Abstract
Background:
Oral squamous cell carcinoma is the main malignancy of the oral cavity; floor of the mouth and the lateral border of the tongue being the most affected sites. This kind of oral neoplasms may require mandibular resection and reconstruction. Treatment options for such mandibular defects include bone grafts, free flaps, and reconstruction plates. Today, the commonly used treatment method is vascularized fibula flaps due to its many advantages when compared to other methods. However, it is a complex procedure and demands much of both practitioners and the patient.
Case Presentation:
In this report, we present a case of oral squamous cell carcinoma of the gingiva of the mandible which was treated with a partial mandibulectomy and resection. Because of the patients age and fragility an immediate mandibular reconstruction with a pre-shaped reconstruction plate, without hard or soft tissue transfer, was performed. Yearly controls showed pleasing results both aesthetically and functionally and the patient showed no plate-related complications up until the patient’s death, 9 years later.
Conclusion:
With this case, we would like to illustrate that using reconstruction plates only may be a viable option in selected cases for continuity defects of the mandible, specifically in fragile patients less suitable for more demanding surgical interventions.
Introduction
The most common oral neoplasm in the oral cavity is oral squamous cell carcinoma (OSCC). Usually, affected sites are the floor of the mouth and the lateral border of the tongue. 1,2 Multidisciplinary management is essential when dealing with OSCC to ensure that the most appropriate and suitable treatment options are generated individually for each cancer patient. 3 Treatment of this kind of neoplasm in the oral cavity may include a mandibular resection.
Repairing mandibular defects is a challenging task. Treatment options for reconstruction of such defects consist of non-vascularized bone grafts, microvascular free flaps, and alloplastic titanium reconstruction plates. 4 Potential osseous donor sites such as the iliac crest, radial forearm, fibula and scapula have been used in mandibular defect reconstruction. 5 The use of vascularized fibula flaps has been the gold standard after mandibular resection for quite some time. Its many advantages include lower donor site morbidity, having wide vessel diameter and allowing several osteotomies because of its blood supply anatomy, having a long pedicle which allows obtaining a sufficient amount of bone as well as having the ability to combine with skin flaps and incorporate the skin paddle. 4,5
Since the 1980s, alternative methods such as the use of alloplastic devices, rigid mandibular reconstruction plates, with simultaneous or subsequent bone grafting for restoring mandibular continuity following a partial or total mandibulectomy, has been developed. 3,6 –9
The use of alloplastic devices in combination with proper soft tissue repair has enabled acceptable restoration of the mandibular tumor defects. Because of the necessity for secondary bone reconstruction to be able to restore masticatory and dental function, these repairs were limited. While lateral defects showed acceptable results, anterior defects proved more complex to repair and complications such as plate fracture and exposure led to less desirable results. Although the usage of alloplastic material has decreased due to the development of surgical technologies, they still are needed in bone flaps for stabilization to achieve function and anatomic position. 10
In this paper we report a case of OSCC of the gingiva of the mandible which was treated with a partial mandibulectomy and resection of the tumor on the same side. At our institution, free fibula flaps have been the norm. However, in this case an immediate mandibular reconstruction with a pre-shaped reconstruction plate, without hard or soft tissue transfer, was decided the treatment method of choice. We present the long-drawn clinical manifestations and follow ups of the case as well as discuss the possible advantages seen with todays’ generation available plates.
Case Report
In December 2010, an 86-year old woman was referred to the department of Plastic & Oral and Maxillofacial surgery at Uppsala University Hospital from her general dental practitioner with a history of long-term pain of the lower left jaw after a tooth extraction 6 months prior. The patient was a non-user of alcohol and tobacco with a history of hypertension and age-related hearing and vision impairment.
The clinical examination showed gingival overgrowth with a bulbous, sharply marked erythematous appearance (Figure 1). Radiography and computed tomography revealed bone involvement from region 34 to 37 (Figures 2 and 3). The lesion also showed an intraosseous structure, with the tumor located more on the alveolar crest without extending to the floor of the mouth or the buccal soft tissues. An incisional biopsy with histopathological examination from the gingival overgrowth was done, and the histopathological analysis indicated presence of OSCC (T4aN0M0).
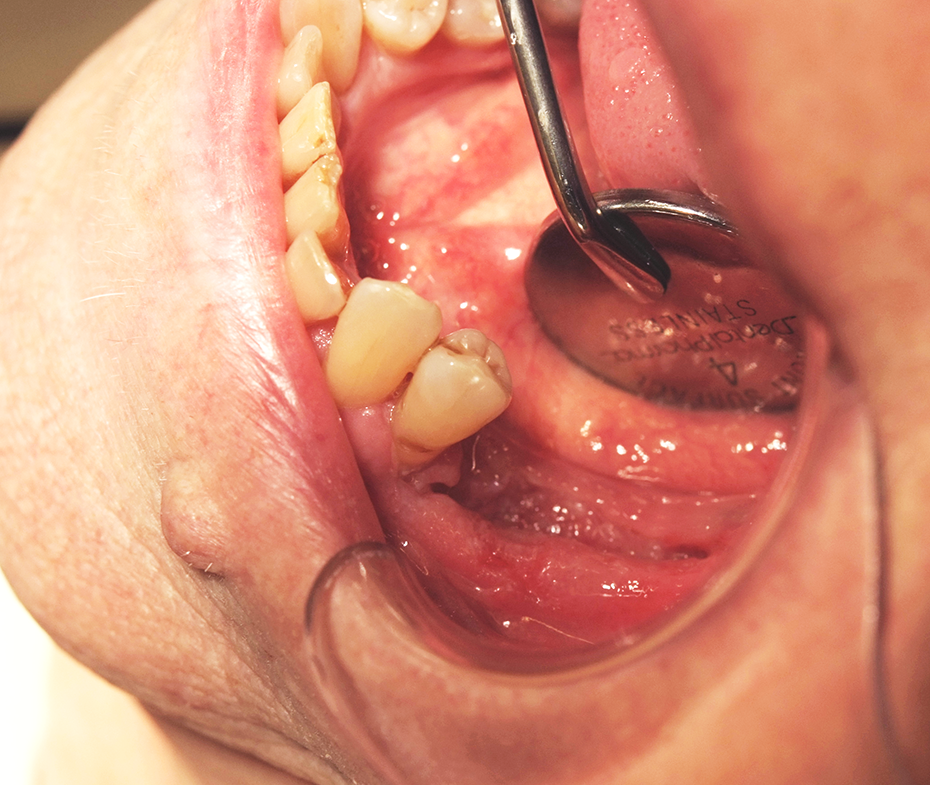
Squamous cell carcinoma of gingiva and bone in the left mandible.
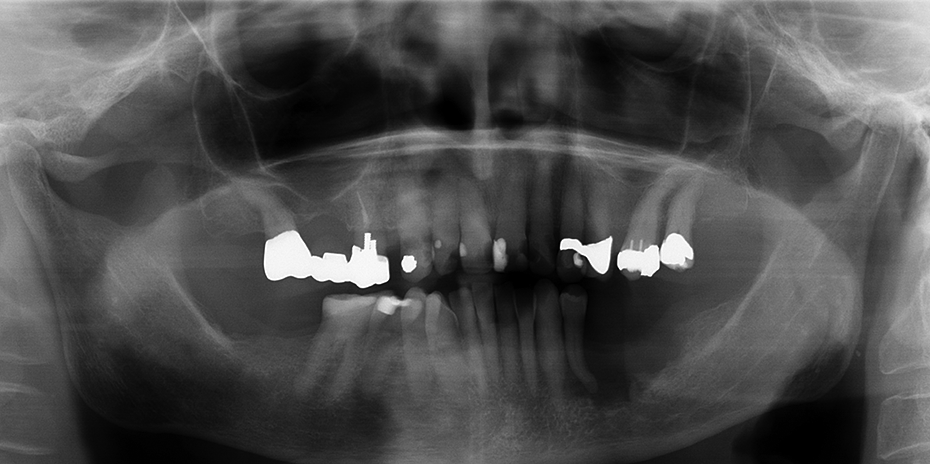
Panoramic view of the case.
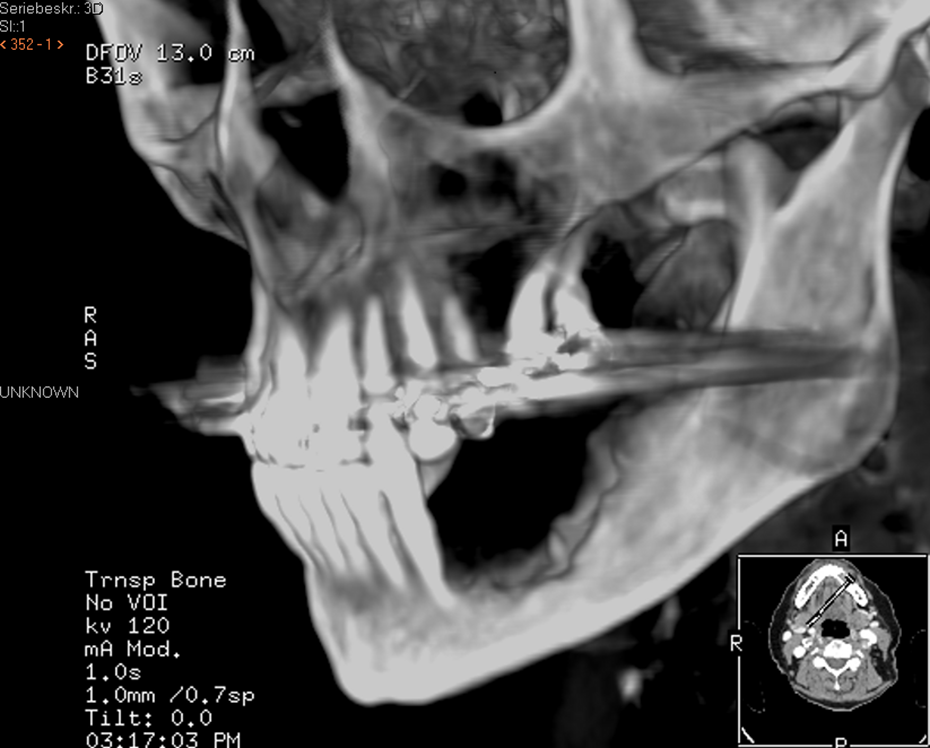
CT imaging reveals deep bony resorption from the lesion.
In January 2011, the patient underwent a left sided partial mandibulectomy with resection of the tumor. Immediate reconstruction was performed using the small 2.5 mm thick, titanium MatrixMANDIBLE preformed locking Reconstruction Plate (©Synthes) with 2.4 mm locking screws (Figure 4A and Figure 4B), which is said to present the advantage of better stability and adaptation post-operatively compared to a non-locking plate. 11
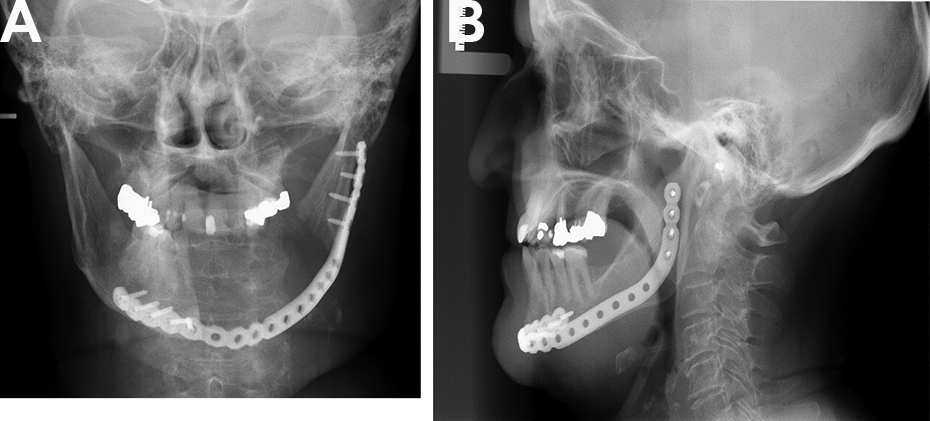
Good restoration of contour with a locking prefabricated/bent plate and (A and B).
In our patient, soft tissue adaptation was accomplished for coverage of the plate from the floor of the mouth and cheek. No pectoralis major myocutaneous flap 12 or free tissue transfer to cover the intraoral defect was planned nor needed. This since the patient was deemed unsuitable to tolerate extended procedures for microvascular reconstruction. For this high-risk patient, a more simplified closure with a reconstruction plate was the most logical option.
Despite minimized surgical time and exposure, the patient developed anemia post-operatively with myocardial infarction and was transferred to cardiac intensive care. The patient suffered a subsequent reduction in overall health. Along with the patients age and inherent risk of further complications, this confirmed the patient’s unsuitability for further reconstruction using non-vascularized bone grafts or vascularized free flaps.
No further treatment with radiation therapy was planned post-operatively, and the patient was referred to prosthodontics for dental rehabilitation and construction of an individually designed partial denture (Figure 5).
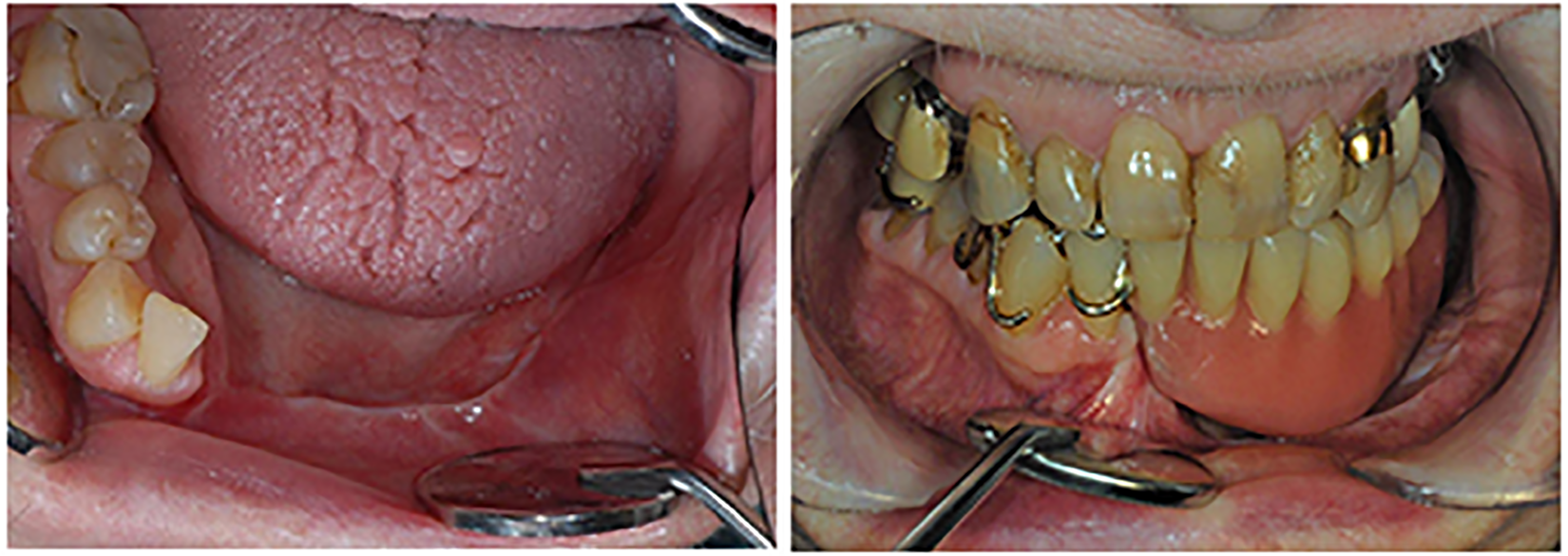
Good healing was achieved and thereafter the subject was closely monitored.).
During a follow-up examination in 2012, an ulcer was seen in the vestibulum, close to the area of surgery. Biopsies verified relapse of cancer in the area and the patient received surgical treatment with radical excision without any signs of plate exposure. Since then, yearly controls were made, and no signs of relapse or infection could be seen.
In 2019, 9 years’ post-reconstruction with plate and close prosthodontic monitoring, the results were both functionally and aesthetically pleasing. Patient complaints included inability to close lips due to retention of the lower lip and a tendency to bite the upper lip. Besides these, there were no major complications or complaints and the follow-up with an orthopantomography showed satisfying results without pathology at the plate site (Figure 6).
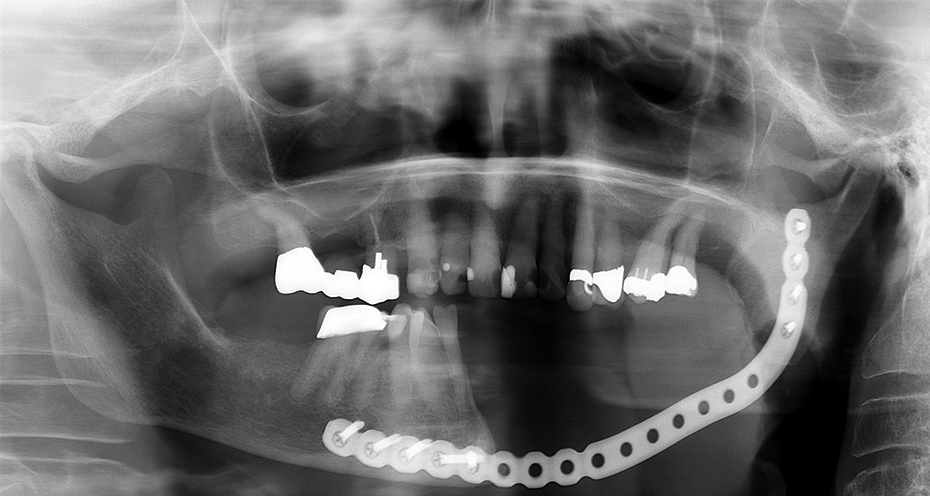
A stable situation was established until the patient passed away 9-years post operatively.
The patient passed away in January 2020, at the age of 95 due to circulatory failure.
Discussion
OSCC accounts for the main malignancy of the oral cavity, comprising 95% of cases, representing the sixth most common cancer worldwide. Squamous cell carcinoma (SCC) of the gingiva is less common than SCC lesions occurring on the buccal mucosa, the tongue and floor of the mouth. Gingival SCC can usually be seen in the premolar and molar region in edentulous areas, and the lower jaw is more commonly affected than the upper jaw. 13 Regardless of location, tobacco use and alcohol consumption are well-known risk factors in developing SCC. 14
Treatment of such tumors and cancers in the oral cavity can alter mastication, due to mandibular resection and displacement of the tongue. In turn, this can cause dysfunction with speech, chewing and swallowing. 6 Mandibular reconstruction should provide restoration of these dysfunctions, leading to optimal functional and aesthetical results that can post-operatively improve the patient’s quality of life. 15,16 This can be provided by restoring the continuity of the mandibular arch, establishing arch form, width, alveolar height, maintaining and restoring internal/external soft tissue coverage, eliminate occurrences of fistulas and provide a basis for future dental rehabilitation. 7,9
Even with the surgical advances, reconstruction entails sacrificing both aesthetic and functional organs, 17 which further demonstrates the importance of choosing a fitting treatment. For decades the use of free fibular flaps for mandibular reconstruction of larger defects has been the method of choice. 18 This due to the relative ease of harvest, bone availability, versatility of the tissue and potential use of the lateral cutaneous nerve at the graft area. 16
For reconstruction of mandibular defects up to 5 to 6 cm, non-vascularized bone grafts such as the iliac crest have been discussed. Although the suitable size to achieve satisfactory results remains unclear, the success rate decreases when dealing with larger defects, due to the non-vascularized nature of the graft. Non-vascularized bone grafts as a treatment alternative are excluded if there is a lack of soft tissue. Studies have shown that the success rate decreases with irradiated patients. To optimize results when using non-vascularized bone grafts with this patient group, combining adjunctive treatment with Hyperbaric oxygen therapy has been suggested. Improvements have been seen in the wound healing and bone regeneration process, by reducing inflammatory damages, decreasing tissue edema, and regulating vascular permeability. 19
A comparison between vascularized bone flaps and non-vascularized bone grafts showed that even when taking age, defect size and irradiation into consideration, vascularized bone flaps outperformed non-vascularized bone grafts when analyzing bony union, the number of required operations for bony union, and implant success rate. In essence, vascularized bone flaps can generally be considered a preferable option in most cases. With smaller defect sizes (<5–6 cm), nonirradiated tissue and fragile patients, non-vascularized bone grafts were considered more suitable. 20
In addition to microvascular free flaps and non-vascularized bone grafts, the use of reconstruction plates is an established method for bridging defects of the mandible. Since the commercial introduction of plates in the 1970’s, they have replaced previous techniques and wire applications. 21,22 These days, titanium plates are commonly used because of their inherent biocompatibility, low density and high strength when compared to the original steel plates. 23 The purpose of using these rigid plates is to bridge the defect, while stabilizing involved segments and maintaining occlusion and contour of the face. 24 A favorable feature of the modern plate types is the locking screw, which minimizes compression between the plate itself and the underlying bone, thereby enabling a more optimized vascularization. 25 Furthermore, locking plates are significantly less likely to be associated with complications when compared to non-locking plates. 26
Commonly found complications include wound dehiscence with exposure of the plate, loosening or breaking of screws, plate fractures, occlusal issues, and unsatisfactory face contour results. These complications are further facilitated by radiation therapy and the location of the resection; crossing the midline of the mandible significantly increases complication risk and thereby the risk for revision or removal of the plate. 27 Other risk factors include re-emergence of tumor and malnutrition. 10,28 A naturally associated issue with reconstruction plates is post-operative imaging and radiation treatment. Plates cause diagnostic problems with radiography and computed tomography (CT) scans, while equally affecting radiation treatment. With regard to magnetic resonance imaging, titanium plates have proven to cause the least number of artifacts in comparison with reconstruction plates of other materials. 29
Another risk-factor is manual bending of the plate to better match the underlying bone of the stumps. This method has been questioned, due to the stress caused in the plates themselves. Especially so in the symphysis and the mandibular angle—areas already prone to fracture during load. 24,30 Because of the strenuous bending process when dealing with the conventional reconstruction plates, the preformed reconstruction plates were developed. These plates have the advantage of reducing surgery time, plate-related biomechanical stress and decreasing the risk of fatigue fractures. With these plates, the known complications of plate exposure and fracture, screw loosening and extra- and intra-oral fistula formation were addressed by a load bearing, pre-shaped osteosynthesis system specifically for the anterolateral part of the mandible. This osteosynthesis system was developed using a 3D morphometric mandible shape analysis based on roughly 2000 CT scans in various adult populations. Even though both the design and material of these plates have improved over time, complication rates have not reduced greatly. For a long-term successful rehabilitation, enough soft tissue coverage is still of the utmost significance. 31
When exploring treatment methods for mandibular reconstruction with plates, biological factors, alcohol and tobacco consumption and radiotherapy should be considered. The outcome of treatment can be more correctly assessed when considering these factors. 1,32 The use of reconstruction plates is associated with a high risk of plate-related fractures, plate exposure and screw fracture, 33 –35 although plate exposure has been tied to both the type of soft tissue flap and radiotherapy. 36 Plate only reconstruction, lateral defects and post-operative dentition is strongly associated with plate fractures. 37 Furthermore, a fibula flap transfer usually shows greater stability over time when compared to reconstruction plates, 38 with favorable aesthetic and functional results. 35 For the average patient, a fibula free flap is still optimal.
However, in more fragile patients, reconstruction plates have their perks. They show a high success rate in general, despite the number of complications. 39 The procedure is less invasive and thus, less technically demanding and time consuming, while showing fewer intraoperative complications, which for these patient groups means less risk of severe complications and morbidity. 16 It also provides immediate mechanical stability. 38 The risk of complications mainly appears to be tied to post-operative dentition, post-operative radiation therapy and dental rehabilitation. Close post-operative maintenance of the occlusal relationship and the surrounding tissues can decrease the risk for complications, 34,35 and the same appears to be true for customized plates when compared to the ready-made type. 40 Our presented case was closely monitored, and this strategy proved to work life-long.
Patient-specific plates using 3D printing technology have been developed to negate the disadvantages of conventional plates. The design of such 3D-printed plates is based on the patients imaging data and therefore it fits precisely to the bone contour, reducing surgery time and improving the accuracy of the operation without the need of any adaptation and bending and often leads to a better surgical outcome. 41 –47 There are several methods to create individualized devices for a specific patient, including patient-specific reconstruction plates, cutting guides and meshes for harboring eventual bone graft or bone substitutes. 48 Technologies such as computer-aided designing and computer-aided manufacturing (CAD-CAM), selective laser sintering (SLS) and electron beam melting (EBM) have been described and used. 49 With these surgical guides the accuracy of the site of osteotomy and position of the screw holes can be improved. This will simplify the intraoperative procedure as well as contribute to planned outcomes. 41 Generally, due to the complex nature of oncological surgery, involving bone, mucosa as well as muscle, with the preparations needed to minimize the risk of plate-related complications, extensive planning must be made before procedure. 34
With presenting this case, we argue that reconstruction plates could be considered when deciding the treatment method. While usage of plates for mandibular reconstruction has been criticized, 33 it might be better suited for certain patients because of its immediate availability, reduced surgery time and the lack of need for previous planning. Namely, more fragile patients, edentulous patients and those without any planned dental rehabilitation. 50,51 All things considered, patients have not reported any significant differences in quality of life when comparing those who were treated with reconstruction plates and those treated with flaps. 6,52 Although the nature of complications naturally differs between the 2 groups, the frequency of complications appears to be equal. 32,53
Conclusion
Considering reconstruction plates only, may be a viable and potentially optimal solution in selected cases for continuity defects of the mandible instead of having to choose between vascularized bone flaps, with the elevated risk of health complications, and non-vascularized bone grafts with a lower success rate, specifically, in fragile patients less suitable for more demanding surgical interventions.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed Patient Consent
The authors can certify that they have obtained all appropriate patient consent forms. In the form the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published, and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
