Abstract
Introduction:
A young boy presented with mandibular swelling at the Department of Oral and Maxillofacial Surgery in Hospital Leforte, São Paulo, Brazil. Radiography showed a mixed bone lesion. Computed tomography (CT) findings were compatible with ameloblastic fibro-odontoma (AFO).
Case Report:
An excisional biopsy was performed under general anesthesia. At the 6-year follow-up, local inflammation and mild exudates were found. Local recurrence of the lesion was observed on CT. Therefore, excision and curettage were performed. No signs of recurrence have been detected to date. Ameloblastic fibro-odontoma is a rare benign neoplasm most commonly occurring in the first decade of life, with minimal probability of malignancy.
Conclusion:
Clinical, radiological, and histopathological findings aid in the diagnosis, and long-term follow-up is necessary as recurrence can develop even after 6 postoperative years.
Introduction
Ameloblastic fibro-odontoma (AFO) is a relatively rare mixed radiopaque/radiolucent tumor. It accounts for 0.3% to 1.7% of the cases of odontogenic tumors. 1 AFO lesions have unique features and are rarely recurrent. 1,2
Ameloblastic fibro-odontoma is a rare benign mixed odontogenic tumor composed of soft and hard tissues. 3 The soft tissue is predominantly the odontogenic epithelium and odontogenic mesenchyme, while the hard tissue has foci of dentin and enamel. 3,4 It occurs most commonly in the first two decades of life. 2
Ameloblastic fibro-odontoma is treated with enucleation, and the prognosis is excellent in children with small and asymptomatic lesions. For severe cases, radical treatments may be performed, but without involving the adjacent teeth. 5 –7
Here, we report a rare case of recurrent AFO in a young child at the 6-year follow-up.
Case Report
In 2011, a 6-year-old boy presented with a slight intraoral swelling of the external cortex of the mandible to the Department of Oral and Maxillofacial Surgery in University Hospital Leforte, São Paulo, Brazil. Radiography showed a mixed bone lesion, with involvement of the germ of the mandibular right third molar and mandibular right second molar. Computed tomography (CT) was performed to analyze the affected areas and evaluate the depth of the lesion. A histopathological analysis of an incisional biopsy specimen showed a mixed lesion compatible with AFO.
The entire lesion, including the tooth germs, was removed under general anesthesia. The removal resulted in a bone defect at the angle of the mandible on the right side (Figure 1A). Due to brittleness in the region of the bone defect, the defect was filled with bone marrow obtained from the iliac crest. Fixation was performed with absorbable inion plates.
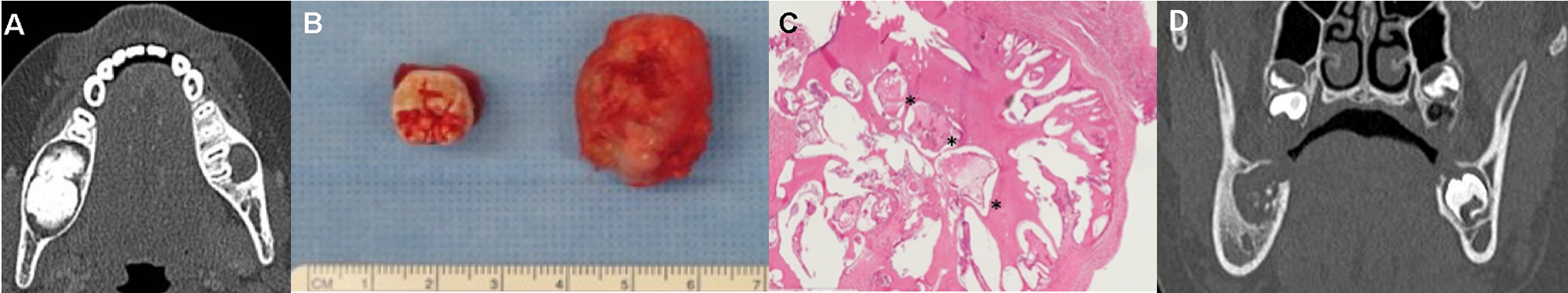
(A) Initial axial CT showing a mixed lesion, with a hyperdense center surrounded by a hypodense halo in the right mandibular retromolar area. (B) Anatomical aspect of the removed lesion and associated tooth. (C) Microscopic appearance of the lesion (hematoxylin–eosin stain, 400 µm). The soft tissue component is similar to those observed in the ameloblastic fibroma. Narrow cord and small islands of odontogenic epithelium impacted well-formed dentin-like component. (D) Postoperative CT after initial surgery. CT indicates computed tomography.
There were no postoperative complications. On postoperative day 37, the patient presented with local dehiscence in a small area in the suture region, which was treated with saline irrigation.
No abnormalities were detected for 6 years of follow-up. However, at the 6-year follow-up, he presented with local unevenness of bone thickness, exposed bone tissue, and mild local inflammatory exudates in the region of the retromolar space on the right side. A new lesion was detected on CT (Figure 2).
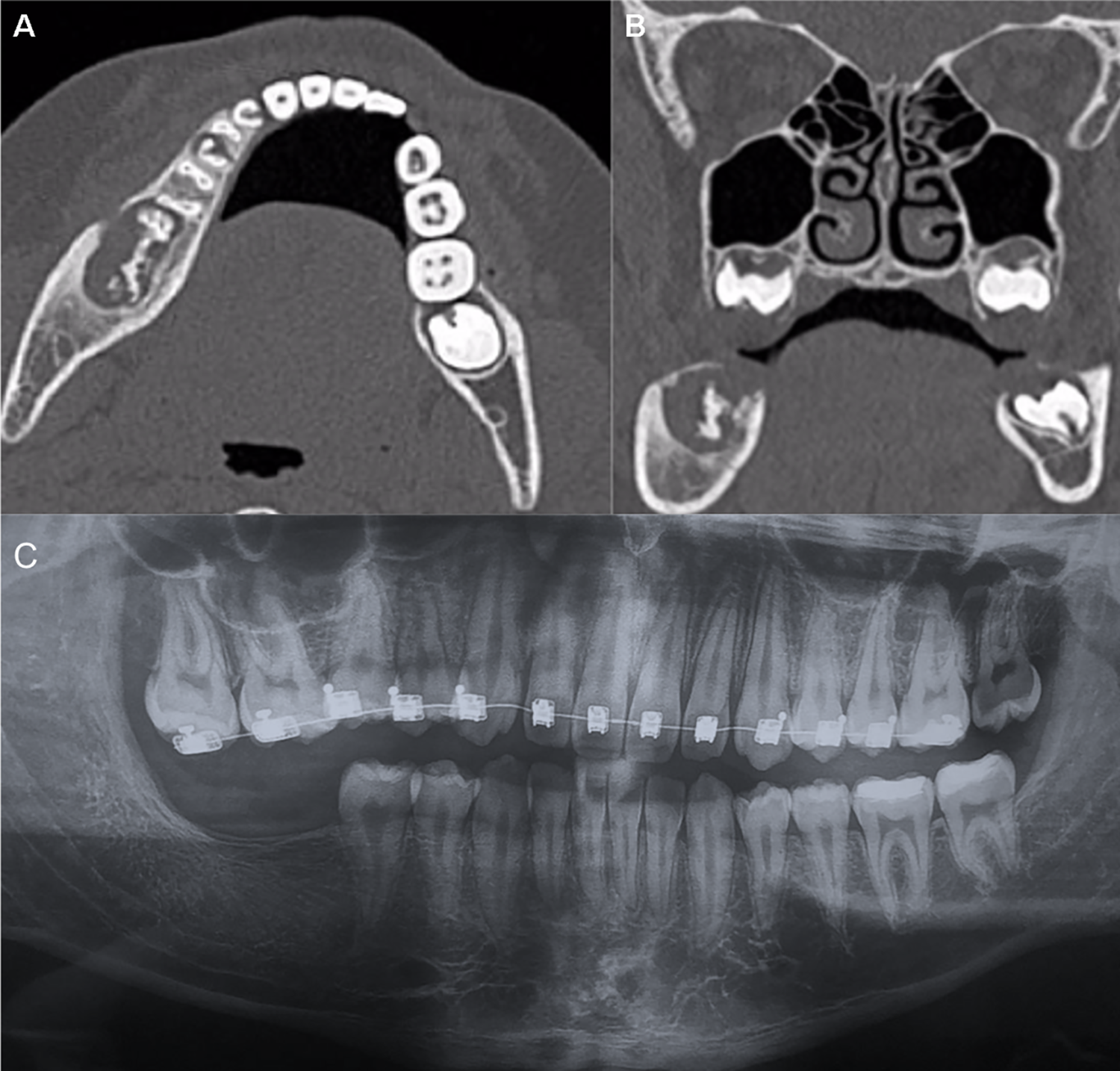
(A) Axial view of the CT scan after 6 years. (B) Coronal view of the CT scan after 6 years. (C) Panoramic radiograph 1 mouth after the second surgery, without lesion and ready for implants. CT indicates computed tomography.
Curettage was performed under general anesthesia to remove the lesion and adjacent soft tissues. A histopathological examination confirmed the relapse of AFO. No abnormalities were detected at the 6-month follow-up.
Discussion
The benign odontogenic tumor AFO is classified by the World Health Organization (WHO) as a rare tumor that exclusively affects children at a mean age of 6.3 years, 2 –7 as in the present case. AFO is not aggressive, so it is not necessary to remove the adjacent oral tissues. Clinical, radiographic, and histopathologic features aid in the diagnosis.
Recurrence of AFO is also rare and occurs in approximately 6% of the cases. 2 The age of the present patient was compatible with that reported in the literature for the development of AFO, and relapse occurred after 6 years. A systematic review 4 showed that frequencies of AFO in the mandibular and maxillary regions were 65% and 35%, respectively.
Howell & Burkes 8 (1977) reported two cases of relapse of AFO and cellular differentiation of AFO to fibro-odontosarcoma. However, such differentiation to malignancy is rare, and the treatment for these cases is chemotherapy and radiotherapy combined with extensive surgical resection. 9
Ameloblastic fibro-odontoma is the histological combination of ameloblastic fibroma (AF) and complex odontoma. It shows the same benign histological behavior as AF. In contrast, ameloblastic odontoma is the histological combination of complex ameloblastoma and odontoma, which has the same invasive behavior as ameloblastoma. 10
There are controversies on the classification of AFO into AF and ameloblastic fibro-dentinoma. 3 In 1971, the WHO defined AF as a benign neoplasm composed of proliferation of the odontogenic epithelium, interspersed with ectomesenchyme, which resembles the ectomesenchyme of the dental papilla. AF involving the dentin and enamel progresses to AFO. 4 In the 2005 classification, AFO, AF, and ameloblastic fibro-dentinoma were defined as separate entities, and the possibility of malignant transformation of AF to ameloblastic fibrosarcoma was highlighted. Finally, in the 2017 classification, an association among the three pathologies was reported: AF and ameloblastic fibro-dentinoma were defined as the progression of AFO. Furthermore, it was reported that the malignant transformation of AF is rare. 5,6
Consensus among the authors on the first-choice treatment for neoplasia is total enucleation. In cases of relapse or malignant potential, resection with a wide margin or marginal mandibulectomy is recommended. Long-term radiographic monitoring is recommended because of the possibility of recurrences.
Conclusion
A long-term follow-up of AFO is necessary because of the possibility of recurrence, and an early diagnosis should be provided to avoid radical procedures.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
