Abstract
Introduction
Despite the well-established role of nutrition in preventing and managing chronic diseases, medical education often lacks sufficient training in nutrition counseling. To address this gap, the Florida International University Herbert Wertheim College of Medicine introduced a 2-hour, case-based active learning session on diabetes-related nutrition education. This cohort study evaluates the session's effectiveness in improving students’ knowledge of nutritional therapy for diabetes, evidence-based research methods, and the role of social determinants of health (SDOH).
Methods
The study followed two cohorts of second-year medical students from the Classes of 2024 and 2025. Students participated in a session that combined an introductory lecture with two small-group case-based exercises. Interactive technology-enhanced quizzes assessed pre- and post-session knowledge on diabetes nutrition, research methodology, and SDOH considerations. Additionally, end-of-course surveys evaluated students’ perceptions of learning. Statistical analyses included the Two-Proportion Z-Test for quiz results and the Mann–Whitney U Test for survey responses.
Results
Significant improvements were observed in students’ knowledge of nutritional management for diabetes and evidence-based research strategies (p < 0.05). However, no significant changes were found in SDOH-related knowledge, likely due to high pre-session baseline scores. End-of-course surveys indicated positive student perceptions of the session, with scores largely stable across cohorts, though perceptions of nutritional guidance benefits were slightly lower in the Class of 2025 (p = 0.0282).
Discussion
The case-based active learning session effectively enhanced knowledge acquisition and was well-received by students while requiring minimal faculty involvement. Future research should assess long-term retention and integrate nutrition education longitudinally across the curriculum.
Keywords
Introduction
Despite strong evidence linking nutrition to disease prevention, medical schools often lack adequate clinical nutrition education, leaving physicians unprepared for dietary counseling. Adopting healthy dietary patterns like the DASH or Mediterranean diet, alongside physical activity, significantly reduces the risk of chronic diseases such as diabetes, cardiovascular disease, and certain cancers. 1 Many medical school curricula, nevertheless, fail to provide sufficient training in nutrition counseling and lifestyle guidance due to challenges like limited curriculum time, lack of faculty expertise, limited faculty availability, and institutional resistance. Educators advocate for structured nutrition instruction, combining theoretical knowledge with practical skills. 2 In one medical school in Europe, for example, medical students and faculty have called for broad-based nutrition education incorporating international recommendations, self-care, and hands-on training. 3
In the United States, surveys highlight critical gaps in medical nutrition education. A 2010 study found only 27% of medical schools met the 25 hours of nutrition training recommended by the National Academy of Sciences, with little improvement by 2018, when 29% of schools surveyed reported meeting the target. In the same 2018 study, only 14% of residency programs reported meeting specialty society recommendations for nutrition training. 4
To address some of these gaps in its own curriculum, the Florida International University Herbert Wertheim College of Medicine (HWCOM) introduced a required take-home assignment in nutrition with regard to diabetes in its endocrinology course, starting in 2017. In 2019, the take-home nutrition assignment was converted into a 2-hour case-based active learning session. The session includes an introductory lecture followed by two case-based, self-facilitated, small-group discussions, requiring minimal faculty involvement while maintaining student engagement. It emphasizes evidence-based medicine and social factors in patient care. Feedback on end-of-course student-perceptions-of-learning questions indicated improved understanding of nutritional recommendations and of research skills related to type 2 diabetes. 5
Building on these efforts, the HWCOM team sought to follow two subsequent cohorts of students and assess their knowledge acquisition related to the session by integrating interactive pre- and post-session quizzes. Studies suggest technology-enhanced learning improves engagement and retention.6–9 The researchers hypothesized that the revised, case-based session would significantly improve students’ knowledge of nutrition therapy in the context of diabetes, enhance their ability to appraise and apply evidence-based research, and reinforce their understanding of social determinants of health (SDOH) as they relate to clinical management. Our specific aims were twofold: (a) to evaluate changes in student knowledge related to diabetes nutrition, research methodology, and SDOH before and after the session and (b) to assess student satisfaction with the learning experience.
Methods
Educational Sessions
The sessions described in this paper expand upon a format designed by the educational research team and described previously. 5 The 2-hour sessions were part of the required Endocrine Systems course for second-year medical students and began with an introductory lecture and concluded with two self-facilitated small-group case-based activities. Students prepared ahead of time by reviewing an American Diabetes Association (ADA) nutrition consensus report. 10
The introductory lecture, delivered by a family physician, covered nutritional guidelines for diabetic patients, a case summary, an evidence-based literature search model, and instructions for the group exercise. The entire session was designed to be interactive, opening with an overview of what to expect plus the learning objectives. Volunteer students then reported out on their assigned reading, the “Nutrition Therapy for Adults with Diabetes or Prediabetes: A Consensus Report,” followed by the case, read out loud by audience participants. The session leader next explained the small group tasks and directed the audience to resources. The lecture closed with an opportunity for the students to ask questions.
The half-hour lecture was altered for the Classes of 2024 and 2025 by the addition of technology-enhanced interactive elements. Prior to the lecture, students took a short three-question quiz. The interactive elements of the lecture and the pre- and post-session quizzes were made using the TurningPoint platform.
In a small-group-within-large-group format, a family physician and two staff members moderated the remainder of the session, in which students, divided into pre-assigned groups of approximately six, analyzed a case of newly diagnosed type 2 diabetes. The case prompted two small-group application exercises. First, each team developed a guideline-appropriate set of nutrition recommendations for the patient with diabetes and found research articles published within the last 5 years to support their nutrition recommendations. The teams compared their findings to the ADA report, selected one exemplary article, and justified their choice. Second, teams developed a problem list, considered SDOH, and developed a problem-by-problem assessment and plan for the patient. Three teams selected at random presented their results at the session's close. Once the debrief was concluded, students took a post-session three-question quiz. Participation in the session counted as 1% of the Endocrine Systems course grade. This allocation towards the course grade was in alignment with HWCOM policies for pass/fail courses, providing incentive for student participation in active learning sessions and based on the curricular time involved.
Case Vignette
The case that animated the application exercises was developed by one of the session facilitators (JB). It was modified from a case previously pilot tested and used as a take-home exercise, administered to prior cohorts of students, and described in the investigators’ prior publication. 5 The scenario involved a 25-year-old man exhibiting symptoms of type 2 diabetes who had also lost his job 18 months prior to the visit and had no health insurance. The case scenario purposely highlighted competencies noted across international nutrition education guidelines, including evidence-based nutrition approaches, sociocultural factors influencing dietary intake, and critical analysis of nutrition evidence. 11
Participants
Participants in this study were students from the Classes of 2024 and 2025, who attended the active learning endocrinology session, known as a “critical thinking” activity. The Class of 2024 consisted of 110 students, and the Class of 2025 consisted of 134 students. Demographically, over the period of the study, cohorts of medical students at HWCOM were 60% female and 40% male. For the Class of 2025, 46% of the cohort was from minorities underrepresented in medicine; 20% of the cohort were first-generation college students; 34% identified as Hispanic/Latino; 12% identified as African American/Black; 19% identified as Asian; and 30% identified as White non-Hispanic. 12
All students in both cohorts were eligible to participate. There were no exclusion criteria. Both elements of the study—interactive knowledge quizzes and end-of-course surveys—were voluntary. The authors aimed for a target response rate of at least 52.7%, as recommended in the work of Baruch and Holtom, to mitigate against potential non-response bias. 13 The study received “Not Human Subject Research (NHSR)” exempt status from the Florida International University Institutional Review Board, IRB NHSR Number IRB-25-0089.
Interactive Knowledge Quizzes
Students from the Classes of 2024 and 2025 who attended the “critical thinking” sessions were invited to take a pre-session quiz at the onset of the session and an identical post-session quiz at the end. The multiple-choice questions addressed nutrition management of diabetes, the preferred approach for evidence-based research to guide clinical management, and the impact of social factors on the management of diabetes. (Please see Appendix A.)
The quiz questions were created based on the session learning objectives (SLOs). These objectives were: SLO 1, describe nutritional recommendations for type 2 diabetes; SLO 2, explain how SDOH affect patient care and health outcomes in type 2 diabetes; SLO 3, select and analyze journal articles, applying understanding of evidence-based medicine; and SLO 4, perform a literature search to address a clinical question. The faculty facilitators for the session (authors SM and JB) created the questions, with quiz question 1 mapped to SLO 1, quiz question 2 mapped to SLO 3 and 4, and quiz question 3 mapped to SLO 2.
The SLOs themselves were based on international recommendations for nutrition education in undergraduate medical education published in 2015 by Crowley et al. 11 These recommendations remain consistent with the most recent JAMA consensus statement nutrition competencies for medical students. Such competencies include: #1 Provides evidence-based, culturally sensitive nutrition and food recommendations to patients for the prevention and treatment of disease (maps to quiz question 1); #8 Integrates evidence-based nutrition information from national nutrition guidelines, scientific publications, and other sources into patient care (maps to quiz question 2); and #10 Demonstrates sensitivity to the social, cultural, emotional, economic, educational, and psychological factors that may affect an individual's nutrition behavior, food choices, and health status (maps to quiz question 3). 14
End-of-Course Surveys
Both the Class of 2024 and Class of 2025 completed identical end-of-course surveys which included questions assessing the “critical thinking” session's impact on literature search skills, understanding of nutritional recommendations for type 2 diabetes, and SDOH awareness. Respondents utilized a five-point Likert scale, ranging from “Strongly Disagree” to “Strongly Agree.” 15 (Please see Appendix B.) The Likert-scale questions were consistent with similar questions used in all end-of-course surveys at HWCOM. One of the investigators (SM) created the questions de novo and another investigator (JB) assessed them for face validity.
Statistical Analyses
Data were analyzed using the R programming language version 4.3.1. The level of significance (alpha) was set at 0.05. For the knowledge quizzes, the Two-Proportion Z-Test was used to compare the proportions of correct answers before and after the class for the three questions. The results were dichotomized into “correct” versus “incorrect” responses for the multiple-choice questions, and the research team analyzed de-identified responses. For the end-of-course student-perceptions-of-learning questions, the Mann–Whitney U Test was used to determine if there were statistically significant differences in the distributions of responses across the two class years (2024, 2025) for each survey question. Investigators analyzed the de-identified responses, comparing mean scores between cohorts.
Results
Small Group Debrief
For both cohorts, the small group report-outs at the end of the session revealed consistent themes. Groups typically identified diet recommendations for the patient consistent with the American Diabetes Association consensus statement. Among the dietary approaches most frequently cited was the Mediterranean diet. Students often selected studies that focused on culturally sensitive diet recommendations, taking into account a patient's background instead of “one size fits all” recommendations. Student groups also tended to note the need to be attentive to cost concerns, highlighting prescription coupon programs or low-cost medication programs in the local community.
Participation Rates in Quizzes and End-of-Course Surveys
The pre- and post-session quizzes and the end-of-course surveys for both cohorts were all voluntary, but large proportions of the cohorts participated. For the Class of 2024, between 82% and 88% of the students completed the pre- and post-session quiz questions. Approximately 64% of the cohort completed the end-of-course survey. For the Class of 2025, from 63% to 68% of the students completed the pre- and post-session quiz questions. Approximately 85% of the students completed the end-of-course survey. Please see Tables 1 and 2.
Response Rates for Quiz Questions.

Response Rates for End-of-Course Survey Questions.

Interactive Knowledge Quizzes
For both cohorts, respondents demonstrated a notable increase in the proportion of students answering correctly for Quiz Question 1. In the Class of 2024 cohort, 56.0% of students answered the question correctly prior to the session, and 76.7% answered correctly after the session [change in proportion +20.6%, CI (+7.2%, +34.1%), p = 0.003]. In the Class of 2025 cohort, 48.4% answered the pre-session question correctly, with 85.6% answering the post-session question correctly [change in proportion +37.2%, CI (+24.6%, +49.8%), p = 1.06e-07].
Question 2 showed similar changes in both cohorts. For the Class of 2024, 89.6% answered correctly before the session and 98.9% afterward [change in proportion +9.3%, CI (+2.8%, +15.8%), p = 0.007]. For the Class of 2025, 92.2% answered the pre-session question correctly and 98.9% post-session [change in proportion +6.6%, CI (+0.7%, +12.6%), p = 0.034].
Question 3 did not demonstrate significant changes in either cohort. In the Class of 2024 cohort, 99.0% of respondents got the correct answer before the session and 96.7% afterwards [change in proportion −2.3%, CI (−1.9%, +6.5%), p = 0.287]. In the Class of 2025, 98.9% got the pre-session question correct and 100% got it correct post-session [change in proportion +1.1%, CI (−3.2%, +1.0%), p = 0.335]. Please see Table 3.
Proportion of Correct Answers for Pre- and Post-Session Quiz Questions.

End-of-Course Surveys
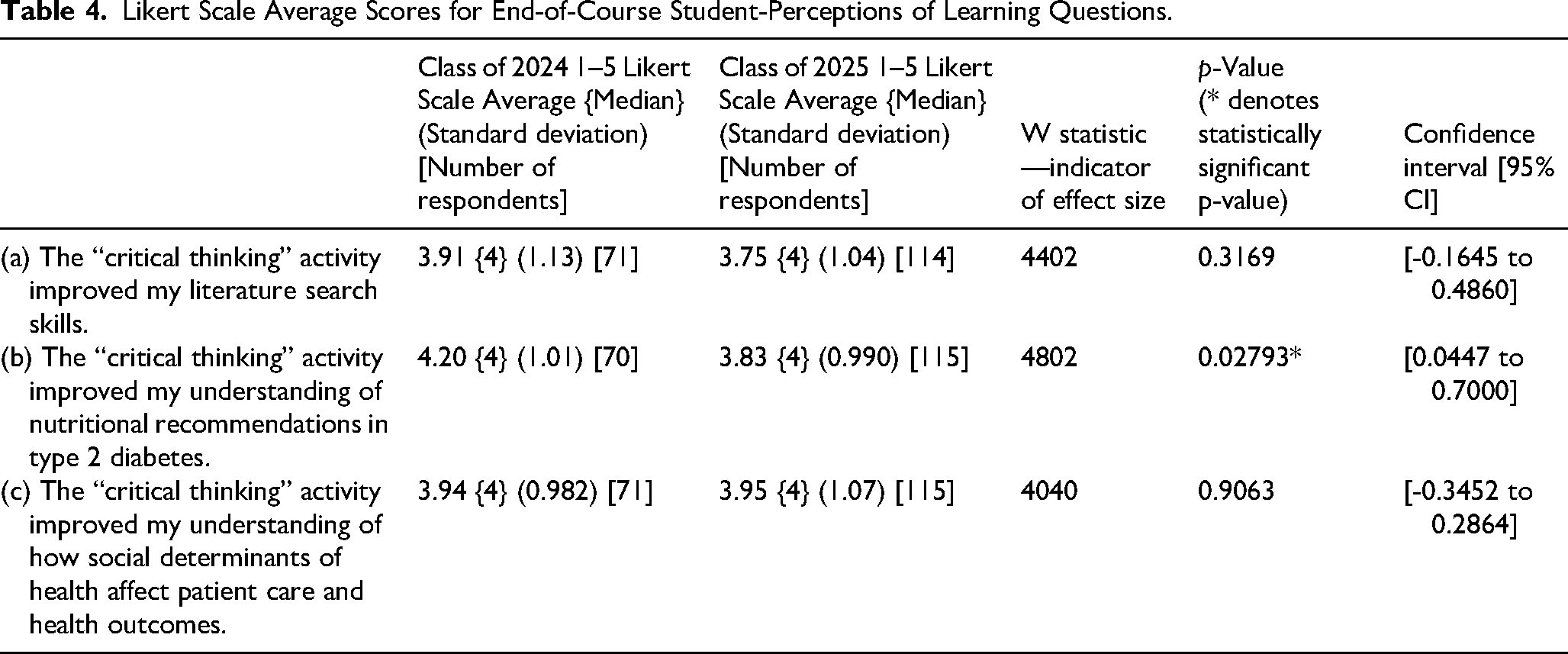
For the Class of 2024, the average score for the literature search skills survey question was 3.91 on a Likert scale of 1 to 5, for the nutritional recommendations question was 4.20, and for how SDOH affect patient care and health outcomes was 3.94. Standard deviations were 1.13, 1.01, and 0.982, respectively. On the same survey questions for the Class of 2025, the Likert scale averages were 3.75, 3.83, and 3.95 for the respective questions. Standard deviations for this cohort were 1.04, 0.990, and 1.07, respectively. p-Values based on Mann–Whitney U tests for the three questions were 0.3169, 0.02793, and 0.9063, respectively. The difference noted on Question 2 is statistically significant. Please see Table 4.
Likert Scale Average Scores for End-of-Course Student-Perceptions of Learning Questions.
Discussion
These results suggest that the small-group-within-large-group session fostered short-term knowledge acquisition with regard to nutritional guidance for diabetes and evidence-based research while maintaining positive student evaluations of the session. With regard to the pre- and post-session quizzes, for both years, the student respondents demonstrated statistically significant improvements in their knowledge of appropriate nutritional guidance for type 2 diabetes and of how best to pursue evidence-based research in a clinical setting. The question related to patients’ social needs did not show significant improvements, but to some extent, this result is expected. The SDOH are a prominent area of focus at HWCOM, and students are exposed to these concepts early on and in multiple courses. For both the Class of 2024 and 2025, the pre-session scores on the SDOH question were already >98% correct. Such scores suggest that the question could be removed or revised to better challenge the students at this stage in their training.
With regard to the end-of-course evaluations, the students across both years largely agreed with the statements that the critical thinking session improved their understanding of nutritional guidance for type 2 diabetes, their ability to perform a literature search, and their grasp of the importance of SDOH in diabetes care. The student perceptions of their learning about nutritional recommendations were statistically significantly lower for the Class of 2025 than the Class of 2024. One possible reason simply could be the result of different response rates. For the Class of 2025 cohort, a larger percentage of the students answered the voluntary survey, which could have altered the results. For comparison, in the researchers’ previously published work, for the Class of 2022, the Likert scale averages were 3.78, 4.00, and 3.93 for the respective questions, which suggests that the student perceptions have remained largely stable. 5
Collectively, the results further confirm the effectiveness of this case-based learning format as being well-received by students while requiring minimal faculty and staff involvement, as previously published. 5 This research provides additional evidence that the format also demonstrates evidence of short-term knowledge acquisition. Designed both with the instructors’ learning objectives and the students’ needs in mind, it required a small amount of pre-session preparation on the part of the students but achieved high yield engagement during the session itself. The session falls within a mini-sequence built to provide the students in the Endocrine Systems course with a multidimensional approach to diabetes care. The three sessions include the “critical thinking” session, a meet-the-patient session, and a complementary and alternative medicine session, which further solidifies the importance of diet while also covering the role of supplements.
The sequencing of educational interventions has emerged as an important factor in fostering student interest, engagement, and learning, when designing active learning sessions within and across courses. As sequenced active learning becomes more frequently utilized in medical education, it represents a shift toward a more student-driven learning environment. 16 Burgess and colleagues, for instance, recommend utilizing active learning approaches like team-based learning earlier in medical school—typically the first year—followed by case-based learning strategies latter, typically in the second year. 17 The HWCOM mini-sequence in the second year of medical school focuses on case-based approaches toward nutrition and evidence-based medicine when treating individuals with diabetes. Many institutions struggle with case-based approaches, due to a scarcity of faculty for small group facilitation. 18 Facing a similar shortage, the HWCOM approach in this session allows for case-based active learning with minimal faculty because of the small-group-within-a-large-group format.
Sessions such as the one described here can play a role in building towards the 25 hours of nutrition education recommended over the course of a medical school education. As mentioned previously, the increasing recognition of the importance of nutrition in healthcare has led to widespread calls for its integration into medical education. 19 Both students and faculty acknowledge significant gaps in nutrition training, with many medical programs offering inadequate contact hours and failing to prepare future physicians to address nutrition-related health issues effectively.20–22 Systemic barriers, such as a lack of faculty expertise, insufficient accreditation requirements, and low prioritization within curricula, have hindered efforts to enhance nutrition education. Studies indicate that practitioners, particularly those in family medicine and primary care, feel unprepared to provide nutrition counseling, leading to missed opportunities in patient care. 23 Consequently, experts advocate for policy reforms that mandate nutrition competencies and ensure their inclusion in accreditation standards, fostering a healthcare workforce better equipped to address diet-related chronic diseases. 24
To accomplish these calls for a better equipped healthcare workforce, active learning strategies have emerged as effective tools for enhancing medical education, with approaches like problem-based learning (PBL), flipped classrooms, and gamification demonstrating positive outcomes. PBL fosters critical thinking, self-directed learning, and collaboration, although its success depends on structured implementation and institutional support.25,26 Flipped classrooms, which prioritize pre-class preparation and in-class engagement, significantly improve knowledge retention, skill development, and student satisfaction. However, their effectiveness varies based on instructional design, student preparedness, and faculty training.27–29 Gamification, including digital simulations and educational games, enhances student motivation and decision-making by providing interactive learning environments. 30 While these methods improve engagement and competency, their long-term impact and optimal integration into medical curricula require further research and refinement. 31 The case-based learning format described in this study represents just one of a range of possible ways to engage students in nutrition education.
Ideally, this range of approaches would incorporate feedback from both faculty and students in order to achieve the best learning outcomes while respecting student preferences and the need to make the most efficient use of available resources. Despite the advantages of active learning, students and faculty emphasize the need for a balanced approach that integrates both traditional and interactive teaching methods. 32 While students recognize the value of active learning in fostering deeper understanding and clinical readiness, they often struggle with its perceived inefficiency and misalignment with standardized exams. 33 Faculty members, on the other hand, face challenges in implementing resource-intensive strategies such as PBL, which demand additional training and workload adjustments. Studies suggest that well-structured interactive lectures, which blend traditional instruction with active engagement elements, can enhance learning outcomes without compromising efficiency. 34
Promising active learning programs specific to nutrition education often involve a variety of approaches, including online modules, interactive workshops, and practical cooking classes. One such pilot program in Australia with high school athletes showed notable knowledge improvement in an enjoyable, well-accepted format. 35 A condensed, 2-week program at a medical school in Germany, which included similar elements and additional workshops on communication skills and an exploration of global food systems, showed high participant satisfaction and increased conviction among the students of the importance of nutrition. 36 Healthcare workers may be particularly in need of such multi-pronged educational approaches, as they demonstrate poor adherence to dietary guidelines themselves. 37 A flexible approach to nutrition education that incorporates diverse teaching methods—such as case-based discussions, structured lectures, and hands-on activities—ensures that medical students receive comprehensive, engaging, and clinically relevant education while addressing their concerns about time management and assessment preparation.
One strength of the current study is its embrace of a flexible active learning approach, incorporating interactive technology within a short opening lecture, followed by a case-based discussion, tied to tangible real-world tasks faced by future physicians. Other strengths include the session's brief but structured format, its real-world case design, and the integration of SDOH and EBM in nutrition education. Tying together a practical set of guidelines, an opportunity for a quick literature search, and a case-based opportunity to discuss nutritional and social interventions represents a novel approach to nutrition training within undergraduate medical education.
Limitations
The study described here is limited by taking place at a single institution. It would need to be replicated at other institutions to assess its generalizability. It also suffered from varying response rates, due the voluntary nature of student participation in the interactive quizzes and post-course evaluations. Further, the quiz questions involved in the session are admittedly broad and could benefit from further refinement, perhaps with a short answer component to demonstrate higher level engagement. In addition, while this interactive session has the benefit of involving balanced active learning in a format that appears to yield short-term knowledge gains and student satisfaction, it is limited by being one small piece in a much larger curriculum. To be most effective, it would need not only to be integrating into a mini-sequence within one course but within a much larger sequence that unfolded with a balanced use of scaffolded active learning methods over the course of years. In the year after this study concluded, for example, HWCOM underwent a curricular revision, in which the order and timing of the organ systems education was shifted, moving the “critical thinking” session into the first year and perhaps affecting its success.
Future Directions
In the future, in order to better assess longer term knowledge and skill acquisition, we will consider a follow-up study, reassessing the students’ nutritional guidance knowledge and literature search skills, in relation to type 2 diabetes during their clinical rotations. Ideally, the session would be incorporated into a longitudinal nutrition education program that incorporated scaffolded traditional and active learning components. For the upcoming iteration of the course, the investigators also plan on highlighting the role of artificial intelligence (AI) within small group education and as a tool for creating health education materials and for performing a literature search. Students may use AI for aspects of the small group activities, but the emphasis will be on their critical appraisal of the evidence cited and the health education materials produced.
Conclusions
The findings of this study support the hypothesis that an interactive, case-based learning session effectively enhances medical students’ knowledge of nutritional guidance for diabetes management, evidence-based research skills, and awareness of SDOH. The integration of technology-enhanced quizzes demonstrated significant short-term knowledge gains in key areas, particularly in dietary management and literature search methodologies. While improvements in students’ understanding of social determinants were less pronounced, pre-session scores were already high, indicating prior familiarity with the topic. Student feedback remained positive across both cohorts, reinforcing the session's effectiveness while requiring minimal faculty involvement. These results highlight the feasibility of incorporating structured, active learning formats into medical curricula to address critical gaps in nutrition education. Future studies should evaluate long-term knowledge retention and explore expanded integration of nutrition training within a longitudinal medical education framework.
Supplemental Material
sj-docx-1-mde-10.1177_23821205251356096 - Supplemental material for Making It Active: A Cohort Study of a Large-Group Learning Session to Improve Nutrition-Related Knowledge and Skills for Second-Year Medical Students
Supplemental material, sj-docx-1-mde-10.1177_23821205251356096 for Making It Active: A Cohort Study of a Large-Group Learning Session to Improve Nutrition-Related Knowledge and Skills for Second-Year Medical Students by Gregory W. Schneider, Julia Bisschops, Prasad Bhoite and Sabyasachi Moulik in Journal of Medical Education and Curricular Development
Supplemental Material
sj-docx-2-mde-10.1177_23821205251356096 - Supplemental material for Making It Active: A Cohort Study of a Large-Group Learning Session to Improve Nutrition-Related Knowledge and Skills for Second-Year Medical Students
Supplemental material, sj-docx-2-mde-10.1177_23821205251356096 for Making It Active: A Cohort Study of a Large-Group Learning Session to Improve Nutrition-Related Knowledge and Skills for Second-Year Medical Students by Gregory W. Schneider, Julia Bisschops, Prasad Bhoite and Sabyasachi Moulik in Journal of Medical Education and Curricular Development
Footnotes
Acknowledgments
The authors acknowledge the team at the Florida International University Medical Library for its assistance with the background literature search. They are also grateful to the students who participated in this research and the support staff at HWCOM who made this work possible.
Author Contributions
All authors contributed to the study conception and design. Material preparation and data collection were performed by Gregory W. Schneider, Julia Bisschops, Prasad Bhoite, and Sabyasachi Moulik. Data analysis was performed by Prasad Bhoite. The first draft of the manuscript was written by Gregory W. Schneider and all authors commented on that and subsequent versions of the manuscript. All authors read and approved the final manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The data that support the findings of this study were collected during the routine administration of the Endocrine Systems Course within the HWCOM curriculum. The data are available from the corresponding author, Gregory W. Schneider, upon request.
Informed Consent
The study received “Not Human Subject Research (NHSR)” exempt status from the Florida International University Institutional Review Board, IRB NHSR Number IRB-25-0089. Such status provides waiver of consent requirements.
Supplemental Material
Supplemental material for this article is available online.
Appendix A
Appendix B
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
