Abstract

Introduction
There has been much discussion toward treatment of hallux valgus (HV) while complicated with concomitant metatarsus adductus (MA) deformity in the literature. 2 MA can hinder the reduction of HV and cause less of a desired outcome and/or increased risk of HV recurrence. 3 Current literature suggests that the population aged 18-65 years and aged 65 years and older have around 23% and 36% rate of HV, respectively.2,3
Many studies have produced results that favor addressing the MA with either midshaft or proximal metatarsal osteotomies, or correction with lesser tarsometatarsal joint arthrodesis. Results have shown when the MA is not addressed that there can be an increased risk of HV recurrence after operative reconstruction, which has been reported between 17% and 30%.1,6
A study by Park and Lee in 2017 found risk factors associated with HV recurrence to be sesamoid position >4, HV >8 degrees immediately postoperative, and preoperative MA >23 degrees that was not addressed. 5 In addition, many other authors have advocated for correction of the MA for HV treatment for overall better foot alignment and decreased recurrence. Furthermore, those with MA are 3.5 times at risk of developing HV secondary to losing the physical buttress that the second digit provides. 4
This article describes the techniques we use to address HV with MA correction using a minimally invasive approach. The techniques describe how to determine the starting point for the lesser metatarsal osteotomy, as well as different fixation constructs depending on the ancillary procedures.
Technique
Analysis of Osteotomy Placement of Lesser Metatarsals
We use a radiographic method to determine where to make the osteotomy along the lesser metatarsals. Based on AP foot preoperative weightbearing films, a linear line is created from the medial cortical edge of the medial cuneiform. Hypothetically, the line represents the desired “anatomical” position that the metatarsal should be parallel to assuming there are no hindfoot deformities influencing the forefoot. The line is then translated laterally to the medial intercuneiform joint, and subsequently is extended distally until it intersects with the medial cortex of the 2nd metatarsal and then extending to the lateral cortex, denoting the osteotomy site to be started, seen in Figure 1. Creating the osteotomy at this junction ensures that as the first metatarsal is reduced, it will not be inhibited by the position of the second metatarsal. This method is then continued laterally for the third and fourth metatarsal, respectively.
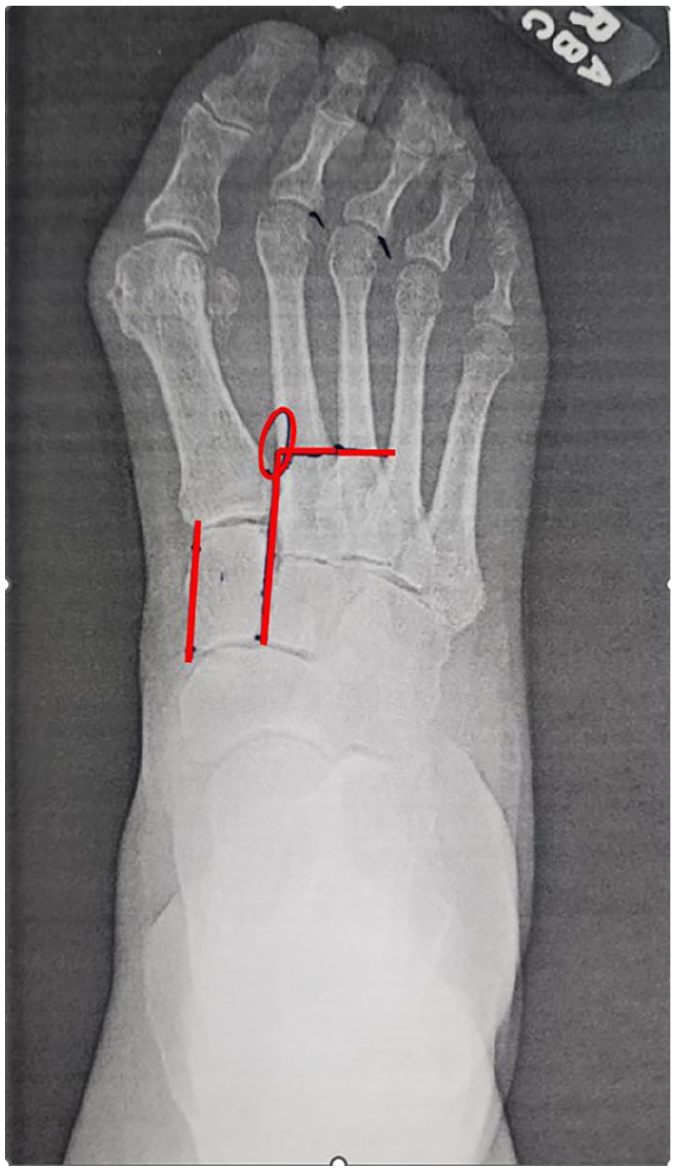
Schematic method for determining the osteotomy site level along the lesser metatarsals highlighted by the red lines.
Surgery
Patients are selected on a radiographic and clinical diagnosis. In the operating room, the patient is placed in a supine position on the operative table and general anesthesia is induced, followed by a popliteal and saphenous nerve block. The extremity is prepared in standard fashion, with a thigh tourniquet and the C-arm on the contralateral side. Incisions are mapped out using radiographic imaging to identify the first tarsometatarsal joint and the bases of the second, third, and/or fourth metatarsals.
Medial incision and dissection are performed to expose the first tarsometatarsal joint (TMT). The first TMT joint is released circumferentially of the capsular and tendinous attachments to mobilize the joint for reduction in triplanar fashion in a modified Lapidus technique, similarly described by Conti et al. 3
With respect to metatarsus adductus correction, a small dorsal stab incision is created at the proximal second and fourth (if the fourth metatarsal is involved) intermetatarsal space, followed by blunt dissection down to the respected metatarsal base. Next a periosteal elevator is introduced to remove the soft tissue off the metatarsals where the Shannon Recta burr (Enovis Corp, Wilmington, DE) is introduced and placed on the lateral cortex for the metatarsal. The burr is set to a low revolution (around 5500 rpm) and high torque to aid in osseous cutting, user tactile, and audible feedback. With guidance of fluoroscopy, the burr is rotated or translated to create a partial thickness transverse osteotomy, leaving a hinge at the medial cortex. The metatarsal is manually manipulated. The deformity is reduced laterally. A Kirschner (K)-wire is then used to percutaneously fixate the osteotomy site from a dorsal-distal to plantar proximal vector. Figure 2 demonstrates this technique as well as preoperative and 6-week consolidated phase. During reduction of the first TMT, if the lesser metatarsals are still hindering reduction, then the burr will be used to make a full transverse osteotomy of the lesser metatarsals. This allows proper reduction of the first TMT, while allowing for the osteotomized metatarsals to be further lateralized and find their resting position. When a full transverse osteotomy is needed, fixation is not applied as reduction and fixation of the first TMT creates a medial buttress to maintain the lesser metatarsals in the reduced position. Figure 3 demonstrates this technique as well as a preoperative and 6-week consolidated phase.

A case of a lateral base-closing osteotomies of metatarsals 2-4 with a burr, fixated with percutaneous K-wires. Also shown is the triplanar fixation of the first tarsometatarsal arthrodesis. Left to right: preoperative, immediate postoperative, and around 6 weeks with consolidation.

Full transverse osteotomy of the lesser metatarsus adductus without fixation, allowing for adequate reduction of the first tarsometatarsal. Note the lateralization of the lesser metatarsal 2-4. Left to right: preoperative, immediate postoperative, and around 6 weeks with consolidation.
Regardless of fixation, the limb is placed into a posterior splint and made nonweightbearing. At around postoperative week 4-6, if radiographic evolution shows adequate osseous bridging of the first TMT, then K-wires are removed and the patient is advanced to protected/full weightbearing in a controlled ankle motion boot.
Discussion
The techniques described above demonstrate two corrective methods to accommodate different operative sceneries. It has favored us well at our institution and we believe this technique provides minimal risk to the patient with the ability to keep the lesser tarsometatarsal joints from being violated. The nonfixated approach relies on metatarsal displacement and reduction maintained through soft tissue tension, and as described the first ray now being a stabilizing buttress to prevent MA recurrence. We have observed excellent osseous consolidation and stability in the postoperative period, as seen in Figure 3. Although there is more stability of the osteotomy site with lateral wedge osteotomies, they are pinned so that the intact cortex does not influence the opening of the wedge after closure and reduction. The K-wire is pulled after adequate callous formation to stabilize the osteotomy site. Our closing wedge is in similar fashion to that of the technique described by Wireman et al 7 in 2025. Wireman et al describes a minimally invasive surgical approach to medial closing wedge of the fifth metatarsal base for bunionette correction with fixation.
The techniques described have provided great outcomes for our patients. We describe our techniques in the hopes of aiding other surgeons with a framework to approach metatarsus adductus deformity correction during Lapidus bunionectomy.
Supplemental Material
sj-pdf-1-fao-10.1177_24730114251327194 – Supplemental material for Approaches to Minimally Invasive Surgery for Treatment of Metatarsus Adductus with Hallux Valgus Correction With Modified Lapidus: A Novel Technique Guide
Supplemental material, sj-pdf-1-fao-10.1177_24730114251327194 for Approaches to Minimally Invasive Surgery for Treatment of Metatarsus Adductus with Hallux Valgus Correction With Modified Lapidus: A Novel Technique Guide by Garrett Wireman, Anthony Schwab, Jason Nowak and Garret Strand in Foot & Ankle Orthopaedics
Footnotes
Ethical Approval
Ethical approval was not sought for the present study.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Garret Strand, DPM, FACFAS, reports he is a consultant for Enovis/DJO. Jason Nowak, DPM, FACFAS, reports he is a consultant for Enovis/DJO. Disclosure forms for all authors are available online.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by Shasta Orthopaedics & Sports Medicine.
Informed Consent
Informed consent was obtained from the patient for the publication of this study and accompanying images.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
