Abstract
Introduction
To deliver evidence-based care, medical professionals must be able to critically appraise scientific literature, a skill often underemphasized in traditional medical education.
Methods
Supported by the teaching commission of the Medical Faculty of Otto-von-Guericke-University Magdeburg, a novel didactic approach was developed, integrating elements of a Journal Club (JC) with e-learning modules, supervised by a mentor. This approach aims to deepen and apply scientific skills acquired in earlier stages of medical education. Final-year medical students independently select, critically evaluate, and present a scientific paper in a JC that is related to a specific patient. Simultaneously, they are required to complete six online modules (including an orientation module) covering the topics evidence-based clinical practice, literature search, Critical Appraisal Skills Program, basic statistical analysis, and effective presentation skills.
Results
In the pilot phase, 25 students and five mentors participated, with 20 students and four mentors completing the evaluation. Students rated the teaching project as relevant (mean 2.4, scale 1 - 4) but expressed mixed views on its suitability for final year (mean 2.5). Self-assessment scores improved across all five learning outcomes, with notable increases in students’ confidence to evaluate clinical relevance and study strengths/weaknesses. Digital modules were rated as comprehensible (scores 1.5 - 2.0) and useful for JC preparation (scores 2.1 - 2.6). The overall teaching project received a mean rating of 2.8 (scale 1 - 6), with 58% (n = 19) of students recommending the course. Mentors unanimously rated the project as highly beneficial (100% recommendation rate).
Conclusion
The evaluation of the pilot phase indicates that this teaching project has the potential to significantly enhance students’ ability to critically engage with scientific literature. Ongoing refinement based on feedback and planned implementation across all departments aim to promote sustainable scientific literacy in clinical training.
Introduction
Evidence-based patient care necessitates continuous engagement with the latest scholarly articles and reviews. Consequently, clinicians across all specialties face an enduring challenge: staying abreast of rapidly expanding scientific literature while relying on traditional educational resources with inherent temporal limitations. Textbooks, while indispensable for foundational knowledge, may already be partially outdated at the time of publication. 1 Medical education must therefore serve a dual purpose: to equip students with robust practical skills and to develop their ability to critically evaluate scientific literature, a competence that is essential for both clinical decision-making and potential academic pursuits.2,3 However, a gap persists between desired and actual evidence-based practice (EBP). 4 Many identified barriers to implementing EBP could be addressed through education, including inadequate research skills and insufficient knowledge for acquiring and appraising studies. 5 Recognizing these shortcomings in the German medical education, recent reforms such as the Masterplan Medical Studies 2020 and the National Competence-Based Learning Objectives Catalogue for Medicine (NKLM) have emphasized enhancing scientific literacy among medical students. 6
Although most medical students recognize research competencies as essential components of clinical practice and endorse both critical literature evaluation and mandatory research project participation, their self-reported scientific competencies remain unsatisfactory across Germany. 7 The final year of medical school in Germany, known as Practical Year (PY), is an excellent time to review, deepen, and practically apply scientific methodology. In the PY, students work on hospital wards, applying and deepening their previously acquired theoretical knowledge, skills, and abilities under supervision. 8 In earlier stages of medical training, students already participate in lectures and seminars that provide an initial overview of scientific methodology including biostatistics and clinical epidemiology.
Building upon this foundation, Journal Clubs (JCs) offer a format that allows for critically appraising recent literature, thereby bridging the gap between research findings and clinical application. It encourages the development of critical appraisal skills in medical education, residency programs, and research. 9 Established in the nineteenth century, JCs have continually been adapted to meet the educational needs of the medical community by fostering an environment of scholarly discourse and critical thinking.10–12 Concurrently, there has been a shift towards the Flipped Classroom (FC) approach, where students first engage with learning materials independently through digital media, allowing them to explore topics at their own pace and on their own terms. 13 This method enhances the in-class experience, focusing on higher-order cognitive activities rather than mere information delivery.14,15 The advent of the COVID-19 pandemic has even accelerated the adoption of digital teaching modalities, supplementing, or in some cases replacing, the traditional classroom experience. 16
In this context, the Department of Gastroenterology, Hepatology, and Infectious Diseases (KGHI), the Institute of Social Medicine and Health Systems Research (ISHSR), and the Office of Student Affairs of the Medical Faculty at the Otto-von-Guericke-University Magdeburg have collaboratively developed and piloted an innovative teaching project. This initiative, supported by the teaching commission, integrates a JC with a FC model to foster and deepen scientific skills in medical students in the PY. The initiative combines online modules covering key skills (eg, literature search, statistics, and critical appraisal) with a structured learning process. Students receive a real patient case, complete the digital modules to identify a related publication, and present their findings in a JC setting. Throughout the process, students are supported by a mentor. Beyond enhancing the educational experience, this project is designed to prepare future physicians to competently navigate and contribute to the medical research landscape. We report on the implementation and evaluation of the concept of the JC. In particular, we have investigated the students’ and mentors’ perceptions of the JC.
Methods
Context
The reporting of the study conforms to the SQUIRE-EDU (Standards for QUality Improvement Reporting Excellence in Education) guideline 17 (see Supplemental Table 1). The study was designed as a prospective single-center local pilot evaluation study on medical students in the PY at the Otto-von-Guericke-University Magdeburg, who participated in the JC. The PY follows the German medical education system, where students complete a mandatory 48-week clinical training period across internal medicine, surgery, and an elective specialty before graduation. During this period, students rotate through different clinical departments and are integrated into daily clinical routines under supervision. The PY JC was initially implemented at KGHI. This was primarily because KGHI was significantly involved in its development. Additionally, the Department of Neurology and the Department of Cardiology and Angiology were recruited to implement the JC. All PY students completing rotations in these departments were eligible to participate in the PY JC. For this pilot phase (February 2024 to June 2025), participation was voluntary. The recruitment of PY students to participate in the JC was achieved through two channels: an information session and one-on-one conversations on the ward.
PY Journal Club
The didactic approach is presented in Figure 1. While all PY students completed the online modules independently, the identification of a ward-based clinical case, selection of a related scientific article, and presentation at the JC could be done individually, in pairs, or in groups of three. Senior physicians were assigned as mentors to support the students throughout this process. Immediately, following each presentation, the mentors provided formative feedback, focusing on critical aspects such as adherence to the prescribed twenty-minute timeframe, the clarity and thoroughness of the topic introduction, the accuracy in presenting the study design and results, the effectiveness in stimulating discussion, and the overall quality of the delivery. This immediate feedback session enabled a dynamic interaction where students could pose follow-up questions, fostering a responsive and interactive learning environment.

Didactic approach (time frame: 8 weeks).
A distinctive feature of this program is the incorporation of the FC teaching method. In our project, this tool was applied by implementing a preparatory phase via the online teaching platform Video and Teaching Platform for E-learning (VIPER), segmented into five specific modules. All of these modules were co-developed by the authors and a purposefully recruited subgroup of medical students, ensuring a user-centric design and the integration of real-time feedback to refine both content and delivery. The modules included an orientation module to ensure a comprehensive understanding of the project requirements, evidence-based clinical practice, literature search methods, the Critical Appraisal Skills Program (CASP) evaluation tool, basic statistical analysis, and effective presentation skills. Each module includes a knowledge quiz to reinforce learning objectives and track individual progress. In addition, participants were provided with high-quality, peer-reviewed resources and curated external links for further in-depth exploration of each topic. Successful participation was confirmed through system-tracked completion of all modules and quizzes. Upon fulfilling all criteria, participants were awarded a final certificate documenting their successful completion of the VIPER curriculum.
Study of the PY Journal Club and Measures
We utilized the plan-do-check-act (PDCA) cycle for continual improvement, aligning with educational best practices and achieving learning outcomes. 18 The evaluation of the JC was accomplished with an anonymized questionnaire that was generated with the evaluation software evasys (https://evasys.de/). Completing the evasys survey is part of the standard evaluation process conducted for all courses at the Medical Faculty.
The evasys survey included 10 items, in which the degree of agreement (ranging from “strongly agree” to “strongly disagree”) is measured using a four-point or six-point Likert scale. 19 This approach not only measures the students’ knowledge acquisition post-course but also captures their self-assessed competencies prior to the course, facilitating a nuanced understanding of the knowledge gains as prescribed by the National Competence-Based Catalogue of Learning Objectives for Medicine (NKLM), which is closely aligned with the course's predefined learning objectives (Table 1). Students were asked about their ability to describe and differentiate parts of a scientific paper, determine the clinical relevance of a study, evaluate a study's strengths and weaknesses, present a study in a JC, and explain the challenges of translating scientific findings into clinical practice. We also asked the students how much time they needed in total to complete the online modules. The second section consisted of open-ended questions, providing an opportunity for free-text responses. To gain insight into the background of participating students, we assessed their prior experience with scientific work.
Learning Objectives.

The mentors were given a separate seven-item paper-and-pencil questionnaire to evaluate the PY JC from the teacher's perspective. This survey included 4 items, in which the degree of agreement (ranging from “strongly agree” to “strongly disagree”) was measured using a six-point Likert scale, two questions, each with three predefined answer options, and one open-ended question asking for suggestions for improvement. First, we assessed mentor attitudes toward the PY JC concept. Second, we evaluated mentor perceptions regarding the importance of e-learning modules within the teaching framework. Third, we examined the extent of support required for scientific article selection. Fourth, we investigated optimal timing for implementation, specifically whether the teaching project should be conducted during the final year of medical school or at an earlier stage. The remaining survey items explored mentor satisfaction with student presentations, elicited recommendations for program enhancement, and assessed willingness to recommend the PY JC to other students and educators.
Data Analysis
Students’ and mentors’ evaluations were descriptively analyzed. Continuous variables were presented as means and ranges. Free-text answers were analyzed using thematic analysis by coding the responses into frames based on recurring themes.
Ethical Considerations
The local ethics committee of the Medical Faculty of the Otto-von-Guericke-University waived the requirement of ethical approval for this study. The surveys were part of standard quality improvement procedures for educational courses. Participation was voluntary and anonymous, and the act of completing the survey constituted implied consent to participate.
Results
Students
Overall, 25 students participated in the PY JC during the pilot phase. Students organized themselves into five groups of three (n = 15 students), three pairs (n = 6 students), and four students presented individually, resulting in a total of 12 presentations. Twenty of the 25 medical students (80%) completed the evaluation. The vast majority of students (16 out of 20; 80%) reported having previous scientific experience, mainly through their doctoral thesis. After participating in the teaching project, the perceived relevance of the initiative averaged at 2.4 (1 = important, 4 = unimportant), and its suitability for the final year of medical school was rated 2.5 (1 = important, 4 = unimportant). Self-assessment scores improved across all five learning outcomes (Table 2). For example, regarding the ability to evaluate clinical relevance of studies, the number of students responding “strongly agree” increased from four pre-course to eight post-course, while those responding “somewhat agree” increased from seven to ten. Similarly, for evaluating studies based on their strengths and weaknesses, no students initially responded “strongly agree,” but seven students did so after course completion. Just under half of the students (45%) required 2-3 h, while around a third (35%) needed 4-5 h. Around a fifth of the students needed 3-4 h.
Mean Response Scores on the Learning Outcome Questions.
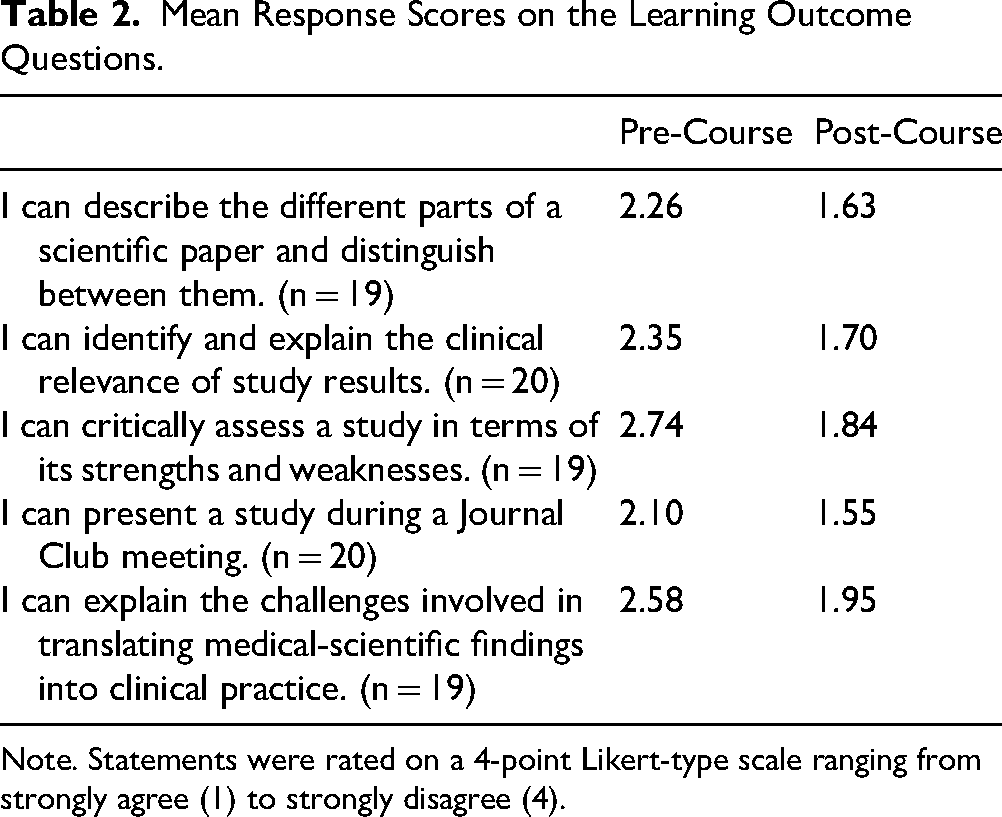
Note. Statements were rated on a 4-point Likert-type scale ranging from strongly agree (1) to strongly disagree (4).
The comprehensibility of various digital modules was rated between 1.5 and 2.0 (1 = strongly agree, 4 = strongly disagree), with the Evidence-Based Medicine module scoring highest and the CASP module scoring lowest. The usefulness of the digital modules for JC preparation ranged from 2.1 to 2.6, with the literature research module rated highest and the CASP module lowest (Table 3). The overall impression of the teaching project received an average score of 2.8 (1 = very good, 6 = very bad). Additionally, about two thirds (57.9%) of students would recommend the course, 15.8% would not, and 22.2% were neutral.
Mean Response Scores for the Evaluation of Online Modules (n = 20).

Note. Statements were rated on a 4-point Likert-type scale ranging from strongly agree (1) to strongly disagree (4).
CASP, Critical Appraisal Skills Program.
Thematic analysis of the free-text responses identified four key themes. First, mentor support emerged as a highly valued component of the intervention, with students particularly appreciating guidance in publication selection and presentation preparation. Second, peer collaboration was perceived as enriching, with students reporting that working together facilitated understanding of the online modules and enhanced their confidence in preparing presentations. Third, concerns about competing priorities were expressed, with some students stating that the PY should primarily focus on developing practical clinical skills rather than scientific competencies. Finally, time constraints during ward rotations were frequently mentioned, leading some students to suggest that protected self-study time could be reallocated to accommodate the teaching project more effectively.
Mentors
Four of five mentors involved in the JC (80%) responded. The mentors’ approval of the PY JC idea resulted in an average score of 1.5 for the project, resulting in a 100% recommendation rate. Three of the four mentors rated the e-learning modules as “very important” and one rated them as “important.” Two of the mentors said that their students had selected their articles largely independently, while the other two stated that their students needed a great deal of support. Three mentors stated that the final year is well suited to the teaching project. According to one mentor, the teaching project should take place prior to the final year of medical school. Mentor evaluations of student presentations yielded consistently positive results, with all ratings distributed between good and very good on the assessment scale.
Discussion
This study aimed to evaluate a novel teaching project designed to strengthen medical students’ scientific competencies as part of EBP during the PY. The course evaluation demonstrated that students appreciated the teaching project and recognized the importance of developing scientific skills. Self-assessments indicated improvements across all learning outcomes. Concurrently, students expressed uncertainty about implementing this teaching project during their final year, in light of concerns that this period should prioritize developing practical clinical skills. Mentors unanimously rated the project as highly beneficial.
In a review, Kyriakoulis et al outlined various educational strategies that have been implemented globally to teach EBP to undergraduate health students. 20 One central research question addressed how EBP should be taught to enhance student engagement and the overall learning experience. The reviewed studies utilized diverse instructional methods, including lectures, computer-based sessions, small group discussions, and class activities. Current evidence suggests that multifaceted approaches are superior in improving knowledge, skills, and attitudes compared to single-session interventions.21,22 Specifically, interventions combining multiple strategies, such as lectures, digital learning modules, small group discussions, JCs, and practical assignments, were shown to be more effective. Accordingly, the implementation of a multifaceted educational approach appears to be the most effective method for teaching EBP to medical students. In fact, our evaluations revealed that discussions with other students in small groups are highly desired and seem to enhance learning success. Students appreciate receiving feedback from both their mentors and their peers. This is referred to as peer-assisted learning in educational research.23,24 The group discussion after the presentation provided students with an additional chance to discuss the content of the e-learning modules and the presented publication, ask any remaining questions, and provide feedback to the mentors. Practical assignments included finding a publication to help students diagnose or treat a real patient on the ward. The survey given to the mentors showed that some of the students found this task somewhat difficult. This illustrates, in our view, the need to teach precisely these skills.
A crucial component of our approach is the digital learning content on VIPER, reflecting the digital transformation process affecting many areas, including education and everyday life. Students today seek more freedom in their learning process, including individual learning preferences. 13 The FC principle supports medical students in the integration of scientific evidence into their clinical decision-making and thus in the development of EBP. 25 By regularly participating in such discussions, students learn to think critically and evaluate the quality and relevance of study results. A JC also provides the opportunity to discuss the implementation of clinical guidelines. Students can learn how guidelines are developed, the evidence they are based on, and how they are applied in practice. This promotes a better understanding of the importance of guidelines and their application in clinical practice. By regularly presenting articles and moderating discussions, students can improve their presentation and moderation skills. These skills are not only important in science but also in clinical practice, as doctors often need to present information to colleagues or patients.
To enhance the effectiveness of the educational project, students are paired with a mentor. Mentorship has been identified as a critical component in the professional development of students. According to a comprehensive review by Atlas AM et al, which compared various mentorship programs from medical schools worldwide, the authors concluded that mentorship is critical in shaping the career trajectories and academic success of students. 26 In this context, it is essential that mentors are able to create a collaborative learning environment, which is something that they can do by fostering a sense of community and inclusivity among their students. 23 Additionally, the benefits of mentorship extend beyond the students. Mentors themselves report greater job satisfaction and a renewed sense of purpose in their professional roles. Participation in these programs allows mentors to refine their educational techniques and interpersonal skills, thereby fostering a more enriching and supportive learning environment. 26
The evaluation process aims to continuously improve the JC. Evaluations highlight the necessity for review and optimization of the digital modules using a PDCA cycle to ensure the sustainable success of the JC. For example, we have identified a particular need for improvement in the CASP and Statistics modules, which has been our priority for revision at the end of the pilot phase. Practical applications of CASP in medical education include improved decision-making, where students challenge study design and statistical analysis to make evidence-based decisions, ultimately improving patient care. 27 Additionally, we will include an introductory video by the head of the KGHI at the University Hospital Magdeburg in the e-learning modules, highlighting that medical education is a continuous process and that physicians must commit to lifelong learning to deliver optimal healthcare. In addition, the current evaluations reveal a trend indicating that the relevance of this form of JC should regularly be communicated to the students. Although students reported improvements in their skills in handling scientific studies, only 12 out of 20 students (57.9%) would recommend the course. This stands in contrast to the 100% recommendation rate of the mentors. We believe that participation in the PY JC benefits all students, not just those pursuing a scientific career. It enables them to learn and deepen the methods required to stay abreast of scientific developments throughout their medical careers, promoting lifelong learning.28–31 Along similar lines, the perceived dichotomy between “scientific” and “clinical” competencies may be artificial. EBP inherently requires both domains, and the JC format, which required students to link current ward cases with relevant literature, was designed to bridge rather than separate these competencies. However, the free-text responses revealed that time constraints during ward rotations were a significant concern for students. Some suggested reallocating existing self-study time to accommodate the PY JC more effectively. This feedback is valuable for future iterations. Protected time for educational activities within the clinical schedule, rather than expecting students to complete the PY JC in addition to clinical duties, may address these concerns. Integration of the PY JC into formal rotation schedules with appropriate workload adjustment could help students view it as a legitimate component of their training rather than an additional burden.
This study has several limitations that should be considered when interpreting the findings. First, the course was implemented in only three departments at a single university, potentially limiting generalizability to other settings. Second, participation in the JC was voluntary, likely resulting in a self-selected sample of motivated and interested students, which may have positively influenced the evaluation outcomes. Third, the relatively small number of completed evaluations limits the reliability of our results. Finally, this study was designed as an educational evaluation rather than formal research. Consequently, no a priori sample size calculation was performed, and the survey instrument was not formally validated or pilot-tested prior to implementation. Additionally, only aggregated data were available, which precluded calculation of standard deviations and statistical hypothesis testing. These methodological aspects inherently limit the methodological rigor of our findings. Future studies should include validated survey instruments, objective measures of knowledge acquisition (eg, pre-post tests), and potentially qualitative assessments to provide a more comprehensive evaluation of the PY JC's educational impact.
Conclusion
A collaborative educational initiative between KGHI, ISHSR, and the Office of Student Affairs was developed to enhance scientific skills among final-year medical students through a JC including digital learning experiences. This JC addressed the critical need for integrating theoretical knowledge with practical application while preparing students for an evolving healthcare landscape. Initial pilot feedback demonstrates promising potential for increasing student engagement in scientific inquiry and improving critical literature evaluation skills, though comprehensive evaluation remains pending.
Supplemental Material
sj-pdf-1-mde-10.1177_23821205261427290 - Supplemental material for An Innovative Journal Club Approach to Enhance the Scientific Skills of Medical Students: A Pilot Evaluation Study
Supplemental material, sj-pdf-1-mde-10.1177_23821205261427290 for An Innovative Journal Club Approach to Enhance the Scientific Skills of Medical Students: A Pilot Evaluation Study by Peter Lemmer, Antje Hoffleit, Niklas Heucke, Marwa Al-Dubai, Tarek Bekfani, Laurin Vinca, Markus Plaumann, Verena Keitel-Anselmino, Christian Apfelbacher and Claudia Buntrock in Journal of Medical Education and Curricular Development
Footnotes
Acknowledgments
We thank all students and mentors for their participation.
Ethical Considerations and Consent to Participate
The local ethics committee of the Medical Faculty of the Otto-von-Guericke-University waived the requirement of ethical approval for this study. The surveys were part of standard quality improvement procedures for educational courses. Participation was voluntary and anonymous, and the act of completing the survey constituted implied consent to participate.
Contribution List
PL contributed to conceptualization, funding acquisition, formal analysis, project administration, investigation, resources, writing—original draft, and writing—review & editing; AH contributed to conceptualization, software, data curation, resources, and writing—review & editing; NH contributed to software, project administration, and writing—review & editing; MAD contributed to project administration, investigation, resources, and writing—review & editing; TB contributed to project administration, investigation, resources, and writing—review & editing; LV contributed to software, resources, and writing—review & editing; MP contributed to software, resources, and writing—review & editing; VKA contributed to investigation, resources, and writing—review & editing; CA contributed to conceptualization, funding acquisition, supervision, and writing—review & editing; CB contributed to conceptualization, methodology, funding acquisition, formal analysis, supervision, and writing—review & editing.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: We acknowledge support by the Open Access Publication fund of the Medical Faculty of the Otto-von-Guericke-University Magdeburg.
Conflict of Interest Statements
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
