Abstract
We report a case of a 40-year-old East Asian male who presented with multiple facial lacerations and was referred to oculoplastics for periorbital assessment and wound repair. On wound closure, the needle of a 6-0 vicryl suture accidentally detached, and a mobile image intensifier was used which did not detect a foreign body. Surgical closure was done, but upon computed tomography scan of the face, an embedded foreign material was seen. Difficult secondary wound exploration was performed but with the aid of an intraoperative magnetic probe, the 11-mm needle was identified in entirety.
Keywords
Introduction
In 2001, the term “never event” was coined by Ken Kizer to refer to medical errors that should never occur and among these include unintended retention of a foreign object in a patient after surgery or other procedure. 1 It has been estimated that incidence of retained surgical instruments and sponges range from 1 in 1,000 to 18,760 operations, and corresponding to 1 case per year for a large hospital. 2,3 There are varying data on its incidence because most are retrospective studies and case reports. Furthermore, the reluctance in reporting these events due to its sensitive nature, confidentiality matters, and legal claims prevent publication of such data. 3 But these are important learning points for the surgical team for future prevention and appropriate management.
Most reports on incidence of retained surgical instrument (RSI) occur in open cavities. And the most commonly reported items are surgical sponges, while needles and instruments are said to be extremely rare. 3 -7 Some of the risk factors identified include increased body mass index, trauma surgeries, intraoperative complications, unexpected change in procedure, and high number of surgical instruments in the field. 4,6
Different surgical procedures have been reported with retained or lost needles. These include dental, obstetric and gynecologic, laparoscopic surgeries, spinal tap procedures and acupuncture procedures.
7
-18
There has been one report of retained intraocular surgical needle that had been incidentally identified 5 years from the inciting surgery
In some of these case reports, the initial surgical teams opted to leave the retained surgical needles after failure of attempted retrieval. It has also been shown that these patients later come back for complications such as inflammation, bleeding, chronic pain, and in severe cases, migration to vital structures such as the heart. 7,10,11 -14,17,18 A summary of these events are presented in Table 1.
Summary of Case Reports on Retained Surgical Needles.
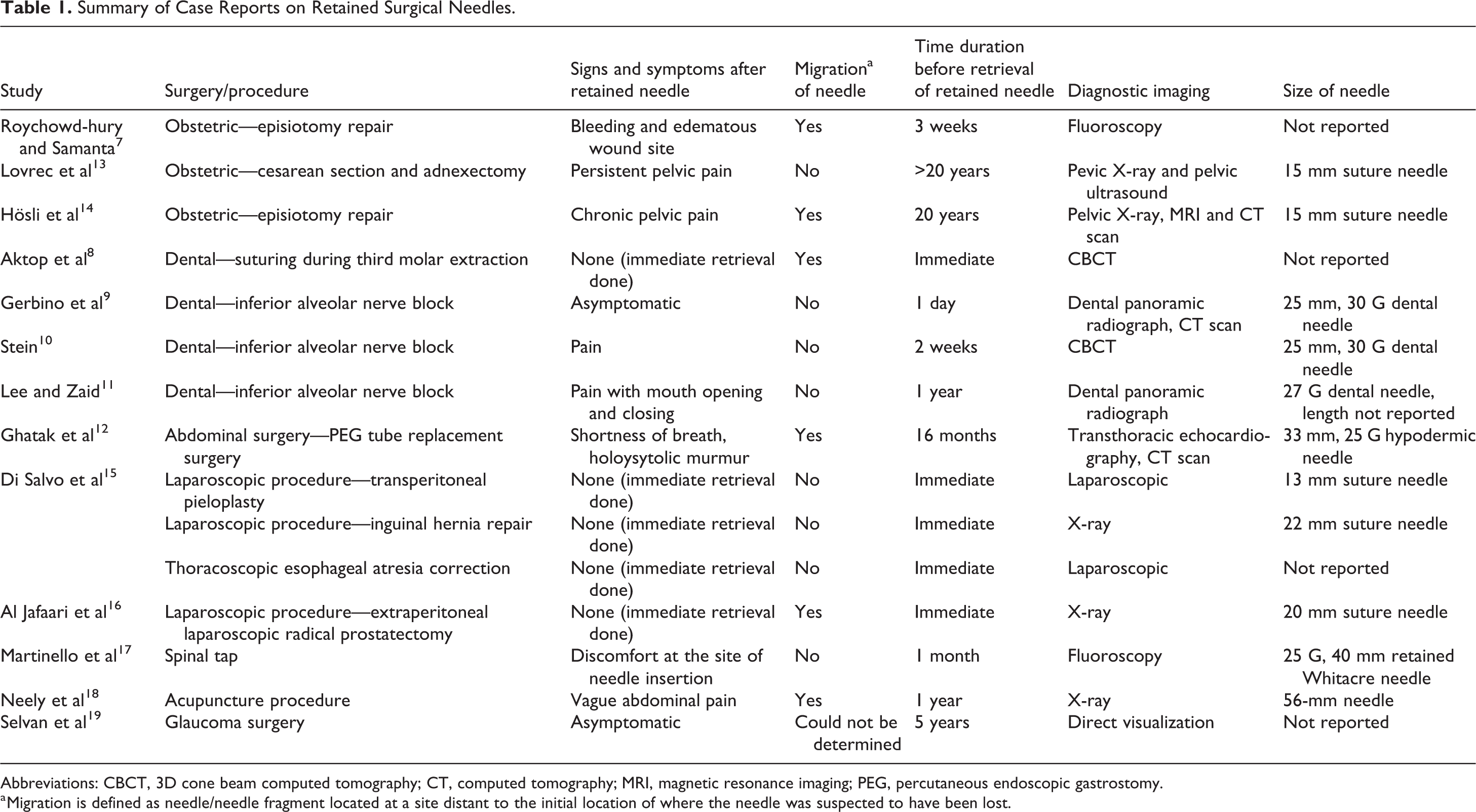
Abbreviations: CBCT, 3D cone beam computed tomography; CT, computed tomography; MRI, magnetic resonance imaging; PEG, percutaneous endoscopic gastrostomy.
a Migration is defined as needle/needle fragment located at a site distant to the initial location of where the needle was suspected to have been lost.
To the best of our knowledge, there are no reports of retained needle during facial laceration repair. Although these “never events” have a negative stigma, we argue that there is value in discussing and dissecting these to draw out invaluable learning points for all surgeons.
Case description
A 40-year-old Chinese male presented at the Accidents & Emergency Department (A&E) after being thrown off of his motorcycle when it rammed on the back of a truck. The patient sustained extensive multiple facial lacerations and was referred to oculoplastics for a deep gaping right upper lid laceration, suspecting involvement of the periorbita and intraorbital penetration. After stabilizing, the patient was brought to the operating theater (OT) for wound debridement. On examination, findings included a gaping macerated nonmarginal laceration at the right upper lid measuring 40 mm × 30 mm extending from the medial upper lid up to the medial 2/3 of the right brow, a large macerated nonmarginal laceration in the right lower lid temporal to the punctum and extending inferolaterally to the cheek, and a 10-mm nonmarginal horizontal laceration on the lateral aspect of the left upper lid (Figure 1).
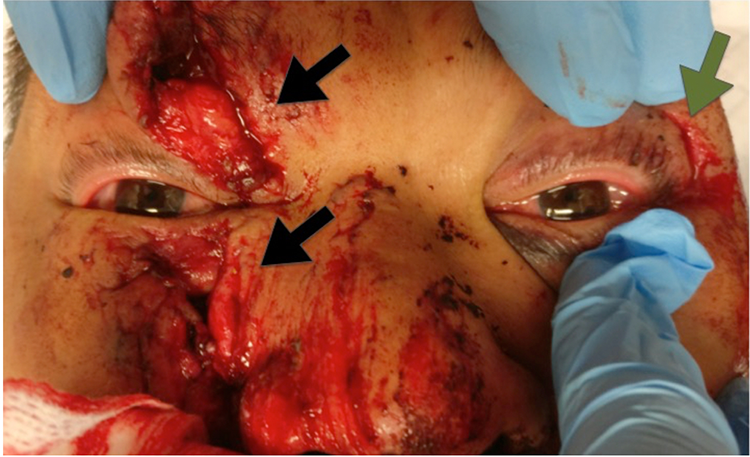
Black arrows show gaping macerated nonmarginal laceration at the right upper and lower lid. Green arrow shows horizontal laceration at the left upper lid.
There was no step deformity palpated along superior and inferior orbital rim, palpebral conjunctiva was not breached. The anterior segment examination was unremarkable, except for sluggish pupillary reflex bilaterally attributed to pharmacological effect of propofol and fentanyl. Posterior segment examination was otherwise unremarkable. At the A&E, a non-contrast CT of the brain was requested that showed soft tissue swelling of bilateral periorbital and facial regions, with embedded foreign bodies on the left supraorbital area. No orbital fractures were identified (Figure 2A and B).
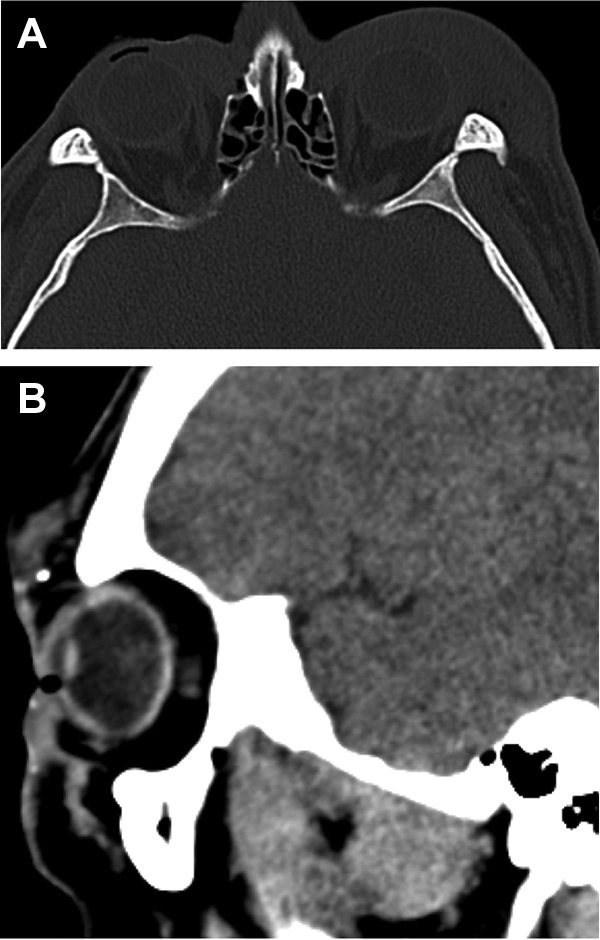
A, CT scan, bony window, axial view showing bilateral periorbital soft tissue swelling, more on the left, with intact bony orbit. B, CT scan, soft tissue window, sagittal view showing embedded pinpoint foreign bodies on the left supraorbital area.
Intraoperatively, debridement was done with copious irrigation of saline admixed with gentamycin. Probing and syringing through the inferior punctum, showed freely patent lacrimal duct. The right upper lid preaponeurotic fat pad was identified and orbital septum was left open. Upon closure of deep soft tissues with reverse cutting vicryl 6-0, the needle detached from the suture. Attempt at locating needle was unsuccessful, and surgical team decided to use a portable X-ray image intensifier which did not show evidence of a needle within the wound site (Figure 3).
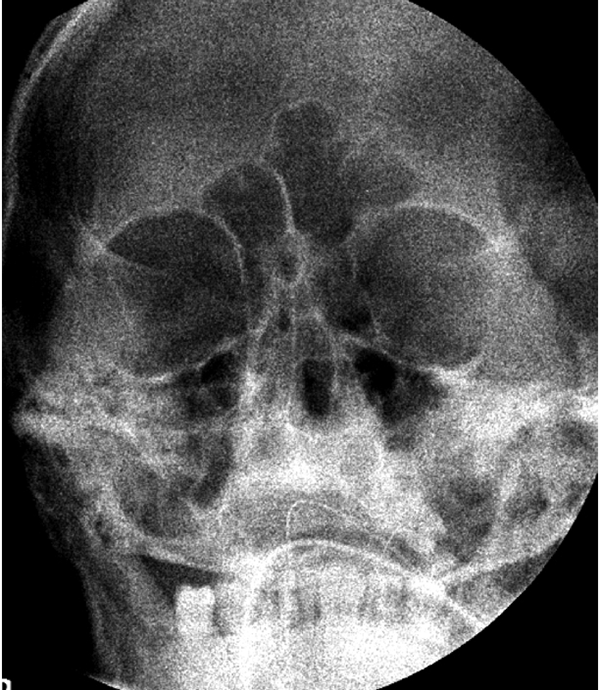
Image intensifier showing no evidence of foreign body.
Closure was then completed, and the patient was sent back to surgical ICU for further monitoring. On postoperative day 1, repeat CT scan of the face was done which revealed a linear metallic density in the right frontal soft tissue, over the medial superior orbital rim, likely representing the detached surgical needle (Figure 4A to B).
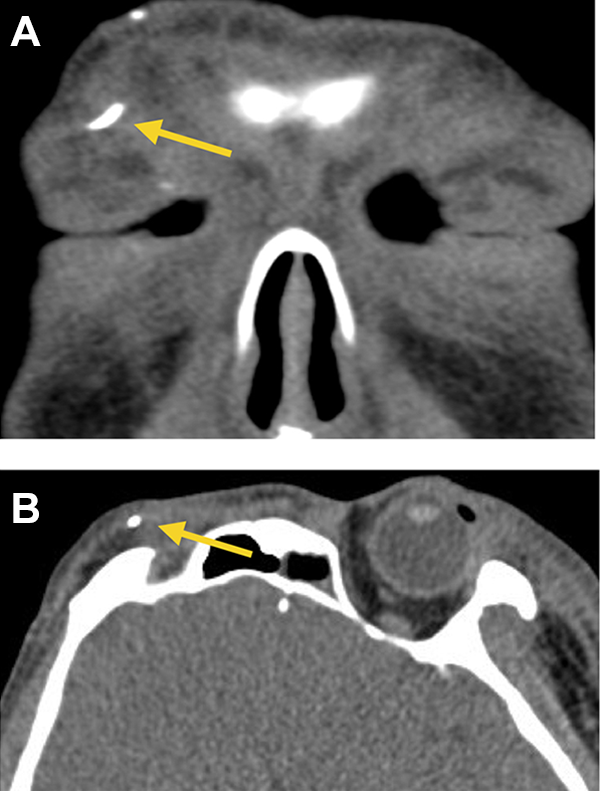
A, CT scan, soft tissue window, coronal view, shows evidence of linear metallic density over right frontal soft tissue as shown by the arrow. B, CT scan, soft tissue window, axial view showing same linear metallic density over the right medial superior orbital rim.
After detailed discussion with the patient, decision was made to perform surgical wound exploration to retrieve the suspected needle foreign body. Under local anesthesia, using the CT scan as a guide, the wound was explored along the expected location of the foreign body superficially along the tissue plane. Despite meticulous dissection, the foreign body was not directly visualized. An intraoperative magnetic probe was utilized which demonstrated tenting of skin upon application (Figure 5A and B). This allowed better localization and detection of the foreign body, which was removed in entirety (Figure 6). Closure of wound was done and the patient tolerated the procedure well.
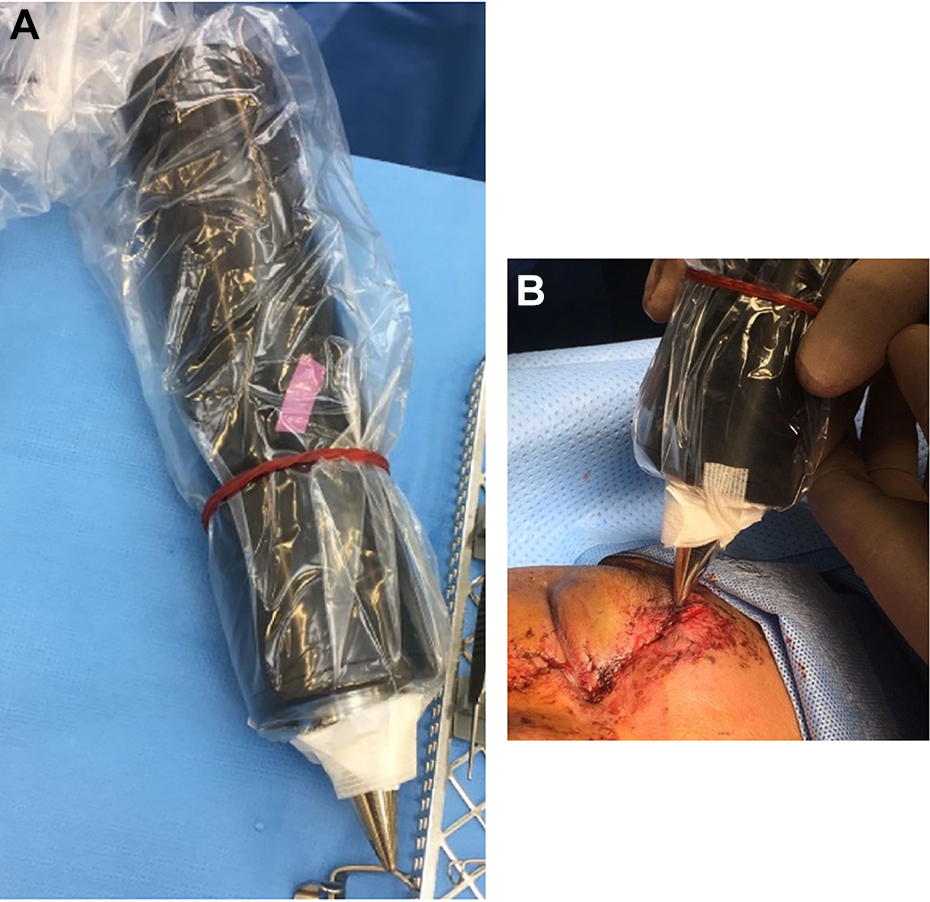
A, Intraoperative magnetic probe. B, Intraoperative magnetic probe being utilized to detect foreign body.
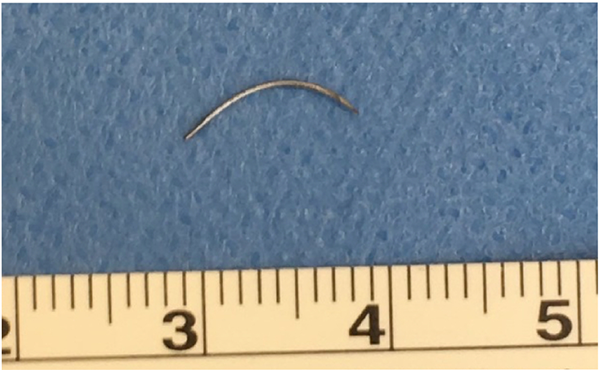
Retrieved surgical needle measuring approximately 11 mm.
Discussion
Managing retained surgical needles begin with demonstrating correct suturing technique and habits. A good surgeon knows when to use the appropriate needle and suture material for anastomosis of specific tissue types, ensuring that suture strength is adequate for different tissues and degrees of tension. In managing the needle while in the surgical field, a coordinated use of tissue forceps and needle holder is criticial. A common error in handling tissue while suturing is to release the forceps from the skin edge, letting the skin retract, and risk losing the needle beneath the skin edge, especially for deep and thick tissues. The key is to maintain the position of the skin edge while releasing the needle from the needle holder. 20 Harnessing good suturing techniques and habits prevent the surgeon from losing sight of the needle at all times during the surgery.
Once the needle is lost, visualization, whether directly or indirectly, while in the surgical field, is the next challenge for the surgeon. One study proposed a protocol for when the needle is lost during minimally invasive surgery. After initial survey does not reveal the needle, they recommend the use of an intraoperative magnetic needle retriever which is a reliable and rapid method for recovery. 21
If this method fails, portable radiographic machine (also known as mobile image intensifier) can be utilized.
In a study by Macilquham et al, majority of their observers were able to identify 17-mm surgical needles, but they report that for needles less than 13 mm, mobile image intensifiers will not be as accurately useful for this purpose. 22 This was demonstrated by this case report where the 11-mm needle was not identified in the image. Detection of the foreign body with X-ray image intensifiers may be limited by patient weight and radiographic exposure, as well as the size of foreign body to create contrast to its surrounding area. Detection rate may decrease with increased patient weight as this decreases radiographic contrast to noise ratio, thereby reducing image quality. 22,23
For attempts with image intensifiers that remain unsuccessful or retained surgical foreign body that is <13 mm, a CT scan is advised. 2 Coupled with an experienced radiologist, CT remains to be the imaging of choice for the diagnosis of RSI, especially radiopaque materials such as needles. 5 Ultrasound does not yield good results in localizing foreign body, especially in areas that they are not used as a primary diagnostic tool such as the orbit, skin, and subcutaneous tissue.
Despite good visualization with CT, an accurate identification of foreign body from imaging data may not be as predictable once in the surgical field. If scans will be used to guide wound exploration, it is recommended that the spatial location of the foreign body should be done with reference to important anatomic landmarks or identifiable surrounding large blood vessels. 22 For foreign bodies found in difficult, narrow, and deep areas, another recommendation is to use image-guided navigation system for preoperative and intraoperative planning. 9 -11,24
Conclusion
The ideal management for retained needles remains to be prevention addressed by surgeon’s good suturing habits. But these intraoperative accidents happen and when it does, it is important to have a systematic judicious response approach. Visualization remains to be the biggest challenge. If available, intraoperative magnetic probes can be utilized. Mobile imaging intensifiers can be utilized for needles >13 mm. Otherwise it is prudent to perform CT scan and will unfortunately require a secondary surgery for exploration. With CT scans as guide for exploration, anatomical landmarks may be used for better spatial orientation. Finally, image-guided navigation systems may also be of benefit in localizing retained needles but can be quite expensive and may not be readily available for most facilities.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
