Abstract
Borderline personality disorder (BPD) and posttraumatic stress disorder (PTSD) share etiological factors, are highly comorbid, and involve disruptions in social cognition. However, little is known about how the co-occurrence of BPD and PTSD shapes social cognitive functioning and associated neurobiological mechanisms. Given uncertainties on the state of the literature in this area of study, we conducted a scoping review of the neurobiology of social cognition across five domains: emotion processing, theory of mind, empathy, social perception, and attributional style/bias. Searches using controlled vocabulary and synonymous keywords for “social cognition,” “borderline personality disorder,” and “posttraumatic stress disorder” yielded 108 studies, with only four directly examining comorbid presentations. Across domains, in individuals with both BPD and PTSD, fMRI findings implicated limbic hyperreactivity (eg, amygdala, insula) and altered engagement of medial prefrontal, lateral prefrontal, posterior temporal, and temporoparietal regions supporting social perception and theory of mind. Patterns diverged across disorders such that individuals with BPD showed medial prefrontal hypoactivation during theory of mind, whereas individuals with PTSD generally showed prefrontal hyperactivation to threat-relevant cues. Ultimately, given the limited evidence in comorbid samples, existing research remains insufficient to delineate which neural and behavioral abnormalities are common across disorders versus uniquely associated with one condition. We identify key methodological and conceptual gaps to outline future directions for research on the neurobiology of social cognition in BPD, PTSD, and their comorbidity.
Keywords
Social cognition is broadly defined as the mental processes underlying social behavior, including understanding and interpreting others’ emotions, intentions, and actions.1,2 Social cognition is foundational for enabling individuals to navigate social environments, communicate effectively, build relationships, and form social groups.3,4 Psychiatric conditions are often associated with disruptions to social cognition, impacting how people receive, assess, and react to their social surroundings.5–8
Two psychiatric conditions, in which exposure to trauma plays a critical role in their etiology, are marked by impairments in social cognition: borderline personality disorder (BPD) and posttraumatic stress disorder (PTSD).9–11 BPD is a personality disorder characterized by instability in emotions and relationships, impulsivity, dissociation, and self-harming behaviors. 12 PTSD is a trauma-related disorder characterized by symptoms such as re-experiencing of the traumatic event, avoidance of trauma-related cues, negative alterations in mood and cognitions, and trauma-related hyperarousal. Both disorders cause a significant burden on the individual, notably in social areas of functioning such as diminished social support and interpersonal strain.13–16
Though BPD and PTSD are often studied separately, these diagnoses frequently co-occur. For example, in U.S. adults diagnosed with either BPD or PTSD, 25-30% of adults are also diagnosed with the other disorder.17,18 The high comorbidity between BPD and PTSD likely reflects shared etiological underpinnings, such as exposure to trauma. 19 Accordingly, the central role of trauma in the development of both disorders has been widely emphasized. 20 Early trauma, particularly when it occurs in caregiving or attachment relationships, disrupts the capacity to understand mental states of self and others, deficits that are characteristic of both BPD and PTSD. 21
Early relational experiences play a critical role in shaping social-cognitive development by providing repeated opportunities to learn how to interpret others’ intentions, regulate emotional responses, and form stable expectations regarding interpersonal safety and trust. 22 When these experiences are characterized by chronic trauma, threat, or emotional invalidation, individuals may develop maladaptive social-cognitive schemas, including difficulties in emotion recognition and regulation, biased attributions regarding others’ intentions, and expectations of future relationships marked by rejection or abuse.23–25 Thus, trauma exposure in both disorders may contribute to shared, transdiagnostic dysfunction, particularly within the domain of social cognition.26,27
At the neurobiological level, both disorders exhibit alterations in overlapping neural systems implicated in social cognition, including the amygdala, prefrontal cortex, and anterior cingulate cortex.28,29 Altered functioning within limbic regions, coupled with dysregulation in prefrontal control systems, may reflect shared disruptions in emotion processing and regulation that contribute to interpersonal difficulties across both disorders. 28 However, despite engagement of overlapping neural systems, these regions may be recruited in disorder-specific ways, giving rise to distinct patterns of social-cognitive dysfunction in PTSD versus BPD.30,31
Studies also reveal clear differences between individuals with BPD and PTSD in social cognitive functioning. For example, following social rejection, individuals with BPD experience exaggerated emotional distress and retaliatory behaviors, 32 whereas individuals with PTSD experience heightened vigilance and withdrawal. 33 Further, compared to healthy controls, individuals with BPD tend to interpret ambiguous social cues more negatively and are more likely to attribute malevolent intent to the actions of others.34–36 On the other hand, individuals with PTSD may be more susceptible to perceiving ambiguous social stimuli, such as neutral faces, as hostile or threatening.37,38 In the domain of emotion processing, individuals with BPD show a generalized disruption to social stimuli, whereas individuals with PTSD demonstrate difficulties primarily with fear-evoking stimuli.34,39 Taken together, these results suggest some congruent and some differential responding across domains of social cognition for individuals with BPD and PTSD.
Examination of neurobiological correlates of social cognition reveals further similarities and differences across these disorders. In terms of similarities, individuals with both disorders show hyperactivity in the temporo-parietal circuits when interpreting social cues, such as the intentions of others and facial emotion processing.40–44 This hyperactivity may reflect compensatory recruitment, inefficient processing, or heightened sensitivity to social information45,46 Further, increased amygdala activity coupled with decreased activation in frontal control circuits appears to be a hallmark feature of both disorders43,47–50 However, distinct patterns of activation also emerge across disorders. For example, individuals with BPD show heightened amygdala activity and decreased activation in frontal control circuits across negative emotional stimuli, 43 whereas individuals with PTSD show this pattern primarily when presented with threat-related stimuli. 51 These results parallel other findings that, while individuals with both disorders display increased activation in limbic regions when processing facial expressions, individuals with BPD show a negative attentional and/or memory bias towards ambiguous stimuli 30 whereas individuals with PTSD show attentional and memory bias to stimuli perceived as fearful. 31 Thus, while BPD and PTSD may have overlapping neural impairments, they may diverge in the specific contexts in which these impairments present.
It largely remains unclear how the comorbidity of BPD and PTSD may influence impairments in social cognition, as most of the extant literature has examined BPD and PTSD separately. In studies that do measure BPD and PTSD in the same sample, the effect on social cognition may not be specifically examined in the comorbid group (eg,52,53), or the researchers may not have examined the corresponding neurobiological deficits. For example, Preißler and colleagues 54 found that individuals with comorbid BPD and PTSD showed deficits in empathy on an ecologically valid task (Movie for the Assessment of Social Cognition (MASC)) 55 as compared to both healthy controls and individuals with BPD only. However, they did not examine the corresponding associated neurobiological features. Though these studies provide some insights, much remains unknown regarding the intersection of BPD, PTSD, social cognition, and its neurobiology.
More broadly, there is a gap in our understanding of the neurobiology of social cognition for individuals with comorbid BPD and PTSD. The extent to which the neurobiological underpinnings of social cognition in comorbid BPD and PTSD have been studied remains unclear, perhaps in part because examining neurobiology and shared transdiagnostic features of disorders are relatively newer areas of research. Second, social cognition is a heterogeneous umbrella construct, and it is unclear how social cognition has been operationalized in the study of BPD, PTSD, and their intersection. Refining the specificity in definitions of social cognition may enhance clarity in harmonizing findings. Ultimately, given the commonalities and differences in social cognitive dysfunction across BPD and PTSD, it is important to understand what features of this dysfunction are truly shared across both disorders and what features may be primarily attributed to one disorder. Mapping the current state of the literature may guide future research into disentangling these questions.
Thus, we conducted a scoping review to explore the state of the literature as it relates to the neurobiology of social cognition in BPD, PTSD, and their comorbidity. A scoping review methodology was chosen to identify knowledge gaps within the field and define key concepts. We utilized knowledge gleaned from this method to understand and suggest future directions for researchers interested in BPD, PTSD, and social cognition.
Method
Protocol and Registration
This scoping review was conducted according to the Joanna Briggs Institute 56 and reported following PRISMA Extension for Scoping Reviews. 57 The protocol was publicly preregistered on Open Science Framework (https://osf.io/abv2j) before the review process.
Inclusion Criteria
Studies were included if they met the following inclusion criteria: 1) documented the influence of BPD and/or PTSD on at least one quantitative measure of social cognition; 2) utilized fMRI methodology; 3) conducted an experiment using adult human subjects; and 3) was peer-reviewed.
Studies were excluded if they involved animal models, children (ie, participants under age 18), or participants with traumatic brain injury/head injury. Studies were also excluded if they utilized qualitative methodologies or did not have a publicly available full text. See Supplemental Material 1, Table S1 for details on inclusion and exclusion criteria.
Search Methods
A medical librarian (MCF) used the Yale MeSH Analyzer 58 to identify relevant keywords and MeSH terms from known articles. Searches were iteratively refined across databases (See Supplemental Material 1, Tables S2, S3a-3e). To maximize sensitivity, the formal search used controlled vocabulary terms and synonymous keywords to capture the concepts of “social cognition”, “borderline personality disorder”, and “posttraumatic stress disorder”. No date or language limits were imposed on the search. The search strategy was peer reviewed by a second librarian, not otherwise associated with the project, using the PRESS standard. 59
On January 16, 2024, and December 19, 2024, the librarian (MCF) performed a comprehensive search of the following databases: Ovid MEDLINE ALL, APA PsycInfo (Ovid), Embase (Ovid), Web of Science Core Collection (Clarivate), and Cumulative Index to Nursing and Allied Health Literature (EBSCOhost). All search strategies are included in the Supplementary Tables 3a-3e. Per JBI protocol, we also checked for additional relevant cited and citing articles using the included studies. Two updated literature searches were conducted on February 2, 2025, and again on December 8, 2025, using the same search strategy and databases to identify any relevant articles published after the last search conducted on December 19, 2024.
Search results were pooled in EndNote 21, 60 de-duplicated using the Reference Deduplicator tool, 61 and uploaded to Covidence 62 for screening. Four screeners (KS, SE, EB, TD) independently reviewed titles, abstracts, and full texts, resolving conflicts through consensus. Articles that were not in English were translated into English using DeepL.
Social Cognition Search Terms
We defined five domains of social cognition constructs to analyze across BPD and PTSD: emotion processing, social perception, theory of mind, empathy, and attributional style/bias (see Supplementary Table S2 and 3a-3e. for databases and search terms). The five domains were derived through a qualitative synthesis of social-cognitive constructs examined in prior systematic reviews of BPD and PTSD.2,9,10,25,63 Domain definitions and operationalization were guided by social-cognitive frameworks proposed by Plana et al. 5 and Janssen et al. 64
Facial Emotion Processing
Emotion processing refers to interpreting or recognizing others’ emotions.65,66 The search terms used to capture this domain included “face* or facial,” “emotion* or anger or happy or fear* or angry or neutral or surprise* or disgust*.”
Social Perception
Social perception refers to the ability to notice, interpret, and respond to social interaction cues, specifically the behaviors and intentions conveyed by others. 1 In our review, we included the Cyberball task and similar tasks only when they were used to assess attention to or processing of others behavior, rather than emotional reactions to exclusion. We did not classify affective, motivational, or regulatory responses to social situations as social perception because these measures reflect emotional experience rather than social cognitive processing. The search terms used to capture this domain in our search included “perception”, “recognition,” or “discrimination.”
Theory of Mind
Theory of mind refers to the ability to mentally represent the thoughts and mental states of others (ie, mentalization. 67 The theory of mind tasks included identifying or inferring mental states or beliefs of another person. 64 The search terms used to capture this domain in our search included “theory of mind, mentaliz* or mentalis*.”
Empathy
Empathy is the ability to both understand another's perspective and feelings as well as feel the emotions of another.68,69 While empathy is a similar construct to theory of mind, empathy refers more specifically to understanding and feeling the emotional states of another person. The search terms used to capture this domain in our search included “attunement or empath*.”
Attributional Style/Bias
Attributional style/bias refers to how people interpret or explain others’ intentions and/or behaviors. 64 For example, holding a hostile attribution bias and attributing malevolent intentions to others. 70 That is, this domain refers to how people explain others’ intentions or the causes of behavior, generally requiring them to infer motives or causes that are not directly observable utilizing higher-order interpretive processes. The search terms used to capture this domain in our search included “attribution* style or bias or intention* and intention* bias.”
Results
Study Characteristics
The final search retrieved a total of 10,524 references. Of these, 5041 were duplicates, 5483 were screened, and 4411 were excluded based on pre-defined criteria. A further 964 were excluded upon full-text review (See Figure 1 for PRISMA flow diagram). In total, 108 studies satisfied the inclusion criteria. Table 1 includes characteristics of the reviewed articles, including publication year, patient population, domain of social cognition, country of origin, study design, comparison groups, and brain regions. Primary results from the scoping review, including authors, publication year, comparison groups, diagnostic methods, operationalization, and main findings, are charted in Supplemental Material 2, Table S4.
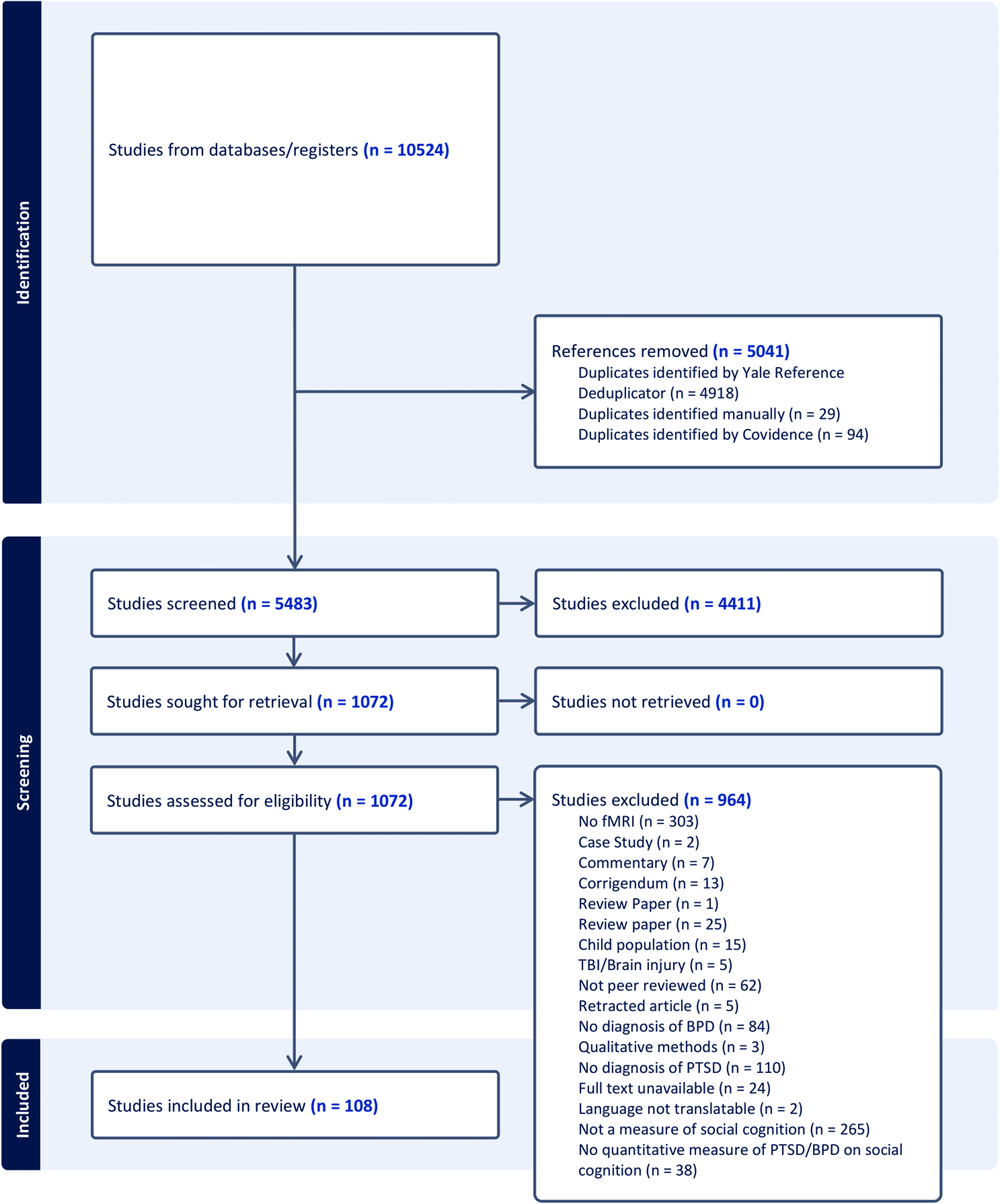
PRISMA flow diagram of study selection process.
Study Characteristics of Articles Included (N = 108).

91 studies (84%) examined one domain of social cognition, and 17 studies (16%) examined more than one domain of social cognition.
HC = Healthy Control; Clinical = comparison group is another clinical population (eg, major depressive disorder); Pre-post = within-subjects’ longitudinal design; TE = trauma-exposed; NC = No Control.
Sample Characteristics
Sample sizes across the included studies ranged from 7 71 to 235 participants, 72 with a mean sample size of 51.97 participants. The 108 included studies reported on a total number of 4975 participants. See Table 2 for a summary of included studies by diagnostic focus, total sample size, mean and range of participants per study, and sample sex composition.
Sample Characteristics of Studies by Diagnostic Focus, Sample Size, and Sex Composition.

Note. Percentages refer to the proportion of studies within each diagnostic group.
One study (ie, 73 ) did not specify sample sex information and is not include in the gender percentage calculation.
Descriptive Findings
Facial Emotion Processing
Seven studies found that individuals with BPD and individuals with PTSD displayed increased amygdala activity during emotional face processing paradigms (all comparison groups are listed in Supplemental material 2, Table S4).74–80 In BPD, this activity was predominantly observed in the left amygdala across neutral, fearful and happy facial expressions,77,80 whereas findings for PTSD showed increased activation in both the left and right amygdala for neutral, fearful and happy faces.76,81 However, five studies reported no significant differences in amygdala or insula activation between BPD or PTSD and controls during facial emotion processing tasks.42,76,79,82,83
Across studies using facial emotion processing tasks, individuals with PTSD, BPD, or their comorbidity showed altered activation patterns relative to healthy controls. Several studies reported increased activation in frontal regions41,74,84 and temporal cortices41,42 when participants completed tasks such as masked-faces paradigms, face-matching tasks, or emotion-discrimination tasks. Other studies reported decreases in prefrontal activity during emotional face processing, but the specific pattern depended on the task demands. For example, vmPFC activity decreased when participants viewed fearful faces that were later forgotten in a memory task 31 and when they processed neutral versus emotional scenes. 85 dlPFC activity also decreased when participants were required to shift attention away from emotional facial expressions, whereas dlPFC activity increased when participants were instructed to regulate their response to emotional faces using cognitive appraisal. 86
Across several studies, individuals with PTSD showed heightened subcortical and insular responses to emotional faces compared to trauma-exposed controls. Three studies reported increased thalamic activity to fearful faces in PTSD relative to trauma-exposed controls,95,104 with one study additionally showing increased thalamic activation post-treatment compared to pre-treatment. 72 PTSD participants also consistently exhibited increased insula activity during fearful face processing.80,91,95,105,106 Elevated insula activation was further observed when viewing angry and fearful faces 91 and angry versus happy faces, 80 again relative to trauma-exposed controls. Importantly, greater insula reactivity predicted symptom reduction following treatment,105,106 suggesting a potential role for insula responsivity in therapeutic change.
Regarding happy facial expressions, both disorders exhibited heightened amygdala responses compared to healthy controls,74,93 while oxytocin administration in PTSD patients increased left anterior insula activation to happy faces. 109 Pre-treatment amygdala activity to happy faces was identified as a predictor of post-treatment symptom reduction in PTSD patients. 82 Patients with PTSD also demonstrated decreased ventral striatum and amygdala activity to happy facial expressions compared to trauma-exposed controls. 110
Social Perception
Individuals with BPD showed heightened sensitivity to social evaluation relative to healthy controls. They exhibited greater rejection distress during the Cyberball task 111 and altered mPFC activity during social exclusion. 112
Compared to healthy controls, individuals with BPD also showed increased activation in the dorsal ACC (dACC), dorsomedial PFC (dmPFC), and precuneus in response to minimal rejection cues. 32 In addition, participants with BPD showed heightened amygdala responses to both unpleasant and pleasant images and to social feedback, again relative to healthy controls.113,114
Individuals with PTSD, compared to healthy controls, showed increased connectivity between the locus coeruleus and limbic, frontal, and subcortical regions during direct eye-gaze processing. 115 They also exhibited increased activation in the right inferior and superior frontal gyri, right TPJ, superior and left temporal gyrus, right angular gyrus and several subcortical regions in response to direct gaze cues.39,116
Theory of Mind
Across studies, both BPD and PTSD demonstrated alterations in theory of mind (ToM) processing, but the underlying neural patterns and task-related behavioral outcomes differed across disorders. Compared to healthy controls, participants with BPD showed reduced accuracy on the MASC, with the largest deficits observed among those with higher levels of childhood maltreatment. 117 In contrast, participants with BPD showed no group differences compared to healthy controls on ToM measures, such as the Reading the Mind in the Eyes Test (RMET), 117 or on theory-of-mind cartoons and RMET accuracy. 118 fMRI studies using the ToM Cartoons task 118 and a Visual Puns and Jokes mentalizing task 119 found that BPD participants displayed increased activation in frontoparietal regions and reduced ACC–TPJ and ACC–superior temporal gyrus connectivity, as well as reduced limbic–prefrontal connectivity relative to healthy controls. 117
PTSD participants performed similarly to trauma-exposed controls on the Social Inference task 73 and showed comparable accuracy to trauma-exposed controls on the Social Working Memory task except under high-load conditions, where PTSD participants showed reduced accuracy.97,98 In the Social Judgment task, participants with PTSD showed increased medial frontal and posterior cingulate activation from pre- to post-therapy. 120 Using a clip-viewing task requiring interpretation of menacing versus prosocial interactions, PTSD participants showed heightened activation in dmPFC, dlPFC, ACC, insula, and hippocampus compared to healthy controls. 85
Empathy
Individuals with BPD exhibited increased amygdala activation in response to others’ distress. 53 In a longitudinal study using the Interpersonal Reactivity Index (IRI), individuals with BPD showed increased baseline connectivity between the right DCG and other brain regions and decreased baseline connectivity between bilateral ACG and other regions relative to healthy controls but demonstrated equivalent IRI empathic concern scores from baseline to post-treatment. 121 Another study using an empathy questionnaire showed that in BPD, greater activation in the medial frontal gyrus, dACC, rTPJ, STG, and precuneus was associated with higher empathy ratings when participants were making trait judgments about others. 122
On the IRI, PTSD participants scored higher on the Personal Distress subscale but did not differ from healthy controls in total empathy scores. 116 In studies using the Multifaceted Empathy Test (MET), PTSD participants demonstrated greater medial and left IFG activation during cognitive empathy and greater left pallidum, anterior insula, and IFG activation during implicit empathy compared to trauma-exposed controls but showed reduced behavioral accuracy on both implicit and explicit emotional empathy tasks. 123 A second MET study found that PTSD participants relied more on amygdala modulation during explicit emotional empathy and showed greater balanced connectivity across PFC and insula during empathy processing compared to healthy controls, while maintaining equivalent cognitive empathy performance. 124
Attributional Style/Bias
Individuals with BPD demonstrated increased activation in the mPFC, TPJ, precuneus, and occipital regions during self–other evaluation compared to HC, 52 heightened left amygdala activation and more negative post-scan attributions to neutral faces relative to HC, 76 and increased fusiform, thalamic, putamen, and anterior medial PFC activation during emotional face processing compared to both HC and participants with complex PTSD. 43 Participants with BPD also showed stronger amygdala and somatosensory cortex responses than HC when approaching aversive facial expressions 44 and greater medial frontal, dACC, STG, and precuneus activation during attribution judgments relative to HC. 122 PTSD studies similarly reported elevated amygdala, hippocampal, and PFC activation and stronger attention bias to negative cues in PTSD patients compared to HC. 40
Discussion
This scoping review examined the neurobiology of social cognition in BPD, PTSD, and their comorbidity. We identified both similarities (eg, amygdala hyperactivation during emotion processing in BPD and PTSD compared to HC) and differences (eg., dmPFC hypoactivation in BPD vs hyperactivation in PTSD during theory of mind tasks) between disorders. Without concurrently measuring both disorders, disruptions in social cognition can be misattributed to one disorder. Most importantly, the presence of comorbid BPD and PTSD may result in a distinct social cognitive profile that cannot be adequately captured by studying each disorder in isolation. Below, we suggest directions for further research, which is necessary to understand the intersection of BPD, PTSD, social cognition, and neurobiology.
Comorbidity of BPD and PTSD
Results of the current scoping review revealed a relative dearth of literature examining comorbid BPD and PTSD. Of 108 included studies, only four (3.6%) investigated BPD-PTD comorbidity, despite high comorbidity rates between these disorders.17,18
Findings regarding emotion processing from the four studies suggest comorbidity effects may be region-specific: comorbid BPD-PTSD showed decreased frontal/occipital activation during fearful face processing compared to HC, 125 but no amygdala differences compared to individuals diagnosed with only BPD. 76 It may be that the mixed findings in frontal activation to fearful faces in PTSD82,96,99,104,126–128 are partially attributable to comorbid BPD that was not assessed. Further, another study demonstrated no significant effect of BPD-PTSD comorbidity on amygdala activation during emotional face viewing, as compared to BPD alone. 76 The differences in activation for individuals with comorbid BPD-PTSD may only emerge in certain brain regions (ie, frontal vs limbic). Finally, we note that, although one study examined BPD and PTSD in the same sample, their analytic plan precluded direct comparison of comorbid BPD-PTSD to BPD alone and/or PTSD alone. 43 Regardless, more work is needed to robustly elucidate social cognitive neural functioning in individuals with BPD and PTSD, as compared to individuals with just one disorder.
Taken together, BPD and PTSD comorbidity may be associated with higher symptom severity and poorer social cognitive functioning. However, more research is needed to understand whether BPD-PTSD comorbidity is qualitatively distinct in terms of behavioral and neurobiological profile from both healthy controls and individuals with BPD or PTSD alone.
Methodological Considerations
Researchers interested in the BPD-PTSD comorbidity may benefit from several methodological considerations when designing studies. Researchers should use gold-standard diagnostic measures (eg, SCID-V-PD; CAPS-5) whenever feasible. Although many researchers choose not to utilize these measures, utilizing gold standard measures for both disorders to increase diagnostic validity, and enables parsing of each disorder's contribution to social cognitive outcomes, and promotes harmonization of results across studies.129,130
Second, future researchers may benefit from methodological design and statistical analyses that allow for parsing of the specific contribution of each disorder to any disruptions seen in social cognition and associated neural features. This approach will further clarify the profile of social cognitive functioning in individuals with comorbid BPD and PTSD. This may require larger sample sizes, and we encourage researchers conducting large-scale collaborative data collection efforts to consider the inclusion of both BPD and PTSD measures in their batteries to promote increased capacity to differentiate outcomes by disorder.
Finally, we encourage researchers to utilize and/or design behavioral paradigms that are ecologically valid. Social cognition often involves complex processes, and we encourage researchers to investigate the impact of comorbid BPD and PTSD on social cognition using experimental paradigms that most closely mirror social situations that individuals may encounter in the real world. This is especially salient given that task-specific findings may only emerge during ecologically valid tasks. 54 Thus, researchers may consider utilizing newer assessment methods, such as video-based tasks, virtual reality paradigms, or interactive social scenarios, which may offer more ecologically valid insights into social cognitive processing.131,132
We recognize that it may not be feasible to assess both disorders and utilize complex tasks in all study designs. When assessing one disorder in the absence of the other, researchers may consider using diagnostic assessments and tasks that facilitate comparison across studies. Our review found that, while similar assessments (eg, CAPS-5, SCID-II)129,130 are used across studies, there are a variety of behavioral paradigms. Further, when similar paradigms are utilized across studies (eg, facial affect recognition, Cyberball task), methodological variations in assessment, task delivery, stimuli, and analytic approaches can make direct comparisons challenging. Thus, researchers building on prior work can consider utilizing standardized tasks and/or comparable stimuli across studies to facilitate harmonization with both prior and concurrent literature.
Domains of Social Cognition
Social cognition domains were operationalized inconsistently across studies, making cross-study comparison difficult. For example, across studies, many utilized different experimental paradigms and/or variations of the same task to measure the same theoretical construct. This inconsistency in operationalization makes it difficult to compare findings across studies and may contribute to conflicting results in the literature. Future research should work toward establishing standardized measures and clearer operational definitions for each social cognition domain to enhance the reliability and comparability of findings across studies.
Results from the present study also highlighted imbalances in the domains of social cognition that are assessed in the BPD and PTSD literatures. Emotion processing was the most studied domain (85 studies examined emotion processing out of 108 total studies), possibly due to well-established fMRI paradigms in this area (eg., emotional go-no-go task, face matching paradigm, masked facial affect task, approach avoidance task). The comparative scarcity of research on other domains limits our ability to determine how significantly and consistently social cognitive disruptions in BPD and PTSD vary across domains.
Our review found relatively few studies examining social perception, theory of mind, empathy, and attributional style/bias. Researchers may consider incorporating measures of additional domains of social cognition into their task batteries and aim to assess these domains more directly (eg, theory of mind inferences through watching movies, playing games that include trust, collaboration, and social intention attributions) to enhance the breadth and validity of measurement of social cognitive functioning. Additionally, future researchers could expand findings by developing suitable fMRI tasks that provide ecologically valid ways of assessing these social cognitive domains. For example, researchers could develop virtual reality paradigms that simulate real-world social interactions or task stimuli programs that dynamically output individual-specific stimuli during neuroimaging assessment. This would allow for enhanced assessment of empathy, mentalizing, and/or social perception difficulties in BPD and PTSD. A more comprehensive assessment approach might reveal more overlapping features or differences in other domains of social cognition than currently recognized.
Neural Activity and Behavioral Performance
Additionally, our results indicate that differences in social cognition for participants with BPD and PTSD, compared to healthy controls, may be most salient in neural activity. Neural differences often emerged in the absence of detectable behavioral performance differences. For example, individuals with BPD showed increased anterior PFC activity when avoiding happy faces and approaching angry faces despite equivalent accuracy and reaction times compared to healthy controls, 133 a pattern also observed in PTSD.110,134
The dissociation between neural and behavioral findings may reflect several non-mutually exclusive possibilities. First, neuroimaging may capture subtle processing differences that behavioral measures lack the sensitivity to detect. Second, behavioral differences may exist but be too fine-grained for typical task paradigms to measure (eg., response variability, confidence ratings, reaction time distributions). Third, many studies may be underpowered to detect small-to-moderate behavioral effects. Future research may benefit from: (1) comprehensive assessment batteries combining neural and behavioral measures, (2) behavioral tasks with greater sensitivity and ecological validity, and (3) larger sample sizes adequately powered to detect both neural and behavioral effects. Larger sample sizes would also enable comparison across three groups–comorbid BPD-PTSD, BPD-only, and PTSD-only– to refine our understanding of how these disorders disrupt social cognitive functioning.
Treatment Integration
Finally, our results suggest that indicators of social cognition may be important considerations in treatment-focused research. Individuals conducting treatment-focused research may benefit from the inclusion of measures of social cognition to track putative treatment mechanisms. For example, individuals studying mentalization-based treatment for BPD, which foundationally operates on theory of mind mechanisms by helping BPD patients increase their ability to represent the mental states of others, 135 may benefit from inclusion of specific measures of social cognition, specifically theory of mind and empathy, to determine if/how treatment augments these and other social cognitive capabilities following treatment. Though evidence-based treatments for PTSD are not founded upon social cognitive treatment mechanisms, a recent meta-analysis suggests that they are effective for improving social functioning. 136 Researchers studying these treatments may benefit from the inclusion of some measure of social cognition to understand a) how PTSD treatment augments social cognitive capabilities and b) if/how social cognitive capabilities may be leveraged to enhance treatment outcomes.
Moreover, additional research is needed to understand how to comprehensively treat comorbid BPD and PTSD. Foundational understanding of the social-cognitive profile for individuals with this presentation will help clarify which treatment protocols and/or treatment mechanisms may be most central to alleviating symptoms. For example, though speculative, if it is confirmed that dysfunction in attributional style is primarily driven by BPD symptoms (eg, 52 ), then individuals interested in alleviating difficulties in attributional style may benefit most from BPD-focused treatment. Alternatively, a transdiagnostic consideration to social-cognitive dysfunction may best suit individuals with BPD and PTSD, should their dysfunction prove to be qualitatively different than individuals with BPD or PTSD alone. Ultimately, much more foundational work on BPD-PTSD comorbidity is needed to promote treatment-focused research in this area.
Limitations
Before concluding, we note several limitations of the present review. First, our adult-only inclusion criteria excluded adolescent populations, an important developmental period for both social cognition and BPD symptom emergence.137–139
Second, restricting to fMRI excluded other neuroimaging methods such as electroencephalogram (EEG), magnetoencephalography (MEG), positron emission tomography (PET), near-infrared spectroscopy, and diffusion tensor imaging (DTI), likely overemphasizing regional activation while underrepresenting temporal dynamics and structural connectivity.
Finally, small, convenience samples of higher-functioning individuals that can tolerate scanning procedures may not represent the heterogeneity in BPD and PTSD populations, limiting generalizability.
Conclusion
The objective of this scoping review was to examine the state of the literature on neural correlates of social cognition in BPD, PTSD, and their comorbidity. Only four papers were found to investigate social cognitive functioning in comorbid BPD and PTSD. Further, most studies focused on emotion processing, whereas other domains of social cognition, like social perception, theory of mind, empathy, and attributional style, were comparatively underexplored. Given the profound social impairments faced by individuals with both BPD and PTSD, understanding how these disorders interact to disrupt social cognition is critical to developing more effective interventions that enhance quality of life and functional outcomes for these individuals. Therefore, recognizing the high comorbidity that exists between these disorders, we encourage future researchers to include measures for both disorders to shed light on their overlapping and unique social cognitive deficits. Moreover, although behavioral studies offer valuable insights, this overview suggests that many differences in social cognition emerge at the neural level. Future research using fMRI will likely be beneficial in capturing these complexities. By addressing these gaps, future research can provide a better understanding of social cognitive functioning in BPD and PTSD, ultimately guiding the development of targeted interventions that alleviate the burden of these disorders.
Supplemental Material
sj-docx-1-css-10.1177_24705470261427216 - Supplemental material for Neural Correlates of Social Cognitive Functioning in Borderline Personality Disorder and Posttraumatic Stress Disorder: A Scoping Review
Supplemental material, sj-docx-1-css-10.1177_24705470261427216 for Neural Correlates of Social Cognitive Functioning in Borderline Personality Disorder and Posttraumatic Stress Disorder: A Scoping Review by Katherine Mary Samonek, Erin Z. Basol, Suzanne Estrada, Tetiana Davydovska, Melissa C. Funaro and Ilan Harpaz-Rotem in Chronic Stress
Supplemental Material
sj-docx-2-css-10.1177_24705470261427216 - Supplemental material for Neural Correlates of Social Cognitive Functioning in Borderline Personality Disorder and Posttraumatic Stress Disorder: A Scoping Review
Supplemental material, sj-docx-2-css-10.1177_24705470261427216 for Neural Correlates of Social Cognitive Functioning in Borderline Personality Disorder and Posttraumatic Stress Disorder: A Scoping Review by Katherine Mary Samonek, Erin Z. Basol, Suzanne Estrada, Tetiana Davydovska, Melissa C. Funaro and Ilan Harpaz-Rotem in Chronic Stress
Footnotes
Author Contributions
KMS, SE and IHR conceptualized the research question, analytic plan and exclusion/inclusion criteria. Searches of databases were conducted by MF. KMS and SE conducted abstract reviews. KMS and EZB completed full text-review with assistance from TD and SE. EZB and TD completed full-text reviews of relevant papers published in 2025. EB created charts and figures. EZB and KMS wrote the manuscript. EZB, KMS, SE, and IHR critically reviewed the manuscript. EZB and KMS completed the revisions to the manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Dr. Harpaz-Rotem reported receiving grants from Boehringer Ingelheim International GmbH outside the submitted work. The authors (KMS,EZB,SE,TD,MF) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability
Search terms and databases are available in the supplemental material 1. All articles that were reviewed and main findings are provided in the supplemental material 2. Additional data supporting the findings of this study may be made available from the corresponding author upon reasonable request and subject to institutional data sharing agreements.
Supplemental Material
Supplemental material for this article is available online.
