Abstract
Background:
Mandibular Condyle fractures are common and the traditional method for the exposure is the retromandibular approach, however it presents some limitations and considerations among facial nerve palsy and parotid gland fistulae. This technical note present a novel approach to the subcondylar fractures, using preauricular incision with an innovative transmasseteric dissection.
Study Design:
Technical note.
Objective:
Present a novel approach to the subcondylar fractures, using preauricular incision with an innovative transmasseteric dissection.
Methods:
Patients diagnosed for mandibular condyle fractures in a Level 1 Trauma Center in Brazil. All the procedures were performed in the shortest possible time since the trauma. Traditional preauricular incision with gentle lower dissection through the superficial musculoaponeurotic system, the facial nerve branches are exposed and retracted. The parotid gland capsule plane is outlined and the parotid gland is retracted posteriorly. The masseteric fascia is exposed and the masseteric muscle is incised and the blunt dissection continues toward the periosteum and the mandibular condyle.
Results:
Eight patients were surgically managed in the acute trauma with a mean of 2.57 days to the operation. Transient parotid gland fistulae was observed in only 12.5% of the patients. Facial nerve palsy was observed in 37.5% of the patients in the first 7 days of postoperative time, with no records of persistent facial nerve paralysis.
Conclusions:
The preauricular transmasseteric approach is a reliable and versatile option for the exposure of the mandibular condyle, being a safe and aesthetic incision on the management of the subcondylar area. The surgical team use it as a novel tool in the approach for condyle fractures.
Mandibular Condylar fractures (MCF) are common, being documented from 17.5% to 52% of all mandibular fractures. 1 The management of MCF remains controversial in the literature. The non-surgical treatment with intermaxillary fixation associated to posterior physiotherapy compared with the open reduction and internal fixation (ORIF) have produced similar results with at least 6 months of postoperative control. 2
The closed treatment consists of 10 to 14 days of intermaxillary immobilization, usually with arch bars. 2,3 Satisfactory results are achieved with this modality, however, poor results have been observed mainly in the subcondylar fractures. Malocclusion, reduced facial height, asymmetry, chronic pain and reduction in mobility have been reported in cases in which the treatment is not successful. 3
The ORIF allows anatomical repositioning and immediate functional movements of the mandible. By contrast, visible cutaneous scar, damage to branches of the facial nerve and other noble structures as the parotid gland are potential complications. 4
Usually the MCF are exposed by the retromandibular incisions which may increase the rates of parotid gland fistulae (PGF) and facial nerve (FN) palsy, due to the deeper dissection plane, closely to the main branches of the FN. 5 –7
The aim of this technical note is to present novel technique for the approach to the subcondylar fractures using preauricular incision with transmasseteric dissection.
Surgical Technique
This present technical note proposes the preauricular approach with transmasseteric dissection (PATD) to expose the subcondylar/ramus area. PATD consists in and traditional preauricular incision with gentle lower dissection thought the superficial musculoaponeurotic system (SMAS), the parotid gland capsule its gently retracted, allowing the anterior border of the glandular tissue to be visualized. The masseteric fascia and facial nerve branches are exposed and retracted. The Parotid gland dissection plane is outlined and is pulled posteriorly. The masseteric fascia and the masseteric muscle are partially incised, in the posterior border, to expose the periosteum. The periosteum is dissected superiorly to expose the mandibular notch and the subcondylar area, see Figure 1.
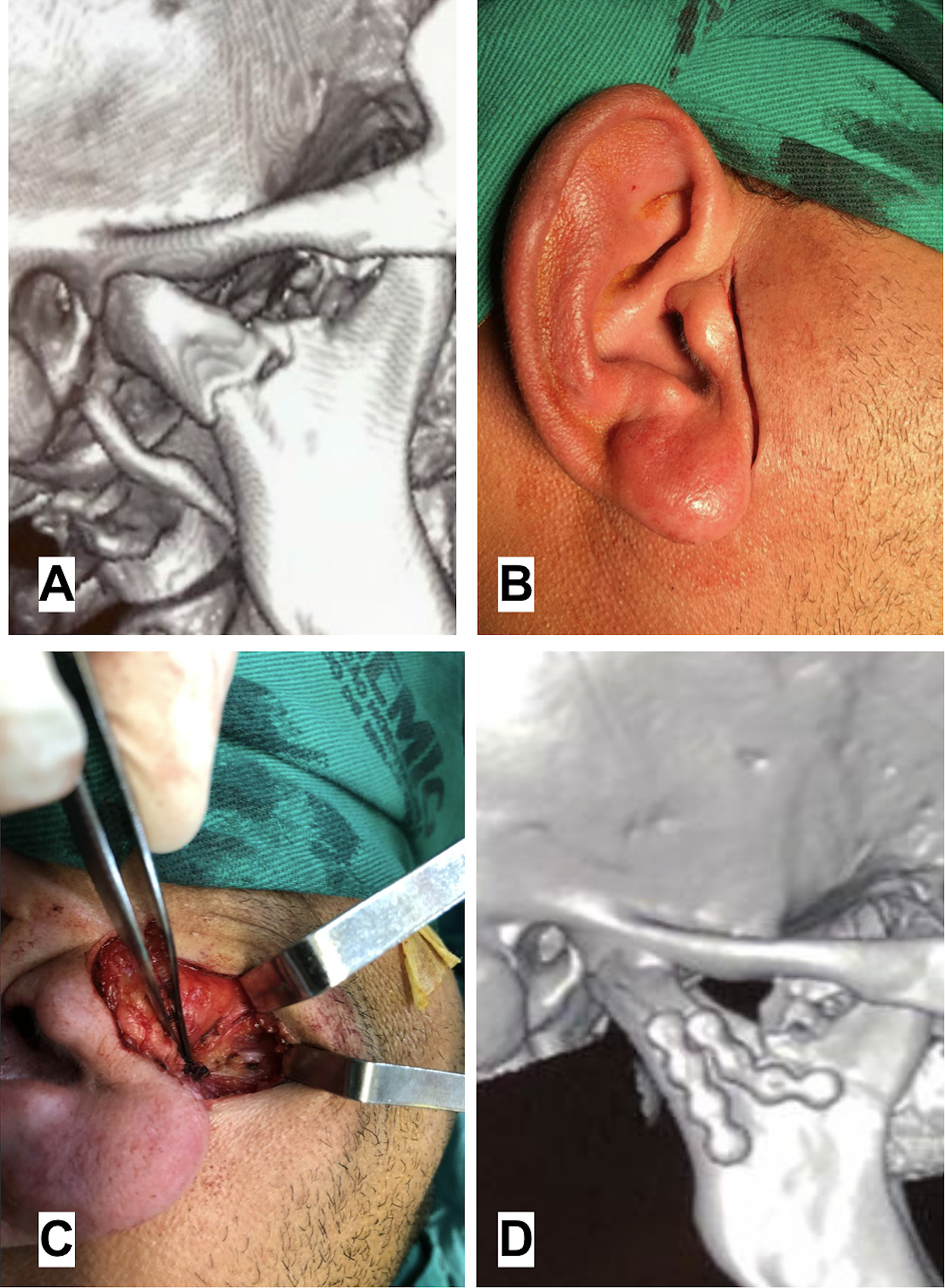
A, 3D-computed tomography demonstrating the mandibular subcondylar fracture. B, Trans operative image showing the preauricular incision. C, Trans operative image demonstrating the transmasseteric dissection with the facial nerve preserved and retracted. D, Postoperative 3D- computed tomography revealing satisfactory reduction and fixation of the condylar fracture.
The approach closing technique is performed as the usual preauricular approach.
Patient and Methods
Study Design
This is a technical note to present a novel approach for the exposure of the mandibular condyle fractures.
First Care
All patients with facial trauma were admitted as preconized for the most advanced trauma protocols in a Level 1 Trauma Center in Brazil. After initial stabilization, the patients went to an image protocol, using Computed Tomography (CT Scan). With the confirmation of the subcondylar fracture, the patients were directed to the surgical room for the correction of the fracture. All the procedures were performed in the shortest possible time since the trauma.
Aftercare and Follow-up
All the patients received complete aftercare. The use of intermaxillary fixation with rubber rings was not preconized, and the patient received occlusal guide elastics only if necessary. The patient was guided to receive soft and liquid diet for 21 days, having its consistency gradually elevated after this time. Early physiotherapy was preconized after 21 days of postoperative time.
All the patients were followed-up for 7, 15, 30, 60, 90 and 180 days.
Results
The novel approach was performed in 8 patients, 6 males (75%) and 2 females (25%), the age varied between 19 and 60 years old, with an average of 34.37 years.
The condyle fracture in association with midfacial segments was the most common diagnose, together with the condyle fracture in association with symphysis fractures, both with 37.5%. Isolated condyle fractures and comminuted ones were less representative with 12.5% each.
The average time for surgical intervention was 2.57 days, however only 1 patient was not operated in the same day of the trauma.
On the postoperative care outcomes the parotid gland salivary fistulae was observed in only 12.5% of the patients, versus 87.5% of the patients presenting no fistulae. The transient facial nerve palsy, in the first 7 days, was observed in 37.5% of the cases, 62.5% of the patients had no palsy in the first week of the postoperative time. None of the patients presented definitive facial nerve palsy.
Discussion
The treatment of condylar fractures has been controversial among maxillofacial surgeons since the development of procedures that uses titanium bone plates and screws. This paper proposes a novel approach for the management of the high and low parts of the condylar neck fractures in the same approach prioritizing less invasive and more aesthetic incision as the preauricular one, see Figure 2.
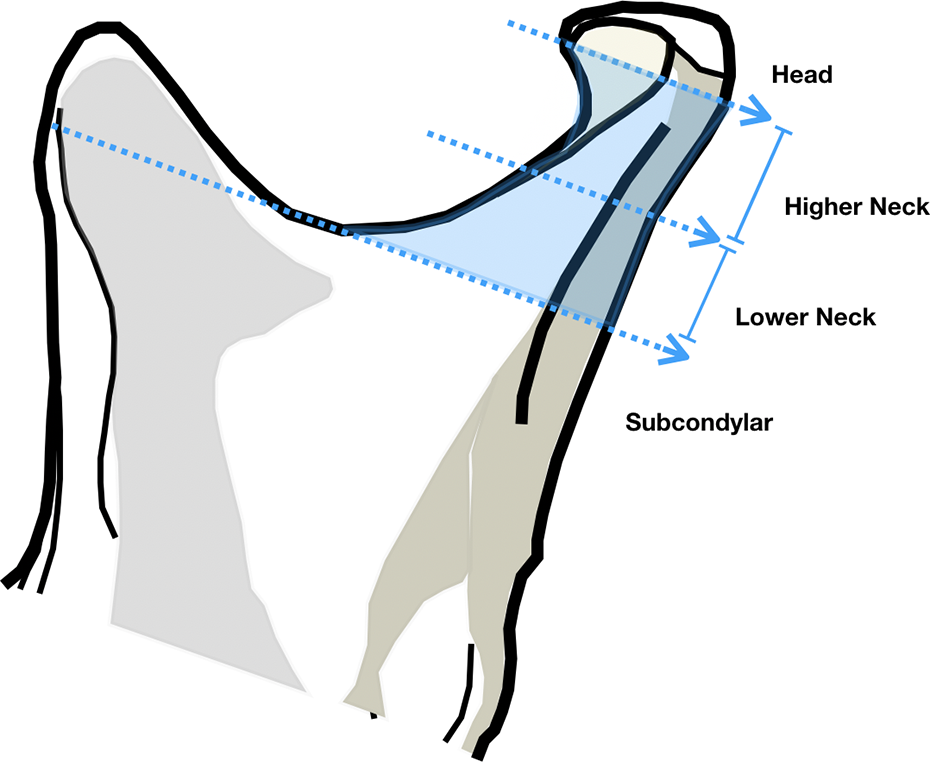
Classification of condylar fractures according to the comprehensive AOCMF classification system.
The patients were surgically managed in the acute trauma, mostly in the same day of the trauma by the Oral and Maxillofacial Surgery Team of ta Brazilian Level 1 Trauma Hospital.
Usually the MCF are exposed by the retromandibular incisions which may increase the rates of parotid gland fistulae (PGF) and facial nerve (FN) palsy, due to the deeper dissection plane, closely to the main branches of the FN. 5 –7 Together with that, it is well described in the literature the relation between small incisions and an increased risk for FN Palsy. 5 –7
We report in this technical note a reliable, simple and versatile approach for the treatment of subcondylar fractures. Small incisions are related with greater chance of Facial Nerve palsy, however the retromandibular incisions are usually transparotid, which may increase the rates of Parotid gland fistulae and VII cranial nerve palsy, due to the deeper dissection plane, closely to the main branches of the nerve. The transmasseteric dissection plane that is preconized in this case series, is considered the one with the lowest rate of nerve damage. 5 –7 A prospective clinical comparative study published by Ramaraj described the minor relation between the transmasseteric route and parotid gland fistulae if compared with the transparotid route. 8
Our proposed incision and approach, although small, preserves the gland capsule and the facial nerve branches are visualized and dissected only in the terminal parts, after the parotid gland. In our experience with this approach, no persistent paralysis was observed, as observed in other similar studies. 9,10
The contra-indications or limitations of this technique are the comminuted fractures and the fractures associated with the posterior border of the mandibular ramus. Together with that, some operational and technical features should be considered when choosing for this approach. The swelling is a complicating factor, as the tissues are distended and the local anatomy may be altered locally. Other point to be considered is the no parotid lesions should be presented as the risks for a salivary fistulae may be increased as the parotid gland capsule could not be preserved, in addition the anatomy of the terminal branches of the VII cranial nerve may not be presented as usual.
The preauricular transmasseteric approach is a reliable and versatile option for the exposure of the mandibular condyle, being a safe and aesthetic incision on the management of the subcondylar fractures when well-indicated.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
