Abstract
Objective
To evaluate whether early exposure to cadaveric surgical simulation influences preclinical osteopathic medical students’ interest in pursuing surgical specialties.
Design
This single-blinded, prospective cohort study utilized pre- and post-simulation surveys to assess changes in specialty interest among participants. Responses were analyzed using Wilcoxon signed rank tests with significance set at P < .05.
Setting
Pacific Northwest University of Health Sciences, College of Osteopathic Medicine (PNWU-COM), during the 2024-2025 academic year.
Participants
Thirty preclinical osteopathic medical students (OMS1 and OMS2) volunteered, with 29 completing all study components (response rate: 97%). Of these, 20 (69%) identified as female and 9 (31%) as male; 19 (66%) were OMS1 students, and 10 (34%) were OMS2 students.
Results
Following participation in two cadaver-based surgical simulations—cardiothoracic and orthopedic—students demonstrated significant increases in overall interest in surgery (P = .004), cardiothoracic surgery (P = .001), and orthopedic surgery (P = .007). Additionally, interest in procedural care and the likelihood of pursuing a surgical residency increased significantly (P = .028 and P = .014, respectively). Conversely, interest in family medicine (P = .022) and internal medicine (P = .021) declined. Notably, 86% of participants reported that the cadaveric simulations influenced their perception of surgical fields, with nearly all stating that early exposure impacted their career considerations.
Conclusion
This pilot study strongly suggests that cadaveric surgical simulation significantly increases interest in surgical careers among preclinical osteopathic medical students. The impact was particularly strong in specialties directly represented in the simulations and among first-year students. These findings highlight the potential value of integrating structured surgical experiences into the early curriculum at osteopathic institutions, especially those without direct affiliations to major academic medical centers. Such interventions may help address the underrepresentation of osteopathic graduates in surgical residency programs and ultimately broaden diversity in surgical care.
Keywords
Introduction
Osteopathic medicine, founded in 1874 by Dr Andrew Taylor Still, encompasses the philosophy and practice of physician care in the United States (US) that emphasizes the body's natural tendency toward health and self-healing. 1 Today, Doctor of Osteopathic Medicine (DO) medical students make up more than 25% of the total US medical students, with more than 35,000 DO students across 35 states.1,2 In the 2023 U.S. News & World Report list of medical schools with the “Most Graduates Practicing in Primary Care,” eight of the top 10 schools were DO medical schools. 1
The 2024 residency match offered 41,503 positions, an increase of 1128 (3.28%) compared to 2023. Of the offered positions in 2024, 38,494 were Post Graduate Year 1 (PGY-1) positions, 1069 (3.78%) more than in 2023. 3 There were 8033 US DO seniors who submitted a rank order list, an increase of 597 (7.4%) from 2023. 4 Of these US DO seniors, 7412 matched to a PGY-1 position, representing a 92.3% first time match rate, an increase of 0.7%. 4 Of the 8033 US DO seniors who submitted a rank list, there were 1020 surgical applications (neurosurgery, orthopedic surgery, plastic surgery integrated, surgery—categorical, surgery—preliminary, thoracic surgery integrated, and vascular surgery) representing 12.7% of total DO applicants. 4 This is in comparison to the 19,755 allopathic (MD) seniors who submitted rank lists in 2024, of which 4187 (21.2%) were for surgical residencies. 4
Some hypotheses have stated MD medical students will gravitate towards the surgical specialties because they have early educational exposure as a result of being connected to either major teaching hospitals or academic centers. 5 While the majority of DO schools are located in rural areas and are not connected to a major academic institution that supplies integrated surgical exposure, this should not hinder DO medical students’ interest within the surgical specialities.6–8
This pilot study assessed DO medical students’ interest in surgical specialties from one institution, determining the impact of cadaveric simulation and exposure on preclinical student's overall surgical interest.6,7,9 The aim of this study was to determine if certain experiences or opportunities such as cadaveric simulation and early surgical exposure increases medical students interest and perception of surgical specialties at an DO institution.
Methods
Study Design and Participants
Preclinical students defined as first-year medical students (OMS1), and second-year medical students (OMS2) at Pacific Northwest University of Health Sciences, College of Osteopathic Medicine in Yakima, Washington (PNWU-COM) during the 2024-2025 academic year were eligible for inclusion. In the 2023 U.S. News & World Report, PNWU-COM ranked third for most graduates practicing in rural areas and fourth for most graduates practicing in primary care, exemplifying current trends in DO graduate specialties. Of the 281 eligible students who enrolled over the academic years 2024-2025, 162 (57.7%) identified as female and 119 (42.3%) identified as male.1,3 Exclusion criteria for the study was any student at PNWU-COM who were above the OMS2 level of education.
This study consisted of a single-blinded design where the study's hypothesis, aim, and the specific simulations were not advertised to participants. A sign-up email via JotForm was sent to current OMS1 and OMS2 medical students and was limited to the first 30 respondents. The IRB allowed the simulation to proceed with a maximum of 30 participants. Respondents were informed that two required sessions would take place across the academic year. Once 30 participants were signed-up, informed consent was carried out with each individual participant after the participant confirmed they were able to participate in both simulations. The reporting of this study conforms to the TREND statement (Supplemental Figure 1). 10
Measures
Interests in Surgery
Interest in surgery was assessed with a 5-point Likert scale from (1) “No Interest” to (5) “Strong Interest.” Additional questions followed (1) “Not Likely” to (3) “Very Likely,” or “Yes”/“No” format. The survey was sent to participants 2 days prior to the first simulation and then 2 days after the last simulation. This survey included the eight core rotations determined by the American Osteopathic Association (family medicine, internal medicine, pediatrics, surgery, psychiatry, OB/GYN, emergency medicine, and osteopathic manipulative medicine). 11 Each specialty was further broken down to include several fellowships/sub-specialties within each core rotation in an attempt to blind the surgical sub-specialties simulated in this study. Additional survey questions included determinants of interests (eg, utilization of anatomy, hand dexterity, immediate results, etc.). The pre- and post-survey used were original surveys thus being pilot tested (Supplemental Figures 2, 3).
Simulation
A body donor who previously consented to be used for research and education purposes was utilized for the simulations, and all rights of the body donor were protected. Two cadaveric surgery simulations were performed on April 5, 2025, and April 19, 2025—cardiothoracic surgery and orthopedic surgery, respectively. Both simulation events were broken down into three parts as follows, (1) a “pre-operative” meeting with participants consisting of a 15-min specialty specific case presentation, (2) the primary 90-min surgical simulation narrated by the presenting surgeons and observed by participants, and (3) a 15-min “post-operative” meeting with participants on what patients should expect for regular follow-up and potential complications.
During the simulations, there were three options to view the simulation. Option 1: a TV displaying a real-time overview video of the simulation. Option 2: a TV displaying a GoPro live stream being worn by the surgeon performing the simulation. Option 3: Direct observation by of the simulation. All participants were cycled through the three different options to ensure equal exposure.
The cardiothoracic surgery simulation was performed by a board-certified osteopathic cardiothoracic surgeon and osteopathic cardiothoracic surgery resident who performed an aortic valve replacement. For the orthopedic surgery simulation, a board-certified osteopathic orthopedic surgeon performed a total knee arthroplasty followed by a total hip arthroplasty. At the conclusion of the two simulations, the participants completed the same survey with additional questions aimed at cadaveric simulation and its impact on specialty interest perception.
Statistical Analysis
Differences of mean rank values between pre- and post-survey were compared using a Wilcoxon signed rank test. 12 Statistical analysis was conducted using JASP 0.19.3, significance was determined by P < .05. Data analysis was performed on the entire participant sample and further broken down by gender and/or cohort (OMS1 or OMS2).
Results
A total of 30 preclinical DO students participated in the study with 29 completed surveys for a response rate of (97%). Overall, 69% (n = 20) of participants identified as women and 31% (n = 9) identified as men. In regard to participant cohort, 66% (n = 19) were OMS1 students and 34% (n = 10) were OMS2 students. Demographic characteristics of the participating preclinical students are displayed in Table 1.
Demographic Characteristics of Preclinical Participants.

SD: standard deviation.
Pre-Simulation Versus Post-Simulation Survey
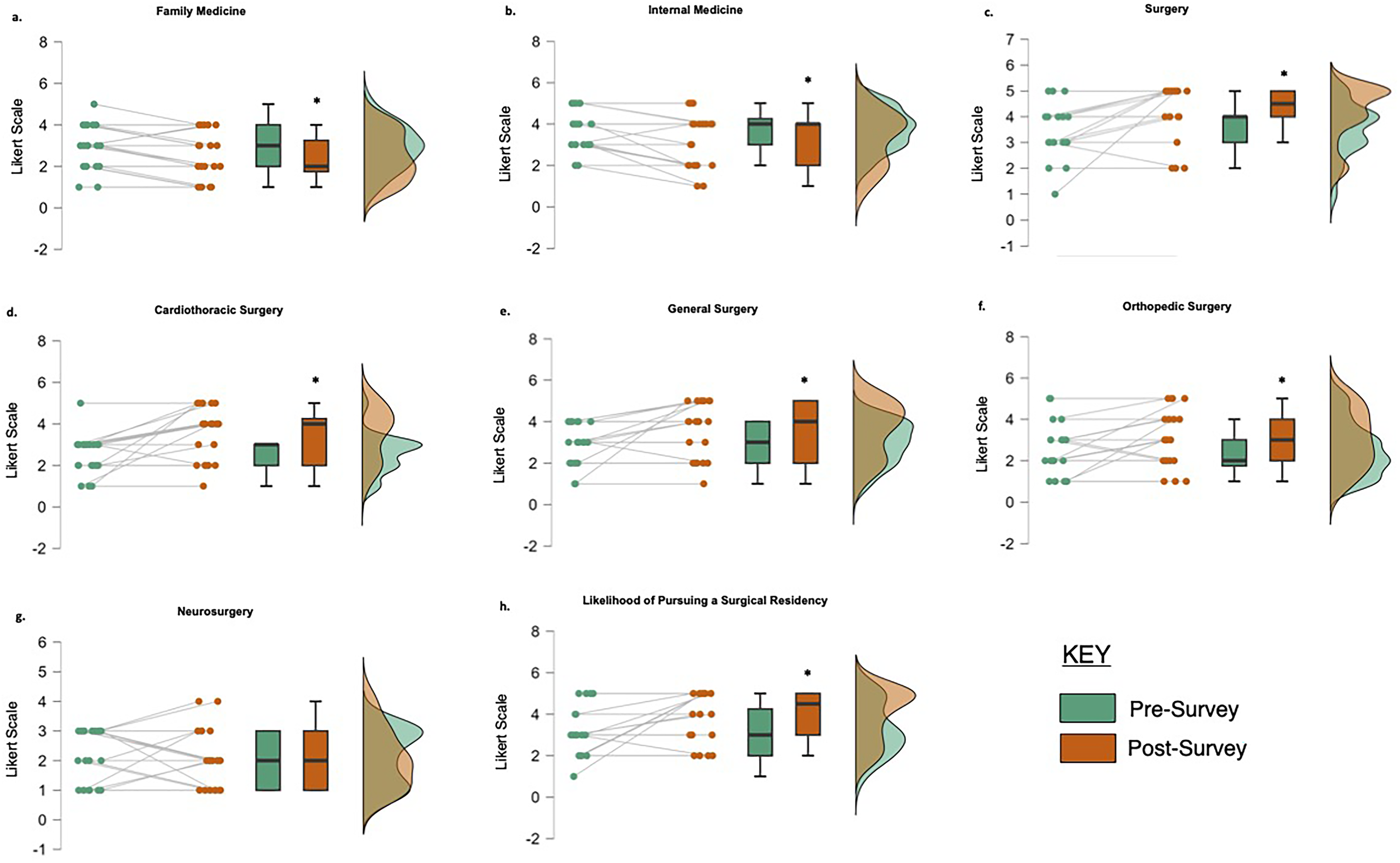
Students’ overall interest in surgery (P = .004), cardiothoracic surgery (P = .001), general surgery (P = .009), and orthopedic surgery (P = .007) significantly increased from pre-simulation to post-simulation (Table 2, Figure 1). Conversely, student interest in family medicine (P = .022) and internal medicine (P = .021) significantly decreased (Table 1, Figure 1). Significant interest increases were also observed in Procedural Care (P = .028) and Likelihood of Pursuing a Surgical Residency (P = .014), shown in Table 2. 25 participants (86%) reported that the cadaveric simulation influenced their answers, and 14 participants (48%) answered “Very Likely,” 14 (48%) “Likely,” and 1 (4%) “Not Likely,” on whether preclinical exposure impacted their overall surgical impression.

Combine Cohorts Interest Results. Dot, Box-and-Whisker, and Rain Shadow Plots of the Overall Cohort. a) Family Medicine Interest. b) Internal Medicine Interest. c) Surgery Interest. d) Cardiothoracic Surgery Interest. e) General Surgery Interest. f) Orthopedic Surgery Interest. g) Neurosurgery Interest. h) Interest in Pursuing a Surgical Residency. Green Data Points are Pre-Survey Responses; Orange Data Points are Post-Survey Responses. *Indicates Significance.
Students’ Outcomes Before and After Cadaveric Simulation.

Overall cohort of 29 preclinical participants. Highlighted boxes indicate survey questions that were significant (P < .05) using Wilcoxon signed rank test. “Pre” is mean +/− SD of pre-observation Likert Scale response with “Post” being the mean +/− SD of post-observation Likert Scale response. *Indicates a survey question that was “Yes (1)” or “No (2).” P: calculated significance level P < .05.
Gender
Women had significant increases in cardiothoracic surgery (P = .004), general surgery (P = .024), orthopedic surgery (P = .044), Likelihood of Pursuing Surgical Residency (P = .033), and whether Cadaveric Simulation Influenced Answers (P < .001), as shown in Figures 2 and 3. For the male participants, procedural care demonstrated the only significant increase in interest (Figure 3).
Female Cohort Interest Results. Dot, Box-and-Whisker, and Rain Shadow Plots of the Female Cohort. a) Family Medicine Interest. b) Internal Medicine Interest. c) Surgery Interest. d) Cardiothoracic Surgery Interest. e) General Surgery Interest. f) Orthopedic Surgery Interest. g) Neurosurgery Interest. h) Interest in Pursuing a Surgical Residency. Green Data Points are Pre-Survey Responses; Orange Data Points are Post-Survey Responses. *Indicates Significance.

Male Cohort Interest Results. Dot, Box-and-Whisker, and Rain Shadow Plots of the Male Cohort. a) Family Medicine Interest. b) Internal Medicine Interest. c) Surgery Interest. d) Cardiothoracic Surgery Interest. e) General Surgery Interest. f) Orthopedic Surgery Interest. g) Neurosurgery Interest. h) Interest in Pursuing a Surgical Residency. Green data Points are Pre-Survey Responses; Orange Data Points are Post-Survey Responses. *Indicates Significance.
Cohort
OMS1 students had significant increases in interest in cardiothoracic surgery (P = .005), general surgery (P = .015), Knowledge of Organ Systems (P = .025), Procedural Care (P = .037), Likelihood of Pursuing Surgical Residency (P = .033), and Cadaveric Simulation Influence on Answers (P < .001), as shown in Figure 4. OMS2 students demonstrated a significant increase in interest in orthopedic surgery (P = .048), shown in Figure 5.

OMS1 Cohort Interest Results. Dot, Box-and-Whisker, and Rain Shadow Plots of the OMS1 Cohort. a) Family Medicine Interest. b) Internal Medicine Interest. c) Surgery Interest. d) Cardiothoracic Surgery Interest. e) General Surgery Interest. f) Orthopedic Surgery Interest. g) Neurosurgery Interest. h) Interest in Pursuing a Surgical Residency. Green Data Points are Pre-Survey Responses; Orange Data Points are Post-Survey Responses. *Indicates Significance.

OMS2 Cohort Interest Results. Dot, Box-and-Whisker, and Rain Shadow Plots of the 2027 Cohort. a) Family Medicine Interest. b) Internal Medicine Interest. c) Surgery Interest. d) Cardiothoracic Surgery Interest. e) General Surgery Snterest. f) Orthopedic Surgery Interest. g) Neurosurgery Interest. h) Interest in Pursuing a Surgical Residency. Green Data Points are Pre-Survey Responses; Orange Data Points are Post-Survey Responses. *Indicates Significance.
Discussion
Over the last decade, both DO and MD medical student interest in pursuing surgery as a career has declined.13,14 Historically, the Halsted apprenticeship model of “see one, do one, teach one” has served as the cornerstone of surgical education.15,16 However, osteopathic medical schools often face limited early exposure to surgical settings, thereby potentially missing the critical “see one” phase. Surgical simulations provide a valuable opportunity for students to familiarize with surgical skills in a safe, structured environment that promotes learning without compromising patient safety.15,17
Pre- Versus Post-Observation Outcomes
Early exposure to surgical simulation has demonstrated a positive influence on student interest in surgical careers and yet, such opportunities remain underutilized in osteopathic medical education.7,13,14 In this study, cadaveric surgical simulations significantly increased surgical interest among preclinical DO medical students. Specifically, we found that student interest in the simulated surgical specialties (cardiothoracic and orthopedic) increased significantly. On the other hand, student interest in the non-simulated neurosurgery specialty did not change (P = .678) in response to observing surgical simulations. This suggests that exposure to specific surgical sub-specialties may be extremely influential in shaping medical students’ interests.
Female Versus Male Post-Observation Outcomes
The effects of surgical simulation exposure were more pronounced among female students. Surgical interest among women increased significantly overall (P = .015), with specific gains in cardiothoracic (P = .004), general (P = .024), and orthopedic surgery (P = .044). Moreover, female students were significantly more likely to report an increased intent to pursue a surgical residency (P = .033). In contrast, male participants did not demonstrate significant changes. These findings suggest that early surgical exposure may play a particularly influential role in promoting surgical interest among female medical students, potentially helping to address gender disparities in surgical fields.7,13
Cohort Outcomes
OMS1 students showed greater increases in surgical interests compared to OMS2 students, possibly indicating that earlier exposure may have a stronger impact on career perception. These findings underscore the importance of integrating surgical simulation experiences earlier rather than later in preclinical medical education.
In addition to live surgical simulations, as medical education continues to evolve, the integration of emerging technologies such as virtual reality and artificial intelligence offers promising avenues to implement surgical simulation into early medical school curriculum.18,19 These tools can provide experiences that may further reduce barriers to early surgical exposures, particularly in those institutions with limited access to resources such as DO medical schools.20–22
Limitations
This study has several limitations. First, participant selection was based on the first 30 students to enroll in the study, introducing potential selection bias. Although study details were not shared during sign-up, students with a preexisting interest in surgery may have been more likely to participate. Secondly, this study relies on self-reported survey data; it is possible that the results reported herein suffer from response bias. Thirdly, attempting to measure any subjective variable such as personal interest provides some level of uncertainty in the quantitative nature of the results. Likert scales represent a mechanism to quantify inherently qualitative data, but how individuals define their subjective interest varies case-by-case. Finally, the variability in simulation exposure, ranging from live stream viewing to direct tableside observation may have influenced the degree of engagement or perceived impact.
Conclusion
In this single institution prospective cohort study, we observed the value of early surgical simulation in fostering surgical interest among osteopathic medical students, particularly women and early-stage trainees. Understanding how early experiences impact students’ perception of the surgical specialties may be important for educators to consider as they work on improving diversity among the surgical field. Future directions will involve offering simulation experiences to entire preclinical classes and conducting longitudinal follow-up to track residency match outcomes. Comparing surgical match rates to previous years will help assess the lasting impact of early exposure on career trajectories in DO surgical education.
Supplemental Material
sj-pdf-1-mde-10.1177_23821205251381961 - Supplemental material for From Simulation to Surgery: Gauging Surgical Interest in Osteopathic Medical Students Through Cadaveric Simulation: A Pilot Study
Supplemental material, sj-pdf-1-mde-10.1177_23821205251381961 for From Simulation to Surgery: Gauging Surgical Interest in Osteopathic Medical Students Through Cadaveric Simulation: A Pilot Study by Schafer Paladichuk, Tanner Chase, Alex Downs, Christian Heck, Matt Cortner, Hannah Cornwell, Tianfu Shang, Zachary Brennan, Ronald F. Walser, Kylie Kerber and Tyler Wallen in Journal of Medical Education and Curricular Development
Supplemental Material
sj-pdf-2-mde-10.1177_23821205251381961 - Supplemental material for From Simulation to Surgery: Gauging Surgical Interest in Osteopathic Medical Students Through Cadaveric Simulation: A Pilot Study
Supplemental material, sj-pdf-2-mde-10.1177_23821205251381961 for From Simulation to Surgery: Gauging Surgical Interest in Osteopathic Medical Students Through Cadaveric Simulation: A Pilot Study by Schafer Paladichuk, Tanner Chase, Alex Downs, Christian Heck, Matt Cortner, Hannah Cornwell, Tianfu Shang, Zachary Brennan, Ronald F. Walser, Kylie Kerber and Tyler Wallen in Journal of Medical Education and Curricular Development
Supplemental Material
sj-pdf-3-mde-10.1177_23821205251381961 - Supplemental material for From Simulation to Surgery: Gauging Surgical Interest in Osteopathic Medical Students Through Cadaveric Simulation: A Pilot Study
Supplemental material, sj-pdf-3-mde-10.1177_23821205251381961 for From Simulation to Surgery: Gauging Surgical Interest in Osteopathic Medical Students Through Cadaveric Simulation: A Pilot Study by Schafer Paladichuk, Tanner Chase, Alex Downs, Christian Heck, Matt Cortner, Hannah Cornwell, Tianfu Shang, Zachary Brennan, Ronald F. Walser, Kylie Kerber and Tyler Wallen in Journal of Medical Education and Curricular Development
Footnotes
Acknowledgements
The authors sincerely thank those who donated their bodies to science so that anatomical research and teaching could be performed. Results from such research can potentially increase scientific knowledge and can improve patient care. Therefore, these donors and their families deserve our highest respect.
Ethical Approval
The Institutional Review Board (IRB) of the Pacific Northwest University of Health Sciences, Yakima, WA deemed this project exempt (IRB #24-037) from full IRB review.
Consent
All participants underwent individual informed consent and were provided copies of the consent form and IRB approval.
Authors Contributions
SP, TC, AD, CH, MC, HC, TS, ZB, RW, KK, and TW conceived and planned the experiments. SP, TC, AD, CH, MC, HC, TS, ZB, RW, and TW planned and carried out the simulations. SP, TC, AD, CH, MC, HC, TS, ZB, RW, KK, and TW contributed to the interpretation of the results. SP took the lead in writing the manuscript. All other authors provided critical feedback and helped shape the research, analysis, and manuscript.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Edwards Lifescience In-Kind Grant [grant numbers GSURG20251917].
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Declarations
All participants underwent individual written informed consent and were provided copies of the consent form and IRB approval.
Supplemental Material
Supplemental material for this paper is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
