Abstract
We present a case of a 69-year-old woman with multiple complicating comorbidities who developed medication-related osteonecrosis of the jaw secondary to extraction of multiple teeth with a history of intravenous bisphosphonate therapy for metastatic breast cancer requiring staged management with segmental mandibulectomy with placement of external pin fixator with subsequent exchange of this device for a titanium reconstruction plate and a submental island pedicled flap for soft tissue coverage of the bridging reconstruction plate. Once the surgical sites were well-healed that patient would immediately return to a satisfactory functional outcome with ability to tolerate a soft diet. Furthermore, the patient did not have complications (ie, cardiac, pulmonary, venous thromboembolism, sepsis, surgical site infection, reoperation) during her hospitalization and has done well with her long-term recovery.
Introduction
The first cases of medication-related osteonecrosis of the jaw (MRONJ) were reported by Marx in 2003 in patients receiving zolendronate (Zometa; Novartis Pharmaceuticals) and pamidronate (Aredia; Novartis Pharmaceuticals). 1 Since then the list of bisphosphonates and other classes of medications implicated with MRONJ has expanded to now include tyrosine kinase inhibitors, immunosuppressants. Today, our understanding of the causes and management of MRONJ continue to evolve, with a myriad of protocols being described for both the nonsurgical and surgical management of MRONJ. Irrespective of the diagnosis in cases requiring a segmental mandibulectomy for the management of MRONJ, the restoration of the integrity of the mandible and the soft tissues of the oral cavity is imperative from a functional and aesthetic perspective. Caldroney and colleagues as well as Hanasono and colleagues have reported on the safety and success of free tissue transfer flaps in the reconstruction of patient undergoing segmental mandibulectomy for MRONJ. 2,3 Nonetheless, not every patient is an ideal candidate for a free tissue transfer flap-based reconstruction. Free tissue transfer flaps could result in increased operative time as well as an increase in the length of intensive care unit stay. 4 Here we present a case of a 69-year-old woman with MRONJ secondary to intravenous bisphosphonate therapy for metastatic breast cancer requiring staged management with segmental mandibulectomy with placement of external pin fixator with subsequent exchange of external pin fixator for a titanium reconstruction plate and a submental island pedicled flap for soft tissue coverage of the plate with the patient subsequently being able to return to a satisfactory functional outcome and without any complications during her hospitalization and long-term recovery.
Case Report
Patient is a 69-year-old woman with a history of type II diabetes mellitus with poor diet compliance and chronic active tobacco smoker who was diagnosed with breast cancer 11 years ago. At that time, her cancer was treated with radiation therapy and chemotherapy, for stage IV breast cancer with bony metastasis to lower extremity and was treated with Zometa for an approximate duration of 8 years. Approximately 1.5 years ago, the patient underwent extraction of multiple mandibular teeth with subsequent development of exposure of mandibular bone 6 months prior to her initial presentation to our surgical unit. The patient on initial assessment was found to have swelling that was erythematous along the chin region that was tender to palpation with exposure of the alveolar bone of the entire symphyseal region of the mandible. On cone beam-computed tomography imaging, the patient was noted to have a pathologic fracture of the mandible (Figure 1). The patient was subsequently admitted to the Oral and Maxillofacial Surgery Service and during her hospitalization underwent segmental mandibulectomy via transoral approach with placement of external pin fixator (DePuy Synthes/Johnson and Johnson). Following resolution of the patient’s acute infection and following completion of her antibiotic regimen per the infectious disease service, the patient was planned for secondary reconstruction. Of note, bony microbial cultures speciated both Rothia and Streptococcus viridans species. Patient was maintained on 6 weeks of metronidazole and ceftriaxone via peripheral inserted central catheter (PICC) line. As the patient was recovering from this operation and was receiving antibiotic therapy via PICC line, she was diagnosed with new spinal metastases requiring palliative radiation therapy.
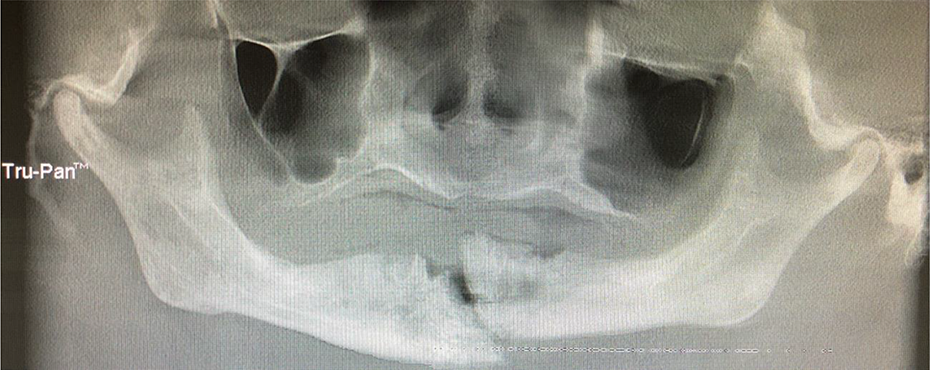
Cone beam-computed tomography panoramic view with lytic process of mandible and associated pathologic fracture.
The patient was a long-standing cigarette smoker and quit leading up to her secondary reconstructive surgery. Furthermore, the patient is wheelchair bound and has a hemoglobin A1c level of 8.4%. During her consultation for surgical reconstruction, the patient was noted to have bilateral lower extremity pitting edema that was 4+. Her body mass index measured 37.51 kg/m2. Utilizing the American College of Surgeons Risk Calculator (https://riskcalculator.facs.org/RiskCalculator/), her risk for a serious complication utilizing a pedicle flap from the head and neck region was 17.7% (average risk = 7.5%) and any complication risk of 21.5% (average risk = 8.9%). Furthermore, in utilizing a distant free tissue transfer flap (ie, fibula free flap, scapula free flap) placed her at a serious complication risk of 43.7% (average risk = 25.6%) and any complication risk of 48.6% (average risk = 26.4%). Therefore, her risk for a serious complication was above average for both a local pedicled flap (ie, submental island pedicled flap) versus a distant free tissue transfer flap (ie, fibula osteocutaneous free flap) but was significantly lower for the pedicled flap versus free tissue transfer flap, 17.7% versus 43.7%, respectively. Based on the above-listed myriad of complicating factors related to her overall performance status and deconditioning, and concern for her lower extremity body habitus that a bone containing flap such as a fibula free in the presence of her pitting edema, the patient would not be an ideal candidate for a fibula free flap-based reconstruction. Additionally, the scapula free flap is another reliable and well-established bony flap option in the reconstruction of segmental mandibulectomy defects; however, due to concerns for the patient’s overall medical frailty as well as the patient being diagnosed with spinal metastasis following segmental mandibulectomy procedure requiring palliative radiation therapy avoidance of a surgery that poses a greater recovery to the patient further reinforced consideration of pedicled flap option. Furthermore, the added surgical time, not allowing for a 2-team approach, inherent to the scapula free flap and skin paddle bulk based on the patient’s body habitus rendered the patient not an ideal candidate for either reconstructive option. Of note, a scapula free flap can be harvested using a 2-team based approach depending on surgeon comfort. The patient has a history of metastatic breast cancer with previous radiation therapy to the breasts, thus a pectoralis major pedicled flap was also not an ideal flap option. Therefore, being that the patient would be undergoing placement of a bridging reconstruction plate via a transcervical approach, a decision was made to utilize a pedicled submental island pedicled flap with incorporation of the mylohyoid muscle. The patient subsequently underwent removal of her external pin fixator and placement of a mandibular reconstruction plate. Prior to making a neck incision, the skin paddle of the submental island pedicled flap was marked out (Figure 2A), and the flap was subsequently elevated (Figure 2B) with incorporation of the mylohyoid muscle using previously described technique by Patel et al. 5 To add bulk circumferentially surrounding the plate, both anterior and posterior portions of the skin paddle were de-epithelialized, and the skin paddle was wrapped around the reconstruction plate and the skin paddle was inset (Figure 2C). The patient’s intraoperative course was uneventful, she was extubated (oral endotracheal tube) in the operating room and transferred to a step-down unit, without need to return to the operation room. Postoperatively, the patient did not require admission to the intensive care unit. Patient was discharged to a rehabilitation facility on postoperative day 8 with an uneventful surgical recovery throughout the hospital stay and did not need any additional surgical intervention. Patient was doing well at her last evaluation 6 months postoperatively and is tolerating a soft mechanical diet with viable flap skin paddle without hardware exposure and with restoration of her facial profile (Figure 3A and B).
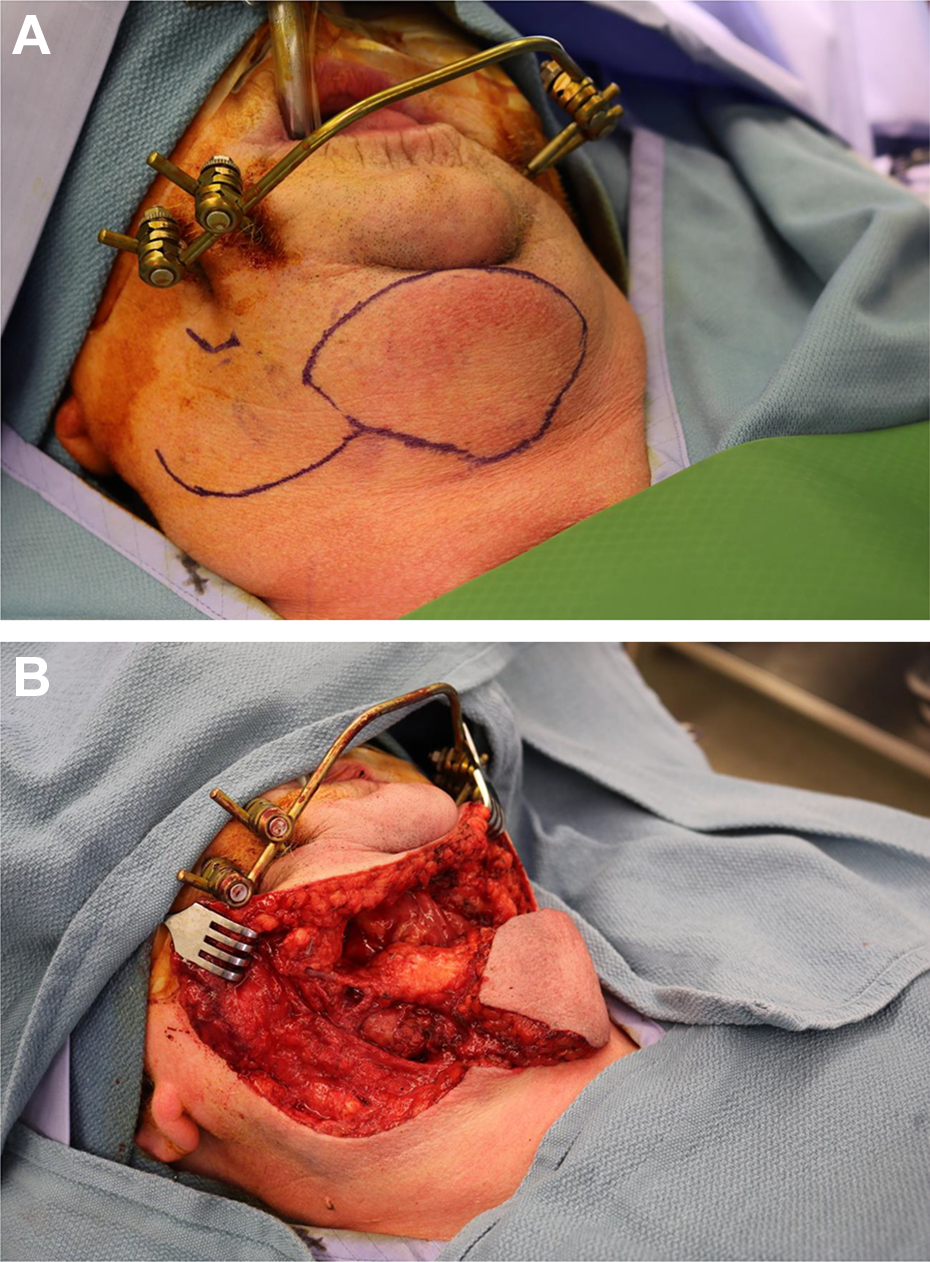
A, Intraoperative clinical photograph with marking of submental island pedicled flap with right sided pedicle. B, Following elevation of submental island pedicled flap. C, Intraoral inset of flap skin paddle.
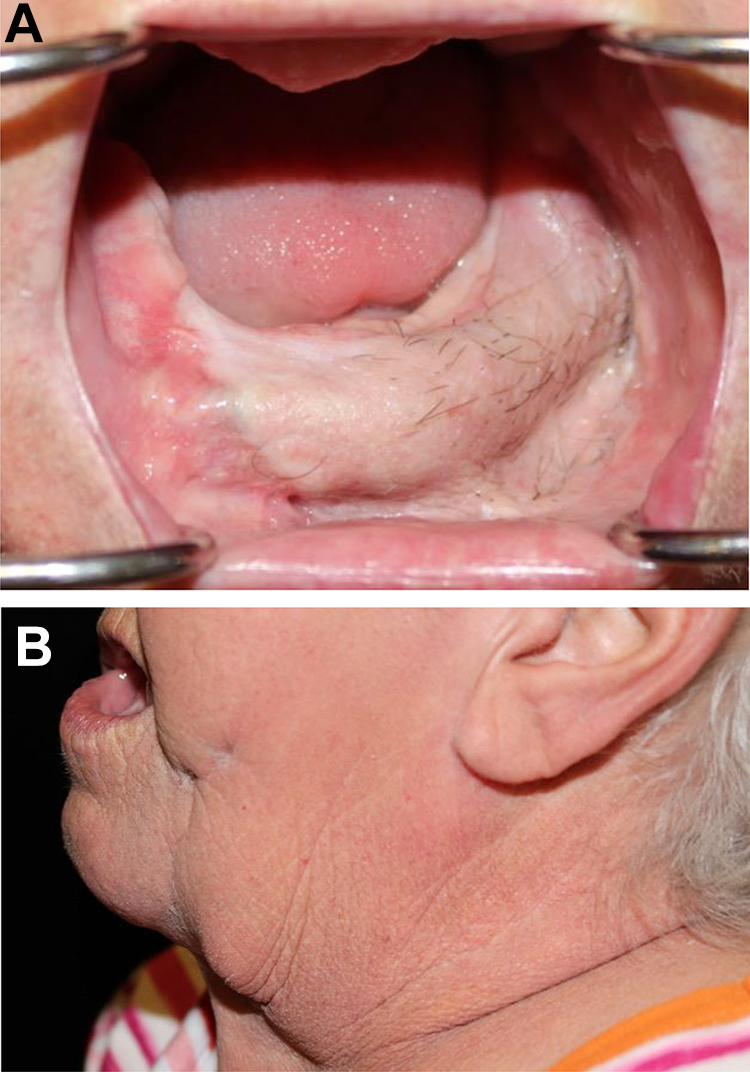
A, Six months clinical photograph of appearance of flap skin paddle with recreation of mandibular vestibule. B, Lateral profile photograph with restoration of chin projection.
Discussion
Today, microvascular free flaps are highly reliable, with a reported pooled survival of 94.8% for free tissue transfer flaps in mandibular reconstruction. 6 Furthermore, free tissue transfer flaps have been reported by several authors as a safe and reliable option for the reconstruction of patients undergoing segmental mandibulectomy for MRONJ. However, one must not forget that free tissue transfer flaps in head and neck reconstructive surgery are not without significant complications with a reported perioperative mortality rate of 1.3% and an overall perioperative complication rate of 36.1%. 7 As one would expect the occurrence of perioperative medical complications (ie, cardiac, pulmonary, and infectious), which have been reported as high as 20.5%, have a statistically significant relationship to the patient’s preoperative comorbidity level. 7 Myocardial infarction has been reported to occur in 3.6% of patients undergoing head and neck reconstruction with a free tissue transfer flap, with 29% of these patients dying within their hospitalization. 8 Therefore, reconstructive surgeons must consider patient comorbidities and reconstructive requirements (eg, recipient vessels) to identify the ideal flap to achieve an optimal reconstructive outcome (both functional and aesthetic). Even though free tissue transfer flaps are more revered in postoncologic head and neck reconstructive surgery, pedicled flaps still have a significant role in select patients. Pedicled flaps have been shown to results in decreased operative time as well as decreased length of intensive care unit stay and decreased hospital charges. 4
For oromandibular reconstruction, a myriad of pedicled flap options exist including the pectoralis major, latissimus dorsi, trapezius, masseter muscle, supraclavicular island, and submental island flaps (SIFs). In our reported case, we utilized the submental island pedicled flap. The submental artery island flap was first introduced by Martin and colleagues in 1993 as either a pedicled or free flap, and since then it has gained significant popularity for reconstruction of local defects such as oral cavity and its subsites (including tongue, floor of mouth, buccal mucosa, retromolar trigone, and mandibular alveolus), oropharynx, and temporal bone defects. 9,10 It has also been used for myriad of other head and neck applications such as the reconstruction of the nose, palatal defects, reconstruction of the neopharynx after laryngectomy, as well as coverage of spinal hardware. 11 Its popularity as a pedicled flap stems from a myriad of reasons, such as proximity of the flap to the recipient site, in cases requiring a transcervical incision it does not require a second donor site, microsurgical armamentarium/skills are not required, technical ease in flap elevation without adding significant operating time, and the flap donor site lending itself to primary closure. 12 Furthermore, the flap donor site in patients with tissue laxity in the submental region lends itself to an acceptable esthetic outcome secondary to tightening of the submental skin and the scar being well hidden in the submental region within the shadow of the mandible. 13 Unique variations of this flap have been described, such as incorporating a segment of the basal bone of the inferior border of the mandible in the symphyseal region resulting in an osteocutaneous flap with the osseous component receiving its blood supply from periosteal perforators. 14 The SIF has also been described as having the potential of being raised in a fashion that allow for elevating bilateral submental flaps by dividing the skin paddle obliquely in a fashion that preserves each submental artery. 13 This modification has been previously reported by Patel and colleagues. 5 In summary, while establishing bony continuity is the ideal in the reconstruction of the segmental mandibulectomy defect, not every patient is a candidate for an osseous free tissue transfer-based reconstruction. In select cases, re-establishing mandibular continuity used a reconstruction plate and when necessary a soft tissue flap (distant vs locoregional) is an appropriate option. Today, with the advent of virtual surgical planning and 3-dimensional printing technologies in utilizing a patient-specific reconstruction, plate reconstructive surgeons are able to minimize surgical time, improve reconstructive accuracy, and reduce the risk of plate fracture, thus strong consideration should be given to such technologies. While the technique of using a pedicled pectoralis major flap and a reconstruction plate has been an accepted reconstructive option for some time now, in our reported case we described using a pedicled submental island for coverage of the reconstruction plate using a modified technique with incorporation of the mylohyoid muscle as a part of the skin paddle was utilized to allow for greater bulk around the plate to reduce the risk of subsequent plate extrusion.
Conclusion
Reconstruction of anterior mandibular defect has many surgical options including staged or simultaneous osteomyocutaneous, myocutaneous, cutaneous pedicled or free flaps. Careful consideration of contributing medical comorbidities, overall frailty of the patient, as well as long-term prosthetic goals and patient desires are important factors to consider when determining the choice of reconstruction. Resources such as American College of Surgeons Risk Calculator (https://riskcalculator.facs.org/RiskCalculator) can be a useful tool to objectively risk stratify patients for surgery.
Footnotes
Authors’ Note
Written informed consent was obtained from the patient.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
