Abstract
This article aims to share a simple method that can be adopted as part of treatment regimen of keloids. Two types of modified oyster splint was done and their usefulness is discussed. As an adjunct method, this device has shown to give a satisfactory result. Further investigation by clinical studies are invited.
Introduction
Wound recovery is a complex biological process that can either end up without much problem or, in some circumstances, turned into an undesirable scarring. Proliferative scars, namely the keloids and hypertrophic scars, occur when the wound healing goes beyond its normal reparative process. These scars can cause functional limitation and compromise the skin aesthetics if it occurs at mobile and exposed area such as the face. Several clinical characteristics differ the keloids and hypertrophic scars. Unlike the latter, keloids progressed beyond the original wound, has an uninterrupted evolution, and have high propensity to recur after treatment. Other than that, symptoms of pruritis, pain, and restriction of movement were also reported to be more prevalent in keloids. 1,2
Various approaches are described in the literature for the management of keloidal scars, but there is no single proven method that guarantees of no-recurrence. Combination of treatment method has been advocated. 3,4 Challenges in managing scar on the facial region including inability to have primary closure after excision, skin color differences post steroids therapy, and compliance of patient to adhere to post-intervention care. In our case, we were dealing with keloid on a movable region that involved in mastication, speech, and part of facial expression.
Case
A 19-year-old patient presented with a raised scar on left cutaneous upper lip. Patient was involved in a road traffic accident 1 year ago, with an abraded skin on the said region and managed with secondary healing. There was no abnormal scarring on patient’s other body parts. Medical history was clear. Family history revealed that patient’s elder sister had keloidal scar at her vaccination site on the left upper arm. Surgical debulking was done until the area of wound bed feels soft on palpation. We preserved the scar edges so as not to disturb ala of the nose and worsen the condition of the already affected white roll (Figure 1). Three doses of intralesional injection of 40 mg/mL triamcinolone acetonide given 1 week after the surgery and continue at 1-month interval thereafter. We constructed a modified oyster splint using expansion screw for the patient to wear at home (Figure 2). Although the device was small and contoured to shape of the lip, patient was not able to insert and remove the splint easily. We then changed it into another form of splint to give a better dexterity and to provide more comfort to the patient’s lip (Figure 3). Other than wearing the splint on nocte basis, the patient was also advised to put it on whenever at home.
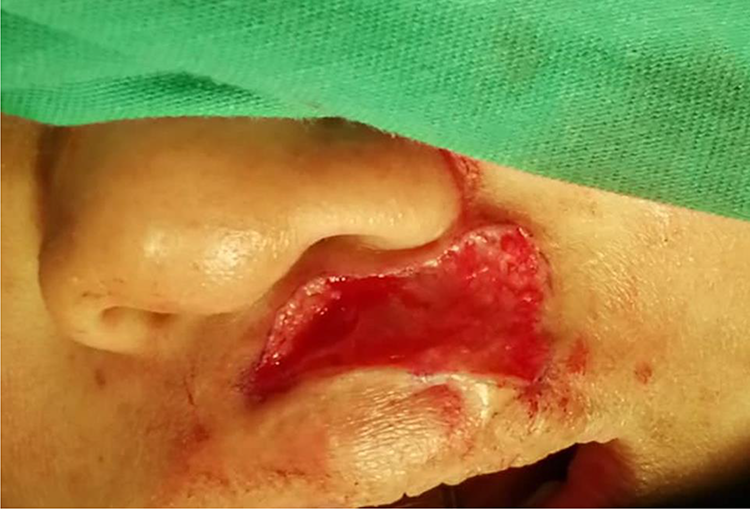
Surgical debulking post-traumatic keloid on the left cutaneous upper lip with the size of 3.0 × 1.5 mm2 was excised to the depth of soft wound bed and preserving its edges.
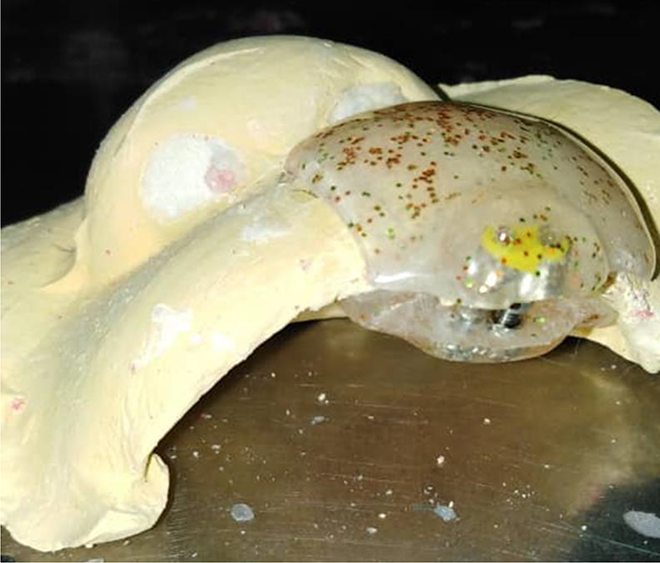
Oyster splint on stone model splint was made using acrylic and an expansion screw.
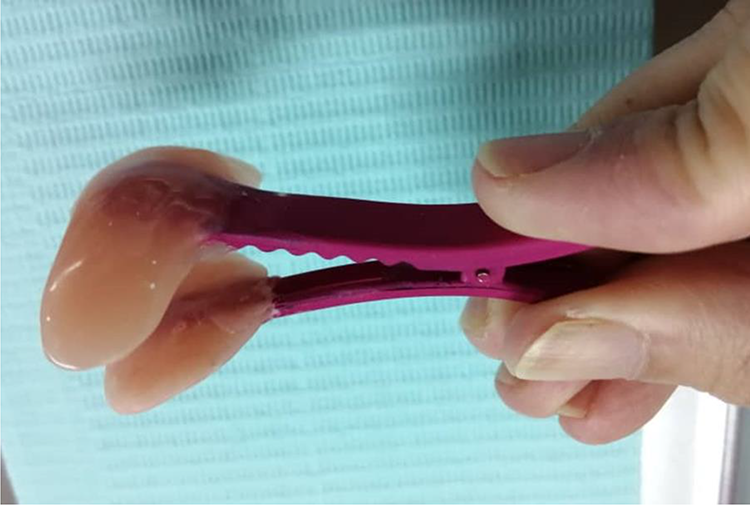
Modified oyster splint with cold cure acrylic incorporated into a shortened plastic clip to serve splint.
Discussion
Several factors contribute to the occurrence of pathological scars such as keloid. Possible mechanisms include mechanical forces, repeated skin irritation, skin structures, and genetic predisposition. 5 Knowing these contributing factors helps the clinician to formulate their treatment plan. It might involve a combination of surgical and medical therapy alongside with an adjuvant.
Oyster splint used as a compression device for the treatment of keloids on ear was dated back in 1983 and since then, various pressure devices have been utilized by many clinicians. 6 Mechanical compression helps control the wound healing and scarring formation by occlusion of small vessels leading to reduction in tissue metabolism, fibroblast proliferation, and collagen synthesis. 4
We have been managing cases of ear keloids using oyster splint and was hoping that it may work similarly for this current case. Prior to debulking surgery, impression of the patient’s lip was taken using alginate (Figure 4). Self-cure acrylic resin was then constructed on the stone model with its margin extended beyond the anticipated surgical excision. The splint was trimmed to 1- to 2-mm thickness and polished leaving no rough surfaces. However, we then realized that the splint with an expansion screw is not easy for the patient to manipulate its grip onto the mobile and slippery soft tissue of the lip.
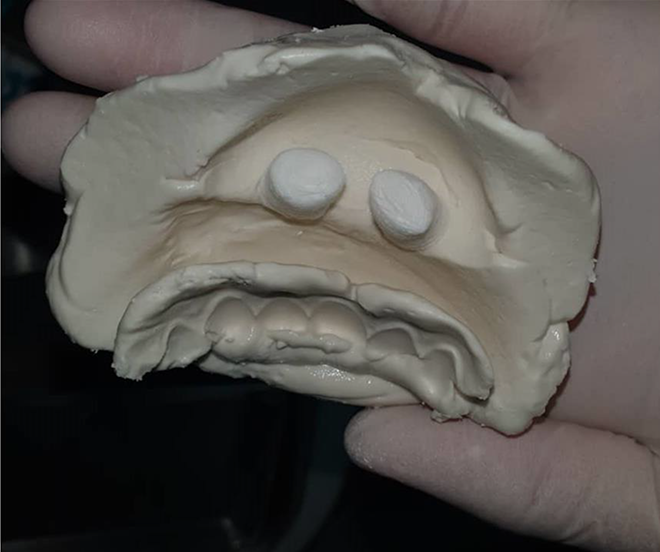
Impression of patient’s upper lip taken using alginate keloid scarring (marked) is studied before surgical debulking and construction of splint.
To give a better dexterity for the patient, we decided to incorporate a small plastic clip into the acrylic. It gives enough retention and compression without exerting too much pressure (as evidenced by non-blanching skin). This modified oyster splint is easy to handle and clean, inexpensive, and simple to create. It also serves to protect surgical wound from irritation and repetitive rubbing on pillow while sleeping at night as what were intended for splint on ear keloids. A 12-hour wearing was advocated in a study using magnets for ear keloids. 7 However, location of the keloid in our case does not permit the patient to wear it during daytime. Patient was advised to put on the splint for at least 8 h/d. After 6 months, we had observed improvement in healing of the surgical site with minimal pigmentation. Due to potential recurrence of keloids, we recommended the patient to wear the splint for more than 6 months.
Conclusion
Managing fibroproliferative scar on the facial region is a challenging clinical situation. Nevertheless, we are keen to look further into the uses of splint on lip for the treatment of these scarring, given its frequent site in trauma cases and its promising effect.
Footnotes
Acknowledgments
Many thanks to both dental officers, Dr Lim Min Jim and Dr Karimah Ab Ghani for their assistance in managing the case.
Author Contributions
Both authors conceived and designed the case study; contributed to data acquisition, both laboratory and clinical/literature search; drafted and provided the final approval to the manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
