Abstract
Cuff design is the most important aspect to work on for the accurate measurement of blood pressure. For the very first time, pressure distribution underneath different parts/components of the fabric cuffs was analysed in detail using an advanced interface pressure sensing system. The pressure distribution at the interface of the selected cuffs and an arm simulator were measured experimentally while simulating blood pressure measurement. Fabrics are the main cuff constructing material and a relationship was found between cuff fabric properties and pressure at the interface of the cuff and the arm simulator. It was also found that the pressure distribution under different parts of the same cuff varied due to the uneven contact of the cuff fabric with the arm simulator. Components attached to cuff fabric which facilitate blood pressure measurement either confine or drive fabric according to their size and placement; they may cause non-uniform interface pressure distribution on the human arm too. It was also examined whether the selected cuffs were applying higher or lower average pressure over the surface of the simulator and the range varied from 8 mmHg to 25 mmHg. This indicates that the subsequent pressure distribution inside the arm tissues and over an artery would also vary further due to the cuffs being of different designs. This study found that cuffs would be unable to transfer the required pressure over the artery to block blood flow as and when needed.
Keywords
Introduction
For indirect or non-invasive blood pressure measurement (BPM), cuffs of numerous designs are constructed and available commercially. BP measurement cuffs comprise different types of fabrics and components. Cuffs are constructed either by joining two layers of fabrics in such a way that a portion is made inflatable or a rubber bladder is sandwiched between two layers of fabrics to facilitate inflation during BPM. The former is termed a bladderless cuff while the latter is called a bladdered cuff. All cuffs have an inflatable portion in which a conduit for air passage is connected (for inflation and deflation) for BPM. Velcro is attached to the cuff to facilitate secure fastening to the limb.
The cuff is wrapped around the limb in such a way that the centre of the inflatable portion, which is known as the “Artery index”, should be over the artery for blocking blood flow during BPM. In case of an upper arm, the artery index is placed over the brachial artery to stop blood flow while inflating the cuff. Different designs have different types of constructing fabrics and varying types and sizes of components/parts as well. There is no specific position of a conduit and Velcro on the cuffs either. It is found that the placement of the components also varies from one cuff design to another. Different types of constructing fabrics along with different components may affect/interfere with pressure transference to the human limbs during BPM and in turn influence BP values. It would be interesting to examine cuffs of different designs by measuring pressure transfer under their bladder and other components.
Variation in pressure distribution under the same cuff over the arms of difference densities was found in the previous studies.1,2 This indicates that the pressure distribution changes as the mechanical properties of the human arm vary. A previous study related to the design of a new cuff found differences between the BP values when measured for soft and muscular arms of the same dimensions. 3 Similarly, it is also essential to carry out experimental investigations to learn about the effect of different designs of the BP cuff on pressure distribution over the arm. Previous studies carried out pressure measurement on metal cylinders; however, a metal cylinder doesn’t deform like an arm.4,5 An arm deforms under the pressurized cuff; therefore it is important to study pressure distribution at the interface of cuffs of different designs and an arm simulator while simulating the phenomena of BPM. The purpose of using the arm simulator is to present the human upper arm which can be deformed under pressure.
For this proposed study, an arm simulator was developed because tests could not be carried out directly on the human arm owing to the fact that the BP of the human subjects varies while performing different activities, due to varying hemodynamic, body mass index (BMI), the white-coat effect and during different times of the day.6–9 Measurement on human subjects requires ethical approval too, that’s why an arm simulator was constructed.
Previous studies did Finite Element Analysis (FEA) to predict pressure distribution and transmission under cuffs while mimicking the phenomena of BPM;5,10 however, simulation couldn’t take into account the effect of the complete cuff design, that is, all properties of constructing fabrics including other components attached to the cuffs. It is difficult to find the impact of the full design on cuffs performance through experimental exploration because it would be difficult to estimate through FEA.
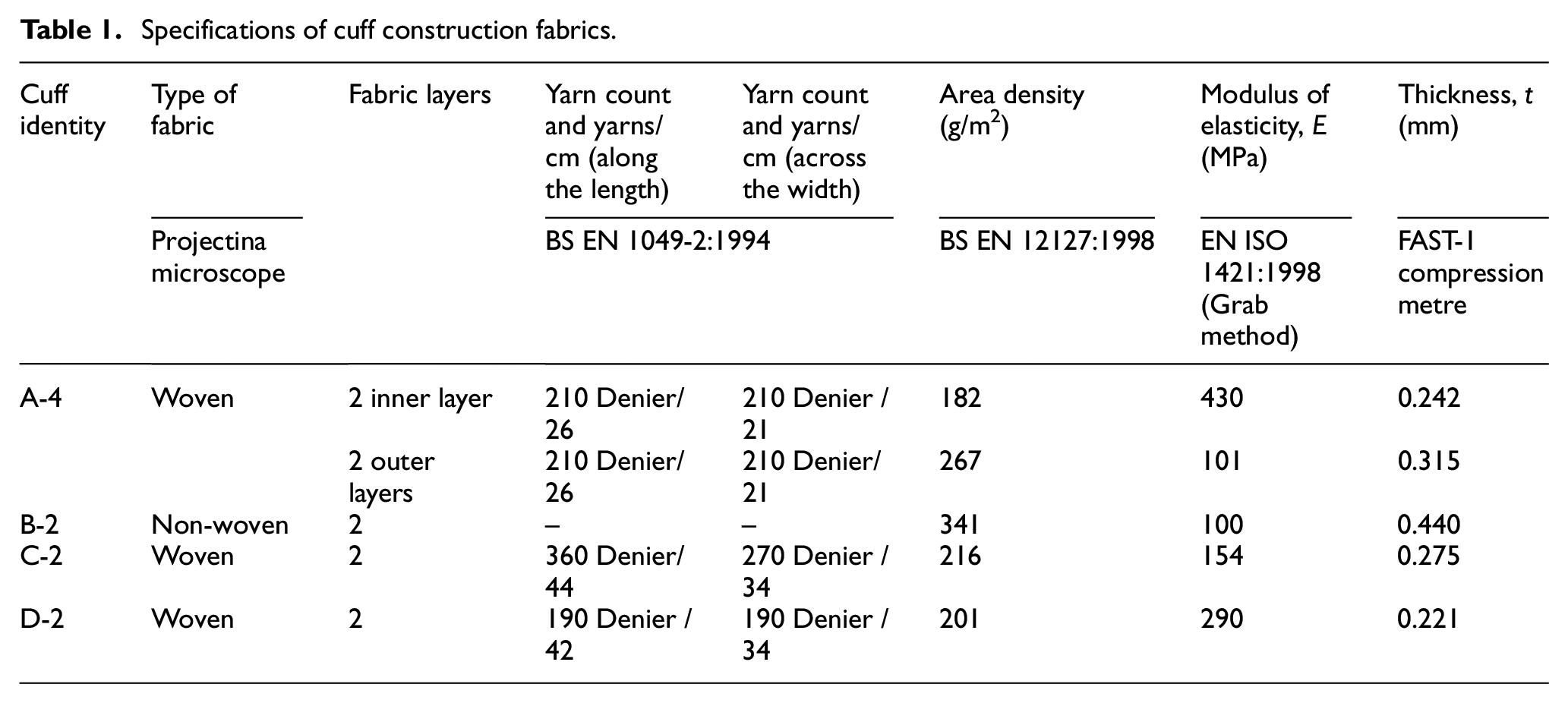
The importance of interface pressure (IP) measurement has been identified in different investigations related to the treatment of different diseases, health care and monitoring devices. Estimation of the IP under different cuffs may become an indicator of the actual pressure required to be transferred to the artery during BPM for accurate estimation of low and high BP values. This study would help in redesigning the cuffs as studies found variable pressure transfer by the cuffs and this may lead to variable values. 11 Since cuffs are constructed using different materials, it is important to examine pressure transference under each part during BPM, because there are no standard specifications of the fabrics and other the components required for cuff construction. Different fabrics have varying characteristics. Geometric and mechanical properties of the fabrics vary from one type to another (Table 1) along with the position of accessories so the pressure distribution and transmission may differ by the cuffs accordingly. Hence, the values of the blood pressure depend on the amount of pressure transmitted by the cuffs to the blood vessel.
Specifications of cuff construction fabrics.
In this experimental investigation, four BP cuffs of different design were selected and examined, constructed of either woven or non-woven fabrics having two or four layers. Velcro tape and air conduit were also attached with all selected cuffs. Cuffs were packaged and unused cuffs to avoid any prior distortion. Pressure distribution was measured at the interface of cuffs and an arm simulator while replicating the phenomena of BPM. Measurement of IP, in real time would help in finding potential effect of all the factors associated to the fabric cuffs design/construction on BPM. And hence it would make it possible to recognize relation between cuffs of different designs and pressure transmission to the arm during BPM. With the help of IP measurement, it was possible that the cuffs were wrapped around the arm simulator in a way that the IP was zero before commencing inflation manoeuvre to avoid inaccuracies due to the varying cuff tightness.1,12,13
Materials and Method
An arm simulator was developed by inserting a metal cylinder inside a foam cylinder, considering the shape of an arm as an axi-symmetrical cylinder. Foam material and a metal cylinder were used to imitate upper arm tissues and bone respectively. The length and circumference of the simulator were 23 cm and 42 cm, respectively. The circumference was within the recommended arm circumference range of the cuffs investigated.
In the selection of the foam material, it was assumed that the upper arm tissues have isotropic, linear and elastic properties. The compressibility of the foam material used was determined according to ISO 3386-1 on Zwick-Roell Z050. From the load-compression curve, stress-strain data were derived and the initial modulus was calculated and found to be 0.06 MPa which is close to the value of human tissues elasticity ranges from 0.09 to 0.145 MPa.
Four different designs of commercially available cuffs were procured, constructed from coated woven and coated non-woven fabrics. Identities were assigned A to D in which ‘4’ or ‘2’ represents the number of fabric layers in the respective cuff. Specifications of the cuff fabrics were evaluated using standard test methods and are listed in Table 1.
An I-Scan pressure sensing system by Tekscan was selected for the measurement of IP between the cuffs and the arm simulator. The selected sensing system is able to record the IP along the length and across the width of the cuffs at 96 sensing points in real time. A thin film calibrated sensor was positioned over the surface of the simulator. Then cuffs (one by one) were wrapped around the arm simulator so that the centre of the cuffs (artery index) was placed over the centre of the sensor. To measure the manometric pressure (inside cuff pressure), a mercury manometer was connected to the cuffs.
The experimental setup is shown in Figure 1. Before inflating the cuffs, it was assured that the IP and the manometric pressure were o mmHg. The pressure inside the cuffs was raised to 140 mmHg followed by step wise deflation with an interval of 20 mmHg to record IP against it.

Experimental set-up for interface pressure measurement.
All the measurements were repeated five times under each cuff with 3 minutes gap between the consecutive measurements. A3 minute gap is recommended between two consecutive BP measurements by the British Hypertension Society. The IP distribution in real time was presented as a colour coded peaks, see Figure 2(a) and (b). The correspondent numerical data as a text (ASCII) file, arranged in a matrix of 16X6, can also be recorded. Subsequently, the numerical data were programmed in the MATLAB 7.6.0.324 (R2008a) to remove the noise from all the observations as recommended by the I-Scan specialist and to average the repeated observations. The numerical data (ASCII) after averaging were transformed in 2D images using MATLAB graphical tools, shown in Figure 3(a)–(c). The new appearance of the results is more extensive to investigate pressure distribution under different parts of the cuffs. It would be easier to visualize the pressure transmitted particularly under the cuff’s artery index, the conduit for the air supply and Velcro.
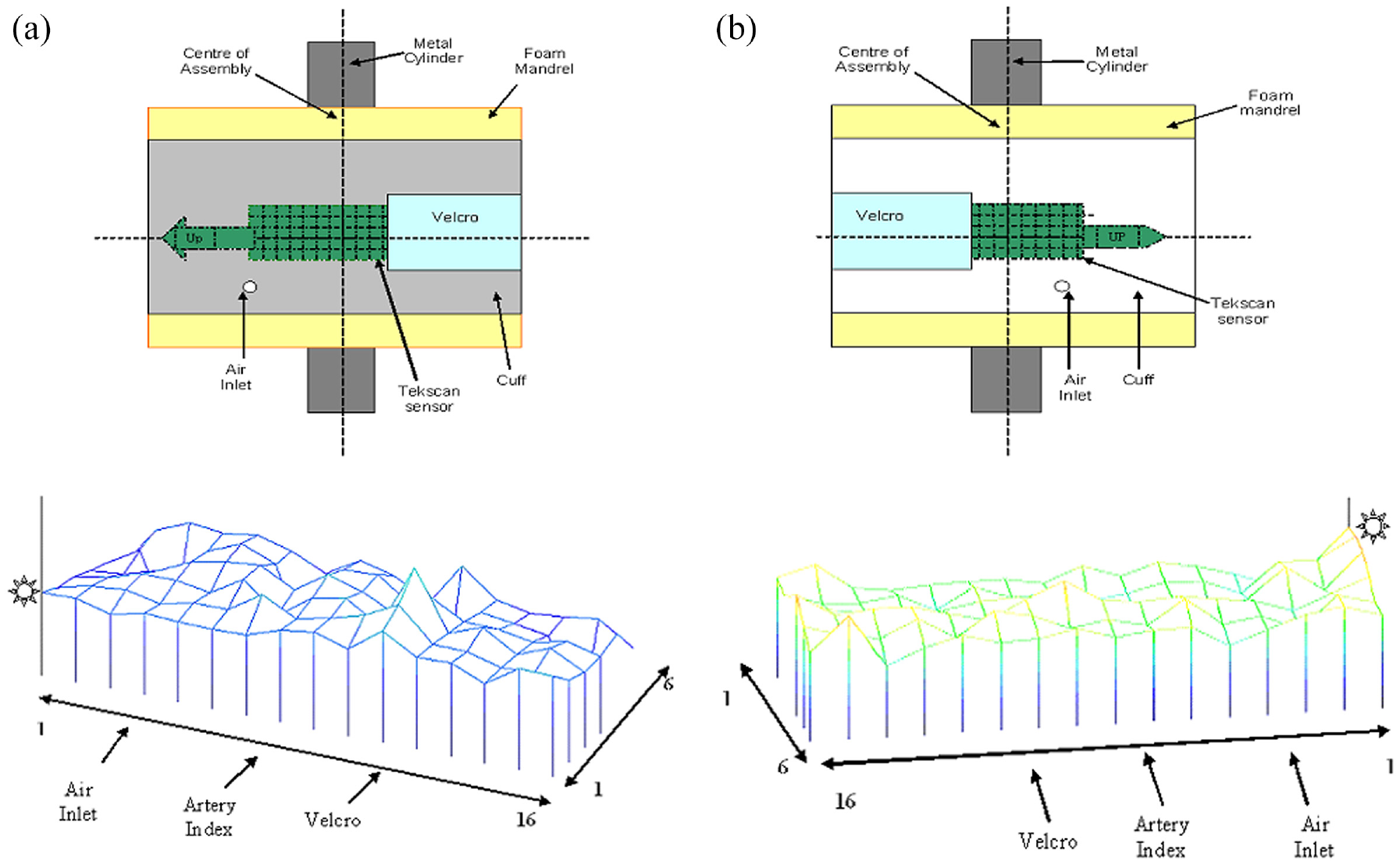
(a) I-scan sensor arrangement for measurement of the pressure at the interface of arm simulator and Cuff A-4 and Cuff D-2. (b) sensor arrangement for measurement of the pressure at the interface of the arm simulator and Cuff BI-scan-2 & Cuff C-2.
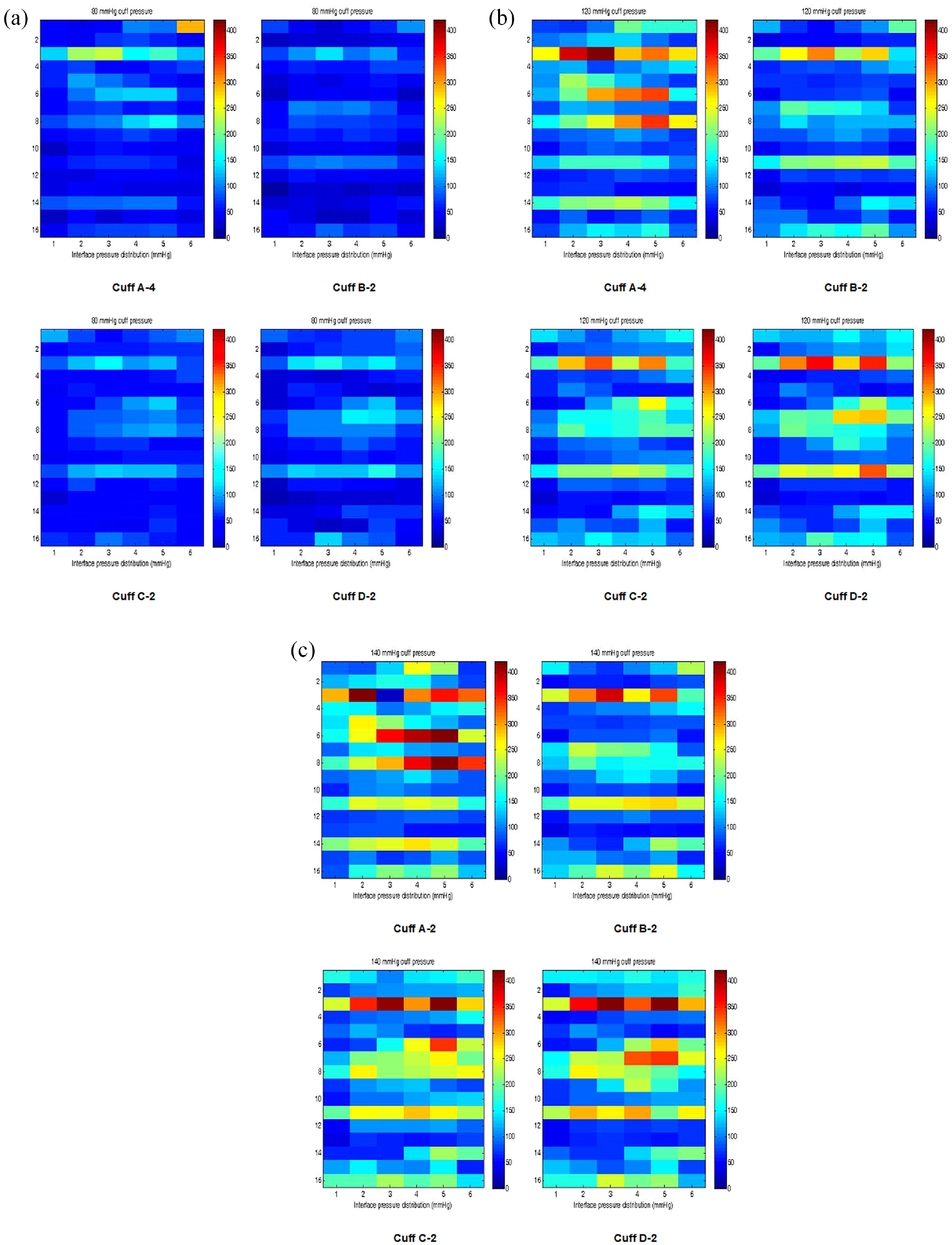
(a) Pressure distribution at the interface of cuffs and arm simulator at 80 mmHg manometric pressure (programmed in MATLAB). (b) Pressure distribution at the interface of cuffs and arm simulator at 120 mmHg manometric pressure (programmed in MATLAB). (c) Pressure distribution at the interface of cuffs and arm simulator at 140 mmHg manometric pressure (programmed in MATLAB).
Results
Figure 2(a) and (b) shows the placement of the pressure sensors under the cuffs to study the effect of design in detail. The effect of the cuffs design on the pressure distribution can easily be examined through this experimental investigation. The results presented below are of the pressure distribution at the interface against 80, 120 and 140 mmHg manometric pressures. These pressures were selected because 80 and 120 mmHg are in the range of normal diastolic and systolic BP values, respectively, while 140 mmHg is in the range of mild hypertension (grade 1) according to the British Hypertension Society guidelines. Pressure distribution under the cuffs is well illustrated by transforming ASCII data into graphical representation, see Figure 3(a)–(c).
The results provide important information about the effect of cuff design on pressure distribution and transmission during BP measurement. Alteration in design leads to varying pressure distribution among the cuffs which may result in different pressure transmission to the arm under each type. It may lead to variable BP values of human subjects if measured using these commercially available cuffs.
Average IP was calculated moreover by the values of average force acting over the arm and an active sensing area, displayed by the I-Scan sensing system during measurement. Average IP was plotted against manometric pressure, see Figure 4. The dotted line represents manometric pressure (pressure inside the cuff). The purpose of this line is to show the deviation of the average IP from the manometric pressure because it is assumed that during BPM the inside-cuff pressures registered by the manometer are the low (diastolic) and high (systolic) BP values.
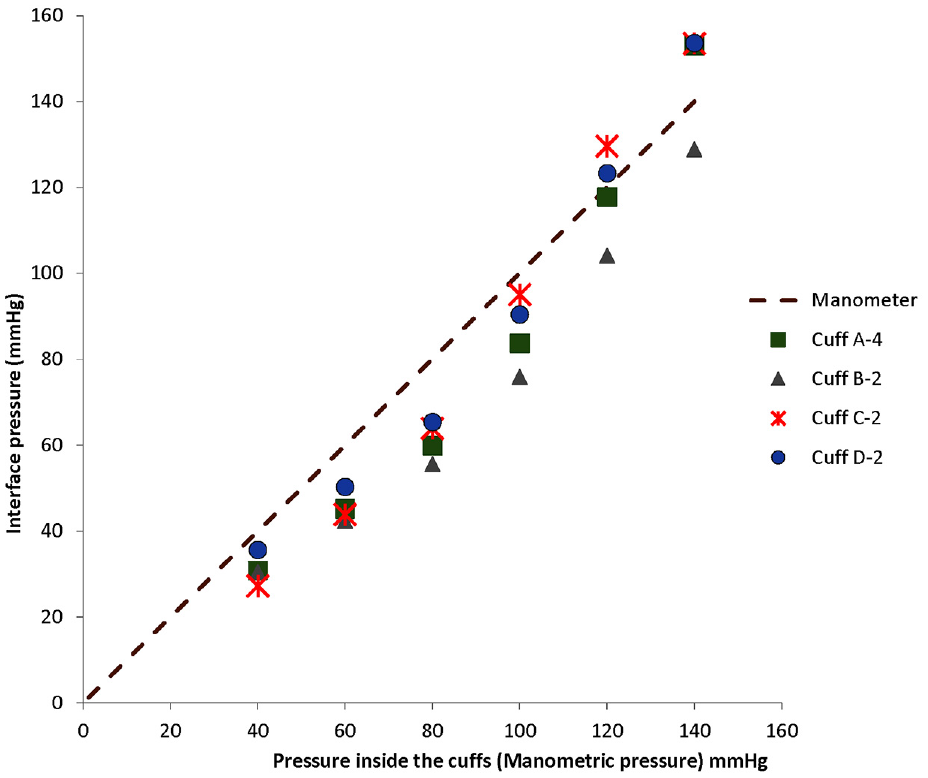
Pressure variation at the interface of cuff and arm simulator.
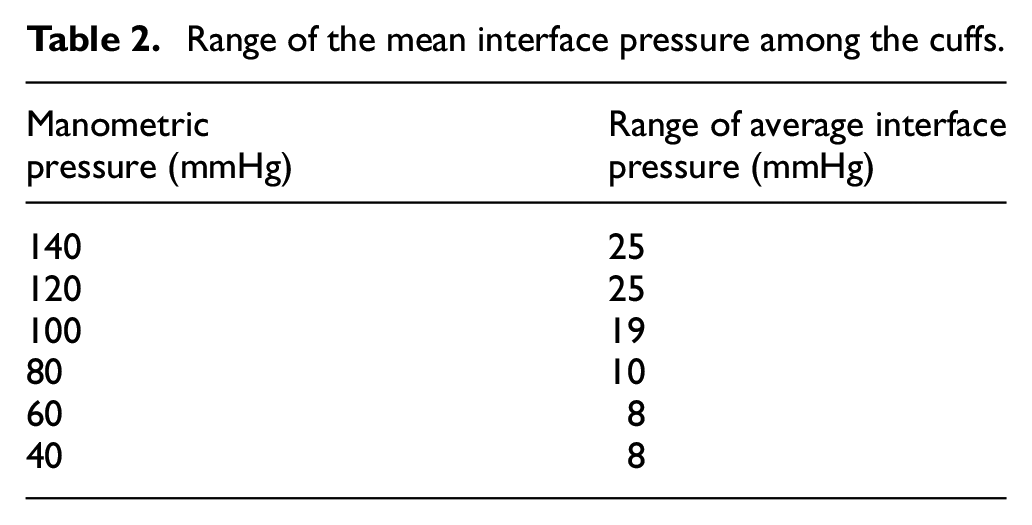
To study the variations among the values of the average IP registered by the cuffs, range is calculated against the corresponding manometric pressure and listed in Table 2. The range varies from 8 to 25 mmHg.
Range of the mean interface pressure among the cuffs.
Discussion
Design of the cuffs includes constructing fabrics and different components to enable BPM. The deformation/wrinkling of the BP cuff during inflation and deflation manoeuvres depends on the constructing fabrics. From the results presented in Figure 3, it can be observed that cuffs are not entirely in contact with the arm simulator. As a result, 100% pressure from the cuff inner wall can’t be transmitted to the arm. For pressure transfer, the cuff inner wall must be in complete contact with the arm. BP cuff redesign can be carried out simply by appropriate selection of constructing fabrics and other components in a way that fabrics don’t wrinkle upon inflation and components don’t hinder fabric movement during BPM. It will aid in maximizing pressure transfer to the arm especially under the centre of the cuffs and other components attached to the constructing fabrics.
Considering design variation in reference to the constructing fabrics, it can be perceived that the performance of the cuffs not only varied between cuff made of woven and non-woven fabrics but also among the cuffs constructed of the same fabric type. Cuffs made of woven fabrics were not showing identical pressure distribution either because of the variances in their mechanical properties. The non-uniform and non-identical pressure distribution under the cuff could lead to an incomplete pressure transmittance from the cuff to the arm surface and varied pressure transfer from one cuff to another.
Cuff constructed of fabric having the highest value of the elastic modulus apply higher pressure at the interface than those cuffs whose constructing fabric has a lower value of the elastic modulus. Constructing fabric of Cuff A-4 has the highest value of elastic modulus (E = 430 MPa) applied the highest pressure while of Cuff B-2 has the lowest value of elastic modulus, applied the lowest pressure at the interface at most of the points underneath it. The other two cuffs are also complying with the same finding; see Figure 3(b) and (c). There is a direct relationship between the elasticity of the cuff fabrics and the pressure transmission to the arm. According to this finding, cuffs constructed of fabrics having higher values of elastic modulus might require lower amount of inside-cuff (manometric) pressure than those cuffs made of fabrics having lower values of elastic modulus in order to occlude artery underneath it at the desired pressure (inside-cuff pressure) to avoid overestimation or underestimation of BP values.
Most of the areas under the cuffs register lower values of the IP against the corresponding manometric (inside-cuff) pressure. The lowest IP value was registered by Cuff B-2 against all values of manometric pressure; however, the IP distribution is uniform against 80 mmHg manometric pressure to some extent if compared with the rest of the cuffs. The fabric of Cuff B-2 has the lowest value of the modulus of elasticity. Cuff A-4, Cuff C-2 and Cuff D-2 were constructed from woven fabric while Cuff B-2 was of non-woven fabric. The difference in their construction method incurred such a contrast despite all of the cuffs being the same size. Cuffs are mainly constructed either from woven or non-woven fabrics. Woven fabrics are constructed by the interlacement of the two sets of yarn and in most of the fabrics, design repeats along the length and across the width. However, non-woven fabrics are directly made from fibres after forming continuous webs and there is no specific design of the fabric. Hence, the transformations of the yarns into fabric or fibres into the fabrics vary their inherent characteristics which result in the differences in their behaviour upon application and removal of the force/pressure. Constructing fabrics of different types and properties distort in an irregular fashion (wrinkled around arm simulator) upon inflation and deflation during BPM. Cuffs deformation around arm simulator is also non-identical which is due to the variations in the constructing fabrics. During inflation and deflation manoeuvres, cuff walls stretched and relaxed, respectively, and wrinkles are formed in the inner cuff wall which doesn’t allow cuffs to remain entirely in contact with the objects underneath.
Thickness is one of the basic properties of fabric. The FAST-1 compression metre provides a direct measure of fabric thickness. The result shows that the thicknesses of the cuff fabrics are not identical either and varied from 0.221 mm to 0.44 mm. The range of thickness is found to be 0.219 mm. Geometrically, the only difference among the selected cuffs was of their thickness otherwise the sizes were identical.
Stiffness of the fabric also depends on the thickness. Fabric having higher value of stiffness is less compliant and as a result constructing fabrics of variable thicknesses wrinkle cuffs in irregular fashions. It might not allow cuffs to encompass arm completely and lead to variable and non-uniform pressure distribution during BP measurement. See Figure 3 which clearly shows cuffs contact with the arm simulator. Cuff A-4, C-2 and D-2 have lower values of thicknesses among; provided non-uniform pressure distribution at the interface which is an indication of more wrinkles in these cuffs while Cuff B-2 which has the highest thickness, offered uniform pressure distribution, in comparison, around the same arm simulator.
Cuff B-2 and Cuff D-2 have the highest and the lowest thicknesses, respectively, and Figure 4 indicates that Cuff B-2 has the lowest values of average IPs while Cuff D-2 has the highest values of the average IP measured against all inside-cuff pressures. Results specify that fabric having higher values of thickness may require more pressure inside the cuff for accurate estimation of BP using indirect methods. It indicates that the thickness of the cuff fabric also affects pressure transfer underneath it.
Every cuff is marked with an artery index at the centre of its inflatable part. The area of the cuff under an artery index is supposed to apply the maximum pressure over the arm (compared to the rest of the cuff during BPM) so that the blood flow in an artery underneath can be ceased completely. Considering pressure under artery index, in most of the cuffs, IP value was lower than the manometric pressure. Cuffs were unable to transmit 100% pressure through artery index over the arm simulator and pressure distribution was non-uniform either. In order to occlude the artery completely under these cuffs, higher manometric pressure would require during BPM otherwise it may lead to the overestimation of the BP values.
Instead of artery index, the part which applied maximum pressure was around an air inlet in all the cuffs except Cuff A-4, which exerted maximum pressure under its centre as well. The lowest pressure value was registered by the cuff under its Velcro tape. It was because of the restricted stretching of the constructing fabric which was attached to the stiffed Velcro tape. It means along with the fabric selection, position of the cuffs components also needs to inspect in details. As discussed that the pressure distribution was non-uniform and non-identical consequently position and properties of the other components used in cuffs construction play their role. Pressure transmission to the arm should neither be augmented nor lessened than required, during BPM. The results of the highly non-uniform pressure around the arm may lead to incomplete obstruction of blood flow due to wrong selection of the cuff constructing fabrics and other components and then their placement; which may give rise to inaccurate BP values.
Investigation depicts that cuffs examined do not fulfil the requirement of applying the highest pressure over the artery only. It has been found by the previous studies that the pressure at the cuff edges was not same as that in its centre1,13 and the pressure variations across the width of the cuff affected BPM. 14 The results of the proposed investigation also showed that the pressure distribution was non-uniform under cuff. This is due to the undesirable distortion of the cuff walls due to inappropriate design.
Along with the numerical data at individual sensing points, average IPs was also analysed in this study. These results show that the average IP also varied under different cuff types. Cuff A-4, Cuff C-2 and Cuff D-2 transmitted lower pressure to the surface of the arm than the corresponding pressure inside it till 100 mmHg Manometric pressure. Against 120 mmHg and 140 mmHg inside cuff pressures, same cuffs were able to transmit either the same or higher pressure over the surface of the arm simulator while Cuff B-2 has the lowest values of average IP throughout the measurements. All cuffs showing different behaviour against same manometric pressure range via individual sensing points, except Cuff B-2. Pressure over the surface of the arm might attenuate while it reaches to the artery underneath the cuff because it is reported by previous study related to the pressure distribution underneath the tourniquet that the pressure inside the tissue was less than the pressure inside the tourniquet. 15 This study also found that the highly uniform pressure by the cuffs would allow it to transmit same average pressure either and cuffs behaviour can be compared in both aspects, that is, individual sensing point values and average value. Due to the highly non-uniformity in pressure transmission average pressure transmitted varied among the cuffs examined. It can be seen in results that Cuff B-2 has the highly uniform pressure distribution but the lowest IP values at individual sensing points and the average IP of the same cuff is the lowest as well.
The lowest deviation of the IP from manometric pressure was found in Cuff D-2 and this cuff has two layers of woven fabric (E = 290 MPa and t = 0.221 mm) and the highest deviation was found in Cuff B-2 (non-woven) having the lowest value of elasticity (E = 100 MPa and t = 0.440 mm). Constructing fabric having the lower value of the elastic modulus has more difference between their IP and inside-cuff pressure. In actual indirect BPM, manometric pressure is considered as BP so the deviation of inside-cuff pressure value and the pressure transmitted (IP) may cause errors in estimation of actual BP measurement.
The range listed in Table 2 shows wide variation from 8 mmHg to 25 mmHg of pressure at the interface of the cuffs and arm simulator. In this case, the amount of pressure transferred to the tissues and subsequently to the artery might vary greatly if measured using the selected cuffs because it would depend on the amount of the pressure each cuff exerts over the arm. The cuffs that transferring higher IP may underestimate the actual value of BP similarly the cuffs that registered lower IP may overestimate the actual value of BP for the same subjects. It may misclassify BP level of human subjects.
Although BP was not measured during the IP measurement in this in-vitro study; however, it was able to indicate the pressure transmission under cuffs studied. For the same patient, values of BP measured under different types of cuff might not be repeatable; could be over or under estimated from actual BP. It would depend on the design of the cuff being used for the assessment. The pressure is transmitted to an artery inside tissues, which might further vary depending on the type of human tissues. The results of the current study indicate that manometric pressure (pressure inside the cuff) may not be a true representation of arterial pressure.
Conclusion
This study shows the importance of the BP cuff design for accurate measurement by analysing the pressure distribution under different parts of the cuffs, mostly constructed of woven and non-woven fabrics. It has been found experimentally that due to varying cuff designs, pressure transmission under the cuffs is not identical. This indicates one of the errors associated with the indirect method of BPM. It is difficult to identify which cuff is able to estimate BP values accurately as the value of the pressure varies under the cuffs which might attenuate or augment further while acting upon the artery.
IP measurement is an uncomplicated procedure to remove design faults of the BP cuffs and would aid in verifying the design for the required pressure transmission to the artery even during different stages of cuff manufacturing and in selection of the constructing fabric.
Since fabric is the main constructing material and this study found a relation between fabric properties and pressure transmission, it is now possible to either select or construct fabrics of specific mechanical properties for accurate estimation of BP values. Selection and placement of the other cuff components should not deform/wrinkle fabric during BP measurement. BP cuffs must be designed in such a way that uniform pressure can be applied on the arm and for that further study on the selection of the constructing fabrics and other components is crucial, to block and resume blood flow at the actual BP value.
Footnotes
Acknowledgements
The authors would like to acknowledge the funding provided by the NED University of Engineering & Technology, Karachi, Pakistan, through the Higher Education Commission of Pakistan, to carry out this study at the School of Materials, The University of Manchester, UK.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The authors received financial support from NED University of Engineering & Technology, Karachi, Pakistan, through the Higher Education Commission of Pakistan.
