Abstract
Introduction:
Orbital roof fractures are uncommon and normally associated with high energy trauma in which multiple other injuries are present. Most can be managed non-operatively with close observation. However, in a small proportion the defect is such that it permits the development of a meningoencephalocele, which can cause exophthalmos, a reduction in visual acuity and pain, all of which are unlikely to improve without surgical treatment. In light of their scarcity and the potential of serious risks with surgery that includes meningitis and visual disturbance (or even loss), thorough planning is required so that the meningoencephalocele can be reduced safely and the orbital roof adequately reconstructed.
Methods:
We report a case of a patient with a frontal bone defect, orbital roof fracture and associated meningoencephalocele that presented years after being involved in a road traffic accident in another country, who complained of a significant headache and orbital pain. The use of 3D modeling to help plan the surgery, and intraoperative 3D navigation to help negotiate the anterior skull base are described along with the reconstruction of the frontal bone and orbital roof using titanium mesh contoured on the 3D model.
Conclusions:
Although conservative management of orbital roof fractures predominates; those that are symptomatic, have associated neurologic symptoms or pose a risk to the eyesight warrant a surgical approach. The methods of repair, which center around separating the intracranial and intraorbital contents, are described in the context of this patient and previous cases, and a treatment algorithm is proposed.
Keywords
Introduction
Fractures of the orbital roof are unusual given the protection offered by the supraorbital bar, accounting for less than 10% of all orbital fractures. 1,2 A traumatic encephalocele that complicates the fracture site, which was first described in 1949, 3 is even rarer with only 24 case reports published in the English-speaking literature to date. 3 –26 The majority of these were in the pediatric population as the added protective layer of a pneumatized frontal sinus is not yet developed.
Most orbital roof fractures can be managed non-operatively if asymptomatic and minimally displaced, 11 but exophthalmos, particularly if it is pulsatile or expanding, is a potential sign of a meningoencephalocele and may be associated with a reduction in visual acuity. 8,10 If this is the case then some form of operative intervention is required to salvage the vision, but treatment strategies are disparate. Furthermore, if there is a concomitant cerebrospinal fluid (CSF) leak secondary to a dural tear, then the risk of meningitis is increased and the need for surgery is reinforced. However, the orbital roof forms part of the anterior skull base and so should be navigated with caution, and with the assistance of Neurosurgical colleagues. Not all traumatic orbital meningoencephaloceles are the same, but rather lie on a spectrum, hence their symptomatology can vary. Larger, symptomatic ones tend to present acutely, others develop more insidiously and some present years after the traumatic event, even as an incidental finding. 4,6,8,17 As such, standardizing treatment is very difficult.
Since individual surgeons will have little experience of operating on these injuries, and the risks of meningitis and visual loss, although low, have the potential to be devastating, comprehensive preoperative planning and in-depth discussion with the patient are essential. We describe a patient with a delayed presentation of a combined post-traumatic frontal bone and orbital roof fracture with an associated meningoencephalocele managed using a combination of 3D modeling and 3D navigation and review the literature to inform future treatment of these injuries.
Methods
A 26-year-old male presented to the Oral and Maxillofacial department of the University Hospital of Basel after sustaining an injury to the left frontal bone and orbital roof, with an overlying soft tissue wound, due to a road traffic accident a number of years previously in another country. At the time of the injury, the soft tissue injury was superficially debrided and closed primarily by the General Surgeons, after which he was monitored on the Intensive Care Unit for 2 weeks, but he had had no other treatment prior to discharge, and was not seen by either the Oral and Maxillofacial nor Neurosurgical teams. His predominant complaint now was of a bilateral chronic frontal headache and associated pain from the left orbit particularly on upward gaze but there was no exophthalmos, enophthalmos, hypoglobus nor visual disturbance.
CT and MRI scans demonstrated a bony defect in the left frontal bone measuring 5 cm horizontally by 3 cm vertically, and a further defect in the ipsilateral orbital roof measuring 3 cm by 2 cm (Figure 1A). In addition, there was a 9 mm meningoencephalocele herniating through the roof defect into the orbit (Figure 1B). Imaging also revealed a rounded 2 cm by 2 cm space occupying parenchymal lesion of the superior part of the left frontal lobe with perifocal gliosis, hemosiderin deposits and fat inclusions, which was given a radiological diagnosis of a foreign body granuloma (Figure 1C).
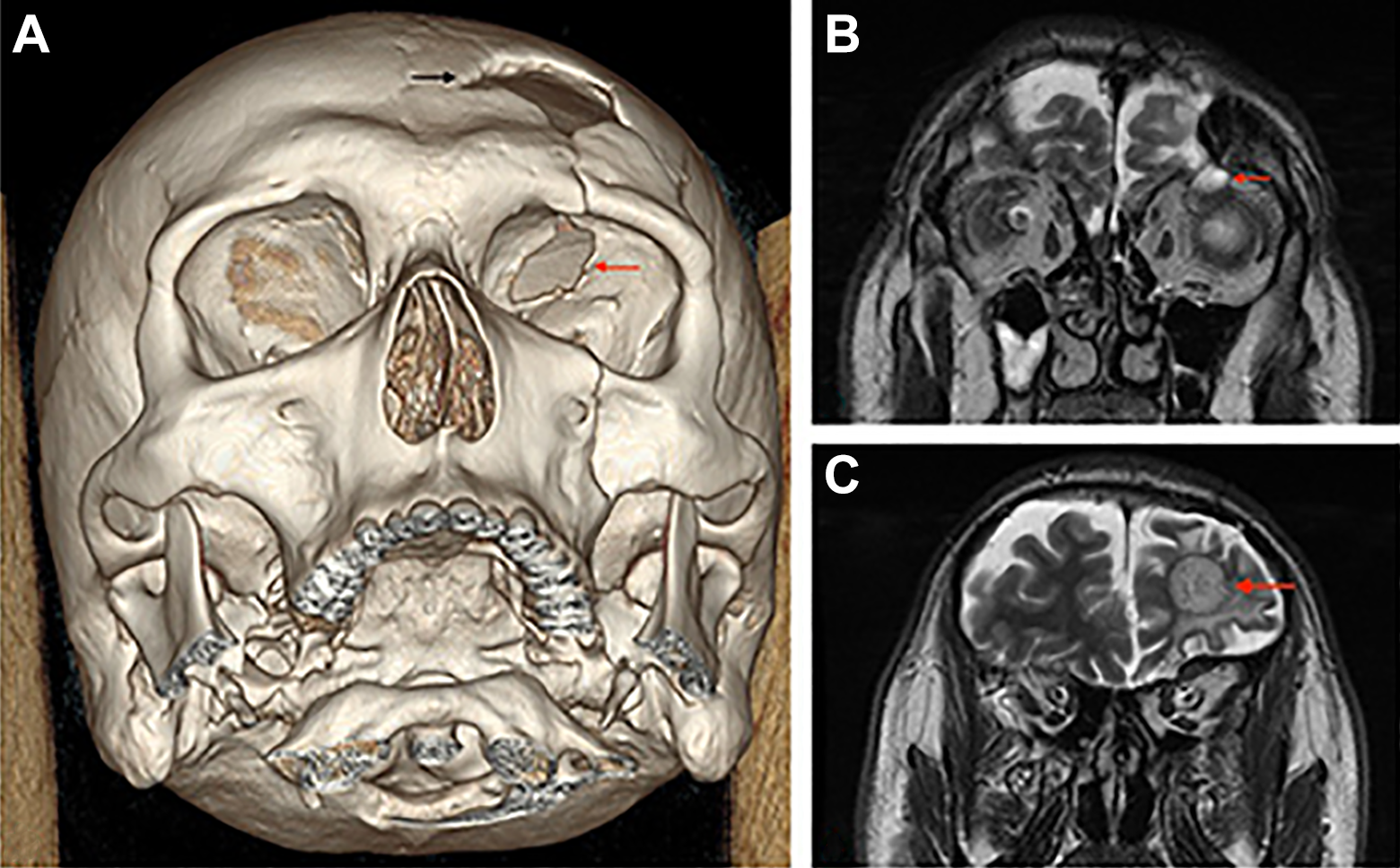
A, 3D reformatted CT scan demonstrating a left frontal (black arrow) and left orbital roof defect (red arrow). B, T2 weighted MRI scan demonstrating a 9 mm frontal meningoencephalocele (arrow) herniating through the left orbital roof fracture defect. C, T2 weighted MRI scan demonstrating a well circumscribed left frontal lesion (arrow).
A 3D model of the frontal area and orbits was made using a MakerBot Replicator+ 3D printer (MakerBot Print v. 4.8, MakerBot Industries, New York, USA) and 1.75 mm polylactic acid (PLA) filament (gray, MakerBot) through segmentation of the DICOM datasets using the Mimics Innovation Suite (v. 22, Materialise, Leuven, Belgium) to demonstrate the defects in the bone and to facilitate reconstruction. The CT and MRI images were uploaded to 3D navigation software (Brainlab GmbH, Munich, Germany).
In a joint procedure with the Neurosurgeons a coronal flap was used to access the fronto-orbital region and the frontal bone defect was expanded through a frontobasal craniotomy using a piezoelectric saw (Figure 2). Under microscopic vision, through an extradural approach, 2 meningoencephaloceles were detected and detached from the bony defects within the orbital roof. Thereafter, the gliotic tissue related to the meningoencephaloceles was coagulated and removed leaving the intracranial tissues separate from those in the orbit. No dural tears or CSF leaks were identified.
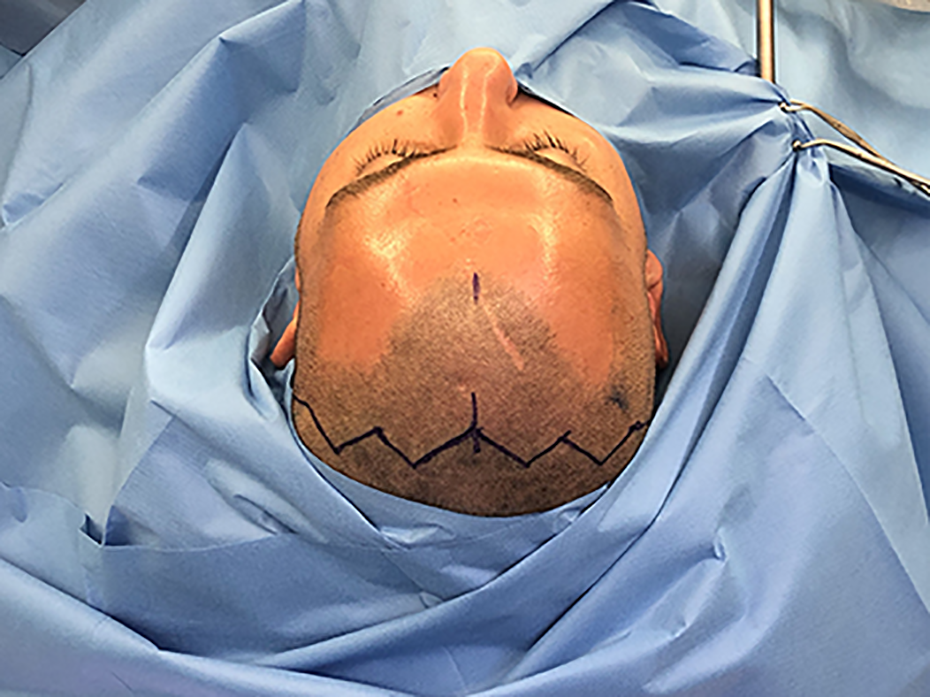
Preoperative on table photograph demonstrating the soft tissue scarring overlying the left frontal bone defect and marking for the coronal incision.
The 3D navigation tool was used to delineate the proximity of the bony defects to the frontal and ethmoidal sinuses as well as the optic canal to ensure that any reconstructive material would not interfere with either. It was also used to navigate to the associated lesion in the left frontal lobe so that it could be explored and completely resected. The lesion appeared to contain connective and inflammatory tissue of mixed density, which was removed and sent for histological analysis. The roof of the orbit was reconstructed using a titanium mesh that was contoured to the dimensions of the 3D model (Figure 3A), and was lined with a pericranial flap, and the frontal bone was reconfigured in a similar fashion (Figure 3B).
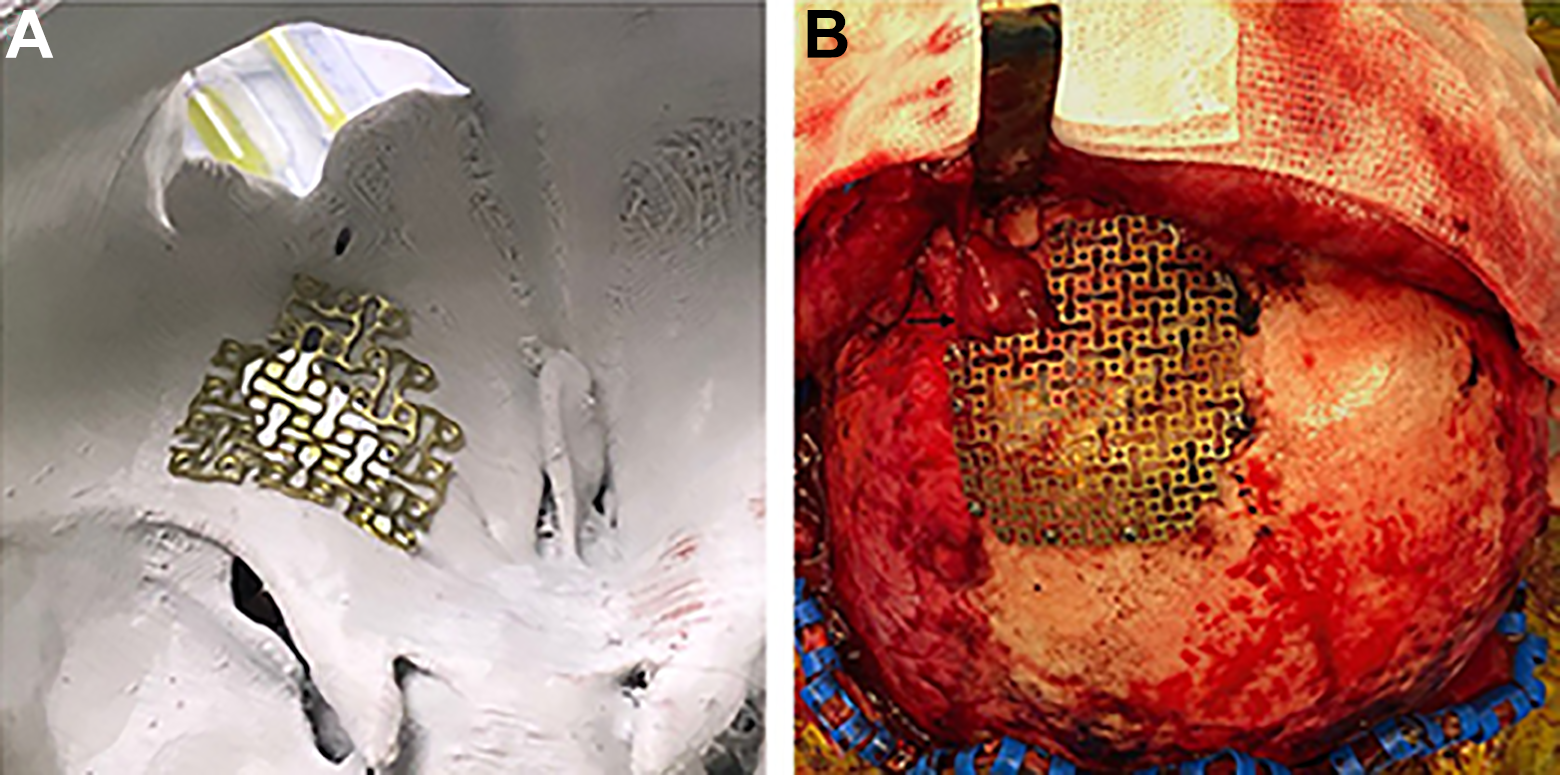
A, 3D model of the fronto-orbital region demonstrating the contoured titanium mesh used to repair the orbital roof. B, Titanium mesh in-situ to cover the defect in the left frontal bone, which had been contoured on the 3D model prior to insertion (the pericranial flap lining [arrow] the orbital roof can be seen entering the skull base at the bottom left of the titanium mesh).
The patient was discharged after 7 days and made a good recovery such that the pain resolved and there was no longer a palpable defect in the forehead, which was now symmetrical (Figure 4). The histology from the tissue removed from the lesion in the frontal lobe showed scarred fibrosed connective tissue with histiocytic and giant cell foreign body reaction around partially birefringent foreign material, which, according to the electronic medical history, was consistent with a post-traumatic frontal lobe foreign body. There were no signs of malignancy, and no further treatment was required.

Postoperative photograph taken at 1 week showing a normal forehead contour.
The present case illustrates the potential sequelae of an untreated fronto-orbital injury, as at the time of injury the fractured bone (and surrounding tissue or debris) from the forehead entered the frontal lobe and became isolated from the surrounding brain parenchyma over time. However, it was the orbit and frontobasal area that were the sources of the patient’s pain and so was likely to originate from the tethered tissue at the orbital roof level. Broadly speaking the pattern of orbital roof fractures are divided into so-called “blow-out” and “blow-in” fractures, which are caused by an increase in intraorbital pressure or an increase in intracranial pressure respectively. 27 Our patient suffered a “blow-in” fracture given the location of the frontal bone defect and high-speed mechanism of injury.
The etiology of the meningoencephalocele was also due to a raised intracranial pressure causing the meninges and brain parenchyma to herniate through a large (3 cm by 2 cm) orbital roof defect; a finding also found by Wei et al, especially where the orbital roof defect exceeded 2 sq cm. 10 Although in our patient the intracranial pressure will have normalized by the time he presented to us, we suspect the meninges and extraconal tissue in the superior orbit were in contact with each other for long enough for them to fuse, leading to tethering and pain. With this is mind, we recommend that any repair of an orbital roof fracture should serve to prevent transmission of intracranial pressure into the orbit and introduce a barrier to separate 1 cavity from another. 15,16
Development of a meningoencephalocele through a traumatic orbital roof defect is not inevitable, but the clinical signs that raise suspicion are progressive pulsatile exophthalmos with evidence of globe or optic nerve compression, while the radiological signs on CT are an enlarging heterogeneous orbital mass with associated widening of the roof fracture segments. 10 Cayli et al suggested a fracture diastasis greater than 2 mm increases the propensity to brain herniation in the pediatric patient population, 16 and the concept of a skull base fracture growing wider as the child grows can explain why some meningoencephaloceles develop years after the initial injury. 6 Although much more unusual this phenomenon has also been described in an adult. 17
To access the orbital roof 2 main approaches are described, the upper eyelid incision and the coronal flap. 10,28,29 Given the need to access the frontal lesion and associated bony defect in this patient, we assessed the coronal flap to be most suitable. In isolated orbital roof fractures, particularly those complicated by a CSF leak requiring dural repair, a craniotomy is required, but in this patient the frontal bony defect served as an access point to deal with both the meningoencephalocele and orbital roof defect simultaneously, even though it had to be enlarged. Sahoo et al accessed the orbital roof through a frontal fracture in an infant with an orbital meningoencephalocele 12 ; and so pre-existing fracture lines should be utilized for access where feasible.
In printing a 3D model, this unique approach to the orbital roof could be checked for feasibility and the surgery simulated preoperatively in conjunction with the Neurosurgeons, such that the operation progressed smoothly. Furthermore, while the Neurosurgeon undertook microscopic dissection of the meningoencephalocele the 3D model was used to cut the titanium mesh to size and contour it to the defect, saving operating room time. We would advocate using a 3D model as a guide in complex fronto-orbital defects such as this in future. Also, the 3D navigation software can be used to check the seating of the titanium mesh, the proximity of the orbital roof defect to the adjacent paranasal sinuses and the location of the optic canal.
Since most orbital roof fractures are asymptomatic few require treatment, but indications for treatment include a CSF leak (due to the risk of meningitis); meningoencephalocele, which may be manifest as pulsatile exophthalmos; intraorbital bone fragments and reduced visual acuity. 4,5,30 We would like to add persistent pain emanating from the orbit, in the absence of any other causes, to this list.
Beyond this there is no consensus on their management. In this patient titanium mesh was used for the repair because it is readily available and osteointegrates. An alternative is a split calvarial bone graft, 5,18 but it is not risk free, is not as malleable as titanium and has a tendency to resorb. By lining the titanium in the orbital roof with pericranium a biological barrier, and therefore seal, was created between the orbit and brain. Zhao et al described a “five-layer gasket seal” to reconstruct the skull base in a patient with bilateral orbital roof fractures and meningoencephaloceles. 4 This may not be necessary in all patients but in cases where the dura has been breached a watertight seal is mandatory. 6,7,10,13 Even though there was no dural tear in our patient, the dura was opened to remove the frontal lesion, and was sealed using a vascularized pericranium flap, gelatin sponge, Tacho-Seal® and fibrin glue, which in our experience seems to be sufficient. 31
In an effort to standardize treatment Connon et al proposed a classification system of orbital roof fractures based on their clinical appearance 27 :
Undisplaced orbital roof fracture
Rim fracture
Roof fracture
Blow-out
Blow-in
Roof and rim fracture
Blow-out
Blow-in
This was further subclassified to include associated facial fractures, neurological injuries, orbital injuries and frontal sinus injuries. In their series of 47 patients, only those with type IV fractures underwent surgical repair, and based on this they introduced a treatment algorithm that reinforced the tendency toward conservative management. Similarly, Ha et al in their treatment algorithm recommended emergent repair when there was attributable neurological or ophthalmologic compromise, but suggested a watch and wait policy otherwise. 5 The presence of a progressive encephalocele causing pulsatile exophthalmos in an orbital roof injury would fall into the category of potential visual impairment, and so in this particular situation surgical repair is advocated. 4,5,10,18 Although treatment of traumatic orbital roof meningoencephaloceles varies from 1 individual to another, there are common themes to the surgical approach employed that are summarized in Table 1, 4 –10,12 –14,17,18 and from which a treatment algorithm modified from those previously reported has been produced (Figure 5). 5,27
Summary of Surgically Managed Orbital Roof Fractures Complicated by a Meningoencephalocele Published Since the Year 2000.
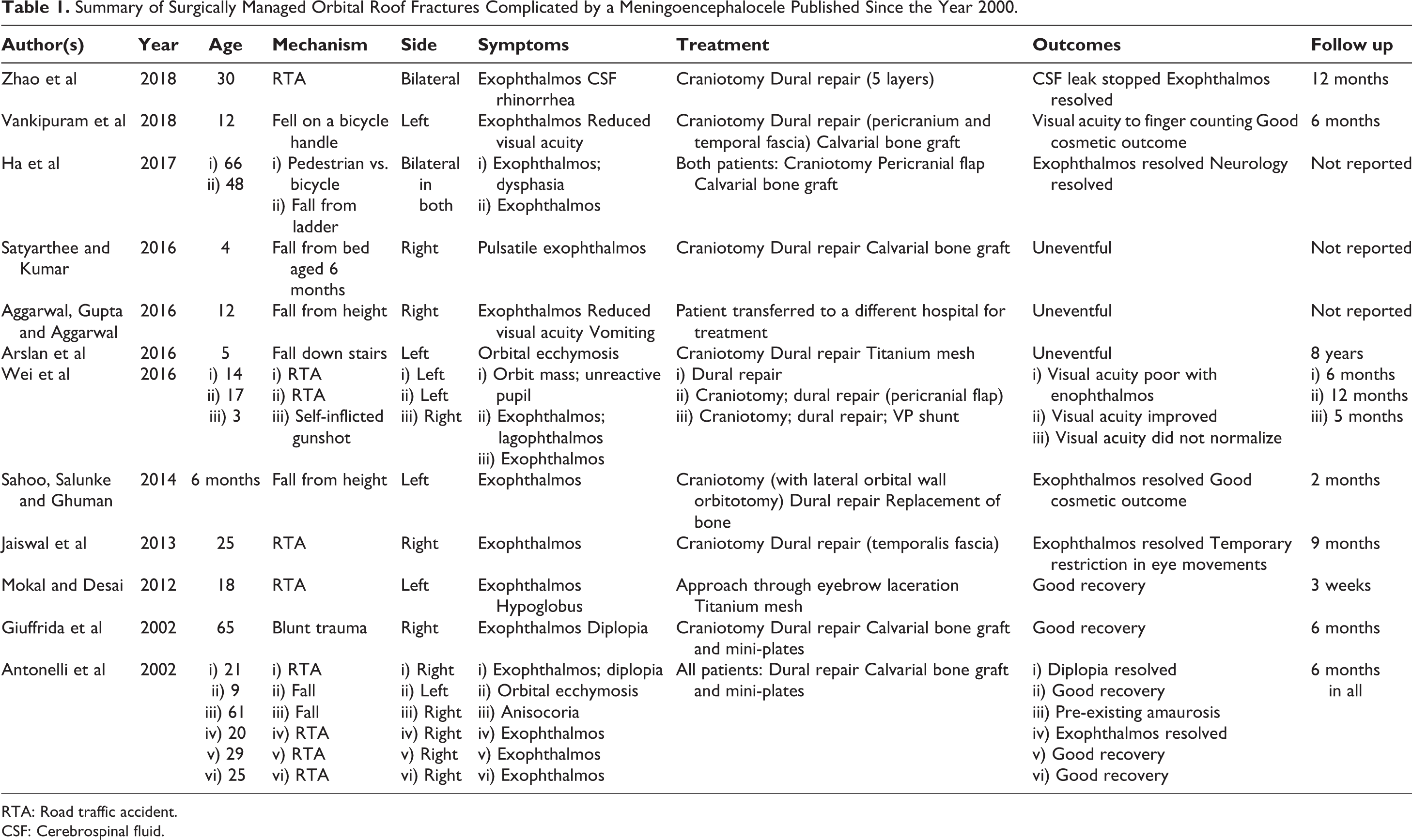
RTA: Road traffic accident.
CSF: Cerebrospinal fluid.
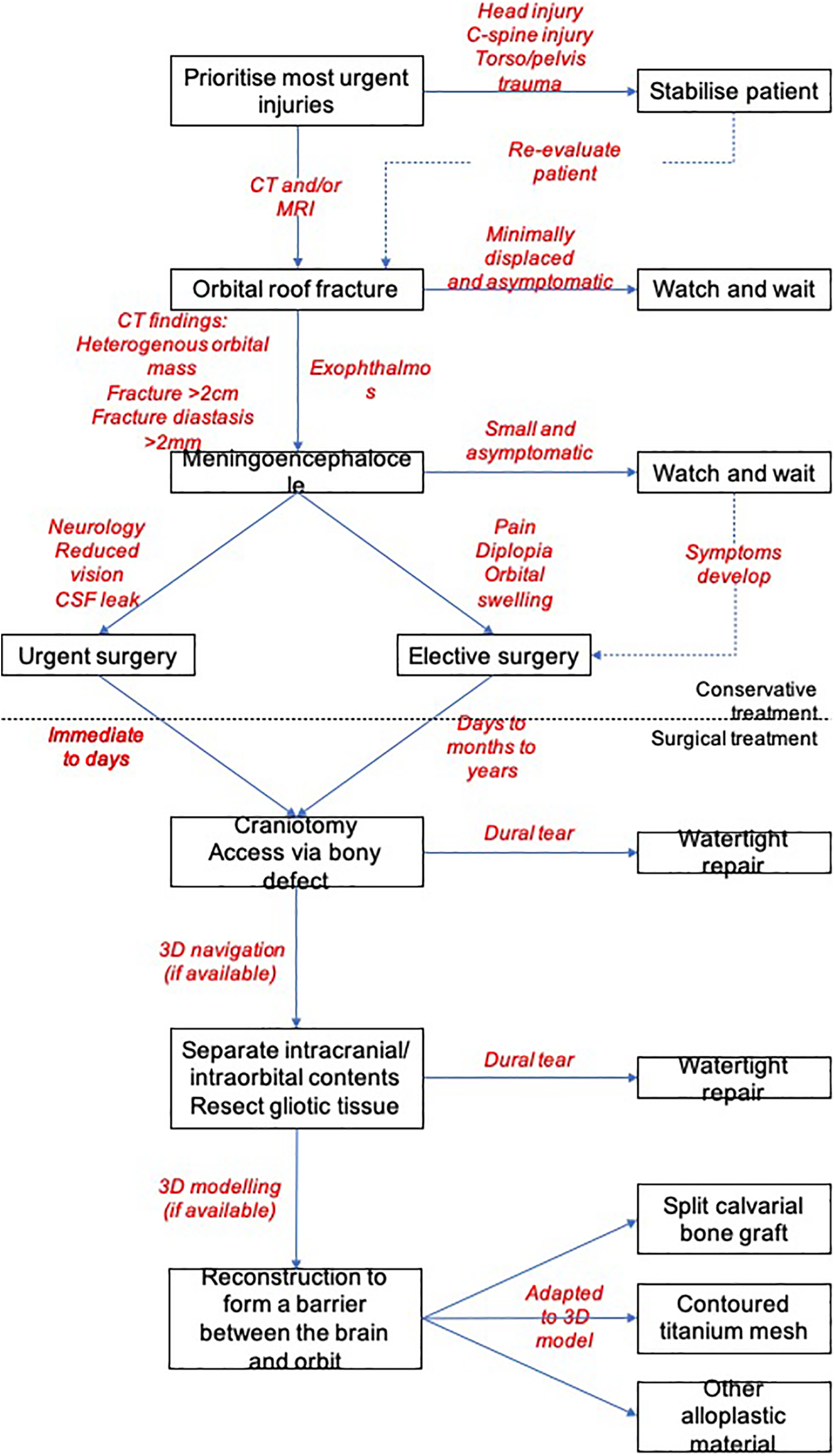
Treatment algorithm for the surgical management of orbital roof fractures complicated by a meningoencephalocele.
Conclusion
Reconstruction of orbital roof fractures requires interdisciplinary management between the Oral and Maxillofacial surgeon and Neurosurgeon, and the Ophthalmologist if there is visual disturbance. The primary aim is to separate the intracranial contents from those in the orbit by inserting a barrier to mitigate the risk of meningitis and in the process alleviate the patient’s symptoms. We recommend using a 3D model and 3D navigation to negotiate these defects as they are rarely uniform and are adjacent to several critical structures. Due to their paucity, standardized treatment approaches are unlikely to be obtainable.
Footnotes
Authors’ Note
Rory C. O’Connor and Sead Abazi are joint first authors.
Acknowledgments
The authors would like to thank Dr. Selina Ackermann for editorial assistance.
Availability of Data and Materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed Consent to Participate
Informed consent was obtained from the patient for case description and photo material.
Informed Consent for Publication
We obtained the patient’s consent for publication.
