Abstract
In naso-orbito-ethmoid (NOE) fractures, a highly complex and delicate region is involved. Commonly, the focus of most clinicians goes to the esthetical disfigurations, such as the loss of nasal projection, position of the medial canthal tendon or enophthalmos/hypoglobus, or the functional problems such as diplopia. Nasal investigation is mandatory in these fractures, but the focus is on nasal septum in the concommitent nasal fractures. In minimally displaced NOE fractures, these clinical problems are not always present to justify surgical treatment. In this article, we present a series of 5 patients with minimally displaced (unilateral) NOE fractures with a nasal obstruction as a solitary and persistent symptom of a NOE fracture.
Introduction
Naso-orbito-ethmoid (NOE) fractures, traumatic defects in the highly complex confluent region of the nasal bone, ethmoidal sinus, frontal sinus, and anterior skull base, account for approximately 5% of all facial fractures. 1 This delicate and small region contains multiple important anatomical structures (eg, the medial canthal ligament, the lacrimal drainage system, and the olfactory and infraorbital nerves). NOE fractures can exist solitary or as part of other midfacial fractures such as Le Fort I, II, and III, orbital blowout, and zygomatic bone fractures. The tortuous regional anatomy of the NOE complex classifies these fractures among the surgically most challenging traumatic defects of the maxillofacial region.
Whereas commonly accepted indications for surgical intervention include a loss of projection of the nose (eg, a saddle nose deformity), asymmetry or functional deficits (diplopia, epiphorea, enophthalmos and hypoglobus in concomitant orbital wall fractures, lacrimal duct damage, or leakage of cerebrospinal fluid in concomitant skull base fractures)—the key factor determining the necessity and method of surgical repair is the presence and type of medical canthal tendon (MCT) malpositioning, resulting in a debilitating traumatic telecanthus. 2,3 Dislocation of the MCT can cause severe disruption of the facial harmony, either through dislocation of the bony fragments (Markowitz type I and II) or because of detachment of the ligament (Markowitz III). An increase of the intercanthal distance or a traumatic telecanthus of more than 35 mm is considered abnormal and is generally considered to require surgical intervention. 4 Hence in most cases, after careful clinical examination and supported by computed tomography (CT) findings, the diagnosis of dislocated fractures with MCT malpositioning determines the decision to operate. However, in minor NOE fractures with only slight displacement and without MCT malpositioning, common associated symptoms such as mild diplopia and infraorbital paresthesia frequently resolve without intervention, and therefore controversy still exists over the proper way to manage fractures with CT evidence of only minimal dislocation. 4
Similarly, in the acute phase of midface injuries, there is often significant mucosal swelling with subsequent nasal congestion which generally resides over time. Unfortunately in clinical practice, these symptoms may camouflage functional nasal disability and subsequently fail to adequately diagnose the resulting of chronic nasal obstruction after the acute phase of NOE fracture management. To our knowledge, it has not been previously reported that chronic nasal obstruction may result from NOE fractures, in the absence of an associated nasal septum deviation. Therefore in this article, a series of patients are presented in whom persistent nasal obstruction, as a forgotten solitary symptom, developed as a result of minimally dislocated (unilateral) NOE fractures. In 2 cases, peak inspiratory flow was measured pre- and postoperatively. In none of the cases, preexistent nasal septum deviation or nasal obstruction was reported or clinically observed.
Case Description
Case 1
A 50-year-old male presented at the emergency department after a sports-related head injury (soccer). Besides a periorbital hematoma on the left side, there was no loss of bony projection of the nose, no eye motility disorders, no diplopia, and the infraorbital nerve was symmetrically intact. On CT scan, a minimally displaced fracture of the left orbital floor and medial wall, a non-displaced nasal fracture, and a minimally displaced fracture of the maxillary sinus were diagnosed. Because of the absence of functional limitations, a conservative treatment strategy was chosen. At a follow-up appointment, 10 days after trauma, the patient complained about anosmia. After careful clinical examination, a complete nasal obstruction on the left side was diagnosed. Transoral open reduction and internal fixation (ORIF) with a paranasal osteosynthesis plate was chosen as suitable treatment. Six weeks after surgery, there was a full recovery of the nasal airway, without other complaints.
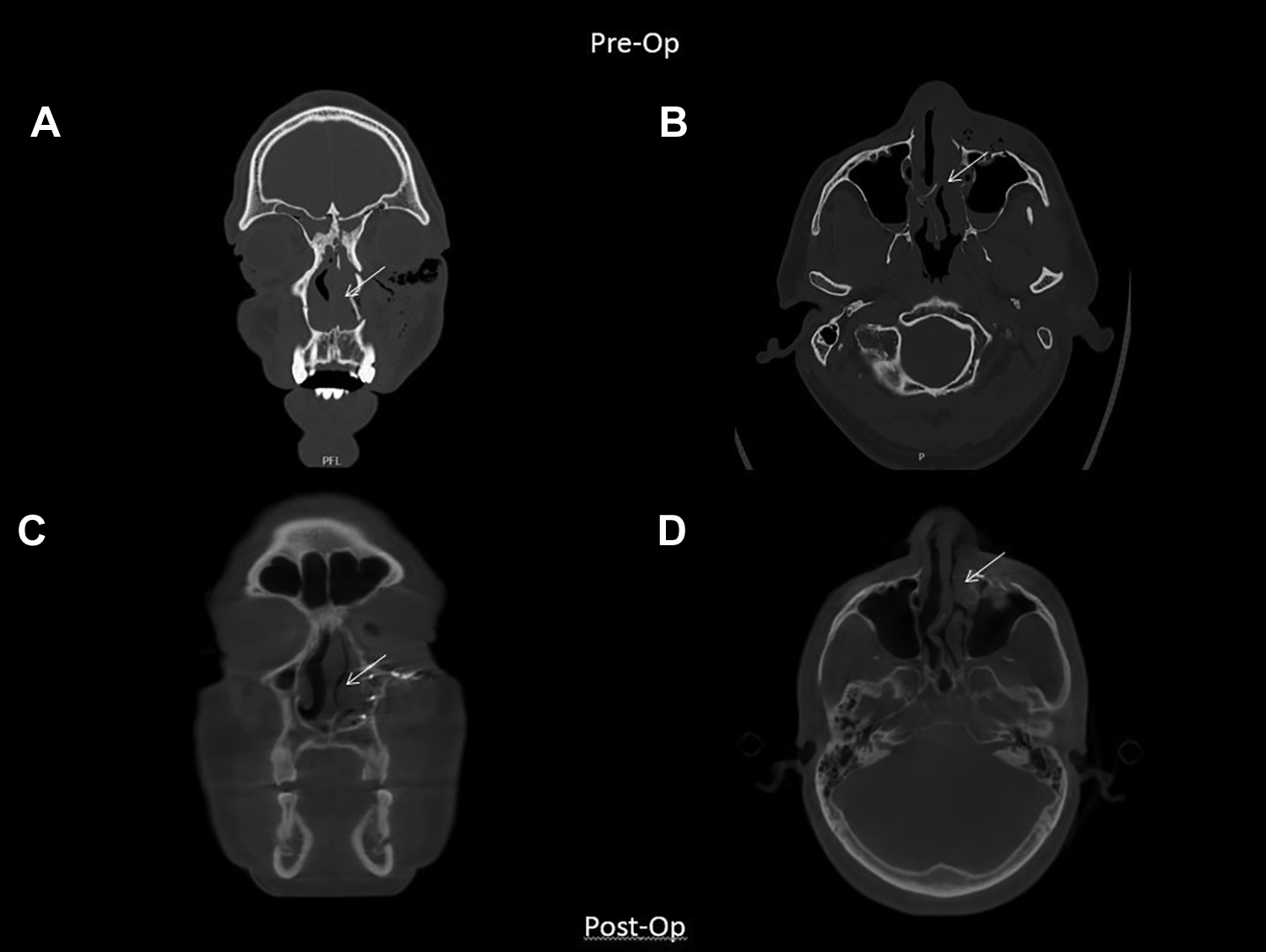
Case 1: (A) coronal slide of nasal obstruction at presentation, (B) axial slide of nasal obstruction at presentation, (C) coronal slide of restored airway 6 weeks after surgery, and (D) axial slide of restored airway 6 weeks after surgery.
Case 2
An 18-year-old male presented with head injury at the emergency department after being physically assaulted. The CT scan showed a non-dislocated zygomatic complex fracture at the left side and a fracture of the nasal bone. There was some paresthesia of the infraorbital nerve. The patient did not suffer from eye motility disorders or diplopia. Ten days post-trauma, the patient experienced complaints of nasal obstruction on the left side, and still some hypesthesia. In retrospect, a unilateral NOE type I fracture on the left side with nasal obstruction was missed. Subsequently, the fracture was reduced under general anesthesia through a transoral approach and fixated with 1 paranasal osteosynthesis plate. Direct after treatment, the patient reported a recovery of the nasal passage.
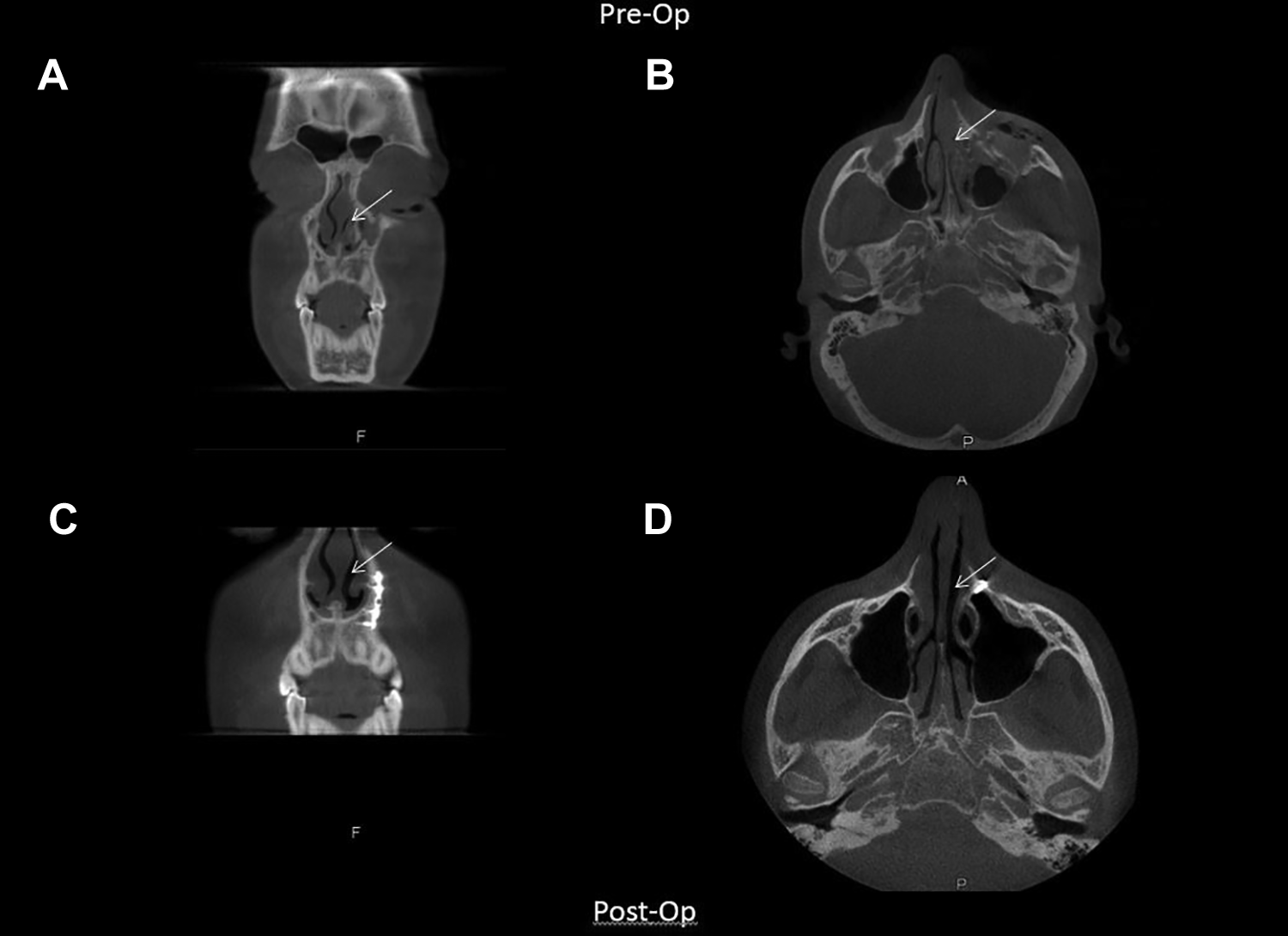
Case 2: (A) coronal slide of nasal obstruction at presentation, (B) axial slide of nasal obstruction at presentation, (C) coronal slide of restored airway 5 weeks after surgery, and (D) axial slide of restored airway 5 weeks after surgery.
Case 3
One day after a sports-related head injury (soccer), a 38-year-old male visited his general practitioner (GP). Apart from a periorbital hematoma on the right side, there were no further clinical symptoms. No radiographic studies were initially performed. However, after 3 months, the patient returned to the GP with complaints of a persistent stuffy nose on the right side. The patient was referred to the department of Oral and Maxillofacial Surgery (OMFS) where a conebeam CT scan showed an untreated and dislocated unilateral NOE fracture. At careful clinical examination, it was further found that there was an obstructed nasal airway on the right. In general anesthesia, the right NOE complex was osteotomized through a combined transoral and transconjuctival approach and fixated with 2 osteosynthesis plates. The patient reported a full recovery of the nasal airway 6 weeks postoperatively.
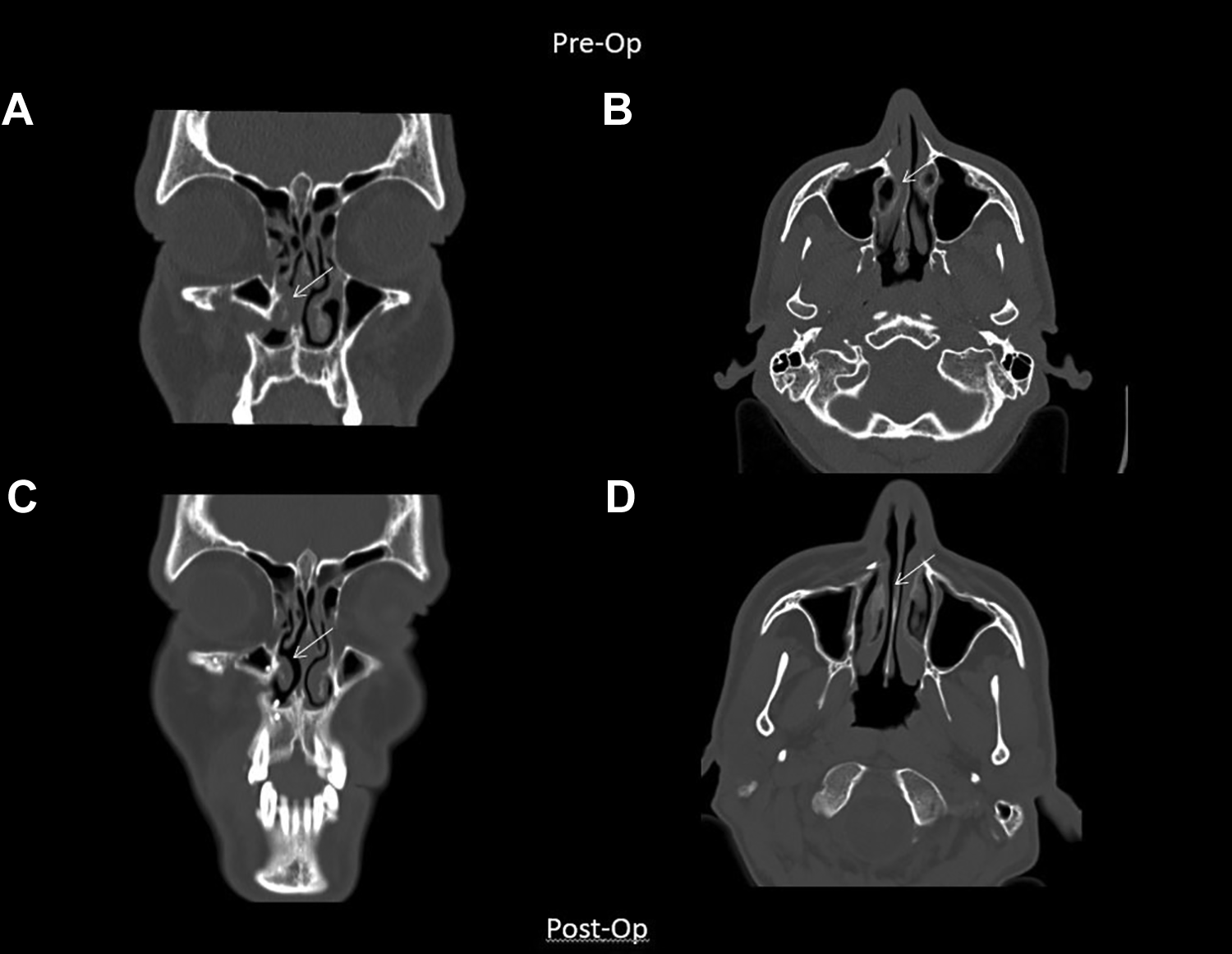
Case 3: (A) coronal slide of nasal obstruction 3 months after injury, (B) axial slide of nasal obstruction 3 months after injury, (C) coronal slide of restored airway 6 weeks after surgery, and (D) axial slide of restored airway 6 weeks after surgery.
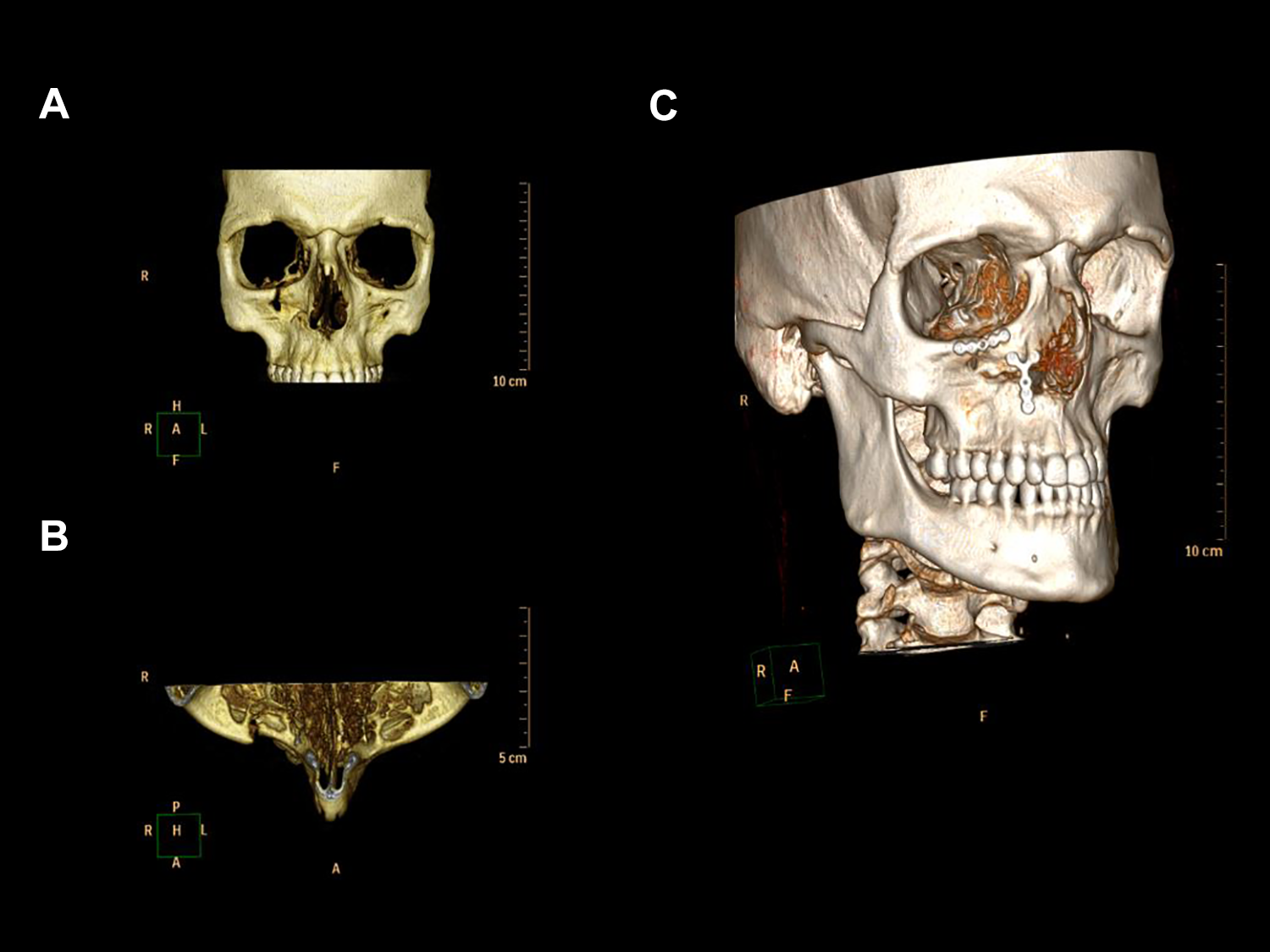
Case 3: (A) 3D reconstruction, frontal view of missed unilateral NOE I fracture 3 months after injury, (B) 3D reconstruction, cranial view of missed unilateral NOE I fracture 3 months after injury, and (C) 3D reconstruction after NOE osteotomy 6 weeks after surgery. NOE indicates naso-orbito-ethmoid.
Case 4
A 71-year-old female presented at the emergency room with facial injury after a traffic collision (car vs car). At clinical examination, there was a periorbital hematoma on the left side. There was a small bony step palpable at the left infraorbital rim. Eye motility was not disturbed, and there was no diplopia. CT examination showed a unilateral NOE type I fracture with minor dislocation. Although there was mild intra-orbital emphysema, the orbital volume was not increased. The patient had a concomitant non-displaced, nonmobile Le Fort I fracture in association with the non-displaced NOE fracture at the left side. As there were no clinical functional symptoms, an expectative conservative policy without intervention was the therapy of choice. Nine days post-trauma, an obstructed nasal airway was the only symptom. A peak nasal inspiratory flow (PNIF) was measured, and the preoperative score was 40 (L/min). One week after transoral reposition and fixation with 1 paranasal osteosynthesis plate, the PNIF increased to 70. At 6-months follow-up, it rose to 73.
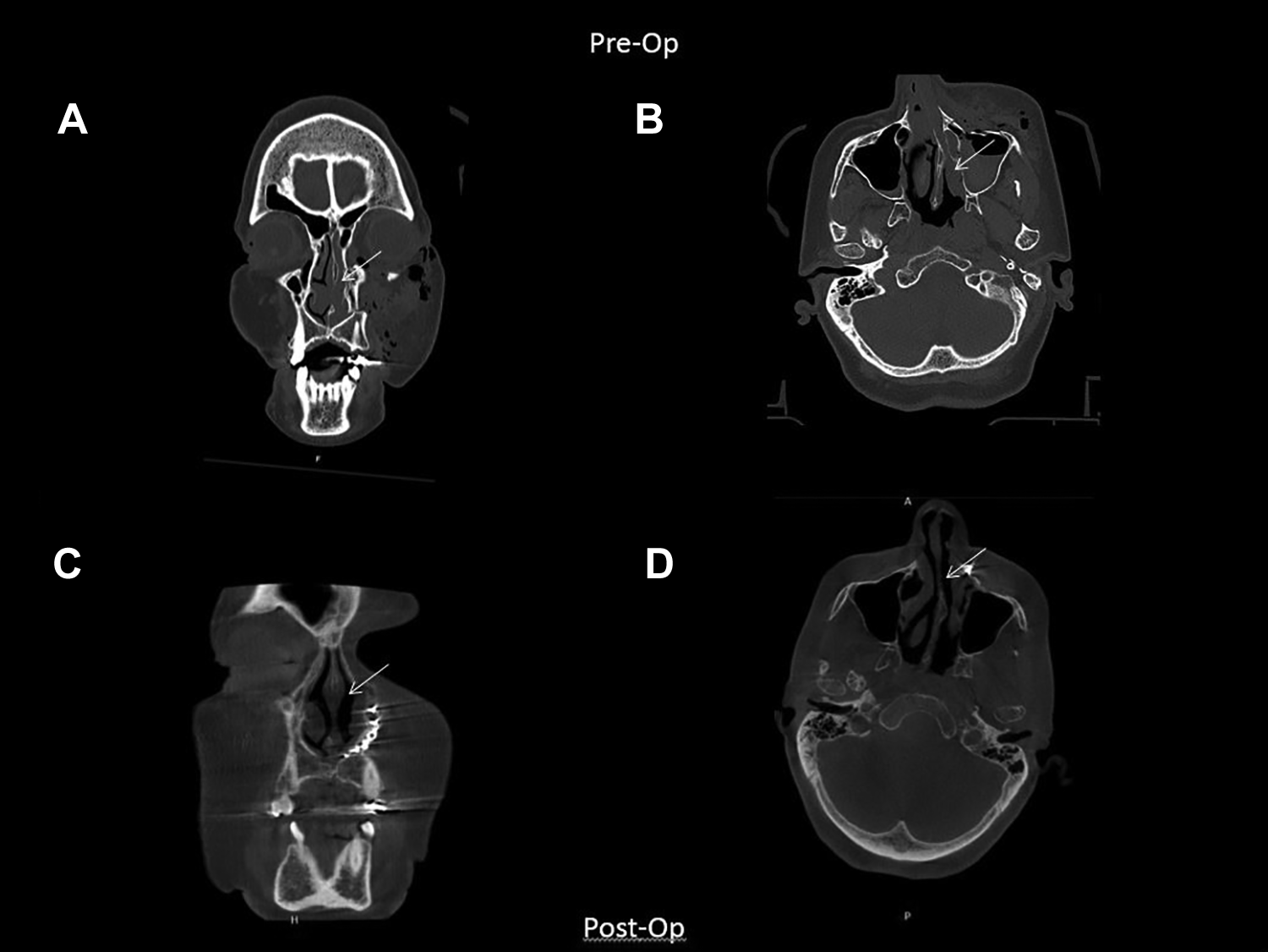
Case 4: (A) coronal slide of nasal obstruction at presentation, (B) axial slide of nasal obstruction at presentation, (C) coronal slide of restored airway 6 weeks after surgery, and (D) axial slide of restored airway 6 weeks after surgery.
Case 5
A 42-year-old male with head injury was referred to the department of OMFS after being physically assaulted. At clinical examination, the bony projection of the face was symmetrically intact, without palpable steps. The eye motility was not disturbed, and there was no diplopia. There was hypesthesia of the left infraorbital nerve, and the nasal airway was congested at the left side. The PNIF was 30 L/min. A CT scan showed a minimally displaced NOE type I fracture on the left.
Through an intraoral approach, the fractures were repositioned and fixated with a paranasal plate. Three months after surgery, the infraorbital nerve had fully recovered. The patient did not have any complaints related to the nasal airway and the PNIF had increased to 150 L/min.
After 6 weeks, none of the patients had complaints of nasal obstruction, nasal secretion, and traumatic rhinitis or experienced an altered sense of smell. All patients had full recovery of the nasal airway, clinically and on the postoperative CT scan.
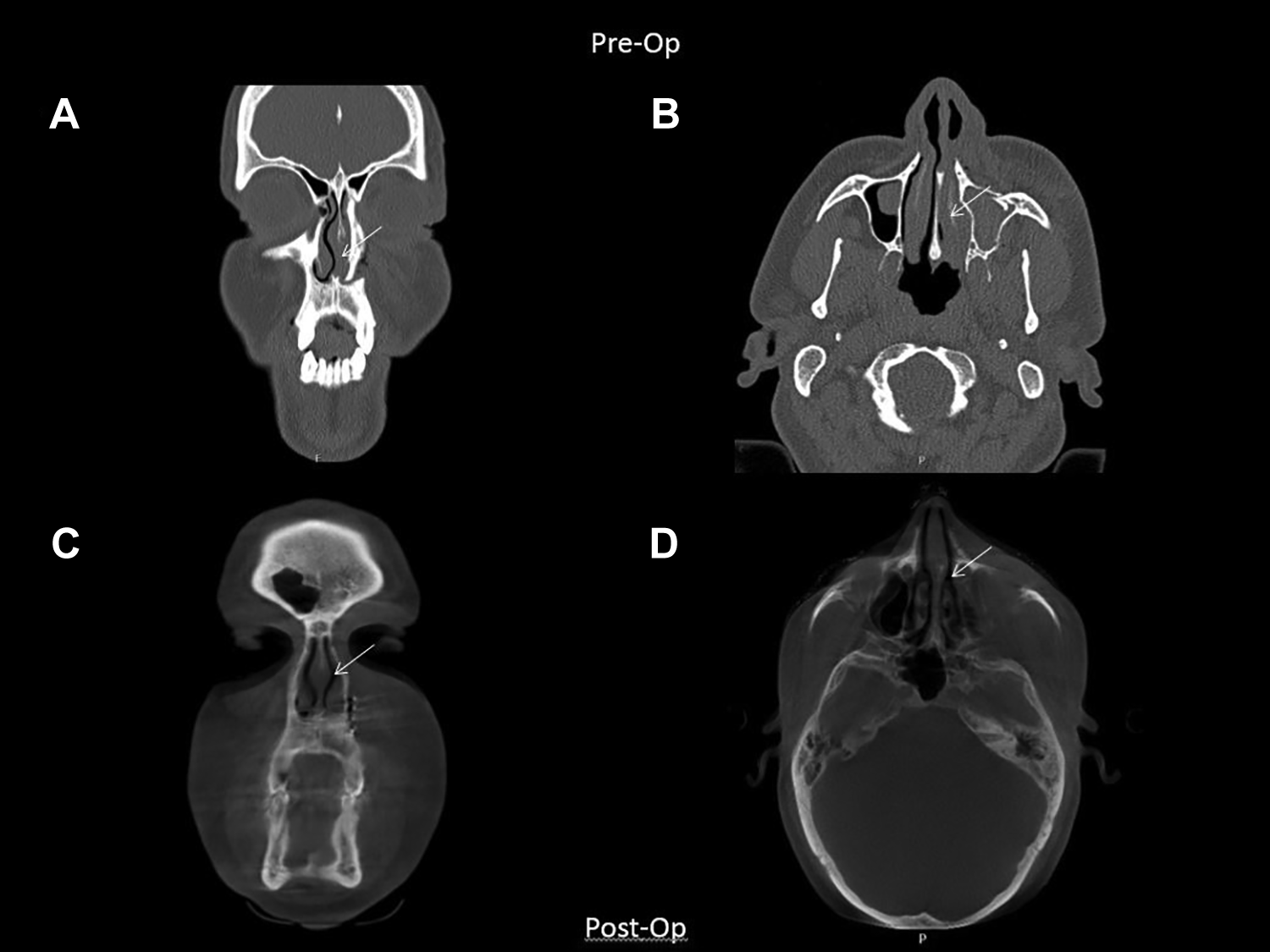
Case 5: (A) coronal slide of nasal obstruction at presentation, (B) axial slide of nasal obstruction at presentation, (C) coronal slide of restored airway 1 week after surgery, and (D) axial slide of restored airway 1 week after surgery.
Discussion
In this case series, 5 patients were presented in whom persistent nasal obstruction, as a forgotten solitary symptom, developed as a result of a minimally dislocated (unilateral) NOE fractures. Nasal obstruction can be caused due to traumatic septum deviations, 5 frontal sinus mucositis, 6 traumatic mucocele, 6 or paranasal sinusitis 6 ; however to the best of our knowledge, no cases with nasal obstruction as a solitary symptom of a slightly dislocated (unilateral) NOE fracture have been previously published in the literature.
All patients presented were diagnosed with a (unilateral) NOE fracture (type I). Apart from the usual post-traumatic discomfort, nasal obstruction was not noted as a distinct symptom on early investigation by any of the 5 patients. In these cases, the clinician involved in the acute phase after trauma may have focused primarily on the extent of the facial fracture and on whether or not there had been an indication for immediate surgical intervention. Further, other functional deficits including diplopia, enophthalmos, hypoglobus, lacrimal duct damage, or leakage of cerebrospinal fluid were not observed (Table 1). In retrospect, disturbance of nasal airway passage was not evaluated carefully, possibly because obstruction was considered to be associated with early post-traumatic intranasal swelling rather than structural bony obstruction. In 2 patients, the diagnosis of an underlying fracture was missed clinically.
Clinical presentation of patients with minimally displaced NOE fracture.
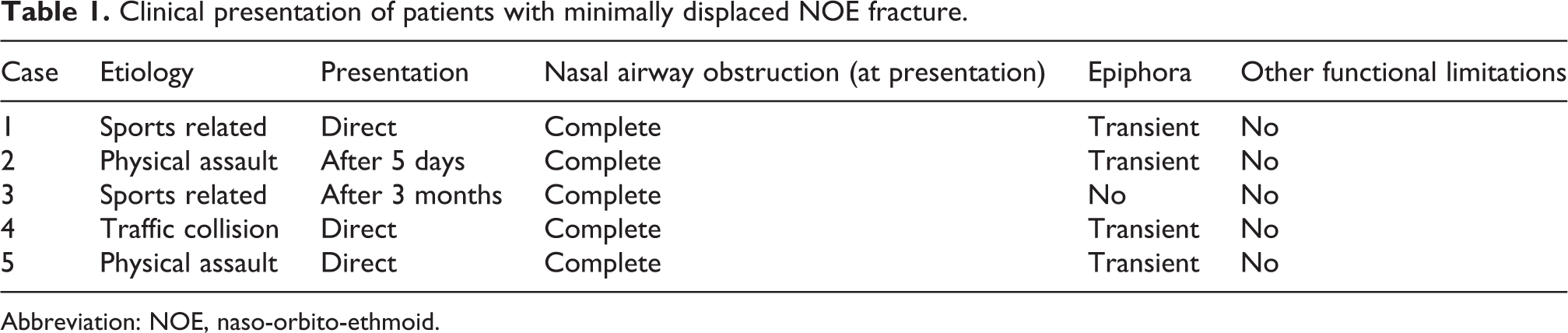

Abbreviation: NOE, naso-orbito-ethmoid.
Initial swelling or hematoma may mask underlying fractures, making it difficult to objectify the facial symmetry in minimally displaced and small fractures. Nowadays, CT scans are routinely performed in the trauma setting, certainly in midfacial trauma. The additional, detailed information that can be extracted from a CT scan about the fracture pattern may have been unnoticed in contrast to conventional plain images. 3 However, clinician ought not to rely on CT scans only in their treatment planning. Careful clinical examination remains mandatory, certainly in minimally displaced fractures. This examination should be repeated after the swelling has subsided to prevent missed and unwanted sequelae such as persistent nasal airway obstruction.
Repositioning of the septum was not required in any of the cases. Dislocation of the lateral nasal wall is frequently seen in NOE fractures and can result in esthetic problems. 4,7 If the dislocation is minor, the esthetic consequence is limited. However, the nasal obstruction can persist, be responsible for annoying disturbed nasal airway passage, and thereby become a clear indication for treatment of the (unilateral) NOE fracture. A simple reduction with a transoral positioned paranasal osteosynthesis plate resulted in direct improvement of the nasal airway passage in all primary cases. In 1 case, an osteotomy with a combined transoral–transconjuctival approach was used (Table 2).
Clinical course after reposition of the NOE fractures.
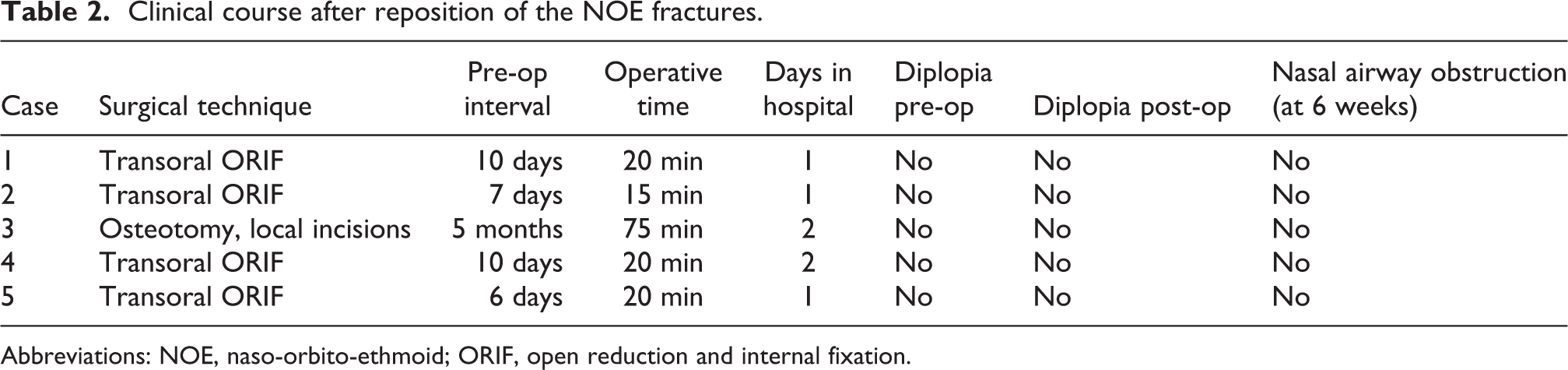
Abbreviations: NOE, naso-orbito-ethmoid; ORIF, open reduction and internal fixation.
PNIF can be used as a method for measuring the flow through the nose which indicates potential changes in nasal patency. In 2 patients, the PNIF was measured pre- and postoperatively and an improvement of PNIF was seen after repositioning of the NOE complex. PNIF can be useful to objectify the disturbed nasal airway passage and inform the clinician about possible changes during follow-up after reduction.
In conclusion, nasal obstruction can be a hidden sequela of NOE fractures, certainly in minor displaced fractures. During this early post-traumatic phase, nasal airway obstruction can easily be attributed to the hematoma and associated facial swelling and not be diagnosed as a separate entity. Attention for the nasal airway is essential for optimizing the clinical outcome. The transoral approach with 1 osteosynthesis plate on the nasal buttress is a simple and safe route for reduction and fixation of these fractures. Radiological and clinical evaluation have shown a well-aligned anatomic reconstruction and full recovery of the nasal airway.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
