Abstract
OBJECTIVES
Coronavirus disease 2019 (COVID-19) has profoundly impacted residency and fellowship training and education. However, how and to what extent the COVID-19 pandemic in Lebanon compromised the daily involvement of trainees on the clinical and ethical levels is currently unknown, which this study will shed light on.
METHODS
We conducted a cross-sectional survey (30 questions) targeting medical residents delivering healthcare services in Lebanon. Residents from different specialties were included in the study to assess the effect of the pandemic on their education and the ethical obstacles they faced when dealing with patients.
RESULTS
A total of 221 postgraduate medical students participated in our study. Results showed that about half of the residents (52.1%) were only able to do a basic physical examination rather than a full examination as a mandatory requirement in the residency curriculum. The majority (60%) agreed that the doctor–patient relationship is contravened. In addition, almost all residents suffered from fear and emotional distress that affected their education (83.7%).
CONCLUSION
The findings of this study identify the effect of COVID-19 on residents’ training, which affects treatment outcomes and greatly impacts the mental well-being of both healthcare workers and patients.
Introduction
Patients’ in-hospital care during the COVID-19 pandemic depended heavily on medical residents and fellows, 1 and the latter experienced disruptions to their education as a result of changed responsibilities, including the cessation of learning activities and the reallocation of duties. 2 This change coincided with a documented rise in stress, anxiety, and depression among healthcare workers during infectious outbreaks. 3 Furthermore, the residents faced difficulties in their education including limitations on the type of cases they could handle, a decrease in medical procedures, and a lack of educational conferences. 4
In Lebanon, the first COVID-19 case was reported on December 21, 2019, subsequently straining the country's healthcare system and healthcare professionals. 5 The mandatory lockdowns significantly disrupted normal life, similar to what one might encounter in a warzone field. 6 These changes caused a rise in anxiety and depression nationwide, as well as common psychological responses including confusion, anger, and post-traumatic symptoms. However, such data was mostly reported from local regional quarantines or exposed groups such as medical professionals. 7
This study aims to assess the medical residents’ perception of the COVID-19 pandemic impact, focusing mainly on education, and to a lesser extent on the psychological and ethical challenges facing healthcare frontliners. Recent similar data was reported in Brazil tackling analogous concepts and trying to answer parallel questions, 8 though the data available in the literature concerning those aspects is limited, especially in Lebanon. Therefore, this survey seeks to identify exposure factors affecting their training, evaluate their mental health in the middle of the crisis, and highlight the ethical dilemmas that they encountered in hospital settings.
Methodology
This is a descriptive cross-sectional study conducted in March–April 2021. The study includes postgraduate medical students (residents and fellows) from a list of selected governmental and nongovernmental Lebanese hospitals affiliated with the Lebanese University (LU). Graduates from other universities were excluded due to the pandemic and ethical restrictions.
The LU offers an average of 60 residency positions every year, that's why a total of 300 medical residents were targeted, and most of them showed interest in answering especially after reading the questions list. Some refused to participate for many reasons (eg, laboratory residents don’t have direct contact with COVID-19 patients); the residents were invited via WhatsApp—a smartphone chatting application—to complete the survey through Google Forms, thus no data was missed. Those who agreed to participate were reminded 3 times to complete the survey to increase the response rate, so a total of 221 residents and fellows completed the survey. They belonged to different specialties (internal medicine, surgery, emergency medicine, pediatrics, gynecology and obstetrics, and others), delivering healthcare services at university hospitals all over the country.
The data collection tool is a web-based questionnaire developed and approved by a working research team that entails professors, senior clinicians, and an epidemiologist enrolled in the committee of master's in medical ethics and bioethics of Lebanese University. Information collected from participants included: (1) demographic and socioeconomic data: age, gender, specialty, and year of residency; (2) Hospital characteristics (3 questions), COVID-19 units coverage (3 questions), residents and COVID-19 patient relationship (3 questions), educational impact (15 questions), and psychological impact (2 questions) along with assessment of the feel of guilt in choosing medicine as a career due to overwhelming responsibilities and burnout, especially after increasing reported cases of moral stress and feeling of guilt among COVID-19 frontliners 9 (2 questions) (Annex 1).
A Likert-type scale was used to assess the impact of the COVID-19 pandemic. Participants score each answer from 0 to 4 (with 0 meaning “strongly disagree”, and 4 meaning “strongly agree”). The outcome was kept as a continuous variable, the total score ranges from 0 to 50, and the higher the score the higher the agreement of the residents with the impact of the COVID-19 pandemic. The reporting of this study conforms to the Strengthening the Reporting of OBSERVATIONAL STUDIES IN EPIDEMIOLOGY (STROBE) Statement 10 (Annex 2).
Statistical analysis
Descriptive statistics were conducted for the overall characteristics of the study population by presenting the numbers and percentages for the categorical variables while means and standard deviations for the continuous ones. Inferential bivariate analysis was carried out where independent t-tests and 1-way ANOVA tests were conducted for the continuous variables. Results were presented with P-values, mean, and standard deviation. Multiple linear regression was carried out to adjust for the potential confounding effects of the variables under study. The results were presented with a beta correlation coefficient and 95% confidence intervals (CIs). P < .05 was set as an indicator of statistical significance. The data analysis was done using SPSS 22.
All patients signed an electronic informed consent before the recruitment in the study. Names and information of participant individuals are not to be shared with third parties. All participants had a designated code to conceal their names and identity.
This study's protocol was reviewed and granted written study approval from the institutional review board (IRB) at the Lebanese University, Faculty of Medical Sciences, Division of Medical Ethics (CUER 50-2021 23/Mar/2021).
This study was conducted following the US Code of Federal Regulation 45 CFR 46.107, 21 CFR 56.107, Good Clinical Practice ICH Section 3, and the principles laid down by the 18th World Medical Assembly (Helsinki, 1964) and all applicable amendments.
Results
General characteristics of participating residents
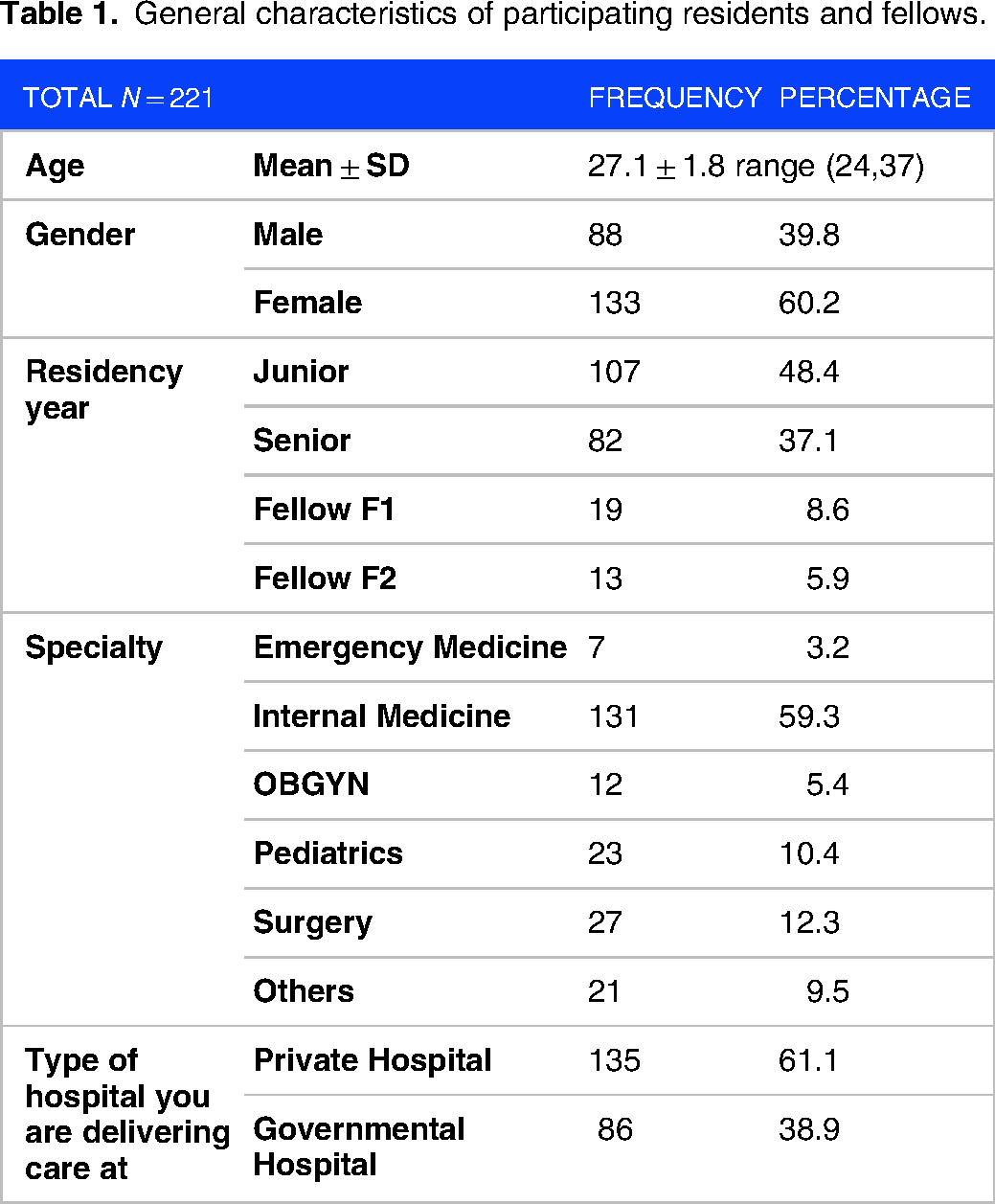
A total of 221 postgraduate medical students including residents and fellows from different hospitals participated in the study (Table 1). The majority of participating residents were females (60.2%) and the average age was 27 years with a range of a minimum of 24 years and a maximum of 37 years old. Almost half of the residents were juniors (48.4%) and 37.1% were seniors while the minorities were fellows (postgraduate residents above 3rd year of residency). Most of the participants were delivering care at private hospitals affiliated with the Lebanese university (61.1%) and internal medicine was the common specialty (59.3%).
General characteristics of participating residents and fellows.
The medical residents’ training during the pandemic
The results showed that the majority of residents noted that their hospital was transformed into centers for receiving COVID-19 cases (75.1%) and considered that this transformation had an impact on the admission of non-COVID-19 patients (80.7%). The survey also showed that 79.2% of the residents were delivering care in COVID-19 units and noted that their involvement was obligatory (68.2%). Interestingly, most of them rated their involvement in the COVID-19 units as being of moderate (38.9%) to minimal (38.9%) benefit to their educational program and medical skills (Table 2).
Hospital characteristics and perceptions towards practicing in COVID-19 units.

Table 3 presents the findings of the survey showing to what extent the doctor–patient relationship and quality of care were altered through the COVID-19 crisis. Half of the participants mentioned that they were able to do the basic physical exam (examine chest/abdomen/lower limb, including auscultation, percussion, palpation… etc) (52.5%) to manage the COVID-19 cases while only 22.2% were able to do the full physical exam (examine all systems). Moreover, the majority of the residents were in full agreement that their minimal contact with patients had affected their proper diagnosis and management of cases (67.9%). When the residents were asked about the impact of the pandemic on the trust of the patients in the provider's service, 61.1% agreed that it badly influenced this relationship.
The doctor–patient relationship during the pandemic.

Table 4 presents the level of agreement of participants on items related to their educational program. Most of the participants (77%) almost agreed that their educational program was affected negatively. The highest proportion of residents disagreed (29%) and strongly disagreed (16.3%) that their educational program was planned adequately to get exposure to different types of clinical practices. They also reflected that the pandemic affected their training program by restricting most of the exposure to COVID-19 cases while reducing the exposure to non-COVID-19 cases (46.6% strongly agreed and 41.6% agreed on that). Moreover, the highest share of the residents and fellows perceive themselves as front liners in patient care and management, in the absence of direct supervision by their attendings (49.3% strongly agreed and 30.8% agreed).
Perceptions of residents and fellows towards the impact of COVID-19 pandemic on their medical educational program.

In terms of elective and non-urgent procedures, most of the participants considered that these were reduced during the pandemic (46.2% strongly agreed and 33.9% agreed on that) and reflected that the exposure to these elective surgeries is considered an essential part of medical practice and capacity building (33.5% strongly agreed and 48.0% agreed on that). Moreover, the highest proportion of residents and fellows didn’t consider that web-based conferences have the same benefit as face-to-face conferences (48.9% disagreed that web conferences have the same benefit as in-person conferences).
As for their perceptions on the long-term impact of the crises on their medical practice, 42.5% of the residents and fellows were uncertain whether the following residency years would recuperate the limitations in the medical training program while 33.9% agreed that. Additionally, more than half of the residents agreed and strongly agreed (41.2% and 14.0%, respectively) that the pandemic will leave a long-term impact on their competence and medical knowledge post-graduation, while 31.7% were uncertain about that.
Mental health and psychological well-being of participants
Almost all residents and fellows suffer from fear and emotional distress not experienced before the pandemic (83.7%). The highest share of residents agreed that their psychological status is affecting their attention and efficacy during the training (52.9% of residents agree and 15.8% strongly agree). The survey also showed that medical graduates are suffering from the feeling of guilt for choosing medicine as a career track due to overwhelming responsibilities and burnout, or even reporting the need to quit the training program: 36.2% mentioned that they feel guilty sometimes while 25.8% feel it frequently. Also, the highest proportion of participants agreed that the COVID-19 pandemic is a key factor contributing to the feeling of guilt and the need to quit (33.5% agree and 14.9% strongly agree) (Table 5).
Mental health and psychological well-being of participants.

Table 6 presents the bivariate analysis of the differences in the scores of COVID-19 impact on medical education and the characteristics of participants including their psychosocial status. No significant differences were reported in the scores by gender, residency year, and specialty, having P > .05. However, the analysis showed that residents practicing in governmental hospitals had higher scores (39.8 ± 3.9) in their perceptions of the impact of COVID-19 on their medical education program in comparison to those who deliver care in private hospitals (38.4 ± 3.6) with a P-value = .008.
Bivariate analysis exploring the differences in the scores of the impact of COVID-19 on medical education and feelings of fear and guilt.

Independent t-test.
One-way ANOVA.
Significant P-value at .005 level of significance.
In terms of fear and emotional distress, participants who are suffering from these emotional fears had a higher score (39.3 ± 3.6) in comparison to those who don’t (37.2 ± 4.4) with a significant P < .03 in terms of the effect of COVID-19 on their educational program. However, the guilt for choosing medicine was not significantly correlated with P = .4. Still, COVID-19 and the guilt for choosing medicine were significantly correlated as those who strongly agreed that COVID-19 had resulted in the feeling of guilt for choosing medicine due to overwhelming responsibilities and burnout, had the highest score (41.2 ± 3.8) with P = .004.
Adjusting for all other variables, the multiple linear regression model showed that fear and emotional distress were correlated with the perception that the COVID-19 pandemic affected medical education with β = 1.8 with a significant 95% CI (0.21, 3.48). Further, the adjusted model showed a significant association between the type of hospital and the score of perception, having those who deliver in private hospitals score lower in terms of their perceptions of the impact of COVID-19 on medical education β = −1.44 with a significant 95% CI (−2.52 to 0.34) (Table 7).
Linear regression model presenting the adjusted correlation for the impact of fear and guilt on perceptions of medical education.

Significant P-value at .005 level of significance.
Discussion
Physicians and other frontline healthcare professionals are particularly vulnerable to negative mental health effects as they strive to balance the duty of caring for patients with concerns about their well-being and that of their family and friends. 11 The pandemic outbreak has caused many difficulties and significant damage to health, the economy, and human relations. It has transformed our world and brought about fundamental changes in human relations and modern civilization. 12
Our recent study has been conducted to assess the effect of this pandemic on residents’ and fellows’ education and to establish how the pandemic psychologically affected the residents and in turn, affected the ethical principles in treating patients. 13 To our best knowledge, this is the first study that compared the physical and mental health as well as knowledge, attitude, and beliefs about COVID-19 of Lebanese medical residents. The most important implication of the present study is to understand the ethical challenges that face Lebanese medical residents.
The cross-sectional study of A. L. Mcguire et al done in the United States showed that during the COVID-19 pandemic, residents faced many ethical challenges; this study reported that more than 60% of the residents agreed that this pandemic affects negatively the relationship between residents and the patients, as a most important concern of the residents was to protect themselves and to protect their family from being infected. 12
These results are consistent with our survey, which showed that 61.1% of residents agreed that COVID-19 affected their relationship with patients negatively. This was mostly contributed by the minimal contact with patients in which only about half of the residents mentioned that they could do only the basic physical exam and only 22.2% could do the full physical exam. Moreover, the minimal contact with patients affected the proper diagnosis and management of cases. So, this can target the 2 main ethical principles of beneficence and non-maleficence. Yet, a study by Hope O. Nwoga, done in China, showed the doctor–patient relationship as reported by the doctors. The majority of the doctors reported that they still take time to listen (89.2%) to their patients and give time to them to make decisions about their treatment (78.0%). 14 However, similar to our findings, only 11.8% of the doctors still do thorough physical examinations on their patients.
An international study done by A. T. Gloster et al reported that one of the most immediate changes introduced to the training programs has been the broad cancellation of in-person medical meetings and conferences, mostly being replaced by recorded lectures, live streams, or webinars. One reason is to flatten the curve; to minimize personal interactions to mitigate and contain the spread of COVID-19. Another reason is to decrease the risk of exposure for trainees, which is an understandable concern. However, many are willing to put themselves at risk and, as such, can be frustrated by these decisions. 15 Our study supported this fact, where most of the students agreed on the less benefit of web-based education compared to face-to-face.
In our study, 29% of the residents disagreed and 16.3% strongly disagreed that their educational program was planned adequately to get exposure to different types of clinical practices. It affected their training program by restricting most of the exposure to COVID-19 cases (38.9% strongly agreed and 28.6% agreed on that) while reducing the exposure to non-COVID-19 cases (46.6% strongly agreed and 41.6% agreed on that). As outpatient volume reduced drastically during this pandemic with the cancellation of non-urgent and non-COVID-19 clinic appointments, most of these consultations happened over the cell phone or through video calls on smartphones. 16 This can be the reason that contributed to the minimal referral of non-COVID patients to the hospitals and explains the reduced exposure of residents to these patients.
Interestingly, the majority of residents noticed that their involvement in treating COVID-19 patients was obligatory, and this sheds light on the lack of well-organized consent regarding their work as front liners. Moreover, this might explain one of the reasons behind the agreement of the greatest proportion of residents (38.9%) that their involvement in the treatment of COVID-19 patients had minimal effect on their education, and that is because they didn’t volunteer for this training.
Reduced non-COVID-19 patient services, both outpatient and inpatient, severely mitigated the opportunities for trainee residents to perform essential procedures. As reported, before the COVID-19 era, residents were likely to see a broad spectrum of cases varying from routine uncomplicated to life-threatening severe cases; however, their focus has now shifted to COVID-19. Their educational program was planned adequately to get exposure to different types of clinical practices, 17 and these findings are in line with our survey that reflects the effect of the pandemic on the training program by restricting most of the exposure to COVID-19 cases (38.9% strongly agreed and 28.6% agreed on that) while reduced the exposure to non-COVID-19 cases (46.6% strongly agreed and 41.6% agreed on that). Moreover, concerning elective and non-urgent procedures, a significant proportion of residents agreed on the great reduction of such actions during the COVID-19 era and reflected that exposure to these elective surgeries is considered an essential part of medical practice and capacity building.
Additionally, more than half of the residents agreed and strongly agreed (41.2% and 14.0%, respectively) that the pandemic will leave a long-term impact on their competence and medical knowledge post-graduation, while 31.7% were uncertain about it. These findings support the conclusion of Patil et al study. 18
The highest share of residents agreed that their psychological status is affecting their attention and efficacy during the training (52.9% of residents agree and 15.8% strongly agree). 11 Another study showed that fear and emotional distress are correlated with the perception that the COVID-19 pandemic affected medical education. 19 These findings are also supported by our results, however, in our study, a comparison was done concerning gender, year of residency, specialty, and type of the hospital (governmental and nongovernmental) where no significant difference was noted (P > .05) except for the residents in governmental hospitals who showed significant impact by the pandemic on their training compared to those rotating in private hospitals.
It seemed, however, that physicians experienced similar amounts of anxiety regardless of their gender and contact with COVID-19 patients. Both stress and anxiety had a strong effect on the overall well-being of physicians.12,20 Students were afraid that confinement and learning online would hinder their progress in their studies, 21 and this can stand behind the fear noticed by the participants who had a higher score (39.3 ± 3.6) in comparison to those who didn’t (37.2 ± 4.4) in terms of the effect of COVID-19 on their educational program. Furthermore, 41.2% strongly agree that COVID-19 has resulted in the feeling of guilt for choosing medicine due to overwhelming responsibilities and burnout as healthcare workers facing the pandemic.
This is the first study in Lebanon that highlighted how fear and anxiety affected the quality of education and knowledge the residents are getting from their training; their knowledge only focused on COVID-19 and its consequences on the patient and the community. As mentioned before, 29% of the residents disagreed and 16.3% strongly disagreed that their educational program was planned adequately to get exposure to different types of clinical practices. In addition, in this study, we found that many residents regret choosing medicine as their major due to their fear of COVID-19 on themselves and their families. However, other studies fail to mention this information in their data.
Limitations
Our study faced several limitations. First, there might be some information bias, as a cross-sectional study the survey was done during the pandemic in Lebanon, and this is essential because our results tend to be more significant, however, if the questionnaire was completed before or after the pandemic, results would be less significant. Second, using an online non-pilot-tested questionnaire put us in front of multiple limitations including nonresponse bias and some missing data, especially since the questionnaire was designed to be easily and quickly filled. Further, the unavailability of a suitable validated questionnaire that aligns perfectly with our specific research objectives and variables of interest led us to create the questionnaire we used without pilot-testing it due to the financial difficulties and shortage in time. Finally, a lot of residents were difficult to reach or didn’t respond, but the 220 respondents, contacted from all over Lebanon, represented around one-third of all Lebanese medical residents, though no sample size/power analysis was performed for this study. Our survey can act as a basis for further future studies that can follow the progress of education and compare the results, also different specialties each on its own can be targeted to improve training, and medical practice and overcome such challenges. Potential selection bias and sampling limitations may limit the generalizability of this study to the entire population. Thus, this study sample may not accurately represent the broader population, rendering the external validity of the findings limited.
Practice implications
This study sheds light on the necessity for better planning and management of the residents’ training programs, especially at times of health crises that would lead to mental distress such as anxiety and depression. This might include offering psychological support programs for trainees at all levels.
Conclusion
The COVID-19 pandemic has been classified as a traumatic event, and healthcare workers had the most direct and longest exposure to this disease. The present COVID-19 pandemic has negatively impacted certain aspects of the doctor–patient relationship which may in the long run influence treatment outcomes, especially as the pandemic is ongoing. This crisis greatly impacts healthcare workers’ mental health, and this was reflected unfavorably from different aspects medically and ethically on admitted patients. This problematic issue is worth addressing in times of pandemics and also would be further studies on how to minimize the effect of different possible pandemics on the quality of clinical training of medical trainees and how to avoid possible ethical concerns.
Supplemental Material
sj-docx-1-mde-10.1177_23821205241262685 - Supplemental material for Professional and Psychological Influence of the COVID-19 Pandemic on the Training of Medical Residents
Supplemental material, sj-docx-1-mde-10.1177_23821205241262685 for Professional and Psychological Influence of the COVID-19 Pandemic on the Training of Medical Residents by Ali Kanso, Natasha Homsi, Ali R. Chaitou, Imadeddine Farfour, Hussein Wehbe, Lubna Tarabay and Fadi Abou-Mrad in Journal of Medical Education and Curricular Development
Supplemental Material
sj-docx-2-mde-10.1177_23821205241262685 - Supplemental material for Professional and Psychological Influence of the COVID-19 Pandemic on the Training of Medical Residents
Supplemental material, sj-docx-2-mde-10.1177_23821205241262685 for Professional and Psychological Influence of the COVID-19 Pandemic on the Training of Medical Residents by Ali Kanso, Natasha Homsi, Ali R. Chaitou, Imadeddine Farfour, Hussein Wehbe, Lubna Tarabay and Fadi Abou-Mrad in Journal of Medical Education and Curricular Development
Footnotes
Acknowledgments
We would like to thank our colleague Aya Noubani for guiding the analysis of the research and reviewing the first manuscript draft. We further thank Nancy Zeaiter, MD, Salim Barakat, MD, Hussein al-Husseiny, MD, and Hussein Moussa, MD, who greatly assisted the research during the data collection.
Author Contributions
All authors helped with the conceptualization. Ali Kanso and Natasha Homsi made equal contributions to every aspect of the study; they also created the questionnaire under the direct supervision of Drs. Fadi Abou-Mrad and Lubna Tarabay. All authors—Hussein Wehbe, Ali Kanso, Natasha Homsi, Ali R. Chaitou, and Imaddedine Farfour—contributed to the data collection. Ali Kanso handled the data analysis, with Aya Noubani serving as the supervisor. Hussein Wehbe and Imadeddine Farfour were in charge of authoring the results section and describing the tables. The final draft of the work was reviewed and approved for submission by Lubna Taraby and Fadi Abou Mrad. Lastly, submission and reviewers’ response management fell to Ali Kanso and Ali R. Chaitou.
Consent to Participate
All patients signed an electronic informed consent before the recruitment in the study. Names and information of participant individuals are not to be shared with third parties. All participants had a designated code to conceal their names and identity.
DECLARATION OF CONFLICTING INTERESTS
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Considerations
This study's protocol was reviewed and granted written study approval from the institutional review board (IRB) at the Lebanese University, Faculty of Medical Sciences, Division of Medical Ethics (CUER 50-2021 23/Mar/2021). This study was conducted following the US Code of Federal Regulation 45 CFR 46.107, 21 CFR 56.107, Good Clinical Practice ICH Section 3, and the principles laid down by the 18th World Medical Assembly (Helsinki, 1964) and all applicable amendments.
FUNDING
The authors received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
