angle (0.881), indicating good to excellent agreement. Bland-Altman analysis demonstrated satisfactory interobserver agreement across all radiographic parameters. A representative Bland-Altman plot is provided in Supplementary Figure 1. The mean differences (bias) between observers were −1.27 degrees for the TAS angle, −0.13 degrees for the TMM angle, −0.47 degrees for the TBM angle, and −0.60 degrees for the TLS angle. The 95% limits of agreement were relatively narrow, particularly for TAS and TLS angles. A single outlier (4.3%) was identified in the TAS, TMM, and TBM angle measurements, whereas no outliers were observed for the TLS angle, indicating high consistency between raters.
Discussion
This study is the first to demonstrate that a lower TAS angle on plain radiographs is associated with MMSFs in athletes. The ROC-derived cutoff value of 87.8 degrees yielded an area under the curve of 0.86, suggesting potential clinical relevance for identifying at-risk individuals. Although the absolute difference in TAS angle between groups was small, the large effect size (Cohen d = 0.95) and high interrater reliability support the relevance of this parameter. These findings suggest that even subtle malalignment may contribute to MMSF susceptibility in athletes. In contrast, other measured angles (TMM, TBM, TLS) showed no significant intergroup differences, indicating limited diagnostic value. Our results should be interpreted with caution. Although the sample size was sufficient to detect differences in TAS angle, the absolute number of cases remains small, limiting generalizability and precluding robust subgroup analyses. Early symptoms of MMSFs are often nonspecific, and initial radiographic findings may be subtle or absent. Because we matched cases and controls on age, sex, and side, future analyses should account for matching (eg, paired tests or conditional models); our between-group tests did not, which may have a modest effect on precision. Therefore, although identifying radiographic features associated with increased susceptibility is important, the TAS angle should not replace definitive diagnostic tools such as CT or MRI. Instead, a smaller TAS angle may serve as a marker of anatomical predisposition, prompting heightened clinical suspicion and further evaluation—particularly in settings where advanced imaging is not immediately available.
Regarding the risk factors for MMSFs, Nguyen et al 9 reported 16 cases in professional soccer players, noting varus alignment in 50% of the cases. However, they did not specify how the alignment was measured or the degrees of varus deformity. Approximately half of the athletes in our cohort were also soccer players, a group potentially predisposed to repetitive medial malleolus stress due to kicking mechanics. Such sport-specific factors may contribute to fracture development independently of radiographic alignment, and future studies should consider stratification by sport.
Both extrinsic and intrinsic factors have been reported to contribute to the development of MMSFs. Extrinsic factors include training errors, inadequate footwear, sudden increases in activity, and weight gain. 2 Intrinsic factors, such as forefoot varus, subtalar varus, limb length discrepancy, muscular insufficiency, tibial varus, and pes cavus, have been hypothesized, although they lack strong supporting evidence.10,11,13 In addition to tibial alignment, other intrinsic or anatomical factors such as anterior ankle impingement and cavus foot posture have been proposed as independent risk factors for MMSFs.5,8 Future investigations should aim to combine radiographic alignment analysis with clinical and biomechanical assessments to develop a more comprehensive risk profile for MMSF development.
By quantifying these angles on plain radiographs, clinicians may be better equipped to recognize athletes with potential anatomical predispositions. Compared with previously reported typical normal values (TAS angle: 88.9 degrees), the control group in our study showed no notable deviations, emphasizing the relevance of the findings observed in the fracture group. 7
Although the TAS angle cutoff of 87.8 degrees is informative, its clinical application requires careful consideration. In athletes presenting with medial ankle pain and borderline TAS angle values, a smaller TAS angle may warrant increased suspicion for MMSFs and justify additional imaging such as MRI. However, TAS angle alone is unlikely to alter management, and conservative treatment remains the standard once a stress fracture is diagnosed. The proposed TAS angle cutoff value of 87.8 degrees should therefore be regarded as a preliminary, requiring prospective validation in sport-specific external cohorts before adoption as a diagnostic threshold.
The limitations of this study include its retrospective nature, relatively small absolute sample size despite adequate statistical power for TAS angle analysis, and lack of patient cohort diversity. Although the MMSFs group included cases from a wider time frame (2006-2025), standard radiographic protocols were consistently applied throughout the study period at our institution. In contrast, the control group was drawn from a narrower time window (2024-2025). Nonetheless, potential improvements in imaging technology or diagnostic criteria over time may have influenced case detection, which we recognize as a limitation. Although we carefully selected control subjects who had undergone radiographic evaluation for minor ankle trauma and showed no evidence of ankle fractures or ligament injuries, we acknowledge the possibility that subclinical stress fractures may have been undetected on initial imaging. This potential misclassification represents another limitation. However, considering the rarity of MMSFs, this study provides valuable data. Future studies should involve larger cohorts and prospective designs, ideally incorporating professional sports registry data, to validate our findings and explore preventive measures for athletes with smaller TAS angle values. Noninvasive interventions, such as alignment-correcting foot orthoses, may hold promise as a preventive strategy to reduce the risk of MMSFs in athletes with predisposing anatomical factors.
Conclusion
This study suggests that a smaller TAS angle on plain radiographs may be associated with increased susceptibility to MMSFs in athletes. Although the TAS angle alone is unlikely to influence management decisions directly, recognizing this alignment feature may help clinicians maintain a higher index of suspicion and prompt earlier diagnostic imaging, thereby supporting timely conservative interventions such as activity modification. Future investigations should also explore ways to advance prevention and treatment strategies for this challenging condition.
Supplemental Material
sj-pdf-1-fao-10.1177_24730114251386024 – Supplemental material for Plain Radiograph Alignment Features Associated With Medial Malleolar Stress Fractures in Athletes: A Matched Case-Control Study
Supplemental material, sj-pdf-1-fao-10.1177_24730114251386024 for Plain Radiograph Alignment Features Associated With Medial Malleolar Stress Fractures in Athletes: A Matched Case-Control Study by Tomohiro Matsui, Kazuya Sugimoto, Kimio Miura, Shinji Isomoto, Akira Taniguchi and Yasuhito Tanaka in Foot & Ankle Orthopaedics
Footnotes
Appendix
Bland-Altman analyses.

| Mean Difference | SD | Upper LoA | Lower LoA | Outliers | Total | Outlier % | |
|---|---|---|---|---|---|---|---|
| TAS angle | −1.26667 | 1.944467 | 2.544489 | −5.07782 | 1 | 23 | 4.347826 |
| TMM angle | −0.13333 | 3.719959 | 7.157786 | −7.42445 | 1 | 23 | 4.347826 |
| TBM angle | −0.46667 | 1.995232 | 3.443989 | −4.37732 | 1 | 23 | 4.347826 |
| TLS angle | −0.6 | 2.131398 | 3.57754 | −4.77754 | 0 | 23 | 0 |
Abbreviations: TAS, tibial anterior surface; TBM, tibial bimalleolar; TLS, tibial lateral surface; TMM, tibial medial malleolus.
Ethical Considerations
Ethical approval for this study was obtained from Saiseikai Nara Hospital Institutional Review Board (Approval No. 2).
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article. Disclosure forms for all authors are available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
