Abstract
Objective
This study was performed to determine whether the results of prevailing in vivo and in vitro studies offer a reliable model for investigation of medication-related osteonecrosis of the jaw (MRONJ).
Methods
Embase, Medline, and the Cochrane Library were searched for articles published from September 2003 to June 2017 involving experimental approaches to the pathogenesis of MRONJ. In vivo and in vitro trials were analyzed with respect to the scientific question, study design, methodology, and results.
Results
Of 139 studies, 87, 46, and 6 conducted in vivo, in vitro, and both in vivo and in vitro experiments, respectively. Rats, mice, dogs, minipigs, sheep, and rabbits were the preferred animal models used. Osteoblasts, osteoclasts, fibroblasts, keratinocytes, macrophages, and human umbilical vein endothelial cells were the preferred cell types. Zoledronate, alendronate, ibandronate, and risedronate were the most frequent bisphosphonates used. MRONJ was most reliably induced in minipigs because of the close relationship with human bone physiology. In vitro studies showed that reduced viability, growth, and migration of cells in the bone and soft tissues were causative for MRONJ. Other than exposed jawbone after tooth extraction, no reliable cofactors were found.
Conclusion
The minipig is the most suitable animal model for MRONJ.
Introduction
Bisphosphonates (BPs) are pharmaceuticals commonly used for the treatment of resorptive bone diseases such as multiple myeloma, 1 bone metastases, 2 primary and secondary osteoporosis, 3 and Paget’s disease of bone. 4 BPs were introduced into medicine around 1960 as derivatives of endogenous inorganic pyrophosphate (PPi), a substance with a chemical P-O-P bond that is well known for its biological activity in interfering with the dissolution and precipitation of calcium phosphate, the main component of mineralized bone. 5
Initial attempts to medicinally influence in vivo bone remodeling by administering PPi showed insufficient clinical effects. Despite its high affinity for skeletal calcium phosphate containing hydroxyapatite crystals, PPi was found to be extremely susceptible to rapid hydrolysis of the P-O-P bond perpetrated by pyrophosphatases. 6 BPs resemble PPi in structure, but the P-O-P bond is substituted with a non-hydrolyzable P-C-P bond enabling BPs to bind to the bone surface before enzymatic breakdown. 7 Once adherent to bone, BPs are incorporated by adjacent cells, predominantly osteoclasts, and induce antiresorptive effects by suppressing osteolytic cell activities. 8 Besides BPs, several other medications also interfere with regular bone physiology, such as denosumab, an immunoglobulin G2 antibody to receptor activator of nuclear factor kappa B ligand (RANKL). 9
Generally, two types of BPs can be distinguished: the less potent non-nitrogen-containing BPs (non-N-BPs) and the highly potent nitrogen-containing BPs (N-BPs). After uptake into the cell, the latter interfere with the mevalonate pathway by inhibiting its key enzyme farnesyl pyrophosphate synthase, thus blocking the biosynthesis of isoprenoids essential for cell signaling. 10 In this group of BPs, the highly potent BP subtypes pamidronate, ibandronate, alendronate, risedronate, and zoledronate inhibit the enzymatic switch of dimethylallyl pyrophosphate to geranyl pyrophosphate. 11 Their linear chemical formula exhibits steric likeness to the dimethylallyl pyrophosphate carbocation within the enzyme; hence, they are called linear BPs. 11 In contrast, non-N-BPs are metabolized into nondegradable adenosine triphosphate compounds that disrupt regular energy gain from adenosine triphosphate hydrolysis. 12 Recent studies suggest that besides their effect on osteoclasts, BPs have a decisive influence on other cells involved in bone metabolism, such as osteoblasts, 13 fibroblasts, 14 macrophages, 15 and keratinocytes. 16
Despite frequent medical prescription and good general tolerability of BPs, a rare yet severe adverse effect called medication-related osteonecrosis of the jaw (MRONJ) was first described in 2003. 17 This adverse drug reaction presents as exposed necrotic maxillary or mandibular jaw bone often associated with mucosal swelling, erythema, ulceration, and pain. 18 The American Association of Oral and Maxillofacial Surgeons describes MRONJ as the persistence of exposed alveolar bone for >8 weeks in patients who currently receive or have a history of receiving BPs in the absence of radiation to the head and neck area. 19 The potency and route of application (oral versus intravenous) seem to be strong predisposing factors because patients with cancer undergoing intravenous N-BP treatment are more likely to show signs of MRONJ than patients receiving non-N-BPs orally. 20 Furthermore, dental surgical procedures in patients on BP medication pose an additional precipitating factor for MRONJ development with an incidence ranging from 1% to 12% in intravenously treated patients and <1% in orally treated patients. 21
Since first described in 2003, the etiology of MRONJ has not been clarified. Many case reports and various literature reviews have outlined the clinical appearance and causative agents of MRONJ, but they have failed to decipher the precise molecular pathway of its pathogenesis. However, several in vivo and in vitro studies have been performed in an attempt to determine the cellular mechanisms of MRONJ development. On the basis of these studies, two scenarios seem likely. In the first (and currently favored) scenario, primary bone infection is the origin of pathogenicity with secondary spread to the overlying soft tissues (inside-out theory). In the second (and less likely) scenario, MRONJ originates from soft tissue necrosis with secondary bone involvement (outside-in theory).
It has become obvious that scientific research in the field of MRONJ does not follow a common line. Therefore, the goal of this study was to compare all in vivo and in vitro studies associated with BP-induced MRONJ research regarding outcomes and methodology to gain a common consensus on current knowledge. In addition, we have paid special attention to what reliable animal models have been developed to date.
Material and methods
We scanned Medline, Embase, and the Cochrane Library for literature concerning MRONJ. We searched a timespan from September 2003 (first description of MRONJ) until June 2017. To retrieve literature solely associated with BP-induced MRONJ, we applied a search filter including the terms “jaw,” “osteonecrosis,” “bisphosphonate,” and “bisphosphonates” connected by the Boolean operator “AND.” The inclusion criteria were 1) literature with special emphasis on MRONJ, 2) availability of an abstract, 3) articles available in the English or German language, and 4) a listing in the three aforementioned databases. We retrieved a total of 1,781 articles. Of these, 404 articles had no available abstract and were discarded. Obtainable abstracts were examined, culminating in further exclusion of 89 articles not available in English or German and another 252 that bypassed the topic of MRONJ. Abstracts unavailable online were attained from Düsseldorf University and State Library. The remaining 1,036 articles were thoroughly reviewed and ultimately included in this study. A reference list is available upon request from the corresponding author. Among articles incorporated in our study, we focused on literature elucidating the pathogenesis of MRONJ using an experimental approach. Attention was paid exclusively to in vivo and in vitro trials. Accordingly, we identified 145 articles with an in vivo or in vitro study design. Data collection from these articles concentrated on the year of publication, authors, scientific question, study design, and final study results.
Next, we divided the in vivo and in vitro trials into two groups. For each group, we tested the intragroup conformity of the presented study results. In addition, we examined the intergroup agreement in understanding the pathogenesis of MRONJ.
This study was fully retrospective with no need for ethics approval. No experiments were conducted and no patient data collected that may have required approval.
Results
Trials with an experimental approach
Of all 1,036 articles included in this study, 145 (14.0%) used an experimental approach to investigate BP-induced MRONJ. Among these, 81 (55.9%) conducted in vivo trials, 57 (39.3%) conducted in vitro trials, and 7 (4.8%) conducted both in vivo and in vitro trials.
In vivo trials
Within the timespan analyzed (2003 to June 2017), the experimental in vivo publications showed a steady increase from 2007 to 2010 and from 2011 to 2013. From 2011 to 2014, the number of in vivo trials reached an all-time low of merely six publications (Figure 1). In 2016, the number of animal studies conducted rose to 15. All studies in the in vivo subset used a mammalian test animal model. Itemized by animal type, 46 (52.3%) studies used rats, 30 (34.1%) used mice, 6 (6.8%) used dogs, 3 (3.4%) used pigs, 1 (1.1%) used rabbits, and 2 (2.3%) used sheep as test animal species. Table 1 summarizes all in vivo studies assorted by test animal species and year of publication.
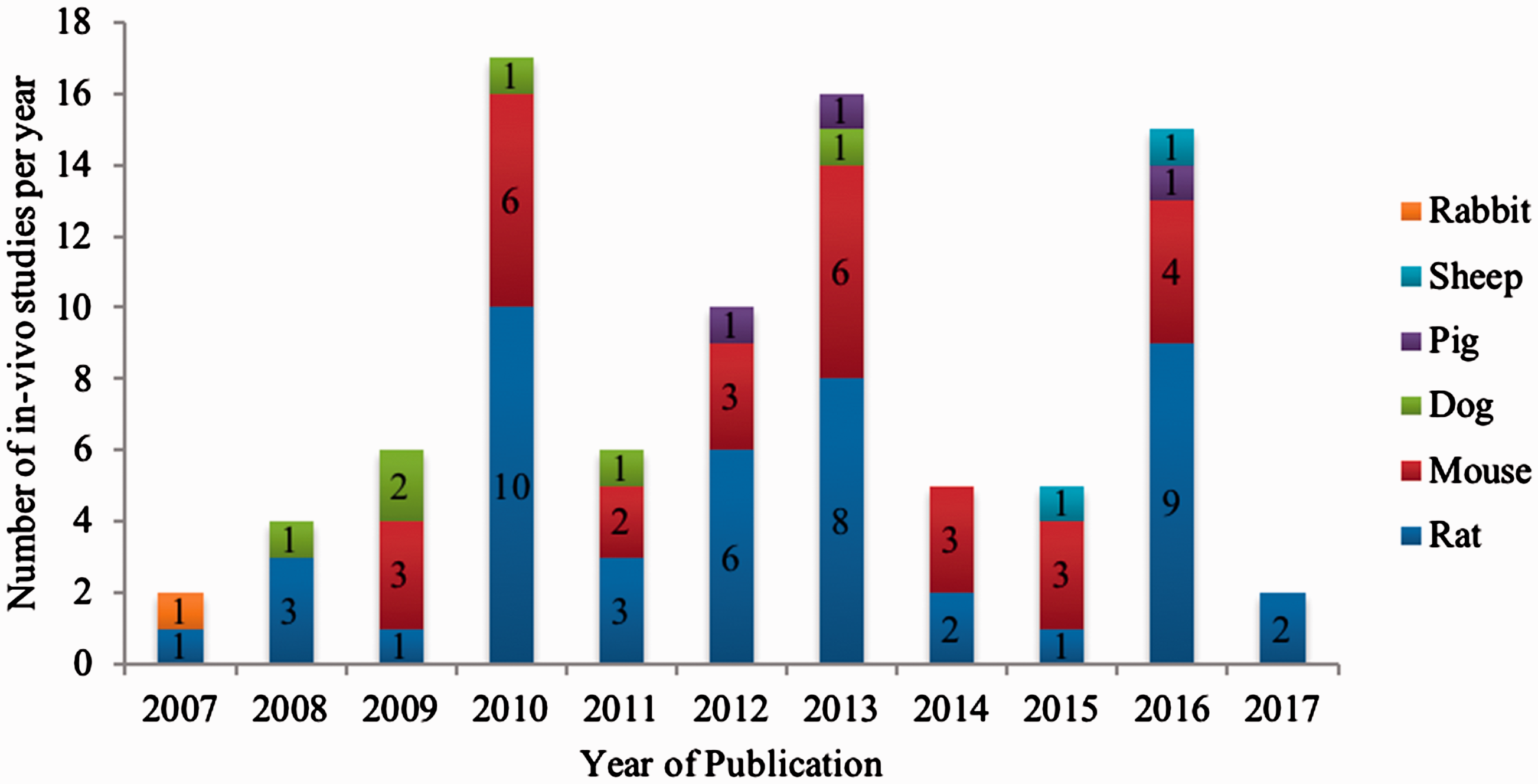
Number of published in vivo studies on medication-related osteonecrosis of the jaw published from 2003 to 2017 assorted by the test animal species used.
Summary of in vivo studies using different test animal models assorted by year of publication.

Rats
Used in 46 studies, the rat was the favored test animal among in vivo studies. In 2007, 4 years after the initial description of MRONJ, Yang et al. 22 were the first to investigate the effects of BPs on mechanical bone properties in a femur rat model. The authors showed that high concentrations (0.5 mg/kg) of pamidronate, an N-BP, decreased mineral bone density and weakened mechanical bone strength. Subsequently, additional scientific questions from 2008 to 2017 addressed the effects of BP administration on MRONJ development with (30 studies) and without (15 studies) tooth extraction. Four trials studied periodontitis as a risk factor for jaw osteonecrosis under BP treatment.23–26 Eventually, oral wound healing (1 study) and bone site-specific BP uptake (4 studies) moved to the focus of scientific interest.27–31 The tissues investigated were bone, oral mucosa, periodontium, and blood vessel supply.23,24,32–43 The studies differed in the type of BP used as well as the route of application.25,44–49 Only 2 studies analyzed non-N-BPs (clodronate at 20 mg/kg and etidronate at 5 mg/kg); the remaining 44 trials used N-BPs with zoledronate (0.01–0.6 mg/kg) being the most commonly used (30 studies), followed by alendronate (0.01–1 mg/kg) (14 studies), pamidronate (0.01–3 mg/kg) (5 studies), and ibandronate (0.003–0.3 mg/kg) and risedronate (0.1–1 mg/kg) (1 study each).26,48,50–53 Twenty-two studies used an intraperitoneal route of application, 15 used subcutaneous, 10 used intravenous, 1 used intramuscular, and 1 used topical.54–63 The absolute number of studies does not equal 46 because some tested more than one BP or tried different application routes. Table 1 summarizes all conducted studies using rats as test animals.
Mice
To date, 30 studies have created a mouse MRONJ model. The first in vivo study using mice as test animals was conducted in 2009 by Huja et al. 64 They injected zoledronate intraperitoneally at a concentration of 0.1 mg/kg and found that new bone formation was significantly decreased while osteoclast apoptosis could not be observed. Since then, many study groups have analyzed a broad variety of different scientific questions such as the effects of BPs on bone formation and remodeling (5 studies) and oral wound healing and angiogenesis (3 studies).65–76 Two studies also showed that non-N-BPs have protective effects on MRONJ development in animals undergoing N-BP treatment.65,77 One study concentrated on the BP effects at different bone sites. 78 In 2013, RANKL inhibitors such as denosumab attained increasing interest, and their effects were compared with those of BPs on bone metabolism (3 studies).70,71,76 Similar to the rat trials, the influence of tooth extraction (13 studies) and periodontal disease (3 studies) on MRONJ development was also analyzed in studies using mice as test animals.77,79–84 Immunotherapeutics and chemotherapeutics such as dexamethasone and melphalan were applied in combination with BP treatment in three studies.68,69,80 The roles of dental infections, systemic and jaw osteopenia, osteoblast function, fracture repair, and technetium-99 conjugated with methylene diphosphonate were each assessed in two studies.81,85 Twenty-four studies used zoledronate (0.001–1 mg/kg), three studies used alendronate (0.1–1 mg/kg), two studies used etidronate (250 μg/kg), two studies used clodronate (21 μg/kg), one study used ibandronate (0.085 μg/kg), two studies used pamidronate (1.3 μg/kg), and one study used risedronate (0.1 mg/kg).85,86 The route of application was intraperitoneal in 14 studies, subcutaneous in 6 studies, and intravenous in 6 studies.87–89 Table 1 summarizes all studies conducted using mice as test animals.
Rabbits
In 2007, Choi et al. 90 established a rabbit test animal model of MRONJ development. Locally applied pamidronate at concentrations of 2 and 3 mg inhibited bone healing in rabbit calvarial bony defects. Table 1 summarizes all conducted studies using rabbits as test animals.
Dogs
Six in vivo studies analyzed MRONJ in dogs.91–96 The preferred BP was zoledronate (0.006–0.1 mg/kg) in five studies and alendronate (0.2–1 mg/kg) in two studies (one study tested more than one BP). Zoledronate was always administered intravenously and alendronate orally. In 2008, Allen and Burr 91 conducted a 3-year study of oral alendronate application in Beagle dogs at doses of 0.2 and 1 mg/kg. The authors observed a decreased intracortical bone turnover rate in the test group compared with the control group. Other trials tested the effects of BPs on osteocytic death (1 study), 94 bone remodeling after tooth extraction (2 studies),91,92 and oral mucosal epithelial cells (1 study). 95 One trial hypothesized that severe MRONJ develops when zoledronate is combined with the immunosuppressive agent dexamethasone. 93 However, this hypothesis could not be proven. Table 1 summarizes all studies conducted using dogs as test animals.
Pigs
Three studies published in 2012, 2013, and 2016, respectively applied zoledronate (0.05 mg/kg and 4 mg) intravenously in a pig model of MRONJ.97–99 After tooth extraction, animals in the zoledronate group displayed improper bone remodeling compared with the controls. One study showed that bone marrow mesenchymal stem cell transplantation after BP treatment restored the number of Foxp3-positive regulatory T cells and the interleukin-17 serum level. 98 Table 1 summarizes all studies conducted using pigs as test animals.
Sheep
In 2016, Voss et al.100,101 established a MRONJ sheep model. After intravenous injection of zoledronate (75 μg/kg), the sheep developed jaw osteonecrosis after tooth extraction. Table 1 summarizes all studies conducted using sheep as test animals.
In vitro trials
Within the in vitro subset, two groups were distinguished. Group I comprised 47 (82.5%) studies that investigated only one cell type, and Group II comprised 10 (17.5%) studies that investigated several cell types. The analyzed cell types in Group I were osteoblasts (15 studies), macrophages (4 studies), osteoclasts (4 studies), keratinocytes (8 studies), fibroblasts (11 studies), and human umbilical vein endothelial cells (HUVECs) (5 studies). In Group II, four studies (40.0%) investigated keratinocytes and fibroblasts; two studies (20.0%) investigated osteoblasts, fibroblasts, and HUVECs; one study (10.0%) investigated osteoblasts and fibroblasts; one study (10.0%) investigated osteoblasts and keratinocytes; one study (10.0%) investigated osteoblasts, keratinocytes, fibroblasts, and HUVECs; and one study (10.0%) investigated osteoblasts and osteoclasts. Figure 2 shows the in vitro studies that were conducted with respect to cell type and year of publication. The figure shows more than 57 in vitro studies because some studies tested more than one cell type.

Number of in vitro studies on medication-related osteonecrosis of the jaw published from 2003 to 2017 assorted by the cell type analyzed. HUVEC = human umbilical vein endothelial cells; FB = fibroblasts; KC = keratinocytes; MP = macrophages; OC = osteoclasts; OB = osteoblasts.
Osteoblasts
Represented by 22 in vitro studies, osteoblasts were the most frequently analyzed cell type.13,102–108 Nineteen studies solely used osteoblasts, and three studies simultaneously experimented with other cell types.109–112 Osteoblast viability, differentiation, proliferation, growth, and migration under BP treatment were the main scientific focus in 19 studies. One study analyzed the gene expression of RANKL and osteoprotegerin, 109 and four trials concentrated on the positive effects of low-level laser therapy and herbal extracts to counteract MRONJ development.107,113–115 Thirteen studies analyzed only one BP; of these, 10 studies used zoledronate (0.01–100 μM), 1 used pamidronate (10−5, 3 × 10−5, 6 × 10−5, and 10−4 M/L), 1 used clodronate (10−5 to 10−9 mM/L), and 1 used alendronate (0.01–100 μM).113,114,116–118 The remaining 11 studies applied a combination of zoledronate, ibandronate, pamidronate, clodronate, and alendronate at concentrations varying from 0.00001 to 500 μM.115,119–121 Table 2 summarizes all studies that evaluated osteoblasts in MRONJ.
Summary of in vitro studies using different cell culture models assorted by year of publication.

HUVECs, human umbilical vein endothelial cells
HUVEC
HUVECs were analyzed in five studies.108,112,113,122,123 In all studies, the effects of zoledronate, ibandronate, pamidronate, and clodronate were tested at concentrations of 5 to 500 μM. After BP application, HUVEC viability and migration decreased and apoptosis was induced. Low-level laser therapy and the isoprenoid geranylgeraniol had positive effects on HUVEC survival. Table 2 summarizes all studies that evaluated HUVECs in MRONJ.
Osteoclasts
Four studies tested the effects of zoledronate (1–10 μM), alendronate (0.01–100 μM), pamidronate, and risedronate (1–100 μM) on osteoclasts.114,124–126 Differentiation of osteoclasts was found to be inhibited by BPs. Herbal extracts from Melia azedarach, Corydalis turtschaninovii, and Cerithium atratum induced apoptosis in osteoclasts. Isoprenoids restored BP-associated inhibition of osteoclast differentiation. Osteoclasts in the jaw showed increased uptake of BPs in the jaw region compared with long bones. Table 2 summarizes all studies that evaluated osteoclasts in MRONJ.
Macrophages
The effects of BPs on macrophages were assessed in five studies.15,127–130 The BPs of choice were zoledronate (0.5–50 μM), alendronate (5–100 μM), and clodronate (10−4 M). Three studies described increased proinflammatory cytokine production by macrophages after BP treatment.15,127,128 In 2009, Masuda et al. 128 found decreased proinflammatory cytokine production. Further, BPs suppressed macrophage differentiation. Table 2 summarizes all studies that evaluated osteoclasts in MRONJ.
Keratinocytes
In 2008, oral keratinocytes gained the attention of many study groups in the pursuit of understanding the pathogenesis of MRONJ. In seven studies, the main objective was to analyze the effects of BPs on this cell type.14,16,104,131–134 One other trial tested the possible positive effects of low-level laser therapy on keratinocyte viability. 113 The BPs used were zoledronate (0.01–500 μM), clodronate, ibandronate (5–500 μM), and pamidronate (0.003–500 μM). Table 2 summarizes all studies that evaluated keratinocytes in MRONJ.
Fibroblasts
As part of the oral connective tissue, oral fibroblasts were analyzed in 13 studies.14,16,103,112,113,135,136 In 2009, Scheper et al. 132 studied the adverse effects of BPs on this cell type. Cell viability and migration deteriorated under BP treatment. Concentrations of 0.01 to 500 μM of zoledronate, 0.01 to 500 μM of pamidronate, 0.01 to 20 μM of alendronate, and 5 to 500 μM of clodronate and ibandronate were used.108,137–140 Table 2 summarizes all studies that evaluated fibroblasts in MRONJ.
Combined in vivo/in vitro trials
Seven studies performed both in vivo and in vitro MRONJ assessment.141–147 Four chose a mouse model141–144 and three chose a rat model.145–147 Figure 3 provides an overview of all combined in vivo/in vitro studies since the first description of MRONJ in 2003.

Number of combined in vivo/in vitro studies on medication-related osteonecrosis of the jaw published from 2003 to 2017 assorted by the test animal species used and cell type analyzed. Ca(OH)2 = hydroxyapatite; MP = macrophages; FB = fibroblasts; KC = keratinocytes; OC = osteoclasts.
Mice
In 2010, Shikama et al. 141 analyzed the effects of BPs on macrophages. They concluded that alendronate stimulates the production of the proinflammatory cytokine interleukin-1β in macrophages, while clodronate inhibits this effect. In macrophage-depleted mice, this production was almost absent. In 2012, Kuiper et al. 142 also concentrated on immune cells, but focused on neutrophils. They showed in vitro and in vivo inhibition of chemotaxis and NADPH oxidase activity by zoledronate and pamidronate. In 2015, Tseng et al. 143 found that N-BPs but not non-N-BPs triggered increased release of proinflammatory mediators from osteoclasts. Additionally, in 2011, Mawardi et al. 144 showed diminished wound healing after pamidronate treatment in animals infected with Fusobacterium nucleatum, suggesting a bacterial role in the etiopathogenesis of MRONJ.
Rats
Hokugo et al. 145 and Kozloff et al. 146 concentrated on calcium hydroxide and the adhesion of BPs to the bone surface. Ogata et al. 147 showed that serum-free conditioned media from human mesenchymal stem cells had potential therapeutic effects on MRONJ.
Discussion
Since the first description of MRONJ in patients undergoing BP therapy, many studies have been performed in an attempt to develop a suitable mammalian model for its etiopathogenesis. Among 46 studies, most of the in vivo rat studies concentrated on the influence that post-BP tooth extractions have on the occurrence of MRONJ. In this manner, only Vasconcelos et al. 29 applied a non-N-BP (clodronate) in their study, accounting for only 2.0% of all studies. They found that clodronate was less likely to cause MRONJ than zoledronate. All other studies applied N-BPs (zoledronate, alendronate, or pamidronate). Trials in which only zoledronate was administered showed signs resembling jaw osteonecrosis. 37 The effects of alendronate are more controversial. Conte-Neto et al. 148 linked alendronate application to the occurrence of osteonecrosis of the jaw (ONJ)-like lesions, while Maahs et al. 45 found no sufficient correlation. Conversely, Aguirre et al. 46 only found a transient negative influence on wound healing in alendronate-only treated rats. A second subset of trials analyzed the effects of concomitant application of a BP (zoledronate, alendronate, or pamidronate) and a corticosteroid. Generally, BP + corticosteroid therapy resulted in the development of ONJ-like lesions. 24 Furthermore, Sonis et al. 32 found that BP + corticosteroid therapy was more relevant for MRONJ development than zoledronate treatment alone. However, Berti-Couto et al. 34 stated that this combination therapy was not at all associated with the occurrence of MRONJ. Two studies showed that systemic antibiotic therapy and mucoperiosteal coverage of extraction sockets were reliable parameters for MRONJ prevention. 149 Besides treatment with different BPs or immunosuppressants, Aghaloo et al. 25 were the first to identify periodontitis as a precipitating factor for the occurrence of MRONJ under high-dose zoledronate treatment. Studies published in 2012 and 2016 support these findings. 89
In another group of studies that used a rodent test animal model, the effects of tooth extraction under BP treatment were analyzed in mice. In contrast to the abundance of rat studies, only 13 tooth extraction studies were conducted in mice. More of these studies examined the effects of BP + corticosteroid combination therapy on MRONJ development than zoledronate-only treatment. In general, BP + corticosteroid therapy predisposes to the occurrence of ONJ-like lesions after tooth extraction. However, like Berti-Couto et al., 34 who studied rats, Kuroshima and Yamashita 68 did not find these effects. Bi et al. 81 induced MRONJ in mice under zoledronate treatment and tooth extraction. Again, a non-N-BP (etidronate) did not cause jaw osteonecrosis. 82 Interestingly, the presence of periapical disease facilitated jaw osteonecrosis under treatment with zoledronate as well as treatment with antireceptor activator of nuclear factor kappa beta ligand antibody. 87 This has not yet been tested in rats. However, rodent bone physiology and regeneration significantly differ from those of humans; therefore, whether the results from these studies can be transferred to MRONJ in humans remains unclear.
One of the first trials concerning avascular bone necrosis as observed in MRONJ was conducted in 2007 by Choi et al. 90 In this study, however, the inhibitory effects of pamidronate on bone healing were only tested in the rabbit calvaria and not the jaw.
While rodent models generally induce jaw osteonecrosis under zoledronate-only treatment, the effects of which could even be intensified by addition of a corticosteroid, dog models do not show these effects. In the studies examined, no significant difference in the occurrence of MRONJ could be distinguished between zoledronate-only therapy and zoledronate + corticosteroid therapy. 93 In two studies without tooth extraction, a reduced bone remodeling rate was observed under alendronate and zoledronate treatment in the absence of exposed jawbone. 94 Among the vast variety of existing dog models of MRONJ, we still lack a uniformly applicable dog model in which BP administration is reliably followed by exposure of jawbone. This was discussed in 2007 by Allen. 150
Li et al., 98 Pautke et al., 97 and Voss et al. 100 showed induction of MRONJ after tooth extraction in a pig model (zoledronate) and sheep model (zoledronate + corticosteroid). Pig models are often used for bone studies because their bone regeneration physiology is similar to that of humans. 97 Histomorphologic conditions found in human MRONJ samples can be reliably reproduced in the pig models. As already stated by Mitsimponas et al., 99 it is necessary to conduct further studies using pig models to understand the immunohistochemical and biomolecular structures leading to MRONJ. We currently regard studies using a minipig model as ideal for the analysis of the occurrence of MRONJ. This was also recently stated by Otto et al.151–153 The minipig model has shown the most promising effects with respect to the comparability of human bone physiology and morphology.
In vitro trials predominantly focused on the inhibitory effects of BPs, most often zoledronate, on the viability, migration, and growth of osteoblasts, osteoclasts, fibroblasts, keratinocytes, macrophages, and HUVECs. We found no direct correlation to an in vivo trial could. Several studies tested whether zoledronate causes apoptosis of bone and soft tissue cells; however, whether jaw osteonecrosis is preceded by soft tissue necrosis or if soft tissue necrosis follows development of necrotic bone remains unclear. A common consensus, as noted by Walter et al. 112 in 2011, is the belief that MRONJ is a multifactorial disease involving many cell lines.
We conclude that in vivo and in vitro analyses of the etiology of MRONJ have not yet been able to present a universally accepted theorem. In line with what has already been observed in patients undergoing BP therapy, tooth extractions seem to profoundly increase the susceptibility to jaw osteonecrosis in rodents, markedly in rats. Whether rodent research can be transferred to humans is questionable; therefore, studies involving models with larger animals were conducted. Of these, minipig test animal models depict the most reliable relationship between BP treatment and jawbone necrosis. With all studies choosing a slightly different study design that varied in both the type and concentration of BPs and culminating in diverse outcomes, we hypothesize that the development of MRONJ might be metabolically dependent. Responsible cofactors, currently unidentifiable, in the pathogenesis of this disease need further exploration using the minipig test animal model in future trials.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
